Brain and brain stem syndromes Neurology course Medical

Brain and brain stem syndromes Neurology course Medical Study in English Split, January 2018. Gordan Džamonja, Md Ph. D 1

• A key issue in the diagnosis of neurological diseases is: Where is the damage? ("Where is the lesion? ") • The presence of certain symptoms and signs in neurological diseases, in most cases, clearly points to the localization of damage within the nervous system 2

• Syndrome (in medicine) is the term for a group of symptoms and/or medical signs that usually appear together • Many syndromes are named following the people who have first described them - the eponymous terminology • Recognizing various neurological syndromes is important for socalled “topical diagnosis” 3

Symptoms/signs in neurology are usually the result of: ü destruction of certain brain structures ü lack of inhibition of lower organizational structures (e. g. , primitive reflexes) ü irritative damage (e. g. , epileptic seizures) 4

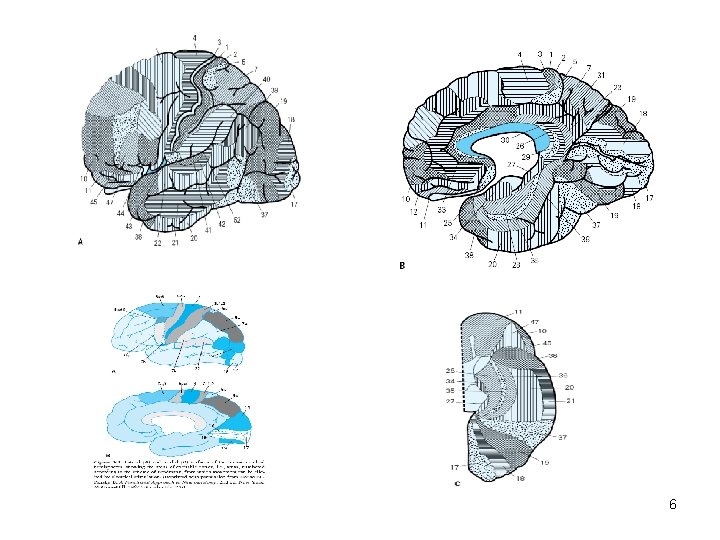
Brain (cerebrum) • • • There is a connection between the histological structure and function of particular regions of the cerebral cortex (Brodmann) The entire cerebral cortex can be divided into: - Primary cortical areas (primary motor, somatosensory, visual, auditory cortex) - Associative areas can be: – Primary (unimodal) – Secondary (multimodal) 5
6

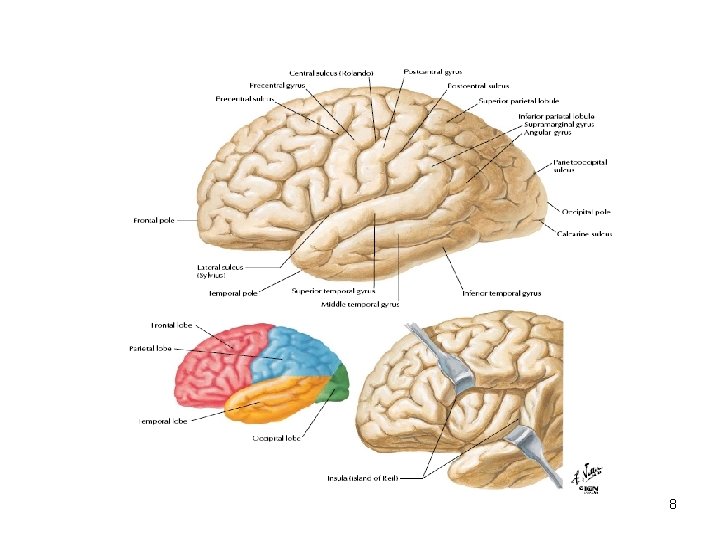
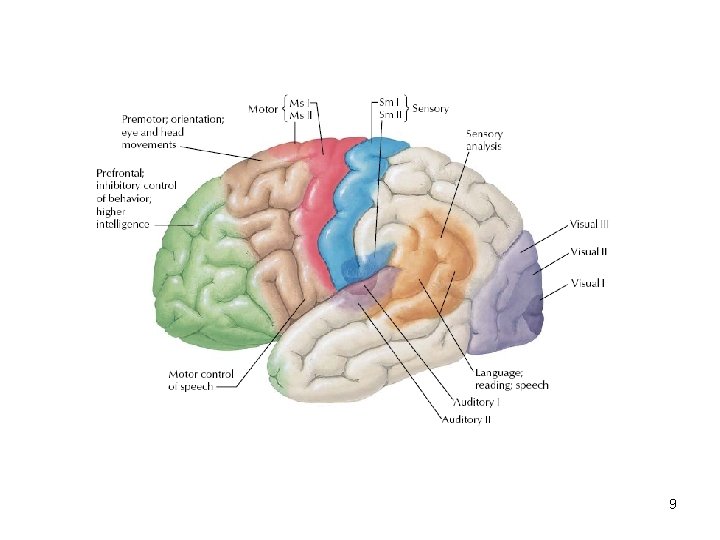
• • Unimodal areas are located around the primary cortical area Multimodal areas are more remote and integrate impulses from several different primary areas • The largest multimodal areas of the cerebrum are: 1) in the anterior parts of the frontal lobe 2) at the border area of parietal, temporal and occipital lobes 7
8
9
10

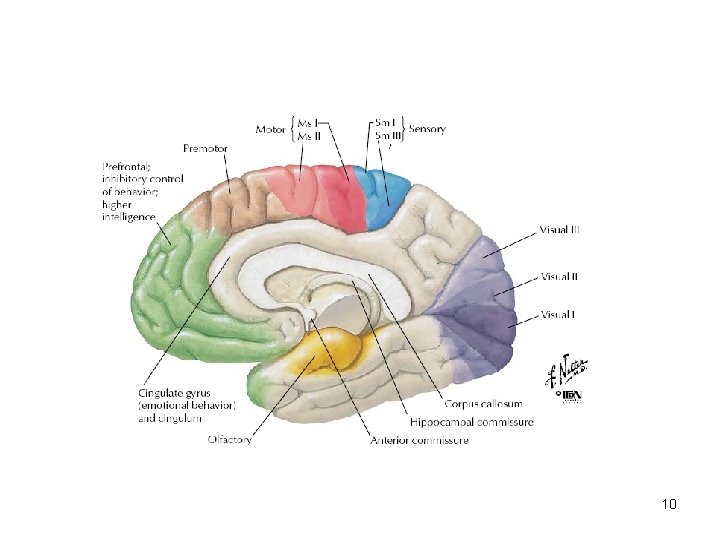
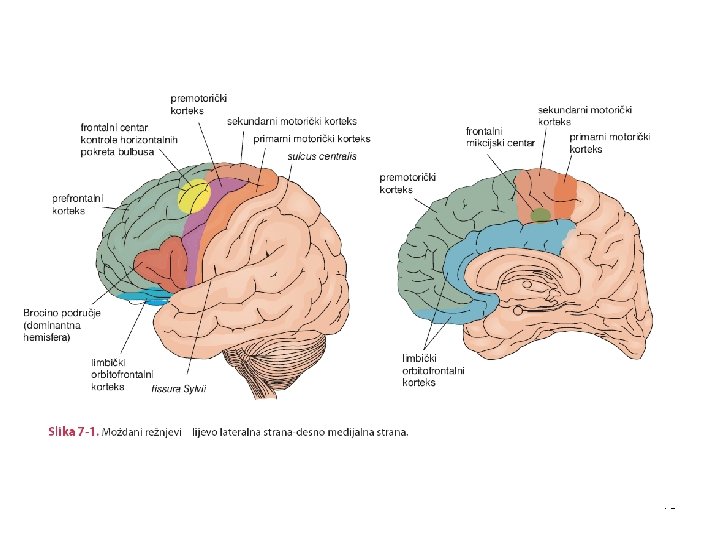
Frontal lobe • Frontal cortex is divided into: 1) Primary motor cortex 2) Supplemental motor area (SMA) 3) Prefrontal region (multimodal associative region) 11

Primary motor cortex • • Its parts are gyrus praecentralis and, from the medial side, lobulus paracentralis Contains pyramidal neurons that allow volitional motor control of the contralateral side of the body They are specifically topographically organized – Penfield’s motor homunculus Lesions can be: – destructive (different paresis: the face, arm, leg) – as well as irritative (Jackson march and epilepsia partialis continua) 12
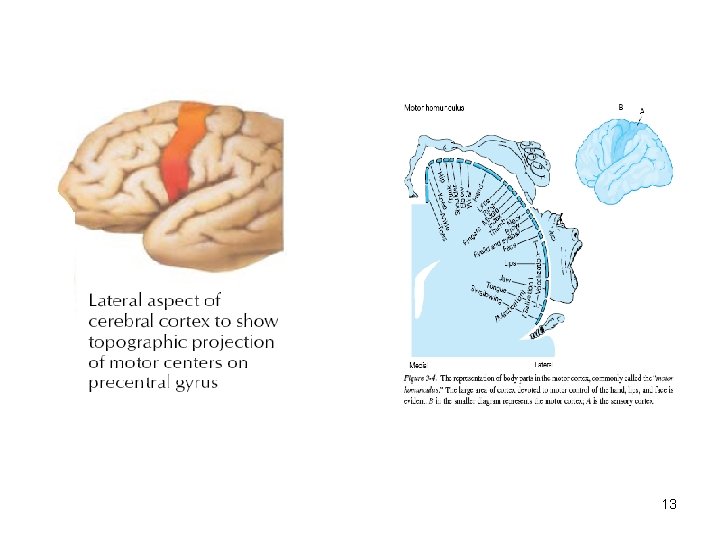
13

Supplemental motor area - SMA • • Higher degree organization area in which learned motor patterns (motor engrams) are stored that can be optionally chosen and after executed through the primary motor cortex area At this level influences on movements execution coming from the cerebellum and basal ganglia are expressed Neurological signs and symptoms related to SMA: 1. Paratonia (involuntary resistance to passive movement) 2. Eye deviation/gaze palsy: irritative lesions cause deviation in opposite direction, destructive lesions cause deviation to the side ipsilateral to the lesion 3. Motor aphasia/dysphasia; lesion is located at the bottom of the SMA of the dominant hemisphere (Broca’s motor centre for speech) 4. Apraxia (impaired execution of voluntary movements without motor palsy, sensory or coordination disorder in the background) 5. Ataxia (may be caused by the lesion of the corticopontocerebellar pathways) 6. Primitive reflexes (of capturing and sucking) 14
15

Prefrontal area/region • • The largest multimodal cortical region in humans Location of the highest mental functions (complex judgment, planning, critical thinking, social functioning, personality) It contains no motor functions It is strongly connected to the medial nuclei of the thalamus, hypothalamus, other primary cortical areas (i. e. for vision, olfaction, hearing), with multimodal area located in TPO region, the limbic system, basal ganglia etc. 16

Prefrontal region Can be divided as: ü Dorsolateral part (for planning and control of social behavior) ü Orbitoventral part (for planning and impulse control) ü Mesial 17

Signs/symptoms of prefrontal area lesions • • Bilateral destructive damage of the frontal lobe convexity lead to attention disorder Also can be found: – disorder of behavior/conduct – personality changes – emotional incontinence (laughing or crying inconsistent to real external life) – lack of initiative – perservations (repeating the same words or movements) – disorders of instinct 18

Signs/symptoms of prefrontal area lesions • Pseudo-depressive syndrome: – apathy – indifference – reduction of vital dynamisms and instinctive impulses – affective dullness • Related to the damage in the frontal lobe convexity area • • Pseudo-psychopathic syndrome: – lack of criticism – lack of instinct control – propensity to lasciviousness and practical jokes (Moria) Generally occurs more frequently in damage of frontobasal structures 19

Signs/symptoms of prefrontal area lesions • • Foster Kennedy syndrome Rarely seen and indicates the expansive process in the anterior cranial fossa: – ipsilateral anosmia – vision problems due to pressure on optic nerve – contralateral papilla stagnans • • Part of the frontal lobe is also the primary gustatory area located in the opercular part of the frontal lobe Destructive and irritative lesions in this area rarely give rise to clinically relevant symptoms 20

Signs and symptoms of parietal lobe disorders • • The primary sensory regions - somatosensory cortex; located in the area of postcentral gyrus and the posterior part of lobulus paracentralis (the medial part of the brain hemispheres) It is responsible for conscious perception of somatosensory stimuli: – pain sensation – temperature – and proprioception of the contralateral half of the body • • • Sensory stimuli in the parietal lobe arrive from posterolateral and posteromedial nucleus of the thalamus Vestibular sensations also ends at primary sensory cortex Perception of vibration and position is not possible without the involvement of the parietal cerebral cortex 21
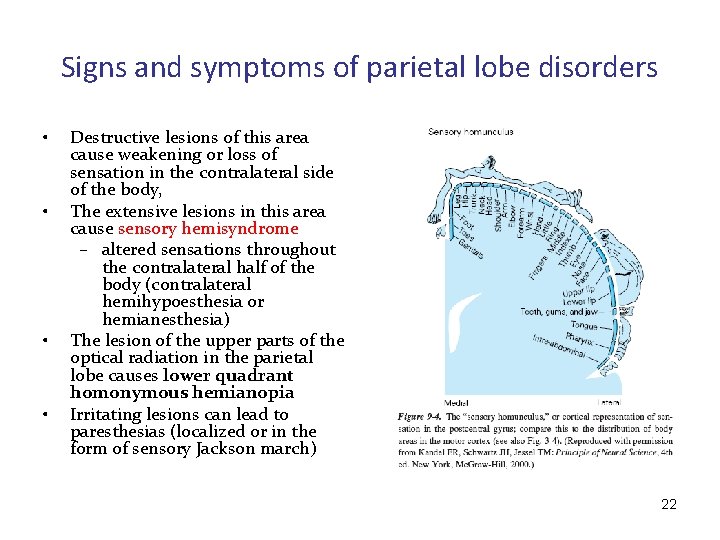
Signs and symptoms of parietal lobe disorders • • Destructive lesions of this area cause weakening or loss of sensation in the contralateral side of the body, The extensive lesions in this area cause sensory hemisyndrome – altered sensations throughout the contralateral half of the body (contralateral hemihypoesthesia or hemianesthesia) The lesion of the upper parts of the optical radiation in the parietal lobe causes lower quadrant homonymous hemianopia Irritating lesions can lead to paresthesias (localized or in the form of sensory Jackson march) 22

Signs and symptoms of parietal lobe disorders • • The posterior parts of the parietal lobe, together with visual associative areas, integrate somatosensory, visual and motor information (i. e. conducting a conversation while preparing lunch) Damages of the associative/posterior areas of the parietal lobe cause different forms of agnosia • Agnosia - disorder where the ability of complex elaboration of elementary sensory stimuli is missing: – astereognosia or tactile agnosia - inability to recognize objects by touch – baroagnosia - the inability of determining the weight of objects held in the hand – fingers agnosia - the inability to recognize and name fingers – prosopoagnosia - failure to identify a person's face, but the recognition of the person involved is preserved by hearing his/her voice 23

Signs and symptoms of parietal lobe disorders • Damage to the dominant hemisphere is characterized by: – – • right-left disorientation dyslexia/alexia dyscalculia/acalculia fingers agnosia and agraphia These disorders, if they occur together, make up the Gerstmann syndrome • Lesion in the parietal lobe of the non-dominant hemisphere can give rise to: – anosognosia (inability to recognize motor deficit) – constructive apraxia (inability to void graphic characters) – neglect phenomenon or syndrome 24
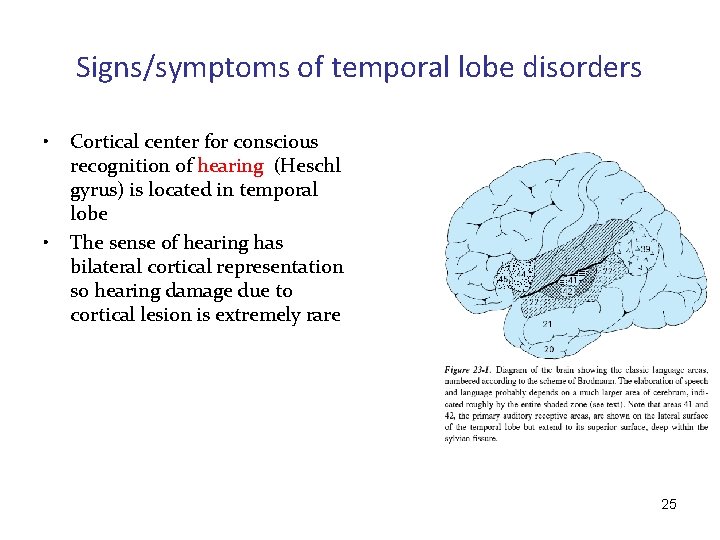
Signs/symptoms of temporal lobe disorders • • Cortical center for conscious recognition of hearing (Heschl gyrus) is located in temporal lobe The sense of hearing has bilateral cortical representation so hearing damage due to cortical lesion is extremely rare 25

Signs/symptoms of temporal lobe disorders • • • Speech is the most complex cognitive function of human being The speech centers are mainly localized in the fronto-temporal associative cortex of the left (dominant) hemisphere of the brain There are two main cortical centers for speech: – main motor speech (Broca) center in the frontal lobe – main sensory speech centre located in the posterior part of the temporal lobe on the border with the parietal lobe (Wernicke center) • These areas are separated from the primary motor and sensory cortex and primary cortical regions for hearing and vision 26

Signs/symptoms of temporal lobe disorders • • Destructive lesion of the posterior portion of the temporal gyrus in the dominant hemisphere causes loss of speech understanding i. e. sensory aphasia Lesions in the white matter of the temporal lobe with affection of the lower parts of optical radiation (Mayer’s loop) cause upper contralateral quadrantanopia 27

Signs/symptoms of temporal lobe disorders • • The lesions in the dominant temporal lobe cause a disorder of learning of verbal information and the same lesion in non-dominant lobe leads to learning difficulties of visuospatial information Irritating lesions to the upper part of the temporal lobe causes auditory hallucinations in the form of tinitus (clinically extremely rare) The excitation of the surrounding areas can rarely cause dizziness and instability Finally the most frequent complex partial seizures are of temporal lobe origin 28

Signs/symptoms of occipital lobe disorders • • • Occipital lobe is mainly related to the function of vision Primary visual cortex is located in the depths of calcarine sulci above and below it on the medial surface of the occipital lobe Due to the macroscopic appearance of the area the term striatal cortex is also used 29

Signs/symptoms of occipital lobe disorders • Destructive lesions to the optic area of the occipital lobe can cause: – Scotoma – Blindness in case of bilateral, complete damage of cortical visual centers – or homonymous hemianopia in case of unilateral cortical damage • Irritative damage to the optic cortical areas causes focal partial seizures 30
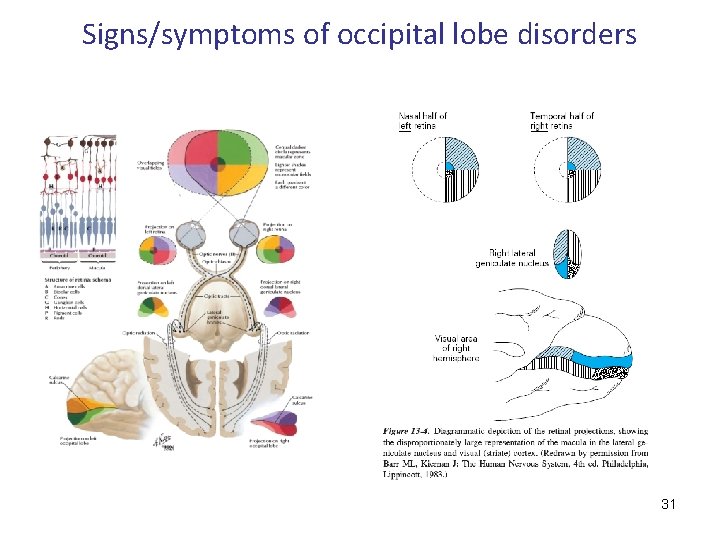
Signs/symptoms of occipital lobe disorders 31

Hippocampus and limbic lobe • • Damage to the hippocampal structures causes amnestic syndrome Damage to the limbic system causes abnormal affective and emotional reactions, aggressive behavior Bilateral or even unilateral damage to the hippocampus and hippocampal gyrus cause substantial damage to short-term memory Bilateral damage to the cingulate gyrus cause apathy, akinesia and mutism 32

Dysconnection syndromes • They arise when pathological process separates one part of the cortex from another: – alexia without agraphia; the patient can write but can not read - the lesion in the left occipital lobe and the posterior parts of the corpus callosum; right occipital lobe has lost communication with the speech network in the left dominant hemisphere – ideomotor apraxia: for example, the patient does not raise his left arm on command, but it is regularly used in everyday life (lesions of the left frontal cortex and the anterior part of the corpus callosum) – conductive aphasia: occurs when fasciculus arcuatus is damaged (it connects Brocka and Wernicke regions) repetition is, of all aspects of speech features, the mostly affected 33

Basal ganglia syndromes • • Hypokinesia – refers to condition of reduced/decreased body movements, usually accompanied with increased muscle tone/rigidity (e. g. Parkinson disease) Hyperkinesia – refers to condition of excessive abnormal movements 34

Hyperkinetic syndrome • • Condition of excessive abnormal movements Tremor – the most frequent hyperkinetic syndrome, occurs due to the rhythmic, alternating contractions of agonist and antagonist muscles (fingers, limbs, tongue, face, head), in tremor movements are always bidirectional while in clonus are unidirectional/unifasic Chorea - rapid involuntary irregular movements of different body parts (HD) Dystonia - a state of prolonged simultaneous contraction of antagonist and agonist muscles causing a abnormal posture or position of body parts (mainly the trunk and proximal parts of the limbs) 35

Hyperkinetic syndrome • • • Myoclonia - the fastest involuntary movements known in neurology, completely irregular, arrhythmic, occur in epilepsy, encephalopathy, deg. disease (JC), but there is also a physiological myoclonus Asterixis - irregular interruption of muscle tone when keeping the limb in a certain position (looks like a specific movement), especially after the patient tries to regain the starting position - negative myoclonus; occurs with encephalopathy, before wrongly marked as flapping tremor Ballismus - basically it is a unilateral chorea but movements are more vehement and engage more proximal muscles, lesion is in contralateral n. subthalamicus 36
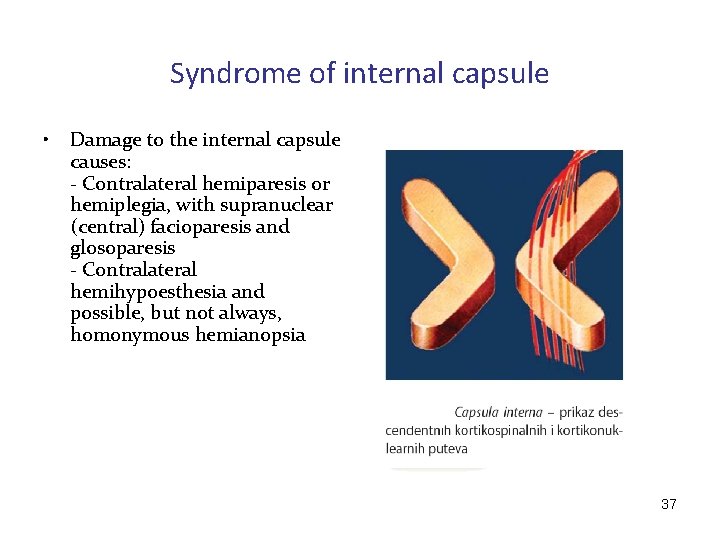
Syndrome of internal capsule • Damage to the internal capsule causes: - Contralateral hemiparesis or hemiplegia, with supranuclear (central) facioparesis and glosoparesis - Contralateral hemihypoesthesia and possible, but not always, homonymous hemianopsia 37

Syndrome of internal capsule • • The motor and/or sensory neurological deficit on one half of the body is called hemisyndrome Lesion in the internal capsule causes: – motor (hemiplegia) hemisyndrome – sensory hemisyndrome – the most common are mixed, motor and sensory, due to the proximity of motor and sensory pathways in the internal capsule 38
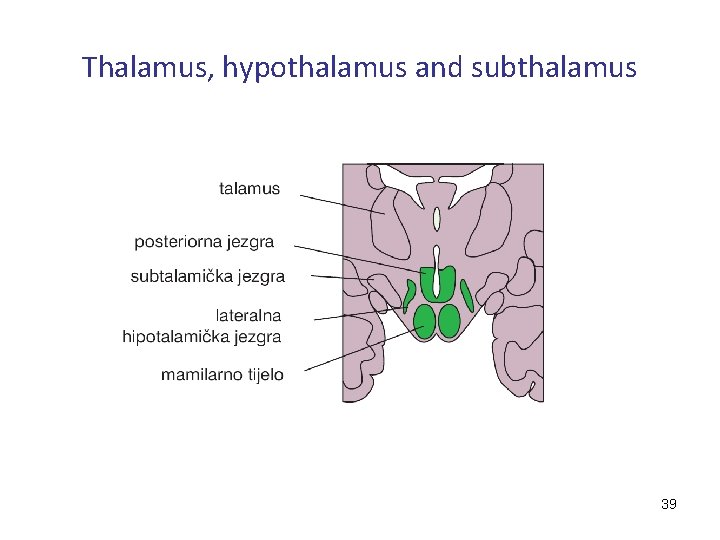
Thalamus, hypothalamus and subthalamus 39

Thalamic syndrome • • loss of sensation in the contralateral half of the body (hemihypoesthaesia) spontaneous pain (thalamic hyperpathia) homonymous hemianopia “thalamic hand" (hand flexion and hyperextension of interphalangeal joints, contralateral damage) mild hemiparesis due to concomitant damage to the internal capsule (which is close to the thalamus) choreoatetotic movements mild incoordination 40

Hypothalamic syndrome • Lesion in hypothalamic area can give rise to: - disorders of temperature regulation - disorders of carbohydrates (hyperglycemia and glycosuria), lipid (Frochlichov syndrome) and water metabolism (diabetes insipidus) - disorders of wake cycle/sleep and appetite (polyphagia, anorexia) 41

Brain stem syndromes • • The brain stem consists of: – midbrain (III and IV cranial nerves) – pons (V-VIII cranial nerves) – medulla oblongata (VIII-XII cranial nerves) Lesions in the brainstem may give rise to crossed/alternating sydromes with affection of cranial nerves ipsilateral to the lesion in the brain stem and contralateral hemiparesis (due to fact that corticospinal tract crosses to the opposite side of the spinal cord in lower parts of medulla oblongata) 42
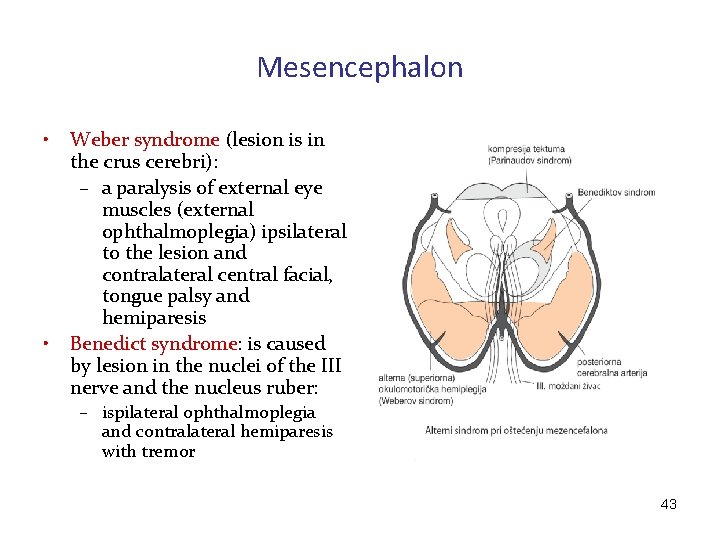
Mesencephalon • • Weber syndrome (lesion is in the crus cerebri): – a paralysis of external eye muscles (external ophthalmoplegia) ipsilateral to the lesion and contralateral central facial, tongue palsy and hemiparesis Benedict syndrome: is caused by lesion in the nuclei of the III nerve and the nucleus ruber: – ispilateral ophthalmoplegia and contralateral hemiparesis with tremor 43
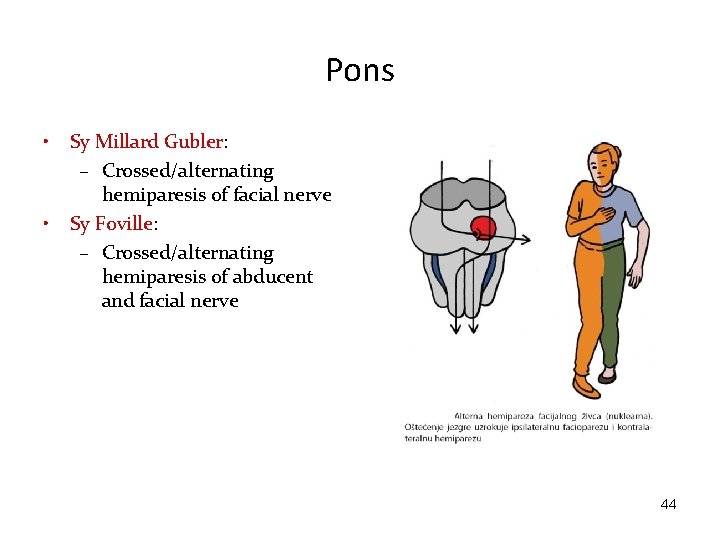
Pons • • Sy Millard Gubler: – Crossed/alternating hemiparesis of facial nerve Sy Foville: – Crossed/alternating hemiparesis of abducent and facial nerve 44

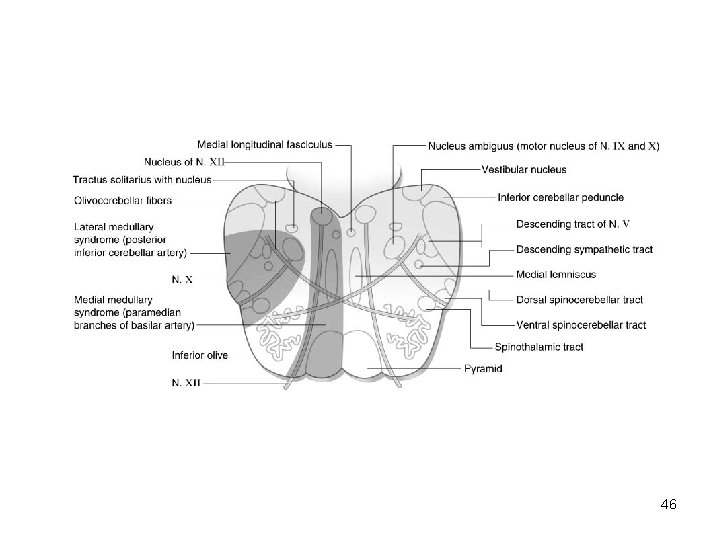
Medulla oblongata • Jackson syndrome: • Wallenberg syndrome (dorsolateral medullary syndrome) crossed sensory syndrome - often occurs after ischemic vacular lesion in irrigation area of art. cerebellaris inferior posterior (PICA): – ipsilateral glosoparesis, paresis of the soft palate, pharynx, larynx, trapezius muscle paresis and sternocleidomastoideus – contralateral hemiparesis – Ipsilateral paralysis of muscles of the soft palate, pharynx and trachea, ipsilateral Horner's syndrome, nystagmus, ispilateral analgesia and termoanesthesia of the face with loss of corneal reflex, ipsilateral limb ataxia – Contralateral analgesia and termoanesthesia due to affection of spinothalamc tract 45
46
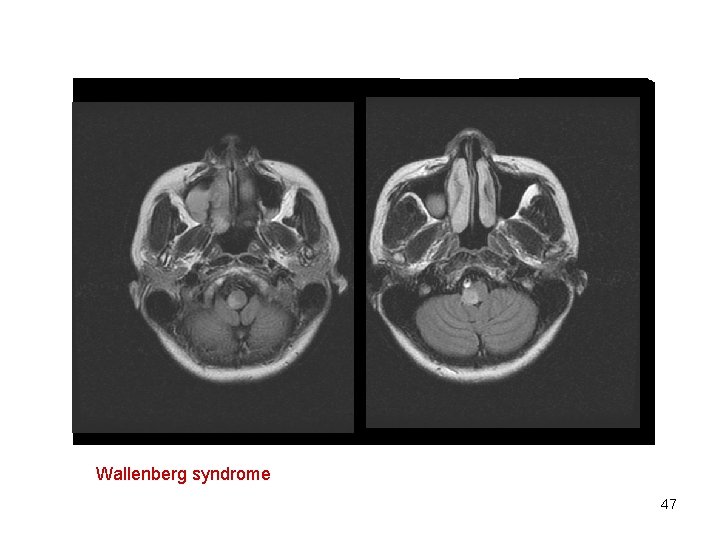
Wallenberg syndrome 47
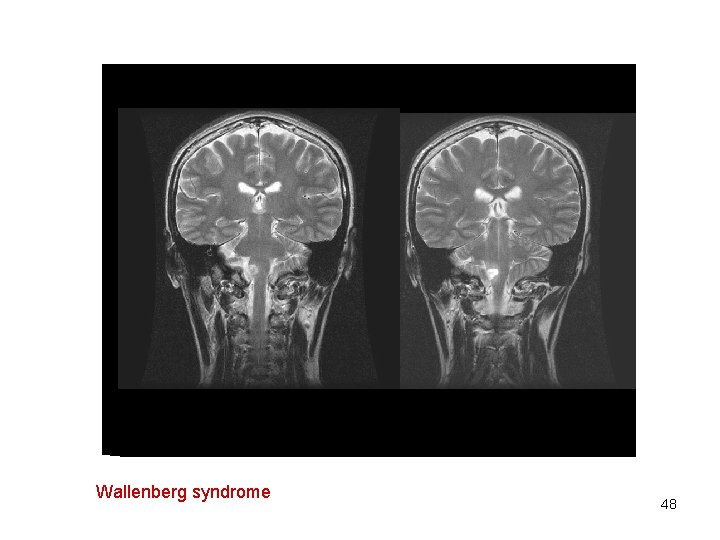
Wallenberg syndrome 48
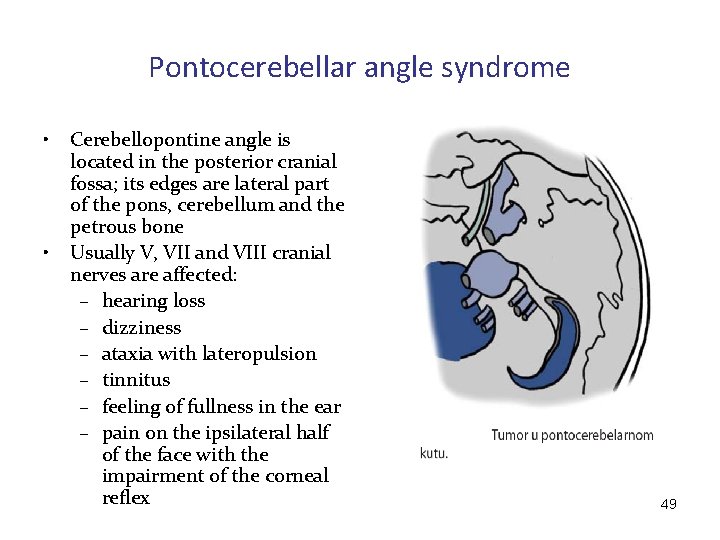
Pontocerebellar angle syndrome • • Cerebellopontine angle is located in the posterior cranial fossa; its edges are lateral part of the pons, cerebellum and the petrous bone Usually V, VII and VIII cranial nerves are affected: – hearing loss – dizziness – ataxia with lateropulsion – tinnitus – feeling of fullness in the ear – pain on the ipsilateral half of the face with the impairment of the corneal reflex 49

Bulbar palsy syndrome • • • The lesion is located in motor nuclei of IX, X, XI and XII cranial nerves (but sometimes V and VII nerves are affected as well) Etiology: cerebrovascular disease or motor neuron disease (MND) Clinically only signs of lower motor neuron lesions are present – paralysis, atrophy and fasciculations of the tongue muscles – dysphagia – dysarthria – reflexes of the soft palate, pharynx and mandibular reflex are lost 50

Pseudobulbar palsy • • The lesion is in the corticobulbar pathways innervating nuclei of IX, X, XI and XII nerves (possibly trigeminal and facial nerve as well) In pseudobulbar palsy functions of breathing, coughing, sneezing, phonation, chewing, swallowing and mimic expression are disturbed It often leads to the release of pathological laughing and crying In neurological status signs of affection of central motor neuron can be found (reflexes are preserved or exaggerated) 51
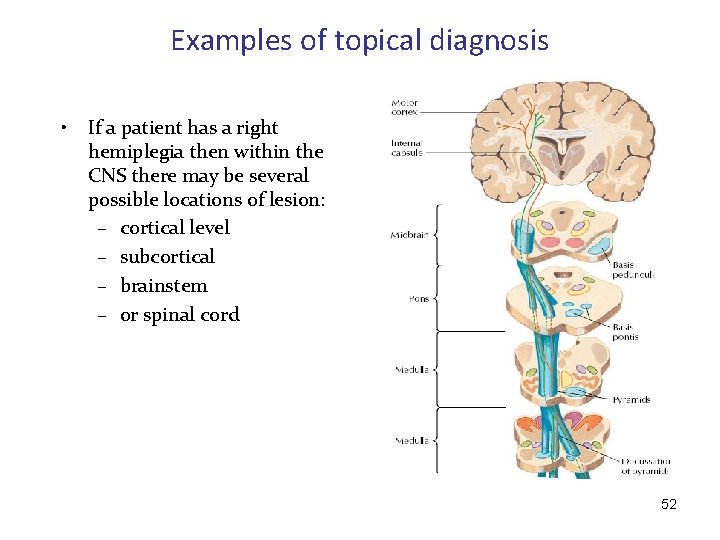
Examples of topical diagnosis • If a patient has a right hemiplegia then within the CNS there may be several possible locations of lesion: – cortical level – subcortical – brainstem – or spinal cord 52

Hemiplegia due to cortical lesions • Examine the speech: – If the patient regularly speaks and understands the speech of another person (if it is not able to do so, then it’s aphasia) – Listen to spontaneous speech – Check are there any paraphasias (wrong words with wrong meaning; phonemic and semantic) – Check whether the patient can designate items that are shown to him – If he/she can repeat the phrase you tell him – Whether it follows your command (e. g. . "Touch the left thumb to the right ear") – Ask if the patient is right-handed (almost all right-handed and in majority lefties have left hemisphere as dominant for speech) 53

Hemiplegia due to cortical lesions • • Check possible loss of cortical sensory modalities (graphesthesia, stereognosia); preserved primary sensation is required in order to perform tests of cortical sensory modalities (e. g. pain, temperature, touch) Touch the patient in different places on his/her leg and arm, he/she should be aware of it Touch the same places on both sides of the body at the same time (to see if there is neglect present) If there is a loss of cortical sensory functions, then it implies damage to the cortex or direct subcortex 54

Hemiplegia due to cortical lesions • • • inequality of neurological deficit in the face, arm and leg: pronounced palsy of the face and arm suggests affection of irrigation territory of the middle cerebral artery (MCA) if the deficit is more pronounced on the leg then the irrigation area of anterior cerebral artery (ACA) is affected conjugate eye deviation in neurological status suggests cortical lesion (more often) or a lesion in the pons (rare) activated cortical centre for horizontal conjugate eye movement moves both eyeballs to the opposite side and the pontine centre to the ipsilateral side 55

Hemiplegia due to cortical lesions • • Examine if there is hemianoptic loss of vision (it suggests a lesion of the occipital cortex or white matter in the frontal and temporal lobes - radiatio optica) Concurrent occurrence of epileptic seizures together with hemiplegia suggests cortical pathology (epilepsy is a disease of the cortical neurons) 56

Hemiplegia due to subcortical lesions • Sites of possible lesions are internal capsule, basal ganglia or thalamus: – Usually the face, arm and leg are equally affected both in terms of motor and/or sensory deficits – Speech is typically spared 57

(right) hemiplegia due to lesions in the brain stem • Crossed/alternating hemiplegia is typical for brain stem lesions: – For example, the right hemiplegia is caused by lesions located in the left part of the brain stem along with the ispilateral cranial nerve deficits • • Sometimes right hemiplegia is accompanied with left-limb ataxia (ipsilateral to the damage in the brainstem) If hemiplegia is accompanied by nystagmus, especially vertical, then it is likely that lesion is located in the brainstem Sometimes there is intersected sensory deficits – crossed sensory hemisyndrome (e. g. failure of sensation on the left side of the face ipsilateral to the lesion along with the loss of sensation for pain and temperature on the contralateral, right arm and leg) Dysarthria, dysphagia and internuclear ophthalmoplegia are also signs of brain stem affection 58

Tips for assessing patients with left hemiplegia • • Left hemiplegia is caused by a lesion in the right side of the brain Right hemisphere is the nondominant one so typically speech disorders by dysphasia type are missing (it is possible to observe some degree of dysarthria), attention should be paid to some other things: – check whether the patient ignores the left side of the body or a room – whether ignores touching the left side of the body while touching the right side of the body in the same time – whethere is a neglect of visual information coming from the left side of space • • Loss of concern for neurological deficit (syndrome of anosognosia – ignoring of serious neurologic deficit) Constructive apraxia and dressing apraxia 59

Thank you for your attention… 60
- Slides: 60