Blood Transfusions Blood Transfusion Therapy Verify identity of
Blood Transfusions

Blood Transfusion Therapy • Verify identity of recipient • • and of donor’s blood group Monitor vital signs Use appropriate filter Use blood within 30 minutes of arrival Infuse over 4 hours maximum
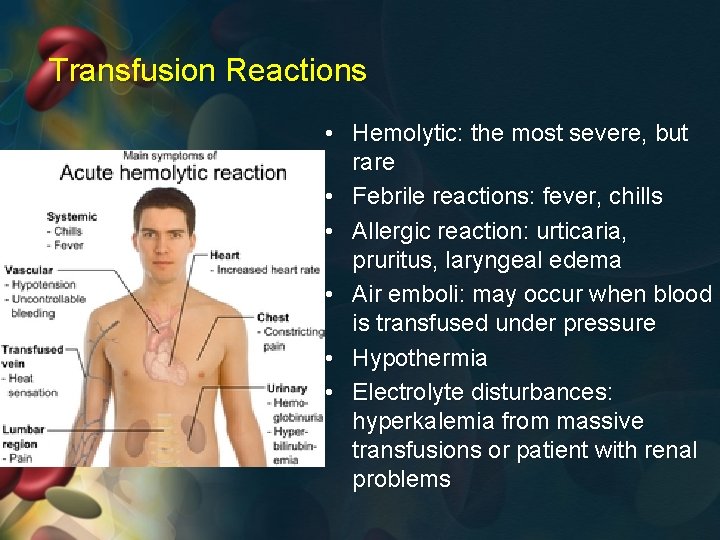
Transfusion Reactions • Hemolytic: the most severe, but rare • Febrile reactions: fever, chills • Allergic reaction: urticaria, pruritus, laryngeal edema • Air emboli: may occur when blood is transfused under pressure • Hypothermia • Electrolyte disturbances: hyperkalemia from massive transfusions or patient with renal problems
Delayed Reactions to Blood Transfusion • Transmission of infection: • Hepatitis, HIV, malaria, syphilis, other • Blood banks test vigorously and discard units of infected blood • Delayed hemolytic reaction: • Destruction of RBCs and fever 5 -10 days after transfusion • Observe for posttransfusion anemia

Apheresis • Definition: removal of blood from an individual; separation of the blood into its components • Nursing considerations

Allogeneic Bone Marrow Transplant (BMT) • Involves matching histocompatible donor with recipient • Limited by presence of suitable marrow donor

Umbilical Cord Blood Stem Cell Transplantation • Rich source of hematopoietic stem cells for use in children with cancers • Stem cells found with high frequency in circulation of newborns • Benefit of umbilical cord blood is blood’s relative immunodeficiency at birth, allowing for partially matched unrelated cord blood transplants to be successful

Autologous BMT • Uses patient’s own marrow collected from disease-free tissue, frozen, and sometimes treated to remove malignant cells • Has been used to treat neuroblastoma, Hodgkin disease, NHL, Wilms tumor, rhabdomyosarcoma, and Ewing sarcoma
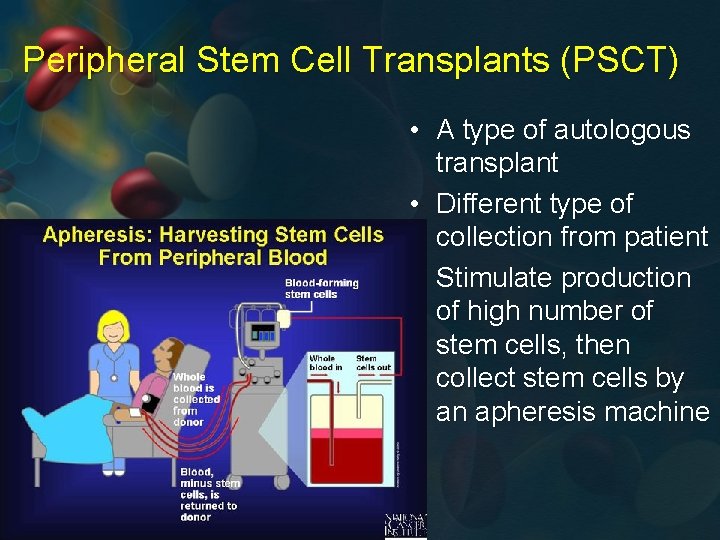
Peripheral Stem Cell Transplants (PSCT) • A type of autologous transplant • Different type of collection from patient • Stimulate production of high number of stem cells, then collect stem cells by an apheresis machine
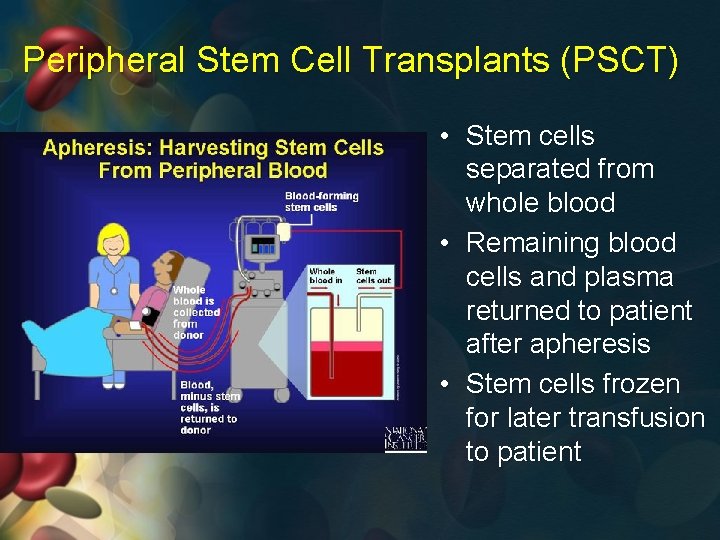
Peripheral Stem Cell Transplants (PSCT) • Stem cells separated from whole blood • Remaining blood cells and plasma returned to patient after apheresis • Stem cells frozen for later transfusion to patient

Family Concerns • Difficult decision for HSCT transplant • Child faces death without transplant • Preparing child for transplant places child at great risk • No “rescue” procedure if complications follow HSCT transplants • Nursing considerations
Administration of Blood and Blood Products ü Identify the child and verify blood with another nurse ü Take v/s including blood pressure before administering blood, then q 15 minutes for the first 2 hrs, then q 30 minutes thereafter until infusion is complete
Administration of Blood and Blood Products Slide 14 ü Administer blood with normal saline on a piggyback setup, through an appropriate filter ü Use blood within 30 minutes of its arrival form the blood bank ü Check blood products-products that appear purplish or are bubbling should not be used because of risk of bacterial contamination ü The rate of infusion of packed RBC’s is approximately 5 ml/kg/hr over not ore than 4 hours

Administration of Blood and Blood Products Slide 15 ü Run transfusion slowly x first 15 minutes; monitor closely for transfusion reaction during this time period ü During administration of blood or blood products, the child and parents should be instructed to notify the nurse immediately if the child feels “bad”, or has fever or chills, headache, nausea, pain at he needle site, or difficulty breathing
Administration of Blood and Blood Products Slide 16 ü In neonates and small infants, auscultate the lungs before and frequently during a transfusion to detect signs of respiratory distress form fluid overload ü If reaction is suspected, stop the transfusion immediately and infuse normal saline through new tubing, notify MD and continue to monitor v/s and hourly urine output ü Send samples of child’s blood to lab
Blood Component Therapy • Administration Procedure • Large bore needle • 19 gauge or higher • Blood Tubing • “Y type” • Microaggregate filter • Isotonic Solution • Normal Saline • Strict Identification process
Blood Component Therapy • Red Blood Cell Transfusions • One unit contains ~ • 200 ml red blood cells • 100 ml storage solution • 30 ml plasma • Must be ABO/Rh compatible • In dire emergencies O- can be used • Do not provide viable platelets nor do they contain significant amounts of coagulation factors

Blood Component Therapy • Red Blood Cell Transfusions • Indications • Pts with symptomatic anemia who are not treatable with specific therapy such as iron, vitamin B 12, folic acid or Erythropoietin • Therapeutic Effect • In 70 kg adult, each unit should increase hematocrit by 3 -4%
Blood Component Therapy Platelets • Platelet concentrate contains ~: • Platelets concentrated by centrifuging whole units of blood • 60 ml plasma • Small numbers of RBCs and WBCs • Pooled platelets • Up to 8 units of platelets from separate donors can be pooled into single bag for transfusion • Expire 4 hours after pooling
Blood Component Therapy Platelets • Platelet Phoresis • Collected from a single donor. Equivalent to ~4 pooled units • Contains 200 -400 ml of plasma • Expire 4 hours after processing for release • Indications • Prevent bleeding d/t thrombocytopenia • Bleeding • Abnormal platelet function

Blood Component Therapy Fresh Frozen Plasma (FFP) • One unit of FFP is plasma taken from one unit of whole blood • FFP contains all coagulation factors • One unit ~ 250 ml • Must be ABO compatible, Rh factor is not considered • Thawed plasma may be transfuse for 5 days after thawing • Indications • Documented coagulation factor deficiencies (r/t liver disease, Warfarin, DIC) • Active bleeding

Blood Component Therapy • Cryoprecipitate (Cryo) • Prepared from plasma and contains fibrinogen • 1 bag contains • ~350 mg Fibrinogen • Pooled = 6 bags or 2100 mg Fibrinogen • Indications • Bleeding • Immediately prior to invasive procedures
Blood Component Therapy Blood Transfusion Reactions • Acute Transfusion Reactions • Acute hemolytic reactions • d/t antibodies in ABO antigen system • May cause acute renal failure, DIC • Treatment: fluids, diuresis, support for bleeding • Most errors are clerical or d/t patient misidentification • Febrile reactions • D/t sensitization on cell components (usually leukocytes) • Treatment: leukocyte depleted RBCs
Blood Component Therapy (cont. ) • Allergic reactions • Most common • D/t proteins on donor’s plasma • Treatment: pre-transfusion treatment with antihistamines or steroids • Circulatory overload • Sepsis • Delayed Transfusion Reactions • Autotransfusion
- Slides: 25