Blood Transfusion and Catheter Size Lynda S Cook

Blood Transfusion and Catheter Size Lynda S. Cook MSN, RN, CRNI Vascular Access Specialist Greensboro, NC May 6, 2017

Abstract: The administration of blood is associated with a certain amount of dogma that professionals carry with them from nursing school or the first day on the job. Certain philosophies become imbedded in practice without judgement until situations force a review of their logic. Illumination occurs with simple questions such as, “If blood has to go through a 20 - or 18 - gauge needle, how is it given to a newborn? ” In this session, we will examine some of the common practices of blood administration and determine if they are dictated by pathology or are simply learned behavior.

Objectives: Examine how red blood cell pathology and catheter physiology intertwine in infusion dynamics. Evaluate three common transfusion practices and their potential to lead to mechanical hemolysis.

Disclosures Clinical Outcomes Specialist for 3 M Critical and Chronic Care Division No conflicts to disclose

Challenge Question: What size catheter should be used to transfuse blood? Initial response: What do the experts say?

Expert Opinion Weinstein SM, et al. Plummer’s Principles and Practice of I. V. Therapy. 9 th ed. Wolters-Kluwer: Philadelphia, PA. 2014. Phillips L, et al. Manual of I. V. Therapeutics: Evidenced-Based Practice for Infusion Therapy. 6 th ed. F. A. Davis: Philadelphia, PA. 2014 Infusion Therapy Standards of Practice. J Infus Nurs. 2016. 39(1 S) Fung, MK, et al. Technical Manual. 18 th ed. AABB: Bethesda, MD. 2014.

Consensus? Generally: - Adults 20 -18 g - Rapid infusion 16 -14 g - Pediatrics 22 -24 g But. . . Use the smallest catheter necessary

So Why Am I Confused? Maryland – 20 -18 g adults, 24 g neonates only Georgia – 20 -18 g adults; 22 g pediatrics Tennessee – 22 -18 g adults; 24 neonates Texas Galvaston – 24 -14 g Austin – 20 g preferred; 22 g with pump

Saskatoon, Saskatchewan – 18 g adults; 25 g min for peds National Blood Users Group, Dublin, Ireland – depends on vein size and desired rate ATI training schools – 20 -18 preferred but smaller can be used Nurses. Lab web-based data base – 18 g

What about central lines? Often not addressed References have stated: Central lines ok Use PICCs with caution UVC preferred for neonates Neonatal PICC not recommended Refer to manufacturer’s guidelines

It’s Making Me Dizzy!

Better question: What concern is related to catheter gauge? Answer: Mechanical hemolysis
Hemolysis: The rupture or destruction of a red blood cell not related to senescence Classifications: - Extrinsic / Intrinsic - Intravascular / Extravascular - Immune / Non-immune o Autoimmune / Alloimmune *Presentation of symptoms depends on the combination of above.

Genetic predisposition Intrinsic: - Genetic malfunction or malformation that may be hereditary or autoimmune - Abnormalities of the red blood cell membrane, enzymatic pathways or the hemoglobin molecule - i. e. , the cell is not normal at the time of formation Extrinsic: - External influences cause the cell to be marked for destruction - i. e. the cell was normal; damage is 2 o to an external force

Location of Hemolysis Extravascular vs. Intravascular What happens to the by-products? stroma, potassium, hemoglobin

Senescence Anticipated destruction Life span 120 days ( if cell not metabolically active) Stroma – ingested by the RES and removed Potassium – available for uptake Hemoglobin Heme - broken down for re-use • Iron – transported to cells • Porphyrins – degrade to form bilirubin Globin - reduced to amino acids which join the protein pool


Extravascular Hemolysis Red cell is marked for destruction by surface markers that appear on the cell; cytokines / antibodies Phagocytosis occurs; macrophage removes cell, usually to spleen Hemolysis takes place entirely within the macrophage Symptoms are few and depend on # cells involved: - increased bilirubin - anemia or low rise in hematocrit after transfusion

Intravascular Hemolysis Red cell contents are spilled directly into the blood stream Unexpected need to remove cellular by-products Systems of elimination are overwhelmed - Oxidative effects of free hgb damages organs - Hyperkalemia with potential cardiac involvement - Excessive stroma activates the clotting cascade and kinin systems Symptoms may be severe and depend on # cells involved: - DIC - Shock - Cardiac arrest - Renal failure

Contributing Factor Immune vs. Non-immune Autogenic vs. Allogenic

Immune Hemolysis Antibody-mediated against an antigen on the red cell surface (i. e. surface marker) Antibody fixes complement - Acute intravascular hemolysis - Delayed intravascular hemolysis - Extravascular hemolysis Result of complement activation Release of histamine and serotonin hypotension Severe inflammatory response May occur with few cells

Antibodies are gamma globulins. Not all antibodies fix complement. Ig. M Ig. G 3 Activation is complete; Intravascular destruction of red cell Ig. G 1 Ig. G 2 Poor or incomplete activation; Opsonization of the cell; Extravascular destruction of cell Ig. G 4 Ig. A Ig. D Ig. E Do not fix complement; Not associated with cell lysis
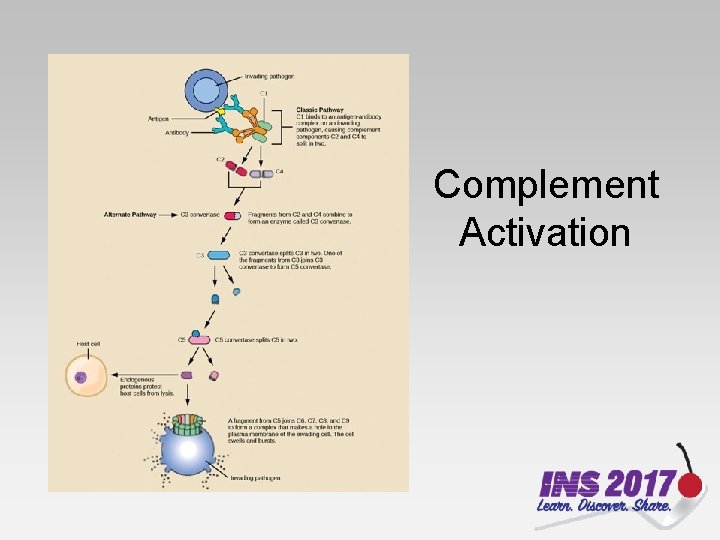
Complement Activation
Non-Immune Hemolysis Cellular destruction is not triggered by markers on the red cell surface; the influence is external The complement system is not activated Severity depends on - Number of cells lysed - Location of hemolysis intravascular or extravascular

Hemolysis Characteristics from 6 Origins Genetic Extrinsic ABO incompatibility x Rh incompatibility x Intrinsic Location Intravascular Extravascular x Immune Nonimmune x x x Sickle cell x x x Thalassemia x x x Malaria parasitic rupture x x Bacterial sepsis x x x

Transfusion-Related Mechanical Hemolysis Extrinsic extrinsic The cell was normal prior to the exertion of outside influences

Transfusion-Related Mechanical Hemolysis Intravascular intravascular extrinsic The contents of the cell are freed while in the bag and spilled directly into the blood stream

Transfusion-Related Mechanical Hemolysis Non-Immune extrinsic intravascular non-immune No antibody-antigen reaction No activation of complement

Symptoms are based on this combination of classification Non-immune extrinsic intravascular = S&S

Mechanical Hemolysis Signs & Symptoms Mild (few cells involved): • no symptoms detectable Moderate: • Possible increased bilirubin • Lack of anticipated rise in hematocrit Severe (massive cell involvement) • Hyperkalemia – cardiac arrhythmias • Renal failure • DIC • Shock

What size catheter should be use to give blood?
How big is a red cell? Average RBC count is 4. 5 – 6. 0 million/μL RBCs suspended in plasma Average diameter of a red cell is 8 micrometers 1 m. L = contains > 5, 000, 000 1 tsp = contains > 25, 000, 000 (5 ml)

The risk of catheter-related hemolysis when blood is run to gravity is. . . As long as rate remains consistent

To maximize flow, use the largest diameter and shortest length possible. Type Gauge Length m. L/min Peripheral 20 1. 8” 60 Peripheral 18 1. 8” 105 Peripheral 16 1. 8” 200 1 http: //emupdates. com/2009/11/25/flow -rates-of-various-vascular-catheters/ 2 https: //www. openanesthesia. org/poise uilles_law_iv_fluids/

Resistance as length Gauge Length Minutes/L Peripheral 14 g 2. 5” 1. 3 Peripheral 14 g 5. 2” 2. 1 CVC 14 g 8. 0” 5. 2 High Type Resistance PICCs not recommended for blood transfusion Low Excessive pressure may rupture PICC lines Long Short Length
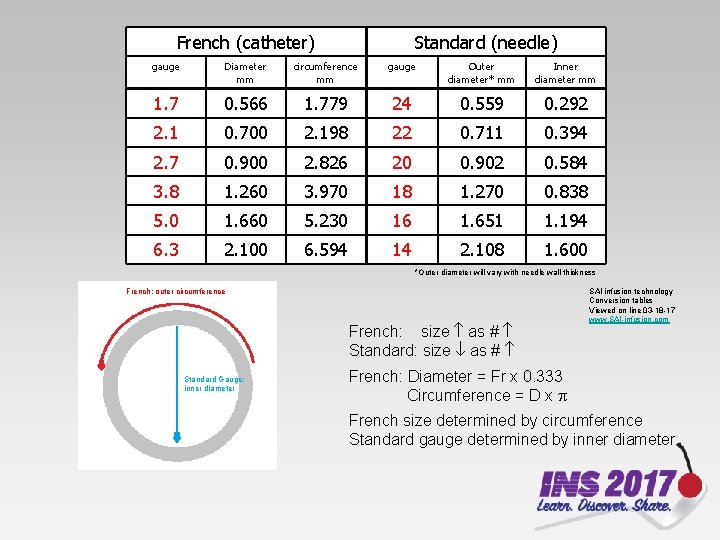
French (catheter) Standard (needle) gauge Diameter mm circumference mm gauge Outer diameter* mm Inner diameter mm 1. 7 0. 566 1. 779 24 0. 559 0. 292 2. 1 0. 700 2. 198 22 0. 711 0. 394 2. 7 0. 900 2. 826 20 0. 902 0. 584 3. 8 1. 260 3. 970 18 1. 270 0. 838 5. 0 1. 660 5. 230 16 1. 651 1. 194 6. 3 2. 100 6. 594 14 2. 108 1. 600 *Outer diameter will vary with needle wall thickness French: outer circumference French: size as # Standard Gauge: inner diameter SAI infusion technology Conversion tables Viewed on line 03 -18 -17 www. SAI-infusion. com French: Diameter = Fr x 0. 333 Circumference = D x French size determined by circumference Standard gauge determined by inner diameter

French/Standard gauge conversion not associated with multi-lumen catheters 18 g 16 g 18 g 7 Fr 16 g 7 Fr Silastic catheters are thicker than polyurethane; same French size ≠ same internal diameter 16 g 20 g 18 g 8. 5 Fr Reddick Emerg Med J. 2011 Mar; 28(3): 201 -2. Epub 2010 Jun 26. PMID: 20581377.

Height makes Might!!!
Velocity depends on catheter gauge, rate of administration, height of fluid . . . and density of the cells (viscosity)

Velocity+ Viscosity = Flow Poiseuille’s law Viscosity of commonly infused intravenous solutions range from 1. 0 centi. Poise to 40. 0 c. P Viscosity of common fluids: 1. 0 c. P Lactated Ringers 10. 0 c. P Whole blood 7, 000 c. P - molasses 50, 000 c. P Ketchup 1, 000 c. P Crisco shortening https: //www. openanesthesia. org/poiseuilles_law_iv_fluids/
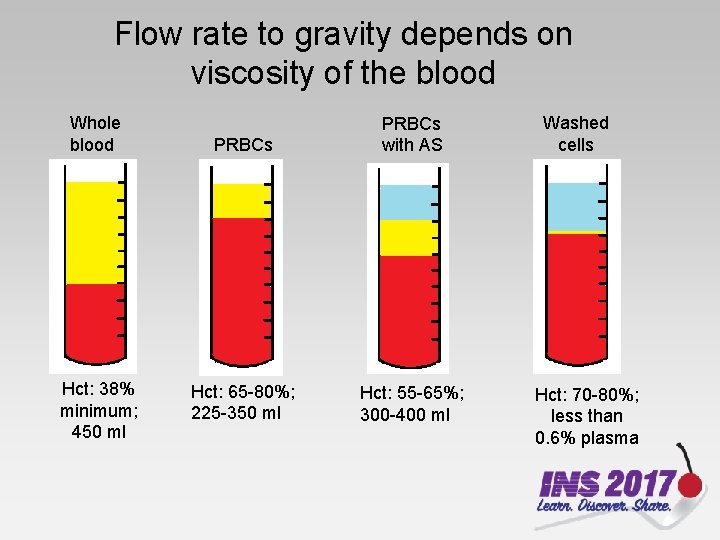
Flow rate to gravity depends on viscosity of the blood Whole blood Hct: 38% minimum; 450 ml PRBCs with AS Hct: 65 -80%; 225 -350 ml Hct: 55 -65%; 300 -400 ml Washed cells Hct: 70 -80%; less than 0. 6% plasma

0. 9% Sodium Chloride. . . still the only solution approved for use

Lactated Ringers Solution Does not cause mechanical hemolysis Contains calcium - Binds with citrate in CPDA preservative - Activates clotting within bag Studies to support use - 1991 Cull et al; concurrent administration - 1998 Lorenzo et al; diluent - No study replicas found. FDA does not approve concurrent use or use as diluent https: //www. openanesthesia. org/poiseuilles_law_iv_fluids/

5% Dextrose in Water Cause osmotic hemolysis Dextrose - Makes the solution isotonic in the bag - Is immediately utilized by the cells for energy Water - The solution becomes profoundly hypotonic after administration - Cells absorb water and rupture https: //www. openanesthesia. org/poiseuilles_law_iv_fluids/
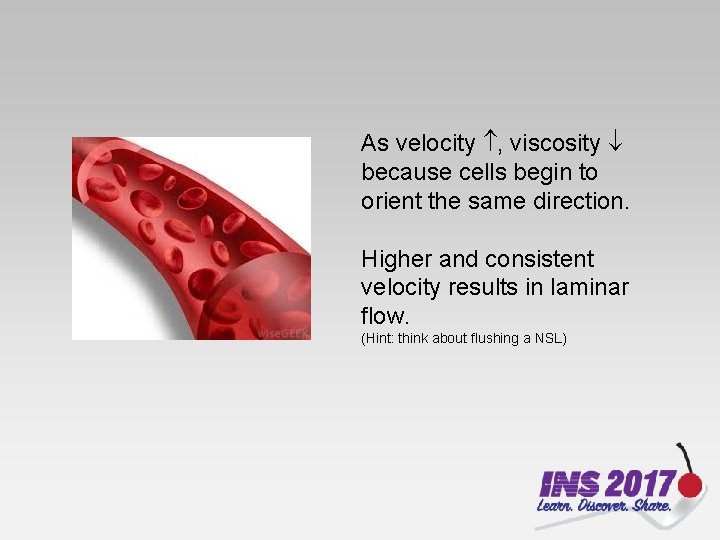
As velocity , viscosity because cells begin to orient the same direction. Higher and consistent velocity results in laminar flow. (Hint: think about flushing a NSL)
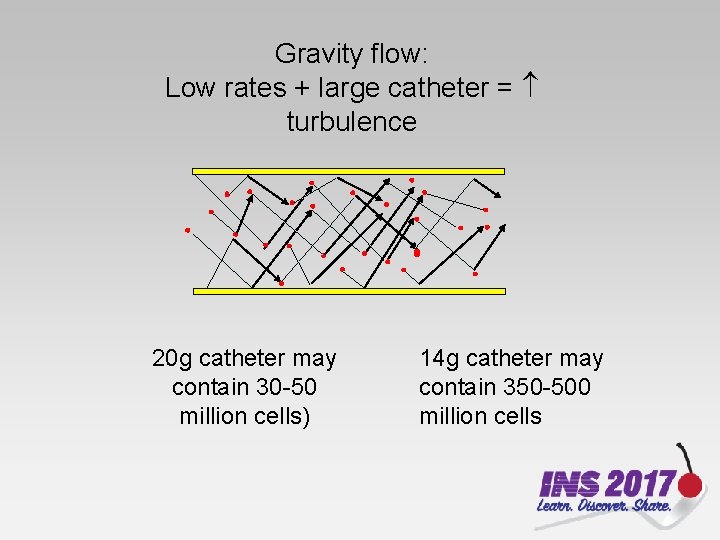
Gravity flow: Low rates + large catheter = turbulence 20 g catheter may contain 30 -50 million cells) 14 g catheter may contain 350 -500 million cells

Velocity + viscosity + temperature = flow Poiseuille’s law Viscosity decreases as temperature increases. https: //www. openanesthesia. org/poiseuilles_law_iv_fluids/ Warm blood recommended for: Rapid, massive transfusion Neonates receiving exchange transfusion Clinical presence of hypothermia May be considered for cold agglutinins Due to reimbursement considerations, use of blood warming devices is not recommended as a general method of increasing rate
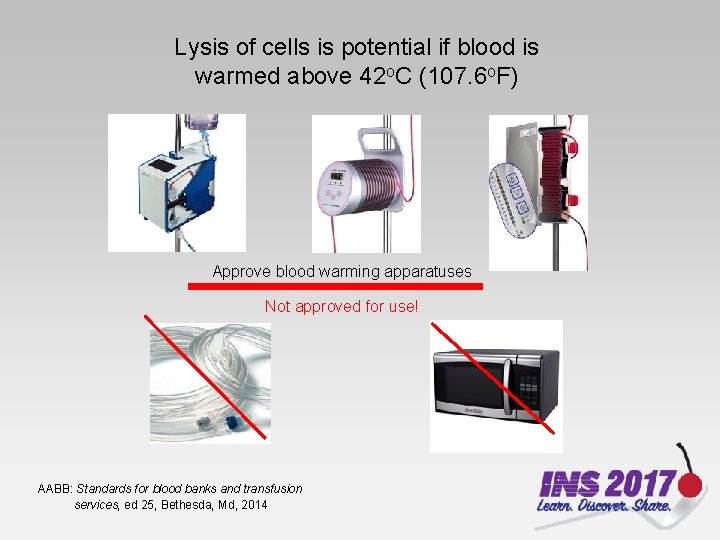
Lysis of cells is potential if blood is warmed above 42 o. C (107. 6 o. F) Approve blood warming apparatuses Not approved for use! AABB: Standards for blood banks and transfusion services, ed 25, Bethesda, Md, 2014

Too cold is bad, too! Blood is stored between 1 -6 o. C (33. 8 -42. 8 o. F) Blood stored at 0 o. C (32 o. F) or below will lyse if not protected Contact with freezer blocks or freezer elements may destroy a unit

Velocity + Viscosity + Temperature + Pressure = Flow Poiseuille’s law Increasing pressure maximizes flow. External pressure must be applied evenly over entire bag - Do not use pressure cuffs - Use FDA approved bags with pressure gauge - Maximum pressure 300 mm. Hg Infusion pumps certified by manufacturer
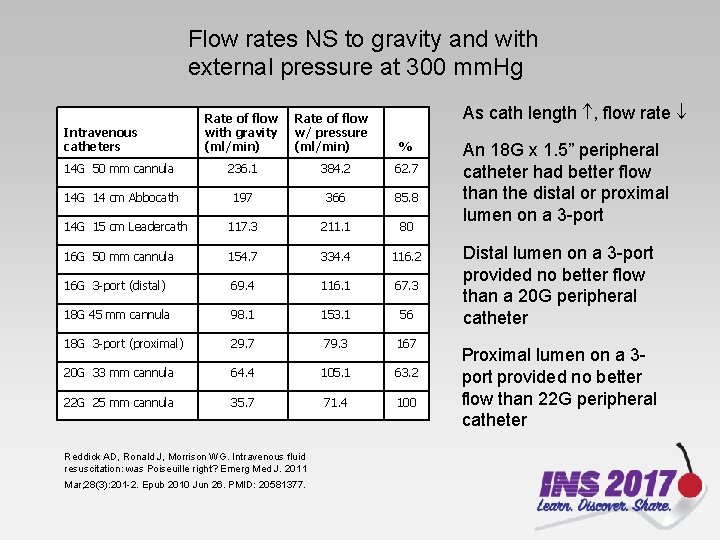

Flow rates NS to gravity and with external pressure at 300 mm. Hg Intravenous catheters Rate of flow with gravity (ml/min) Rate of flow w/ pressure (ml/min) As cath length , flow rate % 14 G 50 mm cannula 236. 1 384. 2 62. 7 14 G 14 cm Abbocath 197 366 85. 8 14 G 15 cm Leadercath 117. 3 211. 1 80 16 G 50 mm cannula 154. 7 334. 4 116. 2 16 G 3 -port (distal) 69. 4 116. 1 67. 3 18 G 45 mm cannula 98. 1 153. 1 56 18 G 3 -port (proximal) 29. 7 79. 3 167 20 G 33 mm cannula 64. 4 105. 1 63. 2 22 G 25 mm cannula 35. 7 71. 4 100 Reddick AD, Ronald J, Morrison WG. Intravenous fluid resuscitation: was Poiseuille right? Emerg Med J. 2011 Mar; 28(3): 201 -2. Epub 2010 Jun 26. PMID: 20581377. An 18 G x 1. 5” peripheral catheter had better flow than the distal or proximal lumen on a 3 -port Distal lumen on a 3 -port provided no better flow than a 20 G peripheral catheter Proximal lumen on a 3 port provided no better flow than 22 G peripheral catheter

Rapid infusion pumps - Used for trauma resuscitation - Warming capability - Pressurized delivery Not associated with hemolysis Kim P, et al. (2004). Can J Surg. Aug; 47(4): 295 -7. Rapid-infusion catheter - 8. 5 Fr x 6. 5 cm

Pressure Tidbits and Caveats 300 mm. Hg maximum is to prevent splitting of bag seams I. V. pumps are certified for safety of the pumping mechanism, not cath gauge Lysis occurs when blood is forced through a too-small catheter or needle.
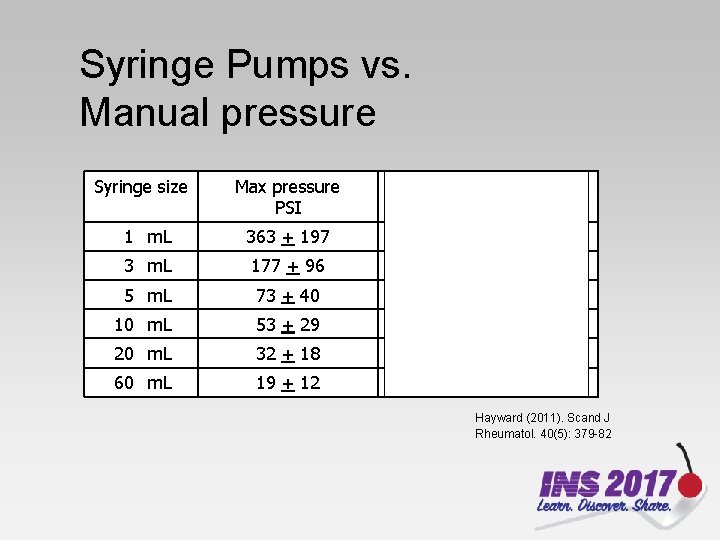
Syringe Pumps vs. Manual pressure Syringe size Max pressure PSI mm. Hg range equivalent 1 m. L 363 + 197 8, 584 – 25, 857 3 m. L 177 + 96 4, 189 – 14, 118 5 m. L 73 + 40 1, 707 – 5, 844 10 m. L 53 + 29 1, 241 – 4, 240 20 m. L 32 + 18 724 – 2, 585 60 m. L 19 + 12 362 – 1, 603 Hayward (2011). Scand J Rheumatol. 40(5): 379 -82
Excessive suction can be as problematic as excessive pressure

Hemolysis Potential - Large needle; high vacuum - Small needle; large syringe - No needle; excessive pull on syringe barrel

Visual hemolysis - by syringe draws = 19% - by evacuated systems = 3%. Bush V, . (2003). Lab Notes. Winter; 13(1). Excessive pulling on syringe plunger can increase the pressure and hemolyze the cells. Smaller syringes created less than vacuum than larger syringes. - 10 ml syringe generated − 435 Torr - 20 ml generate − 517 Torr https: //www. ncbi. nlm. nih. gov/p mc/articles/PMC 3638030/

Provided by Charter, Medical, Winston-Salem, NC 03 -13 -17 Slowly pull required amount of product through filter into syringe at a rate not exceeding 2 m. L/second. IFU should be on file at facility and should be referenced when writing P&P

AABB Standards A syringe pump should be used over manual pressure. Pulsating flow increases risk of lysis. The smallest catheter that should be used to infuse with a syringe pump to infuse red cells is 25 G. AABB is formerly known as the American Association of Blood Banks

Wrap Up Severe mechanical hemolysis is a rare but potentially lifethreatening complication. Catheter selection for blood administration is a multi-faceted decision; catheter gauge should not be a sole consideration.

Wrap Up − A larger bore catheter may be a safer and more effective method than a pressure bag to achieve high flow rates. − It is not the application of a pressure bag that causes hemolysis; it is the rate at which the blood tries to get through the needle.

Wrap Up PRBCs with additive solutions have the same approximate flow potential as whole blood. Short peripheral catheters provide better flow than comparable CVC lumens The use of I. V. pumps is supported to maintain flow but manufacturer’s or hospital’s validation is required.

Thank you Lynda S. Cook, MSN, RN, CRNI Lynda. Kay 123@aol. com

References Reddick AD, Ronald J, Morrison WG. Intravenous fluid resuscitation: was Poiseuille right? Emerg Med J. 2011 Mar; 28(3): 201 -2. Epub 2010 Jun 26. PMID: 20581377. Kim P, Chin-Yee I, Eckert K, Malthaner RA, Gray DK. (2004). Hemolysis with rapid transfusion systems in the training. Can J Surg. Aug; 47(4): 295 -7. Hayward WA, Haseler LJ, Kettwich LG, Michael AA, Sibbitt WI Jr, Bankhurst AD. (2011). Pressure generated by syringes: implications for hydrodissection and injection of dense connective tissue lesions. Scand J Rheumatol. 40(5): 379 -82 Bush V, Mangan L. (2003). The Hemolyzed Specimen: Causes, Effects, and Reduction. Lab Notes. Winter; 13(1). Weinstein SM, et al. Plummer’s Principles and Practice of I. V. Therapy. 9 th ed. Wolters-Kluwer: Philadelphia, PA. 2014. Phillips L, et al. Manual of I. V. Therapeutics: Evidenced-Based Practice for Infusion Therapy. 6 th ed. F. A. Davis: Philadelphia, PA. 2014 Infusion Therapy Standards of Practice. J Infus Nurs. 2016. 39(1 S) Fung, MK, et al. Technical Manual. 18 th ed. AABB: Bethesda, MD. 2014.

References SAI infusion technology Conversion tables; Viewed on line 03 -18 -17; www. SAIinfusion. com AABB: Standards for blood banks and transfusion services, ed 25, Bethesda, Md, 2014

- Slides: 66