Blood Transfusion Fluid therapy Parenteral nutrition Red blood

Blood Transfusion. Fluid therapy. Parenteral nutrition
Red blood cells Most RBC products are derived by collection of 450 -500 (± 10%) m. L of whole blood from volunteer donors and removal of the plasma by centrifugation. After removal of the plasma, the resulting product is red blood cells. Volume off 1 unit = 280 ± 50 ml One unit of RBC will raise the hemoglobin of an average-size adult by ~1 g/d. L (or raise HCT ~3%)

Washed RBS • RBC are washed with 0. 9% sterile isotonic saline to remove the majority of plasma proteins, antibodies and electrolytes. The washed red cells are then resuspended in additive solution.

Clinical Indications for the Use of Wached RBS Waching of RBC: - Decreases risk of anaphylaxis in Ig. A-deficient patient with anti-Ig. A antibodies - Decreases reactions in patients with history of recurrent, severe allergic or anaphylactoid reactions to blood product transfusion

Leukocyte depleted RBC • • Most commonly achieved by filtration Usually soon after collection (prestorage) May be performed at bedside <5 x 106 leukocytes per product

Leukocyte Reduction Decrease risk of recurrent febrile, nonhemolytic transfusion reactions Decrease risk of HLA-alloimmunization

Cryopreserved RBC • Cryopreservation of RBC's is done to store special, rare RBC's for up to 10 years. The units are placed in special sterile containers in a deep freezer at less than -60 degrees C. • Cryopreserved units are thawed and washed prior to use as saline suspended RBC's. These units must be used in 2 - 4 hours to prevent possible bacterial contamination.

Cryopreserved RBC • Cryopreserved blood can help to maintain stores of Rh negative blood, to provide units for persons with antibodies to high-incidence antigens or persons difficult to cross-match because of multiple alloantibodies and to provide plasma-free blood to persons with Ig. A deficiency.

Red Blood Cell Transfusion Red blood cells should usually be administered when the hemoglobin concentration is low (e. g. , less than 6 g/dl in a young, healthy patient), especially when the anemia is acute. Red blood cells are usually unnecessary when the hemoglobin concentration is more than 10 g/dl.

The determination of whether intermediate hemoglobin concentrations (i. e. , 6– 10 g/dl) justify or require red blood cell transfusion should be based on any ongoing indication of organ ischemia, potential or actual ongoing bleeding (rate and magnitude), the patient’s intravascular volume status, and the patient’s risk factors for complications of inadequate oxygenation.

Transfusion of fresh frozen plasma Coagulation tests (i. e. , PT or INR and a. PTT) should be obtained before the administration of FFP in a bleeding patient. Transfusion of FFP is not indicated if PT, INR, and a. PTT are normal.

Clinical Indications for the Use of FFP 1. Correction of excessive microvascular bleeding (i. e. , coagulopathy) in the presence of a PT greater than 1. 5 times or an a. PTT greater than 2 times normal; 2. correction of excessive microvascular bleeding secondary to coagulation factor deficiency in patients transfused with more than one blood volume (approximately 70 ml/kg) and when PT or INR and a. PTT cannot be obtained in a timely fashion; 3. urgent reversal of warfarin therapy

Clinical Indications for the Use of FFP 4. correction of known coagulation factor deficiencies for which specific concentrates are unavailable; 5. heparin resistance (antithrombin III deficiency) in a patient requiring heparin Fresh frozen plasma should be given in doses calculated to achieve a minimum of 30% of plasma factor concentration (usually achieved with administration of 10– 15 ml/kg FFP), except for urgent reversal of warfarin anticoagulation, for which 5– 8 ml/kg FFP usually will suffice

Transfusion of platelets Volume 50 ml Dosage: 1 U/ 10 kg Prophylactic administration (pt without microvascular bleeding): platelet count < 10. 000/mmc. Pts with bleeding: In surgical or obstetric patients with normal platelet function, platelet transfusion is rarely indicated if the platelet count is known to be greater than 100 x 109/l and is usually indicated when the count is below 50 x 109/l in the presence of excessive bleeding.

Transfusion of platelets Vaginal deliveries or operative procedures ordinarily associated with limited blood loss may be performed in patients with platelet counts less than 50 _ 109/l. Platelet transfusion may be indicated despite an apparently adequate platelet count if there is known or suspected platelet dysfunction.

Albumin • Human albumin is a normal constituent of plasma and acts like physiological albumin • is predominantly derived from human plasma, • human serum albumin are commercially available in a 5% solution, 20 % and a 25% solution.

Clinical Indications for the Use of Albumin • to correct hypoproteinemia (serum protein < 50 g/l) • Hypovolemic states • burns • treatment of oedema not responsive to diuretics (ascites, nephrotic syndrome).

Transfusion of cryoprecipitate • • • VIII factor von Willebrand factor XIII factor fibrinogen fibronectin • Volume 15 ml

Transfusion of cryoprecipitate If possible, a fibrinogen concentration should be obtained before the administration of cryoprecipitate in a bleeding patient. Transfusion of cryoprecipitate is rarely indicated if fibrinogen concentration is greater than 1, 5 g/l. Transfusion of cryoprecipitate is usually indicated 1. when the fibrinogen concentration is less than 0, 8– 1, 0 g/d in the presence of excessive microvascular bleeding 2. to correct excessive microvascular bleeding in massively transfused patients when fibrinogen concentrations cannot be measured in a timely fashion 3. for patients with congenital fibrinogen deficiencies.

Transfusion of cryoprecipitate The determination of whether patients with fibrinogen concentration between 1, 0 and 1, 5 g/l require therapy should be based on the potential for anticipated or ongoing bleeding and the risk of bleeding into a confined space (e. g. , brain or eye).

FLUID THERAPY

Colloids are substances that do not dissolve into a true solution and do not pass through a semipermeable membrane.
![Dextrans • The formulations currently available are: • Dextran 40 (Mw 40, 000 [‘Rheomacrodex’], Dextrans • The formulations currently available are: • Dextran 40 (Mw 40, 000 [‘Rheomacrodex’],](http://slidetodoc.com/presentation_image_h2/6415973db6f7c9a9cbfc2ba70ce176fa/image-23.jpg)
Dextrans • The formulations currently available are: • Dextran 40 (Mw 40, 000 [‘Rheomacrodex’], sol. 10% • Dextran 70 (Mw 70, 000 ) [‘Macrodex’], sol. 6% The dextrans cause more severe anaphylactic reactions than the gelatins or the starches. Dextran 70 has a duration of action of 6 to 8 hours. Interference with crossmatching can occurs. Dextran interferes with haemostasis. There is a maximal dosage recommendation of 1, 5 g/kg/day).

Gelatin solutions • Gelatin is the name given to the proteins formed when the connective tissues of animals are boiled. Gelofusine, Gelatinol • The MW ranges from 5, 000 to 50, 000 with a weight-average MW of 35, 000. • Anaphylactoid reactions can occur • No interference with blood cross-matching its use contributes to dilutional coagulopathy

Starches(HAES, Refortan, Voluven, Refortan- plus) • These polydisperse colloid solutions are produced from amylopectin which has been stabilised by hydroxyethylation to prevent rapid hydrolysis by amylase. • Hydroxyethylstarch is removed from the circulation by renal excretion. • Anaphylactoid reactions occur in about 0. 09% of cases. • concern is the possibility that starch preparations can affect the coagulation process. • Molecular weight – 100. 000 -200. 000 - 6% (Refortan), 10% (Refortan plus), Voluven (130. 000, sol. 6%).

Crystalloids pass freely through a semipermeable membrane.

Crystalloids • The most commonly used crystalloid fluid is normal saline, a solution of sodium chloride at 0. 9% concentration • 154 mmol Na and 154 mmol Cl/l • infusion of 1 L of 0. 9% sodium chloride (isotonic saline) adds 275 m. L to the plasma volume and 825 m. L to the interstitial volume.
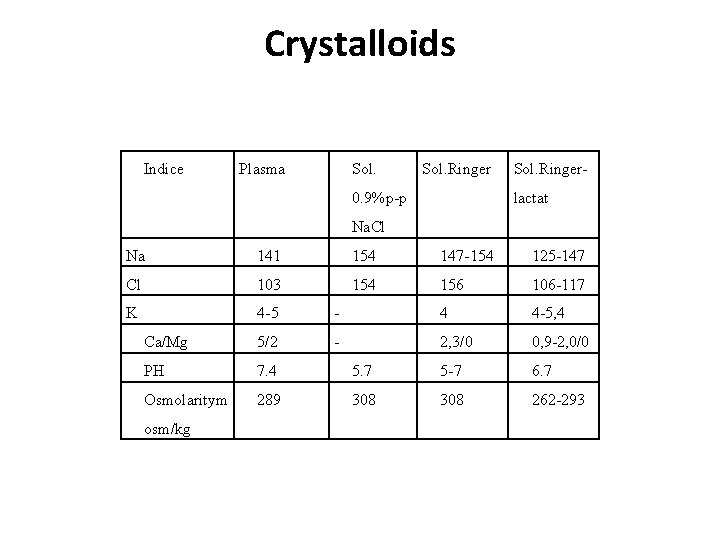
Crystalloids Indice Plasma Sol. Ringer 0. 9% р-р Sol. Ringerlactat Na. Cl Na 141 154 147 -154 125 -147 Cl 103 154 156 106 -117 K 4 -5 - 4 4 -5, 4 Ca/Mg 5/2 - 2, 3/0 0, 9 -2, 0/0 РН 7. 4 5. 7 5 -7 6. 7 Osmolaritym 289 308 262 -293 osm/kg

Parenteral nutrition is usually indicated in the following situations • • Documented inability to absorb adequate nutrients via the GI tract such as: • – Massive small-bowel resection/short bowel syndrome (at least initially) • – Radiation enteritis • – Severe diarrhea • – Untreatable steatorrhea/malabsorption (i. e. , not pancreatic insufficiency, small bowel bacterial overgrowth, or celiac disease) • • Complete bowel obstruction, or intestinal pseudoobstruction

• Severe catabolism with or without malnutrition when GI tract is not usable within 5– 7 days • Inability to obtain enteral access • Inability to provide sufficient nutrients/fluids enterally • Pancreatitis accompanied by abdominal pain • Persistent GI hemorrhage • Acute abdomen/ileus • High output enterocutaneous fistula (>500 m. L) and inability to gain enteral access distal to the fistula site • Trauma requiring repeat surgical procedures

Parenteral nutrition may be indicated in the following situations • Inflammatory bowel disease not responding to medical therapy • Partial small bowel obstruction • Intensive chemotherapy • Major surgery/stress when enteral nutrition not expected to resume within 7– 10 days • Intractable vomiting when jejunal feeding is not possible

Amino acid solutions • • • Protein is provided as a crystalline amino acid solution. 500 ml bottles are standard. Solutions vary in amino acid concentration and amino acid composition. (Aminosteril, Intrafuzin, Infezol, Aminoplasmal). Min 0, 54 g/kg/day, optimal 0, 8 g/kg/day - de 1, 2 -1, 6 g/kgc/day. Should provide 15 -30% of total caloric intake.

Dextrose solutions • Dextrose in solution has 3. 4 kcalories per gram. • Dextrose solutions come in different concentrations • 3 -4 g/kg/day – provides 50 -60% of total caloric intake.

Lipids • Lipids in parenteral nutrition are used as a source of essential fatty acids and energy. Lipid emulsions are composed of soybean and/or safflower oil, glycerol, and egg phospholipid. • IV lipids come in bottles of 10% or 20% emulsions. The 10% emulsion contains 1. 1 kcal/ml the 20% emulsion contains 2 kcal/ml. • (Lipofundin, Intralipid, Lipovenoz) (25 -30% of total caloric intake).

FLUIDS 30 -40 ml/kg/day

• • ELECTROLYTES & MICRONUTRIENTS Minerals and Electrolytes Na 60 -100 mmol K 60 -100 mmol Ca 5 - 8 mmol P 20 -45 mmol

Vitamins • Commercial vitamin preparations for TPN are available. The vitamin requirements for TPN patients are different from non-TPN patients because absorption is not a factor with TPN. When needs are increased for certain disease states, single vitamin supplements can be added to the solution. Serum vitamin levels can be monitored and dosage adjusted accordingly. • SOLUVIT, VITALIPID

Trace Elements • • • Chromium 10 -15 mcg Copper 0, 3 -0, 5 mg Manganese 60 -100 mcg Zinc 2, 5 -5 mg Selenium 20 -60 mcg ADAMEL
- Slides: 38