Breastfeeding and Growth Oregon WIC Inservice August 2020

Breastfeeding and Growth Oregon WIC In-service August 2020 Certifiers must complete this in-service by 12 -31 -2020. It may be completed individually.

Identify signs a breastfeeding baby is growing well. Identify babies at risk for low weight gain. Objectives Make appropriate referrals for low weight gain. Provide culturally responsive breastfeeding support. Practice balancing promotion of breastfeeding with honoring parents’ feeding decisions.

How do we measure infant growth?

Typically, all babies are weighed by their health care provider at birth and regularly for the first few weeks. WIC provides a valuable service by offering weight checks whenever parents are concerned about their baby’s weight.
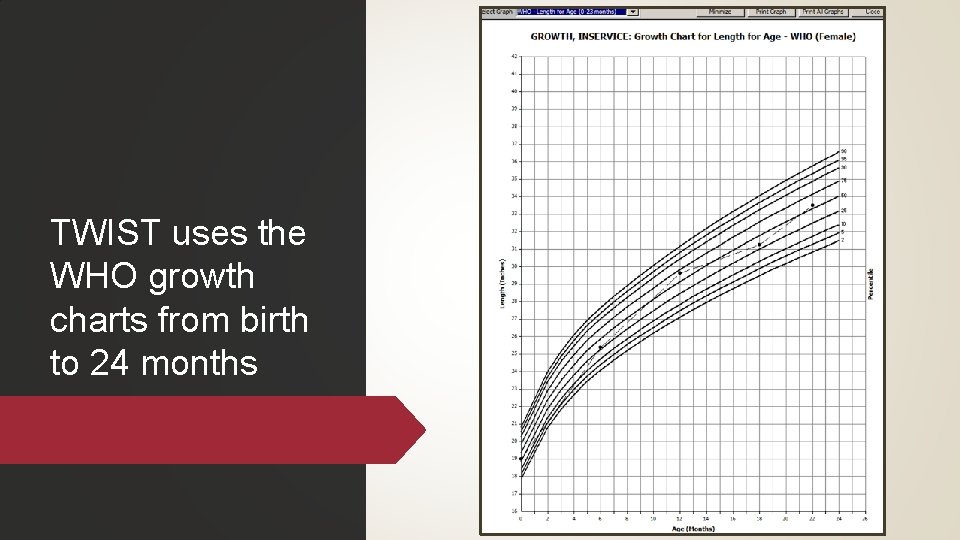
TWIST uses the WHO growth charts from birth to 24 months

Released in 2006 based on new data. About the WHO growth charts Based on healthy breasted infants living in six countries in well-supported environments. CDC (Centers for Disease Control), NIH (National Institutes of Health) and AAP (American Academy of Pediatrics) all agree on their use.

The infants measured to create WHO growth charts were: Mostly breastfed for at least 4 months Breastfed until at least 12 months Fed complementary foods starting at about 5 ½ months

Using breastfed babies to create the WHO growth charts shows how babies grow in healthy environments when fed human milk. . This creates breastfeeding babies as the “normal” for infant growth. Using breastfed babies to create the Research shows growth patterns of WHO growth how breastfed andcharts formulashows fed babies are babies growdifferent. in healthy environments when fed human milk. In the first year, healthy babies fed human milk gain weight more slowly than formula fed babies. Differences in weight patterns continue after solid foods are introduced. https: //www. cdc. gov/nccdphp/dnpao/growthcharts/who/index. htm

Why are newborn babies monitored for weight loss?
Monitoring newborn weight loss It is normal for some babies to lose a little weight after birth. All babies should be monitored to make sure they don’t lose too much weight. Weight loss can be an early sign of feeding or medical problems.

Role of WIC staff WIC weighs babies as requested by parents and also as part of certification to assess risk. Babies should also be followed regularly by their health care provider to monitor weight gain in the first few weeks. If you encounter newborn weight loss, it is important you ensure the baby is followed by a lactation specialist or the health care provider right away.

The WIC data system automatically assigns Risk 135 or 103 if infant weight loss meets certain criteria.

Risk 135 – Infant Weight Loss Birth to 6 months Infants birth to 1 month of age: Weight loss of greater than or equal to 7% of birthweight Infants from 2 weeks to 6 months of age: Any weight loss based on two weight measurements taken at least 8 weeks apart Risk 103 – Underweight Infants and Children Infants under 24 months of age: Weighing less than or equal to the 5 th percentile weight for length

Risk 135 and Risk 103 are HIGH RISK and require a referral to the RDN/WIC nutritionist For breastfed babies, make an urgent referral to the IBCLC or designated breastfeeding expert for your clinic.

How have you helped families? THINK ABOUT How have you helped a family concerned about whether or not their baby was growing enough? How were they feeling? How did you feel helping them? What worked well? What would you change for next time?

Do parents of breastfeeding babies worry more about growth?

Yes. Here are some reasons worry is common: Breastfed babies often gain weight more slowly. Parents cannot “see” how much the baby is taking in. Right after birth, breasts produce colostrum and do not feel full. Mature milk and feeling of breast fullness usually happens by day 3. If a pump is used, very little milk comes out in the first few days. Negative or unsupportive comments undermine the parents’ confidence.

Signs a breastfeeding baby is growing well Baby has adequate wet and dirty diapers Baby is satisfied after feeding Baby’s weight gain is following the channel lines on the growth chart Baby is active and alert when awake After the first few days, the breasts feel softer after feedings Any nipple pain is mild and resolves during and between feedings Also see Is Baby getting enough milk? at Kellymom. com and Why babies breastfeed often available on WIC Shopify

Most babies will grow normally It is important to identify those who aren’t growing enough.

The most common cause of low weight gain is not feeding frequently enough in the first few weeks. Delaying feeding because of visitors Not recognizing early feeding cues Parent’s fatigue Desire for baby to sleep longer Delaying feeding due to pain or frustration with feeding Scheduling feedings

Some newborns are at higher risk for low weight gain. These problems may lead to low weight gain: INFANT Mouth or tongue problems, weak suck Latch problems Neurological issues Medical problems Born preterm or post term Small or large for gestational age BREASTFEEDING PARENT First baby Cesarean or difficult delivery Flat or inverted nipples Prior breast surgery Separation from baby Medications during pregnancy Medical problems Postpartum depression LEAARC, p 343

No transition stools on day 3 – 4 No yellow stools by day 5 Failure to regain birthweight by day 7 Poor muscle tone, weak Signs of dehydration (dry mouth, concentrated urine, crystals in urine, sunken soft spot) Weak cry Very sleepy with infrequent feeding Constantly fussy with frequent feeding Red flags for infant growth (first 28 days) LEAARC, p 344

Red flags require an urgent referral Yield to your designated breastfeeding expert Recommend the parent call the baby’s health care provider This Photo by Unknown Author is licensed under CC BY-SA

1. Protect breastfeeding Babies with inadequate weight gain may need supplementation in addition to feeding at the breast • Get help to identify and fix breastfeeding problems. • Direct observation is needed to evaluate the breastfeeding dyad. • If needed, provide a breast pump to build or maintain breast milk production. • Handouts on hand expression and pumping are available from Oregon WIC Shopify. 2. Make sure baby is adequately fed • If supplementation is needed, it is best to use the parent’s expressed milk. If the parent’s expressed milk is not available, supplement with donor human milk or formula. • Supplementation may be temporary until breastfeeding challenges are resolved.

Social determinants of health Where we live and who we are in our society has an impact on our overall health, including pregnancy, delivery and breastfeeding. Due to systemic and historical oppression, parents who are Black, Indigenous and people of color are more likely to have a cesarean birth, birth complications and give birth to low birthweight infants, which puts the baby at higher risk for low weight gain. Transgender and non-binary parents may have a reduced milk production.

In your clinic THINK ABOUT What have you observed related to the social determinants of health? What has helped in your efforts to support the breastfeeding relationship?

Staff with the same cultural background may provide the most support for historically underserved groups. In cases when this is not possible, listening to the parent’s beliefs about breastfeeding will enhance your breastfeeding support.

The Healthy Children Project Center for Breastfeeding has many blog articles about how different lived experiences can affect breastfeeding. On the right side of this slide are links to articles which focus on breastfeeding experiences from different cultural perspectives. Choose one or two to read that reflect the people served in your community. (Each article takes about 5 minutes read) to Generational trauma among Native American cultures affects infant feeding Changing the narrative around infant feeding in Hmong population Breastfeeding in shelters Breastfeeding as an act of resistance for the Black mother On becoming transliterate: An interview with Diana West, BA, IBCLC

In your clinic THINK ABOUT How does your clinic provide breastfeeding support that is culturally responsive to the different populations of parents you support? Do you have suggestions for improvement to share with your breastfeeding coordinator and local agency staff?

Can we prevent problems?

How does your clinic prepare pregnant parents to breastfeed successfully? THINK ABOUT How does your clinic provide pregnant parents information about breastfeeding? What is your role?

Some information is especially helpful for new parents

Talk about breastfeeding the baby early and often in the first few weeks. Hold baby skin to skin in the hospital and continue at home Breastfeed 8 -12 times (or more) every 24 hours Look for baby’s signs of hunger Watch the baby not the clock Let baby finish the feed Avoid formula, bottles and pacifiers It’s normal to feed several times during the night

Encourage parents to hold the magical hour Hold the baby on mother’s chest skin to skin for first hour after birth.
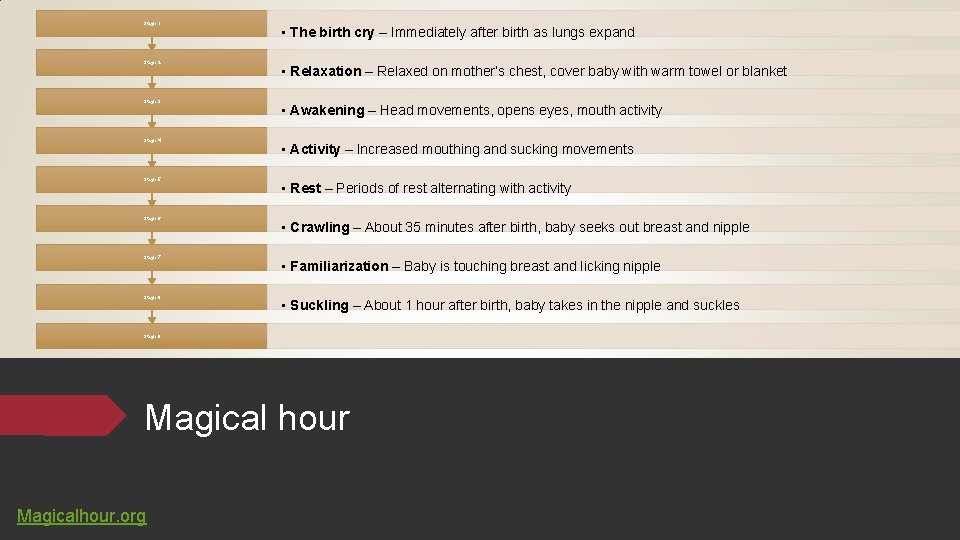

Stage 1 Stage 2 Stage 3 Stage 4 Stage 5 Stage 6 Stage 7 Stage 8 • The birth cry – Immediately after birth as lungs expand • Relaxation – Relaxed on mother’s chest, cover baby with warm towel or blanket • Awakening – Head movements, opens eyes, mouth activity • Activity – Increased mouthing and sucking movements • Rest – Periods of rest alternating with activity • Crawling – About 35 minutes after birth, baby seeks out breast and nipple • Familiarization – Baby is touching breast and licking nipple • Suckling – About 1 hour after birth, baby takes in the nipple and suckles Stage 9 Magical hour Magicalhour. org

Watch for early infant feeding cues Early feeding cues Smacking or licking lips Opening and closing mouth Waking up Turning toward the breast Hand to mouth Making soft sounds Late feeding cues Crying Moving head frantically from side to side Exhaustion Falling asleep

Be honest about what breastfeeding is really like “Breastfeeding might be natural and normal and all those words, but that doesn’t make it easy. Just as it often takes time to develop any other physical skill (such as crawling or walking), it can take time to get the hang of breastfeeding. It might look as straightforward as just latching that baby on the breast, but a whole load of factors are often against us, from a stressful birth to being in an uncomfortable position through to barely having seen anyone else breastfeed so we are less instinctively aware of how to hold and position our baby. …Be more honest about the realities of breastfeeding. For most women it is not immediately straightforward and this coming as a shock makes it harder to deal with and I believe leads more women to stop as they do not expect problems or know where to turn and can feel very alone. ” Dr. Amy Brown. Why breastfeeding grief and trauma matter, p 148 (2019). Photo: National Health Service Foundation Trust

Parents who have concerns about their baby’s growth may question whether or not they should continue breastfeeding.
Some influences their feeding decision self-image prior lived experiences health care provider friends other parent WIC staff grandparents hospital nurses advertisements work and school accommodations social media

How do you balance promoting human milk as the infant feeding norm and also support parents who cannot breastfeed or decide formula is their best option? Participant Centered Services This Photo by Unknown Author is licensed under CC BY-SA-NC

Use PCE skills to ask questions Use: Open-ended questions Don’t use: Closed questions or ones that could suggest problems What have you heard about breastfeeding? Are you going to breastfeed or use formula? How is feeding going? Are you formula or breast feeding? Tell me more about how things are going Are you having problems with breastfeeding? What concerns do you have about starting work next week? Do you have a plan to use formula or pump when you go back to work? How are you feeling? Are you tired? Are your nipples sore? How’s your baby doing? Is he fussy a lot?

Listen and guide to help parents reach their breastfeeding goal Listen Summarize Educate Help • Ask open-ended questions. • “If you had all the support you needed, how do you imagine breastfeeding going for you? ” • Clarify what they want help with. • “You’d like help figuring out how to continue breastfeeding when you return to work? ” • Ask if you can offer help or information. • “I’d like to offer some tips I’ve heard work well for other parents, can I share those with you? ”

There are two types of breastfeeding messages General public health messages Specific for individual families Message: As part of working in public health, we are asked to promote healthy behaviors for all of our families, including promoting human milk as healthy for babies and mothers. As WIC certifiers, we are asked to help individuals meet their healthy behavior goals, including their own goals about feeding their baby We give individualized information so parents can make an informed decision Measure of success: Percent initiating breastfeeding We give anticipatory guidance to help ensure success Exclusive breastfeeding at 6 months Babies breastfeeding to 1 year Measure of success: How will the parents measure success? Did the parents meet their goal? How are the parents feeling?

Compassion We recognize that each family is unique. We help families identify why breastfeeding is important to them and explore solutions when they are faced with challenges. We acknowledge their strengths and applaud their efforts. We allow for any feeding decision to be the right decision for the family. We trust families to make decisions that are best for themselves and their families.

Give support without judgment “For each family, there is a need to balance personal, social, family, and financial factors into all parenting and feeding decisions. ” Joseph Lane Wilson, MD; Bridgid Hast Wilson, MD, Ph. D Department of Family Medicine, East Carolina University Brody School of Medicine, Greenville, NC. Is the "breast is best" mantra an oversimplification? Journal of Family Practice June 2018 vol 67 no 6. “Women need support, not just to breastfeed but to have real answers and to be able to talk through their experiences when it doesn’t work out. ” Dr. Amy Brown (https: //ihv. org. uk/news-and-views/voices/supporting-those-whohavent-been-able-to-breastfeed/)

Supportive family, friends, health care providers and community are the key to helping parents if they face breastfeeding challenges. Vanessa Simmons, CLEC

Listening THINK ABOUT Reflect on why listening skills are important when working with breastfeeding parents. What might you learn by listening?

Case study #1 You are working with a new mom who is breastfeeding, and she tells you that her family wants her to ask WIC formula because a chubby baby is a healthy baby. For your own use, list 3 open-ended questions you might ask her.

Case study #1 – Answer You are working with a new mom who is breastfeeding, and she tells you that her family wants her to ask WIC formula because a chubby baby is a healthy baby. For your own use, list 3 open-ended questions you might ask her. How do you feel about how your baby is growing? How is your baby doing? Tell me more about your plans for feeding your baby? What are your breastfeeding goals? Who gives you support for breastfeeding? How would you like your family to support you? How do you feel about using formula?

Case study #2 A 2 week old infant is in with his breastfeeding mom and hasn’t regained his birthweight. What questions could you ask the mom? What are your next steps?

Case study #2 - Answer A 2 week old infant is in with his breastfeeding mom and hasn’t regained his birthweight. Tell me more about how things are going with breastfeeding? How is the baby doing? What questions could you ask the mom? How are you feeling? What help have you had for breastfeeding? What are your next steps? Assess the number of feedings plus wet and dirty diapers. Assess for additional red flags and refer mom and baby to your Designated Breastfeeding Expert and RDN/WIC Nutritionist

Thank you for completing the Breastfeeding and Growth In-service. You are an important link to helping parents who are concerned about their baby’s growth.

Questions? Reach out to your agency’s breastfeeding coordinator if you have questions or ideas. You can also email the state breastfeeding coordinators at Oregon. WIC. Breastfeeding@dhsoha. state. or. us
- Slides: 53