BN 2028 A Randomized Phase III Trial of

BN 2028: A Randomized Phase III Trial of Pre. Operative Compared to Post-Operative Stereotactic Radiosurgery (SRS) in Patients with Resected Brain Metastases Stuart H. Burri, M. D. - Levine Cancer Institute Anthony Asher, M. D. - Carolina Neurosurgery and Spine Scott Soltys, M. D. - Stanford University Daniel Cagney, M. D. – Harvard University Daniel Trifiletti, M. D. – Mayo Clinic : Jacksonville July 17, 2020 @NRGOnc NRG Oncology
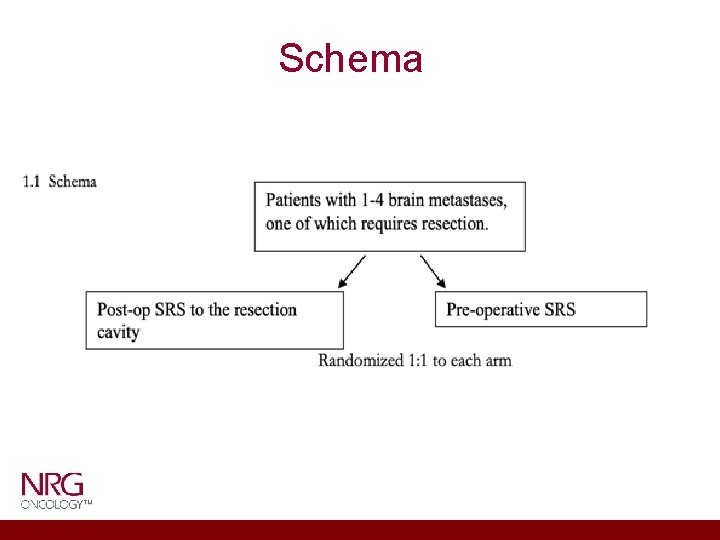
Schema
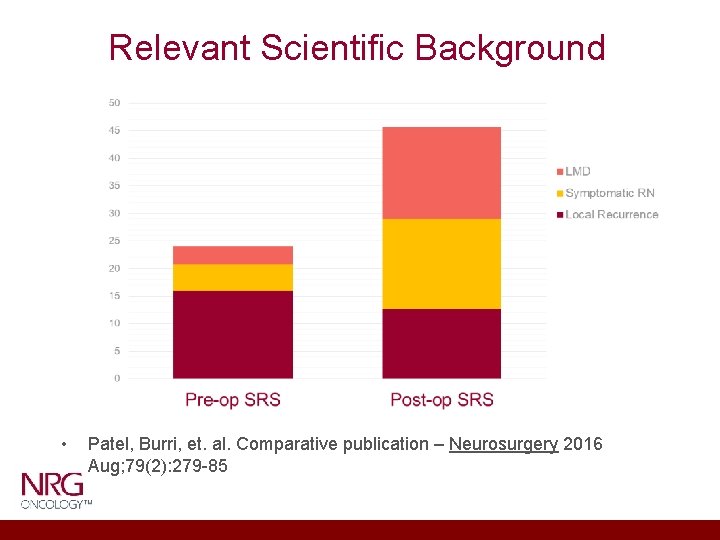
Relevant Scientific Background • Patel, Burri, et. al. Comparative publication – Neurosurgery 2016 Aug; 79(2): 279 -85

Primary Objective and Brief Statistical Design • Endpoint : The risk of the development of composite local failure (cavity recurrence or leptomeningeal disease) would be reduced with pre-op SRS in treatment of resected brain metastases. • An anticipated delta of 13% improvement in pre-op SRS in LMD and local control measured via MRI. An anticipated adverse event risk at twelve months of 27% for pre-op and 40% for post-op as a continuous observation with a predicted hazard ratio 0. 57 using a competing risk approach. To show this difference 224 patients would give an 80% power with a two sided alpha of. 05.

Secondary Endpoints • • QOL measured by FACT-BR, LASA, and EQ-5 D Overall survival Radiation necrosis CNS patterns of failure including distant brain metastases • Avoidance of and/or time to whole brain • Surgical bed failure alone • Combined surgical bed failure, LMD, and symptomatic radiation necrosis

Quality of Life Secondary Endpoints • • To determine if there is better emotional well-being at 9 months as assessed by the FACT-BR in patients with resected brain metastasis undergoing preresection SRS compared to post-resection SRS To determine in patients with resected brain metastases whethere is improved overall QOL as assessed by the FACT-BR and LASA or EQ-5 D in patients who receive pre-resection SRS compared to patients who receive post-resection SRS To determine in long-term survivors (defined as alive more than 12 months from time of randomization) whethere is better emotional well-being and overall QOL as assessed by the FACT-BR and LASA in patients who receive pre-resection SRS to the tumor compared to patients who receive post-resection SRS To ascertain in patients with resected brain metastases whethere is improved QOL as assessed by all other total and individual FACT-BR and LASA items and subscale values in patients who receive pre-resection compared to patients who receive post-resection SRS
- Slides: 6