Blood Transfusion tutorial MBBS Curriculum IOD II Dr

Blood Transfusion tutorial MBBS Curriculum IOD II Dr Dupe Elebute Consultant Department of Haematology

Case Presentation 1 l l A patient with Aplastic Anaemia arrived for her twice weekly infusion of platelets On receiving the platelets from the blood bank and checking the unit the product appeared to be “greenish” in colour The unit was checked and was correct for this particular patient 15 minutes into the transfusion she collapsed and the transfusion was stopped What is the diagnosis? What actions would you take?

Case 1: Actions taken l l l Platelet transfusion stopped immediately ABC Given hydrocortisone 100 mg IV and piriton 10 mg IV Started on IV broad-spectrum antibiotics Platelets returned to the lab and cultured Culture of platelets: Bacillus Cereus

Case 1: Actions taken l l Returned unit to NBS; unit re-cultured and also grew Bacillus Cereus NBS recalled the 3 donors of the platelet pool and swabbed the donors’ arms One of the swabs also grew Bacillus Cereus NBS reviewed technique for swabbing of arms of donors and implemented new national guidelines
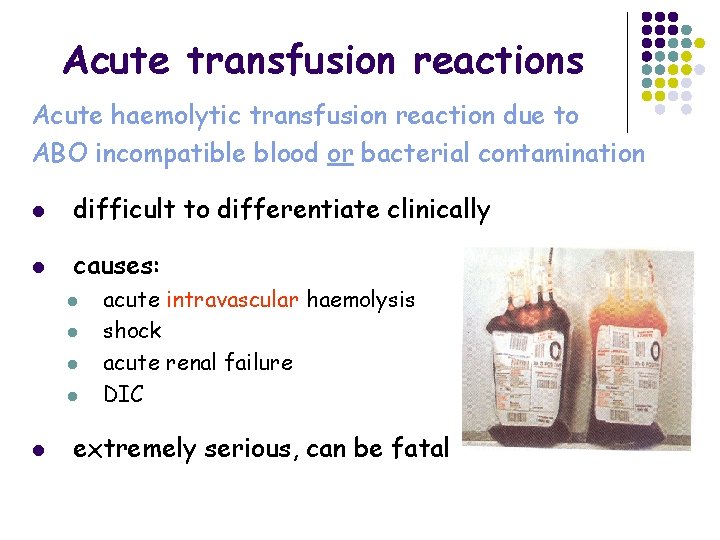
Acute transfusion reactions Acute haemolytic transfusion reaction due to ABO incompatible blood or bacterial contamination l difficult to differentiate clinically l causes: l l l acute intravascular haemolysis shock acute renal failure DIC extremely serious, can be fatal

Management of AHTR A medical emergency: l Stop transfusion immediately Keep line open with N/Saline using new giving set Monitor pulse, BP, temp Call member of medical staff l Check identity of patient against blood bag l l Take urgent blood samples: FBC, cross-match, U & Es, clotting screen, blood cultures Save any urine l Send blood unit back to the blood bank l

Febrile non-haemolytic transfusion reactions l l ‘Allergic’ reaction caused by white cells in blood bag Symptoms: l l l Fever Urticaria Anaphylaxis (rarely) Management: Hydrocortisone and Piriton Very rare in UK now following universal leucodepletion of red cells (v. CJD initiative)

Case Presentation 2 l. A 45 year old was admitted for hysterectomy l. Normal blood count preoperatively l. Received l. Pale three units of blood perioperatively and jaundiced on the 10 day postoperatively • What is the diagnosis? • What haematological tests would you request?

Delayed haemolytic transfusion reactions Due to secondary immune response following reexposure to a red cell antigen l Patient previously sensitised to a red cell antigen by transfusion or pregnancy l Antibody not detected on routine screening for X-match l Patient given transfusion with blood containing same antigen l Provokes an anamnestic (secondary immune) response l Within days, antibody level rises and transfused red cells removed from circulation

Delayed transfusion reactions: 2 l Occurs 24 hr after transfusion (7 -10 days) l Causes extravascular haemolysis l Red cells destroyed in liver, spleen; occurs slowly l Few clinical signs: fever, anaemia, jaundice l Investigations: l l l Coomb’s test positive Re-testing of patient’s serum will now detect antibody In future, patient must be transfused with antigen negative blood

Case Presentation 3 A woman is bleeding profusely post partum l On examination, she is agitated, sweating and cold to the touch l • What would you do first ? • What baseline haematological tests are indicated ? • How should she be managed ?

Massive blood loss Ø Medical emergency l Loss of one blood volume within 24 hour 50% blood volume loss within 3 hours Rate of blood loss 150 ml/min Ø Any blood loss >2 L (SGH) l l Usually occurs in A&E, operating theatre or obstetric department High morbidity & mortality

Massive Blood Loss (2) l l l Ensure adequate venous access Attempt to maintain blood volume with saline, plasma expanders ‘Flying squad’ blood (O Rh Neg, CMV neg) available if blood required in 15 minutes
Complications of Massive Transfusion l l l Hypothermia acidosis Hyperkalaemia: K+ leaks out of red cells during storage Citrate toxicity: red blood cells kept in citrate plus additive solution (SAG-M) l Hypocalcaemia: Ca 2+ ions bound by citrate l Depletion of platelets and coagulation factors l Fluid overload acute respiratory distress syndrome (ARDS)

Case 3 l l l A health care assistant collected a unit of blood from the blood bank fridge without taking any means of identification The checking of the unit was undertaken only with the compatibility slip and the blood unit at the nurses station The patient was blood group B Within 15 minutes of the transfusion the patient had received 50 mls of Group A blood Within 30 minutes the patient became unwell What errors have occurred in the transfusion process?

Case 3: errors that occurred l l l HCA took no means of formal identification to collect the unit of blood No other means of identification was taken for checking the unit of blood No bedside check took place (must be done by 2 trained staff) l No checking of the wrist band

Errors in transfusion Wrong blood to wrong patient 1: 3 ABO incompatible 1: 10 fatal B blood O: † Fatal errors in approx 1: 600 000 (UK, USA) Non-fatal 1: 12000


Further reading • Essential Haematology • ABC of Transfusion (BMJ books) • HMSO Handbook of Transfusion Medicine • SGH handbook of blood transfusion policies and procedures
- Slides: 19