Body Fluid Body fluid n The total body

Body Fluid

Body fluid n. The total body fluid is about 60% of the total body weight. n. In the average 70 kg body weight it is about 42 liters. n. Increase the percentage of fat in the body decreases the % of water. n. Women contain less water than men because have more body fat.
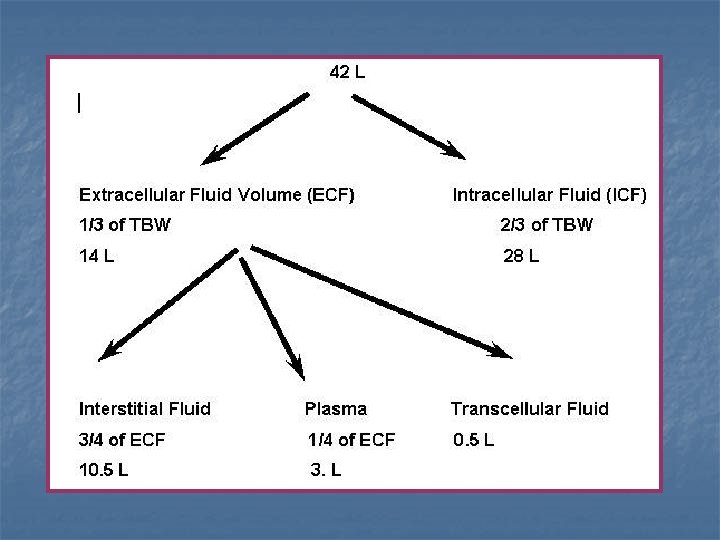

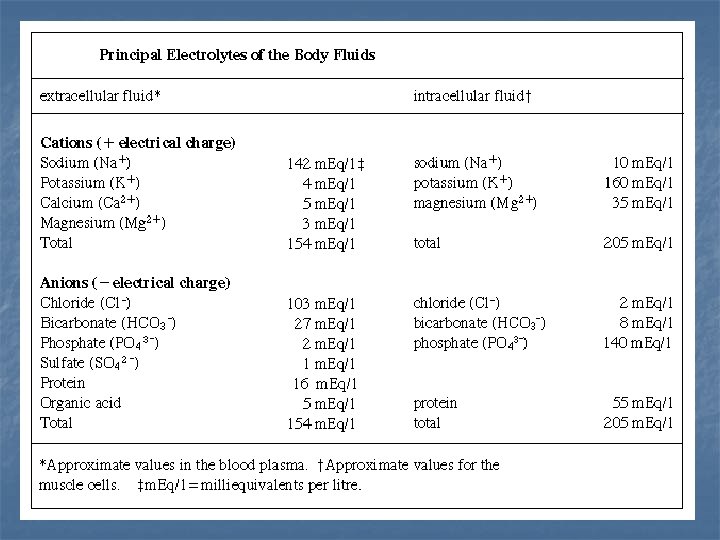
Body fluid compartment Extra cellular fluid : It is about 14 liters: nplasma 3 liters. n. Interstial fluid in spaces between cells 10 L n. Transcellular 1 -2 liters. n n n Intra ocular space Synovial , peritoneal , pericardial spaces. Cerebrospinal fluid.
Body fluid Intra cellular fluid n Equal 28 liters. n It is the fluid inside the cells. n It contains high Concentration of K &less concentration of Na. n Also it contains large amount of magnesium and phosphate.

Regulation of fluid transportation n n The most common routes for transporting materials to and from intracellular compartments are (the fluid and materials transport across semipermiable membrane) : 1 - osmosis 2 - diffusion 3 - active transport 4 - filtration

1 - Osmosis n Through the process of osmosis , the solvent , the water passes from an area of lesser solute concentration and more water to an area of greater solute concentration and less water until equilibrium is established.
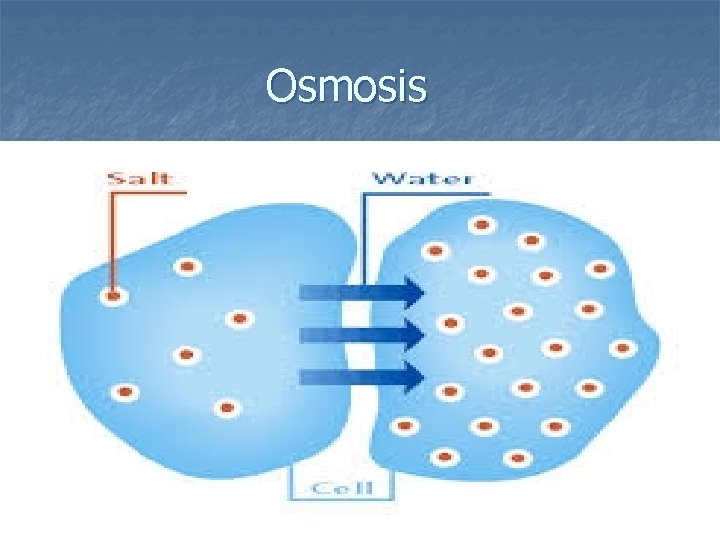
Osmosis

2 - Diffusion n Is the tendency of solute to move freely throughout a solvent. The solute (materials ) moves from an area of higher concentration to an area of lower concentration
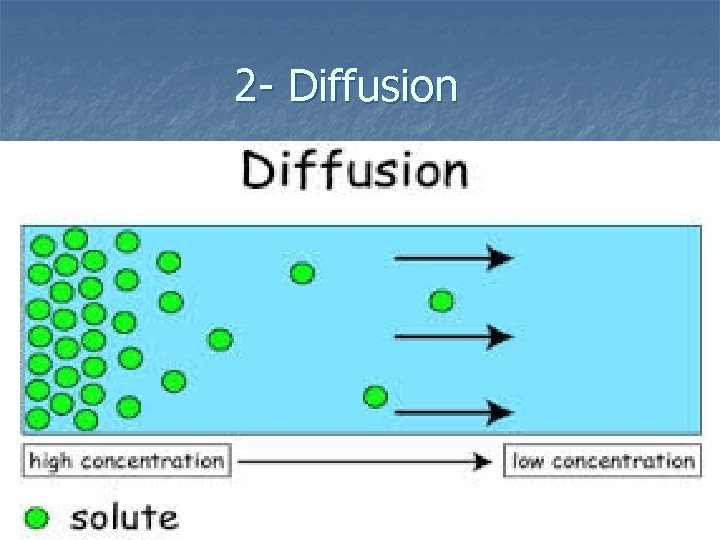
2 - Diffusion

3 - Active Transport n n Is a process that requires energy for the movement of substances through cell membrane from an area of lesser solute concentration to an area of higher solute concentration. Adenosine triphosphate (ATP) stored in all cells , is released from a cell and supplies energy for solute movements in and out of the cell.
4 - Filtration n Is the passage of fluid through a permeable membrane. Passage is from an area of high pressure to an area of lower pressure

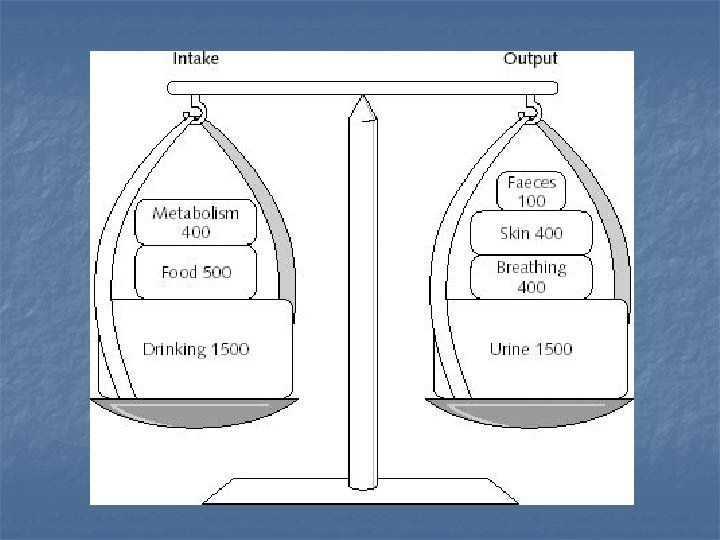
n. Daily Body water intake of water (by two main sources): Ingested in the form of water or liquid which add about 2100 ml/day to the body fluid n Synthesized as a result of metabolism and it is about 200 ml/day. n n. Daily loss of body water: Evaporation 700 ml n Urine 1400 ml n Sweat 100 ml n Feces 100 ml n

Types of Solutions 1. Isotonic solution n 2. Hypotonic solution n 3. The water concentration in IC&ECF is equal and solutes can not enter or leave the cell. There are less solutes less osmotic pressure so water enter the cell and it swell. Hypertonic solution n n High solutes , high osmotic pressure so water leave the cell and cell shrink. Solution of Na. CL 0. 9%and glucose 5%are isotonic so it is important in clinical medicine because the cell neither swell nor shrink.

Water Balance n. Is maintained in the body by adjusting water input and water output. n. Control of water input: Stimulated by thirst sensation. n Thirst sensation occurs as a result of: n Hypertonicity. n Hypovolemia. n

Water loss Drink Increase plasma osmolarity Stimulation of thirst center In Hypothalamus

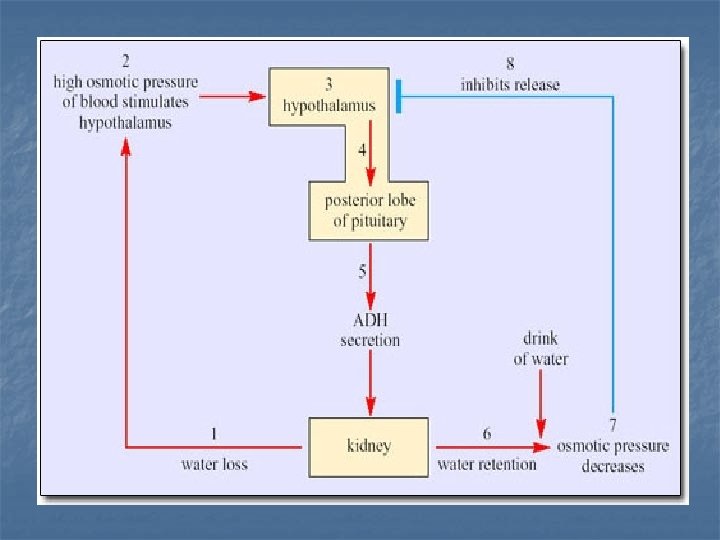
Control of water loss n n n It is controlled by controlling the volume of urine. Volume of urine is controlled by (ADH) Anti- diuretic hormone (ADH): n n n Synthesized in the hypothalamus. Stored in the posterior pituitary until it is secreted. Secretion is stimulated by hypertonicity and hypovolemia.

Disturbances in body fluids 1 - Fluid Volume Excess Also it can be defined as hypervolemia , which occurs from an increase in total body sodium content and an increase in total body water

Causes of hypervolemia 1 - excessive fluid intake 2 - excessive sodium intake 3 - Renal insufficiency or faluire 4 - Steroid Therapy 5 - Low protein intake or malnutrition 6 - Decreased cardiac output (heart disease ) 7 - Head injury 8 - Liver disease 9 - Sever stress 10 – Hormonal disturbances
Manifestations of Hypervolemia o. Weight gain o. Edema o. Bounding pulse o. Abnormal breath sound (crackles ) o. Changes in breathing pattern o. Jugular vein destination o. Change in mental status o. Oliguria o. Specific gravity changes o. Intake greater than output o. Azotemia o. Decrease hemoglobin or o. Changes in electrolytes hematocrit o. Restlessness & anxiety o. Increase blood pressure. Shortness of breath (orthopnea)

Nursing Intervention of Hypervolemia 1 - obtain patient history to ascertain the probable cause of fluids disturbance 2 - weight monitoring & evaluate weight in relation to nutritional status 3 -I &O chart 4 - monitor v/s 5 – evaluate for edema 6 - monitor serum electrolytes Intervention 1 - instruct the patient toward the restriction of fluid 2 - restrict Na intake 3 - Instruct pt to take prescribed diuretics 4 - elevate the edematous leg 5 - skin care 6 - provide information regarding s&s of fluid volume excess
Fluid volume loss (hypovolemia) Fluid volume deficit or hypovolemia. Occurs from a loss of body fluid or shift of fluids into 3 rd space , or from reduced fluid intake Causes : v. Inadequate fluid intake v. Fluid loss (diuresis, bleeding , severe diarrhea v. Fever , infection which leads to increase metabolic rate. v. Fluid shifts (edema or effusion )

Clinical manifestations of hypovelmia v. Decrease urine output v. Concentrated urine v. Output greater than intake v. Decrease venous filling v. Hemoconcentration v. Hypotension v. Thirst v. Dry m. m v. Changes in mental status

Nursing care of hypovolemia I- Assessment : the same as in hypervolemia II- Nursing Intervention : ØEncourage patient to drink prescribed amount ØAdminister IV fluid ØAdminister blood product as prescribed ØProvide oral hygiene ØTreat the underlying causes (diarrhea, vomiting)

Home work Define the following : §Hyponatremia §Hypernatermia §Hypocalcemia §Hypercalcemia §Hypokalemia §Hyperkalemia §

- Slides: 30