Bovine Tuberculosis Monaya Ekgatat NIAH TB Bovine Tuberculosis

Bovine Tuberculosis Monaya Ekgatat NIAH TB

Bovine Tuberculosis -Introduction -Etiology & Epidemiology -Clinical Signs -Post mortem lesions -Diagnosis -Public Health -Prevention and control NIAH

Introduction Zoonosis human -aerosol -ingestion Developed countries -reduced prevalence Control relies on -early diagnosis -removal of infected animal -tracing -exposing infected cases Less developed countries -still common -economic loss NIAH

Etiology and epidemiology Agents Mycobacterium tuberculosis (human Mycobacterium bovis (animal( Mycobacterium avium (bird( NIAH

Etiology and epidemiology Mycobacterium tuberculosis complex (MTB. Complex( M. tuberculosis M. bovis M. africanum M. microti M. caprae M. pinnipedii M. canetti

Mycobacterium bovis • Can survive for several months in the environment (cold, dark and moist condition) • 12 -24 o. C survival time 18 -332 days • Dry or moist soil (34 o. C) : 4 -8 weeks • Summer : 4 days
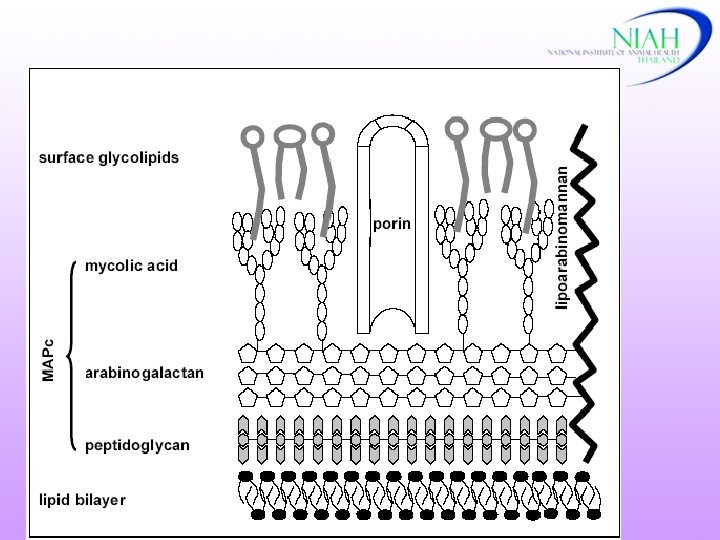

Etiology and epidemiology Maintenance hosts for M. bovis -cattle -buffalo Reservoir hosts -brush-tail possum (New Zealand) - badger (United Kingdom, Ireland) -deer (United States) - bison (Canada) -greater kudu, common duiker African buffalo, warthogs (Africa) NIAH

Badger

African buffalo Warthog

Common duiker Greater kudu

Brush-tail possum

Etiology and epidemiology Transmission Respiration----aerosal (short distance( Ingestion ( unpasteurized milk) Source of infectious bacteria - respiratory secretion -feces -milk ) -urine( -vaginal secretion -semen NIAH

Incubation Period • 3 weeks – years: under natural condition Morbidity and Mortality • 1 -2 animals = 0 - 40% infected = 0 - 10% developed gross lesions • Severity - dose of agents - individual immunity • Mortality : rare

Clinical Signs Chronic ( rare: acute & rapidly progressive( Early infection ---- asymptomatic Late stage: symptomatic -progressive emaciation -fluctuating fever -weakness -inappetite - moist cough (pulmonary involve) - dyspnea No specific signs Asymptomatic and anergic carriers (ill: stress, old age) NIAH

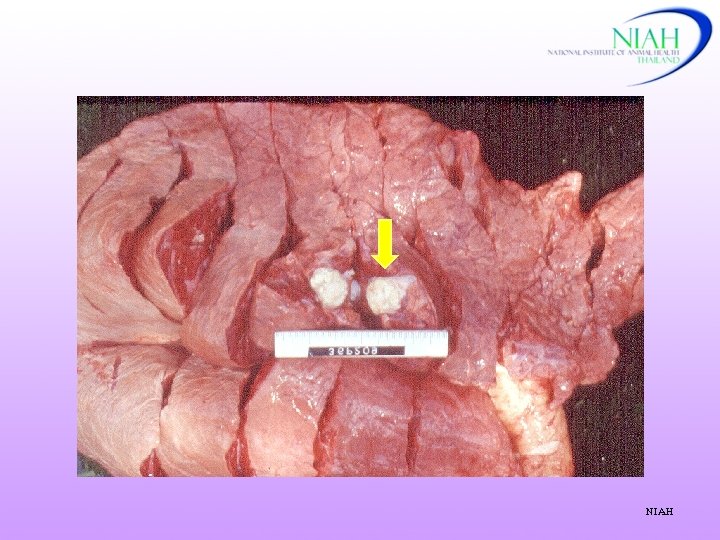
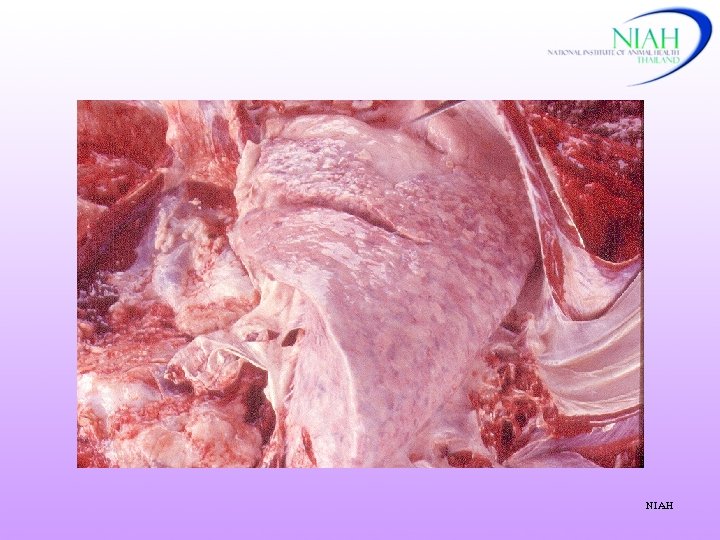
Post mortem lesions NIAH

NIAH
NIAH
NIAH
NIAH

Lymphnodes: calcified NIAH
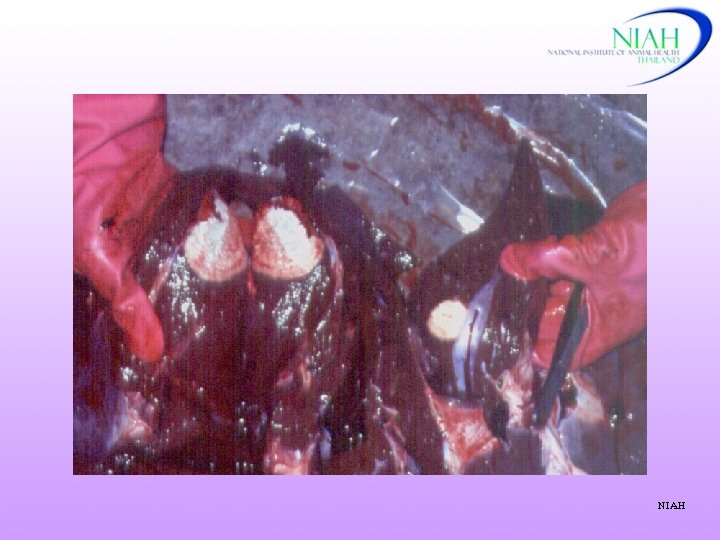
NIAH
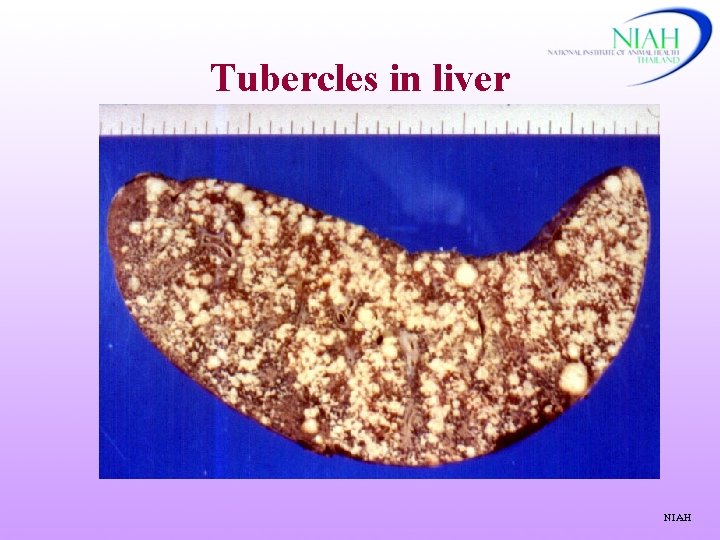
Tubercles in liver NIAH
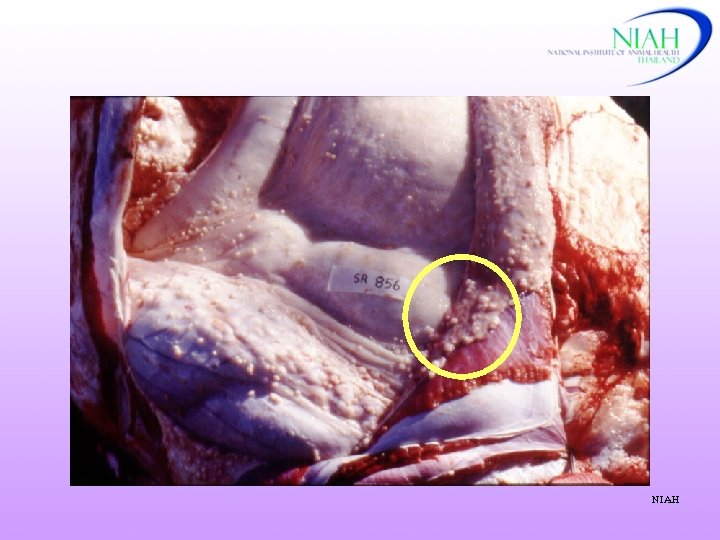
NIAH
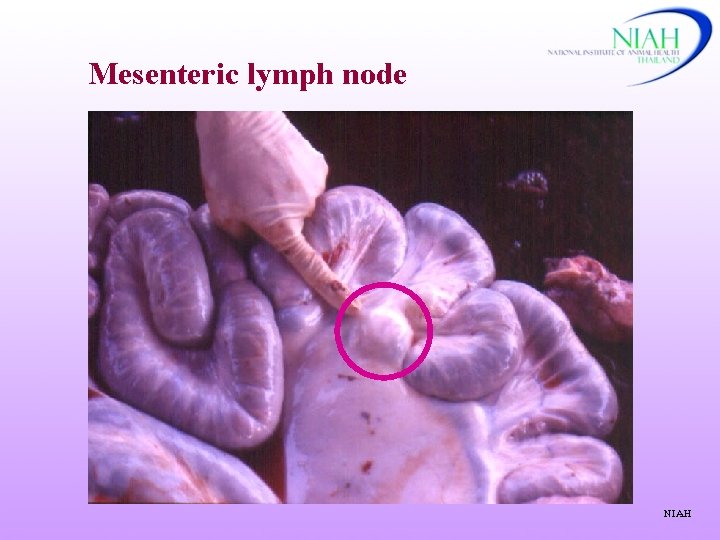
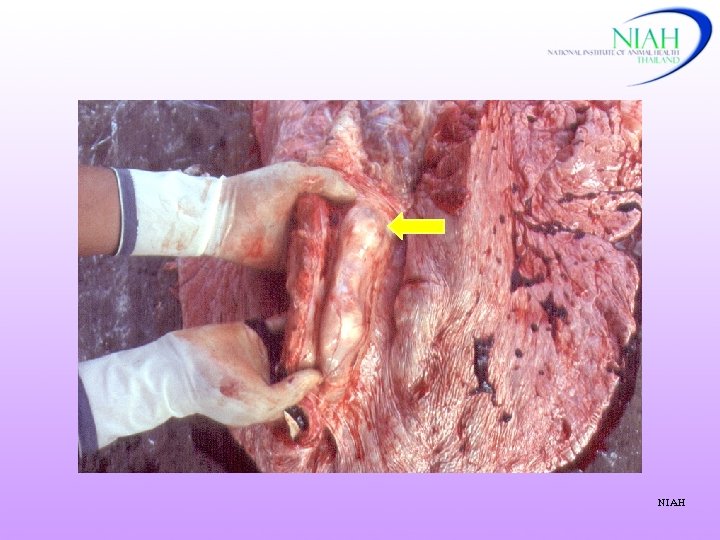
Mesenteric lymph node NIAH

Diagnosis • Clinical signs (lacking) • Laboratory diagnosis. 1 Identification of the agent a) Microscopic examination b) Culture of M. bovis (3 -6 weeks) - biochemical tests - culture characteristics c) Nucleic acid recognition methods NIAH

Diagnosis 2. Delayed hypersensitivity test Tuberculin test : SID, SCITT 3. Blood-based laboratory tests a) Gamma-interferon assay b) Lymphocyte proliferation assay c) ELISA (late stages of infection, anergic cattle)

Presumptive Diagnosis • Histopathology • Microscopic demonstration of acid-fast bacilli • Direct smear from clinical samples/tissues and stained with Z-N stain, fluorescent acid-fast stain or immunoperoxidase

Differential Diagnosis - Contagious bovine pleuropneumonia - Pasteurella or Corynebacterium pyogenes pneumonia - Aspiration pneumonia ( secondary infection) - Traumatic pericarditis - Caseous lymphadenitis or melioidosis (small ruminant) -Chronic aberrant liver fluke infestation NIAH
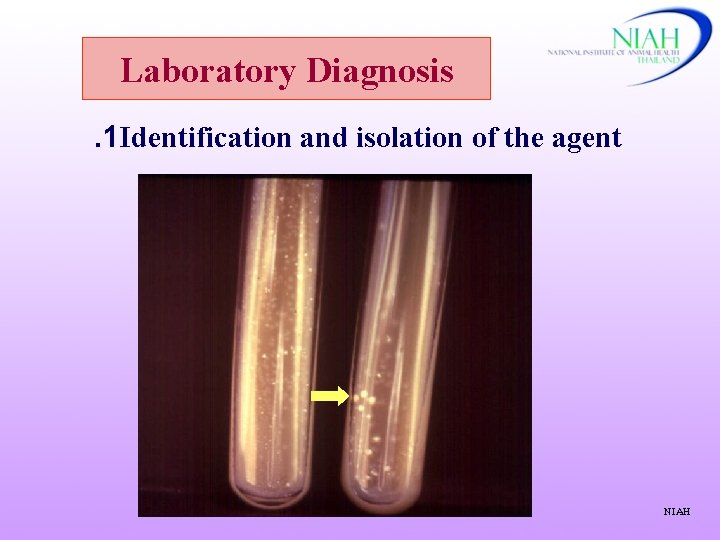
Laboratory Diagnosis. 1 Identification and isolation of the agent NIAH
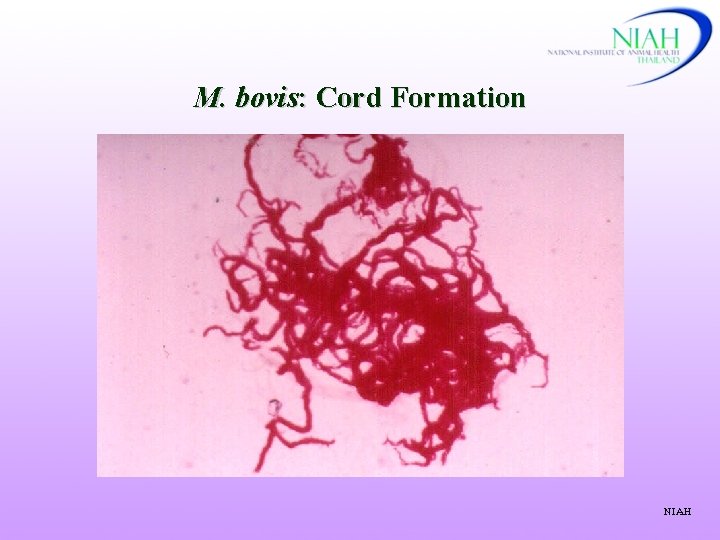
M. bovis: Cord Formation NIAH

M. bovis: granule in P&B NIAH
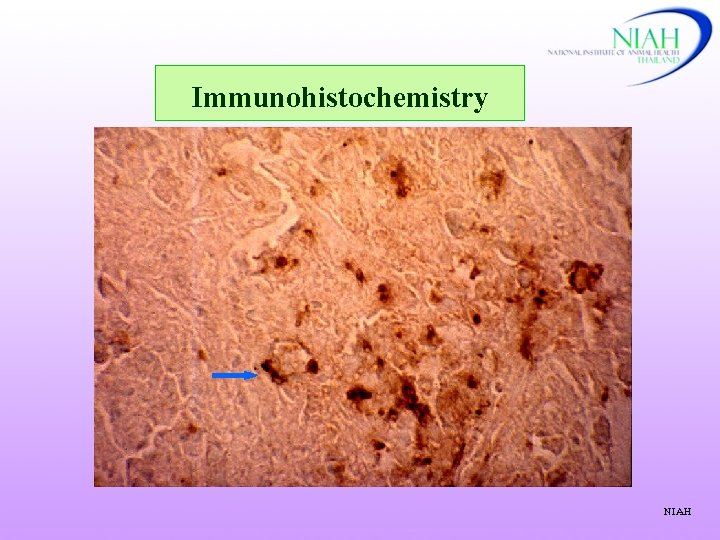
Immunohistochemistry NIAH
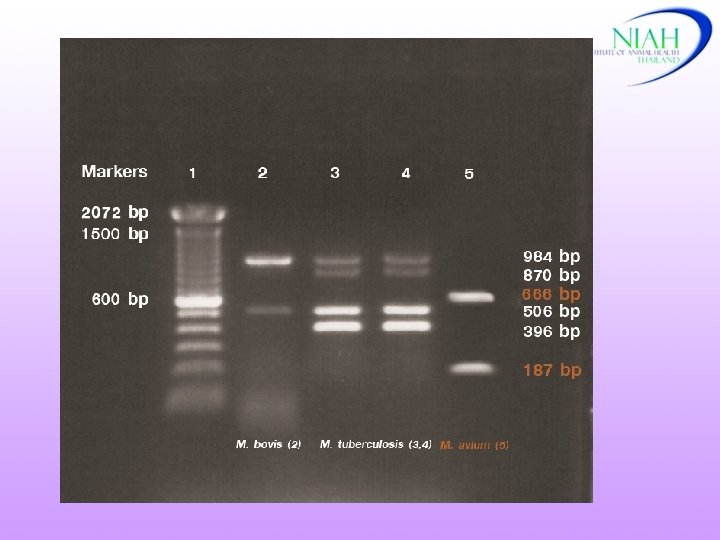
DNA - hybridization NIAH

ELISA: Detection of MTB complex 1 2 3 NIAH
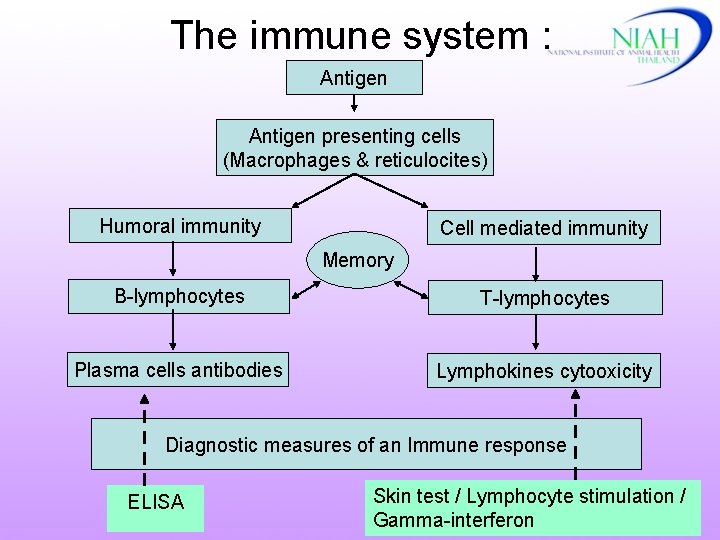
The immune system : Antigen presenting cells (Macrophages & reticulocites) Humoral immunity Cell mediated immunity Memory B-lymphocytes T-lymphocytes Plasma cells antibodies Lymphokines cytooxicity Diagnostic measures of an Immune response ELISA Skin test / Lymphocyte stimulation / Gamma-interferon

2. Tuberculin test Antigen: Bov. PPD 0. 1 ml(not more than 0. 2 ml) = 2, 000 IU – 5, 000 IU Work plan 0 1 stmeasure h injection 24 48 72 hrs 2 ndmeasure Negative reaction < 2 mm w/o local clinical signs Inconclusive reaction 2 -4 mm w/o local clinical signs Positive reaction ≥ 4 mm with or w/o local clinical signs (one fold + ≤ 8 mm) Retest: after 42 - 60 days (cattle), 120 days (deer) NIAH
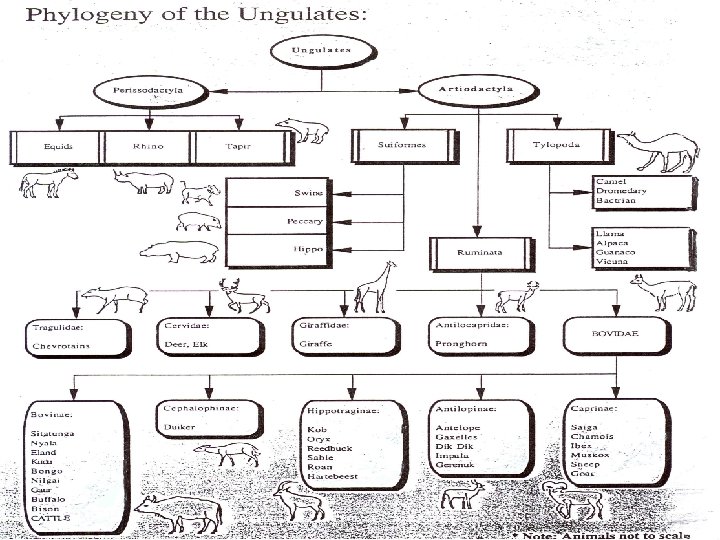
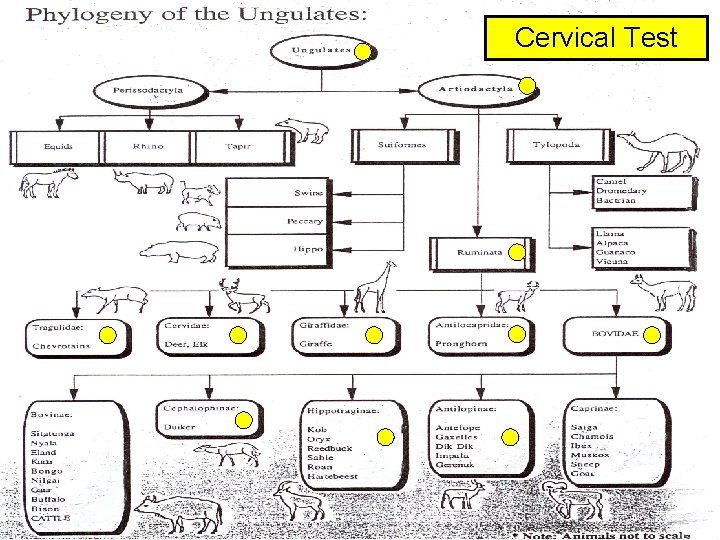
Cervical Test
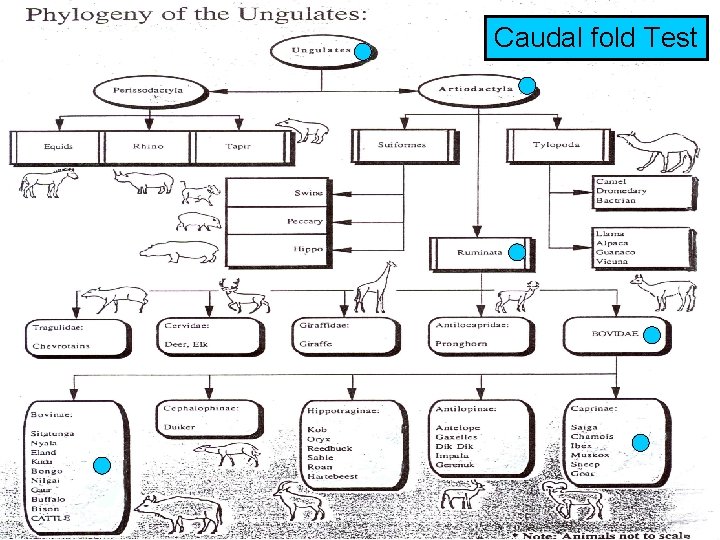
Caudal fold Test
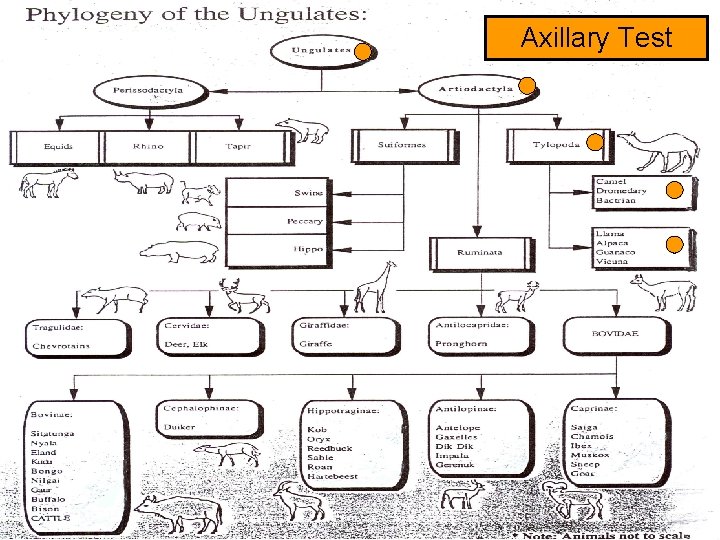
Axillary Test
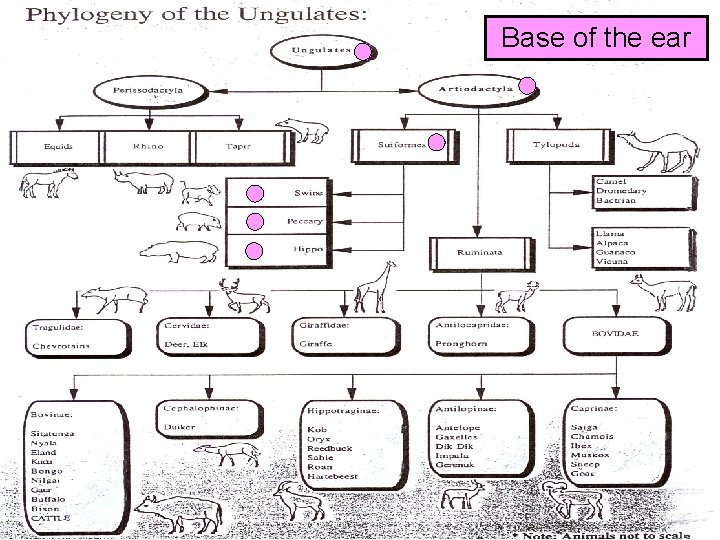
Base of the ear
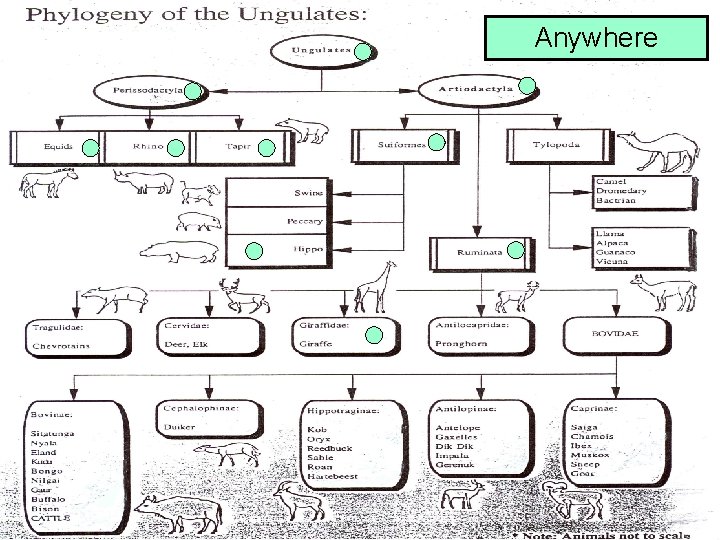
Anywhere

Tuberculin test NIAH

NIAH
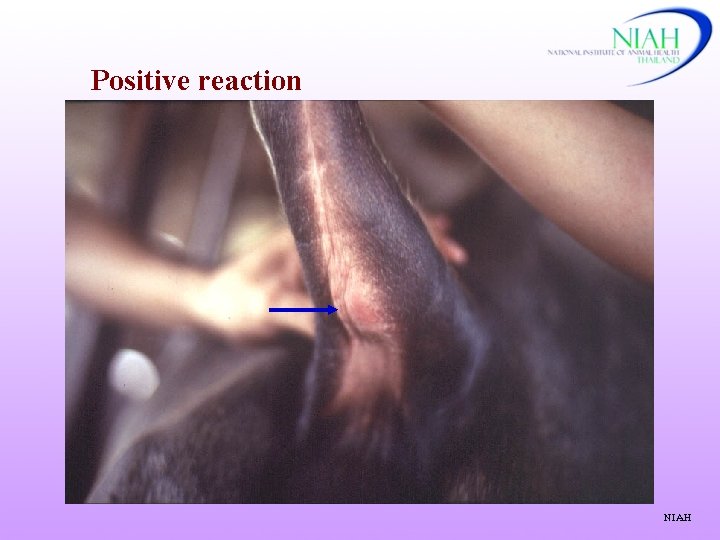
Positive reaction NIAH
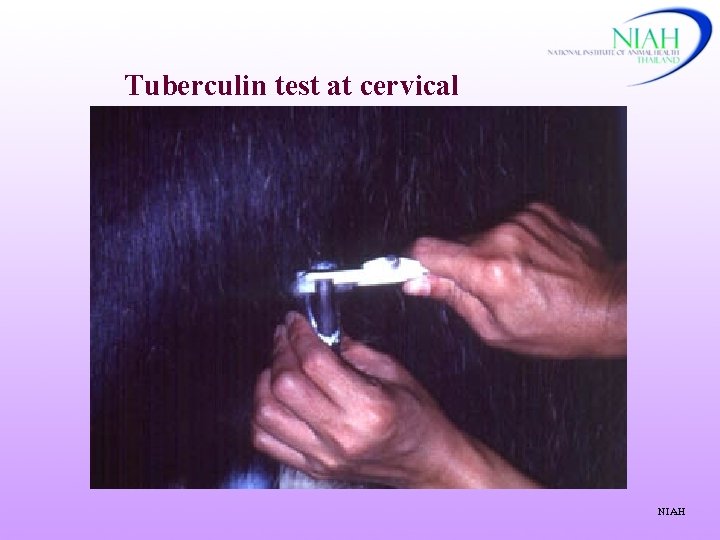
Tuberculin test at cervical NIAH
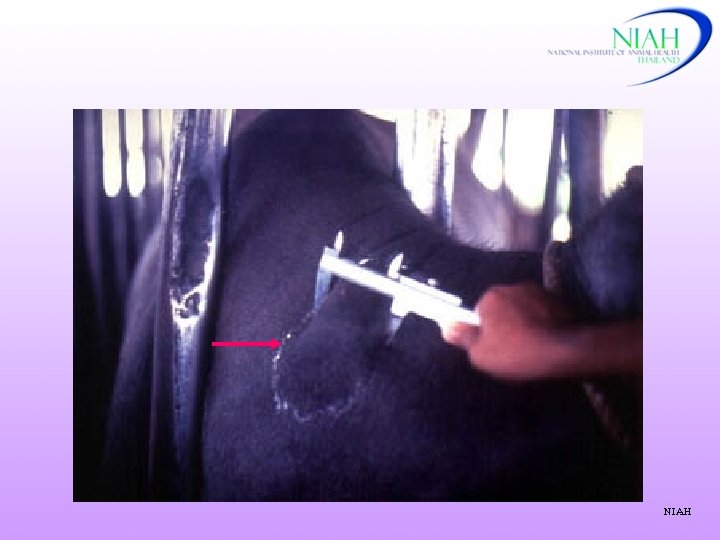
NIAH
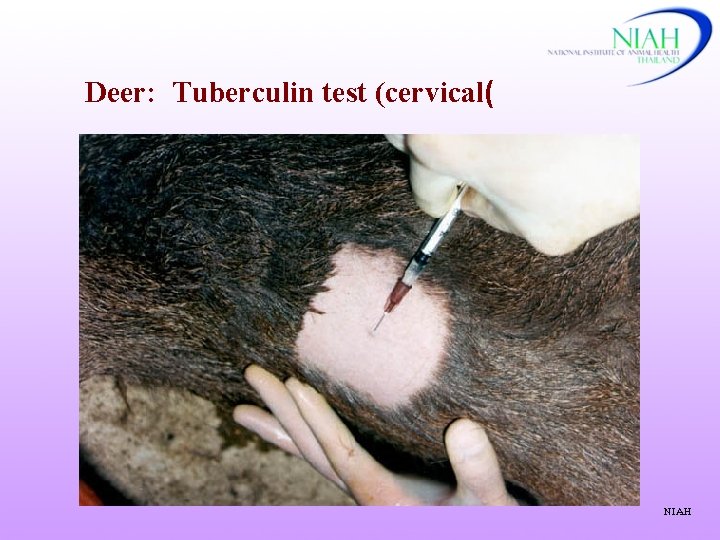
Deer: Tuberculin test (cervical( NIAH

NIAH

. 3 Blood-based laboratory tests a) Gamma-interferon assay) IFN) – early detection NIAH

NIAH

IFN Assay NIAH

b) Lymphocyte proliferation assay • Antigen : PPD-Bov, PPD-Avi • Not used for routine diagnosis - long incubation times - use of radio-active nucleotides • Expensive
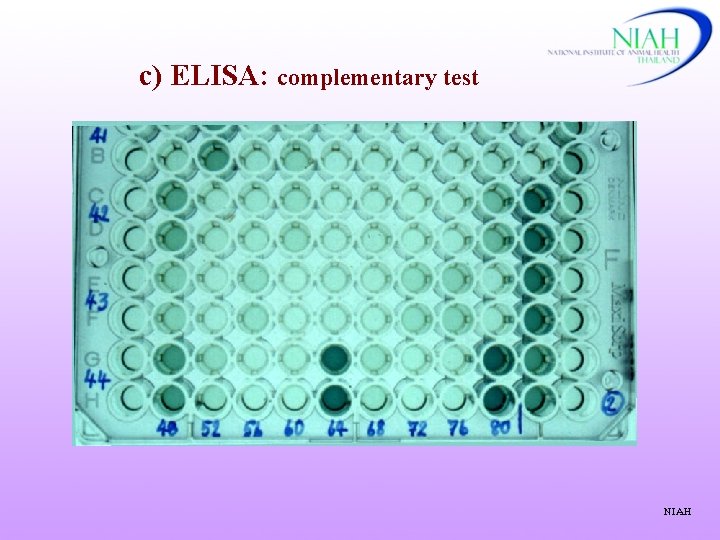
c) ELISA: complementary test NIAH
d) Chromatographic Immunoassay
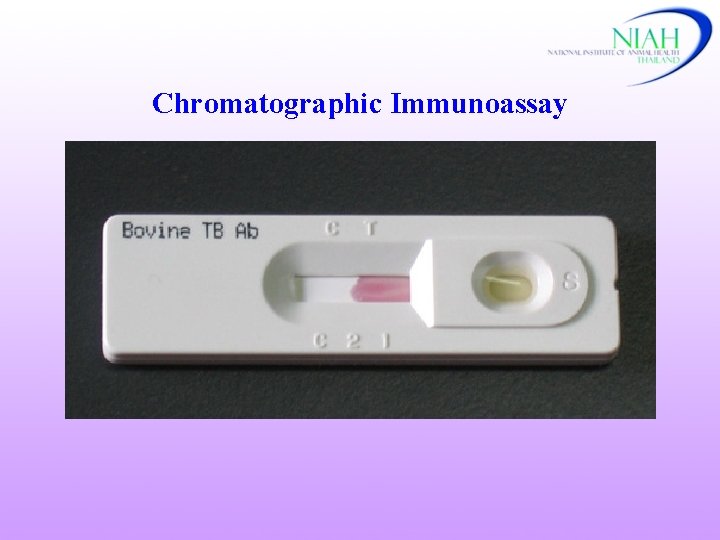
Chromatographic Immunoassay
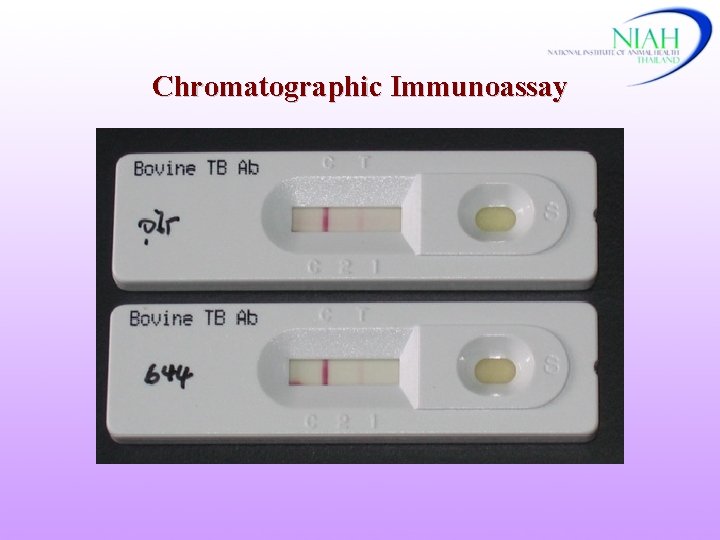
Chromatographic Immunoassay

Samples Collection • Live animal - body fluids: microbiological examination - blood samples: IFN, lymphocyte proliferation - serum: ELISA • Necropsy - abnormal lymph nodes - affected organs (lung, liver and spleen) For bacteriology and histopathology

Public Health • Due to M. bovis : very rare • Asymptomatic • Localized: lymph nodes, skin, bones and joints, genitourinary system, meninges or respiratory system

Prevention and Control Sanitary Prophylaxis - Tuberculin Test - Re-testing schedule for high risk herds - Animal movement control, identification slaughter and surveillance - Disinfection Effective disinfectants: 5 % phenol, iodine solution, glutaraldehyde and formaldehyde Environment : 1% sodium hypochlorite (long contact time) NIAH

Prevention and Control - Quarantine measures - Slaughter inspection surveillance and trace - back Surveillance in other animals Pasteurisation of milk - Medical Prophylaxis No chemophophylaxis or treatment NIAH

Control • Test-and-slaughter (domestic animals) • Test-and-segregation Affected Herds - re-tested periodically


r o f u o y k n a Th n o i t n e t t a r u yo
- Slides: 66