Blood Pressure Hypertension Orthostatics Sina Raissi MD FACP

Blood Pressure Hypertension Orthostatics Sina Raissi, MD, FACP, FASN

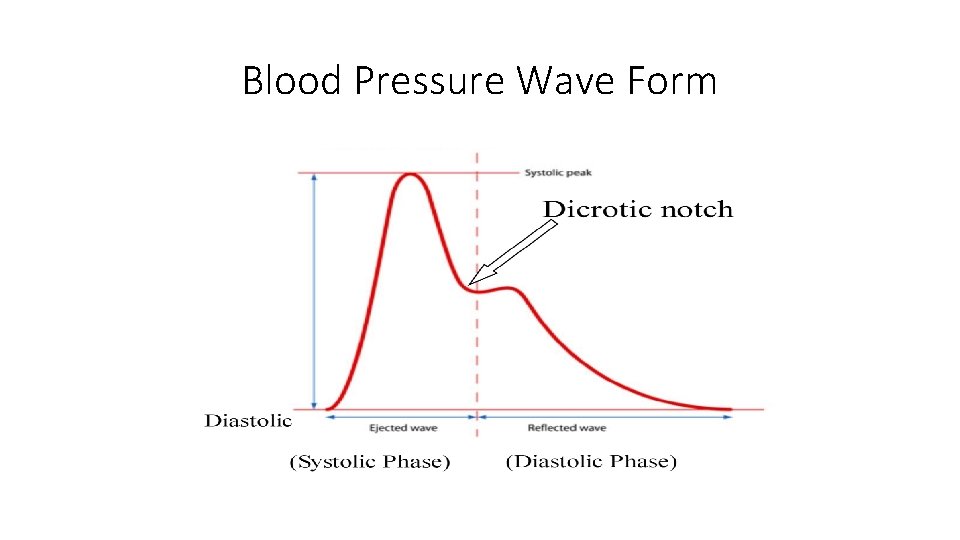
Blood Pressure Wave Form
Hypertension Atherosclerosis Cardiovascular events

Cardiovascular complications of uncontrolled hypertension • Stroke: Ischemic/hemorrhagic
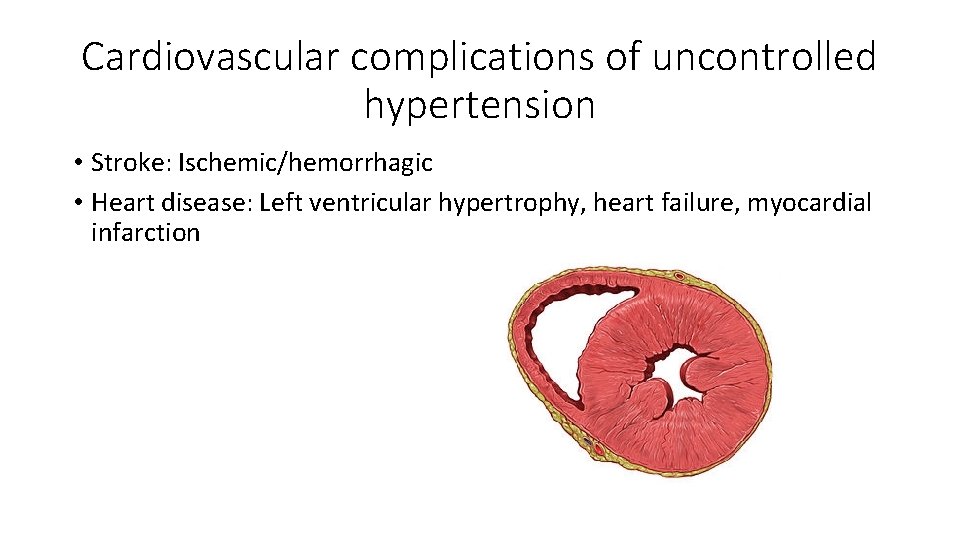
Cardiovascular complications of uncontrolled hypertension • Stroke: Ischemic/hemorrhagic • Heart disease: Left ventricular hypertrophy, heart failure, myocardial infarction
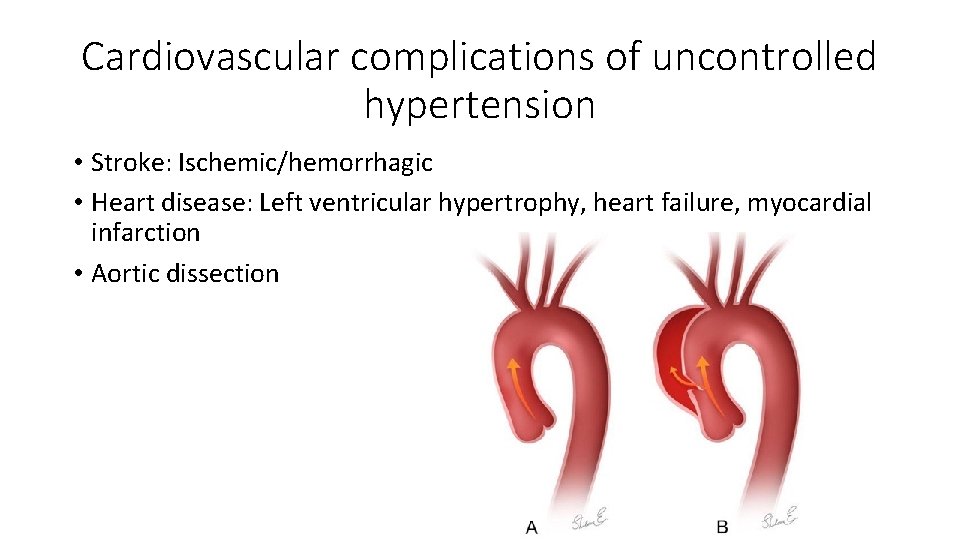
Cardiovascular complications of uncontrolled hypertension • Stroke: Ischemic/hemorrhagic • Heart disease: Left ventricular hypertrophy, heart failure, myocardial infarction • Aortic dissection
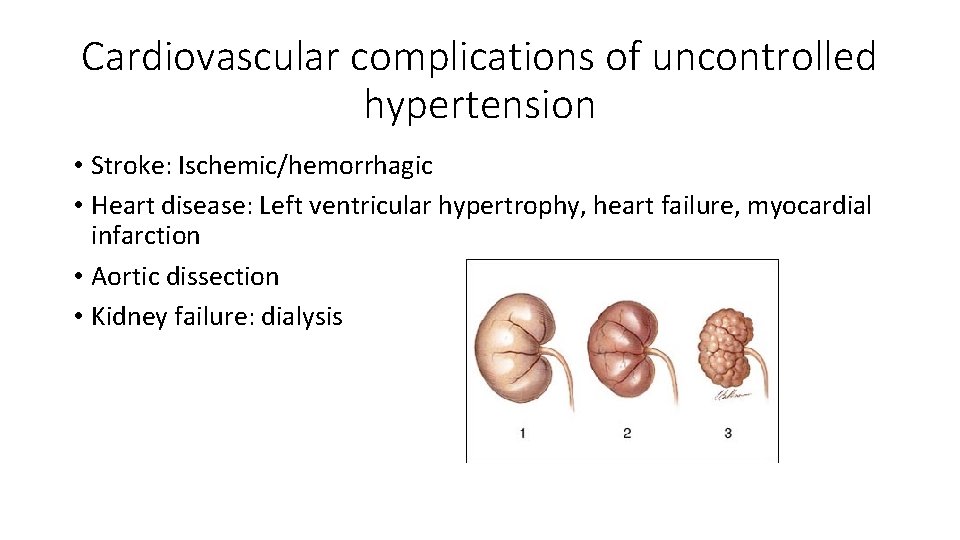
Cardiovascular complications of uncontrolled hypertension • Stroke: Ischemic/hemorrhagic • Heart disease: Left ventricular hypertrophy, heart failure, myocardial infarction • Aortic dissection • Kidney failure: dialysis
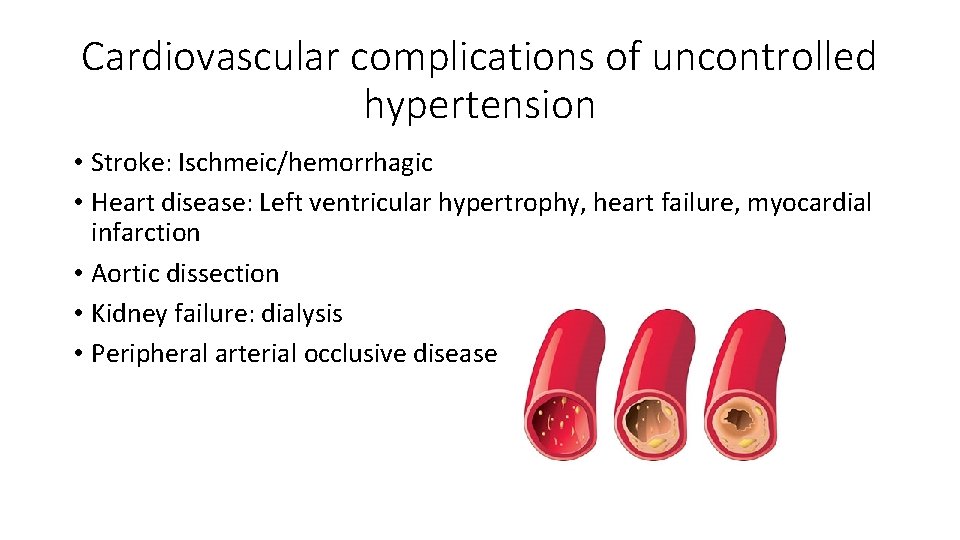
Cardiovascular complications of uncontrolled hypertension • Stroke: Ischmeic/hemorrhagic • Heart disease: Left ventricular hypertrophy, heart failure, myocardial infarction • Aortic dissection • Kidney failure: dialysis • Peripheral arterial occlusive disease

Blood Pressure Measurement • Office-based measurement • Home BP monitoring • Ambulatory blood pressure monitoring
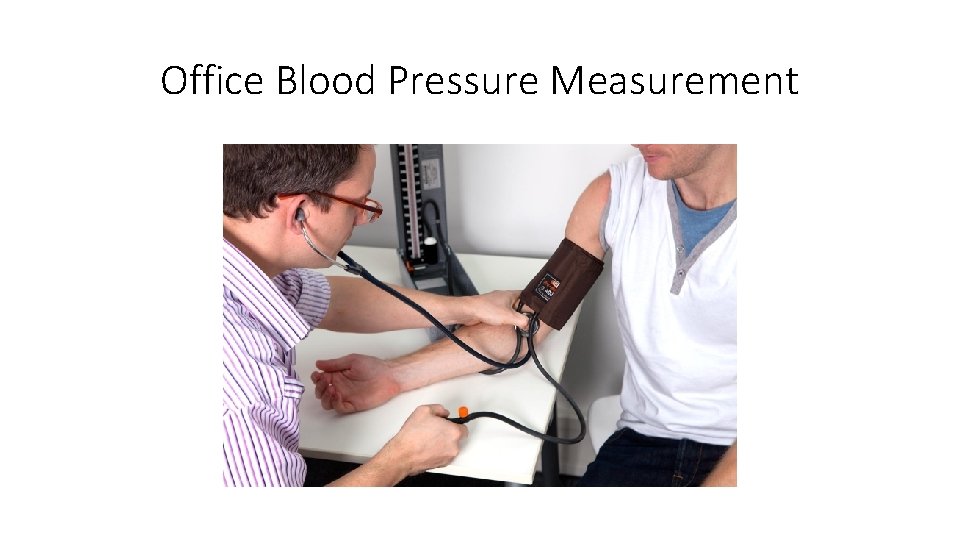
Office Blood Pressure Measurement

Office Blood Pressure Measurement • Time of measurement
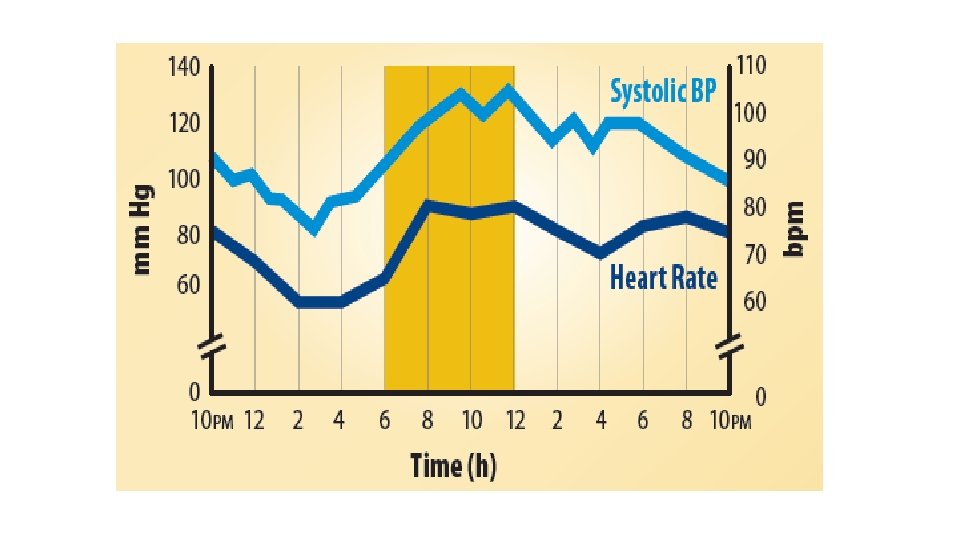

Office Blood Pressure Measurement • Time of measurement • Type of instrument
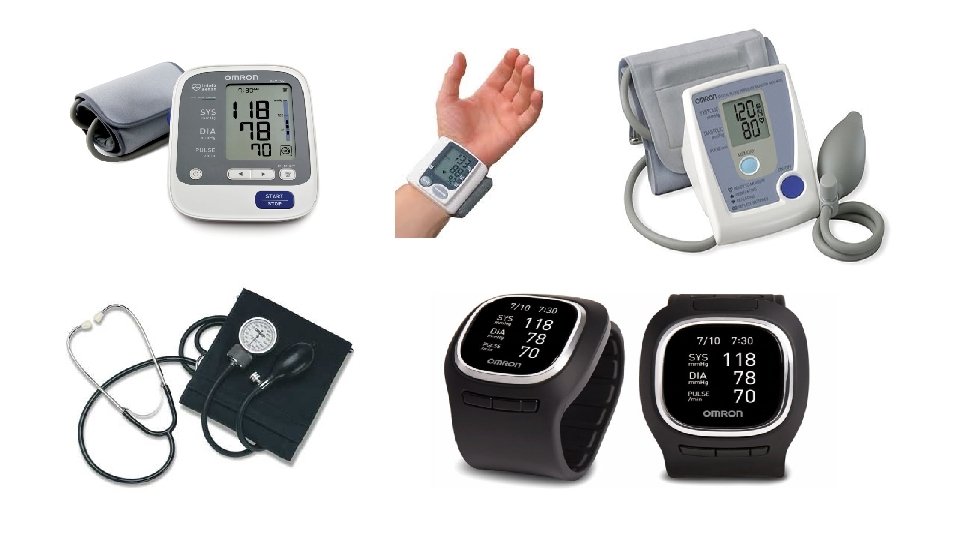

Office Blood Pressure Measurement • Time of measurement • Type of instrument • Cuff size


Office Blood Pressure Measurement • Time of measurement • Type of instrument • Cuff size • Patient position

Office Blood Pressure Measurement • Time of measurement • Type of instrument • Cuff size • Patient position • Cuff placement

Office Blood Pressure Measurement • Time of measurement • Type of instrument • Cuff size • Patient position • Cuff placement • Technique of measurement

Office Blood Pressure Measurement • Time of measurement • Type of instrument • Cuff size • Patient position • Cuff placement • Technique of measurement • Number of measurements

Patients should avoid the following for 30 minutes before measurement • Exercise • Caffeine • Smoking • Food intake • Decongestants

• The wrong size cuff results in higher systolic blood pressure reading than patient’s real blood pressure.

Cuff Size by AHA • Arm circumference 22 -26 cm: SMALL ADULT cuff 12 x 22 cm • Arm circumference 27 -34 cm: ADULT cuff 16 x 30 cm • Arm circumference 35 -44 cm: LARGE ADULT cuff 16 x 36 cm • Arm circumference 42 -52 cm: ADULT THIGH cuff 16 x 42 cm
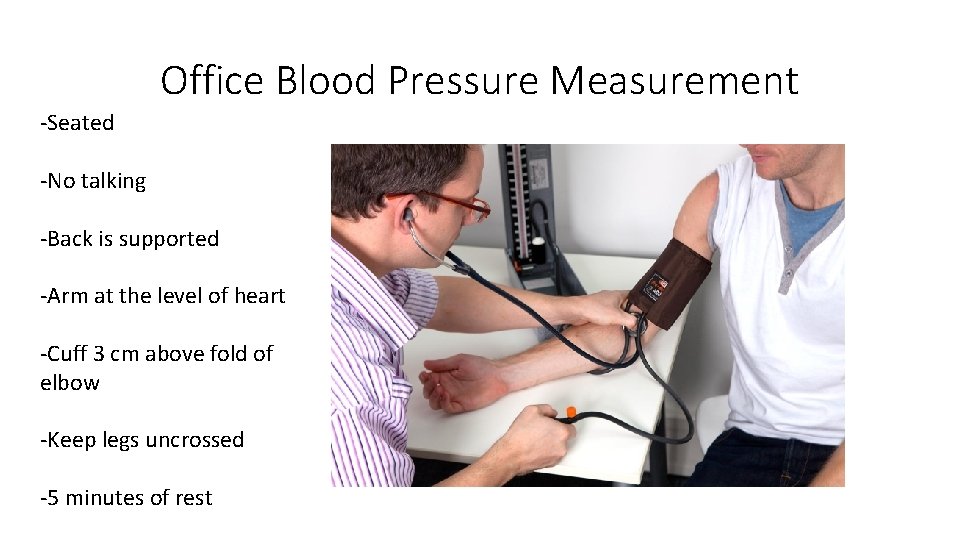
Office Blood Pressure Measurement -Seated -No talking -Back is supported -Arm at the level of heart -Cuff 3 cm above fold of elbow -Keep legs uncrossed -5 minutes of rest

Blood Pressure Measurement Technique • Inflate the cuff up to 30 mm. Hg above systolic BP as detected by disappearance of brachial pulse.

Blood Pressure Measurement Technique • Inflate the cuff up to 30 mm. Hg above systolic BP as detected by disappearance of brachial pulse. • Place the stethoscope LIGHTLY on brachial artery. Otherwise increased turbulence may result in artificial reduction in measured diastolic BP by 10 -15 mm. Hg.

Blood Pressure Measurement Technique • Inflate the cuff up to 30 mm. Hg above systolic BP as detected by disappearance of brachial pulse. • Place the stethoscope LIGHTLY on brachial artery. Otherwise increased turbulence may result in artificial reduction in measured diastolic BP by 10 -15 mm. Hg. • Deflate the cuff slowly (about 5 seconds for each 10 mm. Hg decline). Fast deflation results in lower SBP and higher DBP reading.

Blood Pressure Measurement Technique • Inflate the cuff up to 30 mm. Hg above systolic BP as detected by disappearance of brachial pulse. • Place the stethoscope LIGHTLY on brachial artery. Otherwise increased turbulence may result in artificial reduction in measured diastolic BP by 10 -15 mm. Hg. • Deflate the cuff slowly (about 5 seconds for each 10 mm. Hg decline). Fast deflation results in lower SBP and higher DBP reading. • The first pulse sound (Korotkoff phase I) SBP • Sudden muffling of pulse sounds (phase IV) DBP
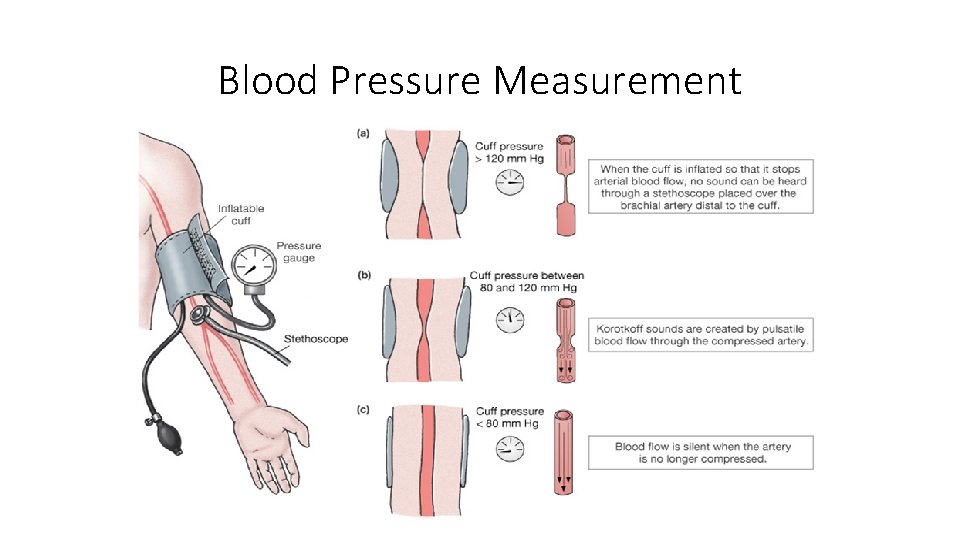
Blood Pressure Measurement

Blood Pressure Measurement • Blood pressure must be measured in both arms, the arm with the higher BP recording should be used for measurement.

Blood Pressure Measurement • Blood pressure must be measured in both arms, the arm with the higher BP recording should be used for measurement. • Blood pressure must be measured at least twice on each office visit.

Blood Pressure Measurement • Blood pressure must be measured in both arms, the arm with the higher BP recording should be used for measurement. • Blood pressure must be measured at least twice on each office visit. • BP should be measured in standing position when indicated.

Blood Pressure Measurement • Blood pressure must be measured in both arms, the arm with the higher BP recording should be used for measurement. • Blood pressure must be measured at least twice on each office visit. • BP should be measured in standing position when indicated. • In the absence of end organ damage, BP should be measured over the course of 3 -6 visits (1 -6 weeks) before a diagnosis of hypertension is made.

Pitfalls of Office BP measurement • White coat syndrome • Masked Hypertension
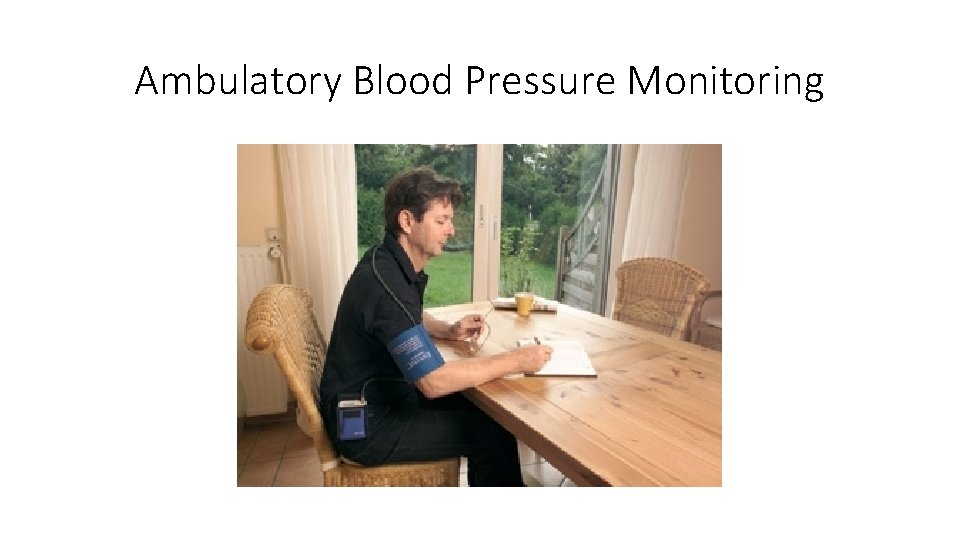
Ambulatory Blood Pressure Monitoring
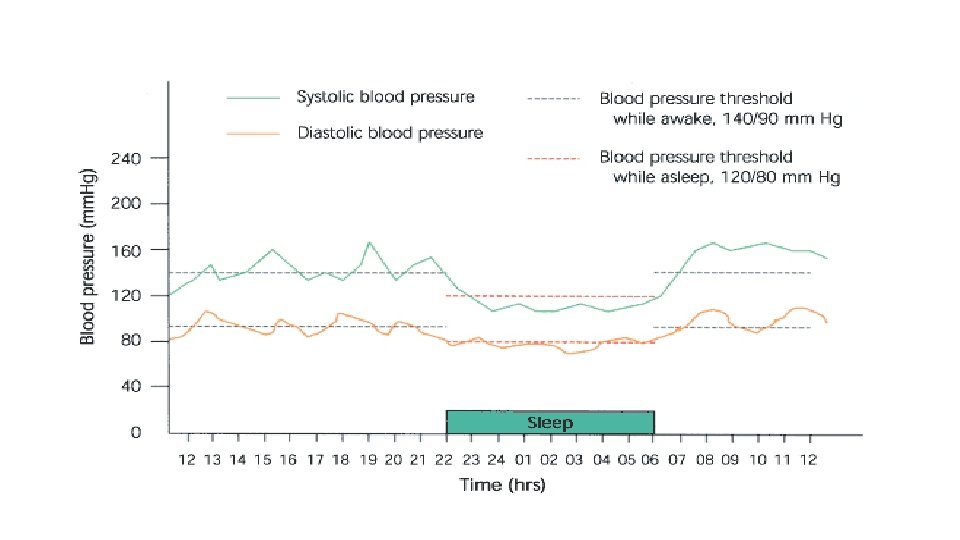
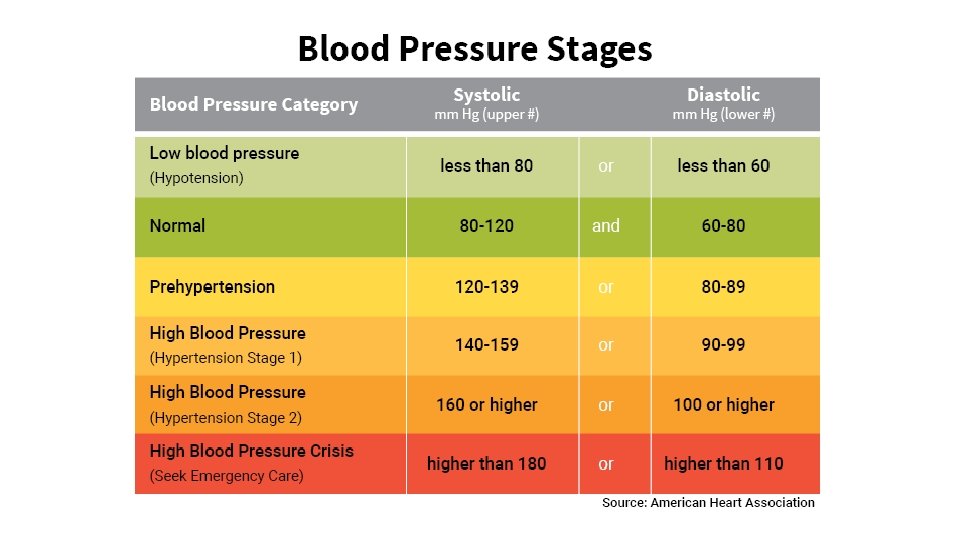

Definition of Hypertension • Office BP measurement: systolic BP > 140 mm. Hg or diastolic BP > 90 mm. Hg. (with an automated oscillometric BP device AOBP threshold of > 135/85 mm. Hg is acceptable. ) • Home BP monitoring: systolic BP > 135 mm. Hg or diastolic BP > 85 mm. Hg. • Ambulatory BP monitoring: Average daytime SBP > 135 mm. Hg or DBP > 85 mm. Hg, or Average 24 hour SBP >130 mm. Hg or DBP > 80 mm. Hg.

Orhtostatic Hypotension

Baroreceptor Reflex
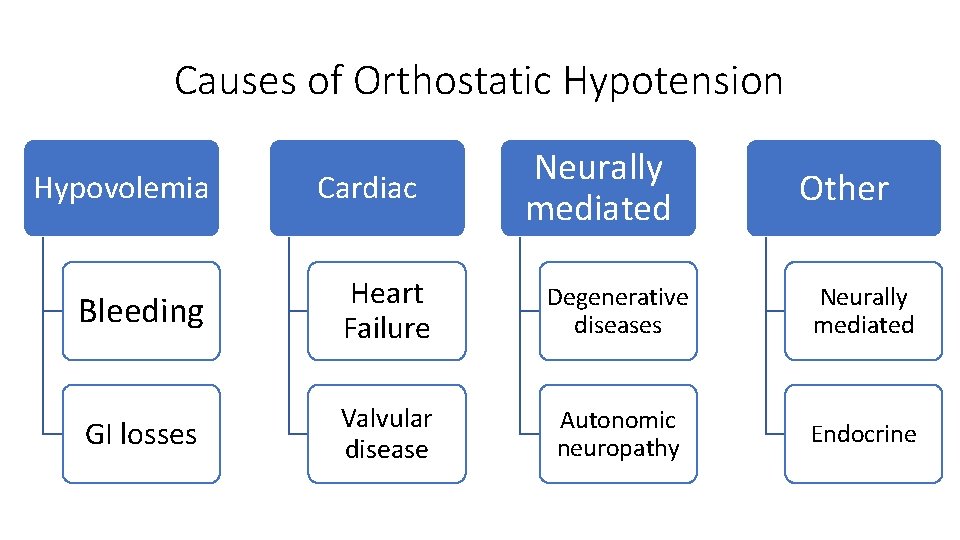
Causes of Orthostatic Hypotension Hypovolemia Cardiac Neurally mediated Other Bleeding Heart Failure Degenerative diseases Neurally mediated GI losses Valvular disease Autonomic neuropathy Endocrine

Orthostatic Blood Pressure • Assess the need for orthostatics.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine. • Have the patient sit up for ONE minute.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine. • Have the patient sit up for ONE minute. • Obtain the patient’s pulse rate and blood pressure while sitting.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine. • Have the patient sit up for ONE minute. • Obtain the patient’s pulse rate and blood pressure while sitting. • If positive orthostatic changes occur while sitting, DO NOT continue to standing position.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine. • Have the patient sit up for ONE minute. • Obtain the patient’s pulse rate and blood pressure while sitting. • If positive orthostatic changes occur while sitting, DO NOT continue to standing position. • Have patient stand up for ONE minute. Free standing, not leaning.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine. • Have the patient sit up for ONE minute. • Obtain the patient’s pulse rate and blood pressure while sitting. • If positive orthostatic changes occur while sitting, DO NOT continue to standing position. • Have patient stand up for ONE minute. Free standing, not leaning. • Obtain patient’s blood pressure and pulse while standing up.

Orthostatic Blood Pressure • Assess the need for orthostatics. • Obtain patient’s pulse rate and blood pressure while supine. • Have the patient sit up for ONE minute. • Obtain the patient’s pulse rate and blood pressure while sitting. • If positive orthostatic changes occur while sitting, DO NOT continue to standing position. • Have patient stand up for ONE minute. Free standing, not leaning. • Obtain patient’s blood pressure and pulse while standing up. • Watch for possibility of orthostatic symptoms or syncope.

Orthostatics Result • Orthostatics are considered POSITIVE if:

Orthostatics Result • Orthostatics are considered POSITIVE if: • Patient becomes severely symptomatic

Orthostatics Result • Orthostatics are considered POSITIVE if: • Patient becomes severely symptomatic • Pulse increases by more than 20 bpm

Orthostatics Result • Orthostatics are considered POSITIVE if: • Patient becomes severely symptomatic • Pulse increases by more than 20 bpm • Systolic BP falls by more than 20 mm. Hg

Orthostatics Result • Orthostatics are considered POSITIVE if: • Patient becomes severely symptomatic • Pulse increases by more than 20 bpm • Systolic BP falls by more than 20 mm. Hg • Increase in pulse by 10 bpm AND decrease in systolic BP by more than 10 mm. Hg in a symptomatic patient


THANK YOU
- Slides: 57