Blood Vessels and Hemodynamics Types of blood vessels

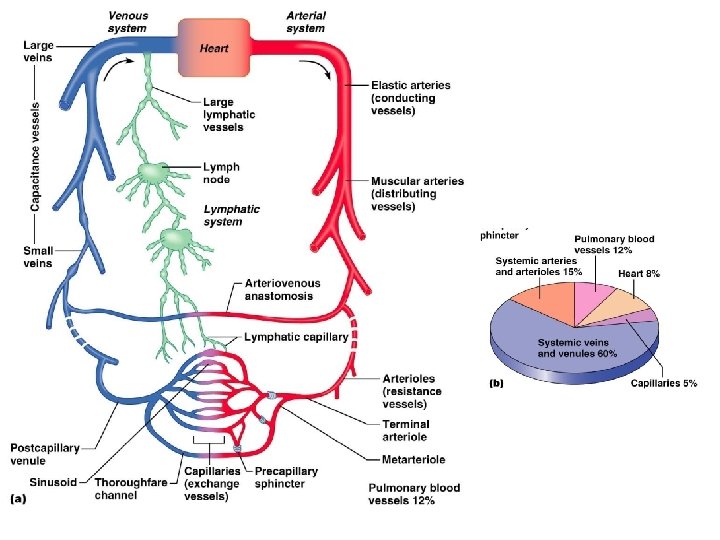
Blood Vessels and Hemodynamics

Types of blood vessels • Arteries divide – Elastic (conducting) arteries – Muscular arteries • • Arterioles branch into Capillaries reunite to form Venules merge into Veins converge and convey blood back to the heart
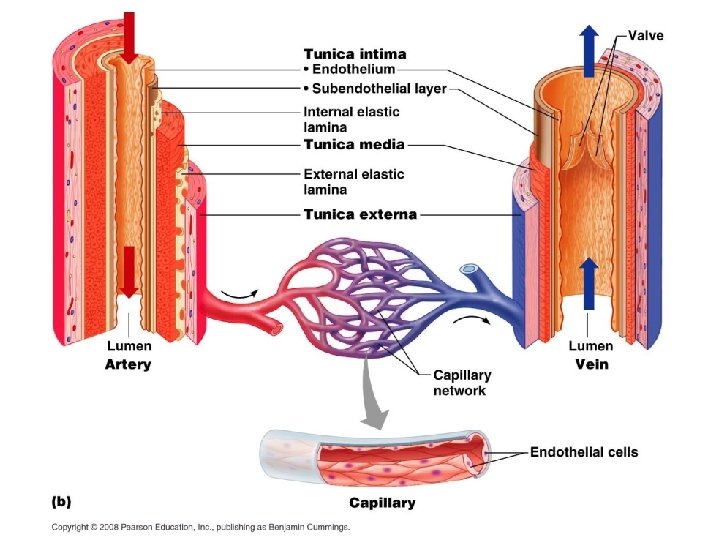
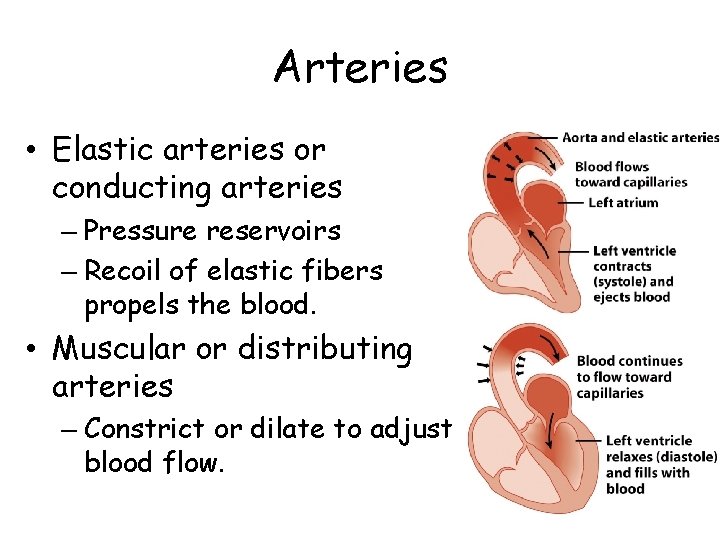
Arteries • Elastic arteries or conducting arteries – Pressure reservoirs – Recoil of elastic fibers propels the blood. • Muscular or distributing arteries – Constrict or dilate to adjust blood flow.
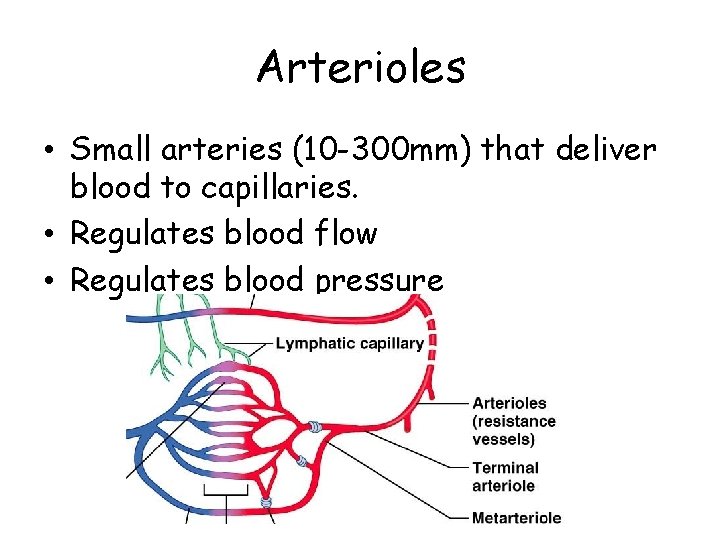
Arterioles • Small arteries (10 -300 mm) that deliver blood to capillaries. • Regulates blood flow • Regulates blood pressure

Continuous Capillaries
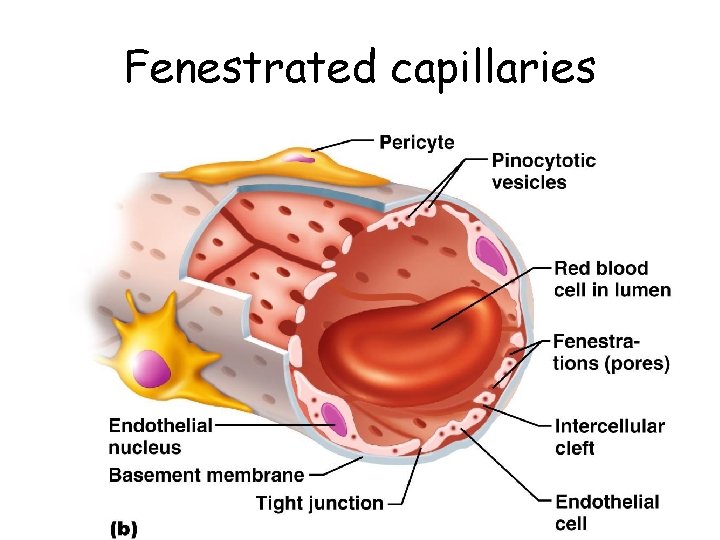
Fenestrated capillaries
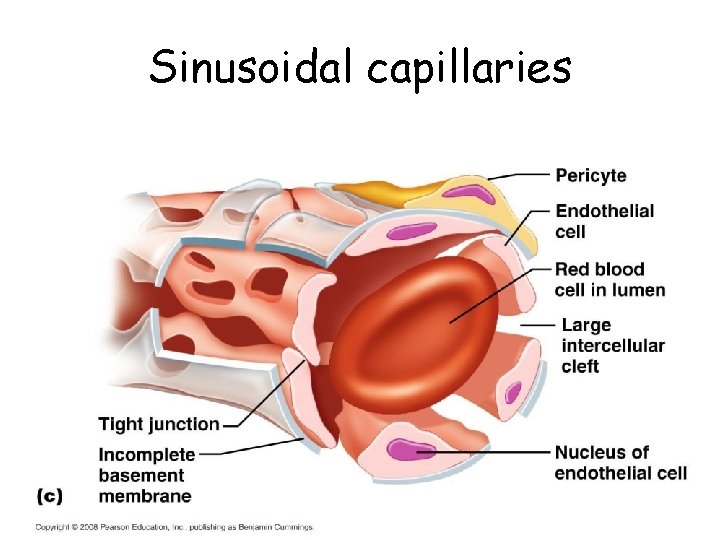
Sinusoidal capillaries
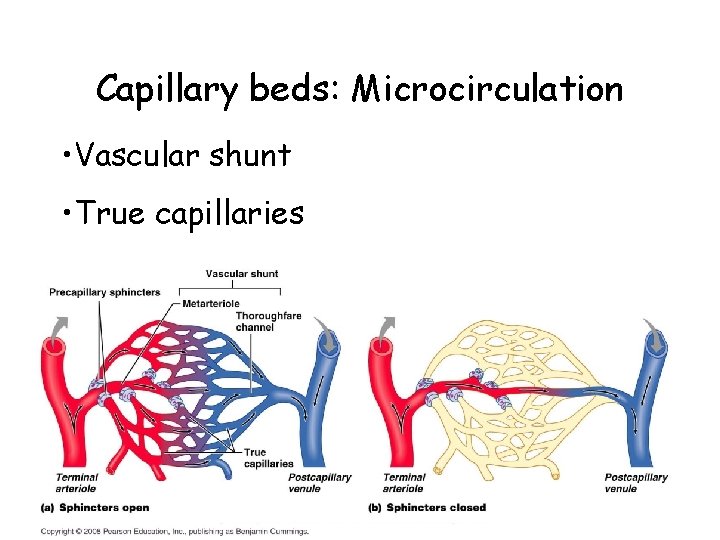
Capillary beds: Microcirculation • Vascular shunt • True capillaries
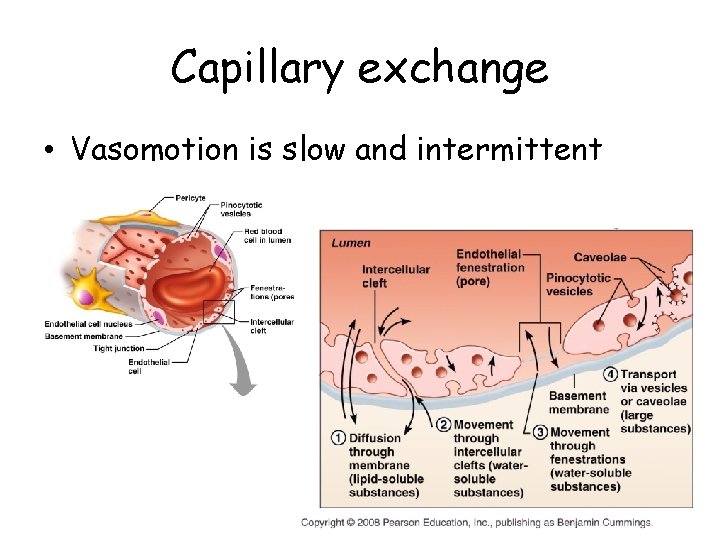
Capillary exchange • Vasomotion is slow and intermittent
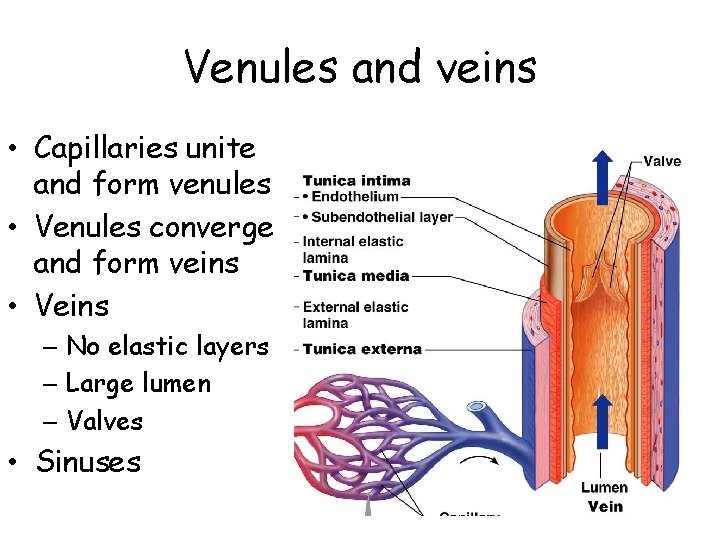
Venules and veins • Capillaries unite and form venules • Venules converge and form veins • Veins – No elastic layers – Large lumen – Valves • Sinuses
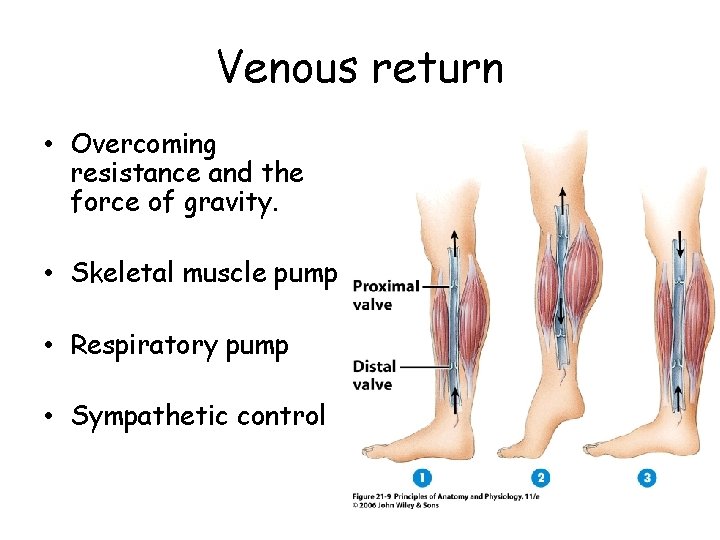
Venous return • Overcoming resistance and the force of gravity. • Skeletal muscle pump • Respiratory pump • Sympathetic control
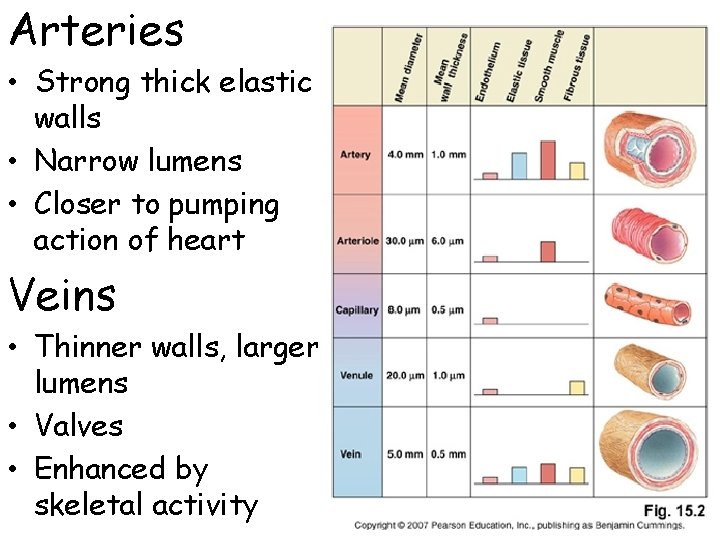
Arteries • Strong thick elastic walls • Narrow lumens • Closer to pumping action of heart Veins • Thinner walls, larger lumens • Valves • Enhanced by skeletal activity
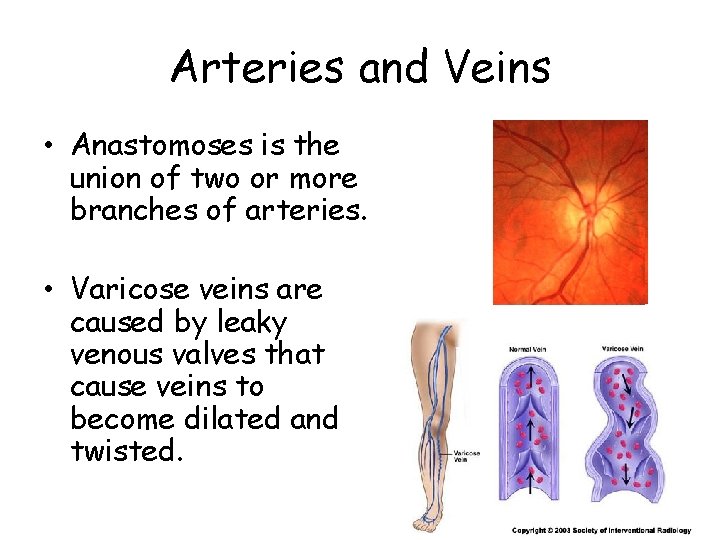
Arteries and Veins • Anastomoses is the union of two or more branches of arteries. • Varicose veins are caused by leaky venous valves that cause veins to become dilated and twisted.
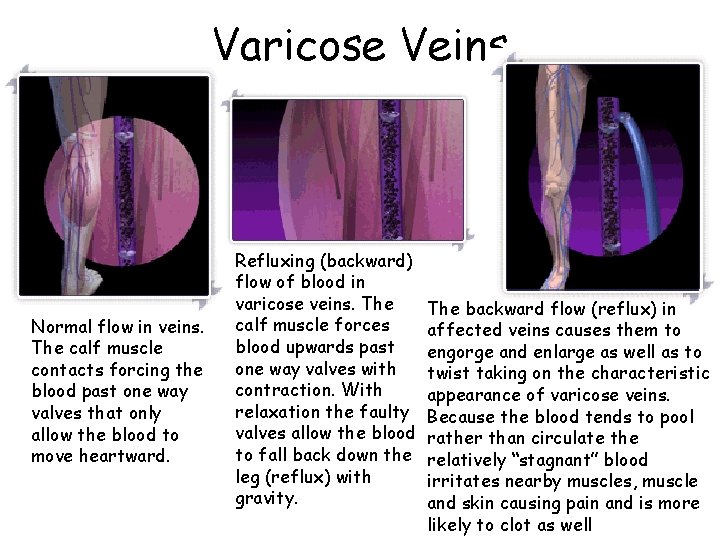
Varicose Veins Normal flow in veins. The calf muscle contacts forcing the blood past one way valves that only allow the blood to move heartward. Refluxing (backward) flow of blood in varicose veins. The calf muscle forces blood upwards past one way valves with contraction. With relaxation the faulty valves allow the blood to fall back down the leg (reflux) with gravity. The backward flow (reflux) in affected veins causes them to engorge and enlarge as well as to twist taking on the characteristic appearance of varicose veins. Because the blood tends to pool rather than circulate the relatively “stagnant” blood irritates nearby muscles, muscle and skin causing pain and is more likely to clot as well

Physiology of blood • Blood flow (ml/min) • Blood pressure (mm Hg) – force generated against arterial walls per unit of area in mm Hg.
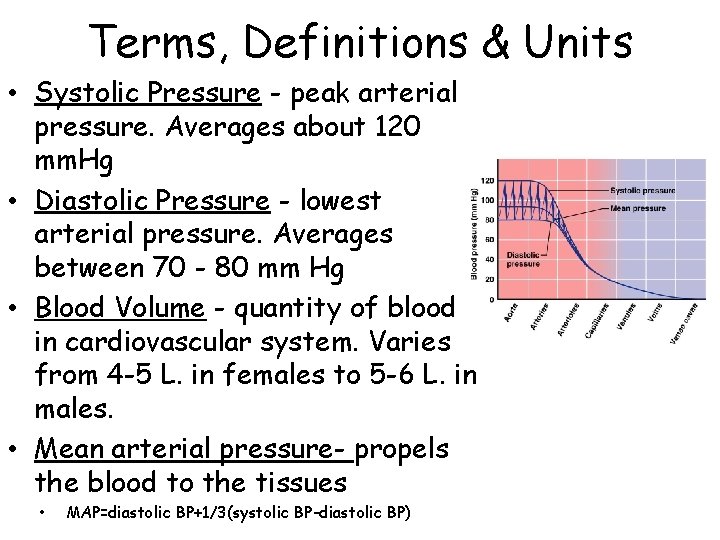
Terms, Definitions & Units • Systolic Pressure - peak arterial pressure. Averages about 120 mm. Hg • Diastolic Pressure - lowest arterial pressure. Averages between 70 - 80 mm Hg • Blood Volume - quantity of blood in cardiovascular system. Varies from 4 -5 L. in females to 5 -6 L. in males. • Mean arterial pressure- propels the blood to the tissues • MAP=diastolic BP+1/3(systolic BP-diastolic BP)
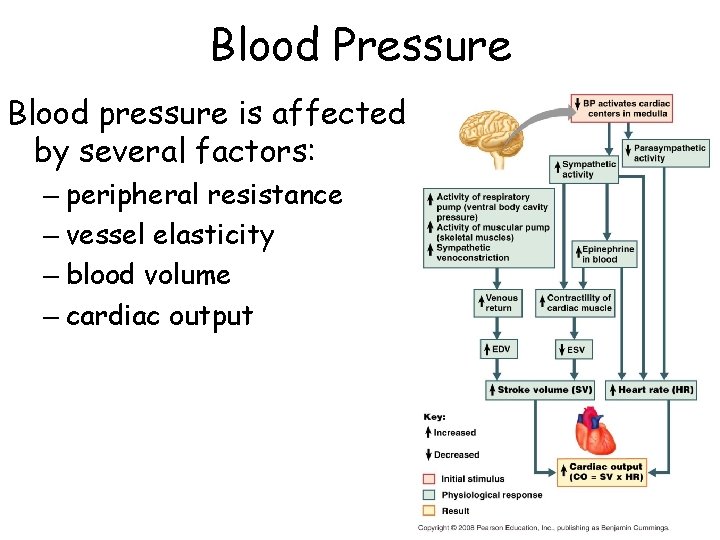
Blood Pressure Blood pressure is affected by several factors: – peripheral resistance – vessel elasticity – blood volume – cardiac output

Peripheral Resistance Blood cells and plasma encounter resistance when they contact blood vessel walls. • If resistance , then more pressure is needed to keep blood moving. Three main sources of peripheral resistance: – blood vessel diameter – blood viscosity – total vessel length F = DP/R
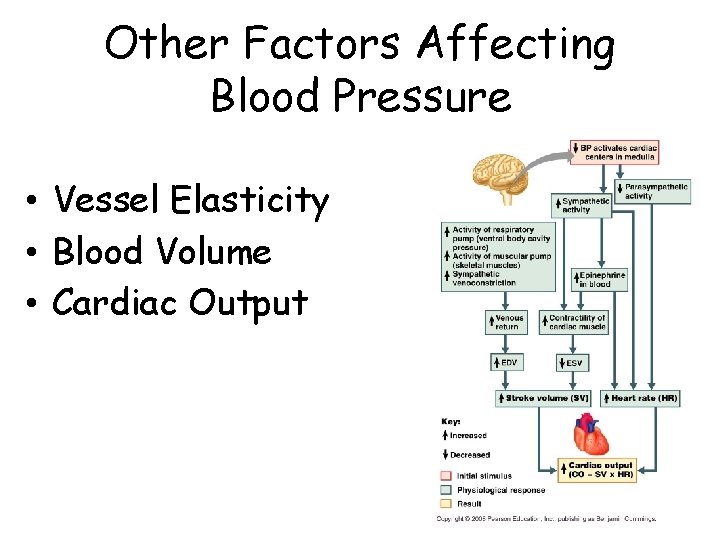
Other Factors Affecting Blood Pressure • Vessel Elasticity • Blood Volume • Cardiac Output

Velocity of blood flow • Velocity is inversely related to the crosssectional area. – The greater the cross section, the slower the blood. • Branching of blood vessels slows velocity. • Veins coming together increases velocity
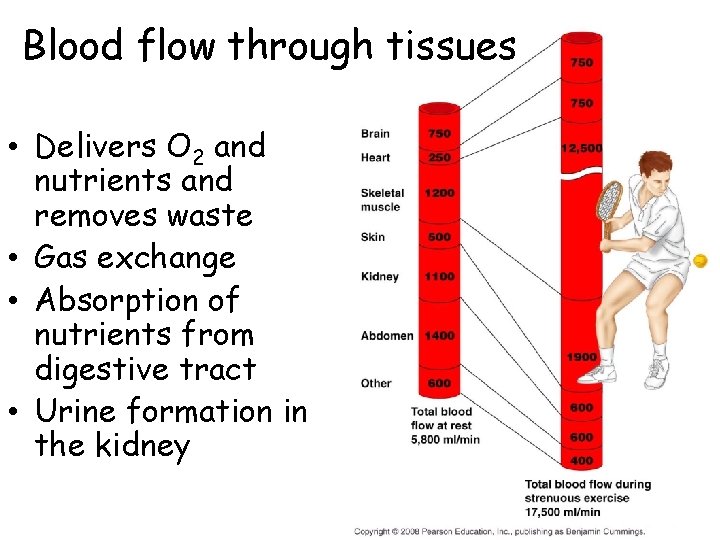
Blood flow through tissues • Delivers O 2 and nutrients and removes waste • Gas exchange • Absorption of nutrients from digestive tract • Urine formation in the kidney
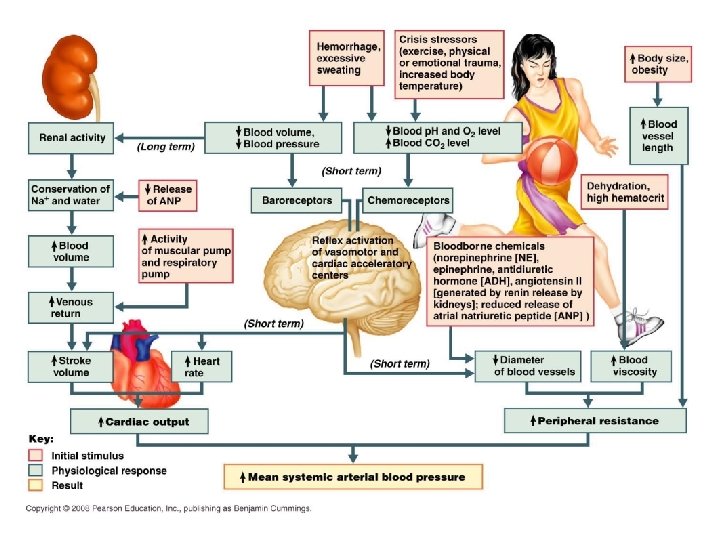
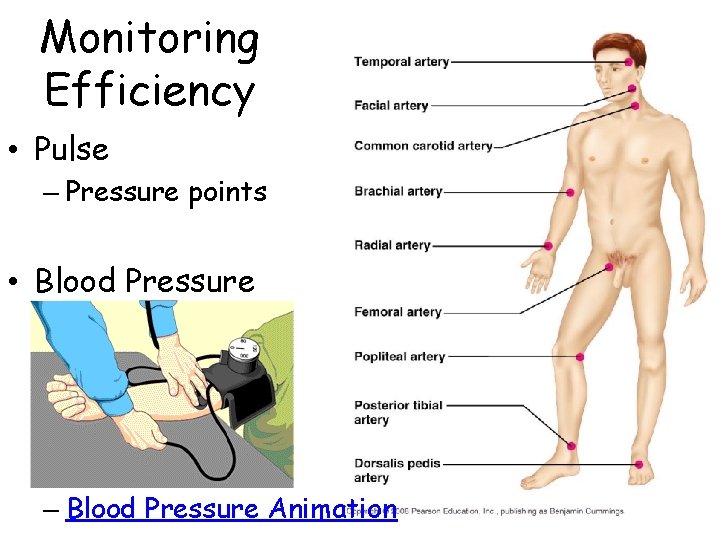
Monitoring Efficiency • Pulse – Pressure points • Blood Pressure – Blood Pressure Animation
Blood Pressure
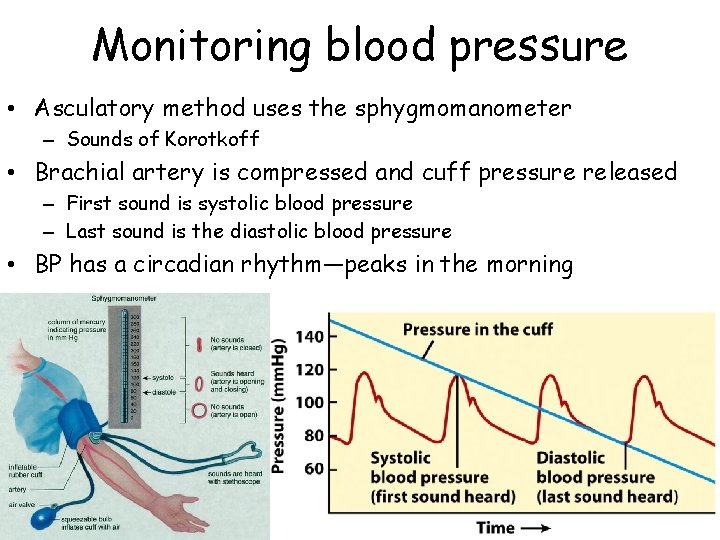
Monitoring blood pressure • Asculatory method uses the sphygmomanometer – Sounds of Korotkoff • Brachial artery is compressed and cuff pressure released – First sound is systolic blood pressure – Last sound is the diastolic blood pressure • BP has a circadian rhythm—peaks in the morning

Homeostatic Blood Pressure Regulation Mechanisms • Medullary Reflex Centers: – Cardioacceleratory - increases heart rate – Cardioinhibitory - decreases heart rate – Vasomotor - changes diameter of vessels • Baroreceptors in aortic arch & carotid sinuses: – sensitive to changes in blood pressure. BP - Stimulates Cardioinhibitory center to Vasomotor center to diameter. BP - Stimulates Cardioacceleratory center to heart rate & Vasomotor center to diameter. heart rate &

Homeostatic Blood Pressure Regulation Mechanisms • Medullary Reflex Centers: – Cardioacceleratory - increases heart rate – Cardioinhibitory - decreases heart rate – Vasomotor - changes diameter of vessels • Chemoreceptors in aortic bodies & carotid bodies: – sensitive to changes in CO 2 & O 2 in blood. in CO 2 or in O 2 stimulates Vasomotor center to diameter (vasoconstrict) of vessels to BP. in CO 2 stimulates Vasomotor center to diameter (vasodilate) of vessels to BP.

Hypertension • High blood pressure. • Sustained arterial blood pressure of 140/90 mm Hg or above. • Rising diastolic pressure generally indicative of progressive hardening of arteries. • Since the heart must work harder to pump blood against higher pressures, there is increased risk of a cardiovascular accident.
Primary hypertension • Diet—high intake of Na+, saturated fats or deficiencies in K+, Ca 2+, or Mg 2+ • Obesity • Age—over 40 • Diabetes mellitus • Heredity • Stress • Smoking

Hypotension • Abnormally low blood pressure. • Sustained systolic blood pressure of below 100 mm Hg. • Generally associated with lower risk of cardiovascular accidents & long life providing that the tissues are adequately perfused. .
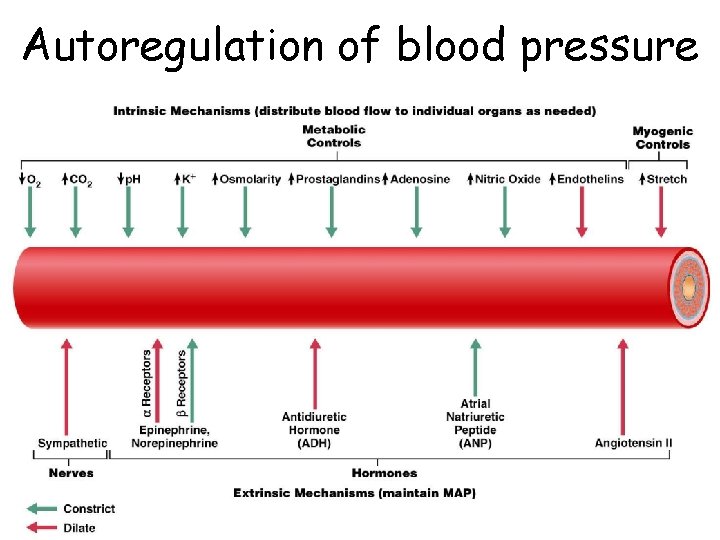
Autoregulation of blood pressure

Shock and homeostasis • Shock is the failure to deliver enough O 2 to meet cellular metabolic needs. • Four types of shock 1. Hypovolemic shock—drop in fluid levels 2. Cardiogenic shock—failure of heart to pump 3. Vascular shock—decrease in vascular resistance 4. Obstructive shock—blood flow through a portion of the circulation is blocked.

Signs and symptoms of shock • • • Systolic blood pressure below 90 mm. Hg Weak and rapid pulse Rapid heart rate Cool and damp skin Altered mental state Reduced urine formation Thirst Acidosis (low blood p. H) Nausea
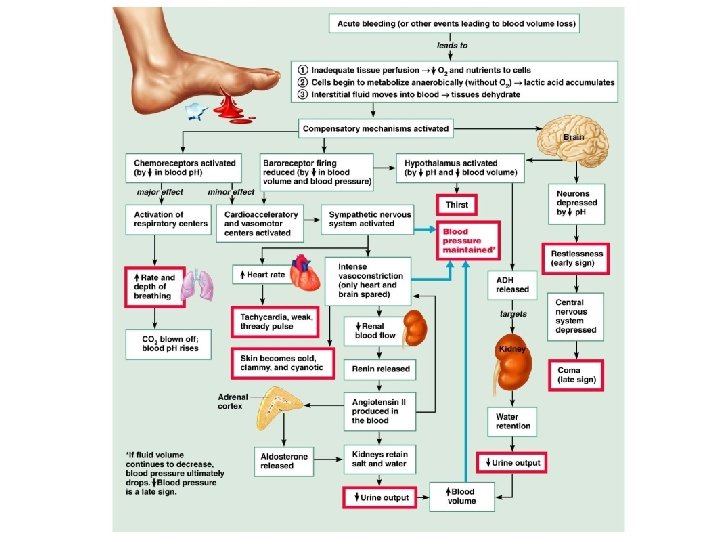

Circulatory Shock • Blood vessels inadequately filled to enable normal circulation & supply of O 2 & nutrients. • May result in death of cells & damage to organs. • • • Common Types: Hypovolemic - severe blood loss Cardiogenic - heart (pump) failure Vascular - excessive vasodilation Septicemic - vasodilation due to bacterial toxins produced during an infection.
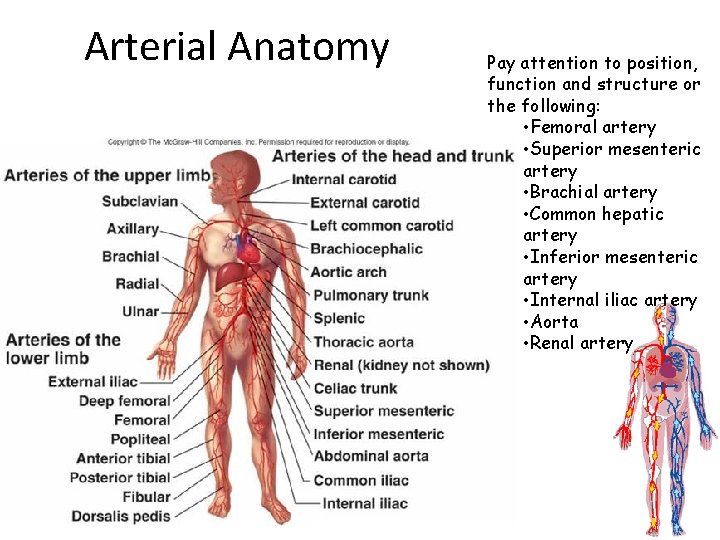
Arterial Anatomy Pay attention to position, function and structure or the following: • Femoral artery • Superior mesenteric artery • Brachial artery • Common hepatic artery • Inferior mesenteric artery • Internal iliac artery • Aorta • Renal artery
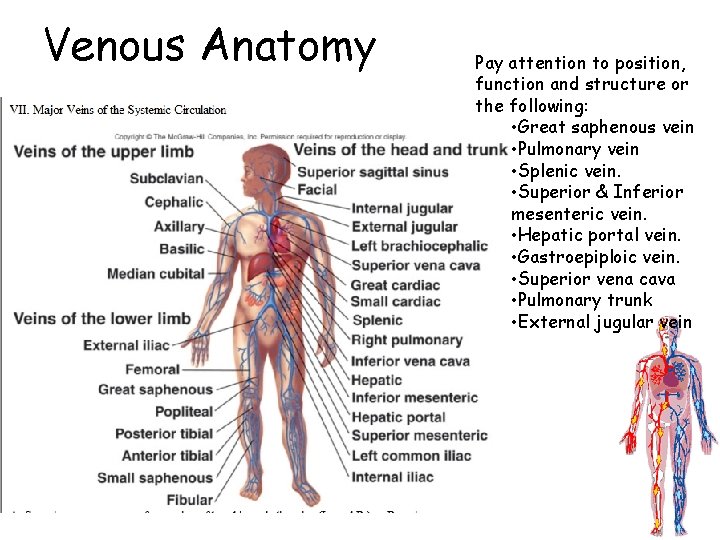
Venous Anatomy Pay attention to position, function and structure or the following: • Great saphenous vein • Pulmonary vein • Splenic vein. • Superior & Inferior mesenteric vein. • Hepatic portal vein. • Gastroepiploic vein. • Superior vena cava • Pulmonary trunk • External jugular vein

Resources • Rutgers Blood Vessels
- Slides: 40