Bone grafts and bone graft substitutes to promote

Bone grafts and bone graft substitutes to promote fracture union—options and outcomes AO Trauma Advanced Principles Course

Learning objectives • List the desired characteristics of bone grafts to obtain union • Compare bone graft substitutes and contrast them with autogenous bone graft • Identify characteristics of each substitute and evaluate its indications

General trends • Use of bone substitutes continues to rise • Vast number of: • Dental 46% • Basic science/animal 25% • Spine 11% • Small series 5% • Review articles 14%
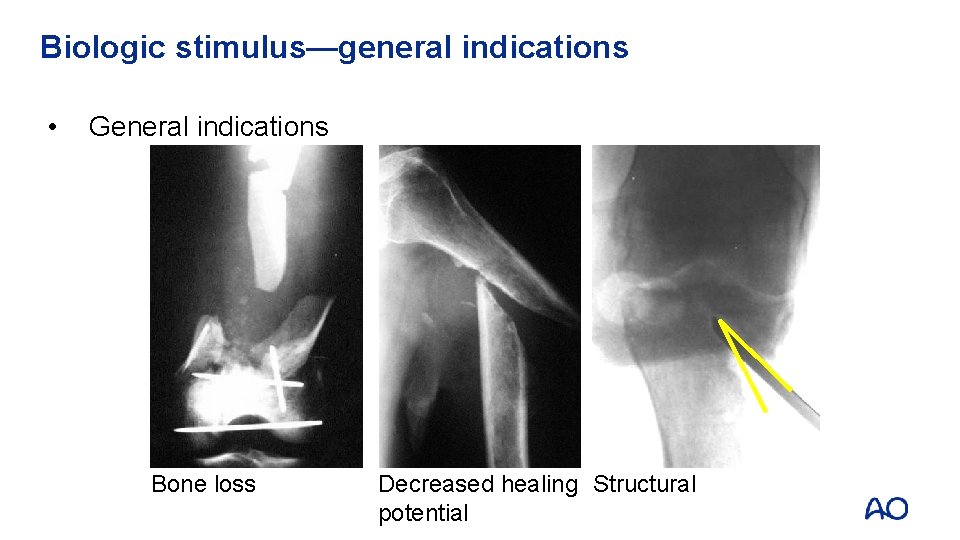
Biologic stimulus—general indications • General indications Bone loss Decreased healing Structural potential
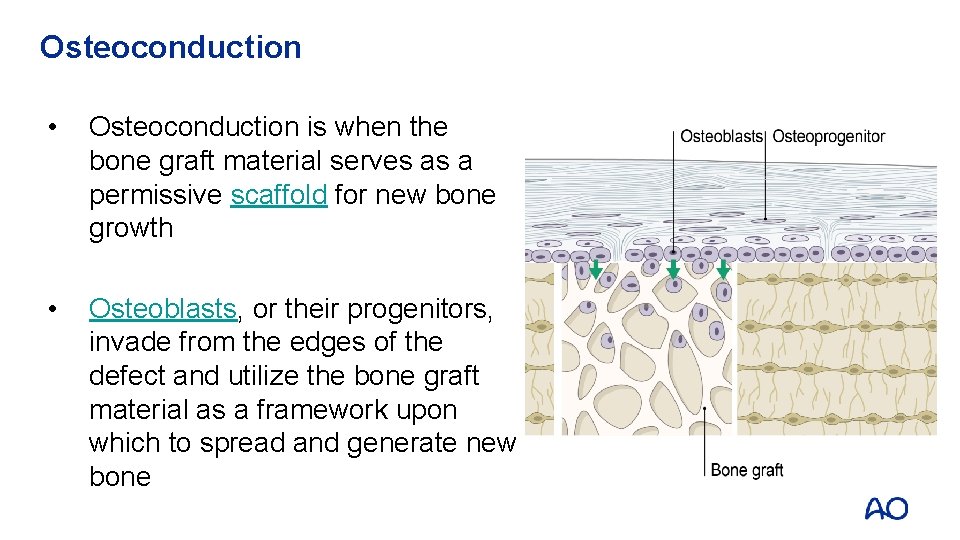
Osteoconduction • Osteoconduction is when the bone graft material serves as a permissive scaffold for new bone growth • Osteoblasts, or their progenitors, invade from the edges of the defect and utilize the bone graft material as a framework upon which to spread and generate new bone

Osteoinduction • • • Osteoinduction involves the differentiation of osteoprogenitor cells into osteoblasts, which are then involved in new bone formation This most commonly involves an incorporated growth factor, such as a bone morphogenetic protein As these growth factors are naturally present in demineralized bone matrix (DBM), osteoinduction is one of the main mechanisms involved when using DBM
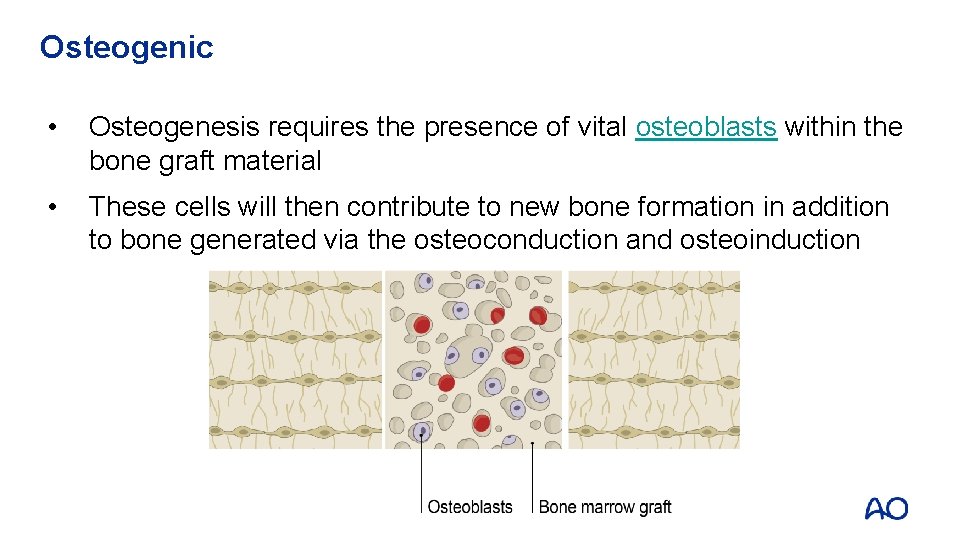
Osteogenic • Osteogenesis requires the presence of vital osteoblasts within the bone graft material • These cells will then contribute to new bone formation in addition to bone generated via the osteoconduction and osteoinduction
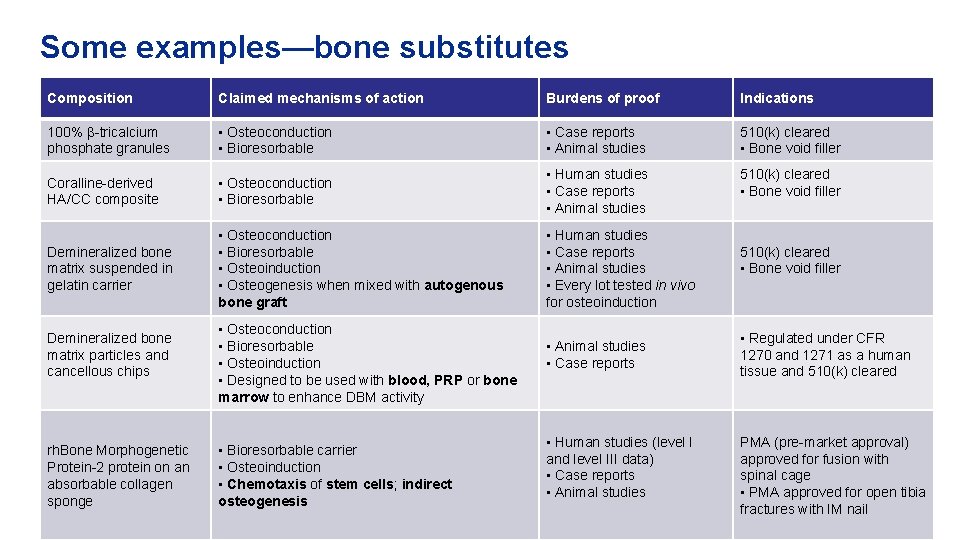
Some examples—bone substitutes Composition Claimed mechanisms of action Burdens of proof Indications 100% β-tricalcium phosphate granules • Osteoconduction • Bioresorbable • Case reports • Animal studies 510(k) cleared • Bone void filler Coralline-derived HA/CC composite • Osteoconduction • Bioresorbable • Human studies • Case reports • Animal studies 510(k) cleared • Bone void filler Demineralized bone matrix suspended in gelatin carrier • Osteoconduction • Bioresorbable • Osteoinduction • Osteogenesis when mixed with autogenous bone graft • Human studies • Case reports • Animal studies • Every lot tested in vivo for osteoinduction Demineralized bone matrix particles and cancellous chips rh. Bone Morphogenetic Protein-2 protein on an absorbable collagen sponge • Osteoconduction • Bioresorbable • Osteoinduction • Designed to be used with blood, PRP or bone marrow to enhance DBM activity • Bioresorbable carrier • Osteoinduction • Chemotaxis of stem cells; indirect osteogenesis • Animal studies • Case reports • Human studies (level I and level III data) • Case reports • Animal studies 510(k) cleared • Bone void filler • Regulated under CFR 1270 and 1271 as a human tissue and 510(k) cleared PMA (pre-market approval) approved for fusion with spinal cage • PMA approved for open tibia fractures with IM nail

Net biological activity Sum of: • Inherent biological activity • Living cells and products • Osteoinduction capacity • Osteoconduction capacity • Capacity of the surrounding tissues to activate
Bone formation requirements Combination of: • Vascularity • Stability • Progenitor cells • Structural matrix • Growth factors
Alterations in healing • Vascularity • Stability • Progenitor cells • Structural matrix • Growth factors

Considerations • Graft material is dependent on the local and systemic environment • The graft must supply what the host lacks • The host must supply what is not inherent to the graft!
Host problems • Local • Infection • Soft-tissue injury • Instability • Vascularity

Host problems—systemic • Systemic disease (diabetes mellitus, thyroid cancer, etc) • Obesity • Post menopausal • Immunocompromised • Tobacco • Medications (steroids, chemotherapy)

Ideal bone graft substitute • Biocompatable • Bioresorbable • Osteoconductive • Osteoinductive • Structural • Easy to use • Cost effective

Types of grafts • Autograft • Allograft • Biosynthetic • Composite • Growth factors

Autogenous bone graft • Osteoconductive • • Osteoinductive • • Hydroxyapatite, collagen BMP, TGF-B, etc Osteogenic • Osteoprogenitor cells

Advantages of autogenous bone graft • Histocompatable • No risk of transmissible disease • Osteogenic cells and proteins • Rapid incorporation • Structural, workable

Limitations of autogenous bone graft • Limited quantity • Limited sites • Limited structure and shape • Variable osteogenic potential • Donor site morbidity

Ideal bone graft substitute • Biocompatable • Bioresorbable • Osteoconductive • Osteoinductive • Structural • Easy to use • Cost effective

Allograft—types Properties determined by processing • Fresh • Problems • Availability, compatibility, storage, and disease • Frozen • At temperatures less than -600° C • Freeze dried • Water removed and vacuum sealed • Demineralized bone matrix (DBM)
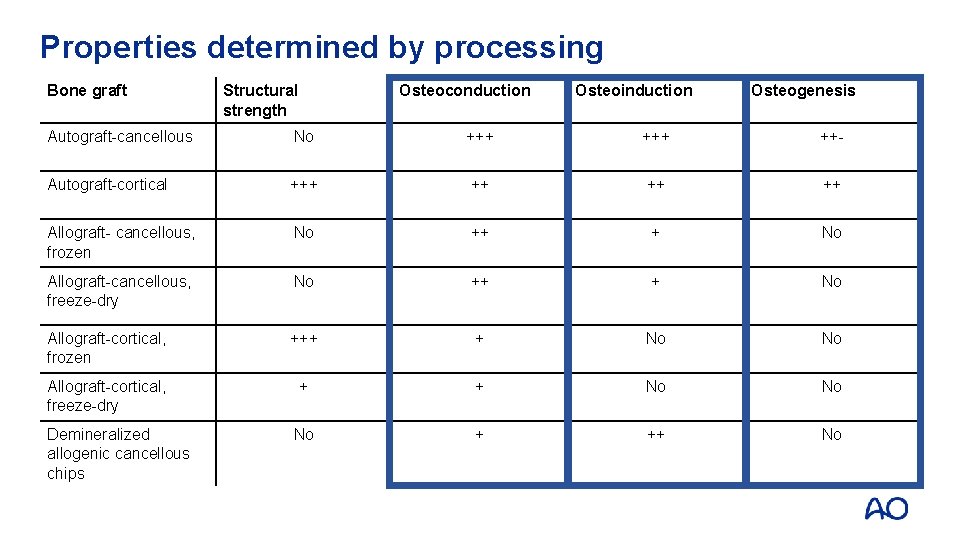
Properties determined by processing Bone graft Structural strength Osteoconduction Osteoinduction Osteogenesis Autograft-cancellous No +++ ++- Autograft-cortical +++ ++ Allograft- cancellous, frozen No ++ + No Allograft-cancellous, freeze-dry No ++ + No Allograft-cortical, frozen +++ + No No Allograft-cortical, freeze-dry + + No No No + ++ No Demineralized allogenic cancellous chips
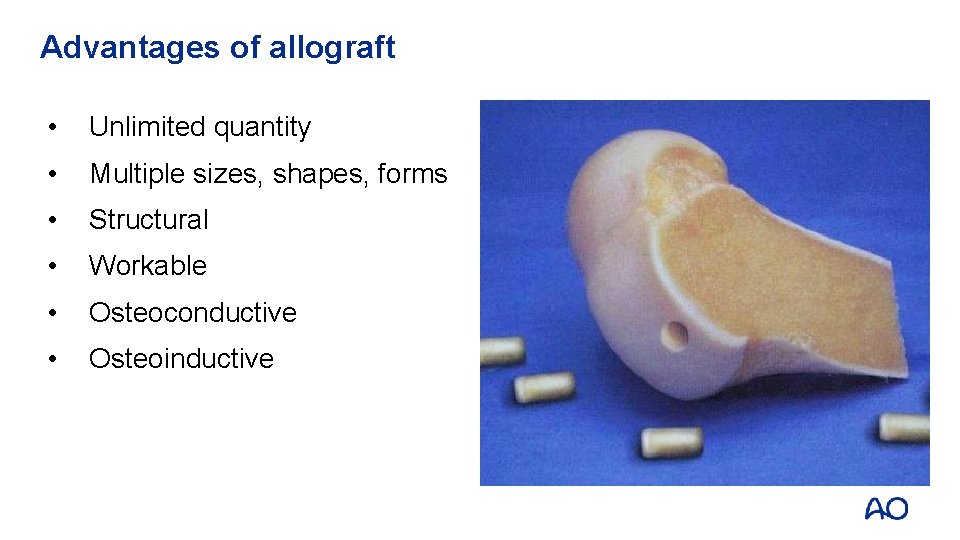
Advantages of allograft • Unlimited quantity • Multiple sizes, shapes, forms • Structural • Workable • Osteoconductive • Osteoinductive

Limitations of allograft • Disease transmission (HIV 1: 1, 000) • Histocompatability • • Problems with incorporation • • Improved with freezing and processing Weakens with revascularization Reliant on a favorable host bed
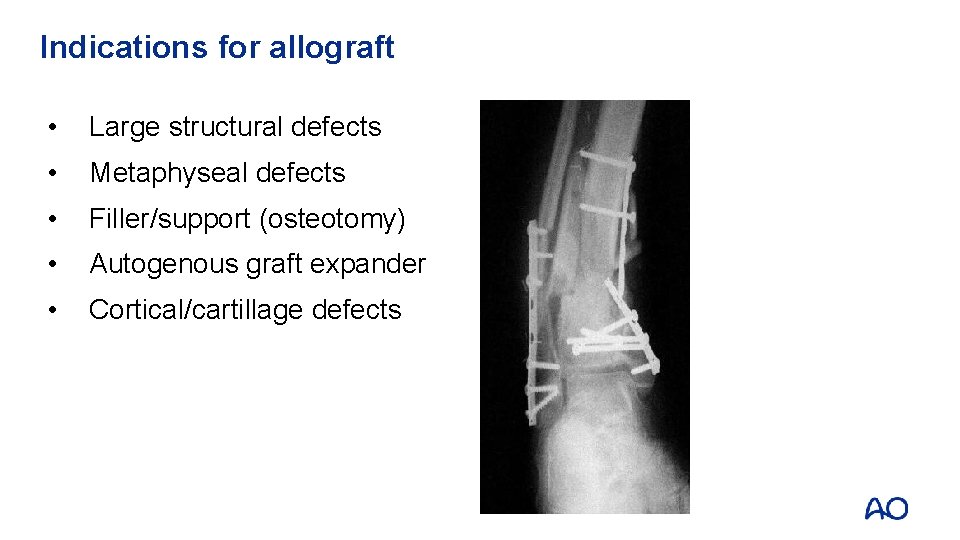
Indications for allograft • Large structural defects • Metaphyseal defects • Filler/support (osteotomy) • Autogenous graft expander • Cortical/cartillage defects

Ideal bone graft substitute—allograft • Biocompatable • Bioresorbable • Osteoconductive • Osteoinductive • Structural • Easy to use • Cost effective

Demineralized bone matrix • Noncollagenous protein, BMP, collagen • Osteoinduction • Limited osteoconductive capacity • Prepared by bone bank • Various forms • Easily stored, readily available

Demineralized bone matrix • Optefil • DBX • Dyna. Graft • Grafton • Osteofil • Regenafil

Limitations of demineralized bone matrix • Not structural • Not workable • Not osteogenic • Minimal osteoconductive • Variable osteoinductive capacity
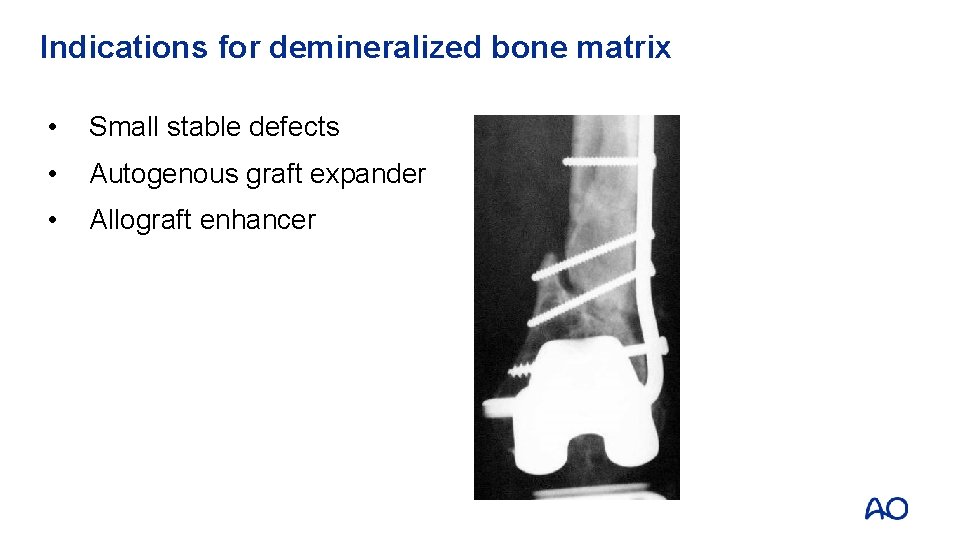
Indications for demineralized bone matrix • Small stable defects • Autogenous graft expander • Allograft enhancer

Ideal bone graft substitute—demineralized bone matrix • Biocompatable • Bioresorbable • Osteoconductive • Osteoinductive • Structural • Easy to use • Cost effective

Biosynthetic grafts—ceramics • Osteoconductive matrix • Composition • • Hydroxyapatite (HA) • Calcium phosphate • Calcium sulfate • Tricalcium phosphate (TCP) • Combinations Varying pore size and interconnectivity

Biosynthetic grafts • Pro. Osteon • Norian. SRS • Calceon • Osteoset • Collagraft • Vitoss

Advantages of biosynthetic grafts • Availability • Osteoconductive • Multiple sizes and shapes • Structural?
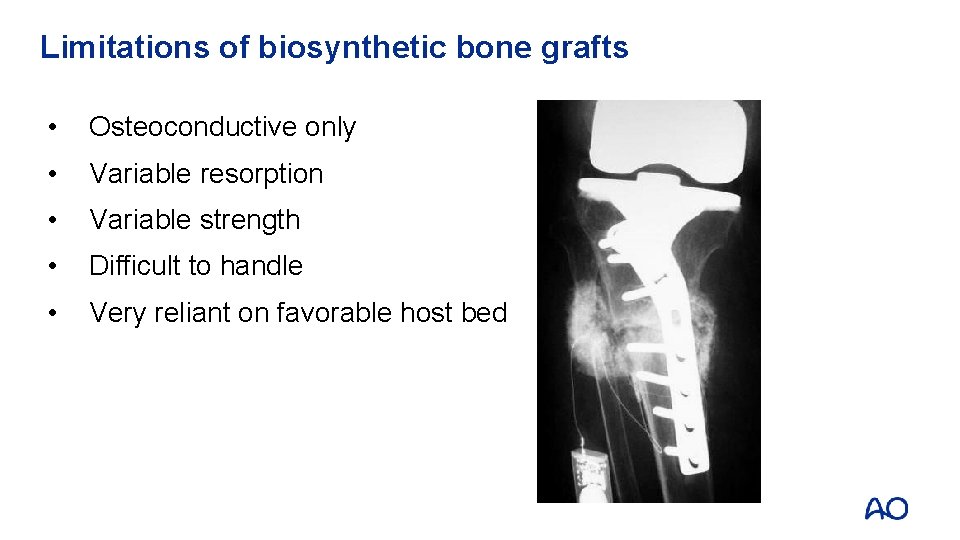
Limitations of biosynthetic bone grafts • Osteoconductive only • Variable resorption • Variable strength • Difficult to handle • Very reliant on favorable host bed
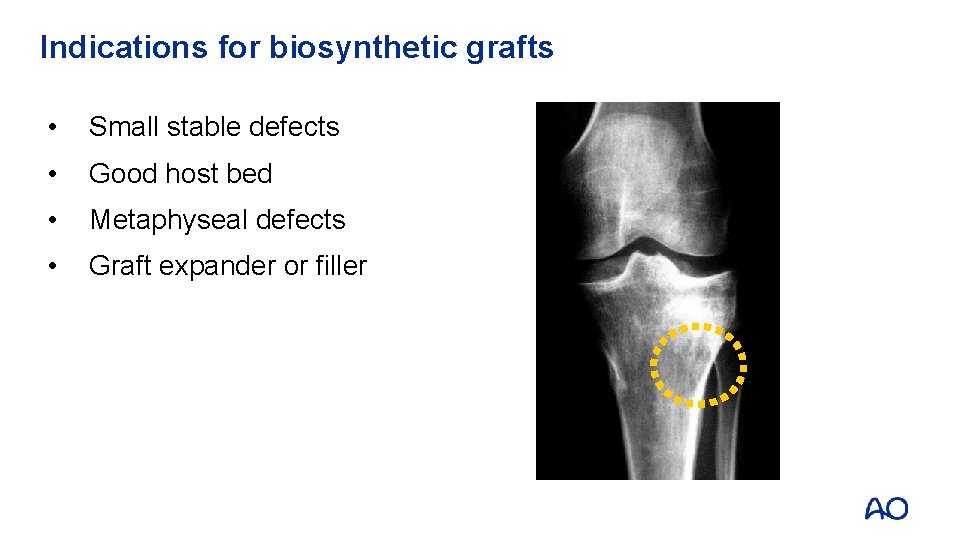
Indications for biosynthetic grafts • Small stable defects • Good host bed • Metaphyseal defects • Graft expander or filler

Ideal bone graft substitute—biosynthetic grafts • Biocompatable • Bioresorbable • Osteoconductive • Osteoinductive • Structural • Easy to use • Cost effective

Composite grafts Collagen + ceramic + hydroxyapatite • Multiple compositions • Osteoconductive • Osteoinductive • Paste or strips • Malleable

Composite grafts • Opteform • Ortho. Blast • Allo. Matrix

Limitations of composite bone grafts • Variable properties • Not structural • Expensive
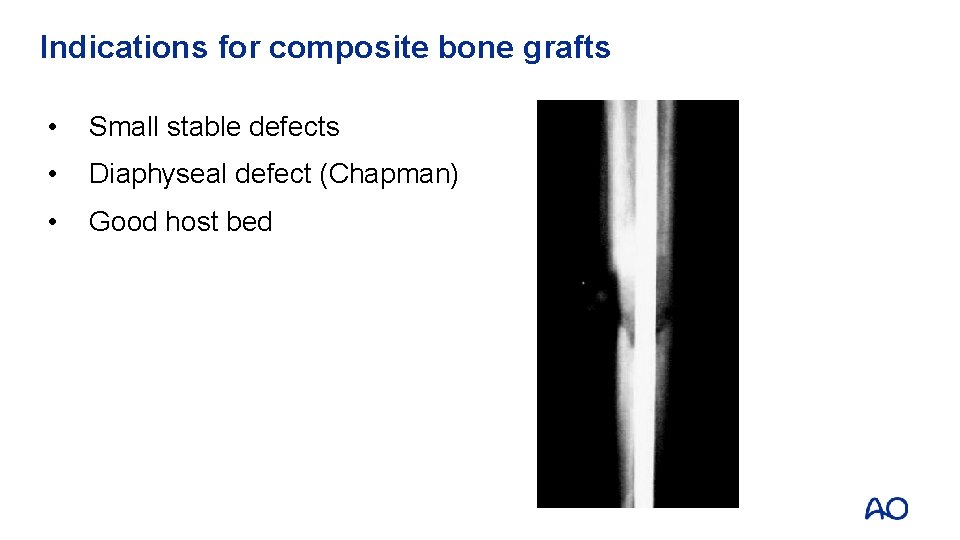
Indications for composite bone grafts • Small stable defects • Diaphyseal defect (Chapman) • Good host bed

Ideal bone graft substitute—composite grafts • Biocompatable • Bioresorbable • Osteoconductive • Osteoinductive • Structural • Easy to use • Cost effective
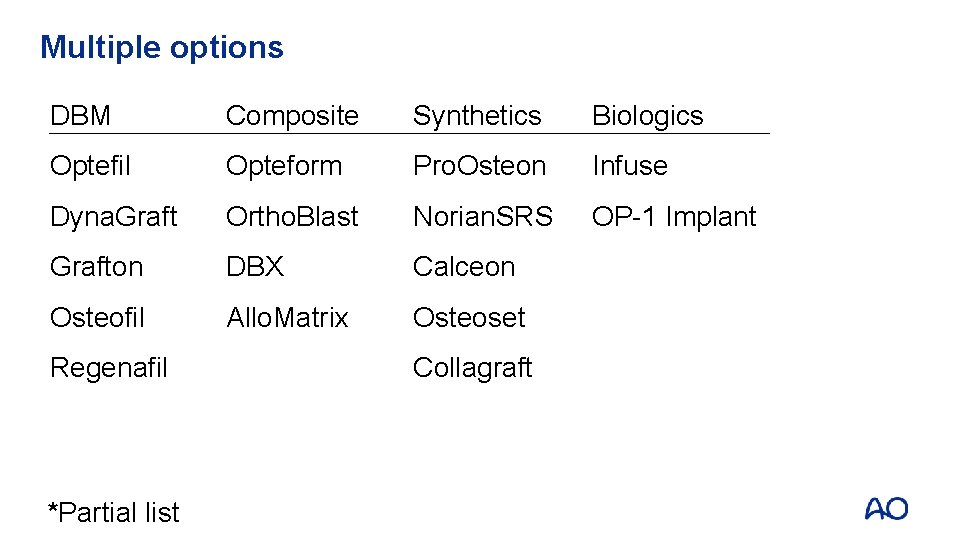

Multiple options DBM Composite Synthetics Biologics Optefil Opteform Pro. Osteon Infuse Dyna. Graft Ortho. Blast Norian. SRS OP-1 Implant Grafton DBX Calceon Osteofil Allo. Matrix Osteoset Regenafil *Partial list Collagraft

Take-home messages • Autograft is the “gold standard” for a good reason • All others are a potential compromise • Must understand the mechanism of graft incorporation and healing problems • Graft must contain “missing factors” • Biologics and composites are promising • A perfect substitute is not yet available
- Slides: 44