Breast Examination Robert Collins GPVTS 1 Topics Breast

Breast Examination Robert Collins GPVTS 1

Topics • • Breast history Examination Investigations Breast conditions – Benign / Malignant • Treatment

History • Presenting complaint is v important • Lump; – always ask how long been present – Relation to menstrual cycle – Does its size vary? Is it getting larger? • Pain; – Is it cyclical? Is the lump painful?

• Nipple discharge; ascertain – Colour, Quantity, pattern, frequency • Age of patient; cancers are uncommon <30 yrs, but fibroadenomas are • Ask if noticed any; – Nipple retraction – Breast distortion – Metastatic related symptoms • Previous breast disease – Was it investigated / treated

• Family history – Genetics; 5 -10% are inherited dominantly • They have early onset & associated with other tumours e. g. Bowel, ovarian. • BRCA 1 (chromosome 17 q 21) • BRCA 2 (chromosome 13 q 24) • P 53 gene chromosome 17 • Medications; HRT, pill • Gynae / Obstetric Hx; – Menarche, menses – Parity? When? After 30 increases risk – Breast fed?

Examination • • Introduce yourself to patient Undress to waist, sit on couch at 45 degrees Maintain patient dignity e. g. Bed sheet Assess in following positions – Patient’s hands behind their head (accentuate lumps, asymmetry, tethering) – Pushing against their hips (accentuate lumps attached to pectoralis muscle) – Patient leaning over side of bed (accentuate abnormalities in large breasts) • Exam good breast first, then the ‘diseased’ breast

• Inspection – 6 S’s • • • Site Size Shape Symmetry overlying Skin associated Scars • Fungation; comment on presence of fungating carcinoma (check inframammory fold) • Asymmetry; carcinoma may be present in higher breast • Tethering; due to infiltration of ligaments of Astley. Cooper • Peau d’orange; micro-oedema • Lymphoedema; may indicate lymphatic infiltration by carcinoma or previous surgery with LN removal • Erythema
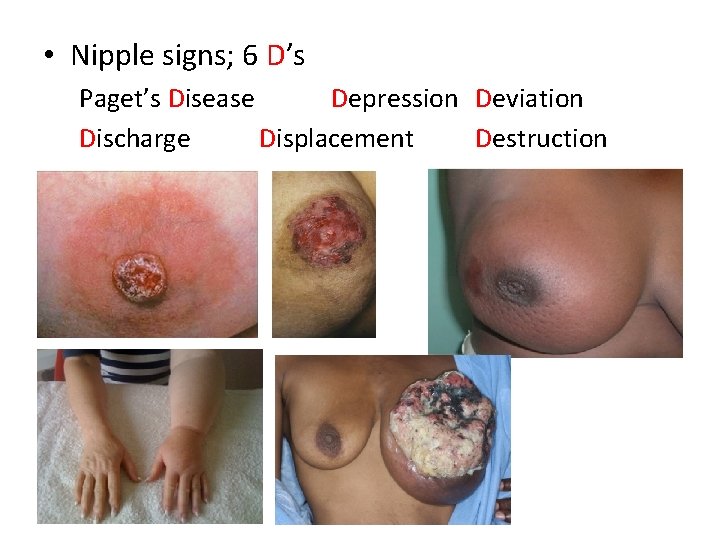
• Nipple signs; 6 D’s Paget’s Disease Depression Deviation Discharge Displacement Destruction

• Palpation – Ask about pain and if patient has a lump. – Examine good breast first then diseased breast – Patient puts hand behind head on exam side – Check for temperature change – Use following with lumps; • • Surface Edge Consistency (hard, firm, soft) Fixity to skin and underlying structures Fluctuance Pulsatility and expansility Transilluminability Reducibility
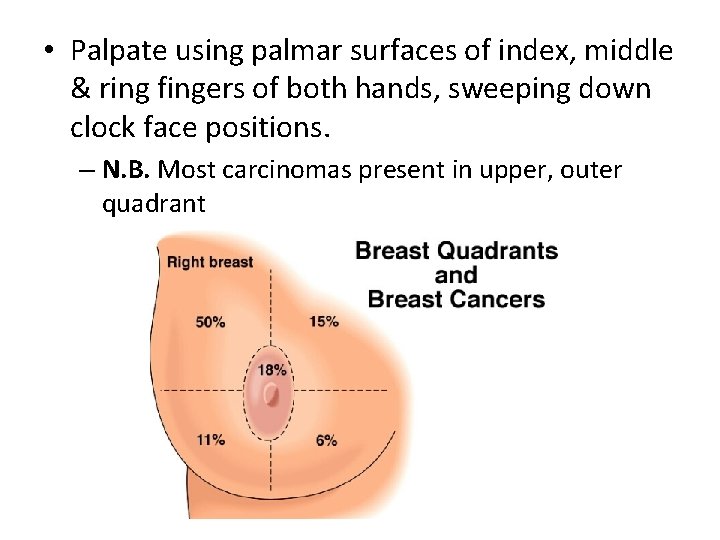
• Palpate using palmar surfaces of index, middle & ring fingers of both hands, sweeping down clock face positions. – N. B. Most carcinomas present in upper, outer quadrant
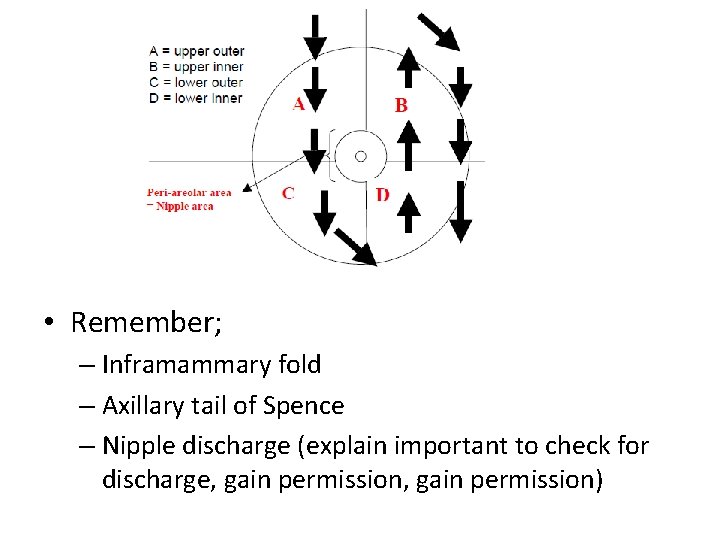
• Remember; – Inframammary fold – Axillary tail of Spence – Nipple discharge (explain important to check for discharge, gain permission)

• Axillary lymphadenopathy – Support their arm with your corresponding arm e. g. Patients right arm with you right arm and palpate with your left hand – Examine anterior, posterior, medial and lateral walls in addition to the apex • • • Medial wall (seratus anterior) Lateral wall (body of humerus) Anterior wall (pectoralis major) Posterior wall (latisimus dorsi) Apices (arch of armpit – high in the head of the humerus)

• Cervical and supraclavicular lymphadenopathy • Always cover the patient when examination complete and thank the patient. • For completion; • Respiratory exam; ? mets • Abdomen exam; palpate liver (if hepatomegaly think mets) • Spinal exam; tenderness ? Mets • Encourage self exam; encourage patient to regularly monitor their breasts using simple examination infront of a mirror • Triple Assessment; If lump detected continue to this
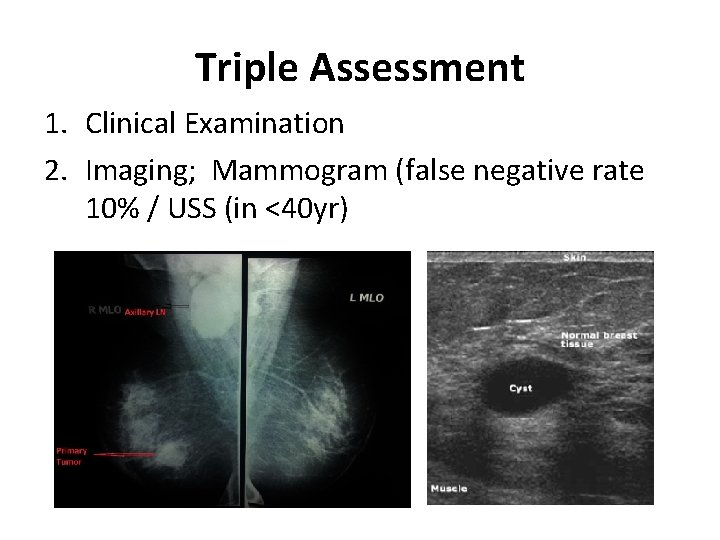
Triple Assessment 1. Clinical Examination 2. Imaging; Mammogram (false negative rate 10% / USS (in <40 yr)
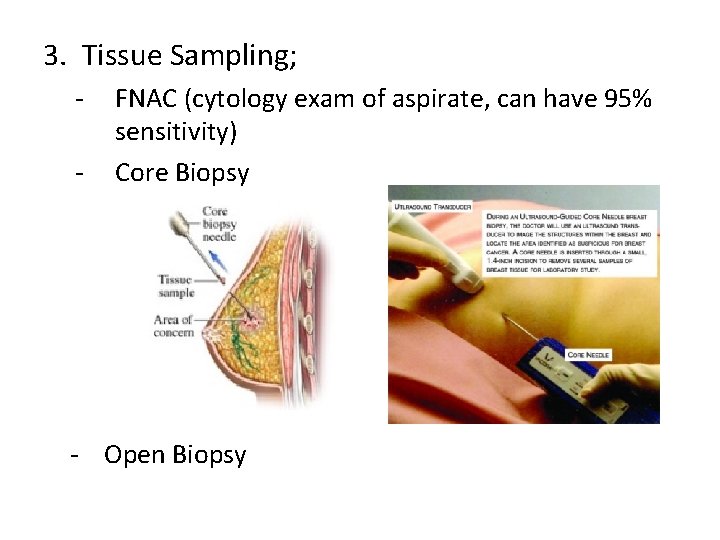
3. Tissue Sampling; - FNAC (cytology exam of aspirate, can have 95% sensitivity) Core Biopsy - Open Biopsy

Breast Disease • Classify as benign or malignant – Benign aetiology classified as Aberrations of normal development and involution (ANDI) Peak Age (years) 15 -25 Development Fibroadenoma & excessive Breast development 25 -40 Cyclical Hormonal Cyclical nodularity & mastalgia 35 -55 Involution Lobular: Ductal: Epithelial: Cyst Duct ectasia & periductal mastitis Hyperplasia & fibrosis

• What is a fibroadenoma? – Most common benign neoplasm. Fibroepithelial tumour, composed of glandular tissue & stroma. – Peak onset 15 -25 yrs. – Painless, smooth, firm, rubbery lump, highly mobile. – Approx 10% resolve spontaneously within 1 yr • What are breast cysts? – Fluid-filled, distended & involuted lobules. – Present as smooth lumps. Maybe painful – Peak age onset 35 -55 yr. – FNA may relieve symptoms and can be analysed

• What are cyclical nodularity & mastalgia? – Affect pre-menopausal females & are hormonal dependent. – Cyclical breast changes occur, result lumps (nodularity) & pain (mastalgia) related to menstrual cycle. – Treatment options classified as; Conservative Medical Surgical Reassurance Evening primrose oil Firm supporting bra Analgesia Evening primrose oil OCP Mastectomy (for treatment resistant severe mastalgia) Danazol Bromocriptin Tamoxifen

• What is duct ectasia? – Involution & dilatation of subareolar ducts – Clinical features; nipple inversion, nipple discharge (may be cheese / blood stained), subareolar mass, mastalgia. • What is periductal mastitis? – Inflammation, often due to infection of subareolar ducts. – May present like duct ectasia – Pus discharge from nipple & mastalgia

• What is epithelial hyperplasia? – Increase no. of epithelial lining cells of the terminal lobular unit. – Atypical dyplasia increased risk of progression to carcinoma. • What is fat necrosis? – Often after trauma to fatty breast tisssue e. g. Surgery / breastfeeding. – Inflammation, fibrosis & calcification may occur – Can be similar to carcinoma – Most cases resolve spontaneouly
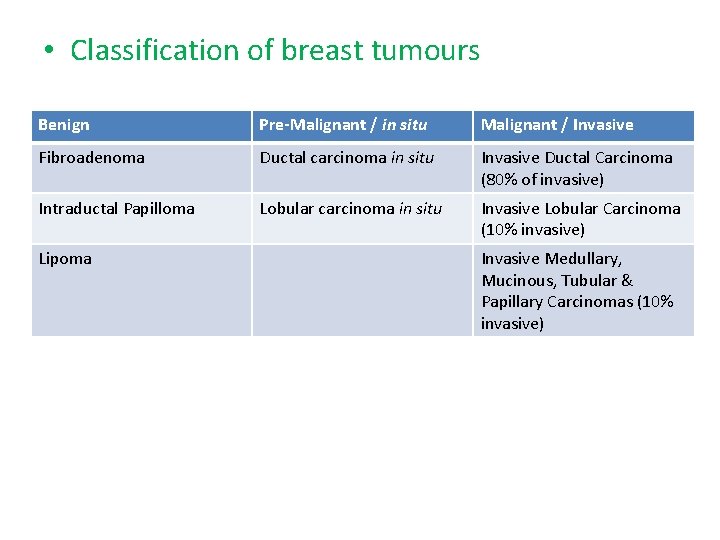

• Classification of breast tumours Benign Pre-Malignant / in situ Malignant / Invasive Fibroadenoma Ductal carcinoma in situ Invasive Ductal Carcinoma (80% of invasive) Intraductal Papilloma Lobular carcinoma in situ Invasive Lobular Carcinoma (10% invasive) Lipoma Invasive Medullary, Mucinous, Tubular & Papillary Carcinomas (10% invasive)

Breast Cancer • Incidence 1: 11 • Age; rare <30 yr • Risk factors; – – – – Early menarche, late menopause 1 st child >30 yr FHx in 1 st degree relative Hx of breast feeding Prev breat ca Radiation exposure Exogenous hormones High intake of saturated fats, alcohol

• Staging of cancer – Bloods; FBC, LFTs, U&Es, ALP, Ca 2+, ESR – CXR – 2 nd line investigation; Liver USS, bone scan, CT-scan, axillary node staging – Clinical staging – TMN • • • Tis (no tumour palpable) CIS / Paget’s T 1 < 2 cm. No skin fixation T 2 2 -5 cm. Skin distortion T 3 5 -10 cm. Ulceration + pectoral fixation T 4 >10 cm. Chest wall extension, skin involved. • • N 0 No nodes N 1 Ipsilateral mobile nodes N 2 Ipsilateral fixed nodes N 3 Internal mammary nodes • M 0 no mets • M 1 Mets in liver, lung, bone

Treatment • Surgical; – WLE plus DXT (need 1 cm excision margin) – Mastectomy – Axillary sampling (removal of lower axillary nodes) – Axillary clearance (removal of contents below the level of the axillary vein) • Level 1 = below pec minor • Level 2 = behind pec minor • Level 3 = above pec minor (full clearance) – SLNB

• Systemic treatment – Can be adjuvant or neo-adjuvant 1. Radiotherapy - Breast and chest wall Axilla Palliation (e. g. For bony tenderness) 2. Chemotherapy - Recurrent disease <70 yr with > 1 +ive axillary node Very large tumours

• 3. Endocrine therapy and Tamoxifen – Tamoxifen in ER + ive females – Up to 15% of ER –ive females also respond – Beneficial in pre- and postmenopausal women, not effective in ER –ive premenopausals – Increased risk of endometrial carcinoma – Aromatase enzyme inhibitor = Anastrazole (Arimidex) • For post-menopausal women ER +ive
- Slides: 26