Breastfeeding by Assoc Prof Dr Susanha Yimyam Faculty

Breastfeeding by Assoc. Prof. Dr. Susanha Yimyam Faculty of Nursing, CMU
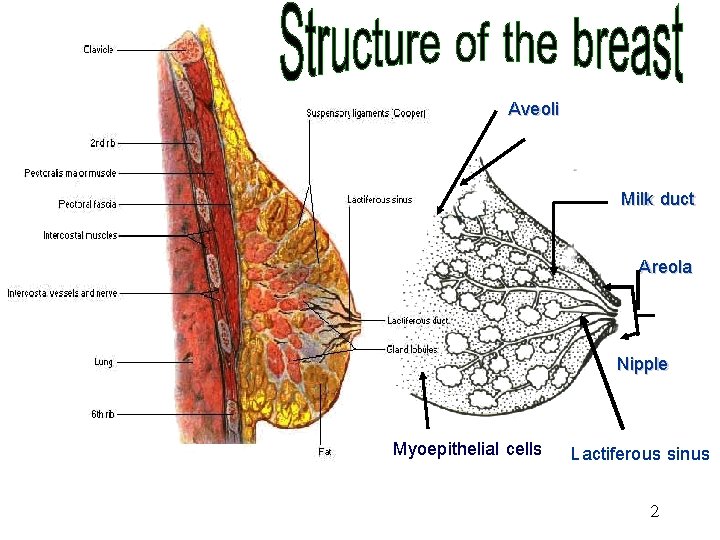
Aveoli Milk duct Areola Nipple Myoepithelial cells Lactiferous sinus 2
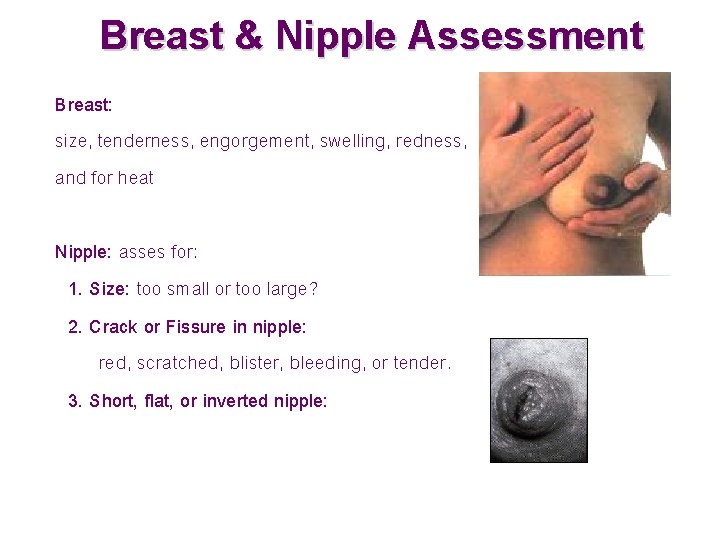
Breast & Nipple Assessment Breast: size, tenderness, engorgement, swelling, redness, and for heat Nipple: asses for: 1. Size: too small or too large? 2. Crack or Fissure in nipple: red, scratched, blister, bleeding, or tender. 3. Short, flat, or inverted nipple:
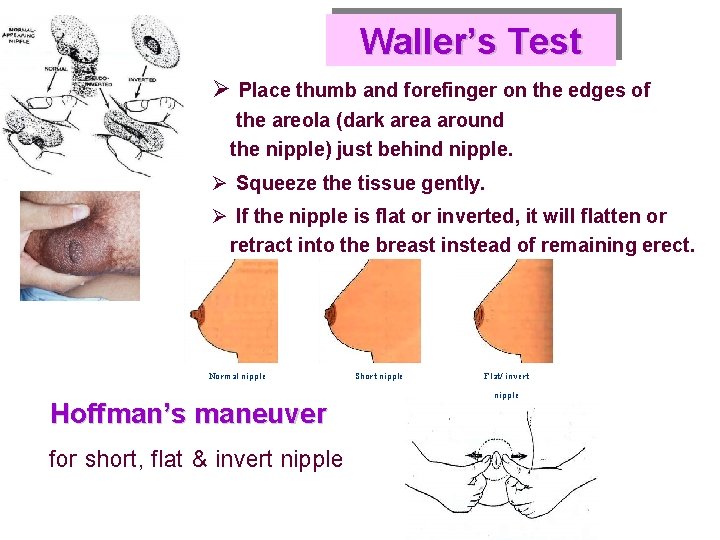
Waller’s Test Ø Place thumb and forefinger on the edges of the areola (dark area around the nipple) just behind nipple. Ø Squeeze the tissue gently. Ø If the nipple is flat or inverted, it will flatten or retract into the breast instead of remaining erect. Normal nipple Hoffman’s maneuver for short, flat & invert nipple Short nipple Flat/ invert nipple

Assessment for Successful Breastfeeding Influencing factors: 1) Maternal factors: - Mother’s beliefs, attitudes, and intention - Mother’s knowledge: learn about the mechanism of milk production and ejection, foods & beverages that promote lactation drink as well as appropriate rest. 2) Infant factors: - Physical abnormalities or other sucking problems. Examined and tested for sucking reflex. 3) Health care provider factors: play an important role to promote and support breastfeeding. Empower mothers to be confident when breastfeeding. Nursing consultation for better care Other factors: advertisement of formula during hospital stay & hospital policy; separation of infant and mother after birth. 5

Preparation for Breastfeeding 1. Breast & nipple care: clean water while bathing; avoid applying soap or chemicals to nipple and breast. 2. Breast massage: promote the let-down reflex for producing and ejecting milk. 3. Separation from infant, express breast milk 10 -12 T/day, then at least 10 T/day thereafter, to stimulate prolactin 4. Suitable maternity bra: supports breasts to prevent pressure against the milk duct & deformity of breasts as well as relieve pain. No wire bras.

Preparation for Breastfeeding 5. Healthy foods, consume about 500 Kcal’s and drink about 2, 000 -3, 000 ml more than pre-pregnancy consumption per day. High protein, milk every day. Avoid salty, sweet and preserved foods, alcohol and caffeine beverages and foods that create gas such as those found in the cabbage family (all cabbage, broccoli, cauliflower) and some beans. Consult physician before taking any medication 6. Adequate rest (8 -10 hours at night and 1/2– 1 hour at midday). 7. Appropriate postpartum exercise daily. 8. Relaxation both physically and mentally.

Techniques for breastfeeding The principle of ‘three suckling’: promptly suckling, frequent suckling and correct suckling. • Promptly suckling: WHO & UNICEF start at ½ - 2 hrs after birth: sensitive period. It also helps establish early bonding.

Techniques for breastfeeding The principle of ‘three suckling’: promptly suckling, frequent suckling and correct suckling. • Frequent suckling: breastfeeding every 23 hrs in order to increase milk production and ejection, and decrease infant jaundice. After initiating breastfeeding, the mother should then breastfeed on demand, or at least every 3 hours during the day and at least every 4 hours at night.

Techniques for breastfeeding The principle of ‘three suckling’: promptly suckling, frequent suckling and correct suckling. • Correct suckling is very important because most breastfeeding problems occur from incorrect suckling. 10

. 1 Wash mother hands before breastfeeding. . 2 Awake the infant to breastfeed. 3 Privacy, quiet place for relaxation and concentration. . 4 Position properly for optimal breastfeeding: cradle hold, clutch position or football hold, modified clutch position and side lying position. 11
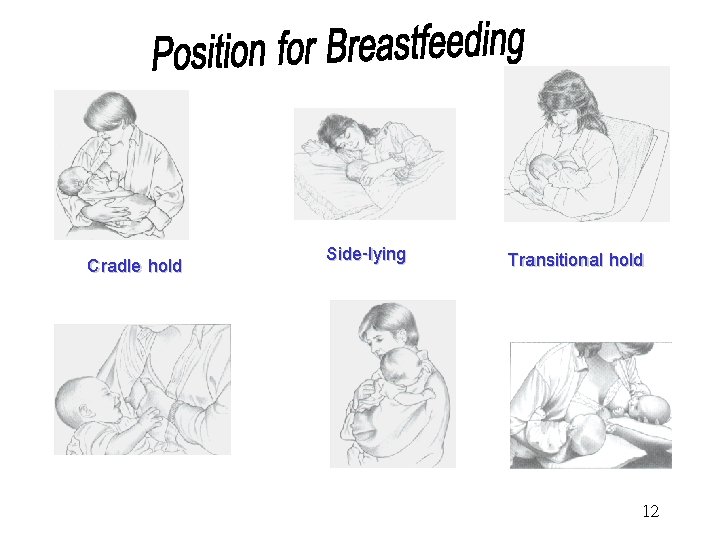
Cradle hold Side-lying Transitional hold 12

5. Mother supports her breast is compressed slightly so that an adequate amount of breast tissue is taken into the mouth with latch-on. 6. During breastfeeding: Eye contact, the infant’s gum on areola, stimulate infant awaken to feed once again if the infant stops sucking. 7. Breastfeed on both breasts; feeding about 10 -15 minutes to stimulate prolactin and oxytocin and not express the milk as it is considered to be ‘hind milk’ that is, higher energy (richer in fat) than ‘fore-milk’. 13
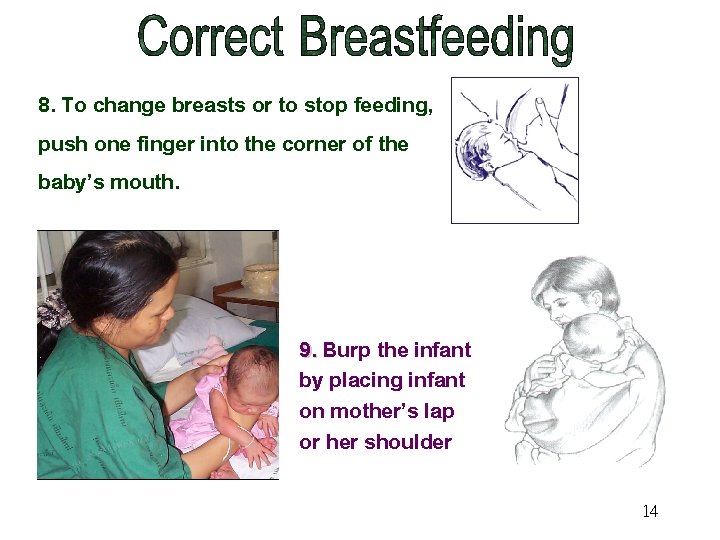
8. To change breasts or to stop feeding, push one finger into the corner of the baby’s mouth. 9. Burp the infant by placing infant on mother’s lap or her shoulder 14

10. Not supplement the child’s diet with formula, food or drink except when medically indicated. 11 No artificial treats or pacifiers: pacifiers nipple confusion. If not suckling from breast; medicine dropper or cup. 12. Manual express breast milk at least 6 -8 times a day for 10 -20 minutes in each time. 15

Objective: Promote let-down reflex by stimulating milk production & ejection. . 1 Conducted after bathing as the mother’s hands & body is clean. 2 Begin at the base of the breast close to areola to remove breast milk from milk ducts through lactiferous sinus, which is located under areola. 3 Methods 3. 1 Mother applies one hand to support the breast and then apply 4 fingers of another hand side to deep circular massage from the base of breast into areola. 16
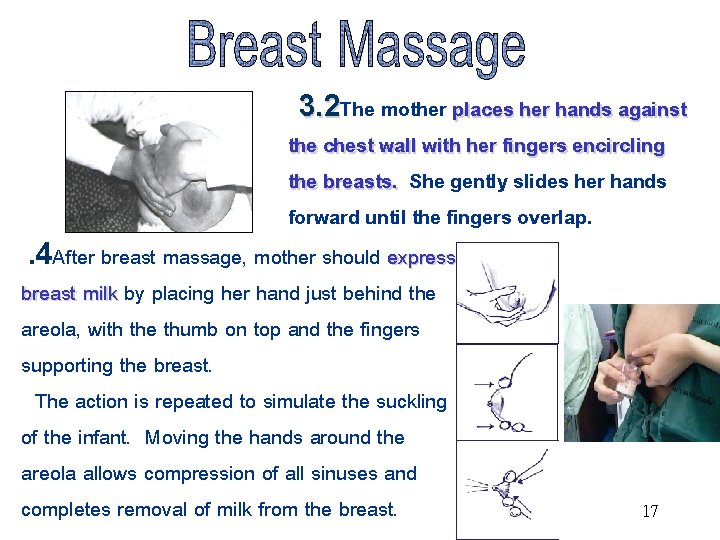
3. 2 The 3. 2 mother places her hands against the chest wall with her fingers encircling the breasts. She gently slides her hands forward until the fingers overlap. . 4 After breast massage, mother should express breast milk by placing her hand just behind the areola, with the thumb on top and the fingers supporting the breast. The action is repeated to simulate the suckling of the infant. Moving the hands around the areola allows compression of all sinuses and completes removal of milk from the breast. 17

5. Suggest appropriate bra for supporting breasts. . 6 Begins breast massage until milk produces enough to satisfy the infant’s need: 6. 1 The infant can sleep for 1 ½ - 3 hours 6. 2 For exclusive breastfeeding, urine output of infant is about 6 -8 times/day. 6. 3 The infant will increase weight about 125 gm. /day or observation of infant’s skin. 18

• Insufficient breast milk supply • Engorged breast - Hot compression Expression of breast milk • Crack or Fissure in nipple • Short, flat, or inverted nipple • Inhibition of breast milk 19

Causes: -Delayed initiated breastfeeding, seldom suckling, and incorrect suckling. - Supplementing with other foods or drink. - Maternal malnutrition. - Postpartum hemorrhage and/ or postpartum infection. - Medications (oral pill). - Lack of confidence in breastfeeding. - Undesired breastfeeding. - Maternal stress and anxiety. - Fatigue or insufficient rest. 20

Problem solving: -Increase frequency & duration of suckling on demand. - Correct suckling for mother’s and infant’s position. - Mental support mother for physical and mental relaxing - Encourage confidence & support breastfeeding. - Encourage hot compresses and breast massage to promote let-down reflex - Using lact-aid nursing. - Suggest mother get adequate foods & drink. - Suggest mother get adequate rest. - Prevent hemorrhage and infection - Consult physician before taking any medications. 21
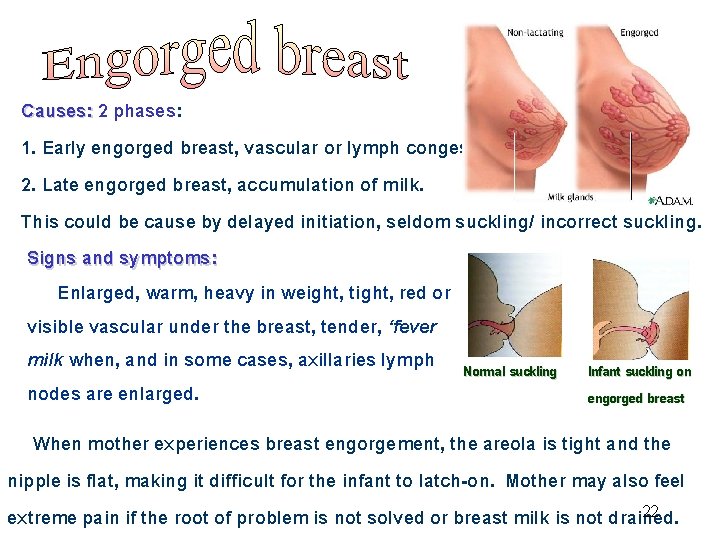
Causes: 2 phases: 1. Early engorged breast, vascular or lymph congestion. 2. Late engorged breast, accumulation of milk. This could be cause by delayed initiation, seldom suckling/ incorrect suckling. Signs and symptoms: Enlarged, warm, heavy in weight, tight, red or visible vascular under the breast, tender, ‘fever milk when, and in some cases, axillaries lymph Normal suckling Infant suckling on nodes are enlarged. engorged breast When mother experiences breast engorgement, the areola is tight and the nipple is flat, making it difficult for the infant to latch-on. Mother may also feel 22 extreme pain if the root of problem is not solved or breast milk is not drained.

Prevention: 1. Suggest mother to breastfed frequently, every 1 -2 hours or 10 -12 times a day during a few days after birth, then every 2 -3 hours or 10 times a day. The infant should be breastfed on both breasts and after breast milk is wellestablished on demand. If the infant cannot suck, the mother should express breast milk. 2. Exclusive breastfeeding; no supplementing foods or drink. 23

Problem solving Early engorged breast 1. Remind the mother this is normal & will disappear within a few days. 2. Encourage infant to feed on schedule with correct suckling until milk is finish or breast is soft. 3. Before breastfeeding, mother should apply hot compresses to the breast since. 4. Breast massage in order to soften breast and nipple. 5. If mother feels extreme pain during feeding, medicine can be given to relieve pain. 6. Suggest mother to wear appropriate bra. 7. If mother does not feel better within 24 hours, she should consult with her physician. 24

Late engorged breast 1. Encourage the infant to suck frequently and correctly. 2. After breastfeeding, mother should express breast milk by hands or electric breast pump, in order to relieve pain from breast and enhance milk production. 3. Suggest mother to wear suitable bra for support. Electronic Pump 25

Objective: Promote pain relief during milk production. Procedure: 1. Position mother in a comfortable sitting. 4. Help mother remove her blouse and place it under her axillaries. 5. Use a big towel to cover mother’s lap to prevent from getting wet. 6. Place a towel in warm water; wrings and compresses mother’s breast slight rolling. 7. Re-dip towel in warm water and repeat until mother feels comfortable. 8. Wipe nipple dry. Encourage mother to wear a well-fitting bra. 26

Objectives: 1. Relieve engorged breast pain. 2. Stimulate regular and continued milk production for infant feeding especially LBW infants whose hospital stay is long. 3. Collect milk for hospitalized infant or during outside work. 4. Stimulate the milk glands. Procedure: 1. Wash hands before expressing milk. 2. Remove her blouse and place it under her axillaries. 3. Use large towel to cover mother’s lap to prevent her from getting wet. 4. Hot compress & Breast massage. 27

Procedure (Cont. ): 5. If mother does not desire to collect breast milk, she can express milk into the kidney bowl. 6. If mother would like to keep breast milk for infant, mother should clean the nipple with a wet cotton, then, squeezing milk for 2 -3 times before start to collect milk and next, squeezing milk through the milk container (bottle). While expressing milk, the mother should slightly bend her body down so that the milk will flow into the container. The mother’s breast should not touch the bottle. Once the 28 bottle is filled, it should be stored in the refrigerator or in

Procedure: 1. Wash hands before breast pump. 2. Remove her blouse and place it under her axillaries. 3. Use a large towel to cover mother’s lap for prevents mother to get wet. 4. 1 Mother uses unskilled hand to support breast, wellfitted covering the flange over the areola, a collecting chamber is under. Slight squeeze a bulb as creating a vacuum and gentle releasing it, then milk flows to a collecting glass-chamber. Next, move a rubber bulb pump carefully and pours milk to the container. 29

4. 2 Like hand breast pump, mother uses unskilled hand to support breast, well-fitted covering the flange over the areola, a collecting chamber is under. Then, milk flows to a collecting glass-chamber by electric mechanism. Repeat expression until clear both side breast pump. 5. Storage in freezer. 6. Feeding breast milk via cup 30

Causes: 1. Incorrect position/ breast engorgement: tight and flat areola, infant is able to suck only the nipple instead of areola. Lactation is decreased so as to cause the infant sucks vigorously, accordingly increasing inflammation. 2. Mother does not break the suction before removing the infant from the breast. 3. Incorrect nipple cleaning such as rubbing vigorously while bathing or using soap to clean the nipples. 31

Preventions: 1. Correct breastfeeding positioning, lubricate the nipple by mother slight squeezes the breast and applies breast milk to the nipple. Open the infant’s mouth wide before latching on, well-fit hold during breastfeeding by chin-breast. If mother feels nipple pain after 1 -2 minutes of sucking, remove the infant from the breast and try to latch on once again. 2. Do not drag the nipple from the infant’s mouth while infant is sucking. 3. Clean the nipples no more than twice a day. 4. Breastfeed frequently or follow infant’s demand in order to engorged breast, and then infant strongly suckling. 32

Problem solving: 1. Evaluate breastfeeding position of mother, breast and areola engorgement. 2. Feed on the less-sore breast first. 3. Gently massage the sore nipple before feeding & Express a little milk by hand in order to help the infant to latch-on well. 4. Suggest mother to hold the infant in a comfort position & alternate positions of feeding to prevent repeated suckling point. 33
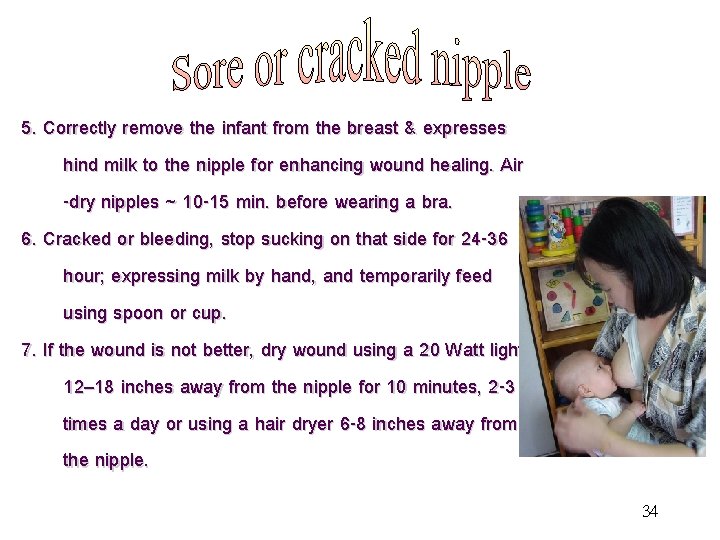
5. Correctly remove the infant from the breast & expresses hind milk to the nipple for enhancing wound healing. Air -dry nipples ~ 10 -15 min. before wearing a bra. 6. Cracked or bleeding, stop sucking on that side for 24 -36 hour; expressing milk by hand, and temporarily feed using spoon or cup. 7. If the wound is not better, dry wound using a 20 Watt light 12– 18 inches away from the nipple for 10 minutes, 2 -3 times a day or using a hair dryer 6 -8 inches away from the nipple. 34

Problem solving: 1. Assure mother that her infant is able to suck. Infant may not adequately grasp the areola early on. If mother is patient and trains the infant to suck frequently, within 1 -2 weeks the areola will become more elastic and the infant can grasp the areola properly. 2. Mother should pull the nipple before breastfeeding by one of these methods 2. 2 Nipple puller including: 2. 1 Hoffman’s maneuver 35

Problem solving (Cont. ): 3. Assist the mother to correctly position the infant. 4. Mother supports the breast and then compresses hand around the lateral margin of the areola in order to reduce the areola size for ease of latching-on. 5. In case of extreme breast engorgement, compressing with warm water & then express a little milk to soften areola in order that infant will latch on well. 6. In case the nipple does not erect, suggest that the mother use a nipple shield, which is made of thin rubber to help the infant breastfeed. 36

Problem solving (Cont. ): 7. Apply Lact-aid-nursing by using formula supplementation during breastfeeding. 8. In case the nipple shield does not work, suggest mother to express milk and cup-feeding. 9. After the infant is satisfied, suggest mother to cover nipple with a breast cup by gently inserting the nipple through the hole, then rotate the air-hold to the top and the base of a breast cup presses on areola then the nipple is everted. 37
Indicators: 1. Infant death. 2. Infant with congenital defect or illness, premature labor, cleft lip or palate, and abnormal GI system. 3. Infant has allergy to mother’s milk. 4. Mother has HIV infection, heart, pulmonary disease, or other disease. 5. Mother receives medication that can transport through breast milk. 6. Mother has intensive mastitis. 7. Mother has psychological or neurological problem. 38
Procedure: 1. Suggest mother to wear a supportive bra 2. 2. Do not express, suck, pump or massage the breast as this will encourage engorgement. 3. 3. Do not place heat compress on breasts as it will stimulate vasodilatation and milk glands to 39

References Lowdermilk, D. L. , Perry, S. E. , & Piotrowski, K. A. (Eds. ). (2004). Maternity & Women’s Health Care (8 th Ed. ). St. Louis: Mosby. Pillitteri, A. (2003). Maternal & Child Health Nursing: Care of the childbearing & childrearing family (4 th Ed. ). Philadelphia: Lippincott Williams & Wilkins. Reeder, S. J. , Martin, L. L. , Koniak-Griffin, D. (1997). Maternity Nursing (18 th Ed. ). New York: Lippincott. Varney, H. (1997). Varney’s Midwifery (3 rd Ed. ). Sudbury, MA: Jones and Bartlett Publishers.

Question & Answer Thank You for Your Attention
- Slides: 41