Boltons Five Year Plan for Reform Transformational Bid

Bolton’s Five Year Plan for Reform Transformational Bid Update Health & Wellbeing Board
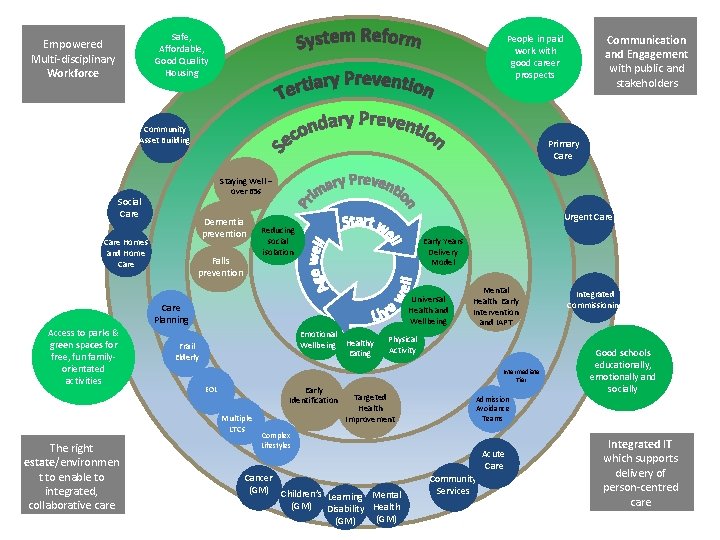
Safe, Affordable, Good Quality Housing Empowered Multi-disciplinary Workforce Community Asset Building Primary Care Staying Well – over 65 s Social Care Dementia prevention Care Homes and Home Care Falls prevention Urgent Care Reducing social isolation Early Years Delivery Model Universal Health and Wellbeing Care Planning Access to parks & green spaces for free, fun familyorientated activities Emotional Wellbeing Healthy Eating Frail Elderly Mental Health Early Intervention and IAPT Physical Activity Intermediate Tier Early Identification EOL Multiple LTCs The right estate/environmen t to enable to integrated, collaborative care Communication and Engagement with public and stakeholders People in paid work with good career prospects Targeted Health Improvement Good schools educationally, emotionally and socially Admission Avoidance Teams Complex Lifestyles Cancer (GM) Children’s Learning Mental (GM) Disability Health (GM) Integrated Commissioning Acute Care Community Services Integrated IT which supports delivery of person-centred care

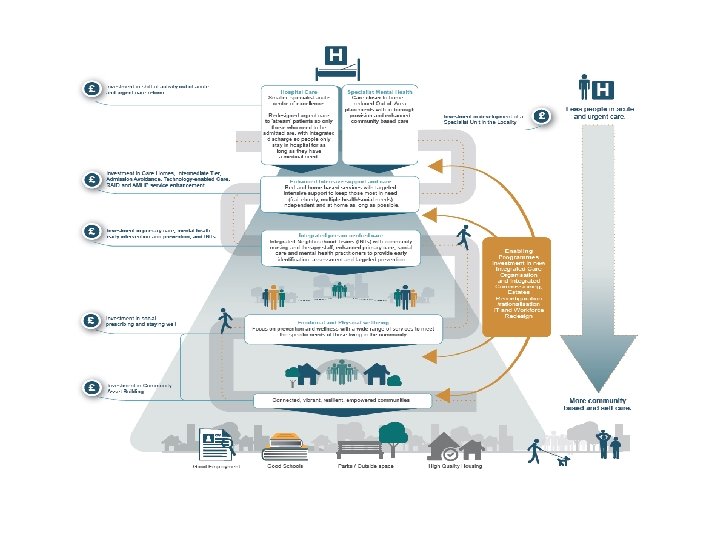
Themed areas of development Population level prevention and health improvement -The establishment of a Bolton Strategic Partnership for Prevention and Health Improvement Building upon Staying Well offer - Development of a locally recruited, preventative workforce comprising of Community Asset Navigators/Builders, and expansion of the voluntary sector to meet the needs of local communities. The Health Improvement Practitioners (HIPs) role will be instrumental in population physical and mental wellbeing. Expansion of falls prevention and Social isolation prevention. Primary care - A redesigned primary care workforce fit for 2020. This new workforce will provide the right professional to address patient’s initial health need and will include direct access to first line assessment and intervention for mental health (10 Mental Health Practitioners), musculoskeletal (10 MSK practitioners) and medication review (10 Pharmacists). More initiatives in primary care to support early identification so we can find the missing 1, 000 s. Primary, secondary and tertiary prevention are key to driving the significant improvements in health and wellbeing for everyone in Bolton. Health Improvement Practitioners (HIP) working in GP practice and local community settings are key to this.

Technology Enabled Care - Technology enabled care allows people to remain independent and mitigate and reduce risks (rather than relying on traditional care packages such as home care delivered by a health or care assistant). This is achieved by aids and equipment to allow people, their carers and families and in care homes to monitor their own health and wellbeing through the use of falls alarms, medication dispensers, remote health monitoring and other similar devices. Targeted support to compliment; Home Care, Residential Care (Dementia), Supported living and Extra Care Homes - scheme is aimed at enhancing the quality of care provided in care homes to reduce the number of unplanned, avoidable hospital admissions (primarily due to falls, UTIs and dementia/delirium) and a reduction in length of stay when care home residents do end up in hospital. This programme has a multi-faceted approach which is integrated across primary, community health and social care and hospital care.

Urgent Care - Development of an alternative workforce (health and social care) to reduce emergency admissions, improve flow, reduce delayed transfers of care, ensure full use of the SAFER metrics There will also be an expansion of the Ambulatory Care service to 7 days per week with expanded hours and Streaming from ED (front end clinical decision maker for directing all ED attenders to the most appropriate place (and person) to deliver the care needed, including the patient’s own GP for appropriate conditions/presentations to include co-location of Out of Hours within the ED There are proposals to expand Intermediate Tier to deliver the “Discharge to Assess” model of care that will include beds outside of the hospital and how an intensive support at home service can be developed. Fracture Liaison Service developments

Acute reconfiguration - Specialist medical care will not be confined to inside the hospital walls; specialist teams will work closely with GPs and those working in social care to make sure that patients have swift access to specialist care when they need it, wherever they need it. Much specialised care will be delivered in or close to the patient’s home. Developments being considered; • • • Virtual Respiratory Clinics within Primary Care Rapid access clinics Community Heart Failure Team Heart Failure Rehab Service Enhancement of Integrated Neighbourhood teams Standardisation of care Mental Health - considered as a key strand through all themes to improve Mental wellbeing. Targeted scheme developments consider; RAID service to be all age, CMAHS redesign, IAPT/Early Intervention and Prevention, expansion of memory and Dementia services as well as specific in borough developments for specialist patients support.
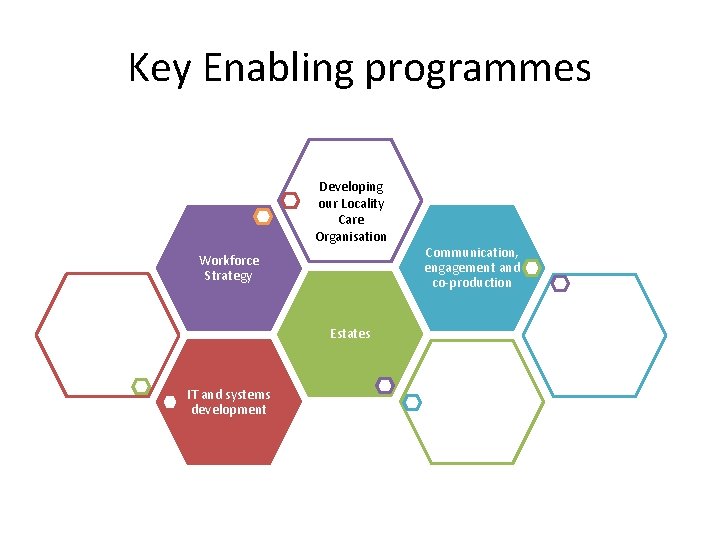
Key Enabling programmes Developing our Locality Care Organisation Workforce Strategy Estates IT and systems development Communication, engagement and co-production

Progress and Next Steps • GM Advisory session completed with steering group • Cost & benefit and scheme details being finalised • Governance for sign off being completed • HWBB part B item November • GM evaluation 6 -8 weeks before final submission anticipated December 2016.
- Slides: 9