Breast Disease Common Problems Jennifer Griffin MD MPH

Breast Disease: Common Problems Jennifer Griffin, MD, MPH Associate Professor Residency Program Director Department of Obstetrics and Gynecology

Why do women seek care for breast problems? • Rarely they have symptoms that are too bothersome and want treatment. • Frequently they are concerned they have a sign/symptom of breast cancer.

Their concern is justified • Breast cancer is diagnosed in 1 in 8 women in the U. S. • Over 200, 000 cases in the U. S annually. • Over half of cases are symptom detected. • Breast cancer is diagnosed in 11% of women presenting with a breast mass, and 4% with any complaint.

Steps of a Breast Evaluation • • • HPI Risk Assessment Physical Exam Imaging Diagnostic Steps Follow up plan

HPI • • Complaint Associated Symptoms Timing Duration

Risk Assessment • AGE – 1 in 2000 in 20 s, 1 in 25 in their 70 s • Family History • Reproductive History • Breast History

Risk Assessment • AGE • Family History – Look for pattern suggesting genetic predisposition – Early age of diagnosis – Multiple relatives, same side of family, 1 st, 2 nd, 3 rd degree relatives • Reproductive History • Breast History

Risk Assessment • AGE • Family History • Reproductive History – Menarche age <12, menopause >55 – Age of first birth >30 – Nulliparity – No breastfeeding – Hormone therapy E+P after menopause • Breast History

Risk Assessment • • AGE Family History Reproductive History Breast History – Prior breast biopsies – Proliferative lesions—slight increase risk – ADH, ALH, FEA, LCIS ~20% LR

Physical Exam • • Think about symmetry Visualization Seated / Supine Take adequate time

Imaging • Mammography/Tomosynthesis • Ultrasound • MRI

Mammo/Tomo • • First imaging step in women >=30 Detects differences in density Sensitivity is limited by density Safe in pregnancy, but limited by density
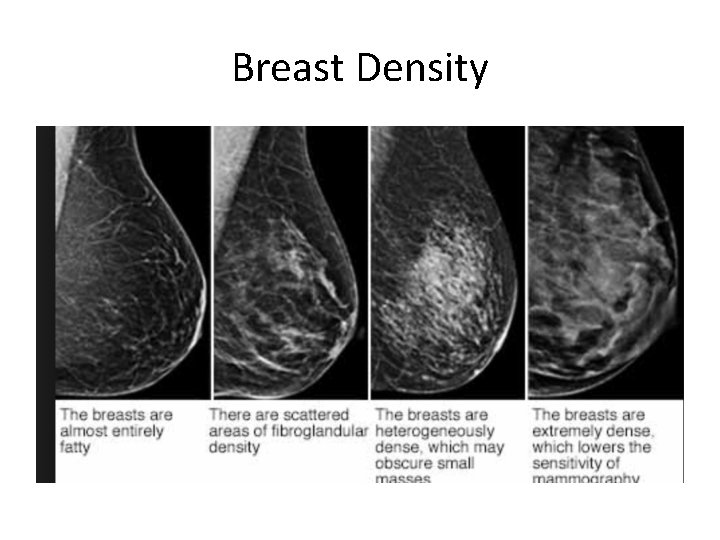
Breast Density

Ultrasound • Initial imaging for women <30. • Adjuvant imaging for women 30+. • Lack of anatomic landmarks limits utility for screening.

MRI • Used to screen high risk women. • Used for cancer treatment planning. • Not helpful in evaluation of breast complaints.

BI-RADS Classification • • 0: Incomplete; needs more imaging 1: Negative 2: Benign findings 3: Probably benign (<2% likelihood) – Repeat imaging in 6 months • 4: Suspicious (3 -94% likelihood) – Consider biopsy • 5: Highly Suspicious (>=95% likelihood) – Biopsy indicated • 6: Biopsy Proven Malignancy

Diagnostic Steps • Core needle biopsy – Preferred in most situations – Correlates with open biopsy ~95% of the time • Excisional biopsy – When core biopsy isn’t feasible – When core biopsy is non diagnostic or requires additional sampling • Fine Needle Aspiration – Cytology specimen – Part of “triple test” – Quick turn around of results.

Breast Mass • Distressing for providers and patients • Systematic approach includes imaging in almost all cases

Workup—Key Elements • Physical Exam – Is there symmetry? – Is this a 3 D mass? • Imaging – When can we trust our radiologists? • Follow up – Have a plan in place

Common Masses • Cysts – Simple, complicated, complex • • Fibrocystic change Fibroadenomas Phylloides tumors Skin problems Fat necrosis Diabetic mastopathy Pseudoangiomatous stromal hyperplasia (PASH) Malignancies
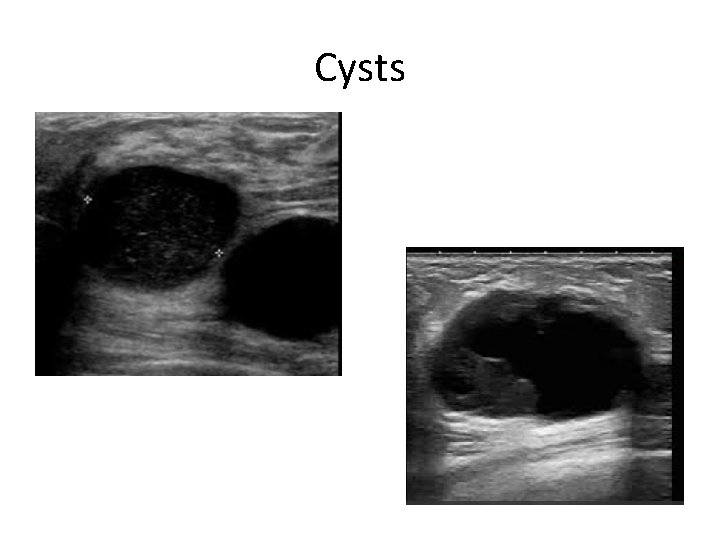
Cysts
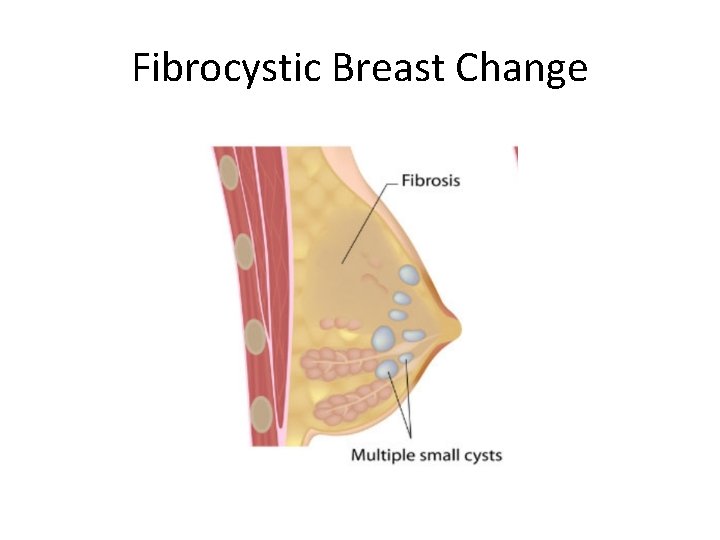
Fibrocystic Breast Change
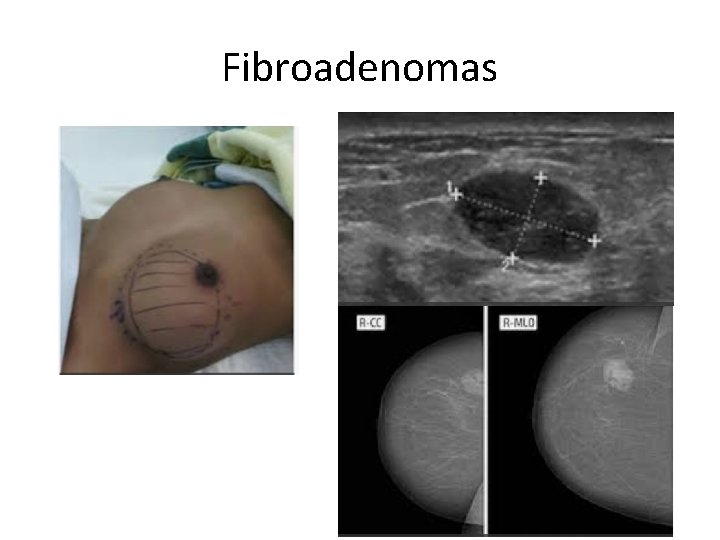
Fibroadenomas
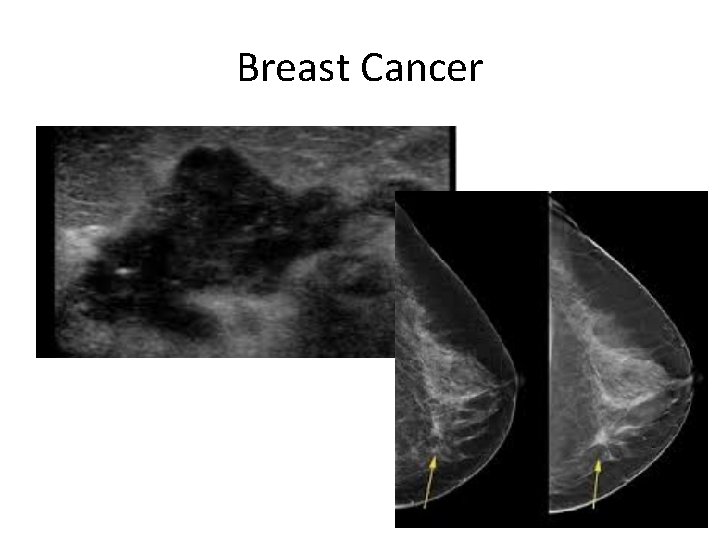
Breast Cancer

Management • Does imaging correlate with exam? • If yes, follow BI-RADS guidelines. • If no, follow up.

Nipple Discharge • Is it a breast or endocrine problem? • Key Questions: – Spontaneous or expressed? – Bilateral or unilateral? – Color? – Multiductal or uniductal?

Galactorrhea • Bilateral, spontaneous, milky • Check prolactin, TSH • Meds: – H 2 receptor antagonists (cimetidine) – Dopamine receptor antagonists (risperidone) – OCPs, SSRIs • Stimulation • If prolactin>40, should have imaging to look for pituitary adenoma

Benign Breast Causes • Multiductal, any color is benign • Inspect nipple for skin change • Duct ectasia – Women 50 -60 s with grey, green sticky discharge – May have nipple inversion • Mammary duct inflammatory sequence • Ecsema

More Concerning Discharge • Serous or bloody, single duct • Requires imaging • Requires biopsy • Majority of cases will be due to benign papillomas. • Can be associated with fibrocystic change or malignancy (DCIS)
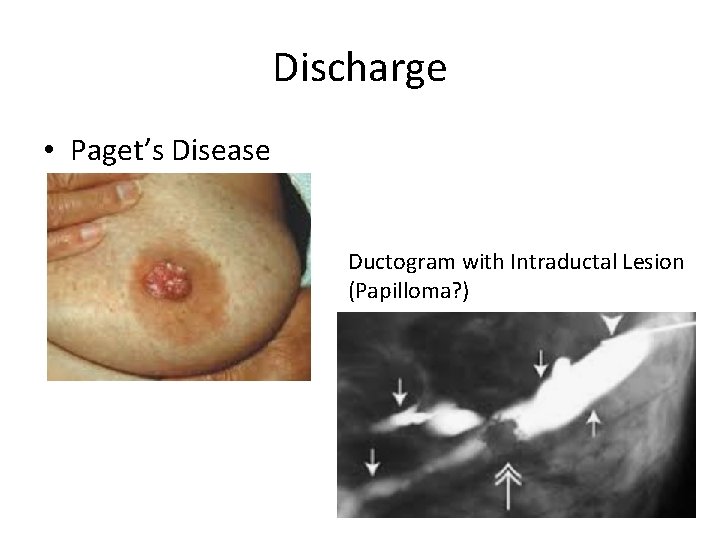
Discharge • Paget’s Disease Ductogram with Intraductal Lesion (Papilloma? )

Inflammation • Lactational mastitis • Non-lactational mastitis • Periductal mastitis/Mammary duct inflammatory sequence • Granulomatous mastitis • Inflammatory cancer

Lactational Mastitis • 1 st Line – Dicloxicillin 500 mg tid x 10 d – Keflex • Think MRSA – Recent hospitalization – Abscess – Start with Bactrim 100 mg bid x 10 d • Drain abscess (aspiration when feasible)
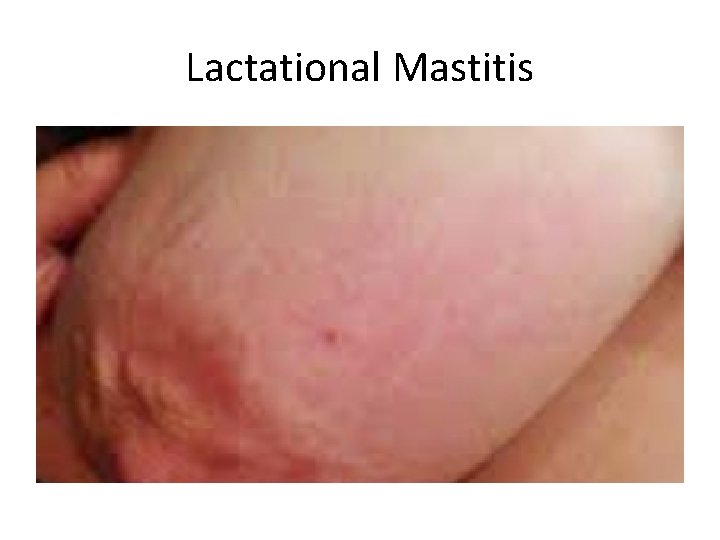
Lactational Mastitis
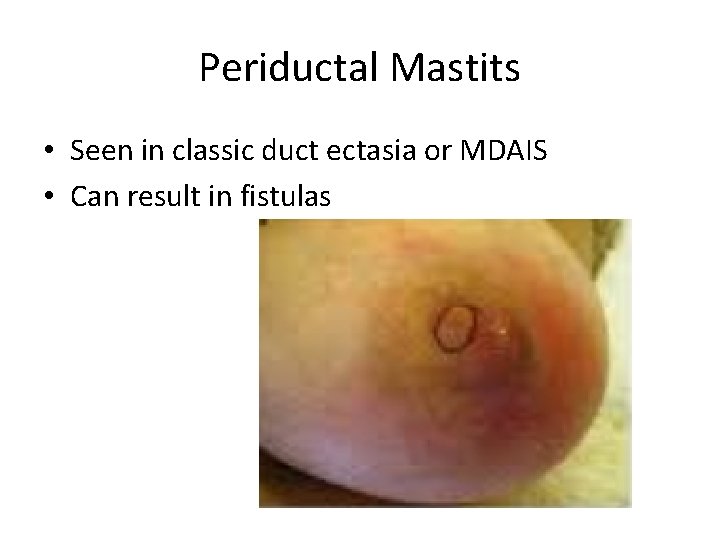
Periductal Mastits • Seen in classic duct ectasia or MDAIS • Can result in fistulas
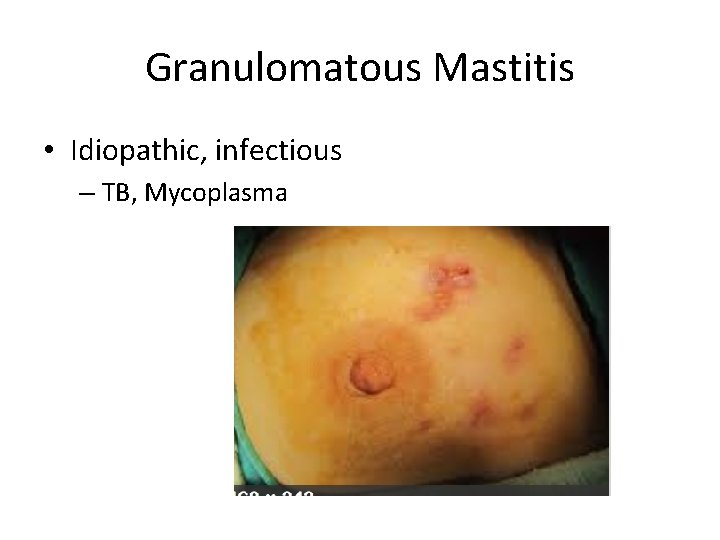
Granulomatous Mastitis • Idiopathic, infectious – TB, Mycoplasma
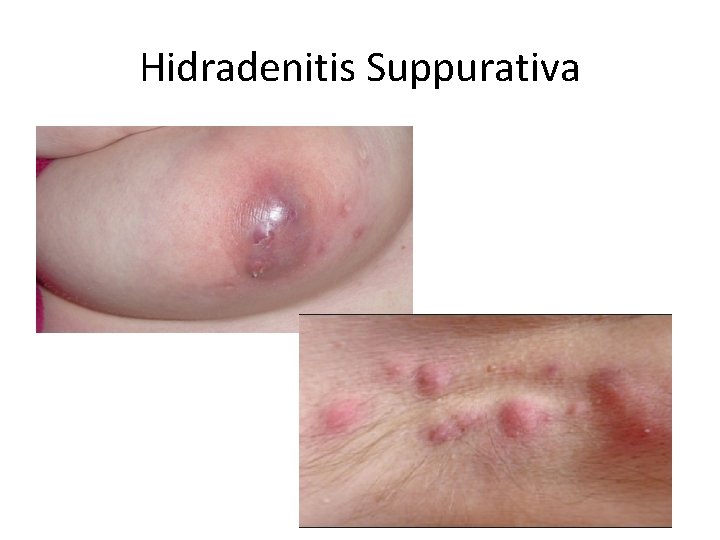
Hidradenitis Suppurativa
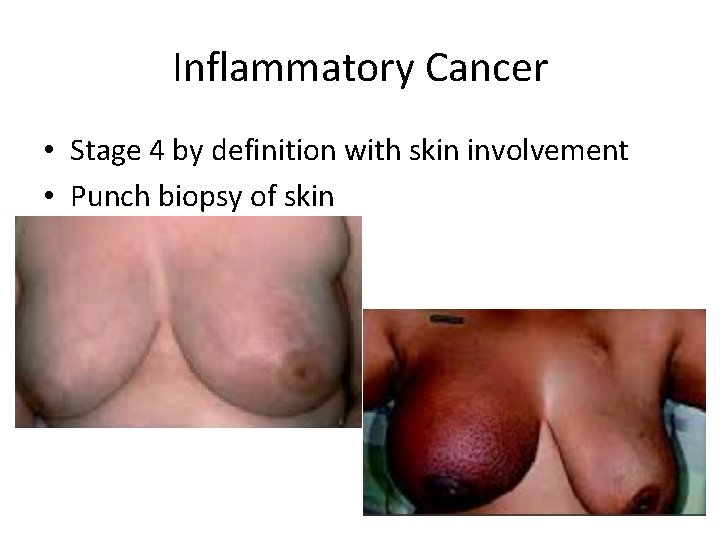
Inflammatory Cancer • Stage 4 by definition with skin involvement • Punch biopsy of skin
- Slides: 37