Blood Vessels Arteries Arterioles Ventricles Heart Capillaries Atria
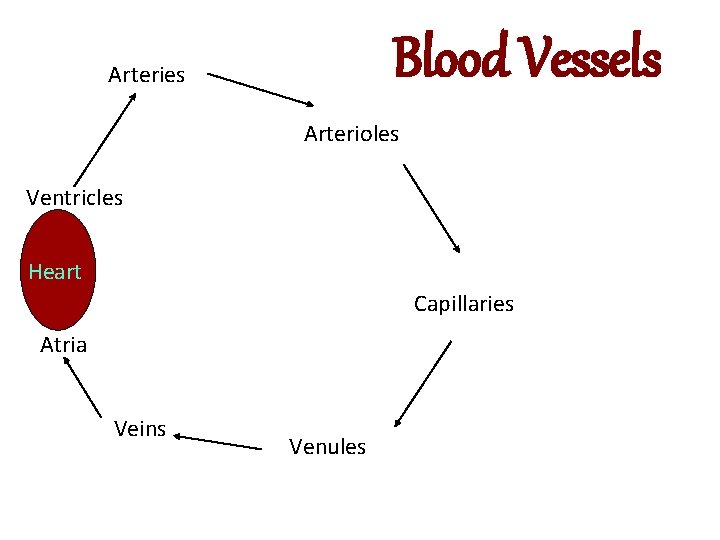
Blood Vessels Arteries Arterioles Ventricles Heart Capillaries Atria Veins Venules
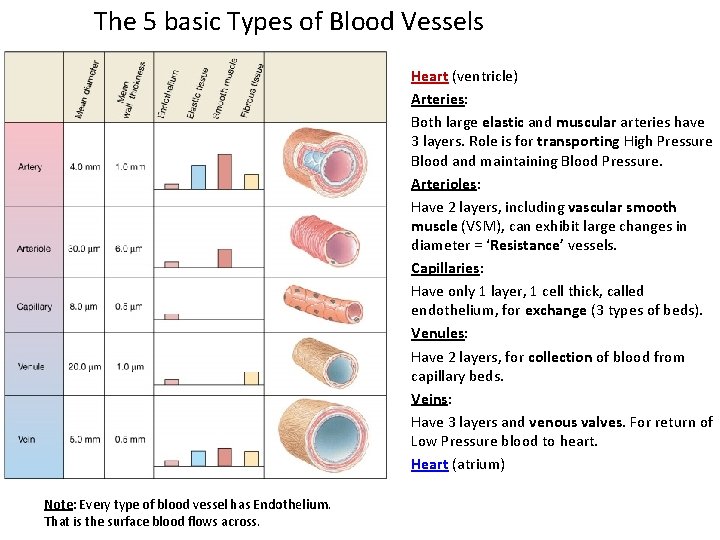
The 5 basic Types of Blood Vessels Heart (ventricle) Arteries: Both large elastic and muscular arteries have 3 layers. Role is for transporting High Pressure Blood and maintaining Blood Pressure. Arterioles: Have 2 layers, including vascular smooth muscle (VSM), can exhibit large changes in diameter = ‘Resistance’ vessels. Capillaries: Have only 1 layer, 1 cell thick, called endothelium, for exchange (3 types of beds). Venules: Have 2 layers, for collection of blood from capillary beds. Veins: Have 3 layers and venous valves. For return of Low Pressure blood to heart. Heart (atrium) Note: Every type of blood vessel has Endothelium. That is the surface blood flows across.
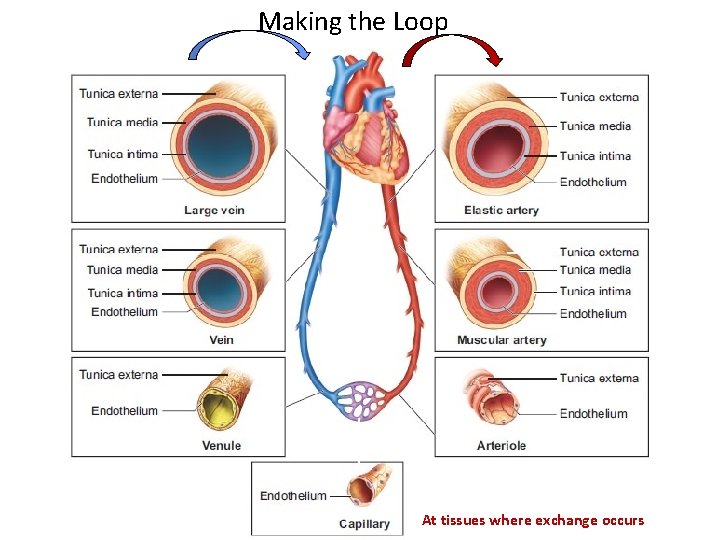
Making the Loop At tissues where exchange occurs
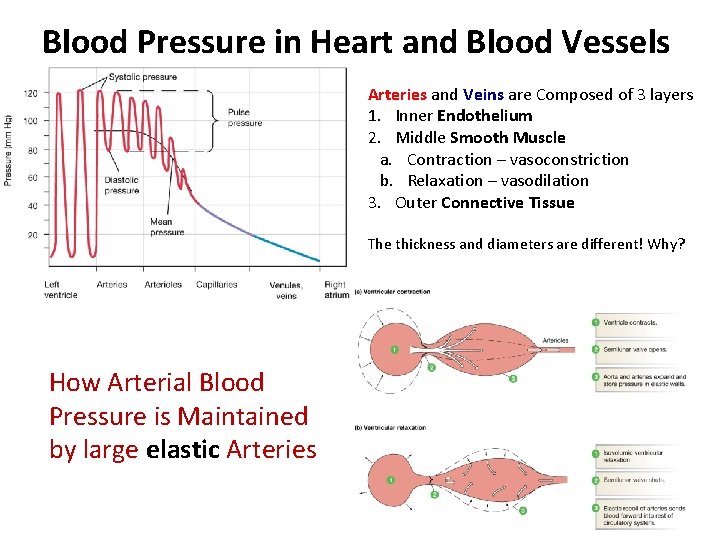
Blood Pressure in Heart and Blood Vessels Arteries and Veins are Composed of 3 layers 1. Inner Endothelium 2. Middle Smooth Muscle a. Contraction – vasoconstriction b. Relaxation – vasodilation 3. Outer Connective Tissue The thickness and diameters are different! Why? How Arterial Blood Pressure is Maintained by large elastic Arteries

List 5 important differences Between Arteries and Veins 1. 2. 3. 4. 5.
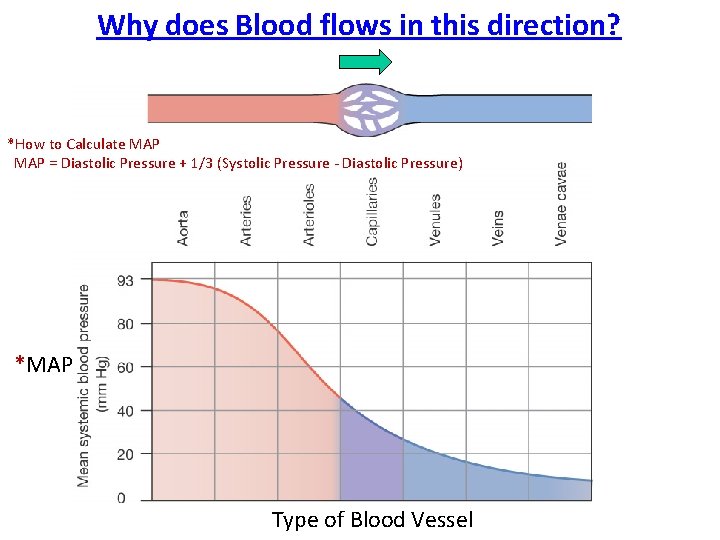
Why does Blood flows in this direction? *How to Calculate MAP = Diastolic Pressure + 1/3 (Systolic Pressure - Diastolic Pressure) *MAP Type of Blood Vessel
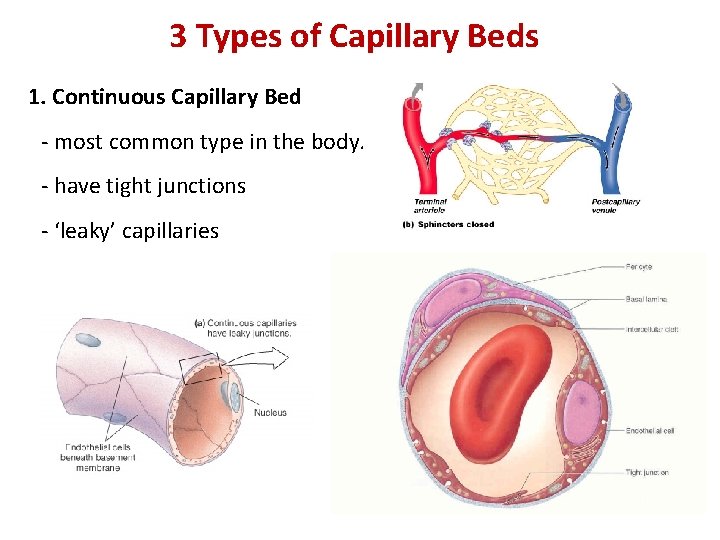
3 Types of Capillary Beds 1. Continuous Capillary Bed - most common type in the body. - have tight junctions - ‘leaky’ capillaries
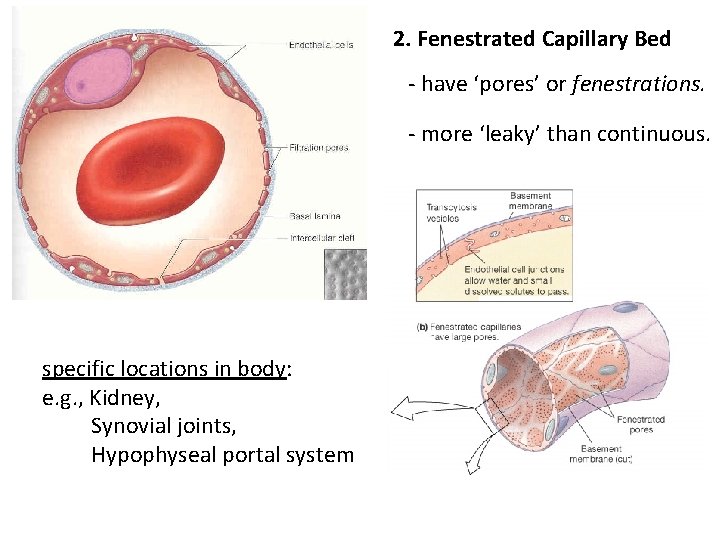
2. Fenestrated Capillary Bed - have ‘pores’ or fenestrations. - more ‘leaky’ than continuous. specific locations in body: e. g. , Kidney, Synovial joints, Hypophyseal portal system
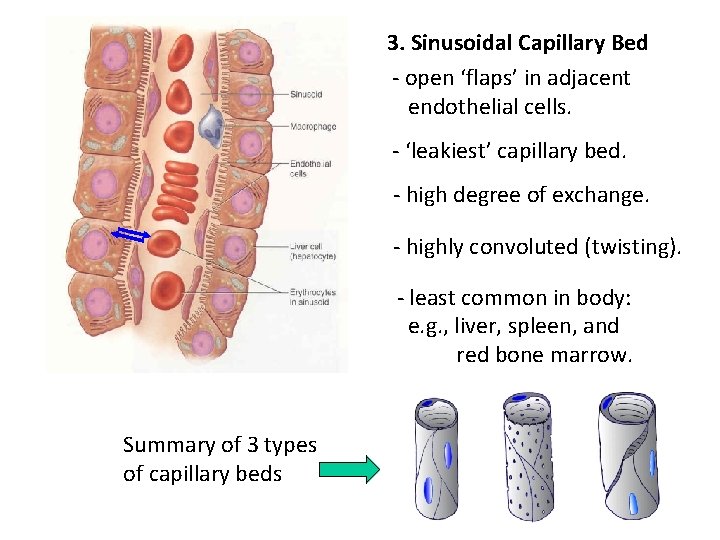
3. Sinusoidal Capillary Bed - open ‘flaps’ in adjacent endothelial cells. - ‘leakiest’ capillary bed. - high degree of exchange. - highly convoluted (twisting). - least common in body: e. g. , liver, spleen, and red bone marrow. Summary of 3 types of capillary beds
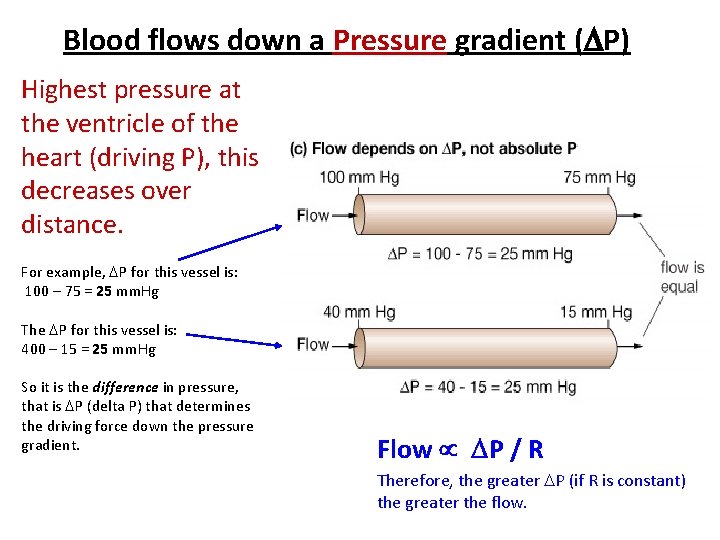
Blood flows down a Pressure gradient ( P) Highest pressure at the ventricle of the heart (driving P), this decreases over distance. For example, P for this vessel is: 100 – 75 = 25 mm. Hg The P for this vessel is: 400 – 15 = 25 mm. Hg So it is the difference in pressure, that is P (delta P) that determines the driving force down the pressure gradient. Flow P / R Therefore, the greater P (if R is constant) the greater the flow.

Resistance (R) Opposes Flow 3 Factors Influence Resistance of fluid flow in a Tube: 1) Length (l) of tube (vessel): length = Resistance viscosity 2) Viscosity (n) of fluid (blood): = Resistance 3) Diameter (radius, r) of tube (vessel): radius = Resistance Note: Factors 1) and 2) do not change much in the body, so we can ignore them. In this way, when we talk about Resistance (R), it’s mostly caused by changes in vessel radius (r). This means we can alter the formula for R : ) See the next slide. Flow P / R Therefore, the greater R (if P is constant) the lower the flow.
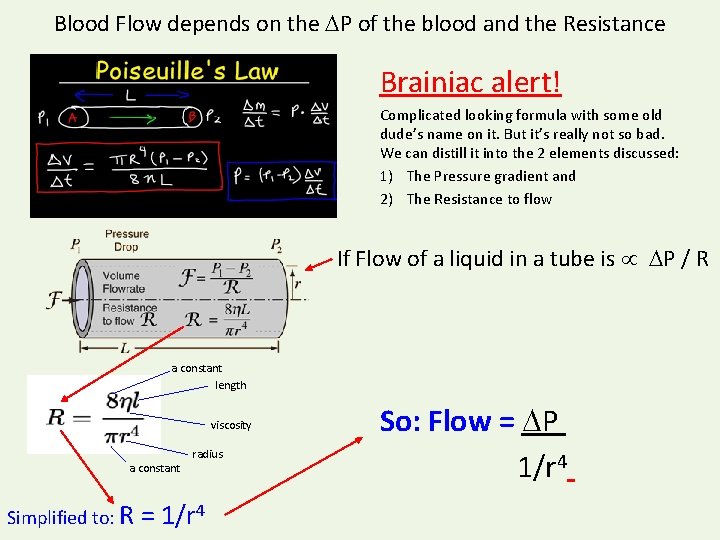
Blood Flow depends on the P of the blood and the Resistance Brainiac alert! Complicated looking formula with some old dude’s name on it. But it’s really not so bad. We can distill it into the 2 elements discussed: 1) The Pressure gradient and 2) The Resistance to flow If Flow of a liquid in a tube is P / R a constant length viscosity a constant Simplified to: R radius = 1/r 4 So: Flow = P 1/r 4

Exercise: Do Calculations of “Flow” through a Vessel: Blood flow through a vessel depends on the pressure gradient and resistance. Write a simple formula for blood flow. __________. Write a simplified version of Poiseuilles’s Law to describe Resistance (R) to flow. Use the information above to calculate the “Flow” (ignore units) of blood through vessels A and B below. Vessel A: P 1 = 35 mm Hg P 2 = 15 mm Hg P = Vessels radius (r) = 2 mm R= Flow = Vessel B: P 1 = 90 mm Hg P 2 = 20 mm Hg P = Vessel radius (r) = 1 mm R= Flow =
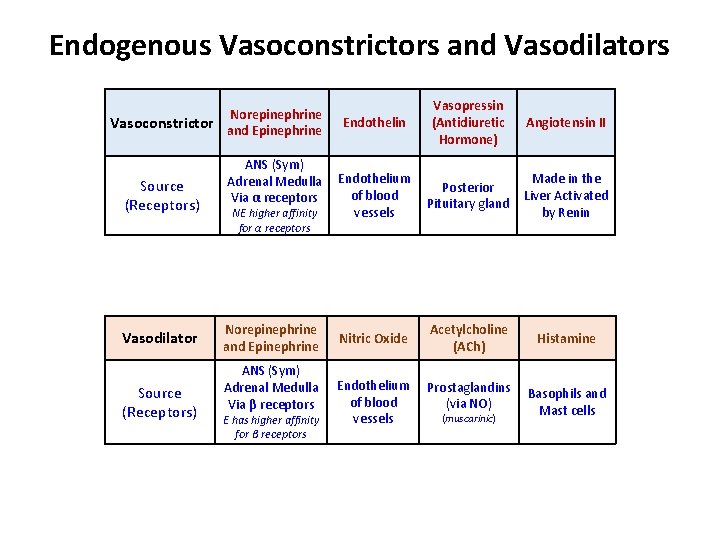
Endogenous Vasoconstrictors and Vasodilators Norepinephrine Vasoconstrictor and Epinephrine Source (Receptors) Vasodilator Source (Receptors) ANS (Sym) Adrenal Medulla Via α receptors NE higher affinity for α receptors Norepinephrine and Epinephrine ANS (Sym) Adrenal Medulla Via β receptors E has higher affinity for β receptors Endothelin Vasopressin (Antidiuretic Hormone) Angiotensin II Endothelium of blood vessels Posterior Pituitary gland Made in the Liver Activated by Renin Nitric Oxide Acetylcholine (ACh) Histamine Endothelium of blood vessels Prostaglandins (via NO) Basophils and Mast cells (muscarinic)
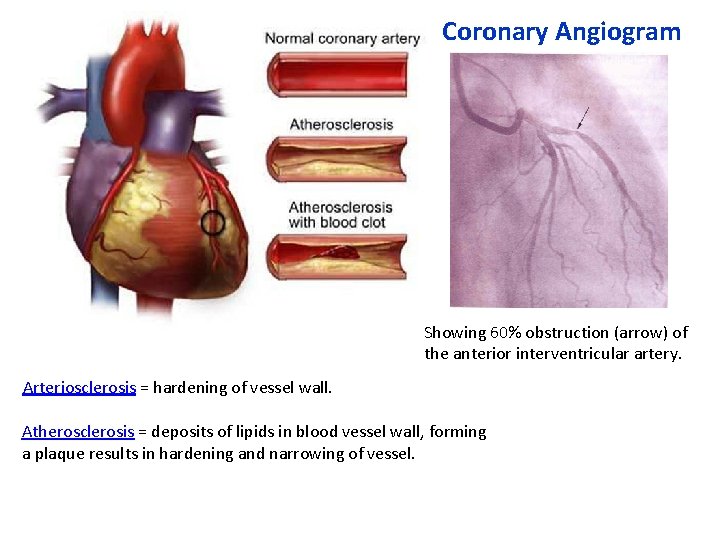
Coronary Angiogram Showing 60% obstruction (arrow) of the anterior interventricular artery. Arteriosclerosis = hardening of vessel wall. Atherosclerosis = deposits of lipids in blood vessel wall, forming a plaque results in hardening and narrowing of vessel.
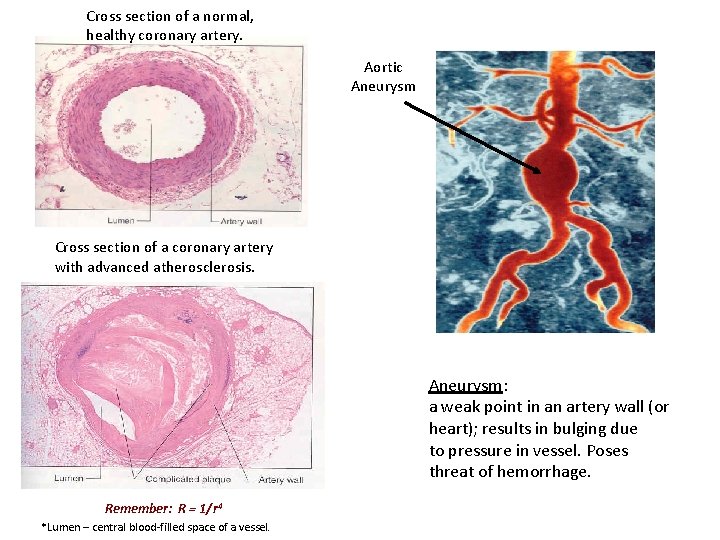
Cross section of a normal, healthy coronary artery. Aortic Aneurysm Cross section of a coronary artery with advanced atherosclerosis. Aneurysm: a weak point in an artery wall (or heart); results in bulging due to pressure in vessel. Poses threat of hemorrhage. Remember: R = 1/r 4 *Lumen – central blood-filled space of a vessel.
Mean Arterial Pressure (MAP) Essentially determined by these 4 Factors 1. Cardiac Output 2. Peripheral Resistance 3. Total Blood Volume 4. Distribution of Blood
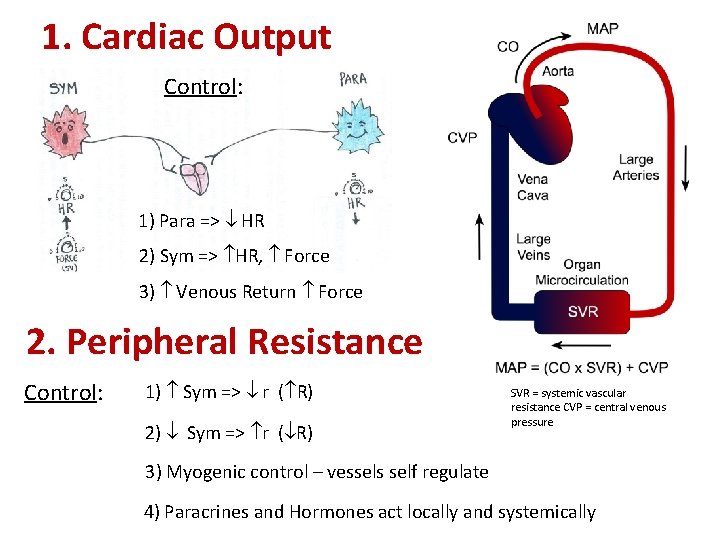
1. Cardiac Output Control: 1) Para => HR 2) Sym => HR, Force 3) Venous Return Force 2. Peripheral Resistance Control: 1) Sym => r ( R) 2) Sym => r ( R) SVR = systemic vascular resistance CVP = central venous pressure 3) Myogenic control – vessels self regulate 4) Paracrines and Hormones act locally and systemically
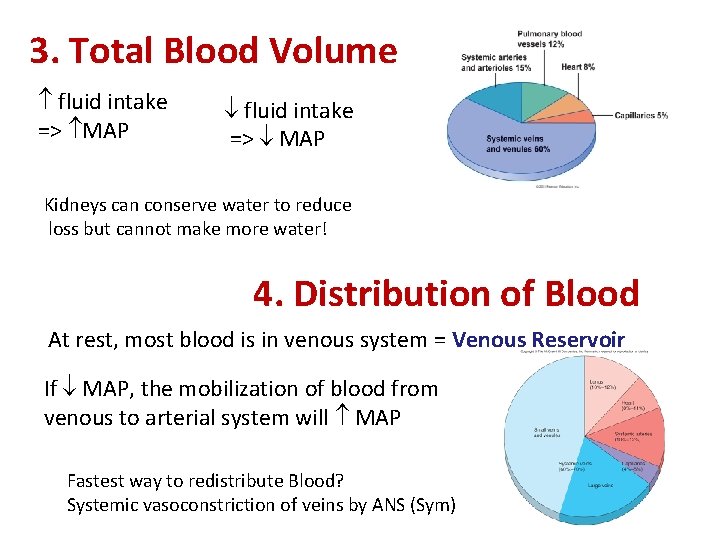
3. Total Blood Volume fluid intake => MAP fluid intake => MAP Kidneys can conserve water to reduce loss but cannot make more water! 4. Distribution of Blood At rest, most blood is in venous system = Venous Reservoir If MAP, the mobilization of blood from venous to arterial system will MAP Fastest way to redistribute Blood? Systemic vasoconstriction of veins by ANS (Sym)
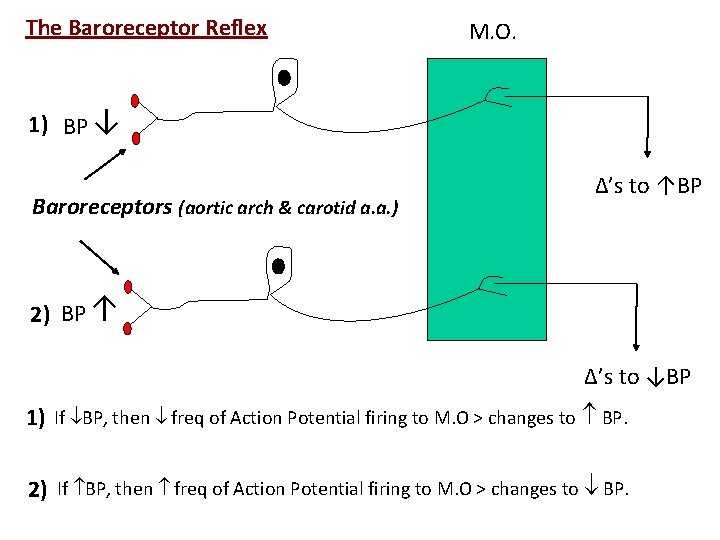
The Baroreceptor Reflex M. O. 1) BP ↓ Baroreceptors (aortic arch & carotid a. a. ) ∆’s to ↑BP 2) BP ↑ ∆’s to ↓BP 1) If BP, then freq of Action Potential firing to M. O > changes to BP. 2) If BP, then freq of Action Potential firing to M. O > changes to BP.

What is Cardiovascular Shock ? It is a failure of the cardiovascular system to adequately perfuse the tissues of the body 1. Cardiogenic 3. Anaphylactic 2. Volumetric 4. Septic
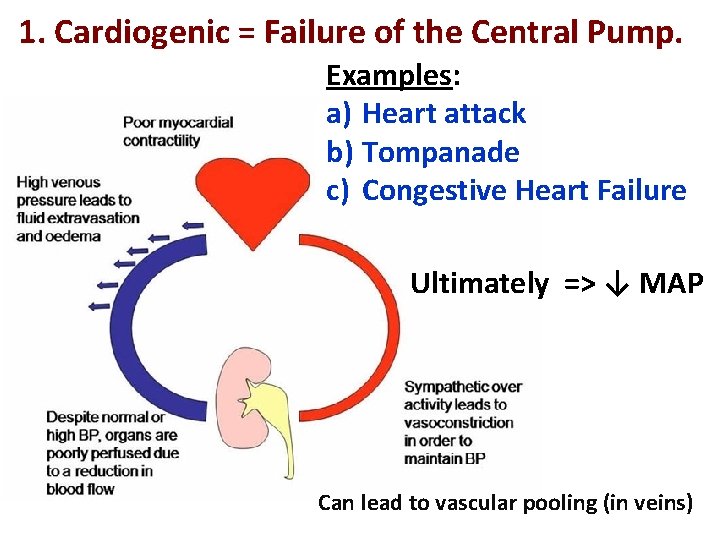
1. Cardiogenic = Failure of the Central Pump. Examples: a) Heart attack b) Tompanade c) Congestive Heart Failure Ultimately => ↓ MAP Can lead to vascular pooling (in veins)

2. Volumetric or Hemorrhagic Shock Significant ↓ in total blood volume. Examples: a) Hemorrhage b) Sever dehydration Table for Class of Volumetric Stroke by amount of Blood loss Class (Volume) I II IV Blood Loss <15% (0. 75 L) 15 -30% (0. 75 -1. 5 L) 30 -40% (1. 5 -2 L) >40% (>2 L) Response ↑ HR Normal BP ↑ HR ↓BP ↑↑ HR↓BP Confusion Critical BP and HR Treatment Minimal I. V. fluids and RBCs Aggressive interventions All =↓ MAP

3. Anaphylactic = Allergic Response. This is an ‘inappropriate’ immune response. Examples: a) Bee sting b) Certain foods (fish, peanuts) c) Medications A ‘harmless’ allergen triggers a massive immune response.

3. Anaphylactic = Allergic Response. Involves the systemic release of histamine, causing massive systemic vasodilation. Leads to vascular pooling (in veins) ↓ MAP Additionally causes: Severe swelling and constriction of bronchioles (↓ air flow). *Epi-Pen

4. Septic = Overwhelming Infection Appropriate immune response! Examples: a) Septicaemia = blood poisoning. b) Bacteria releasing -blockers. * -blockers prevent NE from counter-acting histamine, leads to vascular pooling (↓ MAP).
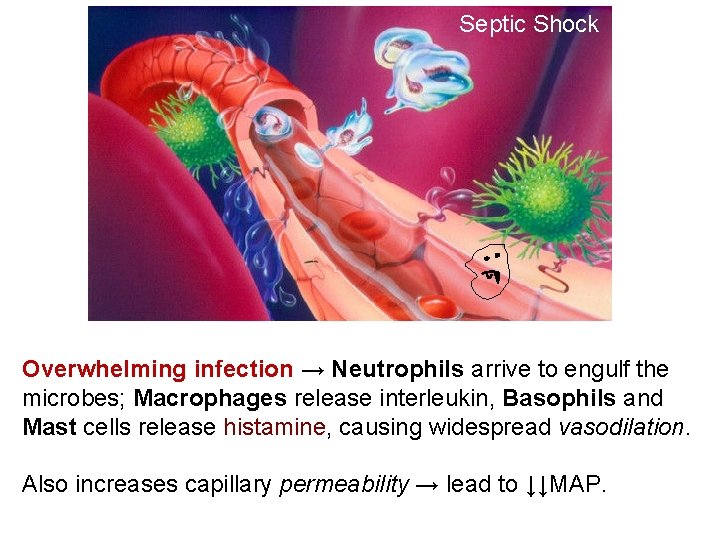
Septic Shock Overwhelming infection → Neutrophils arrive to engulf the microbes; Macrophages release interleukin, Basophils and Mast cells release histamine, causing widespread vasodilation. Also increases capillary permeability → lead to ↓↓MAP.

How does Body Respond to Shock? Ans: Activation of the Sympathetic division of ANS HR and Force (SV) = pump (C. O. ) Venous Vasoconstriction = venous return Water conservation by Kidneys. = Urine output Filtration at capillaries = Interstitial Fluid
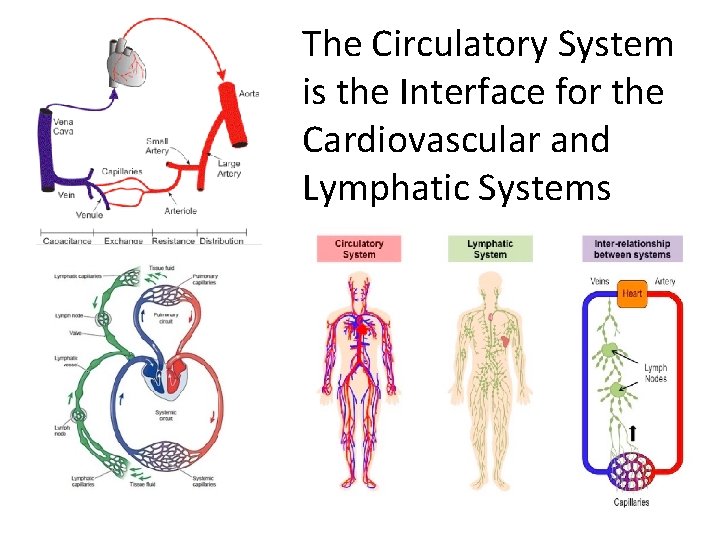
The Circulatory System is the Interface for the Cardiovascular and Lymphatic Systems
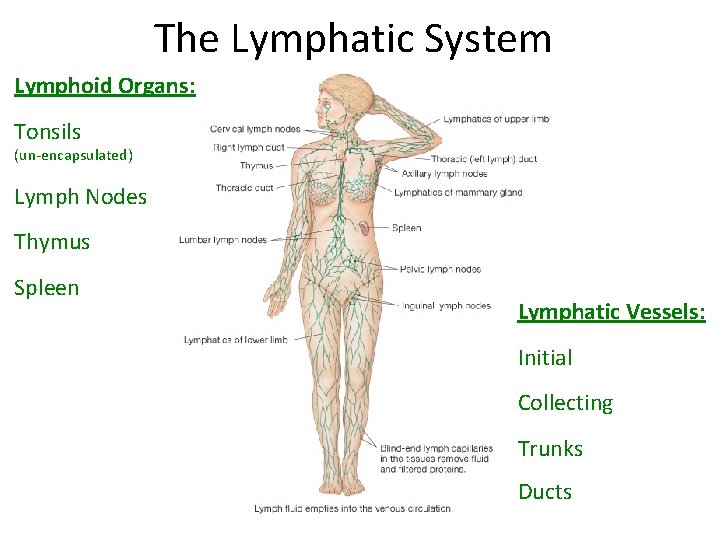
The Lymphatic System Lymphoid Organs: Tonsils (un-encapsulated) Lymph Nodes Thymus Spleen Lymphatic Vessels: Initial Collecting Trunks Ducts

Roles of the Lymphatic System • One-way drainage system. 2) Lipid Absorption from Small Intestine. 3) Produce & circulates Immune cells.
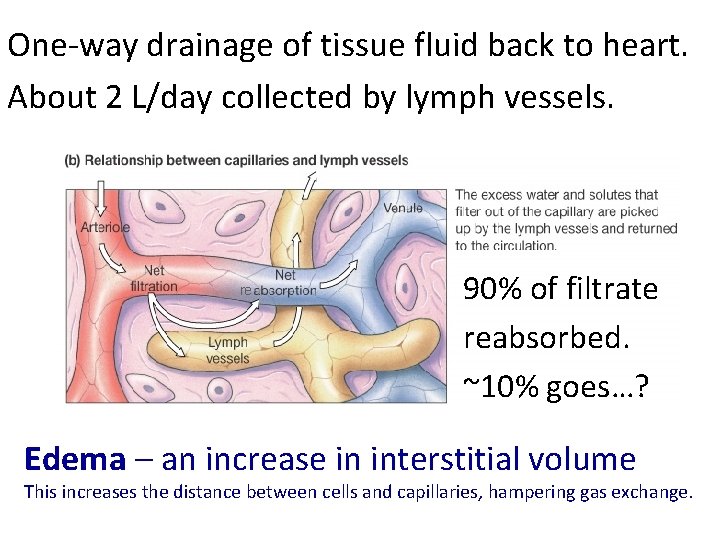
One-way drainage of tissue fluid back to heart. About 2 L/day collected by lymph vessels. re 90% of filtrate reabsorbed. ~10% goes…? Edema – an increase in interstitial volume This increases the distance between cells and capillaries, hampering gas exchange.
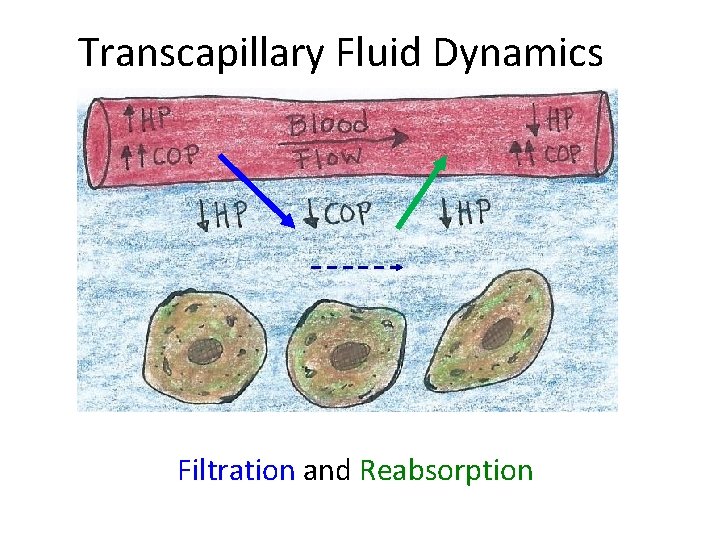
Transcapillary Fluid Dynamics Filtration and Reabsorption

Edema can occur in 2 main ways: 1) Transcapillary Fluid dynamics are Upset. – HPcap increases interstitial volume – COPcap increases interstitial volume – HPi increases interstitial volume – COPi increases interstitial volume 2) Blockage of Lymphatic vessels.
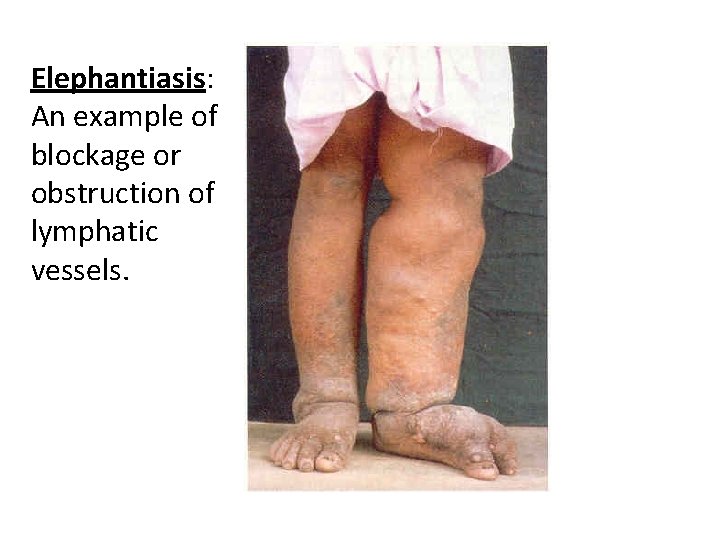
Elephantiasis: An example of blockage or obstruction of lymphatic vessels.
- Slides: 35