Board Review Imaging Equipment Quality Control of Imaging

Board Review Imaging Equipment Quality Control of Imaging Equipment

Components of the Radiographic Unit Overview Creating X Rays X-ray Tube Construction Operating Console Automatic Exposure Control Manual Exposure Controls Beam Restriction Devices/ Grids Image Receptors Fluoroscopy Equipment
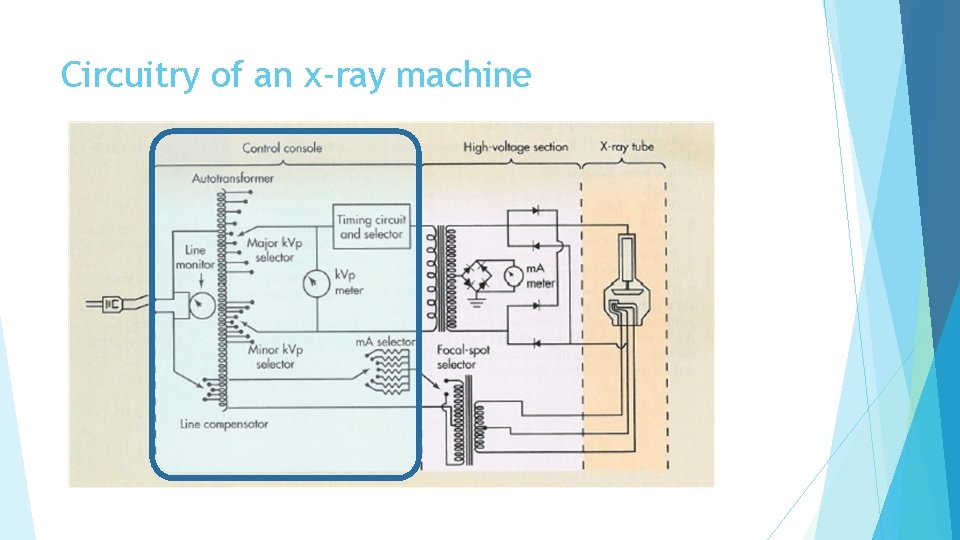
Circuitry of an x-ray machine
X-ray Generator, Transformers, and Rectification System: basic principles Transformer Generator Responsible for increasing the output voltage from the autotransformer to the k. Vp necessary for the production of x-rays High-voltage up) transformer (step- Increases the voltage from volts to kilovolts (V k. Vp) Filament down) transformer (step- Increases the amperage from m. A to A (m. A A)

Rectification System Converts the alternating electrical current from “the grid” to a direct current (AC to DC) Ensures that the electrons flow from the cathode to the anode only Half-wave rectifiers do not allow the voltage to swing negatively during the cycle, but this creates a period of time where there is no electrical current The x-ray tube emits x-rays for only ½ of the exposure time, or 60 times a second Full-wave rectifiers also do not allow the voltage to swing negatively, but during the part of the cycle where the voltage swings negatively, the voltage instead swings positively. Therefore there are no gaps in the electrical current The x-ray tube emits x-rays throughout the exposure time, or 120 times a second
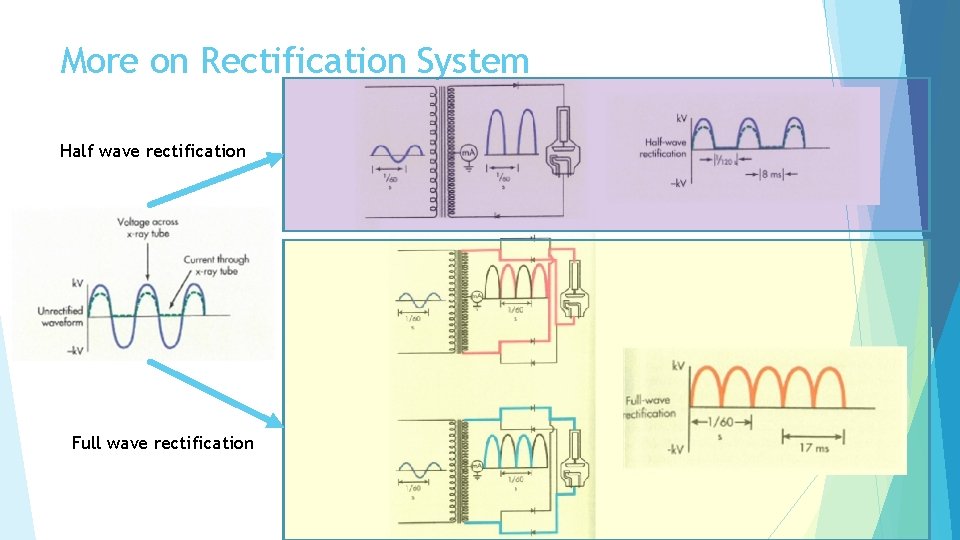
More on Rectification System Half wave rectification Full wave rectification
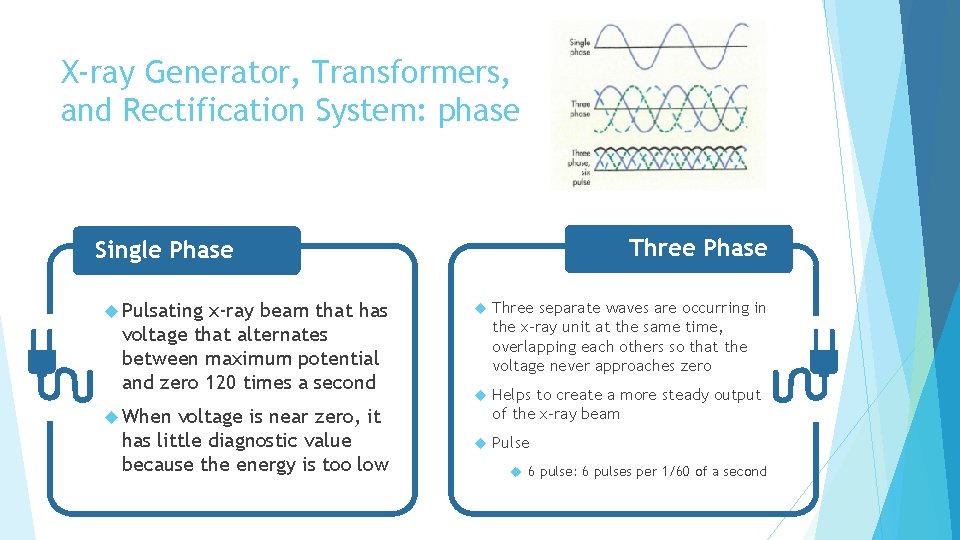
X-ray Generator, Transformers, and Rectification System: phase Three Phase Single Phase Pulsating x-ray beam that has voltage that alternates between maximum potential and zero 120 times a second voltage is near zero, it has little diagnostic value because the energy is too low Three separate waves are occurring in the x-ray unit at the same time, overlapping each others so that the voltage never approaches zero Helps to create a more steady output of the x-ray beam Pulse When 6 pulse: 6 pulses per 1/60 of a second

X-ray Generator, Transformers and Rectification System: high frequency 01. 02. Produce a nearly constant voltage waveform Less patient dose Comparisons of different voltage waveforms. Any ripple represents loss of voltage and therefore can compromise the integrity of the xray beam. As ripple decreases, patient dose decreases as well. High-frequency systems are most efficient at x-ray production. 03. Actually creates smaller generators, which leads to less bulk and cost 04. More efficient than other generators
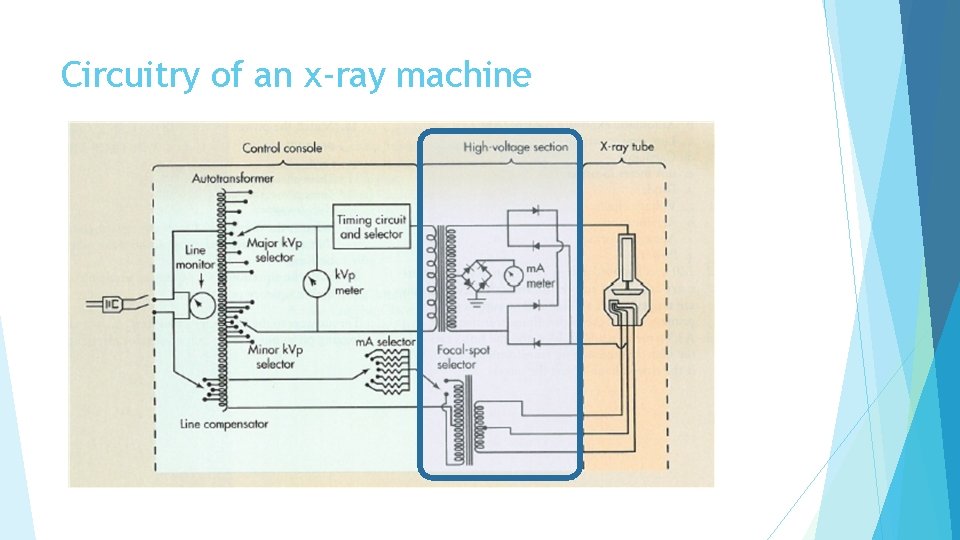
Circuitry of an x-ray machine

Filament Transformer Step down transformer Reduces voltage. Remember that voltage is coming from the autotransformer at 220 volts, but must be dropped down to 12 volts Current is also reduced This can be calculated just like the autotransformer and the high-voltage transformer, but the formula looks a little bit different Ip /Is = Ns / Np Where Ip= primary current
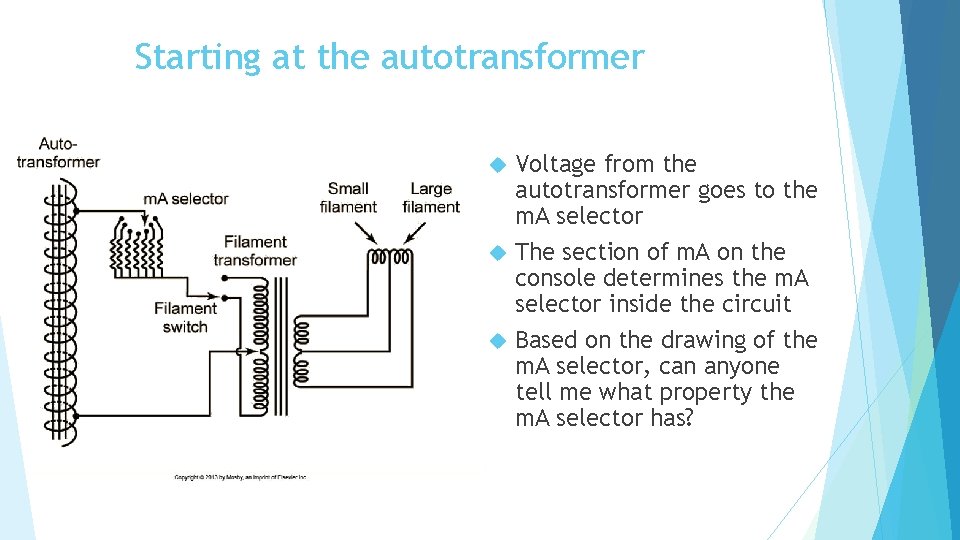
Starting at the autotransformer Voltage from the autotransformer goes to the m. A selector The section of m. A on the console determines the m. A selector inside the circuit Based on the drawing of the m. A selector, can anyone tell me what property the m. A selector has?
The m. A selector is a resistor! https: //www. reddit. com/r/pcmasterrace/comments/48 jkqo/these_windows_10_notifications_are_getting_seriou s/
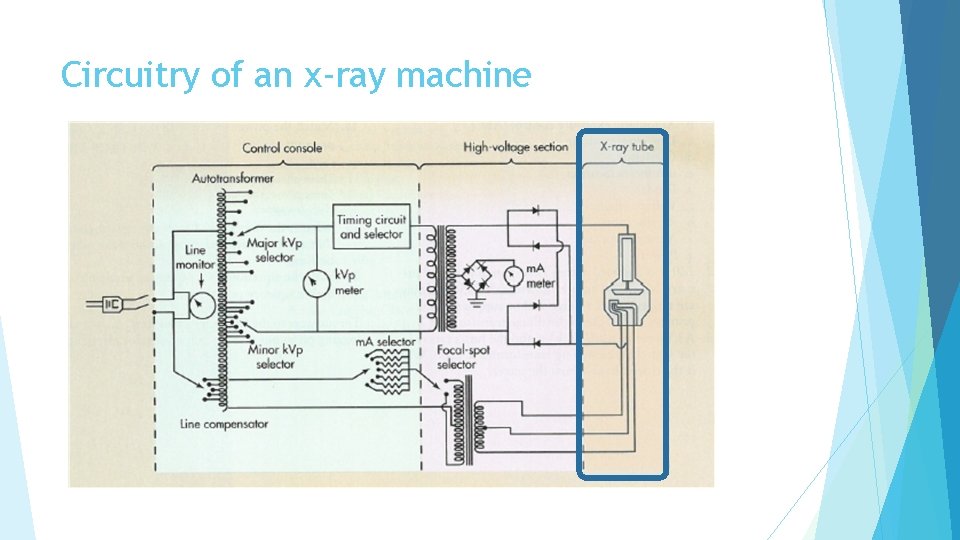
Circuitry of an x-ray machine
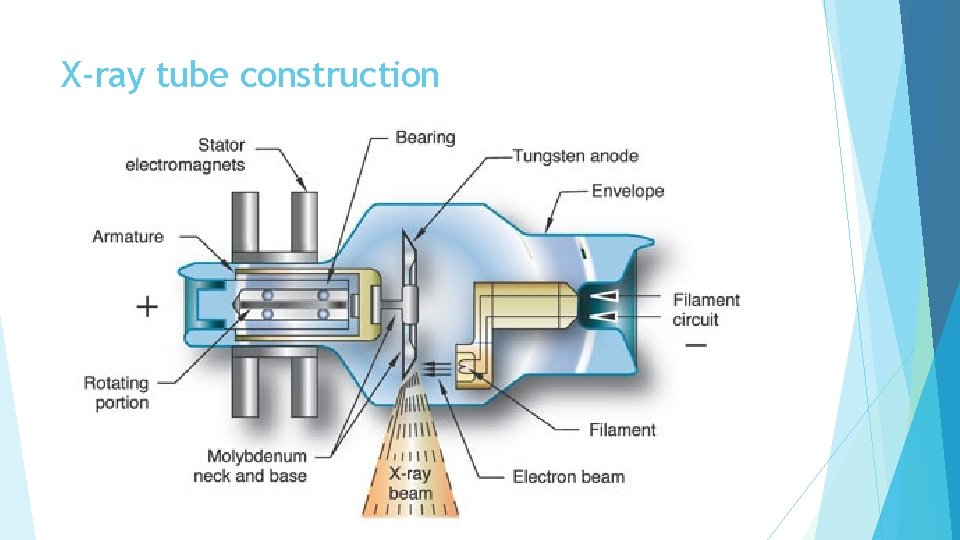
X-ray tube construction
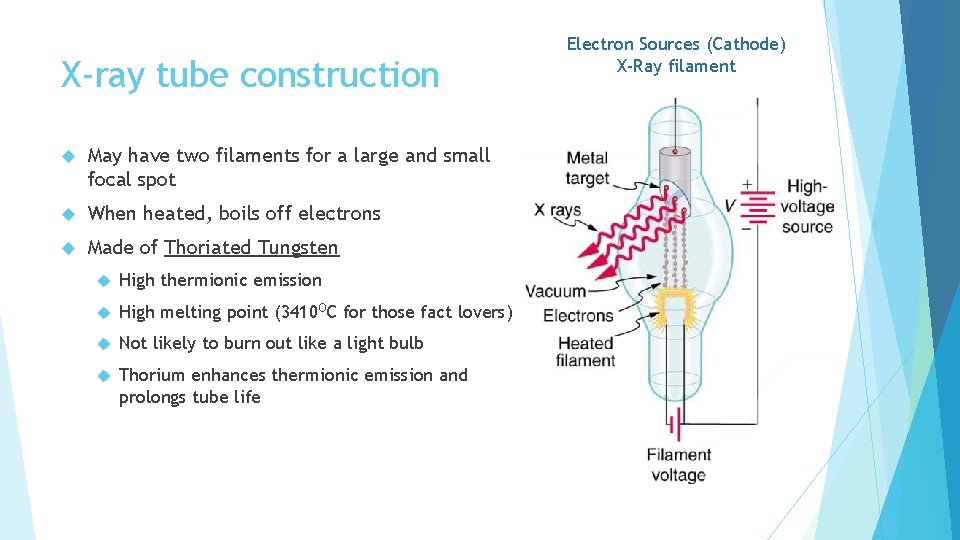
X-ray tube construction May have two filaments for a large and small focal spot When heated, boils off electrons Made of Thoriated Tungsten High thermionic emission High melting point (3410 OC for those fact lovers) Not likely to burn out like a light bulb Thorium enhances thermionic emission and prolongs tube life Electron Sources (Cathode) X-Ray filament

Heated animation Current in - -- -- - - The boiling off of electrons creates a cloud of electrons around the filament called the space charge. Because of the negative charge of the space charge, boiling of additional electrons becomes challenging At a certain point, depending on the tube current, there will be a maximum amount of electrons emitted. This is the saturation current

Thermionic Emission Thermionic emission is the process of heating the filament so that electrons will boil off the filament in preparation for the creation of x-rays. The combination of the low voltage and the amperage creates heat in the filament The electrons are kept close to the filament by the space cloud
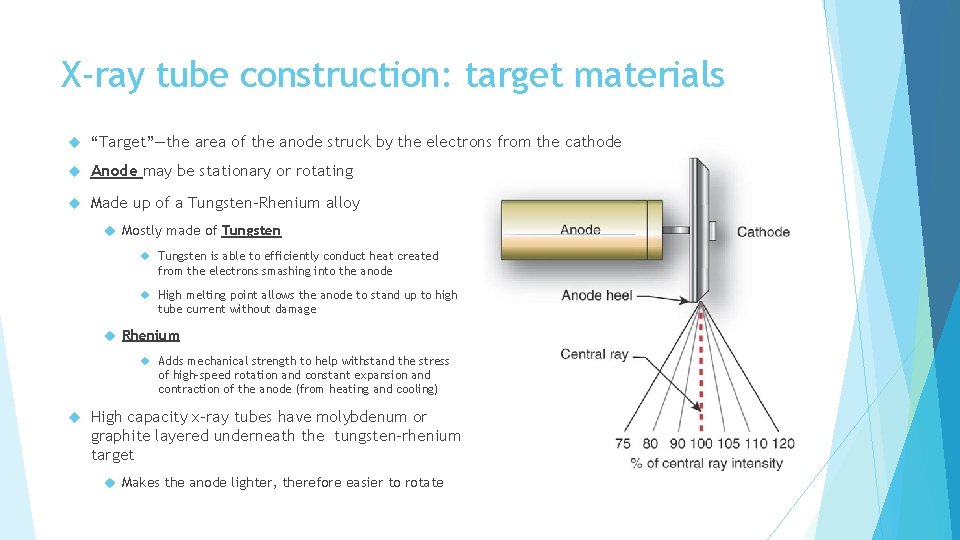
X-ray tube construction: target materials “Target”—the area of the anode struck by the electrons from the cathode Anode may be stationary or rotating Made up of a Tungsten-Rhenium alloy Mostly made of Tungsten is able to efficiently conduct heat created from the electrons smashing into the anode High melting point allows the anode to stand up to high tube current without damage Rhenium Adds mechanical strength to help withstand the stress of high-speed rotation and constant expansion and contraction of the anode (from heating and cooling) High capacity x-ray tubes have molybdenum or graphite layered underneath the tungsten-rhenium target Makes the anode lighter, therefore easier to rotate
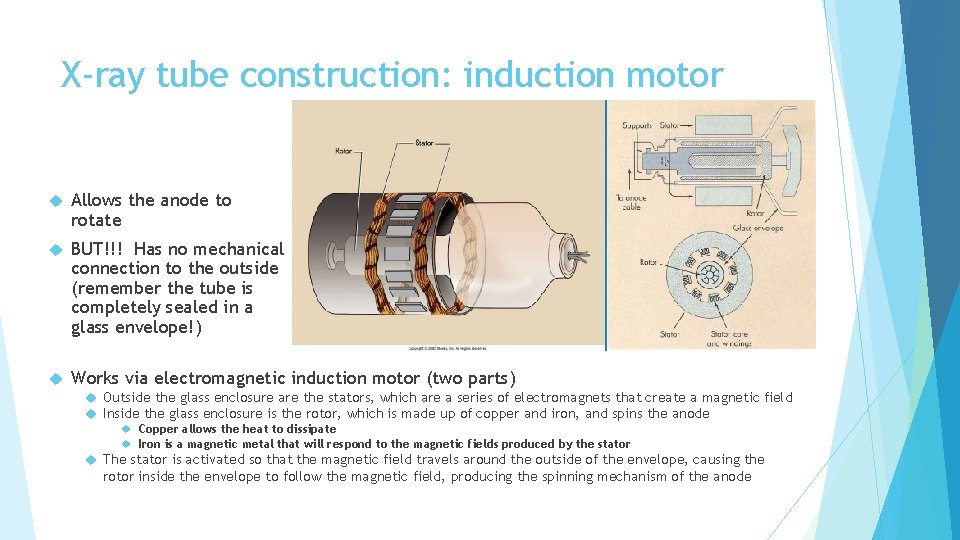
X-ray tube construction: induction motor Allows the anode to rotate BUT!!! Has no mechanical connection to the outside (remember the tube is completely sealed in a glass envelope!) Works via electromagnetic induction motor (two parts) Outside the glass enclosure are the stators, which are a series of electromagnets that create a magnetic field Inside the glass enclosure is the rotor, which is made up of copper and iron, and spins the anode Copper allows the heat to dissipate Iron is a magnetic metal that will respond to the magnetic fields produced by the stator The stator is activated so that the magnetic field travels around the outside of the envelope, causing the rotor inside the envelope to follow the magnetic field, producing the spinning mechanism of the anode

ACCESSORIES FOR YOUR MACHINE

Beam Restriction Devices Filters Inherent in tube design; x-ray tech has no control over these devices Must equal 2. 5 mm Aluminum equivalent Removes low-energy photons who do not contribute to the diagnostic image Also reduces patient dose Aperture diaphragm Cone and cylinder restrictors Flat, lead diaphragm with opening in center Extensions built to attached to x-ray tube Collimators Can be thought of as additive Controlled by the x-ray tech Remember that collimators restrict a beam but do not focus a beam!
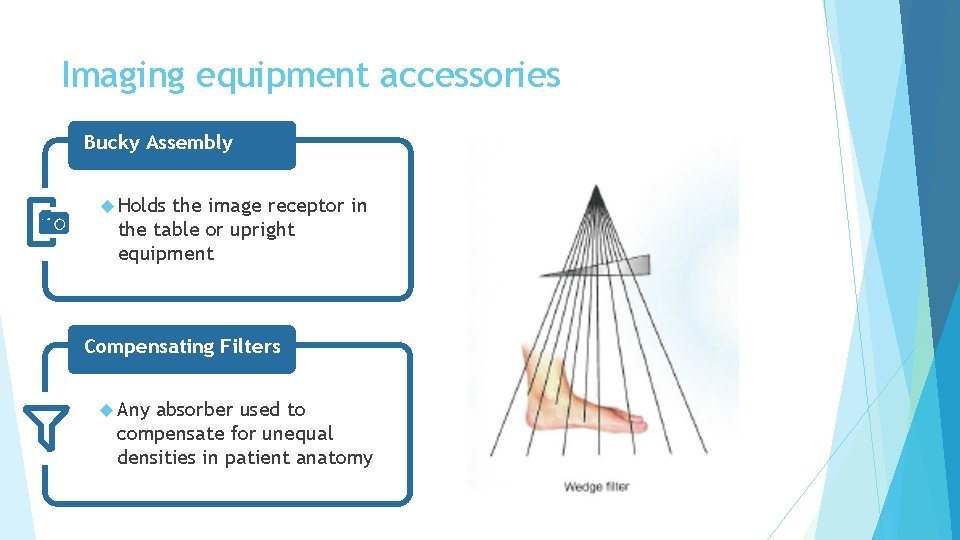
Imaging equipment accessories Bucky Assembly Holds the image receptor in the table or upright equipment Compensating Filters Any absorber used to compensate for unequal densities in patient anatomy
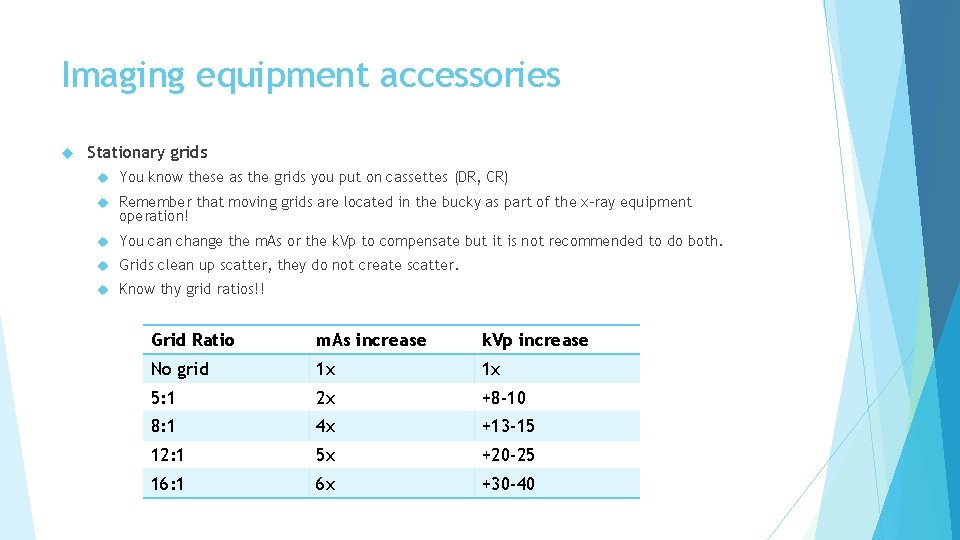
Imaging equipment accessories Stationary grids You know these as the grids you put on cassettes (DR, CR) Remember that moving grids are located in the bucky as part of the x-ray equipment operation! You can change the m. As or the k. Vp to compensate but it is not recommended to do both. Grids clean up scatter, they do not create scatter. Know thy grid ratios!! Grid Ratio m. As increase k. Vp increase No grid 1 x 1 x 5: 1 2 x +8 -10 8: 1 4 x +13 -15 12: 1 5 x +20 -25 16: 1 6 x +30 -40
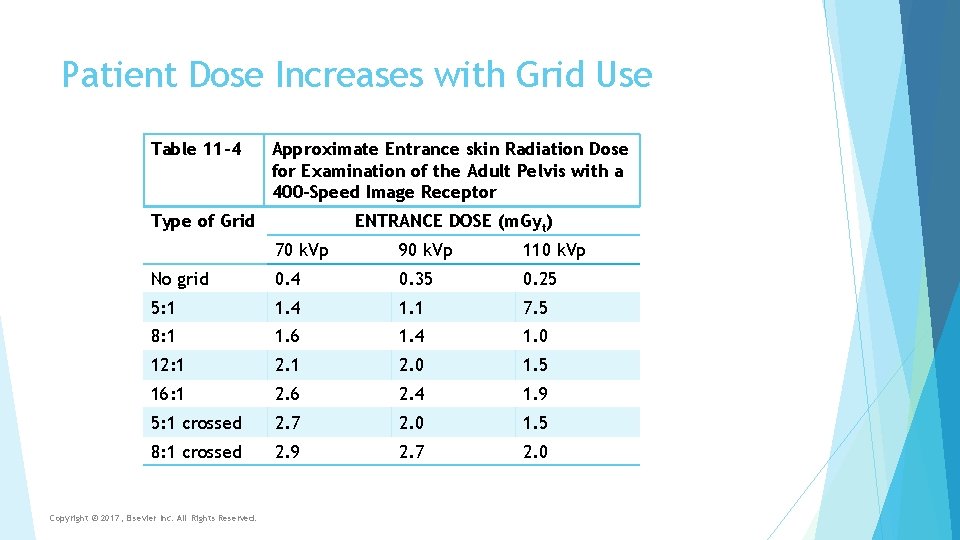
Patient Dose Increases with Grid Use Table 11 -4 Approximate Entrance skin Radiation Dose for Examination of the Adult Pelvis with a 400 -Speed Image Receptor Type of Grid ENTRANCE DOSE (m. Gyt) 70 k. Vp 90 k. Vp 110 k. Vp No grid 0. 4 0. 35 0. 25 5: 1 1. 4 1. 1 7. 5 8: 1 1. 6 1. 4 1. 0 12: 1 2. 0 1. 5 16: 1 2. 6 2. 4 1. 9 5: 1 crossed 2. 7 2. 0 1. 5 8: 1 crossed 2. 9 2. 7 2. 0 Copyright © 2017, Elsevier Inc. All Rights Reserved.
Operating Console Many different looks to operating consoles:

Operating Console All consoles have the same basic controls: On/Off Switch Kilovoltage control Milliampherage control Length of exposure/timer Focal Spot Size Automatic Exposure Control These are examples of manual exposure controls. Anything not performed with AEC is considered a manual exposure. Your distal extremities are manual exposure! Selection of appropriate chamber Density Controls

Manual Control

Automatic Exposure Control (AEC) Automatic Exposure Control is an automatic time that detects the amount of radiation passing through the patient and terminates the exposure after a appropriate amount of time Minimum reaction (response) time is determined by the length of time necessary to for the AEC to respond to the radiation and for the generator to terminate the exposure. Backup time is set at 150% (1. 5 times) that of the anticipated manual exposure. If exposure is expected to be 75 k. V at 100 m. As, it will terminate at 150 m. As. Most common and popular AEC device is the three chambers: ***Remember the selection of an incorrect chamber can cause an over or underexposed image!!!

Digital Image Receptors CR Image Receptor with Photostimulable Phosphor (PSP) imaging plate DR Flat Panel Detector Image Receptor
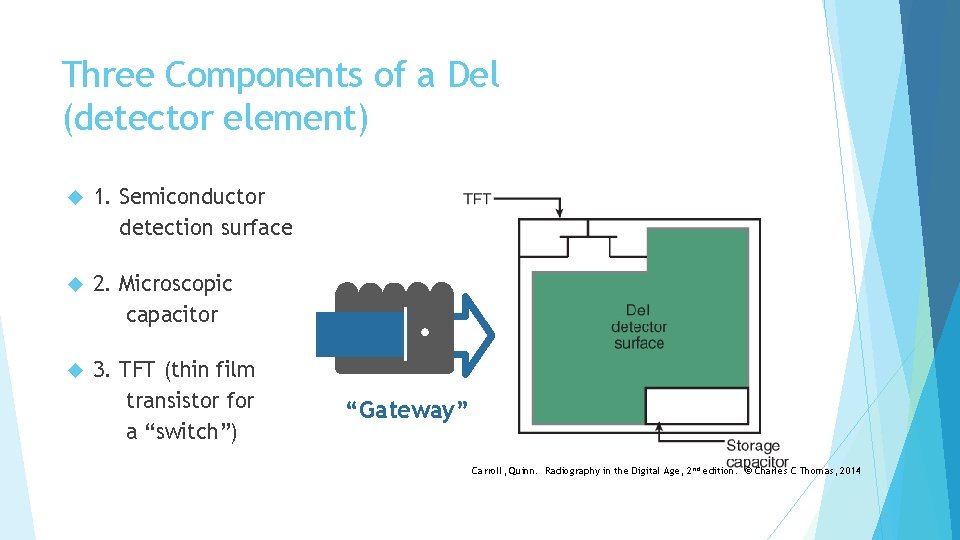
Three Components of a Del (detector element) 1. Semiconductor detection surface 2. Microscopic capacitor 3. TFT (thin film transistor for a “switch”) “Gateway” Carroll, Quinn. Radiography in the Digital Age, 2 nd edition. © Charles C Thomas, 2014

How Dels Work: Microscopic Electronic Capacitor Microscopic electronic capacitor The ability to store electric charge makes direct-capture imaging possible. The amount of charge stored will eventually be represented as the pixel value (gray level) for each pixel (more on this later) In each del, the TFT (thin film transistor) acts as a switching gate to release the built-up electrical charge when the del is “read out”

Flat Panel Detector Systems Indirect Conversion Direct Conversion
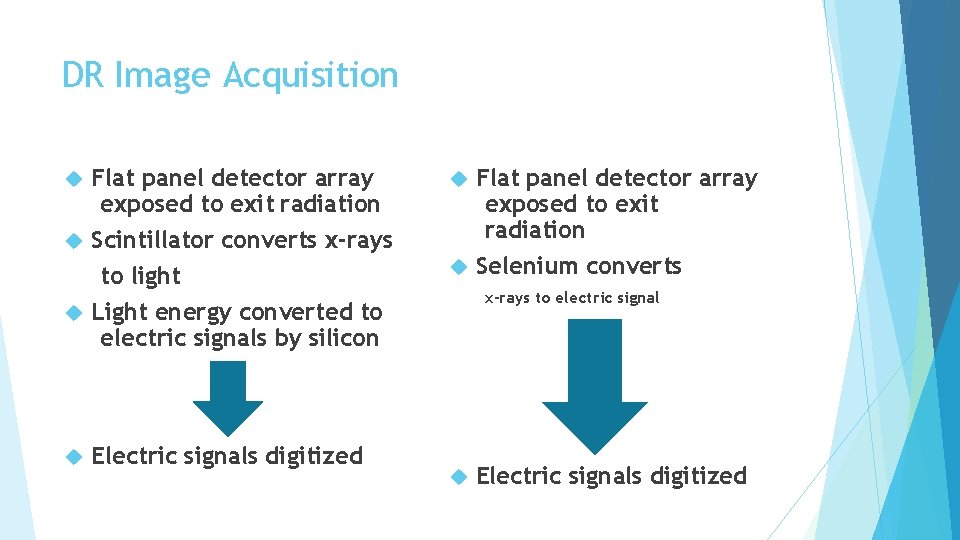
DR Image Acquisition Indirect conversion Direct conversion Flat panel detector array exposed to exit radiation Scintillator converts x-rays to light Light energy converted to electric signals by silicon Electric signals digitized Flat panel detector array exposed to exit radiation Selenium converts x-rays to electric signal Electric signals digitized

CR Image Acquisition Exit radiation interacts with imaging plate composed of barium fluoride bromide crystals coated with europium Absorbed energy stored in photostimulable phosphor material Some energy is released as visible light, but most results in electrons released in phosphor layer due to photoelectric interactions Electrons are trapped in phosphor layer until light energy is released during laser scanning (2 nd release of light) (electrons are trapped in an excited state)
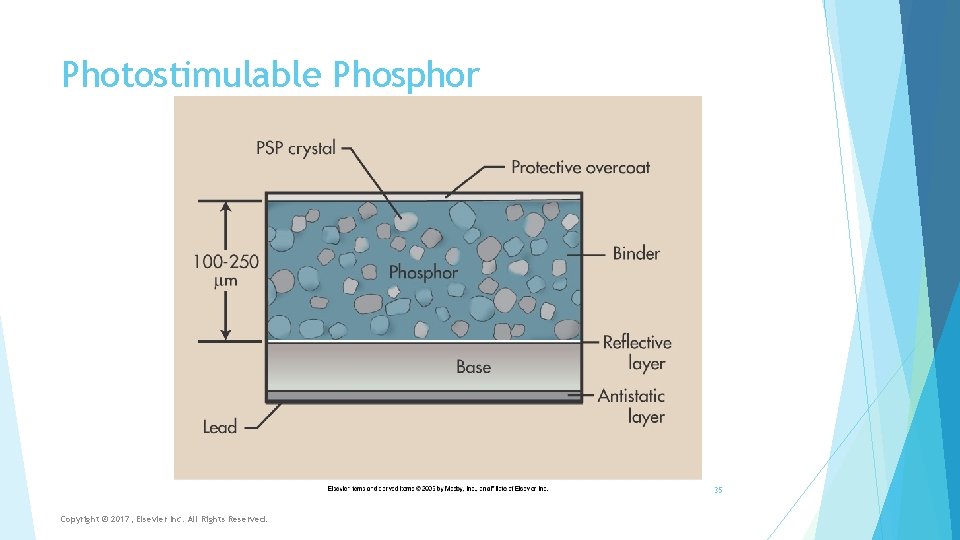
Photostimulable Phosphor 35 Copyright © 2017, Elsevier Inc. All Rights Reserved.
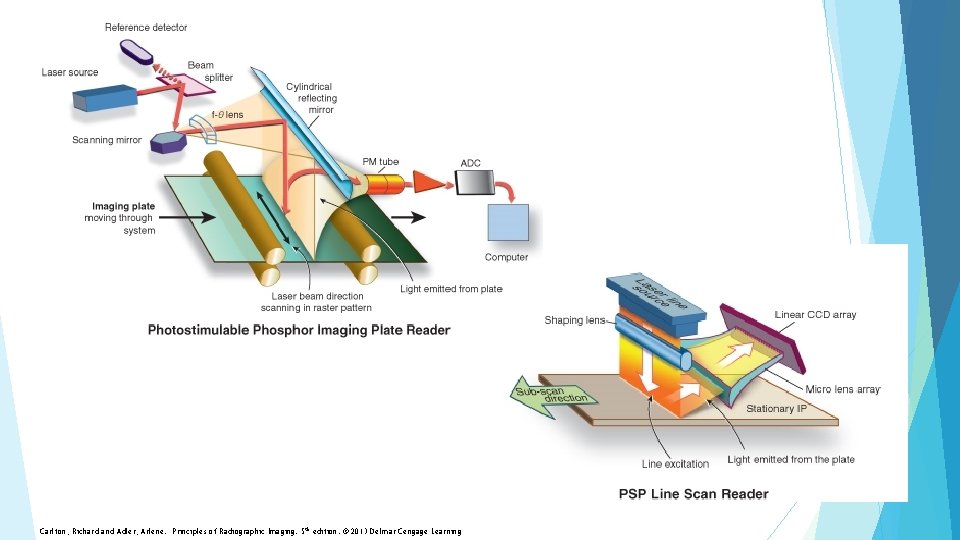
Carlton, Richard and Adler, Arlene. Principles of Radiographic Imaging. 5 th edition. © 2013 Delmar Cengage Learning
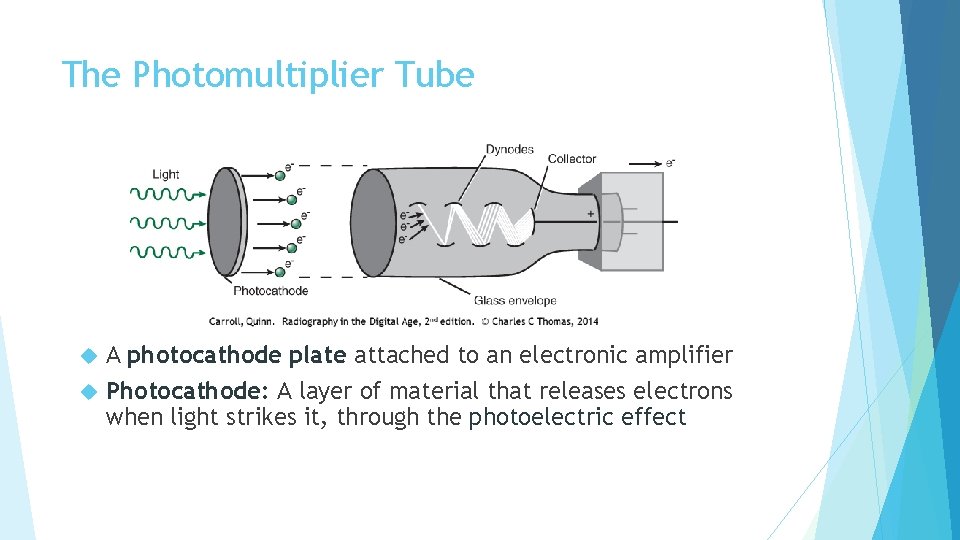
The Photomultiplier Tube A photocathode plate attached to an electronic amplifier Photocathode: A layer of material that releases electrons when light strikes it, through the photoelectric effect
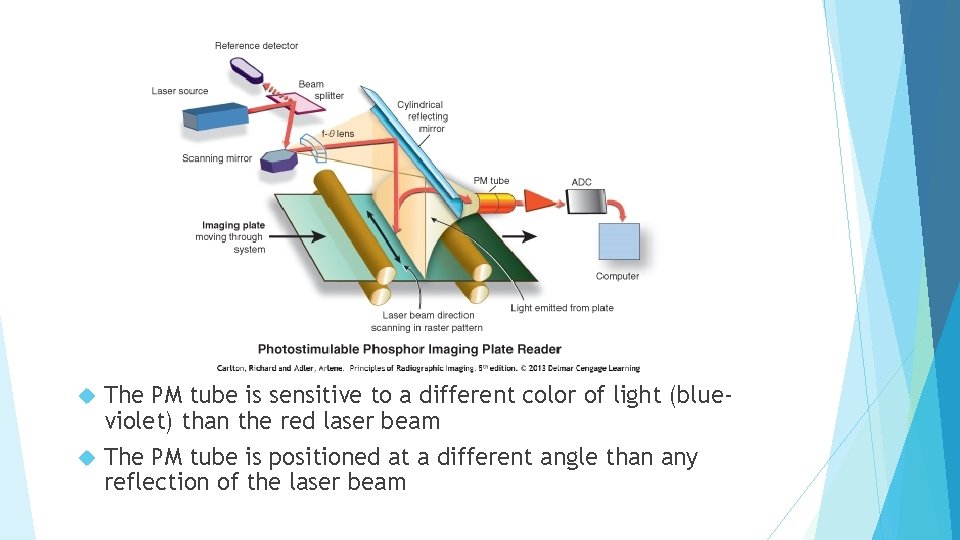
The PM tube is sensitive to a different color of light (blueviolet) than the red laser beam The PM tube is positioned at a different angle than any reflection of the laser beam
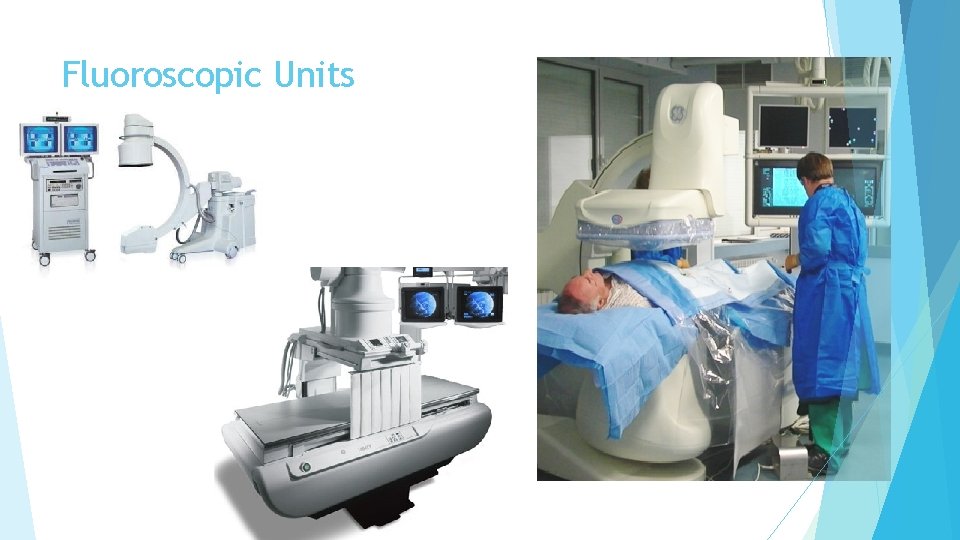
Fluoroscopic Units

Fluoroscopic Units Dynamic viewing—allows physician to view body in real time m. A station is generally set to 5 m. A Long imaging time contributes to patient dose Components of a fluoroscopic unit Image Intensifier Receives the remnant radiation and converts it to a visible-light image of high intensity Located above the patient Viewing Systems Television monitor Recording Systems Spot film cassettes Use of any recording media with adequate memory (i. e. DVDs, etc) Automatic Brightness Control Allows the fluoroscopic equipment to vary k. V and m. A depending on the thickness of the body part being imaged This is why when the fluoroscope moves over a thicker area or an area that has barium in it it’s dark for a few seconds and then it brightens up—the fluoroscope is adjusting for part thickness and pathology Magnification Mode
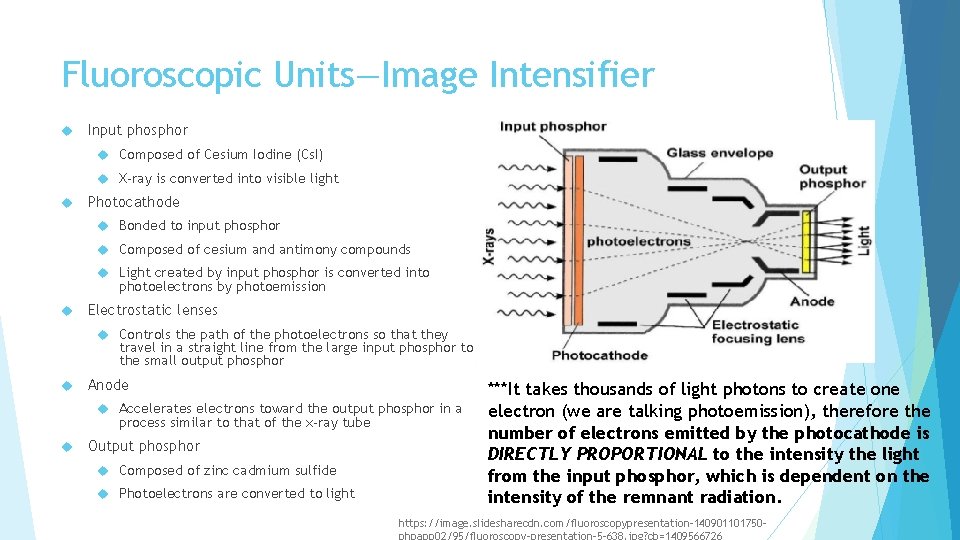
Fluoroscopic Units—Image Intensifier Input phosphor Composed of Cesium Iodine (Cs. I) X-ray is converted into visible light Photocathode Bonded to input phosphor Composed of cesium and antimony compounds Light created by input phosphor is converted into photoelectrons by photoemission Electrostatic lenses Controls the path of the photoelectrons so that they travel in a straight line from the large input phosphor to the small output phosphor Anode Accelerates electrons toward the output phosphor in a process similar to that of the x-ray tube Output phosphor Composed of zinc cadmium sulfide Photoelectrons are converted to light ***It takes thousands of light photons to create one electron (we are talking photoemission), therefore the number of electrons emitted by the photocathode is DIRECTLY PROPORTIONAL to the intensity the light from the input phosphor, which is dependent on the intensity of the remnant radiation. https: //image. slidesharecdn. com/fluoroscopypresentation-140901101750 phpapp 02/95/fluoroscopy-presentation-5 -638. jpg? cb=1409566726

Fluoroscopic Units— Television Camera Tube Target assembly Signal plate Composed of a thin layer of metal (or graphite) Receives light from the output phospohor Metal layer is thin enough to allow light to pass through, but thick enough to conduct electricity Target plate Composed of antimony trisulfide, which is photoconductive (when illuminated it conducts electrons, when dark, acts as insulator) Receives electron beam Electron gun Heated filament that supplies a constant electron current by thermionic emission (like the filament in the xray tube) Control grid surrounding the electron gun forms the electrons into a beam that accelerates toward the anode (in this case known as the target plate) Accelerator grids and steering coils Help propel the electron beam toward the target plate

Fluoroscopic Unit—Television Camera Tube Putting it all together: Light from the output cathode striking the signal plate at the same time and place as the electron beam from the target plate creates a video signal. Depending on the intensity of the light from the output phosphor, the signal will be large or small.

Fluoroscopic Unit—Television Screen Video signal from the target assembly is transmitted by cable to the television monitor where it is converted by to a visible image. Video signal is modulated, meaning that the magnitude of the signal is directly proportional to the intensity of the light received by the target assembly from the output phosphor of the image intensifier (see previous slide) Video signal is converted into an electron beam, which varies in intensity according to the modulation of the video signal Electron beam is focused on the fluorescent screen of the monitor, creating visible light that forms into the image viewed by the radiologist and technologist

Fluoroscopic Unit—Visible Image Technologist can control the contrast and brightness of the image by manipulating the controls on the monitor. This does not change the quantity or quality of the x-ray beam. Frame rate of video monitoring is 30 frames per second This actually causes a flickering of the image, but because the human eye cannot detect flickering at rates above 20 frames per seconds, it is undetectable Spatial resolution is related to the number of lines per frame. The more lines per frame, the better the spatial resolution Raster pattern—method of scanning by which data collection begins at one corner of a plate and moves in a line to the other corner and repeats for each line (think of how you read—the way you read is essentially a raster pattern)

Fluoroscopic Unit—Recording Systems Digital Still images (whether from “spot” or screen capture) are saved digitally and transmitted to patient’s chart in the medical center’s PACS system Can capture pathology quickly Note that only still images are saved and archived The entire study can be recorded to a DVD, which is sometimes the case in “Swallow studies” performed for dysphagia Spot film Uses a cassette (CR or plain-film) that is loaded into an opening between the patient and the image intensifier (this opening is surrounded by lead as to not expose the cassette) When radiologist is ready to capture an image, the cassette moves within the machine to accept the image, and a radiographic (not fluoroscopic) exposure is taken Disadvantages of spot film Increased delay in timing of image, therefore patient or barium/air could move and lose key pathology Increased patient dose

Automatic Brightness Control (ABC) Allows for adjustments based on the anatomy being examined. Image brightness level created by varying the k. V and/or m. As Do not confuse with AEC (Automatic Exposure Control)

Fluoroscopic Units—Magnification Mode Image can be magnified electronically within the IMAGE INTENSIFIER Magnification is accomplished with increased voltage that focuses the electrons closer to the input screen, causing the image to be magnified when it reaches the output screen Depending on the unit, magnification can range from 1. 5 to 4 in sequential steps (you cannot “zoom” it like you would on your smartphone!) Magnification can be calculated as: input screen diameter Magnification = diameter of input screen used during magnification
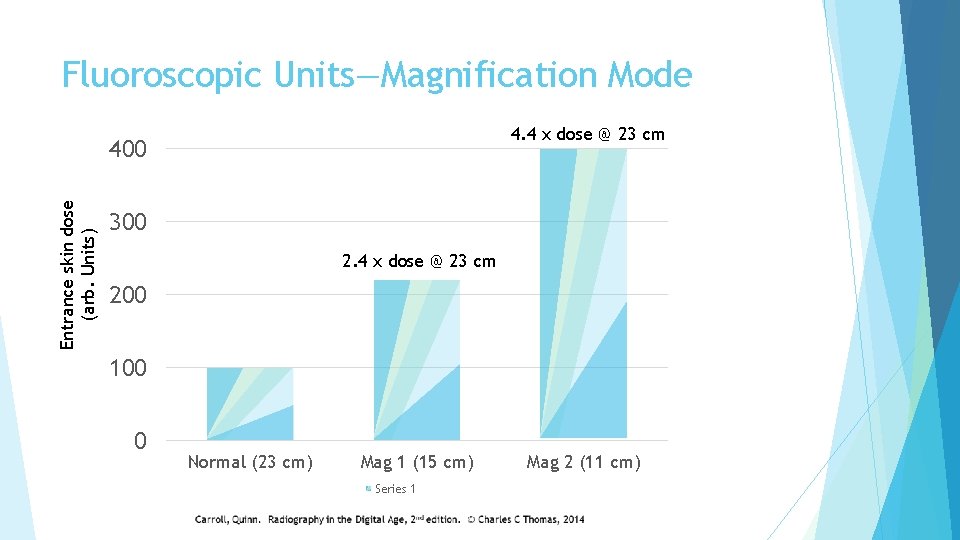
Fluoroscopic Units—Magnification Mode 4. 4 x dose @ 23 cm Entrance skin dose (arb. Units) 400 300 2. 4 x dose @ 23 cm 200 100 0 Normal (23 cm) Mag 1 (15 cm) Series 1 Mag 2 (11 cm)
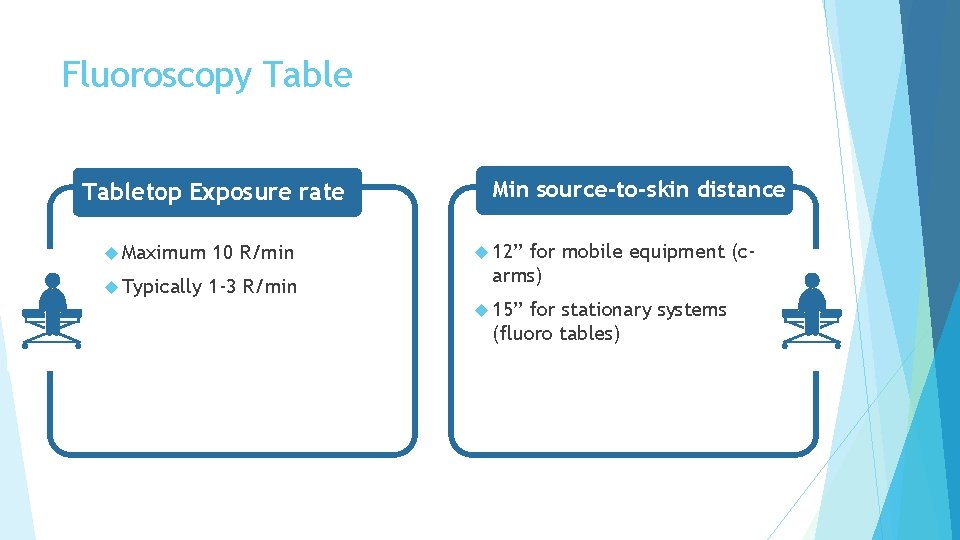
Fluoroscopy Tabletop Exposure rate Maximum 10 R/min Typically 1 -3 R/min Min source-to-skin distance 12” for mobile equipment (carms) 15” for stationary systems (fluoro tables)

Fluoroscopy Table Single step away from table decreases exposure exponentially—this is where knowing your inverse square law becomes important Bucky slot cover 0. 25 mm Lead rubber drape 0. 25 mm Pb/eq Radiologist as shielding

Charge-coupled device Replaces television camera tube Advantages: High spatial resolution High signal-to-noise ratio High detective quantum efficiency (DQE) No warm-up required No lag or blooming No spatial distortion No maintenance Unlimited life Unaffected by magnetic fields Linear response Lower patient dose

REFERENCES Fauber, Terri, L. RT(R)(M), Professor Emeritus of Radiation Sciences, School of Allied Health Professions, Virginia Commonwealth University. Steinsultz, Katrina Lynn RT (R)(M), M. Adm. MPH, Program Director, Radiologic Technology, Lansing Community College Thommen, John RT. (R), Faculty (Retired), Radiologic Technology, Lansing Community College Bushong, Stewart, M. D. , Sc. D, FAAPM, FACR, Professor of Radiologic Science, Baylor College of Medicine Images copyright Copyright © 2018, Elsevier Inc. All Rights Reserved

Thank You!
- Slides: 54