BLOODBORNE PATHOGENS Microorganisms the Chain of Infection OSHA

BLOODBORNE PATHOGENS “Microorganisms & the Chain of Infection” OSHA Standard 29 CFR 1910. 1030
Microorganisms & the Chain of Infection Bloodborne Pathogens (BBP)
Microorganisms

Four. FOUR KINDS Kinds Bacteria Viruses Protozoa – think parasite Fungi and their eggs – called spores (think yeast infections and athlete’s foot)

Microorganism Plant or animal so small it can only be seen with a microscope. On all surfaces of our body and surfaces around us Few areas are not covered: brain, blood stream, lungs, areas surrounding internal organs
Microorganisms Bacteria Image: The bacteria that causes meningitis
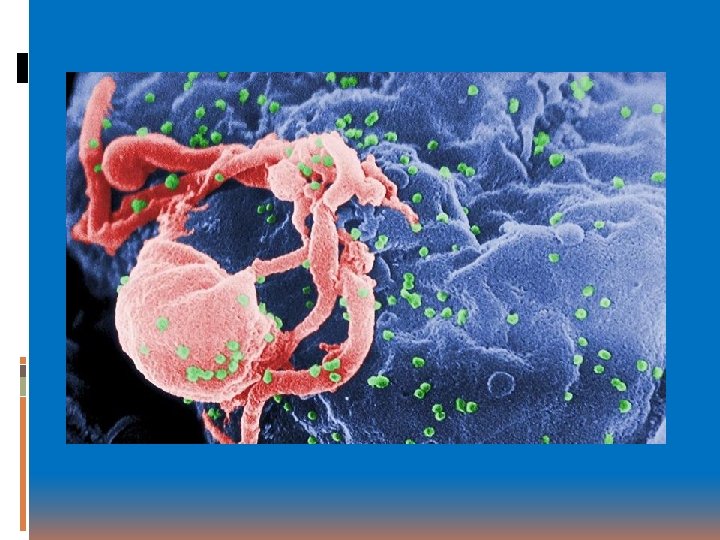
Microorganisms Bacteria Viruses Image: Human Immunodeficiency Virus
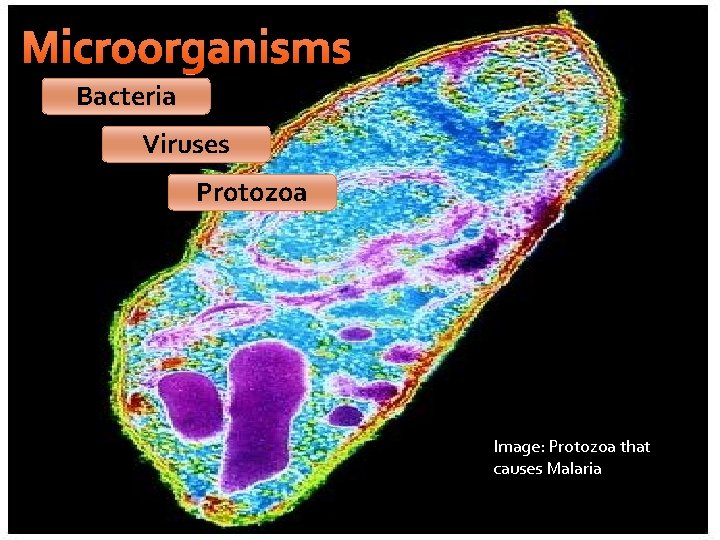
Microorganisms Bacteria Viruses Protozoa Image: Protozoa that causes Malaria
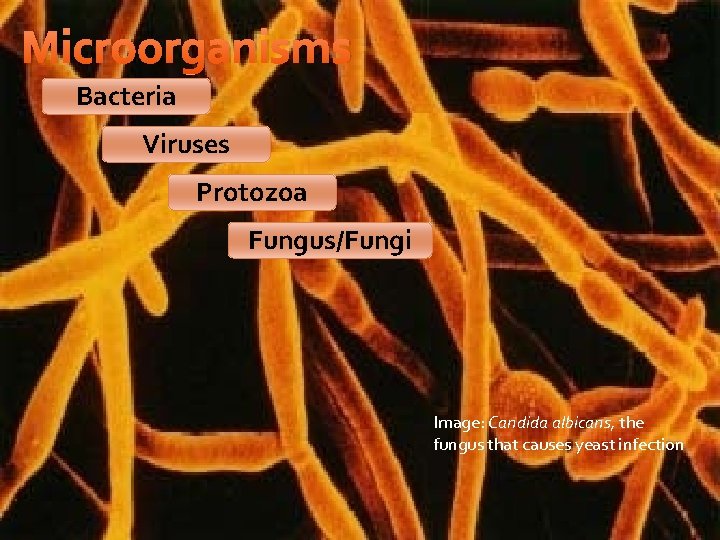
Microorganisms Bacteria Viruses Protozoa Fungus/Fungi Image: Candida albicans, the fungus that causes yeast infection

NORMAL FLORA -Bacteria When a microbe lives on us without harming us or Provides a benefit or protection to us. This relationship is called: mutually beneficial Examples: Escherichia coli (E. Coli) in our bowels Produces Vitamin K as byproduct which helps with clotting of blood. Staphylococcus aureus – on skin and resp. tract MRSA
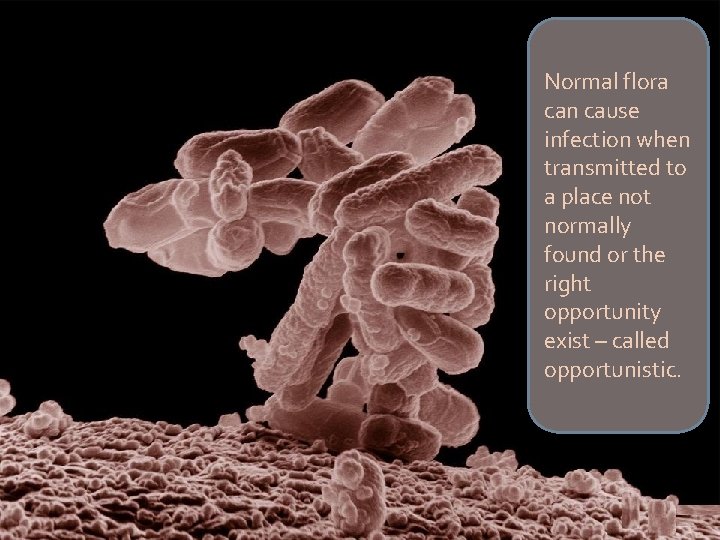
Normal flora can cause infection when transmitted to a place not normally found or the right opportunity exist – called opportunistic.
Escherichia coli (E. coli) First Example

In 1993 An E. coli outbreak resulted in the death of four children and severe illness for hundreds more when undercooked beef was ingested. The following is how the infectious agent, E. coli infected the vulnerable host – the children. We have seen numerous E. coli and bacterial outbreaks in our food sources since then. Most recent involved sprouts; hummus, dips and walnuts – May 2014
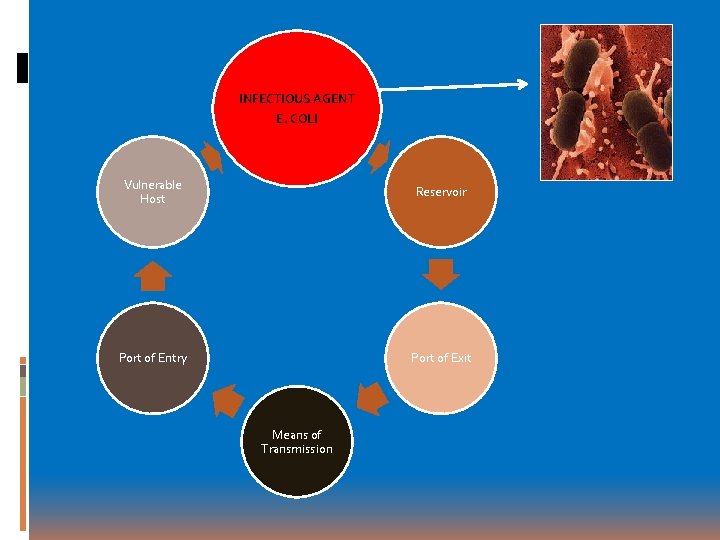
INFECTIOUS AGENT E. COLI Vulnerable Host Reservoir Port of Entry Port of Exit Means of Transmission
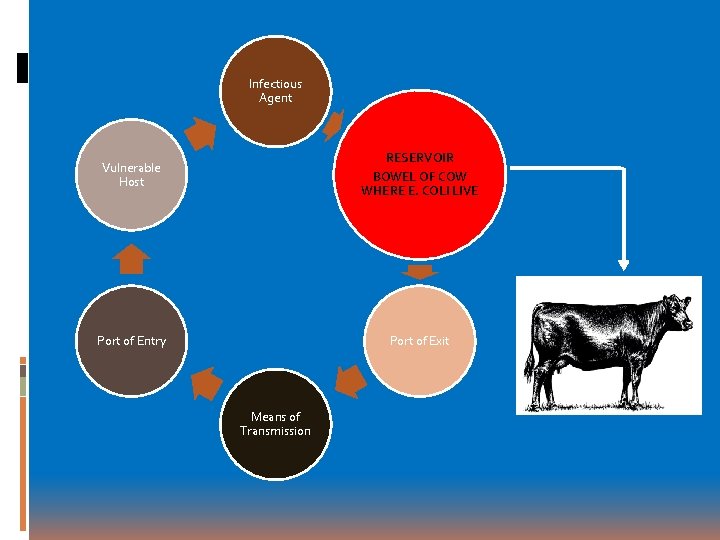
Infectious Agent Vulnerable Host RESERVOIR BOWEL OF COW WHERE E. COLI LIVE Port of Entry Port of Exit Means of Transmission
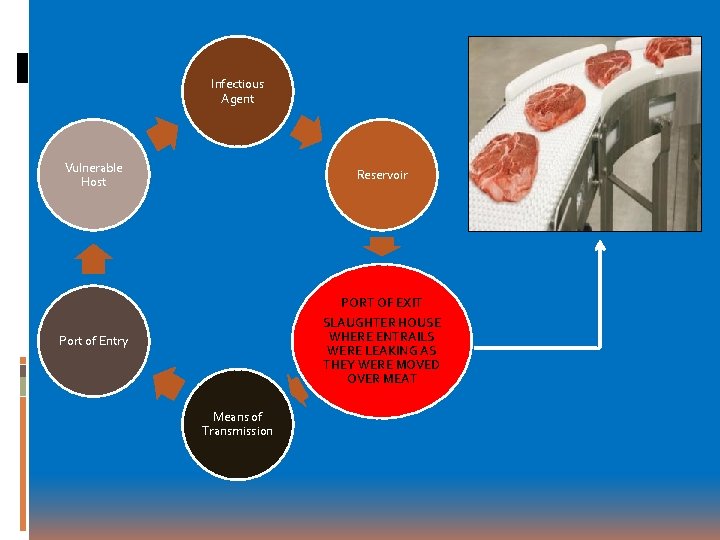
Infectious Agent Vulnerable Host Reservoir Port of Entry PORT OF EXIT SLAUGHTER HOUSE WHERE ENTRAILS WERE LEAKING AS THEY WERE MOVED OVER MEAT Means of Transmission
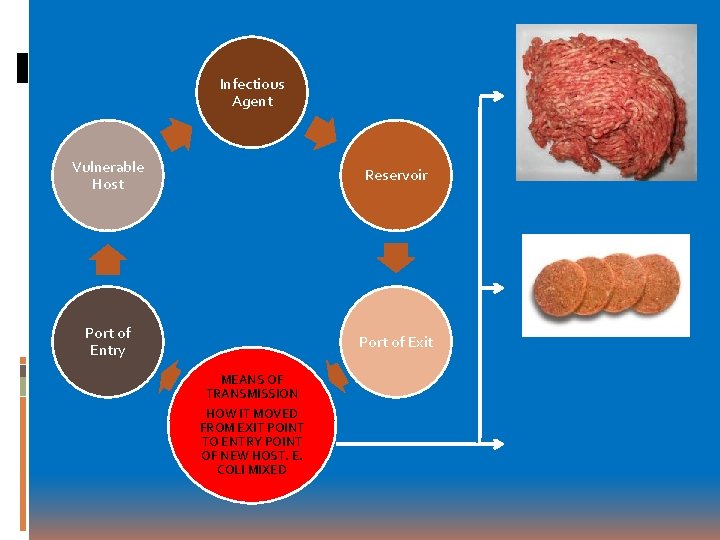
Infectious Agent Vulnerable Host Reservoir Port of Entry Port of Exit MEANS OF TRANSMISSION HOW IT MOVED FROM EXIT POINT TO ENTRY POINT OF NEW HOST. E. COLI MIXED
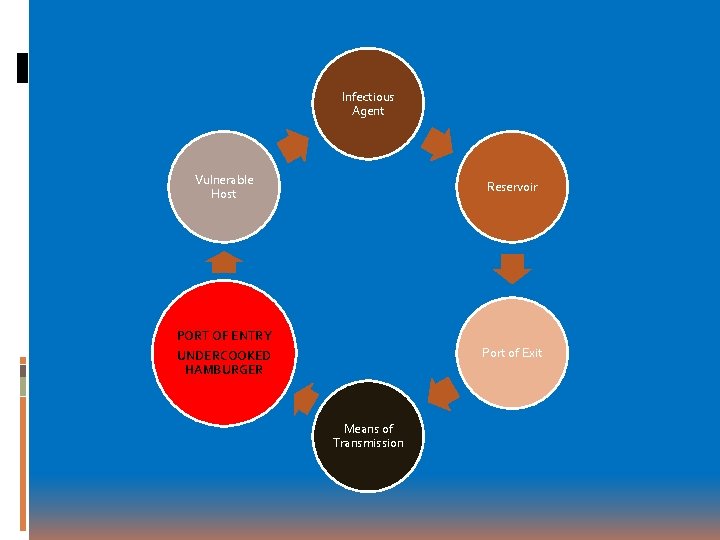
Infectious Agent Vulnerable Host Reservoir PORT OF ENTRY UNDERCOOKED HAMBURGER Port of Exit Means of Transmission

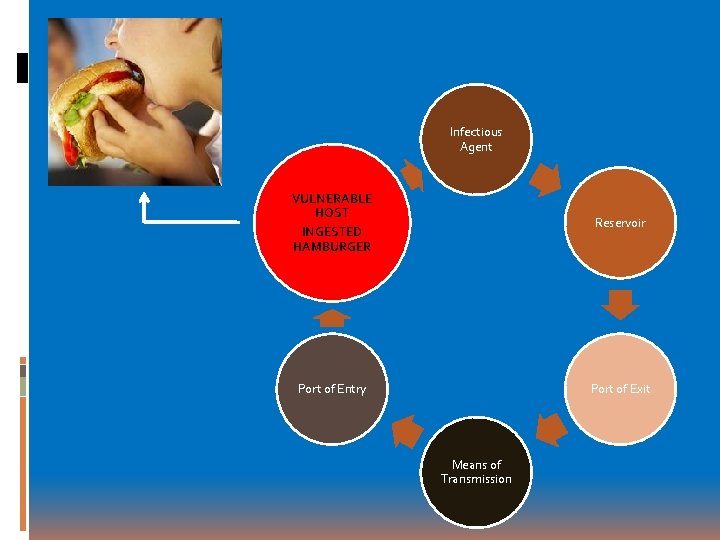
Infectious Agent VULNERABLE HOST Reservoir INGESTED HAMBURGER Port of Entry Port of Exit Means of Transmission

This incident led to restaurants posting warning messages against undercooked meats; a national movement motivated by the US Department of Health.

Infectious Agent: Staphylococcus aureus Second Example
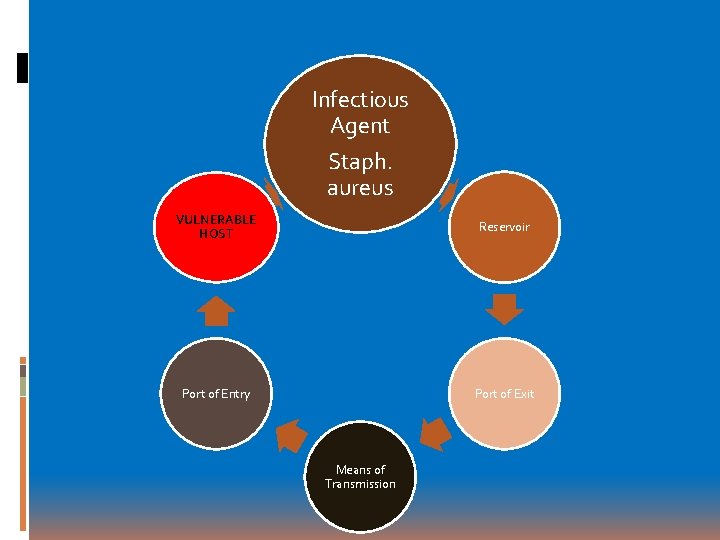
Infectious Agent Staph. aureus VULNERABLE HOST Reservoir Port of Entry Port of Exit Means of Transmission
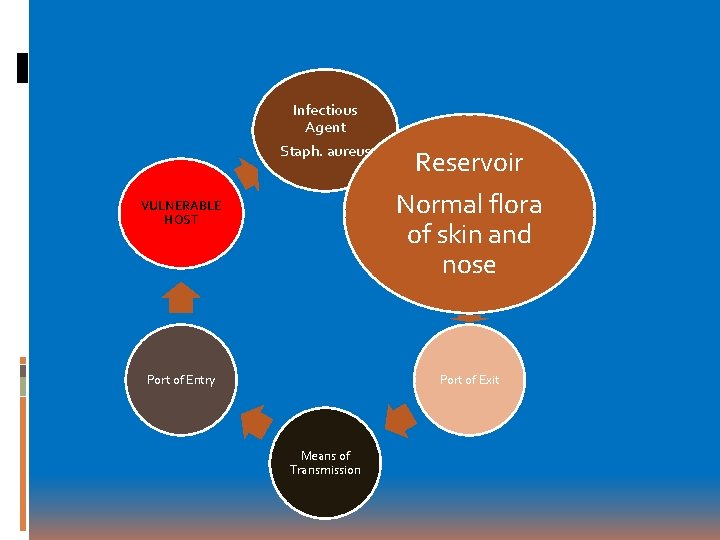
Infectious Agent Staph. aureus Reservoir Normal flora of skin and nose VULNERABLE HOST Port of Entry Port of Exit Means of Transmission
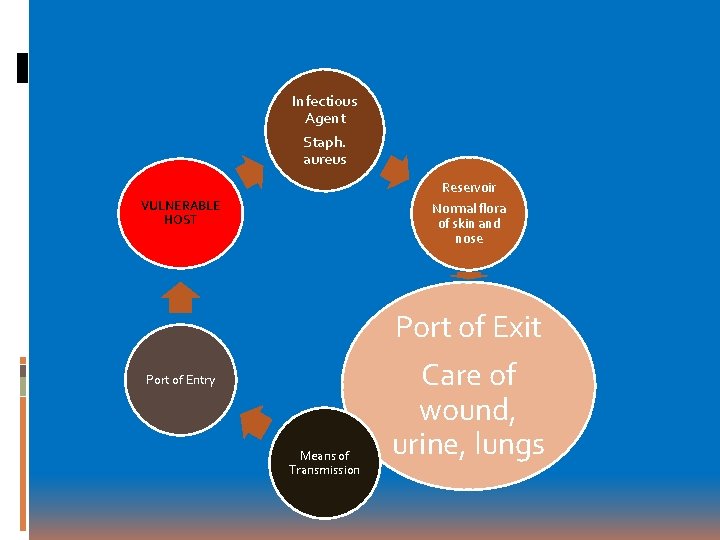
Infectious Agent Staph. aureus Reservoir Normal flora of skin and nose VULNERABLE HOST Port of Exit Port of Entry Means of Transmission Care of wound, urine, lungs
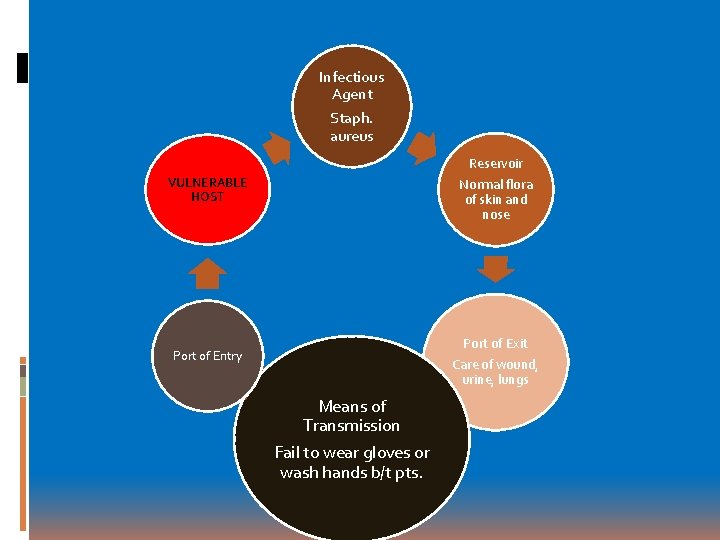
Infectious Agent Staph. aureus VULNERABLE HOST Reservoir Normal flora of skin and nose Port of Entry Port of Exit Care of wound, urine, lungs Means of Transmission Fail to wear gloves or wash hands b/t pts.
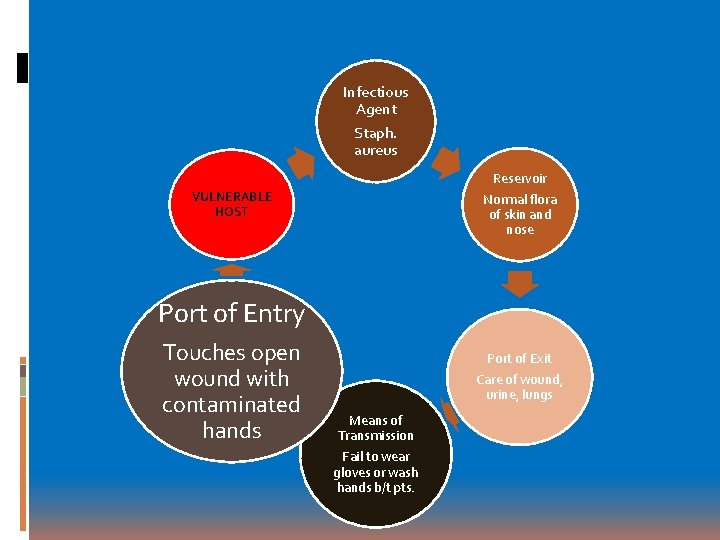
Infectious Agent Staph. aureus Reservoir Normal flora of skin and nose VULNERABLE HOST Port of Entry Touches open wound with contaminated hands Port of Exit Care of wound, urine, lungs Means of Transmission Fail to wear gloves or wash hands b/t pts.

VULNERABLE HOST Infectious Agent Staph. aureus Reservoir Normal flora of skin and nose WOUND, AGE, CANCER, IMMUNE SYSTEM Port of Entry Touches open wound with contaminated hands Port of Exit Care of wound, urine, lungs Means of Transmission Fail to wear gloves or wash hands b/t pts.

Why MRSA from normal Staph? Methicillin Resistant Staphlococcus Aureus Resistant to commonly used antibiotics Hospital acquired and community acquired Spread by skin-to-skin contact Begins as small red bumps (pimples, boils or spider bites) that turn into abscesses Why? Overuse of methicillin based antibiotics Not taking entire course of antibiotics
Viruses Two primary bloodborne pathogens Human Immunodeficiency Virus (HIV) Hepatitis (HBV/HCV)

HIV Human Immunodeficiency Virus – lentivirus Causes acquired immunodeficiency syndrome Progressive failure of the immune system Allows life-threatening opportunistic infections and cancers to thrive Infections with transfer of blood, bodily fluids.

HEPATITIS B Infectious illness of the liver Epidemic in Asia and Africa Transmitted by exposure to infectious blood or bodily fluids, transfusions, dialysis, tattooing, etc. No treatment; most adults clear infection spontaneously. Treatment to stop virus from replicating: PEGlated interferon Vaccine for prevention

Hepatitis C Affects primarily the liver Caused by the hepatitis C virus HCV Chronic infection leads to cirrhosis and liver failure Spread primarily by blood-to-blood contact Associated with IV use, poorly sterilized medical equipment and transfusions. New drugs developed for cure. No vaccine for prevention.

Compare/Contrast Bacteria Virus Larger of microbes Smallest of life forms Complex biology Simplest life form Live outside cells of host Must live within cells of host to survive Able to reproduce without host Many are beneficial to host Must use host’s genetic material to reproduce Most harmful

PREVENTION HAND HYGIENE WASH YOUR HANDS!

GERMS ARE EVERYWHERE Bacteria and viruses are everywhere. Some can survive for weeks on surfaces such as countertops and stethoscopes. Healthcare workers’ hands are the most common way of transferring germs to patients.
YOUR HANDS PICK UP GERMS WHEN YOU. . . Touch the doorknob Shake a patient’s hand Take a patient’s pulse or blood pressure Help a patient move Cover your sneeze or cough with your hands Use the toilet Touch surfaces or objects in the patient care areas

GERMS Use medical equipment in the patient care area. Touch a patient’s clothing.

CLEAN YOUR HANDS CDC recommends washing with soap and water ONLY : When they are dirty or visibly soiled with blood or other bodily fluids. After using the restrooms Before eating USE AN ALCOHOL BASE HAND RUB FOR ALL OTHER HAND HYGIENE SITUATIONS !!!

USE OF ALCOHOL RUB Before direct patient contact Before inserting an invasive device Before moving from a contaminated body site to a clean body site. After contact with a patient’s skin. After removing gloves.

HAND HYGIENE SITUATIONS During a typical patient hour, a healthcare worker could have as many as 8 -12 hand hygiene moments. E. g. , going from one patient to another Touching surfaces in patient rooms Touching medical equipment used on patient

HOW TO WASH WITH AN ALCOHOL RUB Apply amount to palm of one hand Work product in between fingers Rub hands until dry. Make sure they are dry. Takes less time than soap/water. Convenient Efficiently kills germs

MRSA AND C. DIFF Gloves must be worn. Perform hand hygiene after glove removal.

GLOVES Wear if there is a potential for contact with blood or infectious materials, mucous membranes or nonintact skin Change gloves between patients. Change gloves from a contaminated body site to a clean body site. Gloves are not a substitute for washing hands! Wash after removing gloves…

SUMMARY Practice hand hygiene after leaving a patient, even if you didn’t touch the patient. Bacteria can survive for long times on surfaces (think computer keyboards) Change gloves and wash hands after glove contact. Rub it in! Have dispensers in convenient places to use.

References Diffen. Bacteria vs. Virus: Difference and Comparison. Retrieved 12/1/2010 from www. diffen. com/difference/Bacteria_vs_Virus Marler-Clark and Associates. Jack in the Box E. coli Outbreak. Retrieved 11/4/2010 from www. aboutecoli. com 2010 Wikipedia: Staphylococcus aureus. Retrieved 11/4/2010 from www. wikipedia. org
- Slides: 47