Bone Loss and Patterns of Bone Destruction DDS

Bone Loss and Patterns of Bone Destruction 黃仁勇 DDS Ph. D 國防醫學院牙醫學系 三軍總醫院牙周病科

Bone Loss and Patterns of Bone Destruction Ø Periodontitis: infectious disease of the gingiva destruction of bone tooth loss
Bone Loss and Patterns of Bone Destruction Ø Density and height of bone local factors inflammation trauma from occlusion systemic disorders equilibrium of bone resorption and formation

Bone Loss and Patterns of Bone Destruction Ø bone level: experience of past inflammation Ø pocket change: present inflammatory condition Ø both are not necessarily correlated

Bone destruction caused by extension of gingival inflammation u. Chronic inflammation: gingiva bone, PDL gingivitis periodontitis ?

Bone destruction caused by extension of gingival inflammation *bacterial composition in plaque: motile, spirochetes increased cocoid, straight rod decreased *cell composition in infiltrated connective tissue (ICT): fibroblast, lymphocyte predominant plasma cell, blast cell predominant *immune reaction: T-cell predominant B-cell predominant

Bone destruction caused by extension of gingival inflammation u. Extension of inflammation: 1. pathogenic potential of plaque 2. resistance of host: *immunologic activity *tissue-related mechanisms: fibrosis of gingiva width of attached gingiva reactive fibrosis & osteogenesis

Bone destruction caused by extension of gingival inflammation u. Histopathology: gingival inflammation extends along the collagen fibers and follows the course of blood vessels through the loosely arranged tissue around them into the alveolar bone
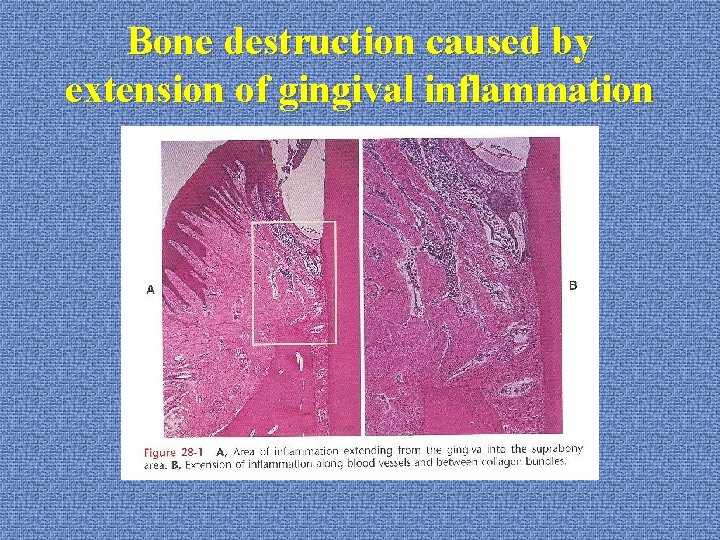
Bone destruction caused by extension of gingival inflammation

Bone destruction caused by extension of gingival inflammation u. Histopathology: pathways (interproximal) *gingiva trans-septal fibers bone crest marrow PDL angle of crest *gingiva PDL

Bone destruction caused by extension of gingival inflammation u. Histopathology: pathways (facial & lingual) *gingiva outer periosteum bone *gingiva PDL
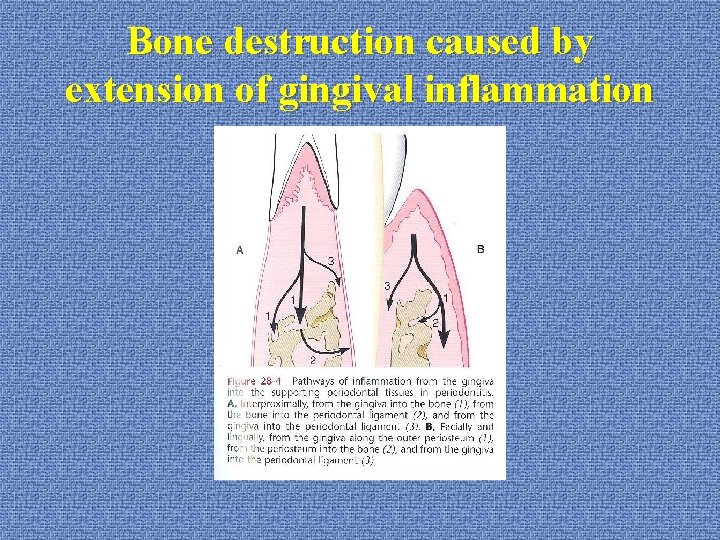
Bone destruction caused by extension of gingival inflammation

Bone destruction caused by extension of gingival inflammation u. Histopathology: there is a continuous tendency to recreate trans-septal fibers across the crest of the interdental septum farther along the root as the bone destruction progresses
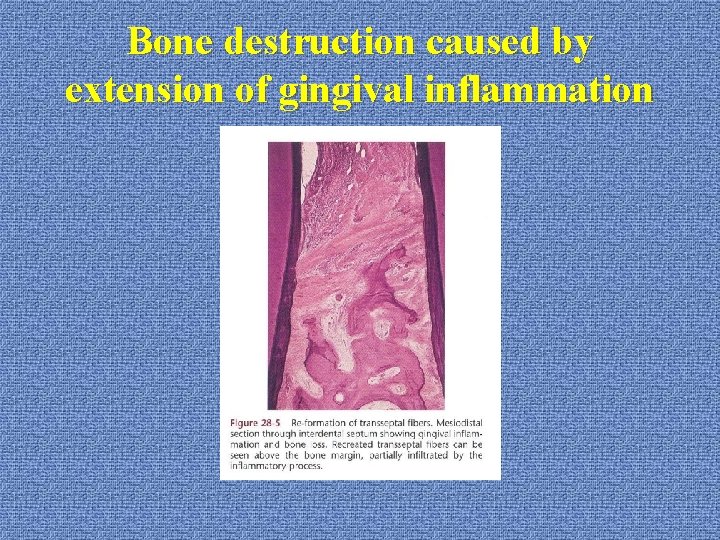
Bone destruction caused by extension of gingival inflammation

Bone destruction caused by extension of gingival inflammation u. Histopathology: *marrow: leukocyte, fluid exudates, new blood vessel, proliferating fibroblast, enlarged marrow space *bone: multinuclear osteoclasts, mononuclear phagocytes, Howship lacunae on the bone surface, thinning trabeculae
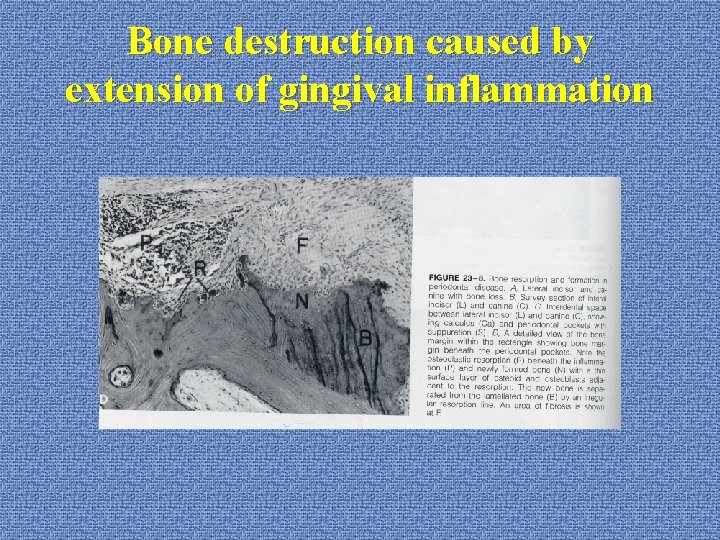
Bone destruction caused by extension of gingival inflammation
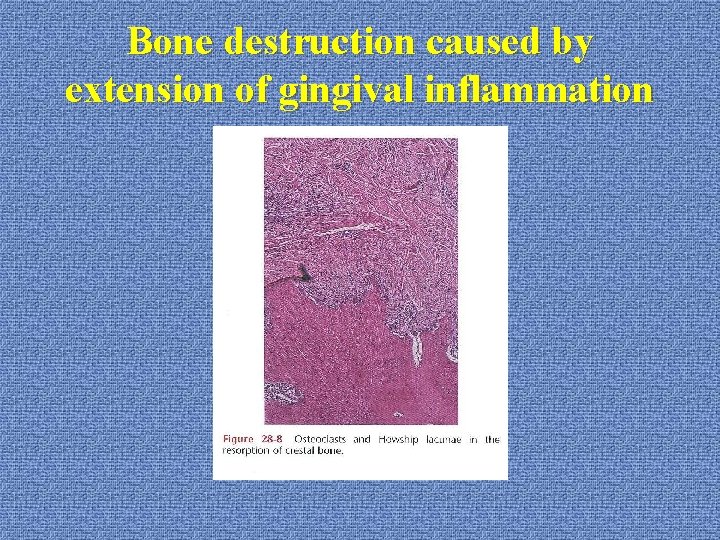
Bone destruction caused by extension of gingival inflammation

Bone destruction caused by extension of gingival inflammation u. Histopathology: *not bone necrosis *tissue necrosis and pus in the soft tissue wall of periodontal pocket *osteoclast: remove mineral portion mononuclear cell: degrade organic matrix

Bone destruction caused by extension of gingival inflammation u. Histopathology: *the amount of inflammatory infiltrate bone loss No. of osteoclasts *the distance from the apical border of the inflammatory infiltrate to the alveolar crest No. of osteoclasts on the alveolar crest total No. of osteoclasts

Bone destruction caused by extension of gingival inflammation u. Radius: (Page & Schroeder) bacterial effectiveness within 1. 5 -2. 5 mm *interproximal angular bony defect occurred only if interproximal space > 2. 5 mm

Bone destruction caused by extension of gingival inflammation u. Rate of bone loss: (Loe in Sri Lankan) *untreated periodontitis: 0. 2 mm(facial), 0. 3 mm(interproximal) bone loss per year *8% rapid loss of att. (0. 1 -1 mm per year) *81% moderate loss of att. (0. 05 -0. 5 mm per year) *11% minimal or no loss of att. 0. 09 mm per year) (0. 05 -

Bone destruction caused by extension of gingival inflammation u. Periods of destruction: episodic, intermittent burst related to: *acute inflammatory reaction *T-lymphocyte to B-lymphocyte & plasma cell *loose, unattached, motile, Gram(-), anaerobic flora *followed by advanced local host defense
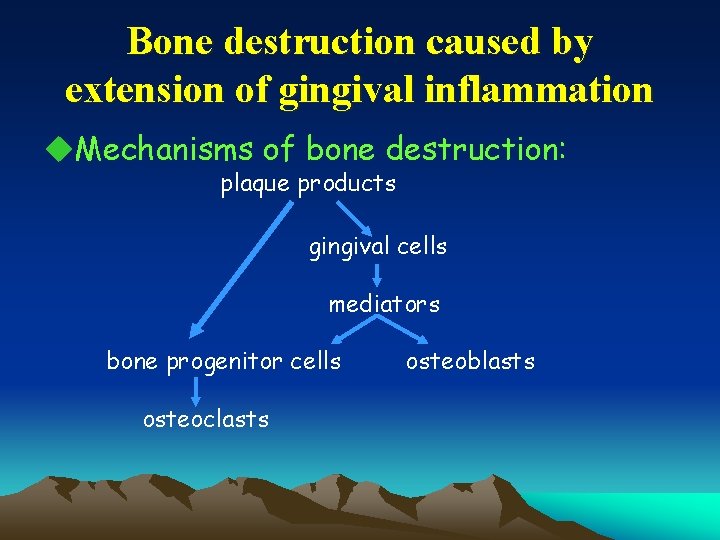
Bone destruction caused by extension of gingival inflammation u. Mechanisms of bone destruction: plaque products gingival cells mediators bone progenitor cells osteoclasts osteoblasts
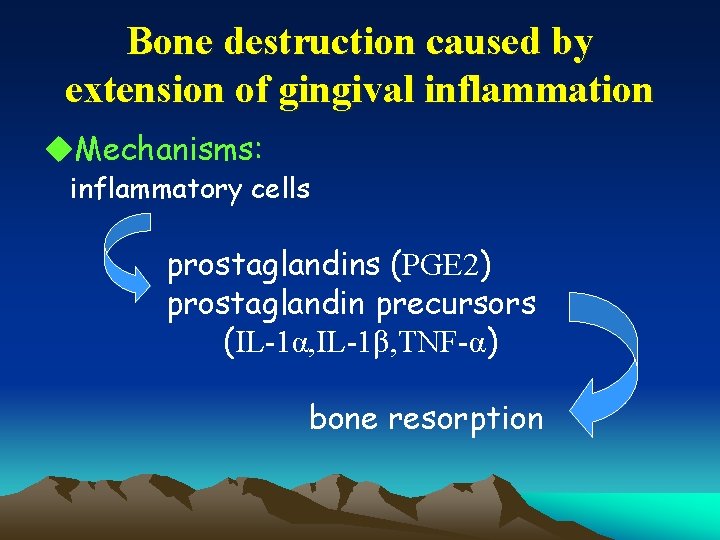
Bone destruction caused by extension of gingival inflammation u. Mechanisms: inflammatory cells prostaglandins (PGE 2) prostaglandin precursors (IL-1α, IL-1β, TNF-α) bone resorption

Bone destruction caused by extension of gingival inflammation u. Bone formation in periodontal disease *response of alveolar bone for inflammation: bone resorption and bone formation *bone formation: adjacent to sites of active bone resorption & along trabecular surface at a distance from the inflammation (buttressing bone formation)

Bone destruction caused by extension of gingival inflammation u. Bone formation in periodontal disease *bone loss: bone resorption > bone formation *the basic aim of periodontal therapy is the elimination of inflammation to remove the stimulus for bone resorption

Bone destruction caused by trauma from occlusion u. TFO without inflammation *funnel-shaped widening of the crestal portion of PDL *bone resorption cause angular shape defect (cushioning effect) *increased tooth mobility *reversible u. TFO with inflammation *speed up the bone loss caused by inflammation
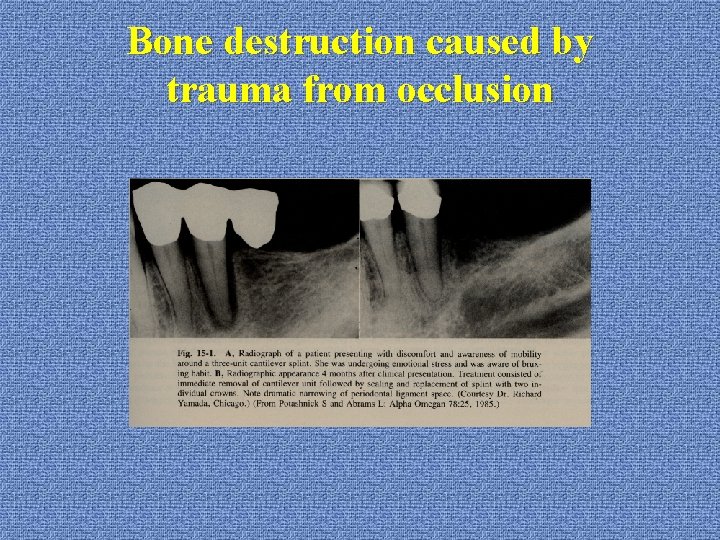
Bone destruction caused by trauma from occlusion

Bone destruction caused by systemic disorders u. Osteoporosis: *menopause women *loss of bone mineral content and structural bone changes *share some risk factors with periodontitis: aging, smoking, disease, medications that interfere with healing u. Generalized skeletal disturbances: *hyperparathyroidism, leukemia, Langerhans cell histocytosis *probably totally unrelated to the usual periodontal problem
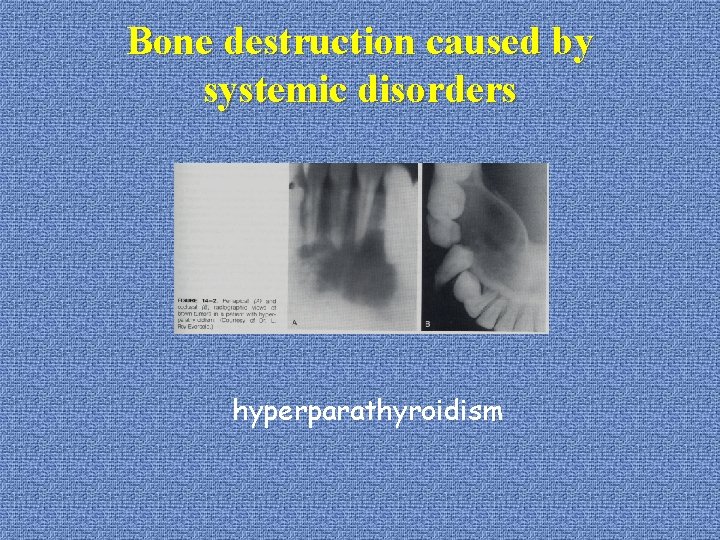
Bone destruction caused by systemic disorders hyperparathyroidism

Factors determining bone morphology in periodontal disease u. Normal variations in alveolar bone u. Exostoses u. Trauma from occlusion u. Buttressing bone formation u. Food impaction u. Aggressive periodontitis

Factors determining bone morphology in periodontal disease u. Normal variations in alveolar bone *the width, thickness & crestal angulation of interdental septa *the thickness of the facial and lingual alveolar process *the presence of fenestration & dehiscence *the alignment of the teeth *root and root trunk anatomy *root position within the alveolar process *proximity with another tooth surface
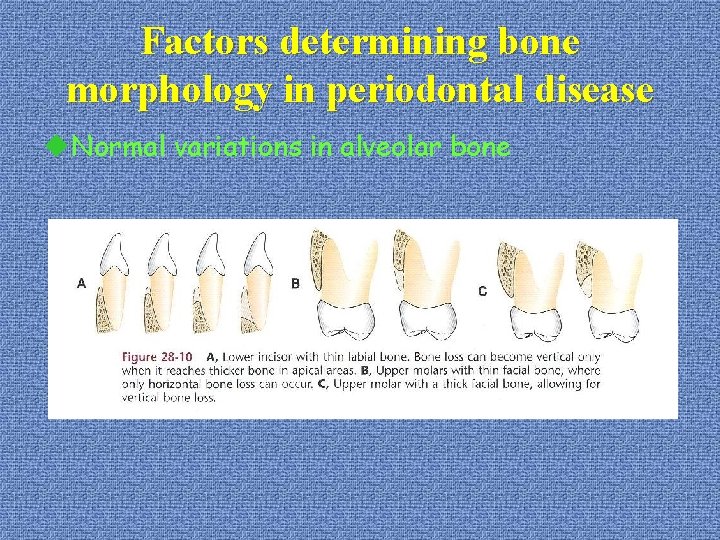
Factors determining bone morphology in periodontal disease u. Normal variations in alveolar bone

Factors determining bone morphology in periodontal disease u. Exostoses *outgrowth of bone of varied size and shape *palatal exostoses: 40%
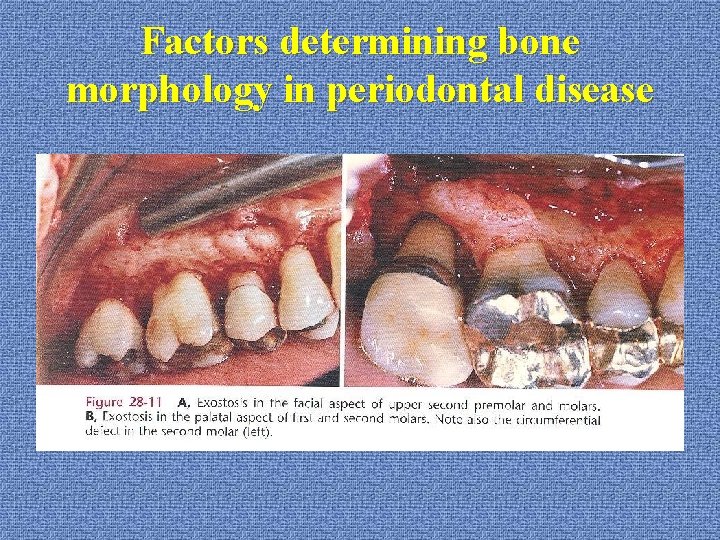
Factors determining bone morphology in periodontal disease

Factors determining bone morphology in periodontal disease u. Trauma from occlusion *thickening of cervical marginal bone *angular bone defect

Factors determining bone morphology in periodontal disease u. Buttressing bone formation *central: within the bone *peripheral: external surface (lipping)
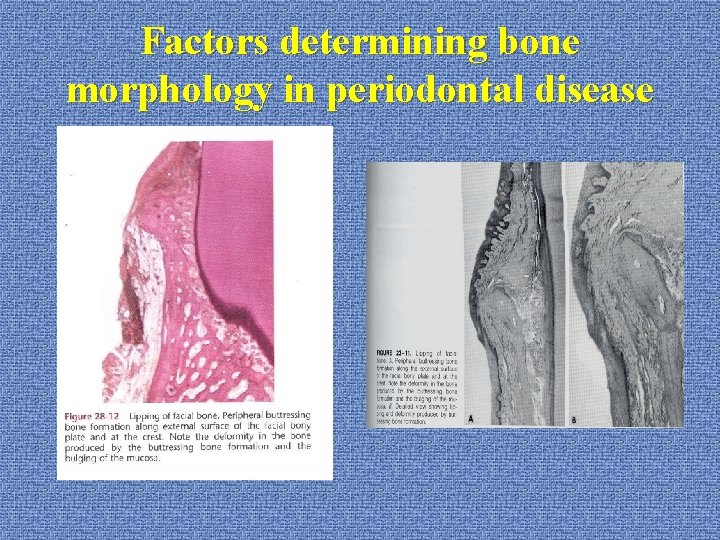
Factors determining bone morphology in periodontal disease

Factors determining bone morphology in periodontal disease u. Food impaction *interdental bone defect *pressure & irritation *complicating factor u. Aggressive periodontitis *vertical or angular defect in 1 st molar

Bone destruction patterns in periodontal disease u. Horizontal bone loss u. Bone deformities (osseous defects) *vertical, angular defect *osseous crater *bulbous bone contour *reverse architecture *ledge *furcation involvement

Bone destruction patterns in periodontal disease u. Horizontal bone loss: *bone height reduced *bone margin perpendicular to the tooth surface *interdental septa and facial & lingual plate affected *x-ray: bone margin parallel to CEJCEJ
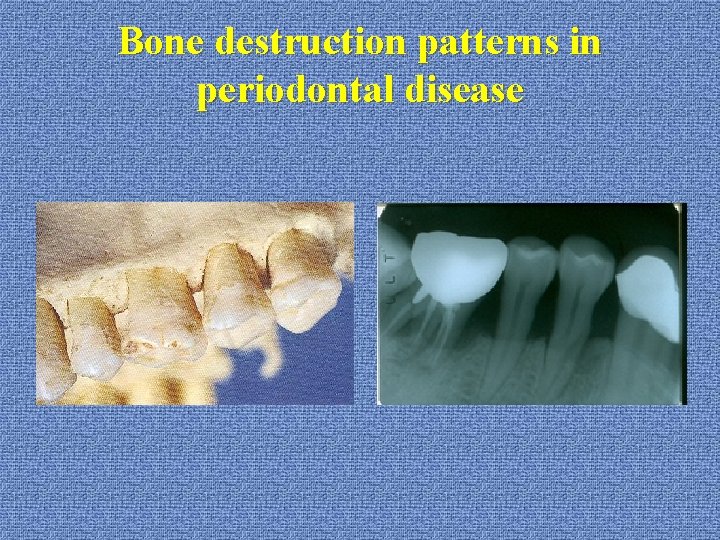
Bone destruction patterns in periodontal disease
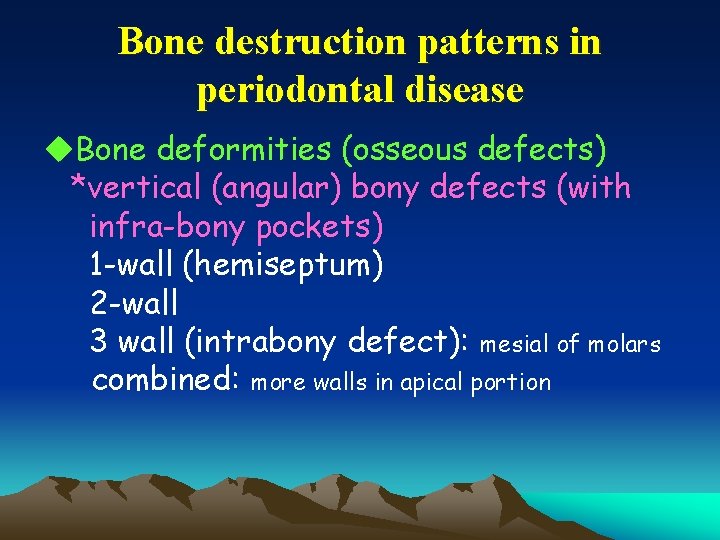
Bone destruction patterns in periodontal disease u. Bone deformities (osseous defects) *vertical (angular) bony defects (with infra-bony pockets) 1 -wall (hemiseptum) 2 -wall 3 wall (intrabony defect): mesial of molars combined: more walls in apical portion
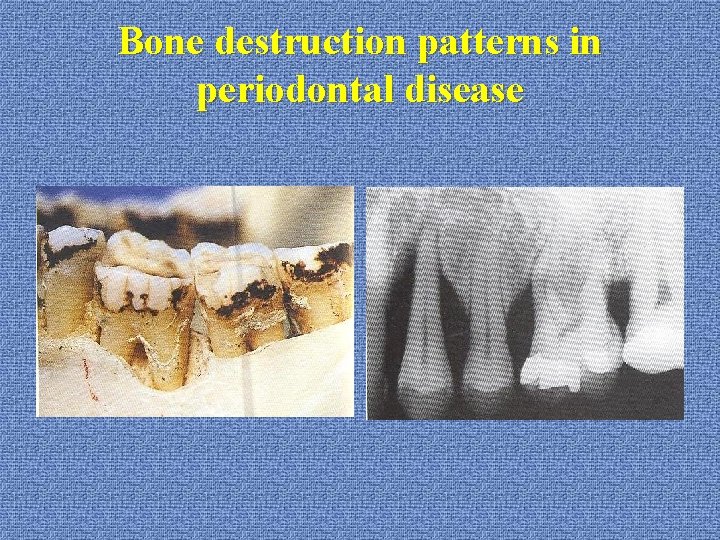
Bone destruction patterns in periodontal disease
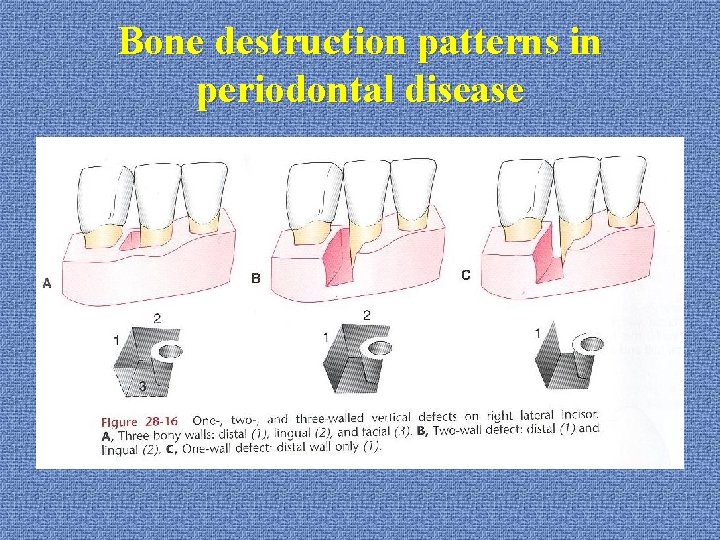
Bone destruction patterns in periodontal disease
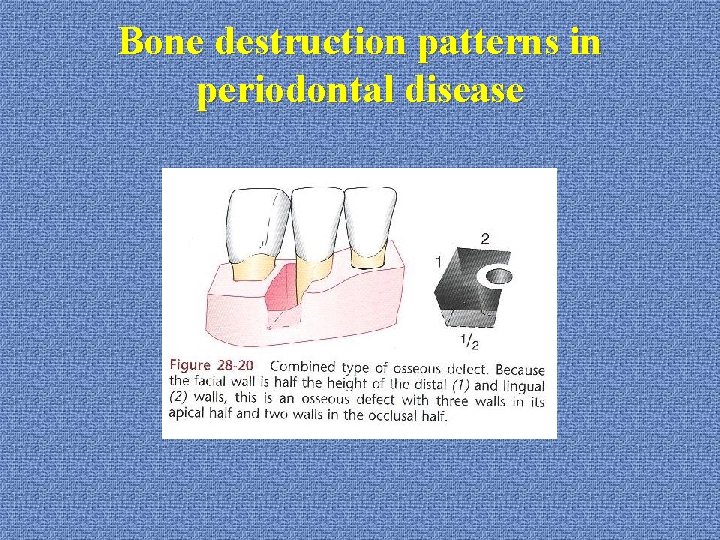
Bone destruction patterns in periodontal disease

Bone destruction patterns in periodontal disease *osseous crater --concavity in the crest of interdental bone --within the facial and lingual wall --35. 2% of all defects; 62% of man. defects --posterior: anterior=2: 1 --causes: difficult to remove plaque flat or concave interdental septum in man. molars vascular patterns from the gingiva to the center of the crest
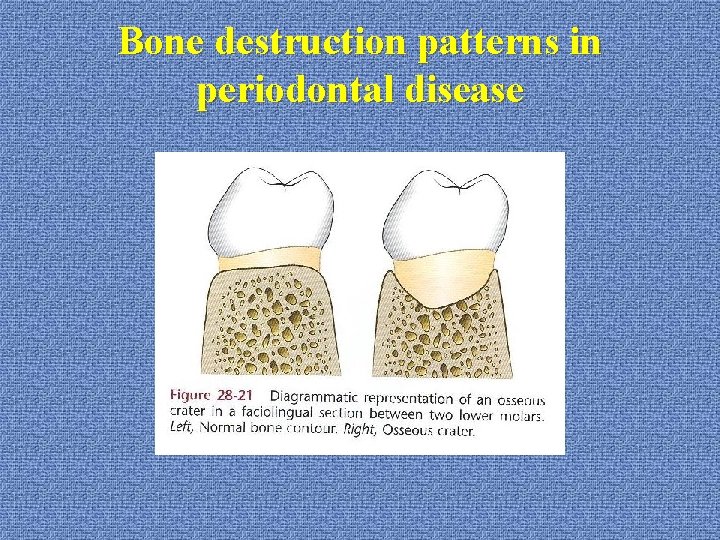
Bone destruction patterns in periodontal disease

Bone destruction patterns in periodontal disease *bulbous bone contours: --bony enlargement --maxilla --cause: exostoses buttressing bone formation adaptation to function
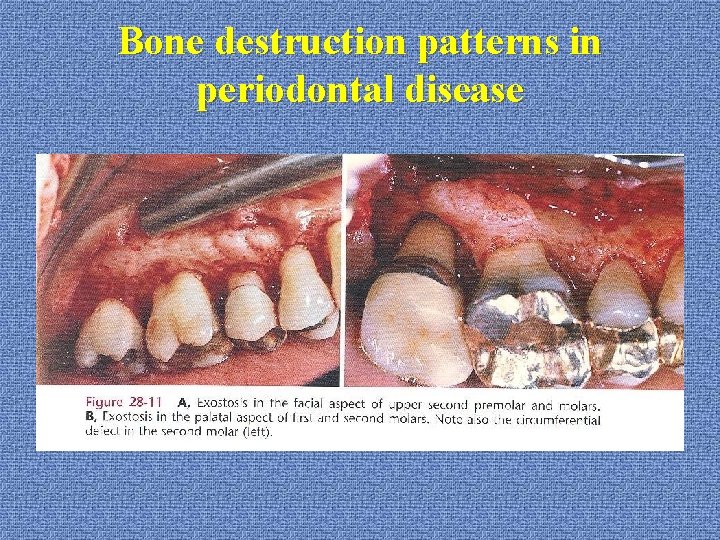
Bone destruction patterns in periodontal disease

Bone destruction patterns in periodontal disease *reverse architecture: --reversing the normal architecture --maxilla --cause: interdental bone loss, radicular bone exist
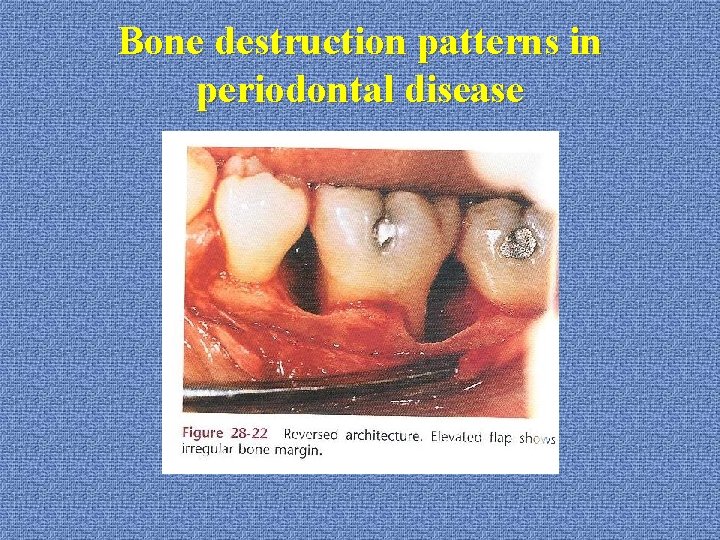
Bone destruction patterns in periodontal disease

Bone destruction patterns in periodontal disease *ledge: --plateau-like bone margin --cause: resorption of thickened bone plate
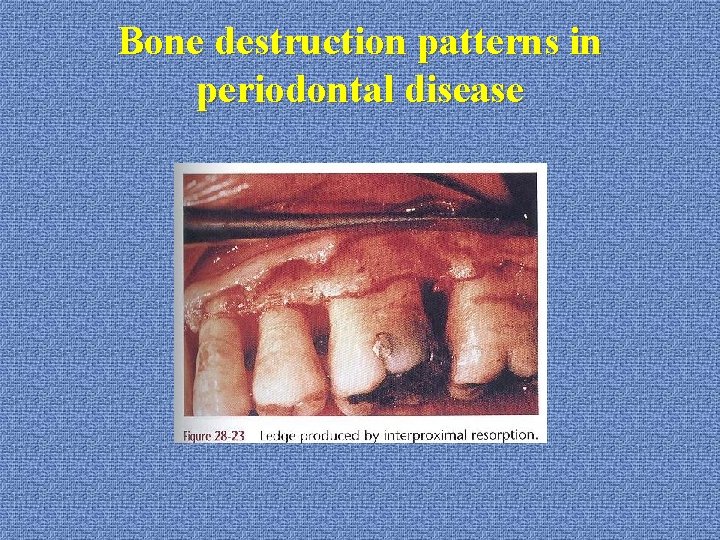
Bone destruction patterns in periodontal disease

Bone destruction patterns in periodontal disease *furcation involvement: --invasion of the bifurcation and trifurcation of multi-rooted teeth by periodontal disease --most in man. 1 st molars; least in max. premolars

Bone destruction patterns in periodontal disease *furcation involvement: --classification: 1958 Glickman(horizontal) Grade I incipient II cul-de-sac III through-and through IV III & gingival recession

Bone destruction patterns in periodontal disease *furcation involvement: --classification: 1938 Lindhe (horizontal) Grade I initial, <1/3 B-L width II >1/3 B-L width III through-and-through & gingival recession
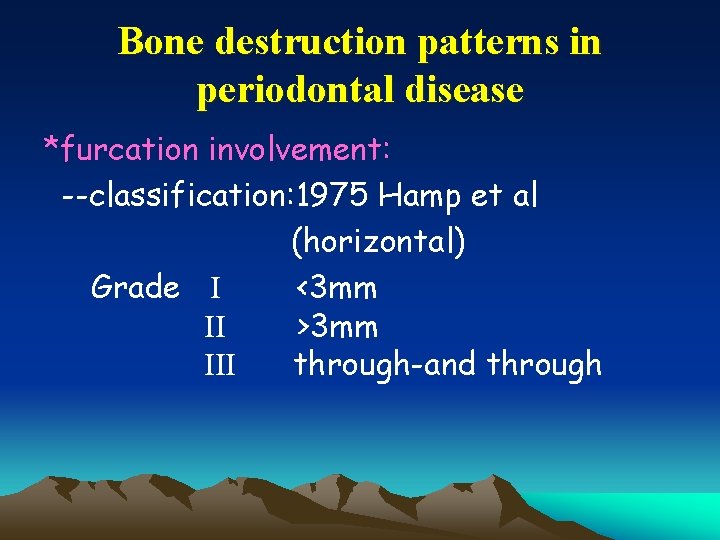
Bone destruction patterns in periodontal disease *furcation involvement: --classification: 1975 Hamp et al (horizontal) Grade I <3 mm II >3 mm III through-and through
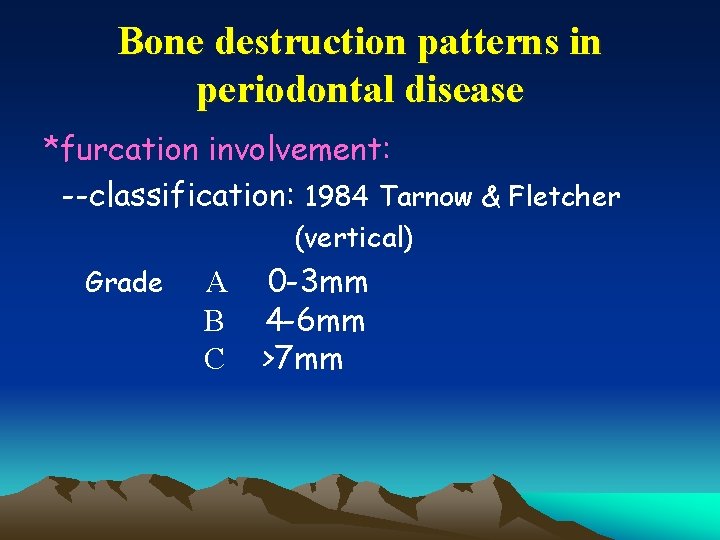
Bone destruction patterns in periodontal disease *furcation involvement: --classification: 1984 Tarnow & Fletcher (vertical) Grade A B C 0 -3 mm 4 -6 mm >7 mm

Bone destruction patterns in periodontal disease *furcation involvement: --causes: plaque TFO (? ): contributing factor enamel projection: 13% proximity of furcation to CEJ: 75% in F. I. accessory pulpal canals: 36% in max. 1 st molars; 32% in man. 1 st molars 12% in max. 2 nd molars; 24% in man. 2 nd molars

Bone destruction patterns in periodontal disease *furcation involvement: --diagnosis: probing (horizontal and vertical) radiography
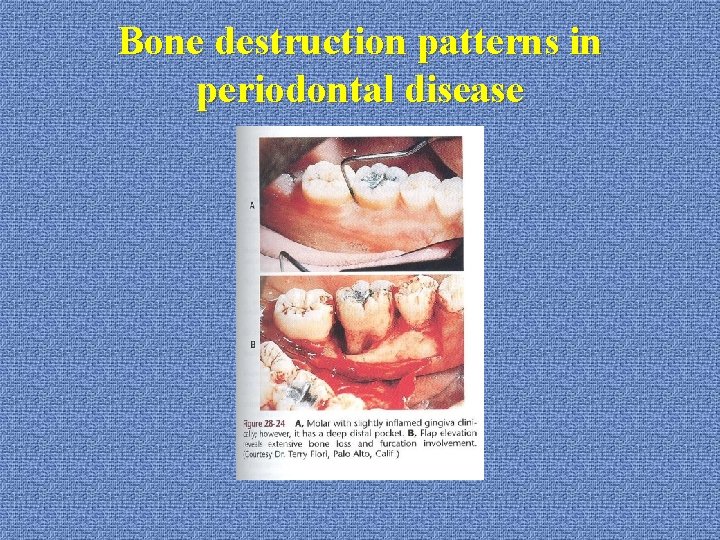
Bone destruction patterns in periodontal disease
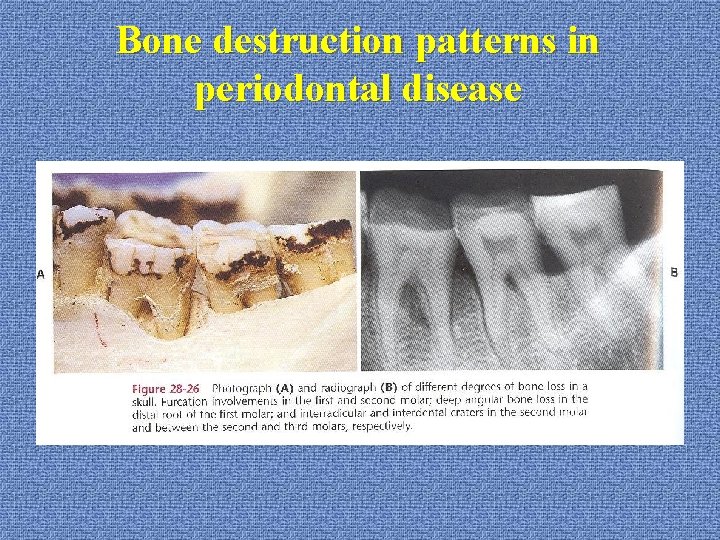
Bone destruction patterns in periodontal disease
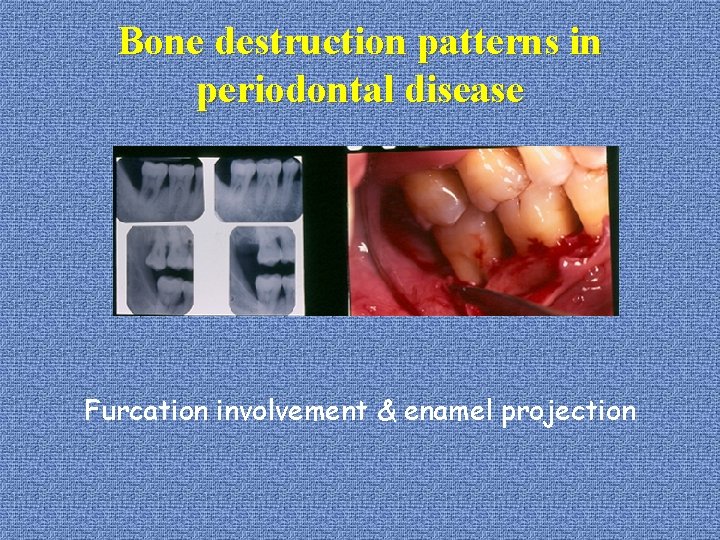
Bone destruction patterns in periodontal disease Furcation involvement & enamel projection
- Slides: 64