Body Fluids and Infectious Complications Body Fluids Intracellular

Body Fluids and Infectious Complications
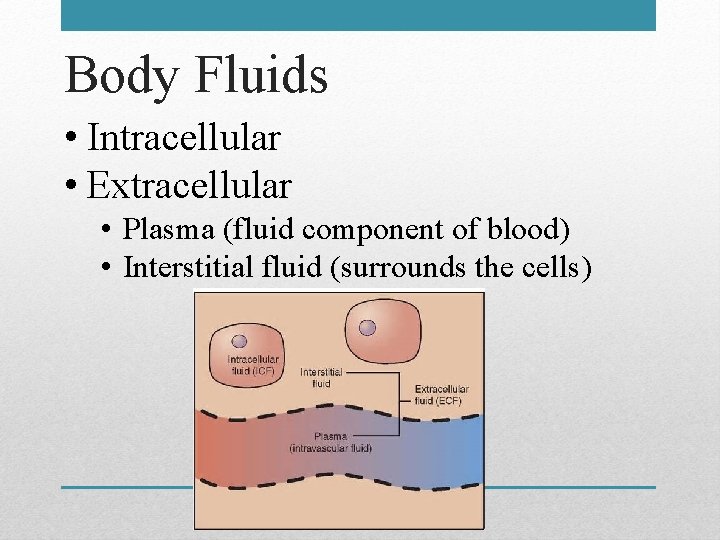
Body Fluids • Intracellular • Extracellular • Plasma (fluid component of blood) • Interstitial fluid (surrounds the cells)
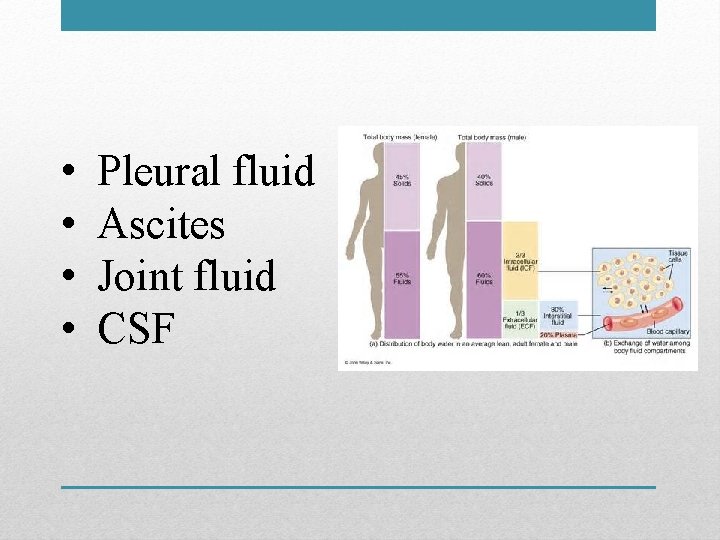
• • Pleural fluid Ascites Joint fluid CSF
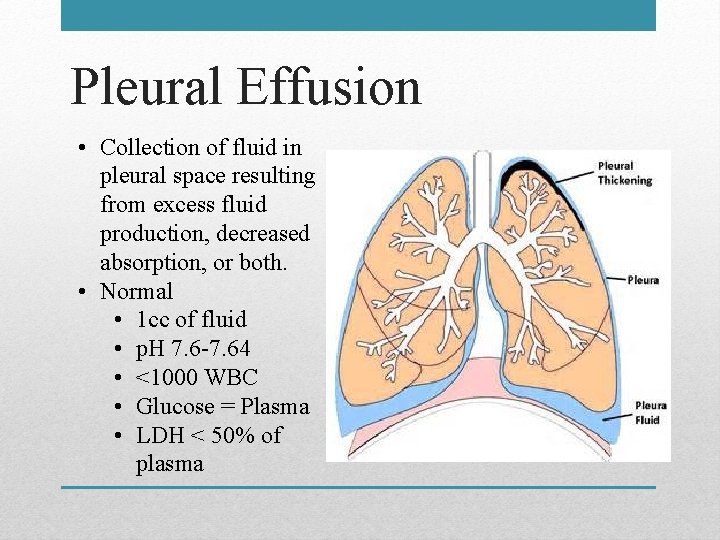
Pleural Effusion • Collection of fluid in pleural space resulting from excess fluid production, decreased absorption, or both. • Normal • 1 cc of fluid • p. H 7. 6 -7. 64 • <1000 WBC • Glucose = Plasma • LDH < 50% of plasma
Pleural Effusion • Most common causes • Cardiac Failure • Pneumonia • Malignancy • 20 -40% of pneumonias will develop an infected pleural effusion

Transudate • Due to imbalance in oncotic/hydrostatic pressures • p. H > 7. 2 • LDH <200 • Glucose >60 • Common causes • CHF • Cirrhosis • Hypoalbuminemia Exudate • Due to inflammation or decreased lymphatic drainage • p. H <7. 2 • LDH >3 x normal • Glucose ≤ 60 • Common Causes • • Pneumonia Malignancy Pancreatitis Collagen-Vascular disorders

Light et al. criteria • Exudate if: • LDH > 2/3 upper limit of nl serum value • Pleural: Serum LDH >. 6 • Pleural: Serum Protein >. 5
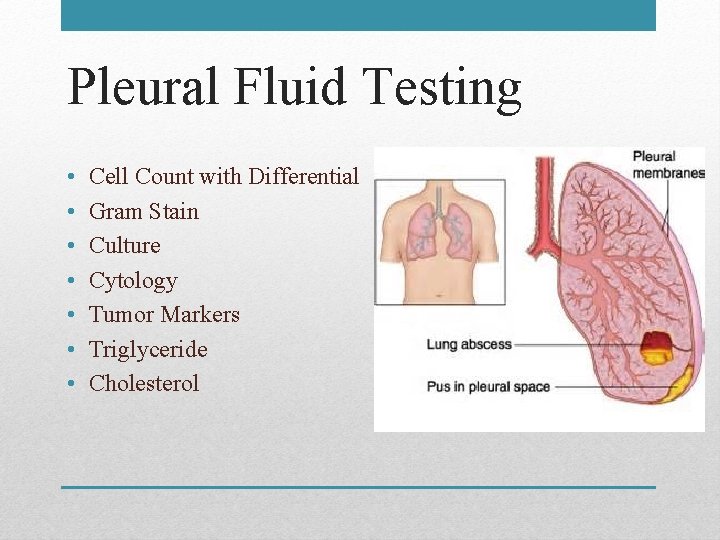
Pleural Fluid Testing • • Cell Count with Differential Gram Stain Culture Cytology Tumor Markers Triglyceride Cholesterol

Ascites

Abdominal Fluid • Common Causes of Ascites • Cirrhosis (80% of cases) • Malignancy • Heart Failure • Can develop over days or months

Paracentesis • Essential to determine diagnosis and to rule out or confirm spontaneous bacterial peritonitis (SBP) • In presence of SBP, mortality delay of paracentesis by 3. 3%/hr • Is infection present? Is portal HTN present? • • Appearance (clear, bloody, cloudy, milky) Serum: Ascites albumin gradient (SAAG) Cell count & differential Total protein
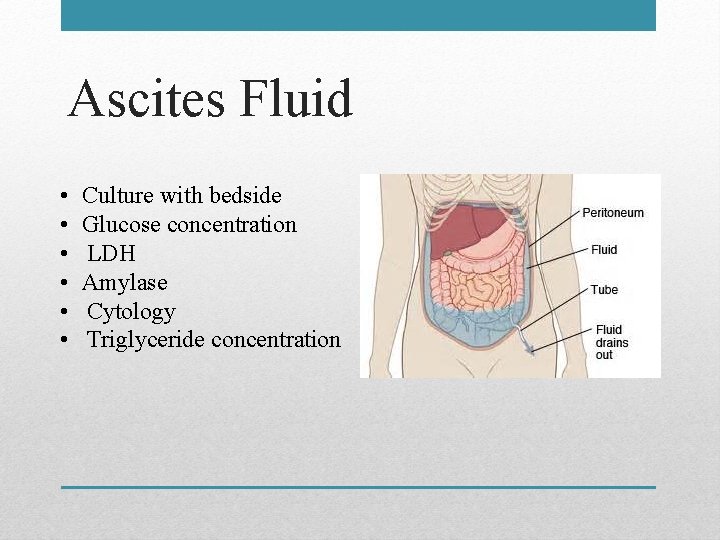
Ascites Fluid • • • Culture with bedside Glucose concentration LDH Amylase Cytology Triglyceride concentration

Ascites Fluid • Appearance • • • Clear (uncomplicated) Cloudy (infected) Milky (chylous / malignant) Bloody (traumatic tap / cirrhosis / malignancy) Brown (high bilirubin concentration) • SAAG • Identifies presence of portal HTN • Ascites fluid albumin – serum albumin • ≥ 1. 1 g/d. L = portal HTN

Ascites Fluid • Cell count & differential • >250 WBC = consider infection • Needs corrected in bloody taps • WBC # - 1 for every 750 RBCs • Neutrophil # - 1 for every 250 RBCs • Protein • ≥ 2. 5 -3 g/d. L = exudate • < 2. 5 g/d. L = transudate • < 1 g/d. L = high risk of SBP • LDH (ascitic fluid/serum ratio) • ~. 4 = uncomplicated, likely due to cirrhosis • ~ 1. 0 = SBP • Amylase • ~2000 int. unit/L = pancreatic ascites
Septic Arthritis
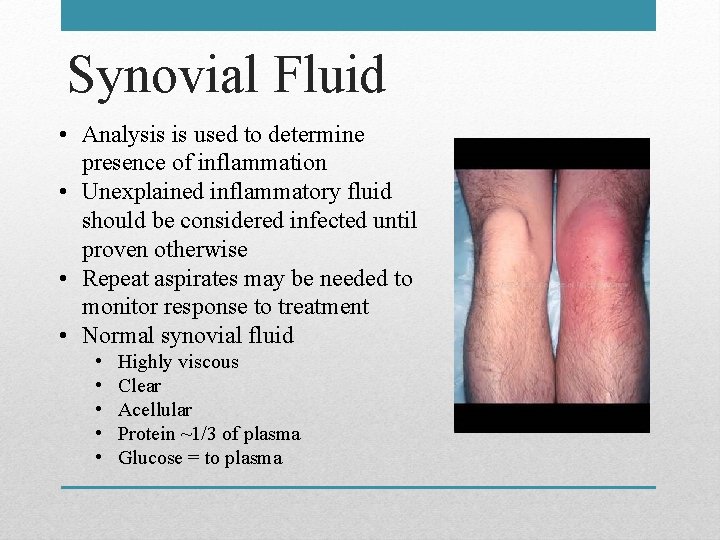
Synovial Fluid • Analysis is used to determine presence of inflammation • Unexplained inflammatory fluid should be considered infected until proven otherwise • Repeat aspirates may be needed to monitor response to treatment • Normal synovial fluid • • • Highly viscous Clear Acellular Protein ~1/3 of plasma Glucose = to plasma
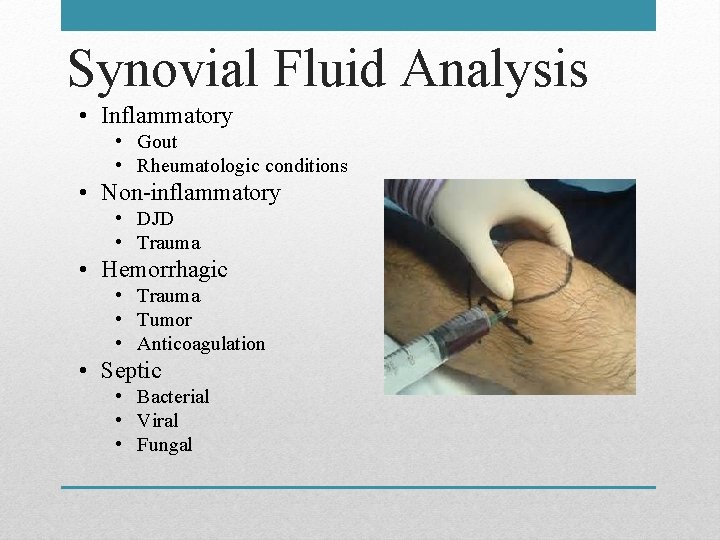
Synovial Fluid Analysis • Inflammatory • Gout • Rheumatologic conditions • Non-inflammatory • DJD • Trauma • Hemorrhagic • Trauma • Tumor • Anticoagulation • Septic • Bacterial • Viral • Fungal

Synovial Fluid Analysis • Cell count • < 2000 WBC = non-inflammatory • > 2000 WBC = inflammatory • 50 k – 150 k WBC = bacterial • • Crystals Gram stain & Culture Cytology Lower WBC counts can do not rule out infection. • Septic joints can coincide with inflammatory “gouty” joints.
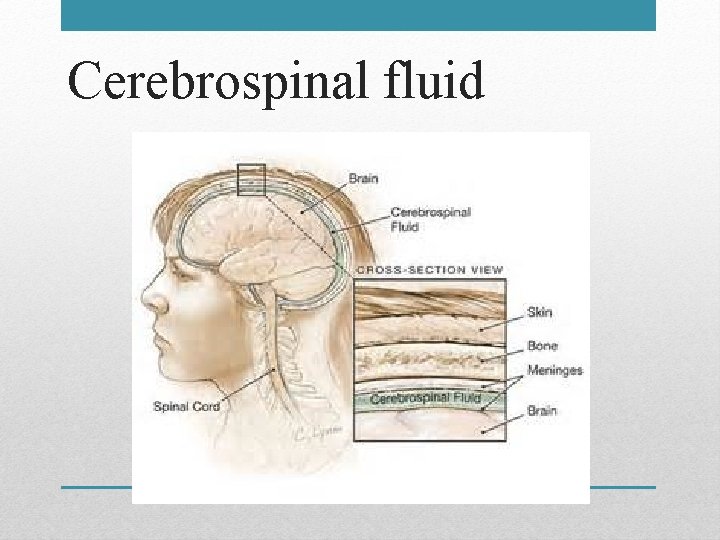
Cerebrospinal fluid
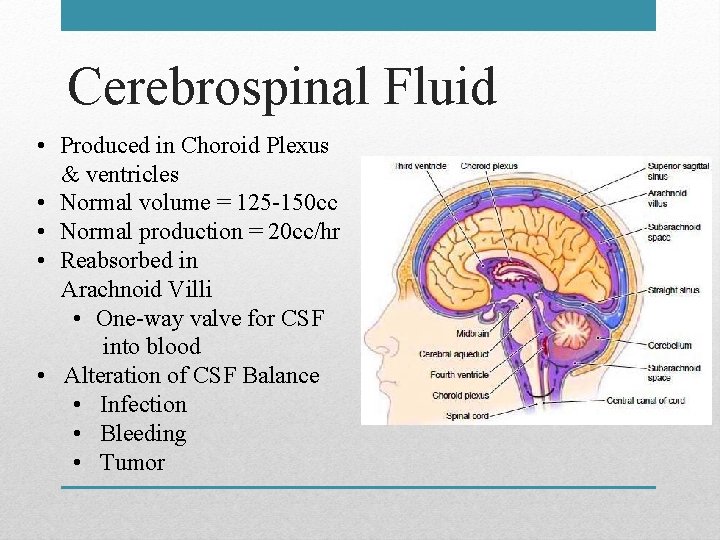
Cerebrospinal Fluid • Produced in Choroid Plexus & ventricles • Normal volume = 125 -150 cc • Normal production = 20 cc/hr • Reabsorbed in Arachnoid Villi • One-way valve for CSF into blood • Alteration of CSF Balance • Infection • Bleeding • Tumor

Meningitis • Inflammation of meninges (tissue surrounding the brain and spinal cord) • Bacteria enter through blood-brain barrier • Bacteria rapidly replicate due to low concentration of immunoglobulins • Inflammatory response can lead to cerebral edema, increased ICP, and neuronal damage • Nuchal rigidity, Brudzinksi sign, Kernig sign • Viral / Aseptic / Bacterial
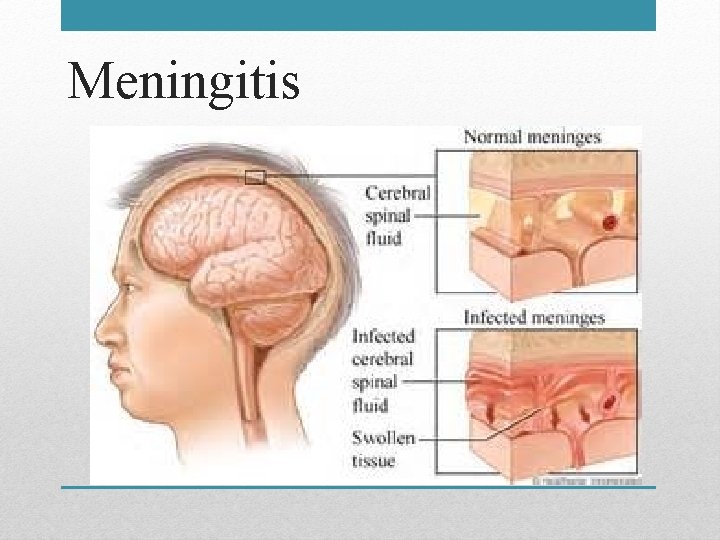
Meningitis
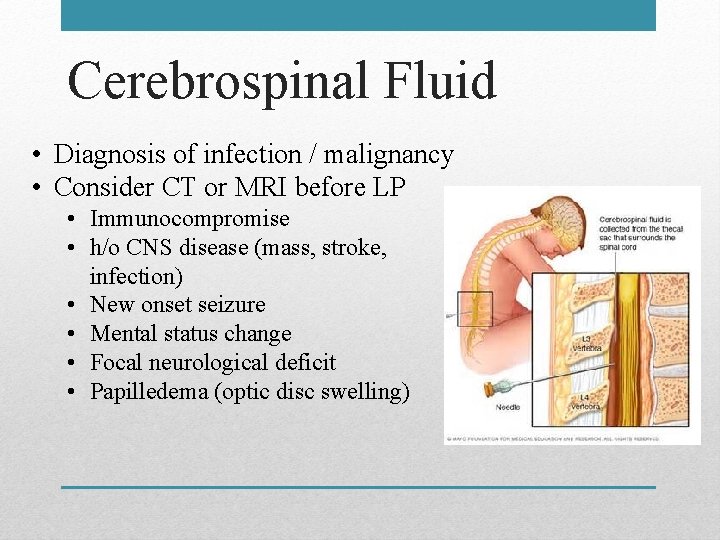
Cerebrospinal Fluid • Diagnosis of infection / malignancy • Consider CT or MRI before LP • Immunocompromise • h/o CNS disease (mass, stroke, infection) • New onset seizure • Mental status change • Focal neurological deficit • Papilledema (optic disc swelling)

CSF Composition • Clear & Colorless • Xanthochromia – discoloration of CSF due to RBC • WBC: 0 -5 • Increase WBC can be seen in infectious/non-infectious etiologies • RBC: 0 -5 • Protein: 20 -50 mg/d. L • Can be elevated by SAH, traumatic LP, infection, noninfectious etiologies (flow obstruction) • Glucose (CSF: Serum ratio): ~. 6 • Typically low in infections

Pleural Fluid Normal • p. H 7. 6 – 7. 64 • WBC <1000 • Glucose = Plasma • LDH <50% of plasma Exudate • • p. H < 7. 2 WBC >1000 Glucose < 60 LDH >3 x normal of plasma
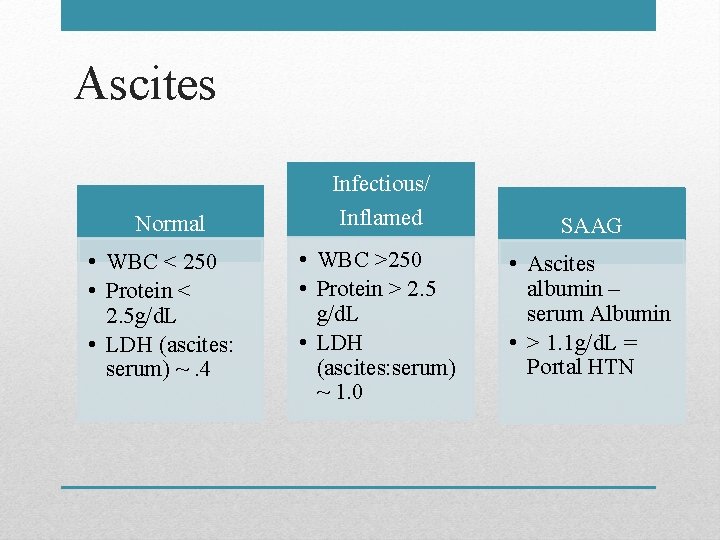
Ascites Normal • WBC < 250 • Protein < 2. 5 g/d. L • LDH (ascites: serum) ~. 4 Infectious/ Inflamed • WBC >250 • Protein > 2. 5 g/d. L • LDH (ascites: serum) ~ 1. 0 SAAG • Ascites albumin – serum Albumin • > 1. 1 g/d. L = Portal HTN

Synovial Fluid Infected Normal • WBC = none • WBC • <2000 = noninflammatory • >2000 = inflammatory • > 50 K = septic

CSF Normal • WBC 0 -5 • Glucose: CSF: Serum ratio = ~. 6 • Protein 20 -50 mg/d. L Abnormal • WBC = elevated • Glucose = decreased • Protein = elevated

Jessica Doiron, DNP, ANP-BC Washington University School of Medicine jdoiron@DOM. wustl. edu
- Slides: 29