Bones and Skeletal Tissues PART A Skeletal Cartilage

Bones and Skeletal Tissues PART A

Skeletal Cartilage Contains no blood vessels or nerves ¡ Surrounded by the perichondrium (dense irregular connective tissue) that resists outward expansion ¡ Three types – hyaline, elastic, and fibrocartilage ¡

Hyaline Cartilage Provides support, flexibility, and resilience ¡ Is the most abundant skeletal cartilage ¡ Is present in these cartilages: l Articular – covers the ends of long bones l Costal – connects the ribs to the sternum l Respiratory – makes up larynx, reinforces air passages l Nasal – supports the nose ¡

Elastic Cartilage Similar to hyaline cartilage, but contains elastic fibers ¡ Found in the external ear and the epiglottis ¡

Fibrocartilage Highly compressed with great tensile strength ¡ Contains collagen fibers ¡ Found in menisci of the knee and in intervertebral discs ¡

Growth of Cartilage Appositional – cells in the perichondrium secrete matrix against the external face of existing cartilage ¡ Interstitial – lacunae-bound chondrocytes inside the cartilage divide and secrete new matrix, expanding the cartilage from within ¡ Calcification of cartilage occurs l During normal bone growth l During old age ¡
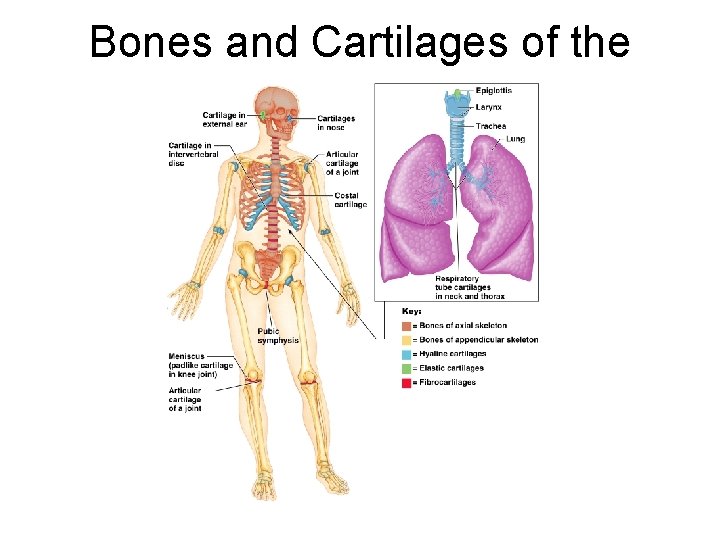
Bones and Cartilages of the Human Body

Classification of Bones Axial skeleton – bones of the skull, vertebral column, and rib cage ¡ Appendicular skeleton – bones of the upper and lower limbs, shoulder, and hip ¡
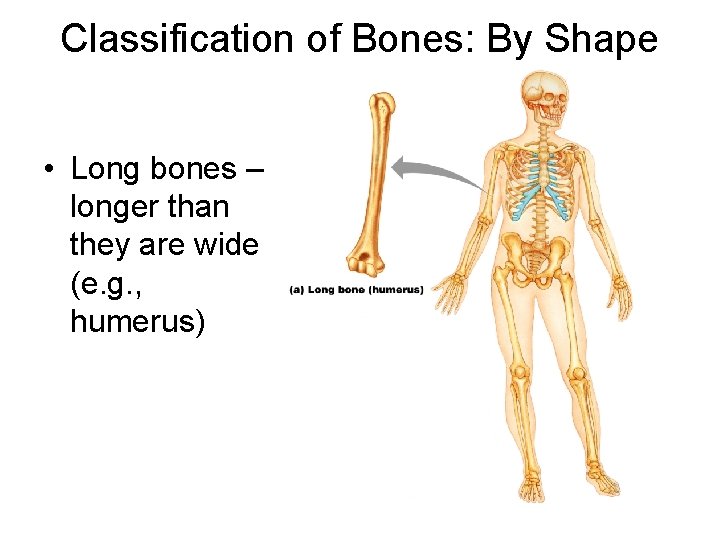
Classification of Bones: By Shape • Long bones – longer than they are wide (e. g. , humerus)
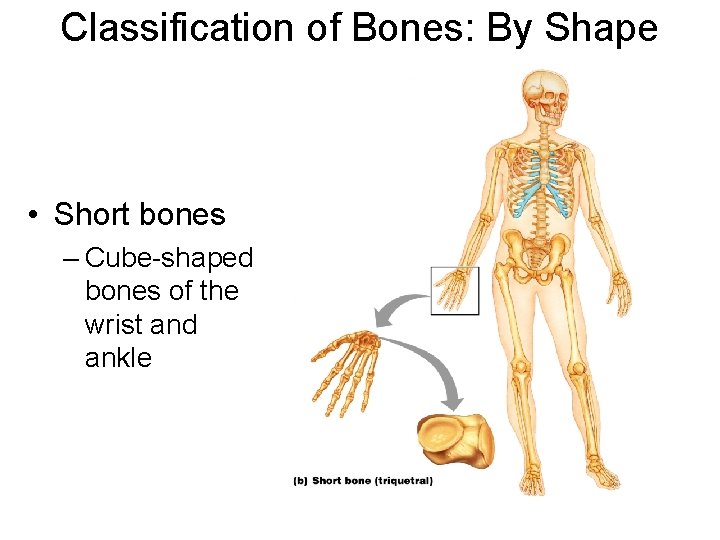
Classification of Bones: By Shape • Short bones – Cube-shaped bones of the wrist and ankle
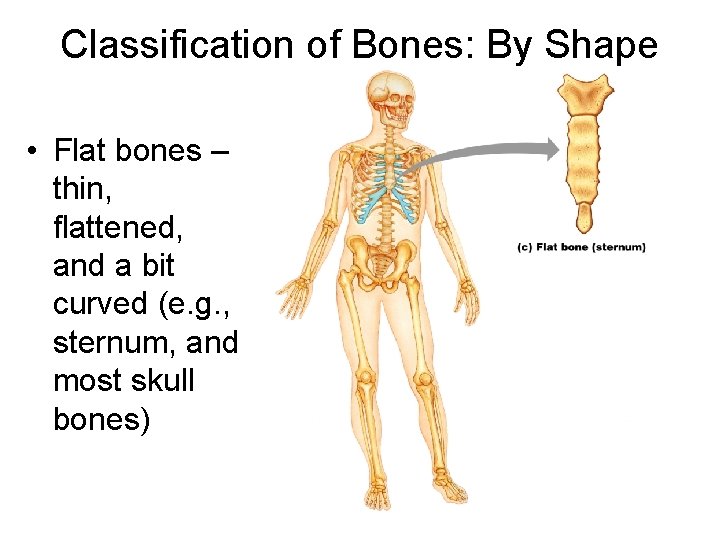
Classification of Bones: By Shape • Flat bones – thin, flattened, and a bit curved (e. g. , sternum, and most skull bones)
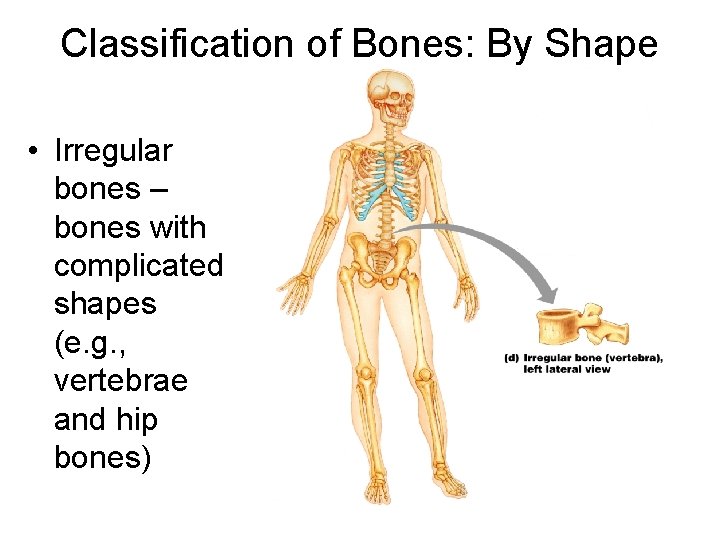
Classification of Bones: By Shape • Irregular bones – bones with complicated shapes (e. g. , vertebrae and hip bones)

Classification of bones by shape ¡ Sesamoid bones l Short bones located in a tendon ¡ Patella

Function of Bones Support – form the framework that supports the body and cradles soft organs ¡ Protection – provide a protective case for the brain, spinal cord, and vital organs ¡ Movement – provide levers for muscles ¡

Function of Bones Mineral storage – reservoir for minerals, especially calcium and phosphorus ¡ Blood cell formation – hematopoiesis occurs within the marrow cavities of bones ¡

Bone Markings ¡ Bulges, depressions, and holes that serve as: l Sites of attachment for muscles, ligaments, and tendons l Joint surfaces l Conduits for blood vessels and nerves

Projections – Sites of Muscle and Ligament Attachment Tubercle – small rounded projection ¡ Tuberosity – rounded projection ¡ Trochanter – large, blunt, irregular surface ¡ Crest – narrow, prominent ridge of bone ¡ Line – narrow ridge of bone ¡

Projections – Sites of Muscle and Ligament Attachment Epicondyle – raised area above a condyle ¡ Spine – sharp, slender projection ¡ Process – any bony prominence ¡

Projections That Help to Form Joints Head – bony expansion carried on a narrow neck ¡ Facet – smooth, nearly flat articular surface ¡ Condyle – rounded articular projection ¡ Ramus – armlike bar of bone ¡

Bone Markings: Depressions and Openings Meatus – canal-like passageway ¡ Sinus – cavity within a bone ¡ Fossa – shallow, basin-like depression ¡ Groove – furrow ¡ Fissure – narrow, slit-like opening ¡ Foramen – round or oval opening through a bone ¡

Gross Anatomy of Bones: Bone Textures Compact bone – dense outer layer ¡ Spongy bone – honeycomb of trabeculae filled with yellow bone marrow ¡

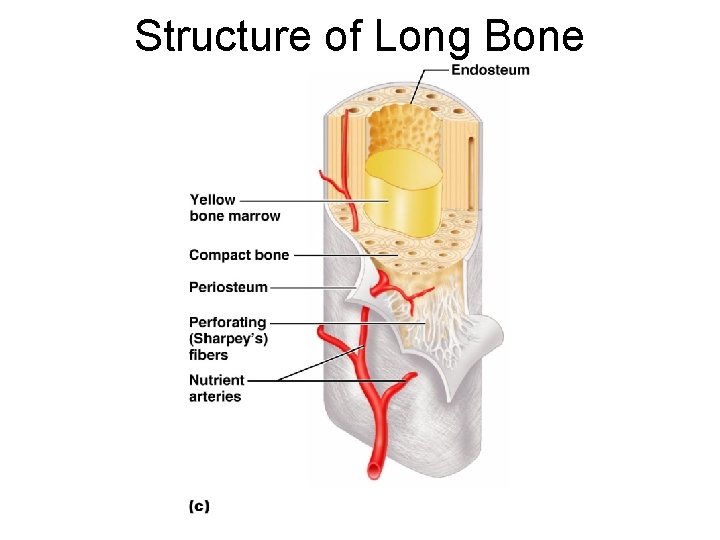
Structure of Long Bone ¡ Diaphysis l Tubular shaft that forms the axis of long bones l Composed of compact bone that surrounds the medullary cavity l Yellow bone marrow (fat) is contained in the medullary cavity

Structure of Long Bone ¡ Epiphyses l Expanded ends of long bones: distal and proximal l Exterior is compact bone, and the interior is spongy bone l Joint surface is covered with articular (hyaline) cartilage l Epiphyseal line separates the diaphysis from the epiphyses (metaphisis)
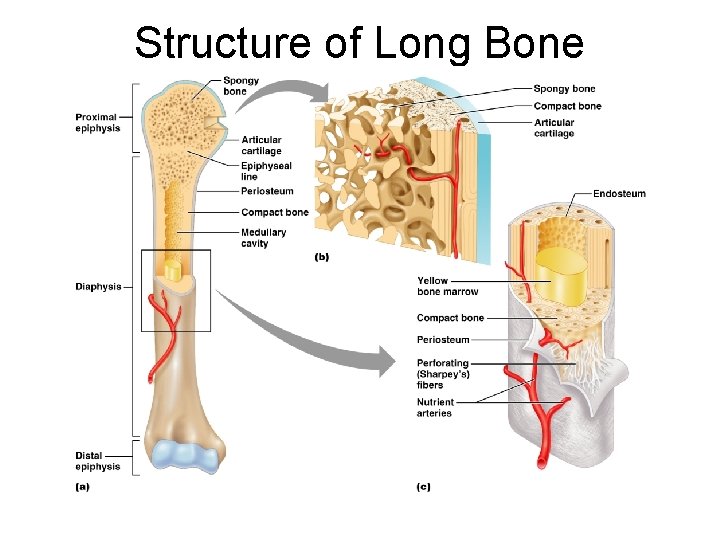
Structure of Long Bone
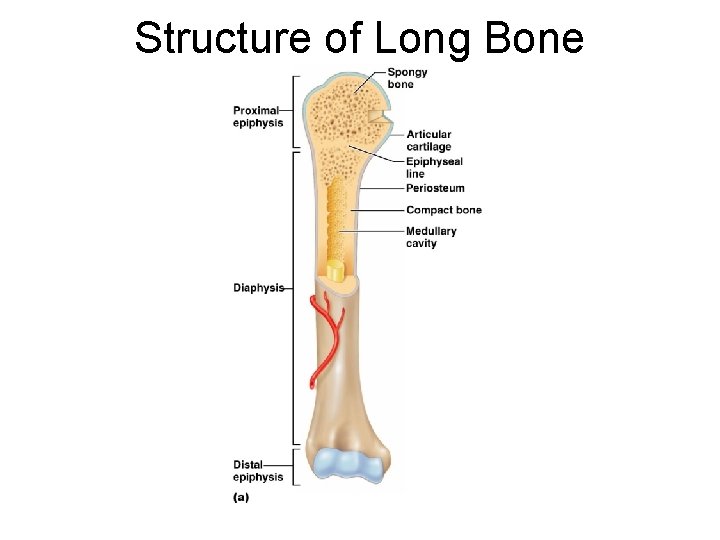
Structure of Long Bone
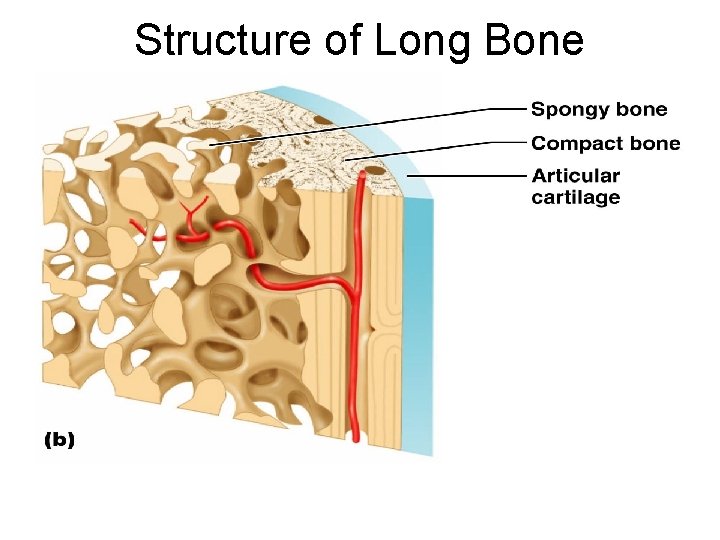
Structure of Long Bone
Structure of Long Bone

Bone Membranes ¡ Periosteum – double-layered protective membrane l Outer fibrous layer is dense regular connective tissue l Inner osteogenic layer is composed of osteoblasts and osteoclasts l Richly supplied with nerve fibers, blood, and lymphatic vessels, which enter the bone via nutrient foramina

Bone Membranes Secured to underlying bone by Sharpey’s fibers ¡ Endosteum – delicate membrane covering internal surfaces of bone l It contains osteoclasts and osteoblasts l

Structure of Short, Irregular, and Flat Bones Thin plates of periosteum-covered compact bone on the outside with endosteum-covered spongy bone (diploë) on the inside ¡ Have no diaphysis or epiphyses ¡ Contain bone marrow between the trabeculae ¡
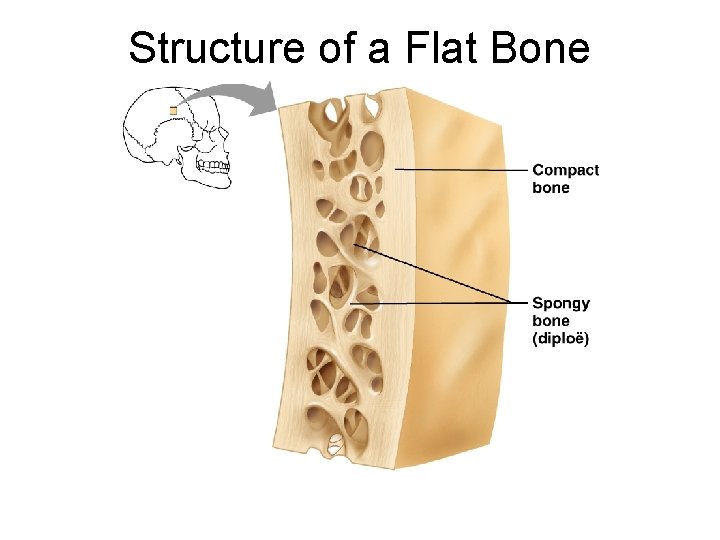
Structure of a Flat Bone

Location of Hematopoietic Tissue (Red Marrow) In infants l Found in the medullary cavity and all areas of spongy bone ¡ In adults l Found in the diploë of flat bones, and the head of the femur and humerus ¡

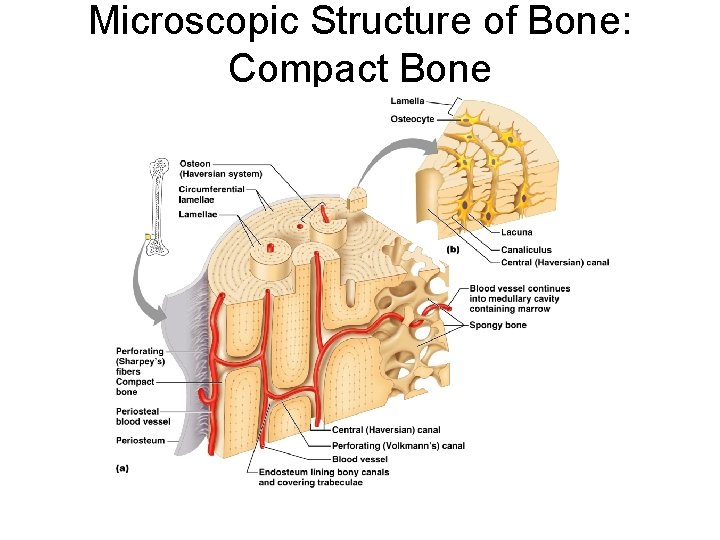
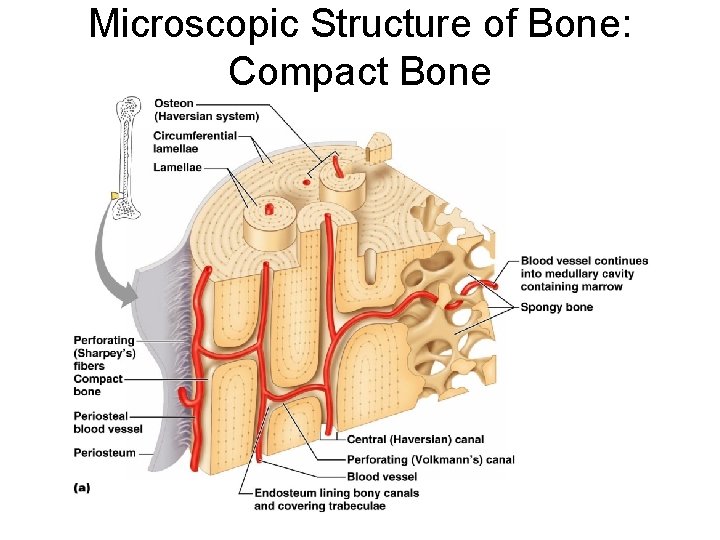
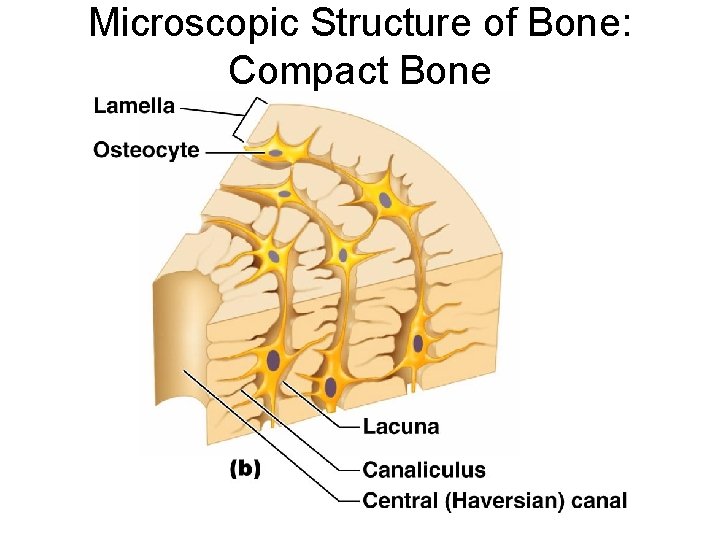
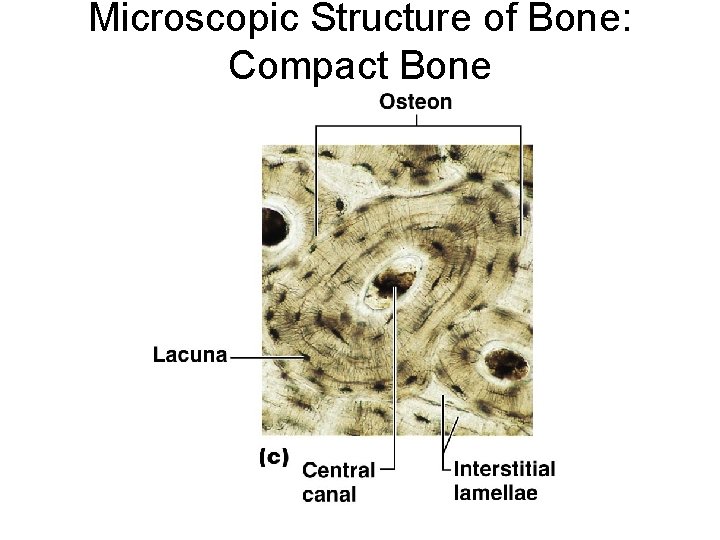
Microscopic Structure of Bone: Compact Bone ¡ Haversian system, or osteon – the structural unit of compact bone l Lamella – weight-bearing, column-like matrix tubes composed mainly of collagen. Concentric, circumferential, interstitial l Haversian, or central canal – central channel containing blood vessels and nerves

Microscopic Structure of Bone: Compact Bone ¡ Volkmann’s canals – channels lying at right angles to the central canal, connecting blood and nerve supply of the periosteum to that of the Haversian canal

Microscopic Structure of Bone: Compact Bone Osteocytes – mature bone cells ¡ Lacunae – small cavities in bone that contain osteocytes ¡ Canaliculi – hairlike canals that connect lacunae to each other and the central canal ¡
Microscopic Structure of Bone: Compact Bone
Microscopic Structure of Bone: Compact Bone
Microscopic Structure of Bone: Compact Bone
Microscopic Structure of Bone: Compact Bone

Chemical Composition of Bone: Organic Osteoblasts – bone-forming cells ¡ Osteocytes – mature bone cells ¡ Osteoclasts – large cells that resorb or break down bone matrix ¡ Osteoid – unmineralized bone matrix composed of proteoglycans, glycoproteins, and collagen ¡

Chemical Composition of Bone: Inorganic ¡ Hydroxyapatites, or mineral salts l Sixty-five percent of bone by mass l Mainly calcium phosphates l Responsible for bone hardness and its resistance to compression
Bone Development Osteogenesis (ossification) – the process of bone tissue formation l The formation of the bony skeleton in embryos l Bone growth until early adulthood l Bone thickness, remodeling, and repair ¡ Calcification ¡
Formation of the Bony Skeleton Begins at week 8 of embryo development ¡ Intramembranous ossification – bone develops from a fibrous membrane ¡ Endochondral ossification – bone forms by replacing hyaline cartilage ¡

Intramembranous Ossification Formation of most of the flat bones of the skull and the clavicles ¡ Fibrous connective tissue membranes are formed by mesenchymal cells ¡
Stages of Intramembranous Ossification An ossification center appears in the fibrous connective tissue membrane ¡ Bone matrix is secreted within the fibrous membrane ¡ Woven bone and periosteum form ¡ Bone collar of compact bone forms, and red marrow appears ¡
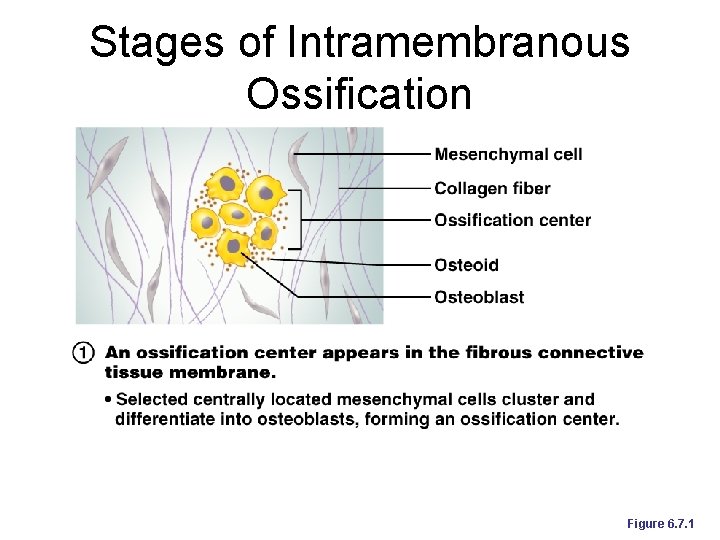
Stages of Intramembranous Ossification Figure 6. 7. 1
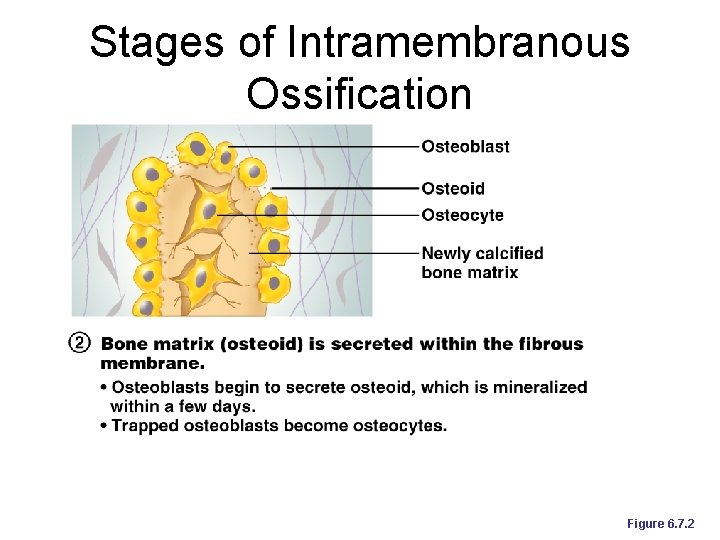
Stages of Intramembranous Ossification Figure 6. 7. 2
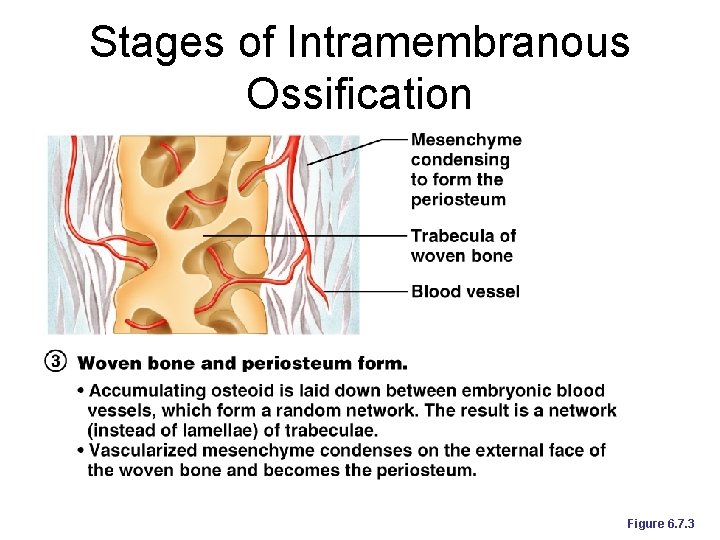
Stages of Intramembranous Ossification Figure 6. 7. 3
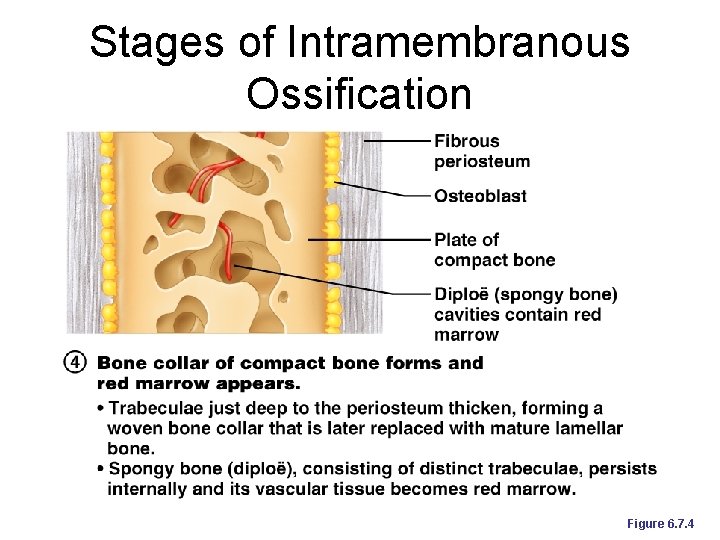
Stages of Intramembranous Ossification Figure 6. 7. 4

Bones and Skeletal Tissues PART B

Endochondral Ossification Begins in the second month of development ¡ Uses hyaline cartilage “bones” as models for bone construction ¡ Requires breakdown of hyaline cartilage prior to ossification ¡
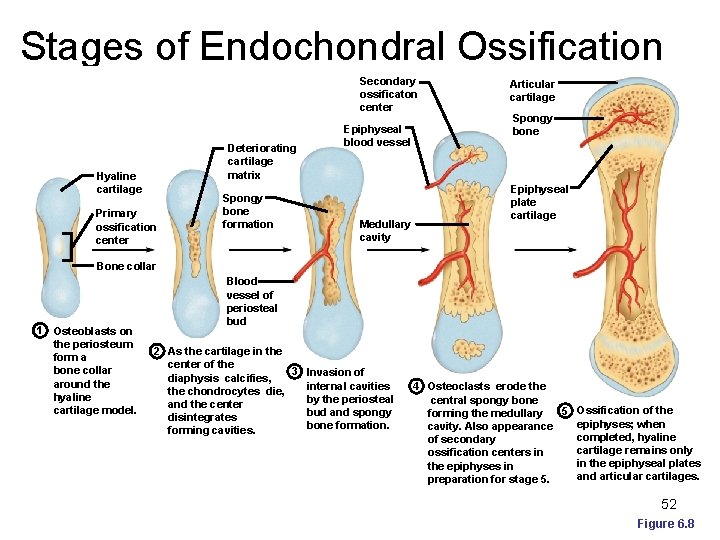
Stages of Endochondral Ossification Secondary ossificaton center Deteriorating cartilage matrix Hyaline cartilage Primary ossification center Spongy bone formation Epiphyseal blood vessel Medullary cavity Articular cartilage Spongy bone Epiphyseal plate cartilage Bone collar 1 Osteoblasts on the periosteum form a bone collar around the hyaline cartilage model. Blood vessel of periosteal bud 2 As the cartilage in the center of the 3 Invasion of diaphysis calcifies, internal cavities the chondrocytes die, by the periosteal and the center bud and spongy disintegrates bone formation. forming cavities. 4 Osteoclasts erode the central spongy bone 5 Ossification of the forming the medullary epiphyses; when cavity. Also appearance completed, hyaline of secondary cartilage remains only ossification centers in in the epiphyseal plates the epiphyses in and articular cartilages. preparation for stage 5. 52 Figure 6. 8

Postnatal Bone Growth in Length The epiphyseal plate consist of hyaline cartilage in the middle, with a transitional zone on each side ¡ Metaphysis l The transitional zone facing the marrow cavity ¡

Functional Zones in Long Bone Growth Resting zone l Facing the epiphysis l Zone of inactive cartilage ¡ Proliferation zone l Chondrocytes multiplying and lining up in rows l Epiphysis is pushed away from the diaphysis ¡

Functional Zones in Long Bone Growth ¡ Hypertrophic zone l Cessation of mitosis l Enlargement of chondrocytes l Enlargement of lacunae

Functional Zones in Long Bone Growth Calcification zone l Calcification of the matrix l Death and deterioration of chondrocytes ¡ Osteogenic zone l Bone deposition by osteoblasts l Formation of the trabeculae of the spongy bone ¡
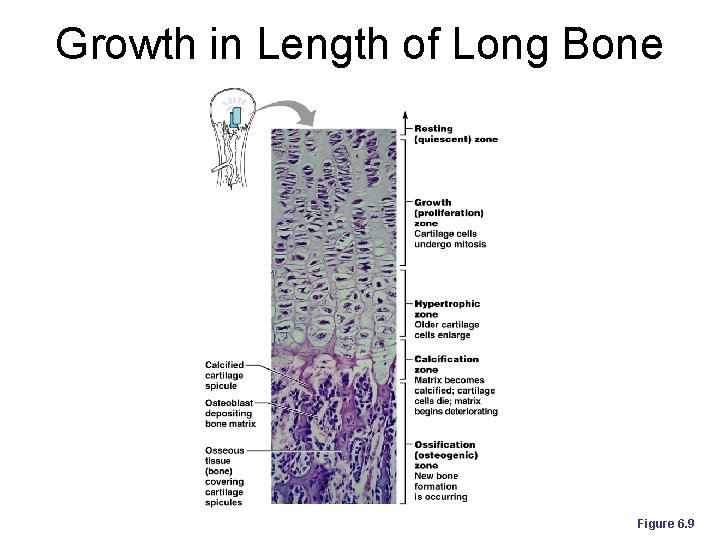
Growth in Length of Long Bone Figure 6. 9

Long Bone Growth and Remodeling ¡ Growth in length l During growth the epiphyseal plate maintain a constant thickness l Growth on the epiphysis side is balanced by bone deposition on the diaphysis side l Interstitial growth
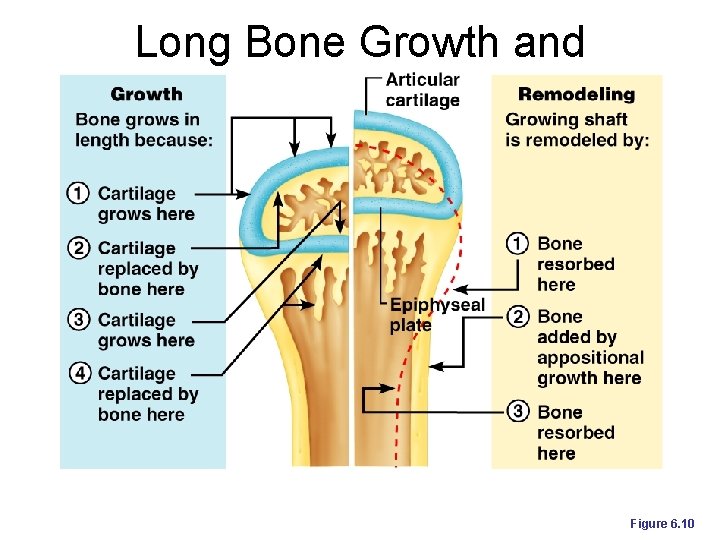
Long Bone Growth and Remodeling Figure 6. 10

Hormonal Regulation of Bone Growth During Youth ¡ During infancy and childhood, epiphyseal plate activity is stimulated by growth hormone

Hormonal Regulation of Bone Growth During Youth ¡ During puberty, testosterone and estrogens: l Initially promote adolescent growth spurts l Cause masculinization and feminization of specific parts of the skeleton l Later induce epiphyseal plate closure, ending longitudinal bone growth

Bone Growth in Width It is by appositional growth ¡ Osteoblasts in the inner layer of the periosteum deposit osteoid ¡ Osteoid calcifies ¡ Osteoblasts become osteocytes ¡ Circumferential lamellae is formed ¡ Osteoclasts of the endosteal layer resorb bone tissue to keep its proportion ¡

Bone Remodeling Also by appositional growth ¡ Remodeling units – adjacent osteoblasts deposit bone at periosteal surfaces and osteoclasts resorb bone at endosteal side ¡

Bone Remodeling Deposition ¡ Occurs also where bone is injured or added strength is needed ¡ Requires a diet rich in protein, vitamins C, D, and A, calcium, phosphorus, magnesium, and manganese ¡ Alkaline phosphatase is essential for mineralization of bone ¡

Bone Remodeling ¡ Sites of new matrix deposition are revealed by the: l Osteoid seam – unmineralized band of bone matrix l Calcification front – abrupt transition zone between the osteoid seam and the older mineralized bone

Bone Remodeling Resorption ¡ Accomplished by osteoclasts l Lysosomal enzymes digest organic matrix l Hydrochloric acid convert calcium salts into soluble forms l Resorption bays – grooves formed by osteoclasts as they break down bone matrix ¡

Bone Remodeling ¡ Dissolved matrix is transcytosed across the osteoclast’s cell where it is secreted into the interstitial fluid and then into the blood

Importance of Ionic Calcium in the Body ¡ Calcium is necessary for: l Transmission of nerve impulses l Muscle contraction l Blood coagulation l Secretion by glands and nerve cells l Cell division

Control of Remodeling ¡ Two control loops regulate bone remodeling l Hormonal mechanism maintains calcium homeostasis in the blood l Mechanical and gravitational forces acting on the skeleton

Response to Mechanical Stress Wolff’s law – a bone grows or remodels in response to the forces or demands placed upon it ¡ Observations supporting Wolff’s law include l Long bones are thickest midway along the shaft (where bending stress is greatest) l Curved bones are thickest where they are most likely to buckle 70 ¡

Response to Mechanical Stress Trabeculae form along lines of stress ¡ Large, bony projections occur where heavy, active muscles attach ¡
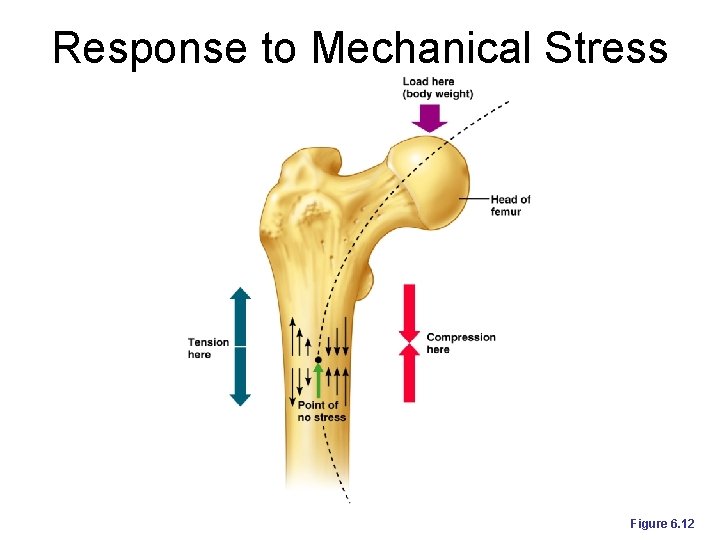
Response to Mechanical Stress Figure 6. 12

Bone Fractures (Breaks) ¡ Bone fractures are classified by: l The position of the bone ends after fracture l The completeness of the break l The orientation of the bone to the long axis l Whether or not the bones ends penetrate the skin

Types of Bone Fractures Nondisplaced – bone ends retain their normal position ¡ Displaced – bone ends are out of normal alignment ¡

Types of Bone Fractures Complete – bone is broken all the way through ¡ Incomplete – bone is not broken all the way through ¡ Linear – the fracture is parallel to the long axis of the bone ¡

Types of Bone Fractures Transverse – the fracture is perpendicular to the long axis of the bone ¡ Compound (open) – bone ends penetrate the skin ¡ Simple (closed) – bone ends do not penetrate the skin ¡

Common Types of Fractures Comminuted – bone fragments into three or more pieces; common in the elderly ¡ Spiral – ragged break when bone is excessively twisted; common sports injury ¡ Depressed – broken bone portion pressed inward; typical skull fracture ¡

Common Types of Fractures Compression – bone is crushed; common in porous bones ¡ Epiphyseal – epiphysis separates from diaphysis along epiphyseal line; occurs where cartilage cells are dying ¡ Greenstick – incomplete fracture where one side of the bone breaks and the other side bends; common in children ¡

Common Types of Fractures Table 6. 2. 1
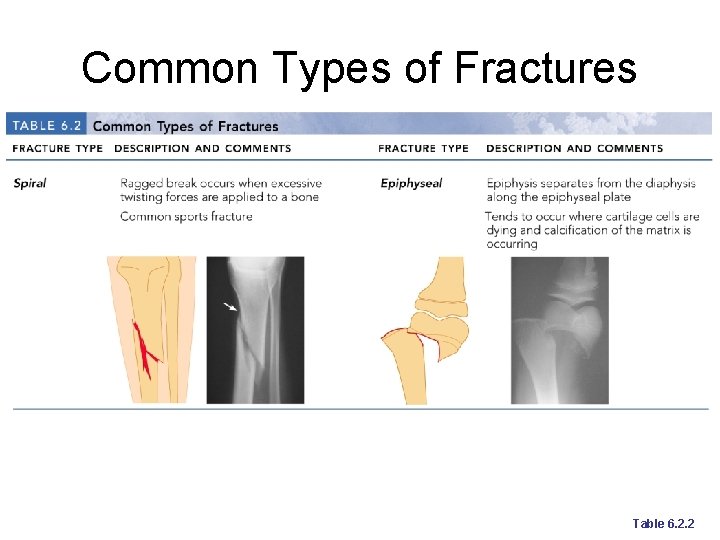
Common Types of Fractures Table 6. 2. 2
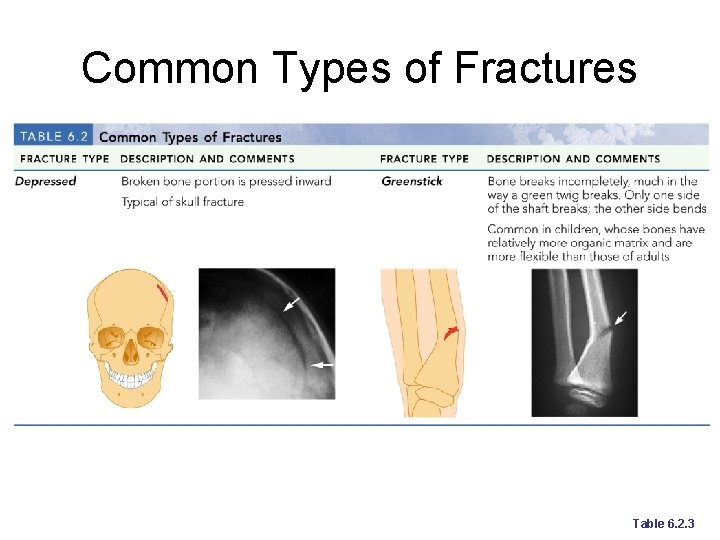
Common Types of Fractures Table 6. 2. 3
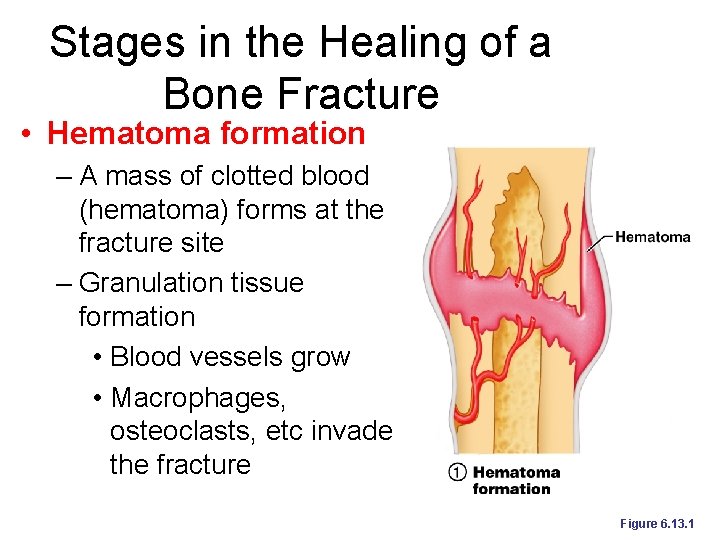
Stages in the Healing of a Bone Fracture • Hematoma formation – A mass of clotted blood (hematoma) forms at the fracture site – Granulation tissue formation • Blood vessels grow • Macrophages, osteoclasts, etc invade the fracture Figure 6. 13. 1
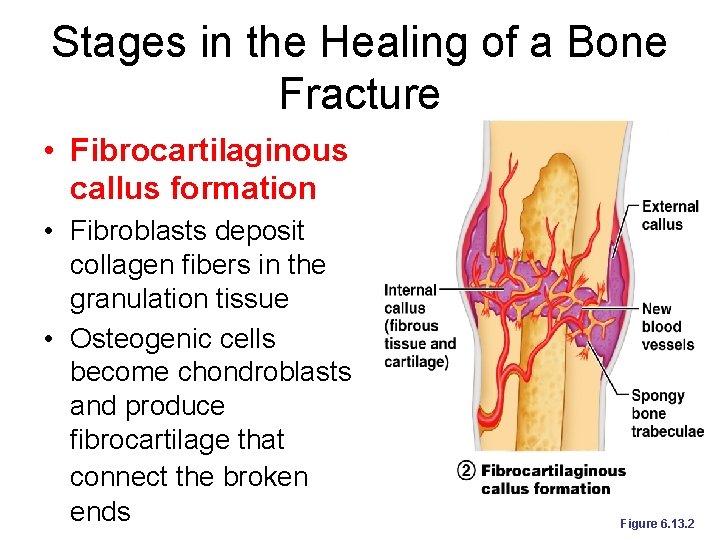
Stages in the Healing of a Bone Fracture • Fibrocartilaginous callus formation • Fibroblasts deposit collagen fibers in the granulation tissue • Osteogenic cells become chondroblasts and produce fibrocartilage that connect the broken ends Figure 6. 13. 2
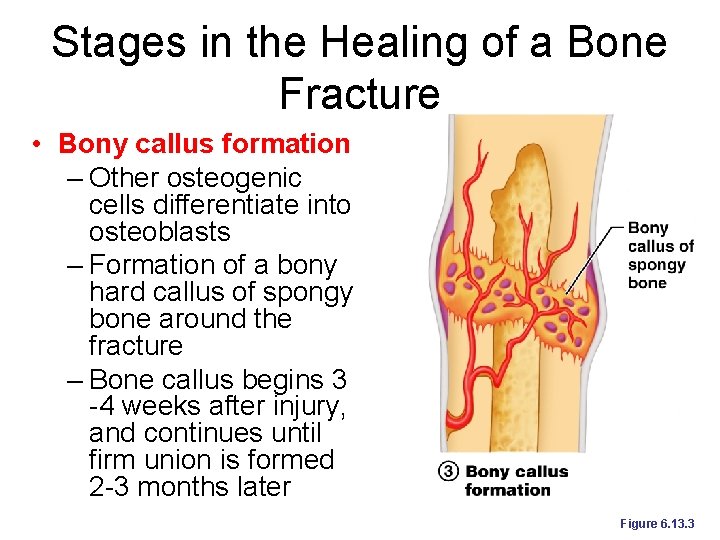
Stages in the Healing of a Bone Fracture • Bony callus formation – Other osteogenic cells differentiate into osteoblasts – Formation of a bony hard callus of spongy bone around the fracture – Bone callus begins 3 -4 weeks after injury, and continues until firm union is formed 2 -3 months later Figure 6. 13. 3
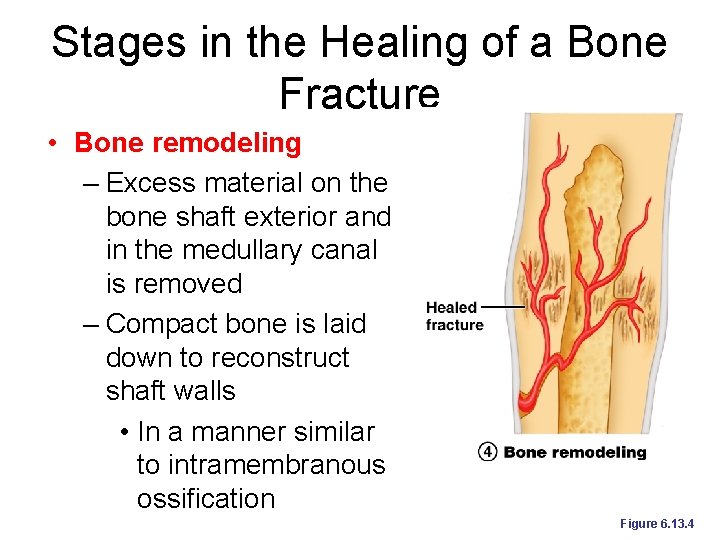
Stages in the Healing of a Bone Fracture • Bone remodeling – Excess material on the bone shaft exterior and in the medullary canal is removed – Compact bone is laid down to reconstruct shaft walls • In a manner similar to intramembranous ossification Figure 6. 13. 4

Homeostatic Imbalances ¡ Osteomalacia l Bones are inadequately mineralized causing softened, weakened bones l Main symptom is pain when weight is put on the affected bone l Caused by insufficient calcium in the diet, or by vitamin D deficiency

Homeostatic Imbalances ¡ Rickets l Bones of children are inadequately mineralized causing softened, weakened bones l Bowed legs and deformities of the pelvis, skull, and rib cage are common l Caused by insufficient calcium in the diet, or by vitamin D deficiency

Homeostatic Imbalances ¡ Osteopenia l Osteoblast activity decreases, osteoclast activity remains the same l Epiphysis, jaw, vertebra

Homeostatic Imbalances ¡ Osteoporosis l Osteopenia beyond expected l Spontaneous fractures l Spongy bone of the spine is most vulnerable l Occurs most often in postmenopausal women

Paget’s Disease Characterized by excessive bone formation and breakdown ¡ Pagetic bone, along with reduced mineralization, causes spotty weakening of bone ¡ Osteoclast activity wanes, but osteoblast activity continues to work ¡
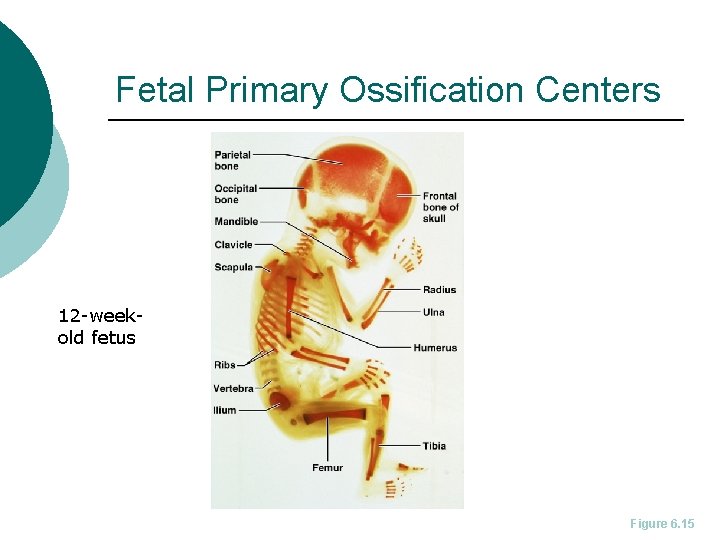
Fetal Primary Ossification Centers 12 -weekold fetus Figure 6. 15

Developmental Aspects of Bones Mesoderm gives rise to embryonic mesenchymal cells, which produce membranes and cartilages that form the embryonic skeleton ¡ The embryonic skeleton ossifies in a predictable timetable that allows fetal age to be easily determined from sonograms ¡ At birth, most long bones are well ossified (except for their epiphyses) ¡

Developmental Aspects of Bones By age 25, nearly all bones are completely ossified ¡ In old age, bone resorption predominates ¡ A single gene that codes for vitamin D docking determines both the tendency to accumulate bone mass early in life, and the risk for osteoporosis later in life ¡
- Slides: 93