Blood Transfusion Dr Dupe Elebute MD MRCPath Consultant

Blood Transfusion Dr Dupe Elebute MD, MRCPath Consultant in Haematology and Transfusion Medicine

Objectives Blood components n Ordering blood & MSBOS n Risks of blood therapy n Adverse reactions n Massive blood transfusion n

Blood - Where From? n Human source - no synthetics yet - not risk free n Scarce resource n 1 donor can give 1 unit every 4 months n Need 10, 000 units of blood/day in U. K. Ø Use carefully!

When To Use Blood? n Balance between benefits vs risks n Doctor’s decision n n Ø Definite indication must be recorded in the patient’s medical records Correct anaemia pre-operatively Try to reduce unnecessary exposure to blood products

Blood components n Unpaid, volunteer donor n n Pooled products Single donations by apheresis

Blood donors n n n Ø Medical selection process to protect both recipients and donors Minimum age: 17 years Maximum age: 70 years (60 for first time donations) Donor deferral system

Blood donations Tested in the UK for: n Hepatitis B, C n HIV-I, II n Syphilis n ABO and Rh. D blood group n ? v. CJD universal leucodepletion
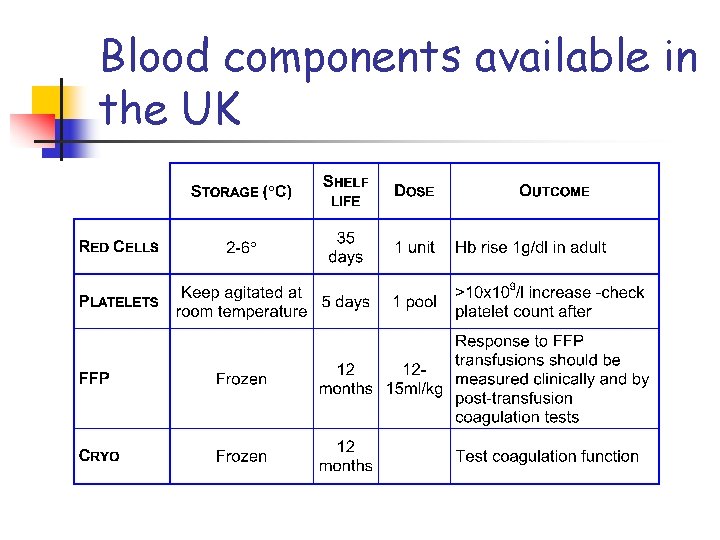
Blood components available in the UK
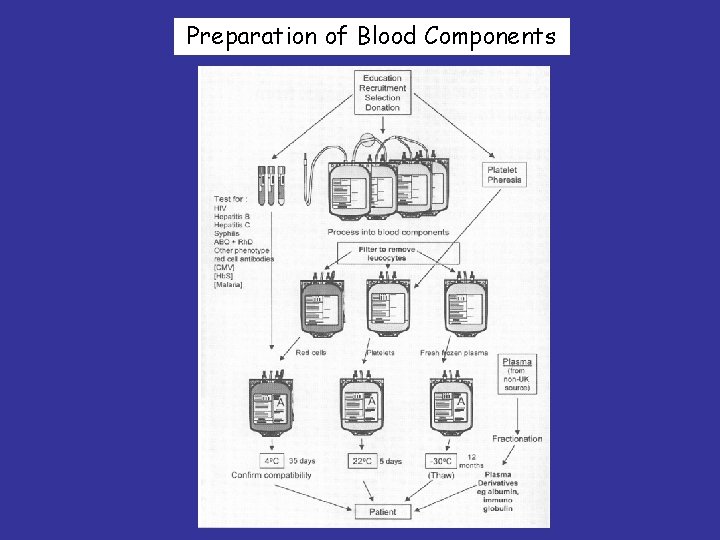
Preparation of Blood Components

Blood components issued in the UK (2001 -2002) n n Red cells Platelets Fresh frozen plasma Cryoprecipitate 2, 683, 463 251, 451 385, 236 88, 253 TOTAL 3, 408, 402
Red cells n Whole blood n n n <1% used as ‘whole blood’ in UK Deficient in labile clotting factors Packed red cells 0. 75) n n n (450 ml; PCV 0. 35 -0. 45) (350 ml; PCV 0. 55 - Stored at 2 -6 ºC for up to 35 days 1 unit -> Hb rise by 1 g/dl in adult New Hb trigger of 8 g/dl

White cells (granulocytes) n n n Very rarely used in the UK Only for severe infections in neutropenic patients unresponsive to antibiotics/antifungal Rx Transfused as ‘buffy coats’ or collected by apheresis

Platelet concentrates n n n Adult single dose (1 pool): 300 x 109/L Stored at room temperature for up to 5 days (kept agitated) Obtained in two ways: n n Pooled platelets from 4 -5 single donations Single donor platelets collected by cell separator machine (apheresis)

Platelet concentrates (2) Indications for platelet transfusions: n Bone marrow failure (aplastic anaemia) n Post chemotherapy, BMT n Massive blood transfusion (dilutional) n Platelet dysfunction (CABG, aspirin)

Fresh frozen plasma (FFP) n n n Stored frozen at – 30ºC for up to 1 yr Not routinely virally inactivated in UK To be sourced from USA (volunteer, nontransfused male donors) Provides replacement for most coagulation factors Methylene blue FFP for neonates and children born after 1 st January 1996

Fresh Frozen Plasma (2) n Essential to give adequate volume Dose: 12 -15 ml/kg ABO compatible Ø Definite indications only: n n § Massive blood transfusion n DIC n Coagulation defect with no available factor concentrate

Cryoprecipitate n n Separated by freezing FFP, allowing it to thaw to 4 -8ºC Re-frozen & stored at – 30ºC for up to 1 yr Enriched with FVIII, v. WF and fibrinogen Indications: n n DIC Fibrinogen deficiency

Plasma products Blood products derived by fractionation of plasma: n n Albumin Factor VIII concentrate Factor IX concentrate Human Ig

Ordering blood n Can only be done by a registered medical doctor Weigh up advantages vs risks! Consider alternatives n Take blood sample for ‘group & screen’ n n ABO and Rh. D group Screen for antibodies
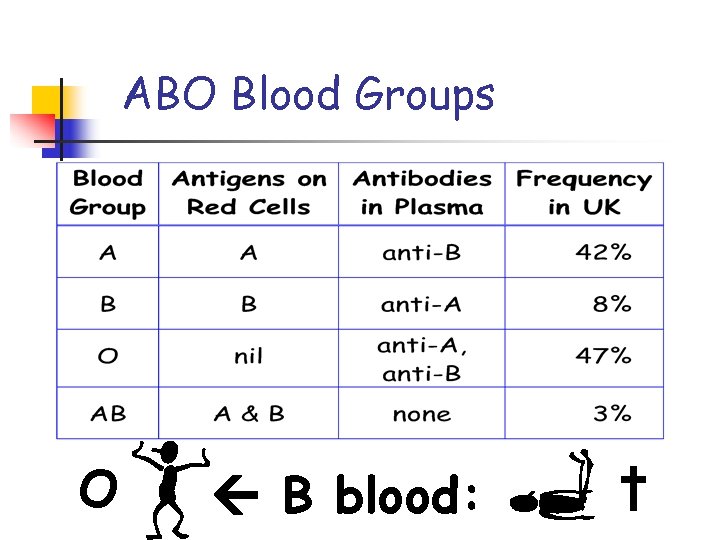

ABO Blood Groups O B blood: †
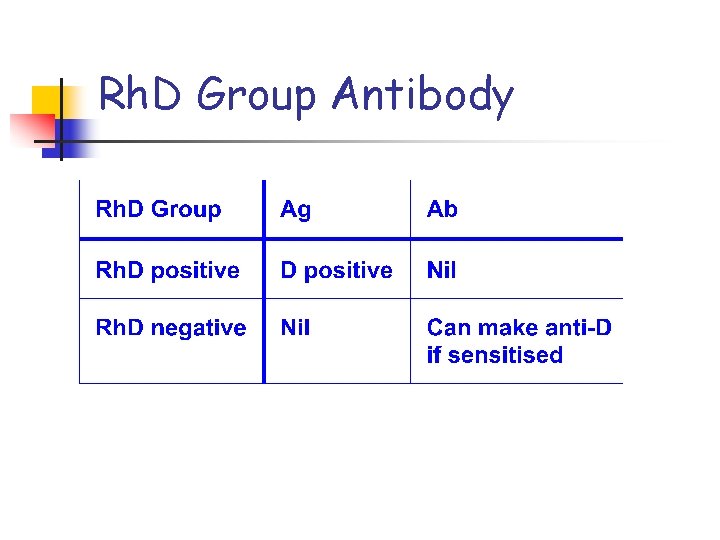

Rh. D Group Antibody


Blood sampling n Label request form with: n n n Patient’s surname Patients first name(s) Date of birth (not age) Hospital number (or A&E number) Label sample bottle at bedside Addressograph labels must not be used

Patient identification n n Positively identify conscious patient by asking him/her to state their name and date of birth Check information against patient’s identification wrist band

Record in hospital notes n Reason for blood transfusion n n Blood loss Nature of surgery Pre-transfusion Hb Number of units to be transfused Planned date (and time) of transfusion

Maximum Blood Order Schedule n n Pre-operative schedule of units to be crossmatched for each surgical procedure Clear guidelines in Transfusion handbook Blood sample still required 24 hours pre-op to check for antibodies Does not apply to emergencies; acute bleeding; patient known to have red cell antibodies

Risks of blood transfusion n n Infections: - hepatitis B, C - HIV I & II - bacteria - protozoa (malaria) - v. CJD (? ) Transfusion reactions Immunological reactions Getting the wrong blood!
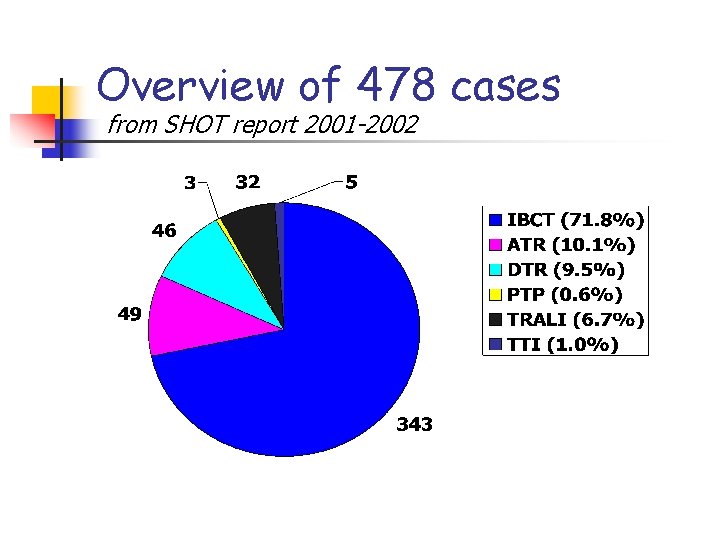
Overview of 478 cases from SHOT report 2001 -2002
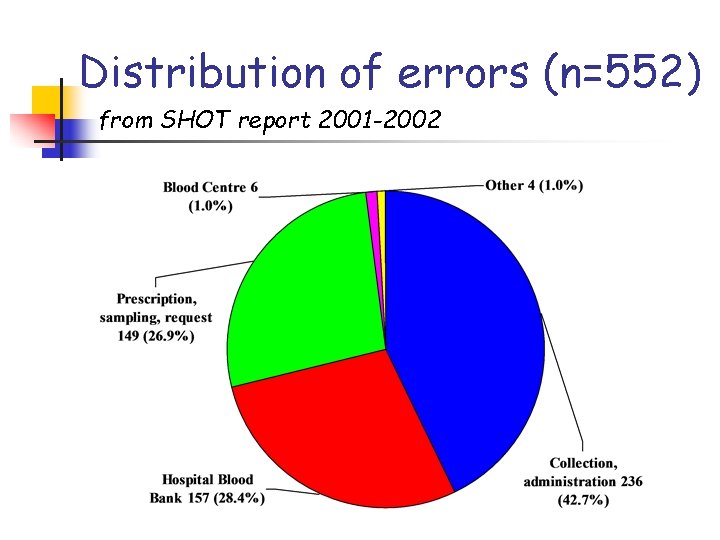
Distribution of errors (n=552) from SHOT report 2001 -2002

Transfusing blood Inform patient! n n Indication Benefits Risks Alternatives
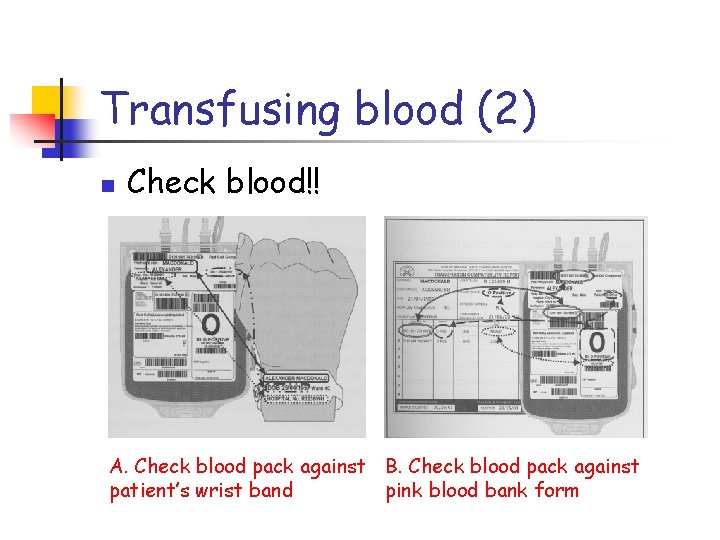
Transfusing blood (2) n Check blood!! A. Check blood pack against B. Check blood pack against patient’s wrist band pink blood bank form

The final check! n n Must be done at the bedside Must be done by TWO people Must NOT be done by untrained staff If any discrepancy is found: n n Do NOT transfuse blood Inform blood bank immediately

Adverse effects of transfusion n Immunological reactions: n n n Immediate (ABO incompatibility, TRALI) Delayed (DHTR, PTP, Gv. HD) Non-immunological: n n Immediate (Bacterial, fluid overload) Delayed (e. g. viral infections, malaria)

Transfusion Reactions n Acute haemolytic: n n Febrile non-haemolytic: n n n Incompatible blood; can be fatal Due to cytokines from transfused WBCs Acute bacterial infection Allergic/urticarial

Transfusion Reactions (2) n n Fever >38ºC Rash Rigors Acute haemolytic specific: n n Hypotension, loin pain, dark urine Febrile non-haemolytic specific: n Urticaria, pruritis

Transfusion Reactions (3) n n STOP the transfusion (spigot off) Using a new giving set, keep line open with normal saline Check I. D of patient, bag and cross-match form Refer to handbook for further management

Massive blood loss Ø Ø n n Any blood loss >2 L (SGH) Medical emergency Usually occurs in A&E, operating theatre or obstetric department High morbidity & mortality from: n n n Underlying cause of haemorrhage Pre-existing disease (liver, renal) Complications of massive blood transfusion

Massive Blood Loss (2) n n n Ensure adequate venous access Attempt to maintain blood volume with saline/plasma expanders Inform blood bank Send 2 group & X-match samples If ‘flying squad’ blood used, inform BB

Massive Blood Loss (3) n n n Call Blood Bank for : “Code Red” “Code Blue” - Obstetric patients Necessary blood products issued automatically Haematology Sp. R will co-ordinate

Code Red Procedure Blood components issued: n First Stage n 6 units blood n 1 litre FFP n 2 pools platelets

Code Red Procedure (2) Second Stage n 6 units blood n 10 units cryo if fibrinogen <0. 8 g/l n 2 pools platelets if count <100 x 109/L n Send blood for repeat FBC, chemistry, coagulation screen

Complications of Massive Tx n n n Ø Ø Hypothermia Hypokalaemia Hypocalcaemia Acidosis ARDS Monitor U & Es Calcium, arterial p. H ECG, CXR
- Slides: 43