Breast history and examination Soma Farag Breast conditions

Breast history and examination Soma Farag

Breast conditions you need to know about • Breast carcinoma • Benign cystic change/fibroadenosis • Benign ductal disease (duct ectasia and papilloma) • Fibroadenoma • Breast cysts • Mastitis

Breast carcinoma • Usually older women • Risk factors: positive family hx, OCP, HRT, previous cancers (ovarian, endometrial, bowel cancer), increased exposure to oestrogen • Presentation of lump: • Rough consistency • Poorly defined edges • Can be fixed to skin/underlying muscle • Associated symptoms: Nipple discharge Pain Nipple inversion Skin changes (dimpling, peau d’orange/puckering, eczema like changes – Pagets disease of the breast) • May have lymphadenopathy/other systemic symptoms • •

Benign cystic changes/fibroadenosis • 35 – 50 years old • Single or multiple lumps commonly in upper quadrant • Cyclical changes (in size and tenderness) • Lumpy, cobblestone texture • Smooth, well defined borders • Not fixed to skin/muscle

Fibroadenoma • Patient < 40 years • usually subject to same cyclical changes as other glandular breast tissue • Highly mobile lump • Lump not tethered to surrounding breast tissue • Well defined borders – but lobulated and lumpy on palpation
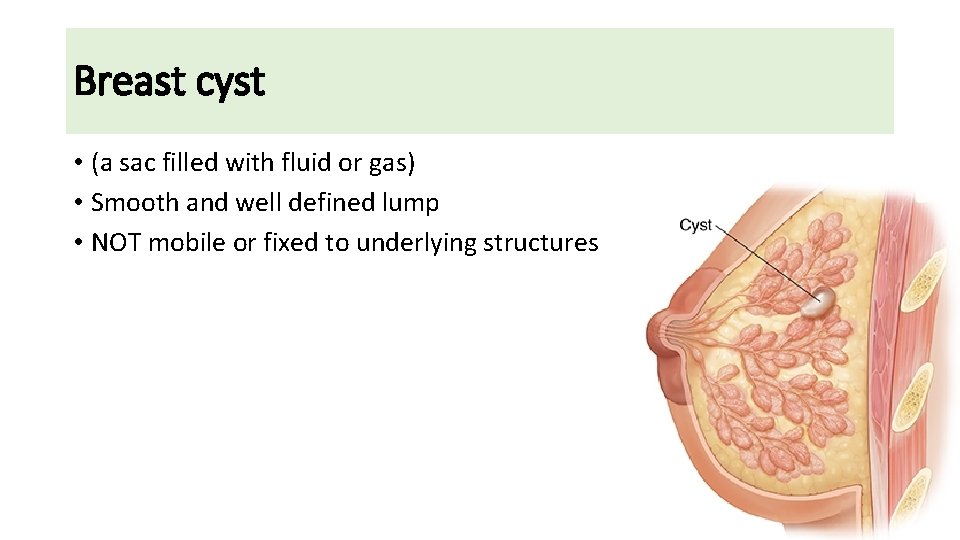
Breast cyst • (a sac filled with fluid or gas) • Smooth and well defined lump • NOT mobile or fixed to underlying structures

Duct ectasia • Middle aged women • Inflammatory condition with no relationship malignancy • Mammary ducts dilate and fill with stagnant green brown cheesy secretion • Fluid may discharge from nipple and irritate the surrounding areolar skin • Common in SMOKERS Intraductal Papilloma: benign tumour within the duct in women nearing menopause. Green/Blood stained discharge

Mastitis/abscess Mastitis/ • Associated with breast feeding • Infection of breast tissue (most commonly S. aureus): transferred from nasopharynx of infant during lactation/cracked nipple • Non lactational mastitis also exists and heavily associated with smoking • Associated symptoms: pain, nipple discharge (yellow/green), skin changes (redness), swelling, warm, itching, fever. • Characteristics of lump: lump can be present and palpable especially if abscess is subsequently formed

How to take a breast history (4 minutes) “Good morning my name is Soma, I am a fourth year medical student. I’ve been asked by your doctor to have a chat with you about what’s brought you in today, would that be okay? Can I confirm your name and DOB?

Structure • • • Presenting complaint – characterise the lump Summarise (optional) ICE Associated symptoms Risk factor questions Past medical/surgical history Drug history Family history Social history

Characterise the lump • What: Describe the lump to me • Shape, describe the consistency • Have you noticed it move? • Where is it and have you noticed it elsewhere? • When did you first notice it (duration)? • How has it changed? Bigger? Any points in the month/your menstrual cycle you notice it is worse? • Has this/similar breast problems happened before? • Pain?

I “Do you have any thoughts what your lump could be due to? ” C “Is there anything in particular you’re worried about regarding your health? ” E “Before I move on any further, is there anything specific you were hoping to get out of today’s appointment, which I can pass onto your doctor”

Associated symptoms “Now I am just going to ask you some quick yes/no questions to find out more about what’s going on…” • Nipple discharge colour, smell, amount, consistency • Pain • Have you noticed any skin changes? Redness? (erythema) • Itching • Fever • Lethargy • Appetite loss • Weight loss • Night Sweats • Backpain • Difficulty breathing

Asking about risk factors More oestro gen More cancer • Bleeding: early menarche (<13 Y), late menopause (>55 Y) • Oestrogen: OCP, HRT • Other disease: previous cancer: endometrial/ovarian • Breast feeding: = protective • Young ‘un: age they had first child (>35 Y increases risk)/Nuliparity) • Sister: family hx – first degree relative with BC increases risk 2 -3 x • Others: • Radiation • Lifestyle: obesity, alcohol, smoking

Past medical/surgical history Breast, endometrial, bowel cancer If you have not already covered in the risk factors section Drug history • What medication are you on? • We have already covered oral contraceptive pill and hormone replacement therapy in the risk factor section • Allergies

Family history • Breast, endometrial, bowel cancer • If you haven’t already covered it in the risk factors section

Social history • Smoking (have you ever smoked in the past, pack years) • Alcohol • Recreational drugs • Work? • Who is at home with you?

Breast examination (5 -6 minutes) • “Given what you have just told me, I am going to check your breasts. This will involve me having a look and feeling for any abnormalities in your breasts, such as the lump you have mentioned. Would that be okay? • For this, you will need to be undressed from the waist upwards, including your undergarments. The examiner here will act as a chaperone, would you like anyone else here with you? • I’ll just draw the curtain here for you to get undressed, there is a robe there to cover yourself with. Do you have any questions for me? • Call me when you are ready. ” Wash hands Introduce Position - sitting up Exposure Reposition – lying at 45 o Chaperone and Consent

Inspection • Ask about tenderness/discharge • End of the bed: • Cachexia • Arm swelling • Jaundice • Breathlessness • General wellbeing Wash hands Introduce Position - sitting up Exposure Reposition – lying at 45 o Chaperone and Consent
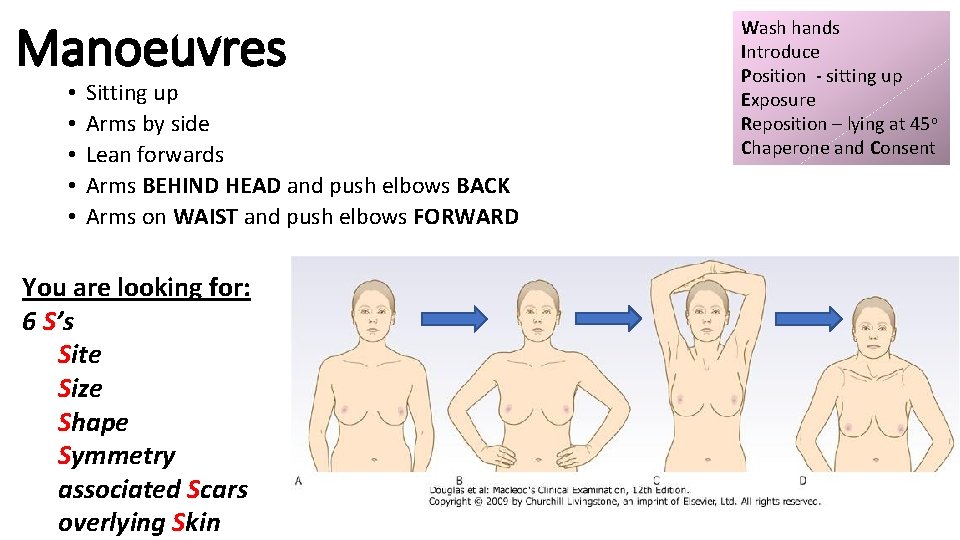
Manoeuvres • • • Sitting up Arms by side Lean forwards Arms BEHIND HEAD and push elbows BACK Arms on WAIST and push elbows FORWARD You are looking for: 6 S’s Site Size Shape Symmetry associated Scars overlying Skin Wash hands Introduce Position - sitting up Exposure Reposition – lying at 45 o Chaperone and Consent

Skin changes to look for: • Tethering; due to infiltration of ligaments of Astley-Cooper • Peau d’orange; micro-oedema • Lymphoedema; may indicate lymphatic infiltration by carcinoma or previous surgery with LN removal • Erythema • Nipple inversion • Puckering • Dimpling

Palpation • Position bed at 45 o and ask the patient to lie down with the ipsilateral hand, to the side being examined, behind head • Start with the NORMAL breast first • Cover the other breast • Palpate with flat fingers (index, middle and ring) to gently press the tissue against the chest well • Cover all 4 quadrants, axillary tail, areola and nipple • Thank patient and repeat on the other breast • If you feel a lump - don’t stop, continue palpating, then come back to it and feel it again for: shape, size, boarder, mobility, fixation • IF the patient has experienced discharge, ask them to press on the nipple to express discharge. Wash hands Introduce Position - sitting up Exposure Reposition – lying at 45 o Chaperone and Consent

Palpation • Palpate with flat fingers (index, middle and ring) to gently press the tissue against the chest well • Cover all 4 quadrants, axillary tail, areola and nipple • Thank patient and repeat on the other breast • If you feel a lump - don’t stop, continue palpating, then come back to it and feel it again for: shape, size, boarder, mobility, fixation • IF the patient has experienced discharge, ask them to press on the nipple to express discharge. Wash hands Introduce Position - sitting up Exposure Reposition – lying at 45 o Chaperone and Consent
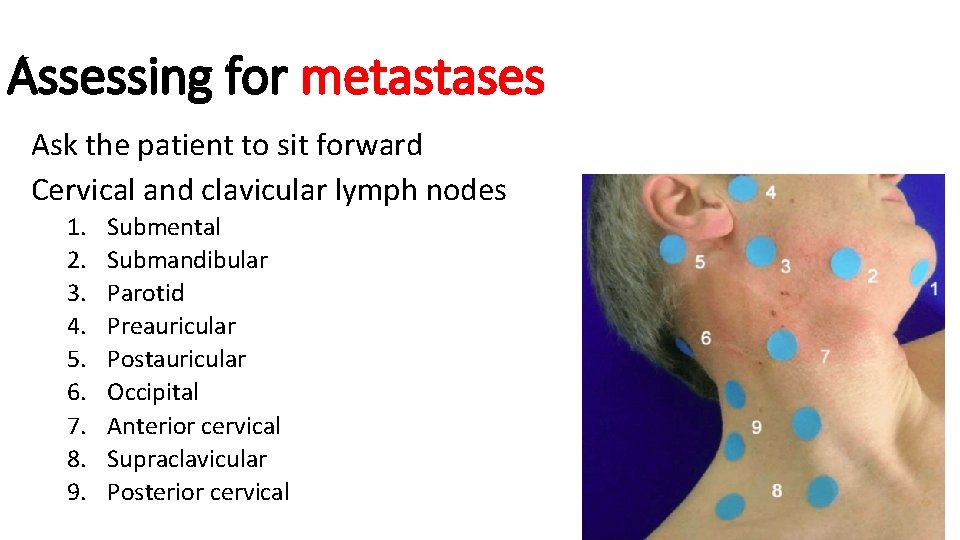
Assessing for metastases Ask the patient to sit forward Cervical and clavicular lymph nodes 1. 2. 3. 4. 5. 6. 7. 8. 9. Submental Submandibular Parotid Preauricular Postauricular Occipital Anterior cervical Supraclavicular Posterior cervical

Assessing for metastases • Spinal palpation • Auscultate lung bases Flatten the bed and ask the patient to lie down again. Offer to palpate for the liver

Assessing for metastases Flatten the bed and ask the patient to lie down again. Offer to palpate liver Ask patient to sit on edge of the bed • Palpate axillary lymph nodes • Support their arm with your corresponding arm e. g. Patients right arm with you right arm and palpate with your left hand 1. Apical 2. Lateral 3. Medial 4. Anterior 5. Posterior Thank patient and draw the curtains so they can get dressed

Presentation • Location: • Which breast • Quadrant • Appearance • Size (estimate diameter/ x by x cm) • Shape • Edges: • Rough or Smooth • Boarder • Well or ill defined • Tenderness • Mobility • Tethered to underlying structure? • (Temperature)

“I felt a round 2 cm lump in the lower inner quadrant of the right breast. It felt rough with poorly defined boarders. It was not mobile and attached to the underlying muscle” • Differentials • They could ask you to draw diagram: • Demonstrate this Triple assessment: Breast history/examination Imaging USS (<35 years) Mammogram (35 years) Histology (FNA/ core biopsy) Core biopsy: used when lesion is large, non palpable FNA: palpable lump, cytology

Demonstration
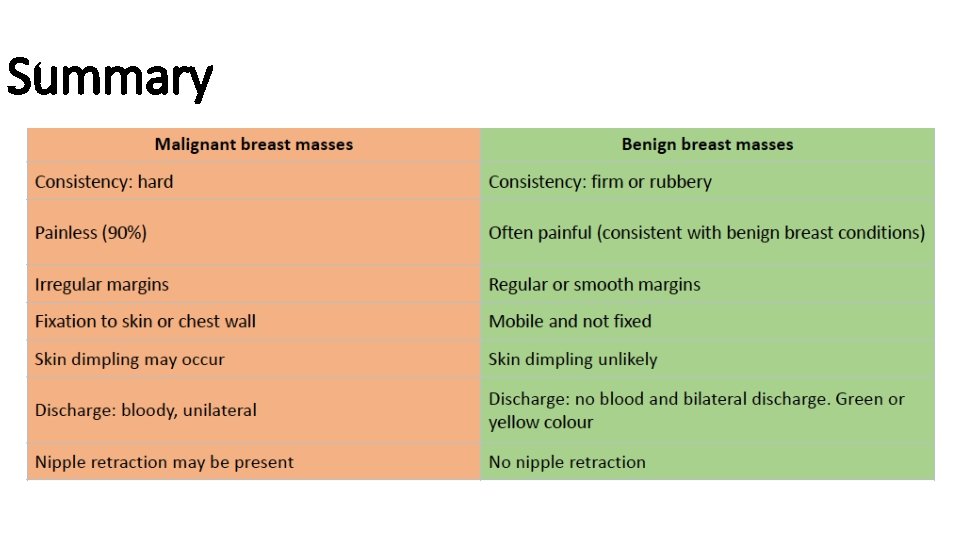
Summary
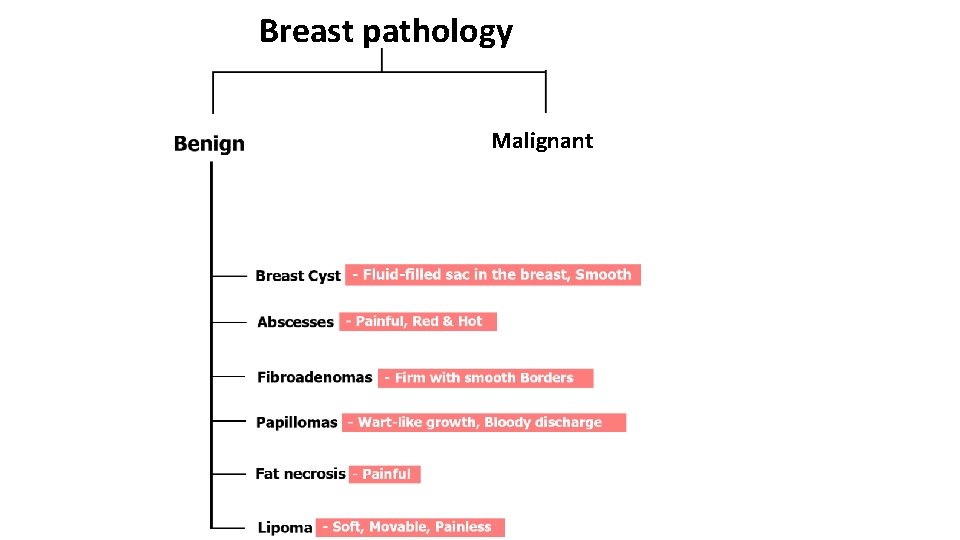
Breast pathology Malignant
- Slides: 32