Body Fluids Objectives By the end of the

Body Fluids

Objectives � By the end of the sessions the students should be able to: � Classify body fluid compartments � Recall the indicator that is used to measure the volume of a body compartment and explain the principle involved in measuring the volume. � Estimate the changes in ECF & IFC osmolarity and volumes in clinically relevant conditions. � Measure interstitial fluid volume and ICF volume

Total body water � Total Body Water (TBW) = 60% (50 to 70) of body weight; depends on fatty tissue. � The 70 kg 'standard male' contains 42 liters of water - 60 -65% of his body weight. � Adult female contains 55% of her body weight as water due to a higher fat content.

Total body water (cont’d) � TBW is highest in the newborn (80 - 85%) , child (75%) � Total body water as a percentage of total body weight decreases progressively with increasing age. � By the age of 60 years, total body water (TBW) has decreased to only 45 -50% of total body weight.

ECF & ICF � The major division is based on which side of the cell membrane the fluid lies � Intracellular Fluid (ICF: approximately 2/3 of total body water) � Extracellular Fluid (ECF: approximately 1/3 of total body water).
![Plasma [about 1/4 th of ECF volume] Interstitial Fluid [ISF]; About 3/4 th of Plasma [about 1/4 th of ECF volume] Interstitial Fluid [ISF]; About 3/4 th of](http://slidetodoc.com/presentation_image/28ee248f1d300b8d722f45724431941f/image-6.jpg)
Plasma [about 1/4 th of ECF volume] Interstitial Fluid [ISF]; About 3/4 th of ECF volume Intracellular Fluid [ICF]; 2/3 of total body water is inside cells ECF
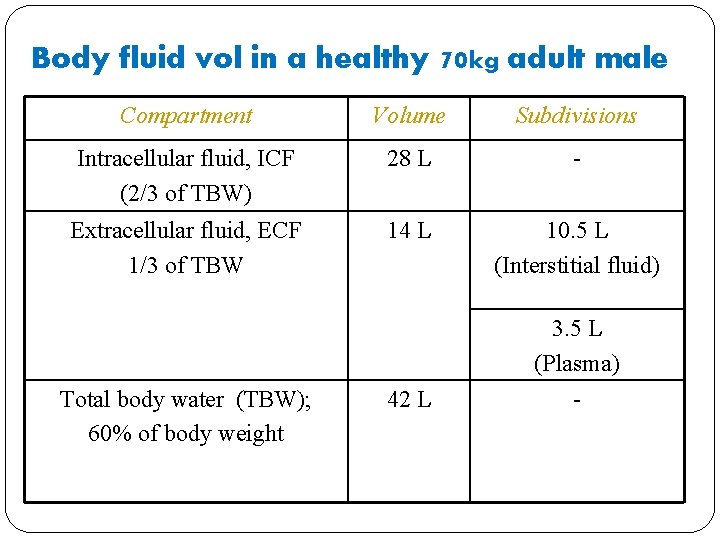

Body fluid vol in a healthy 70 kg adult male Compartment Volume Subdivisions Intracellular fluid, ICF (2/3 of TBW) 28 L - Extracellular fluid, ECF 1/3 of TBW 14 L 10. 5 L (Interstitial fluid) Total body water (TBW); 60% of body weight 42 L 3. 5 L (Plasma) -

Intracellular Fluid � Water forms about 75 - 80% � The major cations are K+ and Mg 2+ � The major anions are protein and organic phosphates such as ATP, ADP and AMP; � p. H of ICF is 6. 8 - 7. 4 in dependence on the metabolic processes;

Extracellular Fluid � Water constitutes about 93% of the plasma compartment � The major cation is Na+; � The major anions are Cl- and HCO 3 -; � The ions in ECF determine osmotic pressure and p. H of the inner environment; � p. H of ECF is 7. 4

Trans-cellular water �is a compartment of ECW. Divided from the others by capillary endothelia and by epithelia. Plasma � Comprises 1/4 of the ECF � It is therefore 1/12 of TBW � The major plasma proteins are albumin and globulins

Interstitial fluid � Comprises 3/4 of the ECF; � It is 1/4 of TBW � The composition is the same as plasma except it has little protein thus, interstitial fluid is an micro filtrate of plasma.

Net Osmotic Force Development � Through Semi-permeable membrane � Movement of some solute obstructed � H 2 O (solvent) crosses freely across membrane � End point: �Water moves until solute concentration on both sides of the membrane is equal �OR, an opposing force prevents further movement
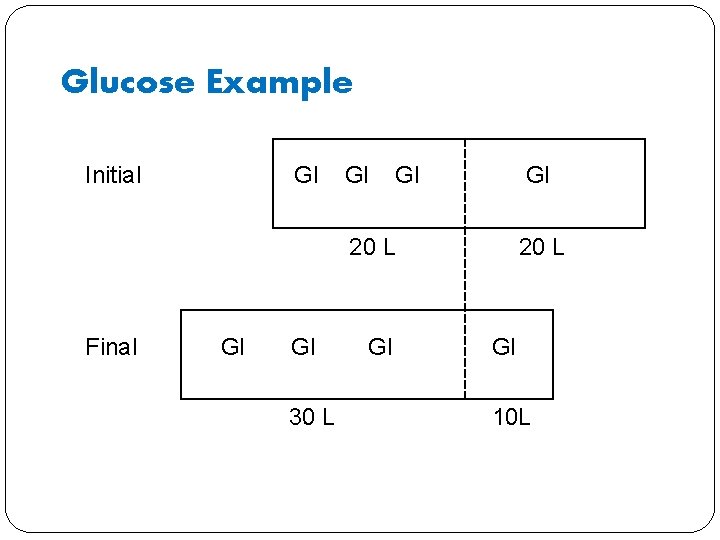
Glucose Example Initial Gl Gl Gl 20 L Final Gl Gl 30 L 20 L Gl 10 L

ICF Vs ECF � The two compartments are separated by cell membrane which is freely permeable to water � In a steady state ECF and ICF osmolarity is same i. e around 300 milliosmoles.

ICF Vs ECF � Effective osmolarity: The difference in the concentration of impermeable particles determines the osmotic movement of water across the membrane. � Na. Cl represents most of the effective osmolarity of ECF � Plasma proteins which determines the effective osmolarity between interstitial and plasma fluid

Principles of Body Water Distribution � Body control systems regulate ingestion and excretion: � constant total body water � constant total body osmolarity � Osmolarity is identical in all body fluid compartments (steady state conditions) � Body water will redistribute itself as necessary to accomplish this

Shifts of water between compartments � Water shifts between ECF and ICF so that the osmolarity of the two compartments become equal � The osmolarity of ICF and ECF are assumed to be equal after a brief period of equilibration

� It is important to understand how body osmolarity and ICV and ECV change in clinically relevant situation. � Darrow-Yannet Diagram shows the osmolarity and volume changes of body fluids. �X axis represents volume. �Y axis represents solute concentration.
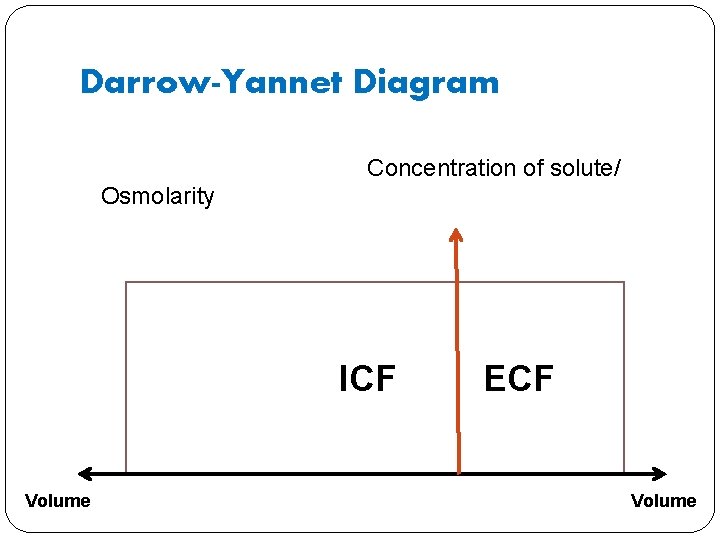
Darrow-Yannet Diagram Concentration of solute/ Osmolarity ICF Volume ECF Volume

Remember: � All volume disturbances originate in the ECF compartment. � When there is a net gain of fluid by the body, ECF always enlarges. � A net loss of body fluid decreases extracellular volume.

Remember: � Changes in ICF are in response to changes in ECF. � Intracellular volume varies with the effective osmolarity of the extracellular compartment. � An increase in extracellular osmolarity decreases intracellular volume and the opposite occurs with the decrease in extracellular osmolarity.

How to make the graph in your head �Step 1. �Figure out what happens to the osmolarity and volume in the ECF compartment (ECF is the smaller compartment) �Step 2. �Think how is ICF affected?

Problems � Loss of whole blood � Adult diarrhea � Infusion of excessive isotonic saline � Loop diuretics � Addison's disease � Syndrome of inappropriate ADH secretion � Insensible water loss in fever, � Diabetes insipidus, � Alcohol. � Excessive intake of Na. Cl
Loss of whole blood & Adult Diarrhea � What will happen to volume in ECF compartment? � It will decrease. � What will happen to osmolarity in ECF compartment? � It will not change because Isotonic fluid is lost � What will happen to ICF volume and osmolarity? � No osmotic gradient, therefore, will not change � What will happen to plasma protein and haematocrit � Plasma protein concentration and Haematocrit increase because of the loss of ECF
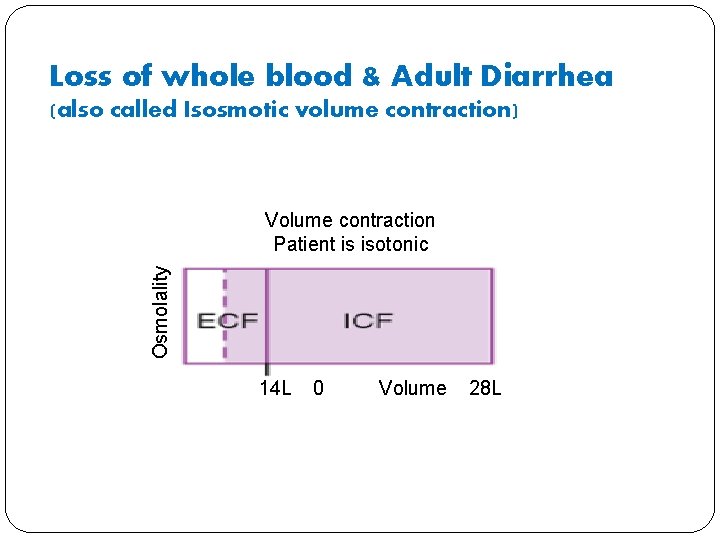
Loss of whole blood & Adult Diarrhea (also called Isosmotic volume contraction) Osmolality Volume contraction Patient is isotonic 14 L 0 Volume 28 L

Infusion of excessive isotonic saline � What will happen to volume in ECF compartment? � It will increase. � What will happen to osmolarity in ECF compartment? � It will not change because Isotonic fluid is lost. � What will happen to ICF volume and osmolarity? � No osmotic gradient, therefore, will not change. � What will happen to plasma protein and haematocrit � Plasma protein concentration and haematocrit decrease because of addition of the fluid
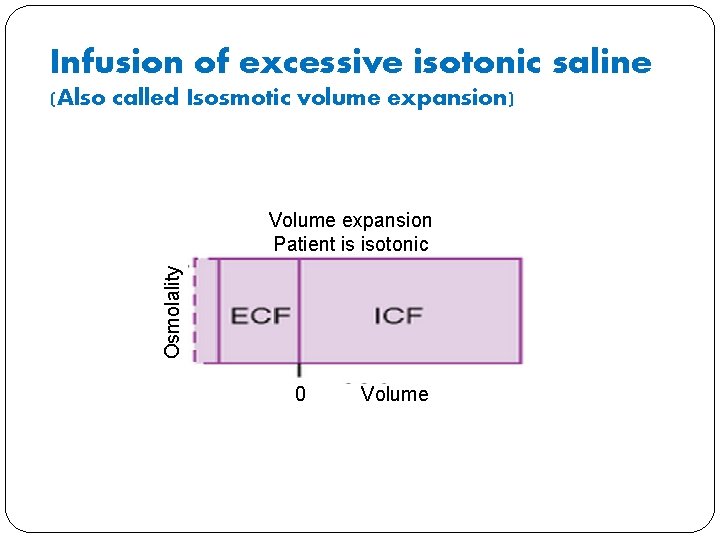
Infusion of excessive isotonic saline (Also called Isosmotic volume expansion) Osmolality Volume expansion Patient is isotonic 0 Volume

Loop diuretics & Addison's disease � Loops make you lose sodium and water, but more of sodium than water. � Addison's disease is adrenal insufficiency. � Aldosterone makes you retain sodium so in the absence of aldosterone, you will lose sodium.

Loop diuretics & Addison's disease � What will happen to osmolarity in ECF compartment? � It will decrease because the kidneys lose more Na. Cl than water � What will happen to volume in ECF compartment? � It will decrease because water shifts into the cells and ICF osmolarity decreases until it equals ECF osmolarity � What will happen to ICF volume? � It will increase. (Decrease in osmolarity shifts the fluid into ICF) � What will happen to plasma protein and haematocrit � Protein concentration and haematocrit increases because of the decrease in ECF volume
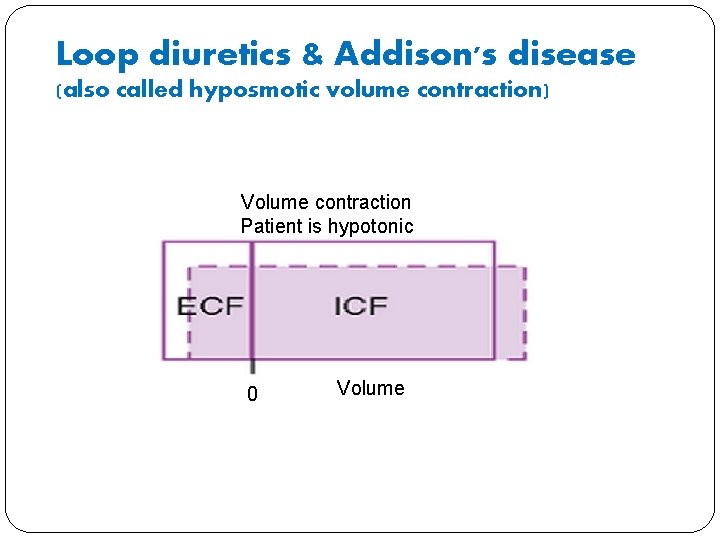
Loop diuretics & Addison's disease (also called hyposmotic volume contraction) Volume contraction Patient is hypotonic 0 Volume

Syndrome of inappropriate ADH secretion (also called hyposmotic volume expansion). Compulsive water drinker � SIADH: You are conserving too much water due to ADH. � Water drinker: You are having too much water

Syndrome of inappropriate ADH secretion. � What will happen to osmolarity in ECF compartment? � It will decrease because of retention of excess water � What will happen to volume in ECF compartment? � It will increase because of water retention � What will happen to ICF volume? � It will increase. (Decrease in osmolarity shifts the fluid into ICF) � What will happen to plasma protein and haematocrit � Protein concentration decreases because of an increase in ECF volume and haematocrit is unchanged because water shifts into the red blood cells increasing their volume
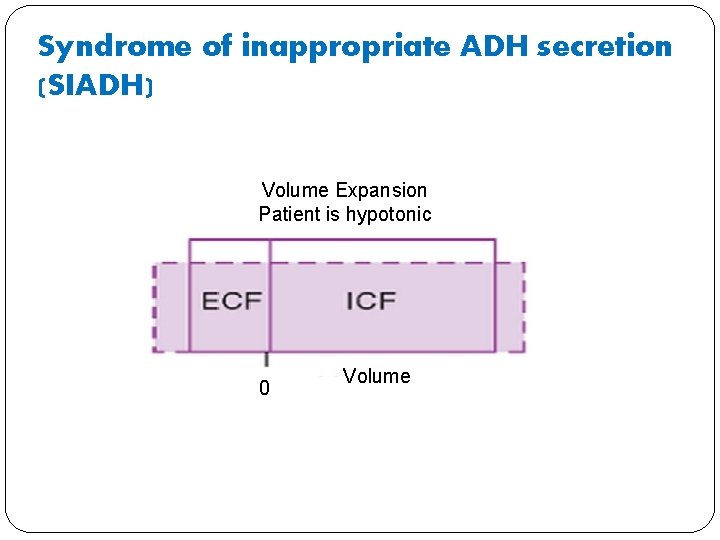
Syndrome of inappropriate ADH secretion (SIADH) Volume Expansion Patient is hypotonic 0 Volume

Sweating in a HOT desert � What will happen to volume in ECF compartment? It will decrease because of the loss of sweat � What will happen to osmolarity in ECF compartment? � It will increase because sweat is hyperosmotic, relatively more water than salt is lost during sweating � What will happen to ICF volume? � It will decrease because ICF osmolarity increases until it is equal to ECF osmolarity � What will happen to plasma protein and haematocrit � protein concentration increases because of the loss if ICF volume and Haematocrit may increase but it is unchanged because water shifts from erythrocytes which decrease their volume
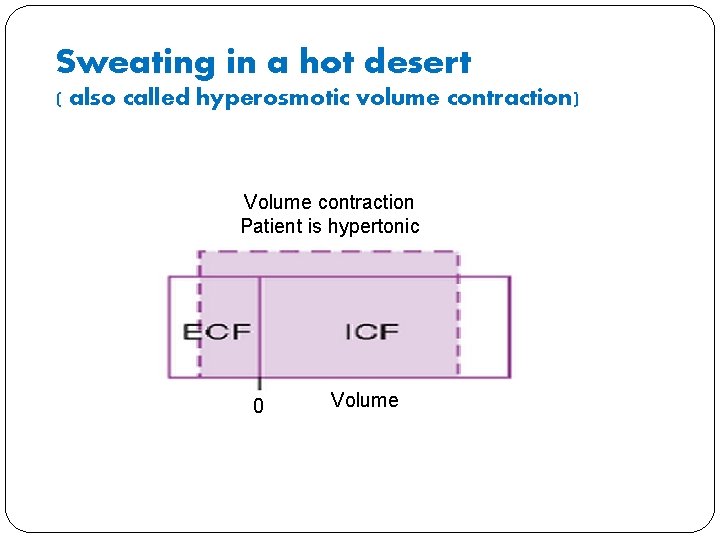
Sweating in a hot desert ( also called hyperosmotic volume contraction) Volume contraction Patient is hypertonic 0 Volume

Insensible water loss in fever or Diabetes Insipidus or Alcohol � What will happen to volume in ECF compartment? � It will decrease because water is lost in all these conditions such as ADH action is lost in Diabetes insipidus, alcohol inhibits pituitary secretion of ADH, water evaporates from the warm skin surface in fever) � What will happen to osmolarity in ECF compartment? � It will increase as fluid loss is hypotonic � What will happen to ICF volume? � It will decrease because ICF osmolarity increases until it is equal to ECF osmolarity
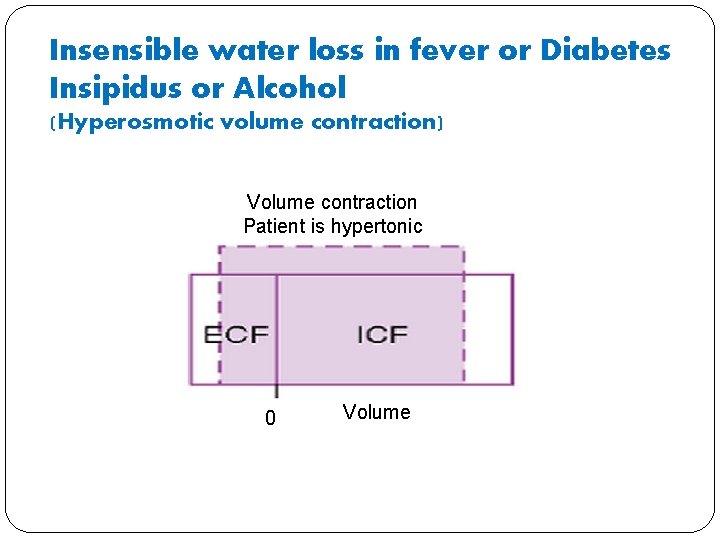
Insensible water loss in fever or Diabetes Insipidus or Alcohol (Hyperosmotic volume contraction) Volume contraction Patient is hypertonic 0 Volume

Excessive intake of Na. Cl or Infusion of sodium containing antibiotics � What will happen to osmolarity in ECF compartment? � It will increase because there has been an addition of osmoles to the ECF � What will happen to volume in ECF compartment? � Will increase because fluid moves from the ICF to ECF) � What will happen to ICF volume? � It will decrease.
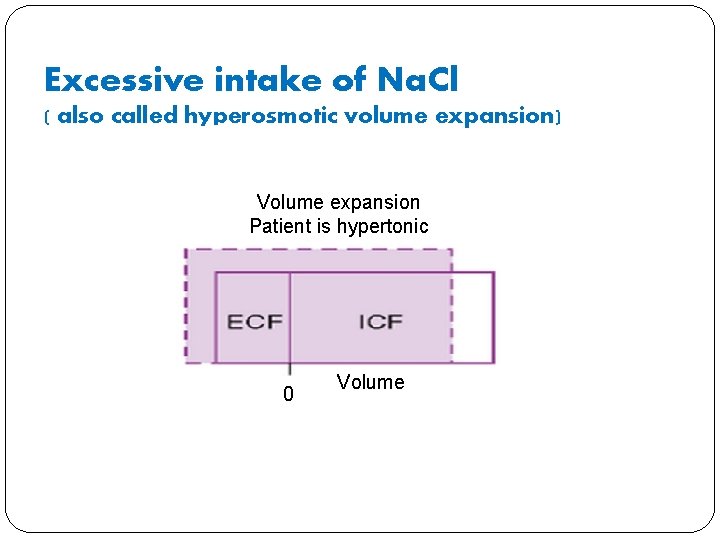
Excessive intake of Na. Cl ( also called hyperosmotic volume expansion) Volume expansion Patient is hypertonic 0 Volume

� What will happen if a person running a marathon replaces all the volume lost in sweat by drinking water? � What will happen to total body volume? � Will remain the same because all the volume lost will be replaced by drinking water � What will happen to osmolarity in ECF compartment? � It will decrease only salt is loss as water loss has been replaced � What will happen to volume in ECF compartment? � It will decrease because water will shift from ECF to ICF � What will happen to ICF volume? � It will increase What will happen to osmolarity in ICF compartment? It will decrease
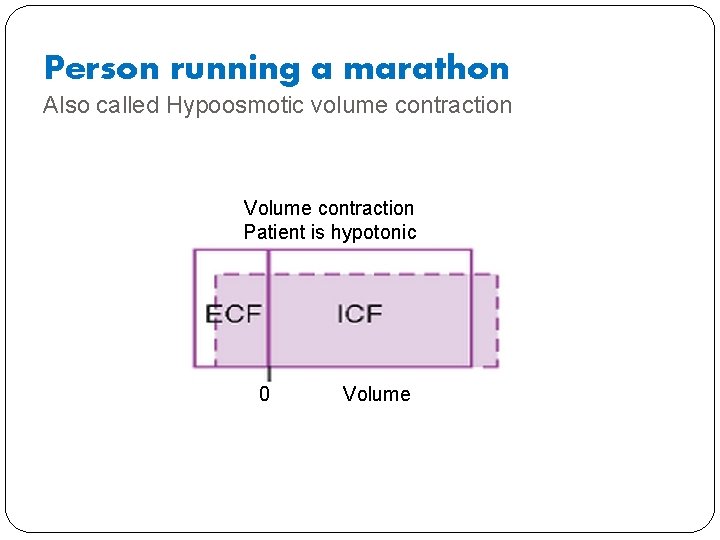
Person running a marathon Also called Hypoosmotic volume contraction Volume contraction Patient is hypotonic 0 Volume

Measuring body fluid volumes: � Principle: Indicator-dilution principle � Method: � Administer a known amount (A) of a substance that will get distributed in a particular body fluid compartment; � Determine the final steady state concentration (C) of this indicator in blood; � Volume of distribution Vd of the indicator = Amount of indicator injected (A) Concentration in blood after mixing (C)
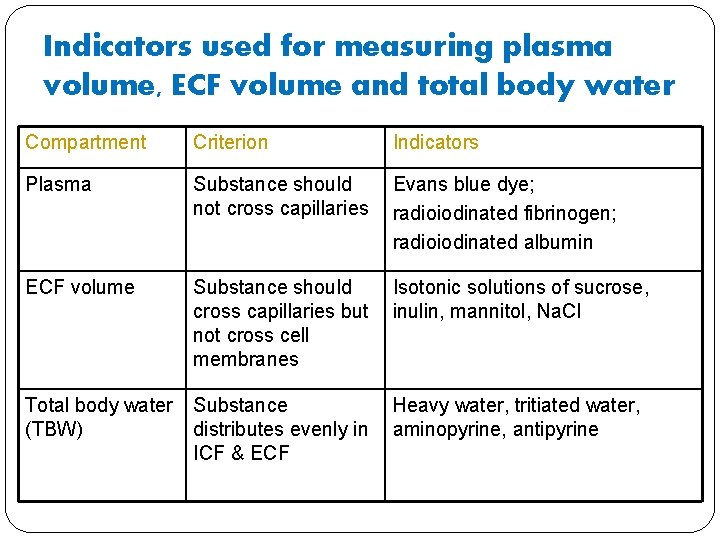

Indicators used for measuring plasma volume, ECF volume and total body water Compartment Criterion Indicators Plasma Substance should not cross capillaries Evans blue dye; radioiodinated fibrinogen; radioiodinated albumin ECF volume Substance should Isotonic solutions of sucrose, cross capillaries but inulin, mannitol, Na. Cl not cross cell membranes Total body water Substance Heavy water, tritiated water, (TBW) distributes evenly in aminopyrine, antipyrine ICF & ECF

Recall � How would you measure interstitial fluid (ISF) volume? � Cannot be measured; it is calculated (estimated) by � ISF volume = ECF volume – plasma volume � How would you measure ICF volume? � Cannot be measured; it is calculated (estimated) by � ICF volume = Total body water – ECF volume

� Blood volume can be calculated (estimated) as: � Blood volume = plasma volume × (100/100 -Hct) � In a healthy 70 kg adult male, plasma volume (measured using the Evans Blue dye) was found to be 3300 ml. Hematocrit was 40%. Calculate his blood volume. A. 5000 ml B. 5200 ml C. 5500 ml D. 5600 ml

References � BARRETT, K. E. , S. M. BARMAN, et al. (2010). Ganong’s Review of Medical Physiology, The Mc. Graw-Hill Companies, Inc. � Guyton, A. C. (2011). Textbook of Medical Physiology Elsevier Inc. � Costanzo, L. S. (2013). Body Fluids. Physiology, Elsevier. � Dunn, R. B. (2010). USMLE Step 1 Physiology Lecture Notes, Kaplan Medical. � Agro, F. E. and M. Vennari (2012). Body Fluid Management: From Physiology to Therapy, Springer. � Koeppen, B. M. and B. A. Stanton (2012). Renal Physiology, ELSEVIER MOSBY.

Thank you
- Slides: 47