Boot Camp Executive Summary Chiefs Topics Inpatient Diabetes

Boot Camp Executive Summary Chiefs

Topics • Inpatient Diabetes • AMS • Hypotension • Dyspnea • Cross Cover • Chest Pain • For more and details check out the night guide

• TIPS • MINDSET: No dumb pages. Take time to explain your thoughts if you have time or give them parameters for when to call you for certain complaints • Make sure to forward the pagers before or right after you receive sign out • Try and respond to pages in 15 minutes or less. Don’t need to interrupt patient care to return page • Triage your calls and let the nurse know when to expect a response or order • Delete pages once you have returned them • MOST IMPORTANTLY – communicate with your senior and never be scared to ask for help!

How can we cut down on Cross-Cover Pages? • Make sure PRN meds are in and nurse knows they’re there. • Provide a good sign out to your fellow intern and think ahead of what issues may come up with a patient • Ensure Nurse knows the plan. If you have time go to the floor and ask if there is anything anyone needs prior to sign out • Pay attention to CC signout on your team and make adjustments to prevent further issues.

Documentation • If a cross cover page warrants seeing the patient or if it results in a change of plan (blood cultures positive, etc) – write a BRIEF cross cover note • “Called by bedside RN regarding tachycardia. Patient asymptomatic. HR 126, BP 145/78. EKG with afib with RVR. Patient given metoprolol 5 mg IV with improvement in HR. Will continue to monitor on telemetry. ” • This is the ideal – there will be times when you are too busy to do this--Take notes on your sign out and make sure the day team knows about what you did overnight • Use your senior! They can help write cross cover notes if warranted

How do you call a Rapid Response/Code Blue? • ANYONE can call a rapid at any time. No matter what anyone says. If you need help or are uncomfortable you can call it • Call #3333 ( or operator), give them the room number • Can I just press the button on the wall? • That doesn’t go to the central system but will go to the HUC
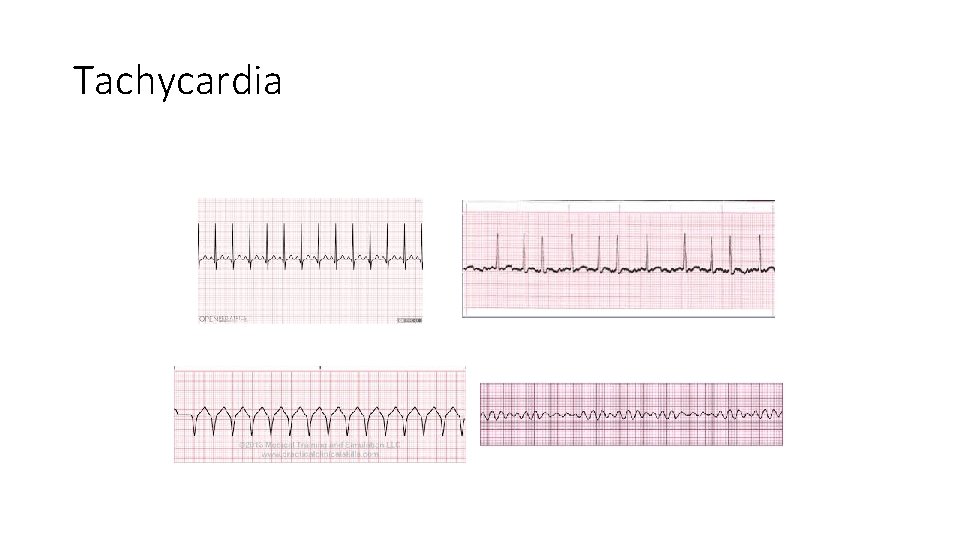
Tachycardia

Death Exam • You WILL be called for a death exam, usually will be an expected death for someone on Hospice • Take your senior with you the first time • If family is in the room, introduce yourself and explain you have been called to perform an exam, as there are signs that the patient has died (RN’s vitals, monitor, etc). Be sensitive to the needs of the family and allow them to stay • Exam: Auscultate precordial heart sounds (usually 30 seconds in each location), palpate carotid pulse, check pupils, check for response to pain • Inform the family that the patient has died and offer your condolences • Give the RN time of death • Document your death exam in the chart • Notify your Attending

Final Tips • Keep your senior informed of changes in status of your patients • If you are wondering if you should call your Attending, you probably should – they will only be upset if you DON'T call them when you should, not if you DO call them • Medical care occurs 24/7 and although you may not be the primary physician for the patient during the morning hours, you are the primary physician for them RIGHT NOW

Basal Bolus Insulin Coverage • Weight based total daily insulin • For a 100 kg individual using 0. 5 units/kg estimate: • Total daily insulin = 50 units • 50% long acting • 50% short acting • 33% with each meal • Choose correction scale per TDI • Insulin TDI <40 units: 0 -5 • Insulin TDI 40 -80 units: 0 -8 • Insulin TDI >80 units: 0 -12

What's our goal? • Inpatient glucose control goal = Goldie Locks • 140 -180 • NICE-SUGAR Trial (Normoglycemia in Intensive Care Evaluation-Survival Using Glucose Algorithm Regulation) 11
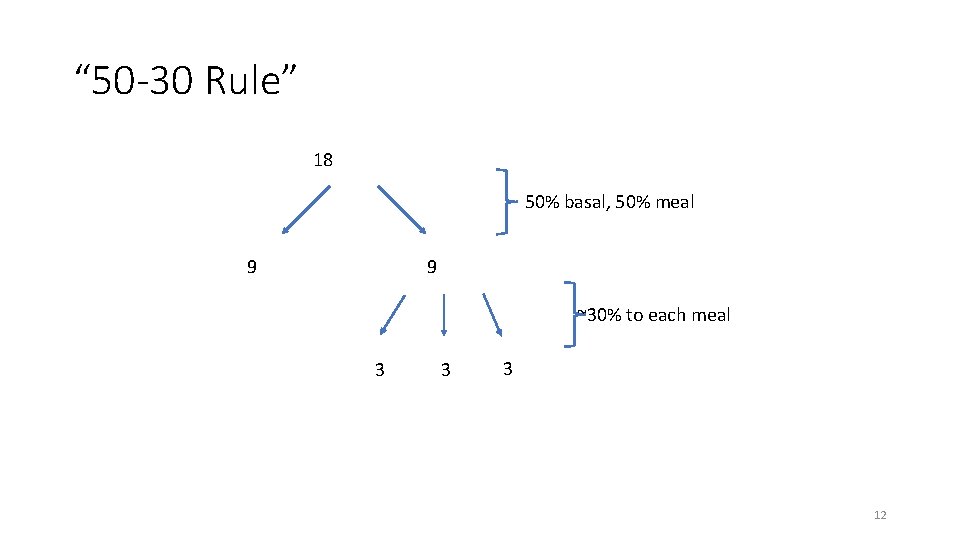
“ 50 -30 Rule” 18 50% basal, 50% meal 9 9 ~30% to each meal 3 3 3 12
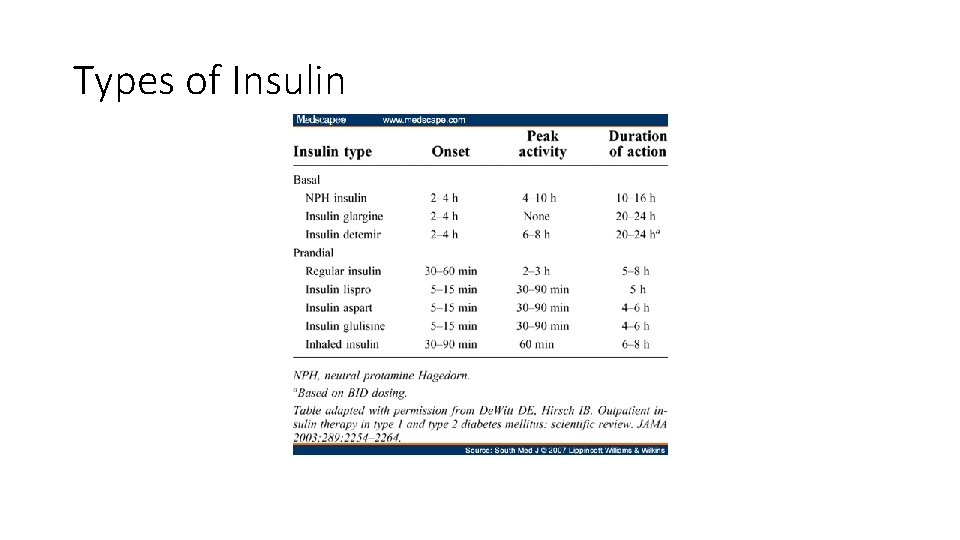
Types of Insulin

Hyperglycemic Hyperosmolar State vs. DKA • DKA • Insulin deficiency -> cortisol, glucagon and catecholamine release -> ketone generation from the liver -> acidosis • Very active monitoring of gap, potassium and acidosis, always have some form of insulin • HHS • Fluid deficiency, but will need insulin as well • Also needs close monitoring of electrolytes
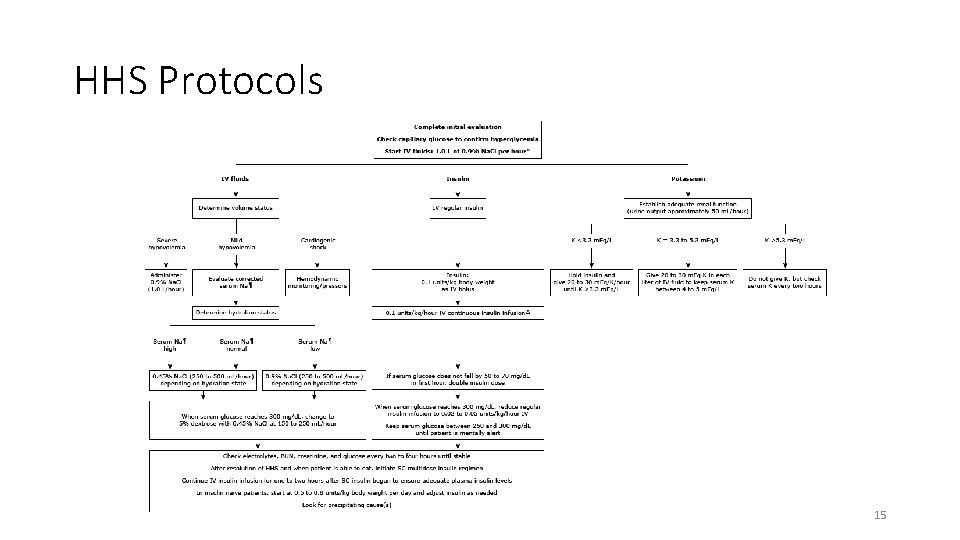
HHS Protocols 15
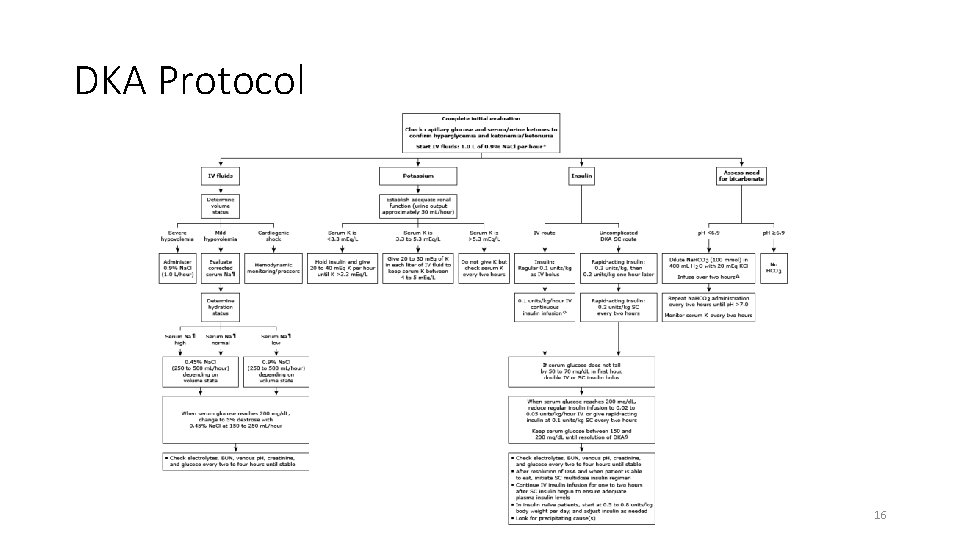
DKA Protocol 16

Important Concepts • Benign Hypoglycemia • DKA vs HHS

Altered Mental Status • Disorder of arousal • • Sleepy Not talking Unresponsive Obtunded • Disruption of cognitive function • Confused • Disoriented • Slurred speech

Ask follow up questions • - What seems different to you? • - When did the change start? (time course) • - What medications have they received recently? • - Was there any trauma? • - What do YOU think could have caused this? • - ALWAYS ask for a set of vitals

How do you evaluate? Helpful tests for ACUTE AMS: Et. OH Metabolic panel, ammonia CBC, UA, CXR, LP, blood cultures Head CT Blood glucose • UDS, serum osm, Medication levels (dig, anticonvulsant, lithium)

Few more thoughts on meds… • - Remember to check GFR and ensure all medications are appropriately dosed - What have we NOT given them? Are there any home meds we are holding? - Baclofen, SSRI, benzos

Ammonia Pearls • - Hyperammonemia is neither sensitive nor specific for the presence or degree of hepatic encephalopathy • - Ammonia can be helpful for evaluation of patients without known liver disease with acute mental status changes • Other causes for elevation? • Convulsive seizures, TPN, GI hemorrhage, steroids, portosystemic shunts, meds, urea cycle disorders


Types of Shock 1. Hypovolemic Shock = intravascular VOLUME problem 2. Cardiogenic Shock = PUMP problem 3. Distributive shock 4. Obstructive shock = VESSEL problem = PUMP problem Categorize each item in your differential into these buckets…

MAP= CO x SVR Types of Shock CO = HR x SV 1. Hypovolemic Shock 2. Cardiogenic Shock 3. Distributive shock 4. Obstructive shock PCWP CO SVR

Cardiogenic Shock o Muscle → pump failure due to MI, sepsis depressed myocardium, myocarditis o Rhythm → decreased filling due to tachycardia o Mechanical → valve defects (papillary muscle rupture), VSD/ASD→ pulm htn → Rt Ht failure, atrial myxoma, LV wall rupture after MI • Extracardiac (Obstructive) →PE, constrictive pericarditis, tamponade, tension PTX 1. Preload 2. Afterload 3. Contractility

3 categories for how a patient looks… Awake Distressed Vitals & exam Access IVF? Diagnostic studies Level of Care Reassess Then check and look for an etiology Check the chart -BP over last 24 h -I’s and O’s -recent meds given Reassess Non-Responsive Rapid response Vitals & exam Access Fingerstick IVF? Diagnostic studies likely at the next level of care

Dyspnea DDx • Cardiac • • Heart Failure MI Tamponade Arrhythmia • Hematologic: • • Pulmonary Embolus Acute Chest Syndrome Anemia CO poisoning • Pulmonary • Obstructive • COPD, Asthma, Bronchospasm • Anaphylaxis • Mechanical • Pneumothorax, Hemothorax • Pleural effusion • Interstitial: • Infectious: Pneumonia • Cardiogenic: Pulmonary edema • Non-cardiogenic pulmonary edema (ARDS, TRALI) • Neurologic: • NM failure: GBS, MG

ABG vs VBG and ABG closely approximate in p. H, lactate, bicarbonate. • PCO 2: correlation between the arterial and venous p. CO 2, but the confidence intervals are large • PO 2: does not correlate Take home 1. Hypoxemic patients get an ABG 2. VBG can be used for p. H, screening for hypercapnia
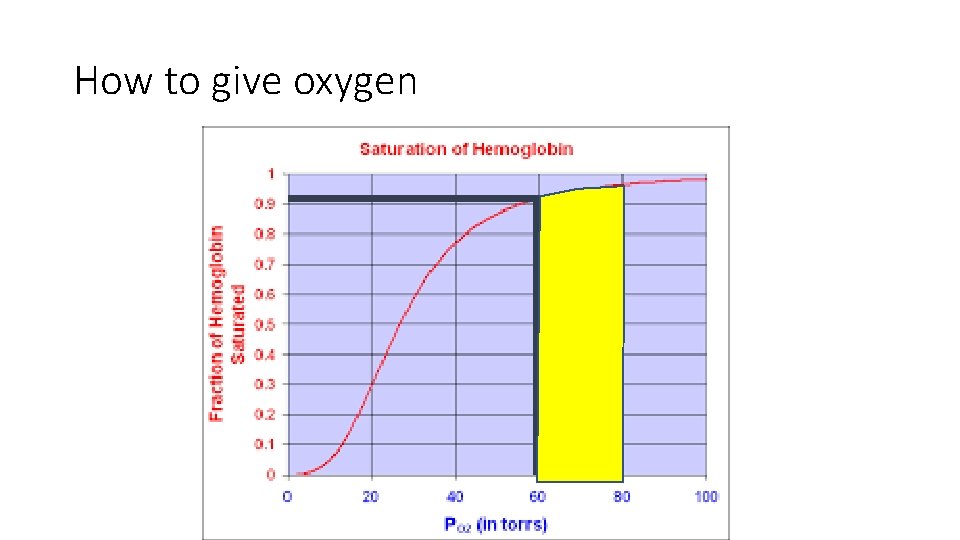
How to give oxygen
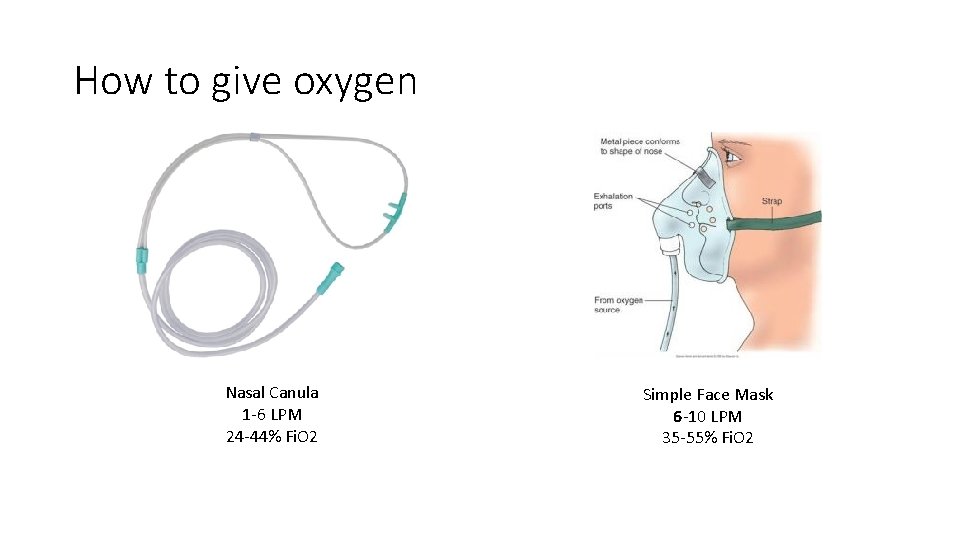
How to give oxygen Nasal Canula 1 -6 LPM 24 -44% Fi. O 2 Simple Face Mask 6 -10 LPM 35 -55% Fi. O 2
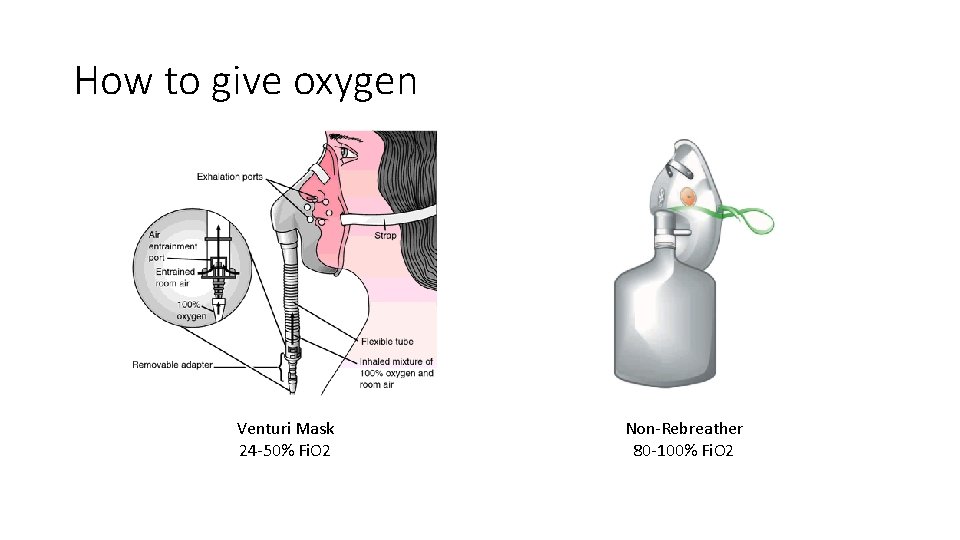
How to give oxygen Venturi Mask 24 -50% Fi. O 2 Non-Rebreather 80 -100% Fi. O 2
Key points • Do these devices help with ventilation? • NO! • A word about NIPPV on the next slide • IF you are increasing the Fi. O 2, you need to understand why! • • • Shunt: perfusion w/o ventilaton (HF, PNA) Dead Space: ventilation w/o perfusion (PE, PTX) Ventilatory failure Worsening clinical status Sleep apnea

NIPPV • Must be used appropriately • Conditions known to respond: • COPD exacerbations with hypercapnia • Cardiogenic pulmonary edema • Repeat ABG in 1 -2 hours predicts success • HACOR score • Heart rate, Acidosis (p. H), Consciousness (GCS), Oxygenation, and Respiratory rate (HACOR)

NIPPV Contraindications • Not able to cooperate, protect airway, or clear secretions • Not able to remove mask • HIGH aspiration risk • Never in restraints • Facial deformity that prevents proper fitting • Anticipate prolonged duration of positive pressure

Quick quiz • What are 3 initial things you should ask for on a patient with dyspnea? • Vital Signs, Chest x-ray, Blood Gas, EKG • What should your goal Pa. O 2 be on a arterial blood gas? • 60 -80 • What is the dose and route of epinephrine for anaphylaxis? • 1: 1000 0. 3 to 0. 5 mg IM • What should you always think in a sickle cell patient with dyspnea? • Acute Chest

Quick quiz • What is the Fi. O 2 for a nasal cannula? For a non-rebreather? • 24 -44% • 80 -100% • What are the contraindications to NIPPV? • Inappropriate mental status, high aspiration risk, prolonged need for positive pressure, failure to improve, inability to closely monitor • What are 2 indications for NIPPV? • COPD exacerbation, cardiogenic pulmonary edema

Life-threatening causes of chest pain • Acute Coronary Syndrome • Pulmonary Embolus • Aortic Dissection • Esophageal Rupture • Pneumothorax • Pericarditis with cardiac tamponade

Differentiating Cardiac from Noncardiac Favor ischemia Favor Noniscemia • Character: -squeezing, burning, heaviness • Location: -substernal, across mid-thorax, radiation to arm/ neck • Provocative Factors: exercise, stress/excitement • Duration: minutes • Character: sharp, stabbing • Location: localized with one finger, back pain suggesting dissection • Provocative Factors: relieved by exercise, by specific body motion • Duration: seconds, hours w/o + troponin
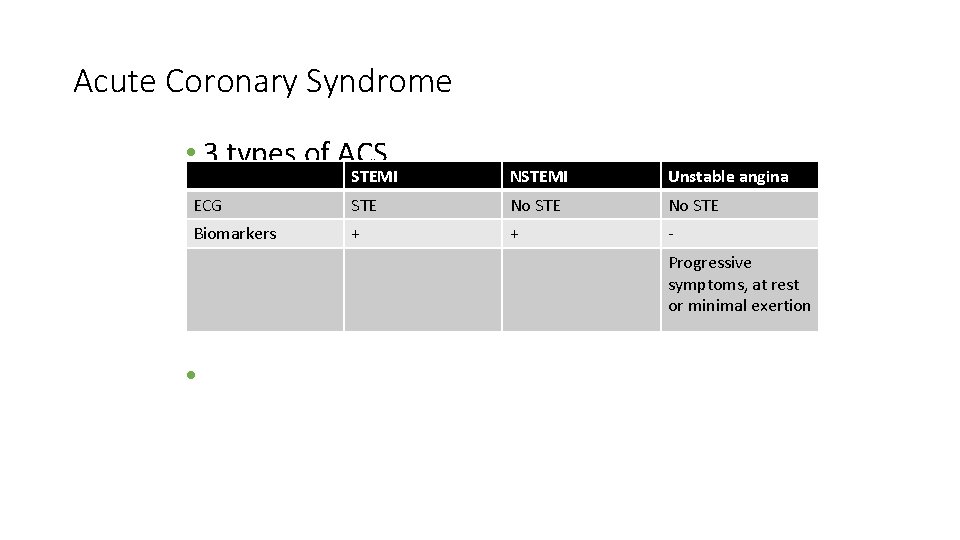
Acute Coronary Syndrome • 3 types of ACS STEMI NSTEMI Unstable angina ECG STE No STE Biomarkers + + Progressive symptoms, at rest or minimal exertion • Importance of serial EKG monitoring: sensitivity of single EKG is only 50% sensitive for acute MI
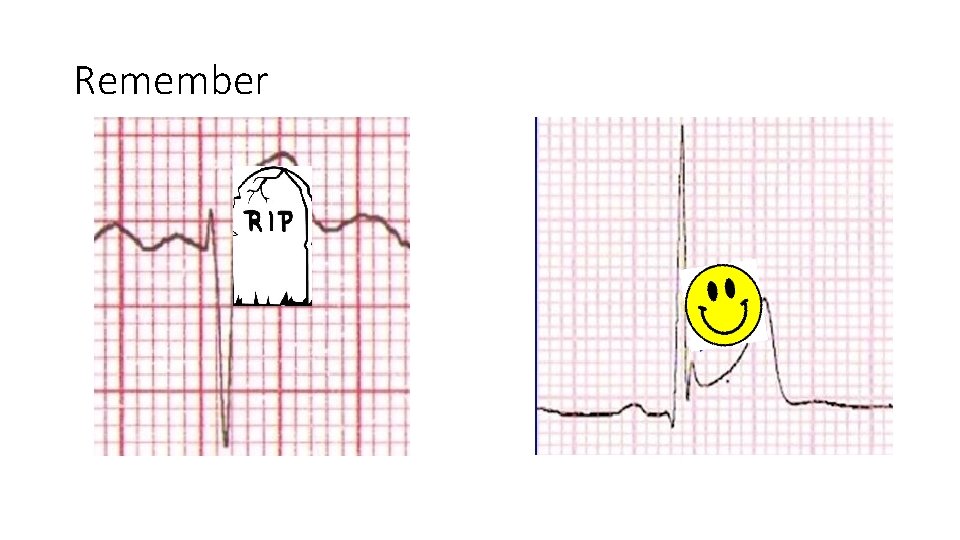
Remember

Medical Management of UA/NSTEMI • ASA 325 mg chewed or crushed • 80 mg PO atorvastatin • Antiplatelet therapy with P 2 Y 12 receptor blocker (clopidogrel, prasugrel, or ticagrelor) • Beta-blocker, without contraindications • Heparin gtt, without contraindications • Nitrates for relief of ischemic symptoms • Supplemental O 2 if Sa. O 2 </= 90%

Aortic Dissection Initial management A (Debakey I, II) • Surgery! • Do not delay surgery, even for LHC • Beta blockers, titrate to HR 50 -60 (labetalol, esmolol) • BP control- add nitroprusside or similar agent to SBP goal 100120 mm. Hg B (Debakey III) • Beta blockers, titrate to HR 50 -60 (labetalol, esmolol) • BP control • Surgery for those with end organ damage or those who do not respond to medical therapy

Pneumothorax Management • • 100% O 2 and observation in stable patients for PTX < 3 cm in size Needle aspiration in stable patients for PTX >3 cm Chest tube placement if PTX >3 cm and if needle aspiration fails Chest tube placement in unstable patients • Tension Pneumothorax – • 14 G angiocath into 2 nd intercostal space in midclavicular line • • Perpendicular to skin with syringe of saline attached Insert over suprior margin of rib, aspirate while inserting Once breached, advance cannula, allow decompression now patient needs a chest tube
- Slides: 44