Borderline Ovarian Tumors BOT Prof Dr A Ph

Borderline Ovarian Tumors (BOT) Prof. Dr A. Ph. MAKAR Gynaecology/Oncology ZNA Middelheim University Hospital Gent © 2008 Universitair Ziekenhuis Gent 1
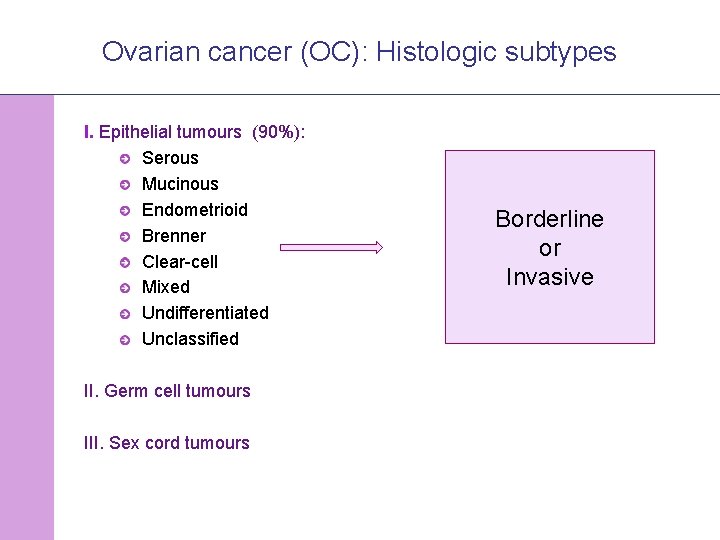
Ovarian cancer (OC): Histologic subtypes I. Epithelial tumours (90%): Serous Mucinous Endometrioid Brenner Clear-cell Mixed Undifferentiated Unclassified Borderline or Invasive II. Germ cell tumours III. Sex cord tumours © 2008 Universitair Ziekenhuis Gent 2

Borderline Tumors of the Ovary = separate entity Differs from invasive cancers Etiology Genteic profile Epidemiology Clinical & pathological presentation CA 125 Prognosis Response to adjuvant chemotherapy Overtreatment: surgically and pharmacologically © 2008 Universitair Ziekenhuis Gent 3
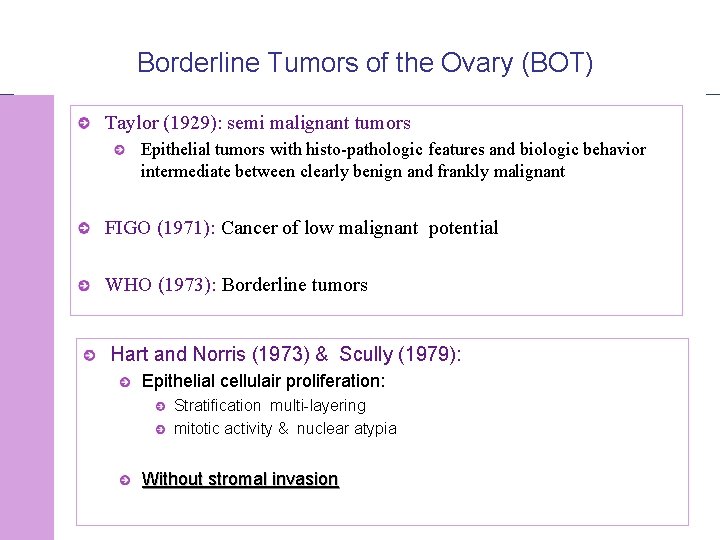
Borderline Tumors of the Ovary (BOT) Taylor (1929): semi malignant tumors Epithelial tumors with histo-pathologic features and biologic behavior intermediate between clearly benign and frankly malignant FIGO (1971): Cancer of low malignant potential WHO (1973): Borderline tumors Hart and Norris (1973) & Scully (1979): Epithelial cellulair proliferation: Stratification multi-layering mitotic activity & nuclear atypia Without stromal invasion © 2008 Universitair Ziekenhuis Gent 4

Etiology & Risk Factors Increased serum gonadotrophin levels: postmenopausal & fertility treatment ? ? Increasing parity & lactation reduces risk of BOT Talc minerals in hygienic powders Oral contraceptives decrease relative risk of IOC of 0. 6 (Kumle 2004): This protective effect was persistent and related to duration of use Not in case of BOT No correlation with positive family history BRCA mutations don’t increase the risk of BOT © 2008 Universitair Ziekenhuis Gent 5

Incidence OC in western Europe 14 -19/100. 000 females per year: OC in Belgium (1998): 813 patients BOT represents (9 -20%) of OC: Norwegian Radium Hospital: 12% Mean age: 45 years vs (invasive >55 y) 27% are <40 years Localized tumors (FIGO stadium I): 93% Regional (stage II) or distant spread (stage III) : 7% vs 70% (invasive) © 2008 Universitair Ziekenhuis Gent 6
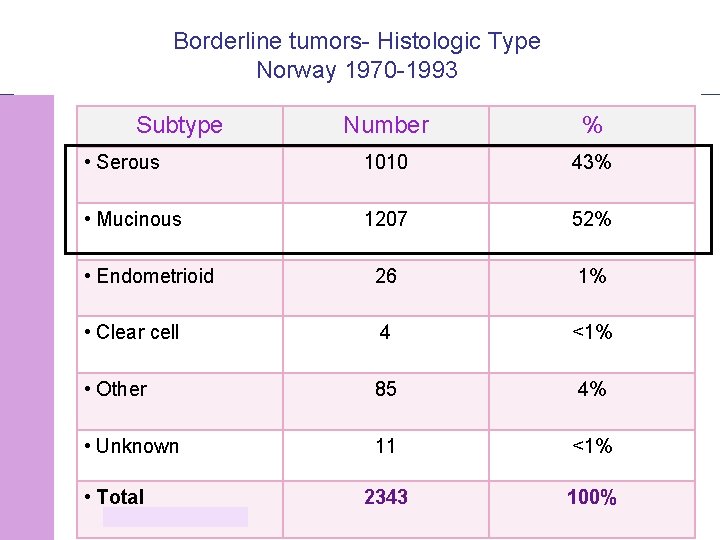
Borderline tumors- Histologic Type Norway 1970 -1993 Subtype Number % • Serous 1010 43% • Mucinous 1207 52% • Endometrioid 26 1% • Clear cell 4 <1% • Other 85 4% • Unknown 11 <1% 2343 100% • Total © 2008 Universitair Ziekenhuis Gent 7
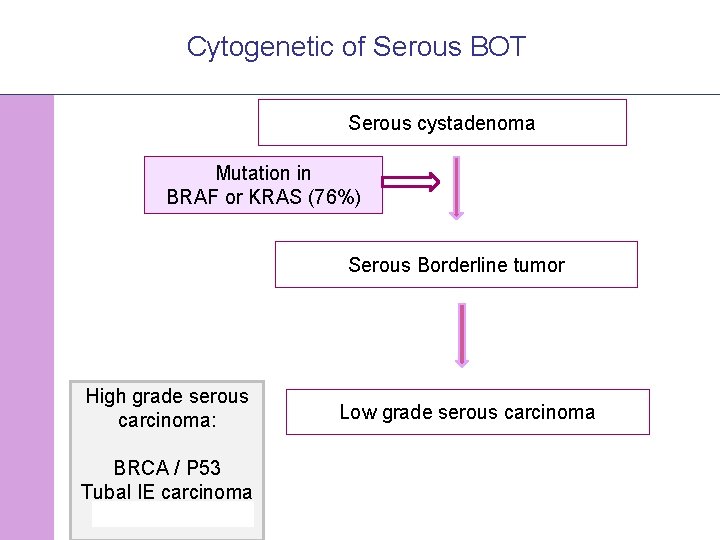
Cytogenetic of Serous BOT Serous cystadenoma Mutation in BRAF or KRAS (76%) Serous Borderline tumor High grade serous carcinoma: Low grade serous carcinoma BRCA / P 53 Tubal IE carcinoma © 2008 Universitair Ziekenhuis Gent 8

I. Serous Borderline Tumors >40% of borderline tumors Bilaterality is frequent: (40%) Stage I: 67% of cases: Exophytic implants: hidden peritoneal spread? No impact on prognosis Micro-invasion Micropapillary pattern A. MAKAR Advanced stage: Serosal implants Invasive vs non invasive © 2008 Universitair Ziekenhuis Gent 9
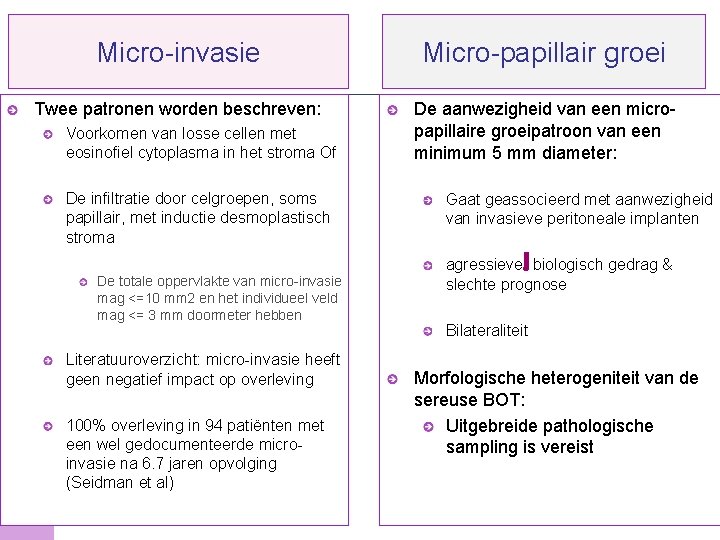
Micro-invasie Micro-papillair groei Twee patronen worden beschreven: De aanwezigheid van een micropapillaire groeipatroon van een minimum 5 mm diameter: Voorkomen van losse cellen met eosinofiel cytoplasma in het stroma Of De infiltratie door celgroepen, soms papillair, met inductie desmoplastisch stroma De totale oppervlakte van micro-invasie mag <=10 mm 2 en het individueel veld mag <= 3 mm doormeter hebben Literatuuroverzicht: micro-invasie heeft geen negatief impact op overleving 100% overleving in 94 patiënten met een wel gedocumenteerde microinvasie na 6. 7 jaren opvolging (Seidman et al) © 2008 Universitair Ziekenhuis Gent Gaat geassocieerd met aanwezigheid van invasieve peritoneale implanten agressiever biologisch gedrag & slechte prognose Bilateraliteit Morfologische heterogeniteit van de sereuse BOT: Uitgebreide pathologische sampling is vereist 10

Extra Ovarian Spread of Serous BOT: Stage II-III 35% peritoneal & omental implants True implantation metastases ? Multifocal in situ lesions of peritoneum ? Non-invasive vs invasive implants DD: Invasive implants vs endosalpingosis © 2008 Universitair Ziekenhuis Gent 11
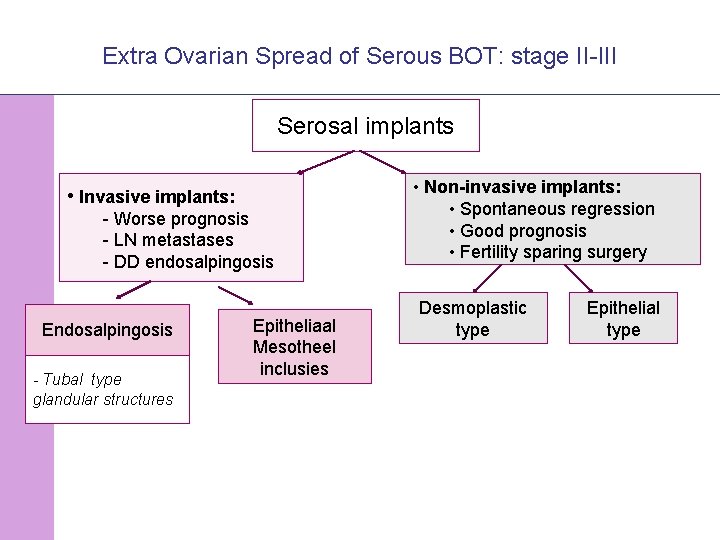
Extra Ovarian Spread of Serous BOT: stage II-III Serosal implants • Invasive implants: - Worse prognosis - LN metastases - DD endosalpingosis Endosalpingosis - Tubal type glandular structures © 2008 Universitair Ziekenhuis Gent Epitheliaal Mesotheel inclusies • Non-invasive implants: • Spontaneous regression • Good prognosis • Fertility sparing surgery Desmoplastic type Epithelial type 12

Prognosis of Serous BOT 10 y survival is related to FIGO stage Stage I: 99% survival Stage II - III: 60 -80% survival, depending on type of extra –ovarian (serosal) implants: Non-invasive implants: 93% survival Regression after removal of primary tumor Invasive implants: 60% survival Progression to invasive cancer Lymphatic metastases © 2008 Universitair Ziekenhuis Gent 13

II. Mucinous Borderline Tumors 50% of all borderline tumors Intestinal subtype (90%): Unilateral, multicystic, smooth capsule Pseudomyxoma peritonei Non intestinal subtype (10%): Bilateral 20 -30% Exophytic paucilocular, implants (sero-mucinous) FIGO stage I: 84% (67% serous tumors) 10 years survival FIGO stage I: 97% © 2008 Universitair Ziekenhuis Gent 14

Pseudomyxoma Peritonei Only with mucinous tumors of intestinal type Not related to pre or intraoperative rupture Often with pseudomyxoma ovarii Mucinous tumors of the appendix Influence on survival is unclear Primary surgical treatment: Repeated surgery & peritoneal stripping HIPEC © 2008 Universitair Ziekenhuis Gent 15

Norwegian Cancer Registery (1970 -1993): 2343 BOT Age adjusted 5 years survival ( 93%) Survival related to: FIGO stage (localized vs EO spread) Histologic type Residual disease after primary surgery Invasive peritoneal implants Age (<44 vs older) < 44 ys old: 5 y survival of 99% 75 -89 ys old: 5 y survival of 85% 45 -64 y: RR 4. 7 (CI: 2. 46 - 8. 99) 65 -74 y: RR 11. 09 (CI: 5. 84 – 21. 95) 75 -89 y: RR 34. 16 (CI: 18. 23 -64. 02) DNA ploidy state © 2008 Universitair Ziekenhuis Gent 16
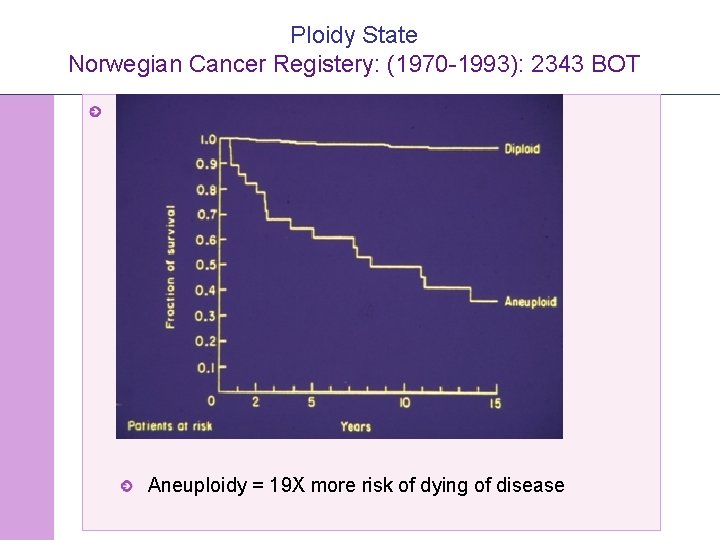
Ploidy State Norwegian Cancer Registery: (1970 -1993): 2343 BOT Kaern et al (1993): 370 tumors >10 y FU 90% diploid 10% aneuploid Aneuploidy = 19 X more risk of dying of disease © 2008 Universitair Ziekenhuis Gent 17

CA 125 in Borderline tumors. Makar et al. (1992 & 1993) Preoperative level lower than with invasive ovarian cancer (IOC): Borderline : 66 (5 -272) U/ml vs Invasive cancer: 327 (2 -125000) U/ml Grade 1: 68 U/ml Grade II: 221 U/ml Grade III: 490 U/ml Serous BOT: 131 vs 391 U/ml for IOC Mucinous BOT: 62 vs 49 U/ml for IOC CA 125 was elevated in only 15% BOT with disease recurrence vs 82% with IOC © 2008 Universitair Ziekenhuis Gent 18

BOT & Hormonal Receptor State Almost 100% positive ER and/or PR Invasive counterpart <10% positive hormonal receptors What is the place of hormonal therapy? © 2008 Universitair Ziekenhuis Gent 19

Patterns of Spread in BOT I. Transperitoneal © 2008 Universitair Ziekenhuis Gent 20

II. Lymphatic spread ? ? Not in case of mucinous BOT (intestinal) Serous BOT with: Extra-ovarian spread of invasive implants 19% (Camatte 2002) Aneuploid tumors True metastases? In situ transformation ? 2 ry Mullerian epith in LN? Endosalpingosis? No impact on prognosis © 2008 Universitair Ziekenhuis Gent 21

Borderline Tumors - Symptoms Accidental: Following cystectomy for asymptomatic adnexal mass Urinary symptoms Abdominal mass Less gasterointestinal symptoms compared with invasive tumors Torsion © 2008 Universitair Ziekenhuis Gent 22

© 2008 Universitair Ziekenhuis Gent 23

Frozen section DD: grade 1 vs BOT DD: benign cystadenoma vs BOT More difficult with mucinous than serous BOT A. MAKAR © 2008 Universitair Ziekenhuis Gent 24
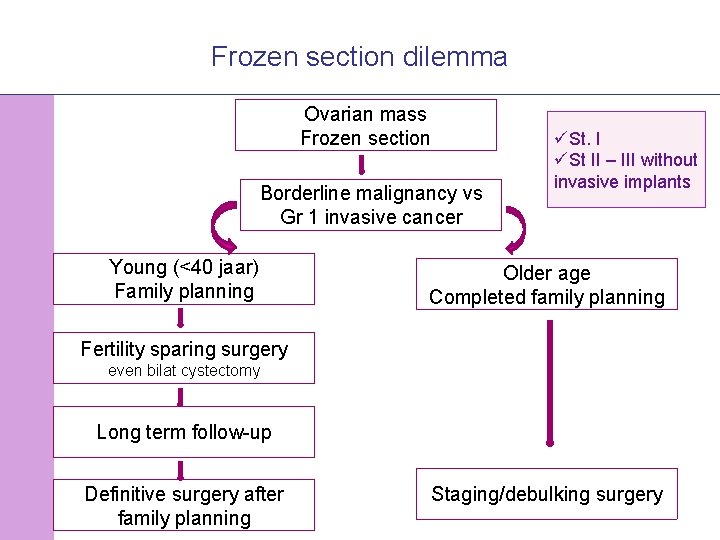
Frozen section dilemma Ovarian mass Frozen section Borderline malignancy vs Gr 1 invasive cancer Young (<40 jaar) Family planning üSt. I üSt II – III without invasive implants Older age Completed family planning Fertility sparing surgery even bilat cystectomy Long term follow-up Definitive surgery after family planning © 2008 Universitair Ziekenhuis Gent Staging/debulking surgery 25

Conservative Surgery Inspection & palpation Laparoscopic staging Cytologic washing More cyst rupture Incomplete No difference in OS Unilateral adnexectomy – cystectomy Omentectomy (10% relapse risk with serous tumors) Appendectomy (mucinous tumors) Biopsy contralateral ovary (serous tumors) ? Biopsy pelvic peritoneum Curettage (endometrioid tumors) © 2008 Universitair Ziekenhuis Gent 26

Conservative surgery & Contralateral Ovary Serous tumors: bilateral in 40% of cases Wedge resection ? Microscopic disease was rarely found in grossly normal ovary Tazelaar (1985): normal pathologic findings in wedge specimen did not exclude tumor Adhesions and mechanical sterility © 2008 Universitair Ziekenhuis Gent 27

Restaging Procedures Snider (1991), Hoskins (1995), Boccara (2004), Morice (2011): No upgrading in stage I mucinous tumors Multifocal appendicular tumor Upgrading in 12 -20% of serous tumors In case of cystectomy Omentectomy ( serous tumors) Per laparoscopy Restaging had no impact on recurrence rate © 2008 Universitair Ziekenhuis Gent 28

Cystectomy in case of bilateral tumors Cave mucinous tumors A. MAKAR © 2008 Universitair Ziekenhuis Gent 29
A. MAKAR © 2008 Universitair Ziekenhuis Gent 30

Conservative surgery -Cystectomy Even cystectomy with bilateral tumors Recurrence rate 15% in case of: positive resection margins or multifocality Risk invasive cancer with mucinous tumors Meticilous pathological examination of the resection margins Careful follow-up: survival is not affected if patients are reoperated at recurrence © 2008 Universitair Ziekenhuis Gent 31

Conservative surgery Close Long Term Follow-up Papadimitriou (1999): late recurrence in 70% of cases with stage I Makar (1993): CA 125 was elevated in only 15% at recurrence Vaginal sonography Removal of the remaining ADNEX following completion of family planning ? © 2008 Universitair Ziekenhuis Gent 32

Conservative Surgery in Stage II-III Camatte (2002 BJOG): Conservative surgery in 17 with stage II-III 14/17 with non invasive implants 6 spontaneous and 2 assisted pregnancies No deaths 2 recurrences (one with non invasive implant) Morice et al (2011) in literature review: Invasive implants is associated with >40% risk of recurrence, 2% death © 2008 Universitair Ziekenhuis Gent 33

Pregnancy following Conservative Surgery No difference in recurrence rate (5. 4% & 6. 9%) Maintenance of menstrual cycle in patients who received cisplatinum as adjuvant treatment Assisted fertility treatment: successful Patients who wished to procreate succeeded No higher incidence of miscarriages or dystocia No increased risk of foetal malformations © 2008 Universitair Ziekenhuis Gent 34
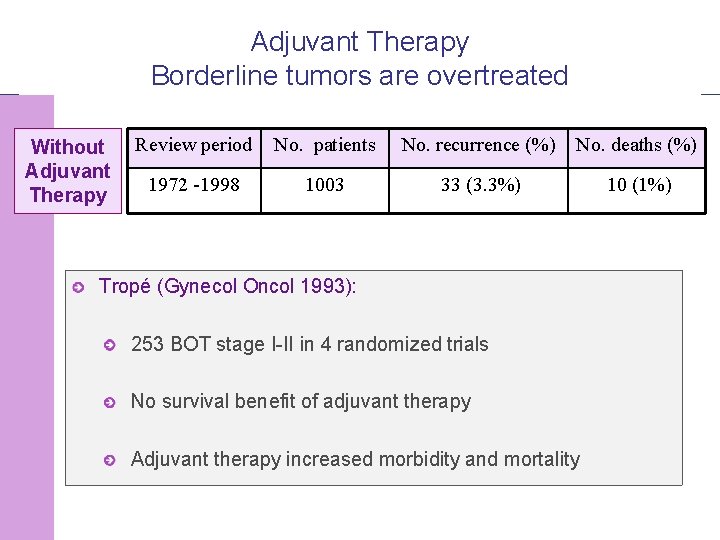

Adjuvant Therapy Borderline tumors are overtreated Without Adjuvant Therapy Review period No. patients No. recurrence (%) No. deaths (%) 1972 -1998 1003 33 (3. 3%) 10 (1%) Tropé (Gynecol Oncol 1993): 253 BOT stage I-II in 4 randomized trials No survival benefit of adjuvant therapy Adjuvant therapy increased morbidity and mortality © 2008 Universitair Ziekenhuis Gent 35
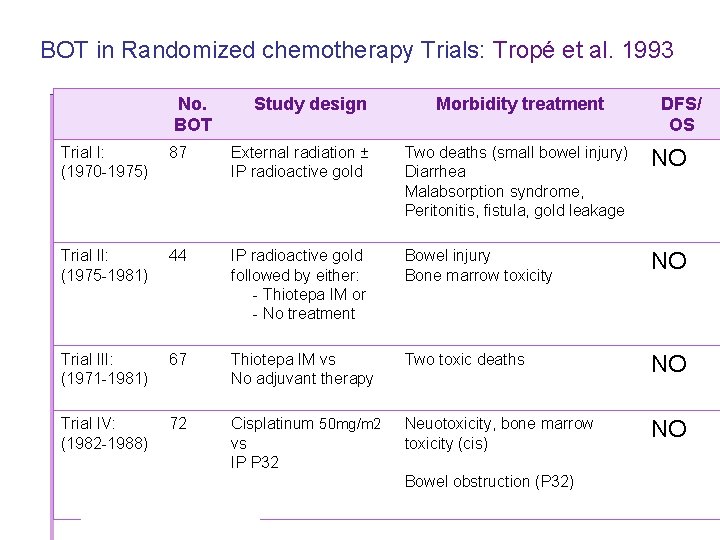
BOT in Randomized chemotherapy Trials: Tropé et al. 1993 No. BOT Study design Morbidity treatment DFS/ OS Trial I: (1970 -1975) 87 External radiation ± IP radioactive gold Two deaths (small bowel injury) Diarrhea Malabsorption syndrome, Peritonitis, fistula, gold leakage NO Trial II: (1975 -1981) 44 IP radioactive gold followed by either: - Thiotepa IM or - No treatment Bowel injury Bone marrow toxicity NO Trial III: (1971 -1981) 67 Thiotepa IM vs No adjuvant therapy Two toxic deaths NO Trial IV: (1982 -1988) 72 Cisplatinum 50 mg/m 2 vs IP P 32 Neuotoxicity, bone marrow toxicity (cis) NO Bowel obstruction (P 32) © 2008 Universitair Ziekenhuis Gent 36
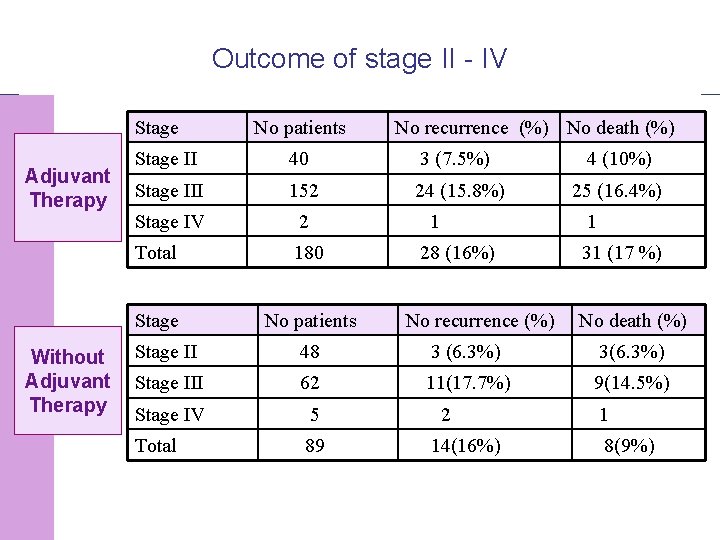
Outcome of stage II - IV Stage Adjuvant Therapy Without Adjuvant Therapy No patients No recurrence (%) No death (%) Stage II 40 3 (7. 5%) 4 (10%) Stage III 152 24 (15. 8%) 25 (16. 4%) Stage IV 2 Total 180 Stage No patients 1 1 28 (16%) No recurrence (%) 31 (17 %) No death (%) Stage II 48 3 (6. 3%) 3(6. 3%) Stage III 62 11(17. 7%) 9(14. 5%) Stage IV 5 Total 89 © 2008 Universitair Ziekenhuis Gent 2 14(16%) 1 8(9%) 37

Chemotherapy in Stage (II-III) ? ? Excellent survival without adjuvant therapy Low response rate (<15%) Increased morbidity Non-invasive implants: Good prognosis = no adjuvant therapy Conservative surgery in young patients Invasive implants: only progonostic factor is residual disease © 2008 Universitair Ziekenhuis Gent 38

© 2008 Universitair Ziekenhuis Gent 39

Conclusion-I Borderline Ovarian Tumors Mostly as stage I with excellent long term prognosis Women in reproductive age deserve conservative surgery Surgery is corner stone of treatment of advanced stages and in recurrence No place for adjuvant CT = overtreatment = mobidity/mortality Careful and long term follow-up CA 125 is of limited value in follow up © 2008 Universitair Ziekenhuis Gent 40
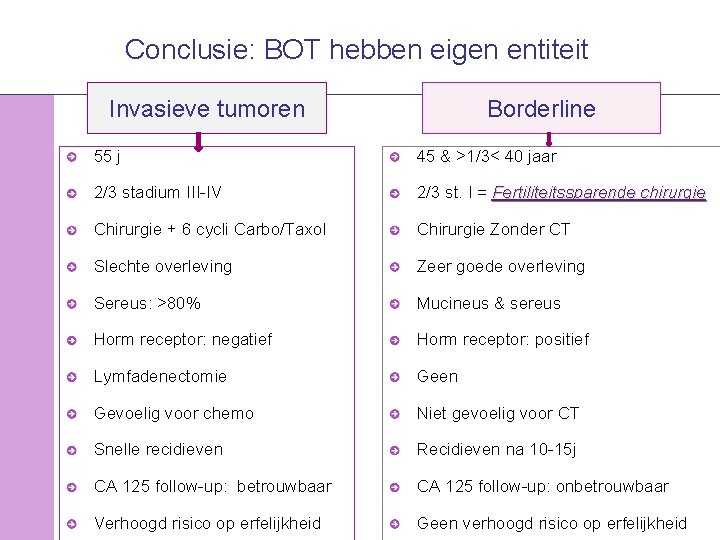
Conclusie: BOT hebben eigen entiteit Invasieve tumoren Borderline 55 j 45 & >1/3< 40 jaar 2/3 stadium III-IV 2/3 st. I = Fertiliteitssparende chirurgie Chirurgie + 6 cycli Carbo/Taxol Chirurgie Zonder CT Slechte overleving Zeer goede overleving Sereus: >80% Mucineus & sereus Horm receptor: negatief Horm receptor: positief Lymfadenectomie Geen Gevoelig voor chemo Niet gevoelig voor CT Snelle recidieven Recidieven na 10 -15 j CA 125 follow-up: betrouwbaar CA 125 follow-up: onbetrouwbaar © 2008 Universitair Ziekenhuis Gent Verhoogd risico op erfelijkheid Geen verhoogd risico op erfelijkheid 41

Stop georganiseerde moord op christenen in het Midden-Oosten © 2008 Universitair Ziekenhuis Gent 42

© 2008 Universitair Ziekenhuis Gent 43
- Slides: 43