Blood Physiology The functions of blood are Transport

Blood Physiology
• The functions of blood are • Transport • Regulation • Protection The functions of blood

The functions of blood - Transport functions of blood include: • Delivering oxygen from the lungs and nutrients from the digestive tract to all body cells. • Transporting metabolic waste products from cells to elimination sites • to the lungs to eliminate carbon dioxide • To the kidneys to dispose of nitrogenous wastes in urine • Transporting hormones from the endocrine organs to their target organs.

Regulatory functions of blood include: • Maintaining appropriate body temperature by absorbing and distributing heat throughout the body and to the skin surface to encourage heat loss. • Maintaining normal p. H in body tissues. • Contains buffers in the form of proteins, solutes and the body’s “alkaline reserve” of bicarbonate ions. The functions of blood Regulation • Maintaining adequate fluid volume in the circulatory system. • Blood proteins prevent excessive fluid loss • Keeps the fluid volume in the blood vessels steady

The functions of blood - Protection Protective functions of blood include: • Preventing blood loss. • When a blood vessel is damaged, platelets and plasma proteins initiate clot formation, halting blood loss. • Preventing infection. • Contains antibodies, complement proteins, and white blood cells, all of which help defend the body against foreign invaders such as bacteria and viruses.
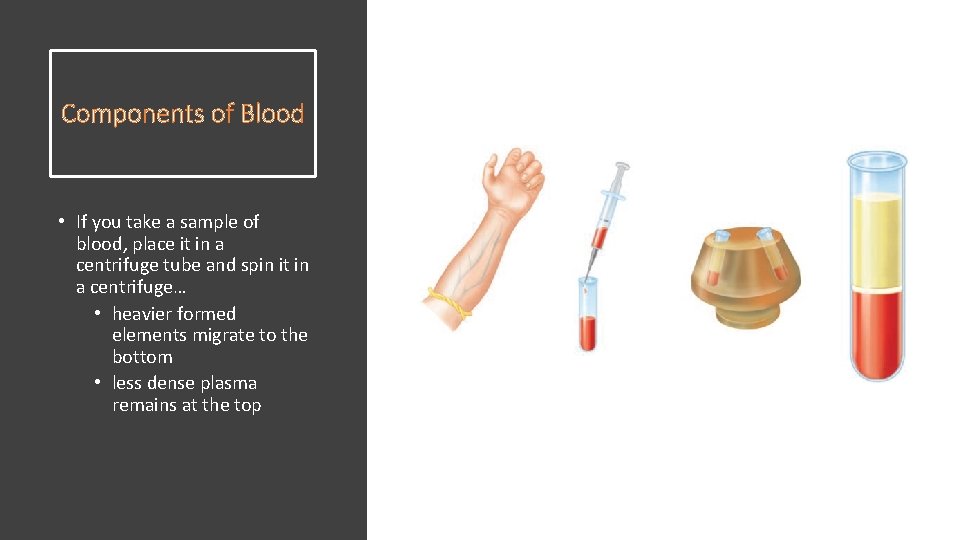
Components of Blood • If you take a sample of blood, place it in a centrifuge tube and spin it in a centrifuge… • heavier formed elements migrate to the bottom • less dense plasma remains at the top
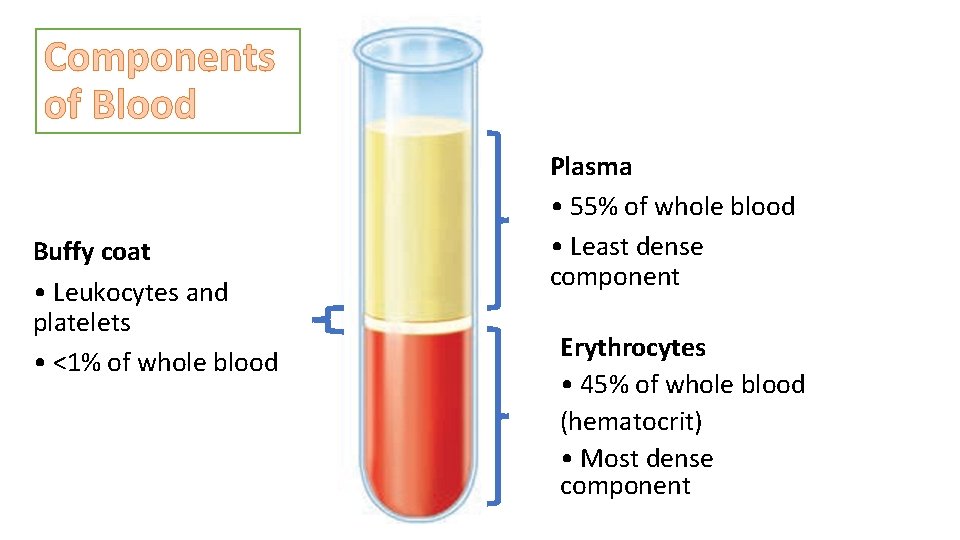
Components of Blood Buffy coat • Leukocytes and platelets • <1% of whole blood Plasma • 55% of whole blood • Least dense component Erythrocytes • 45% of whole blood (hematocrit) • Most dense component

• Most of the reddish mass at the bottom of the tube is erythrocytes, the red blood cells that transport oxygen. • Erythrocytes normally constitute about 45% of the total volume of a blood sample, a percentage known as the hematocrit • Normal hematocrit values vary. Components of Blood hematocrit • In males ~ 47% • In females ~ 42%
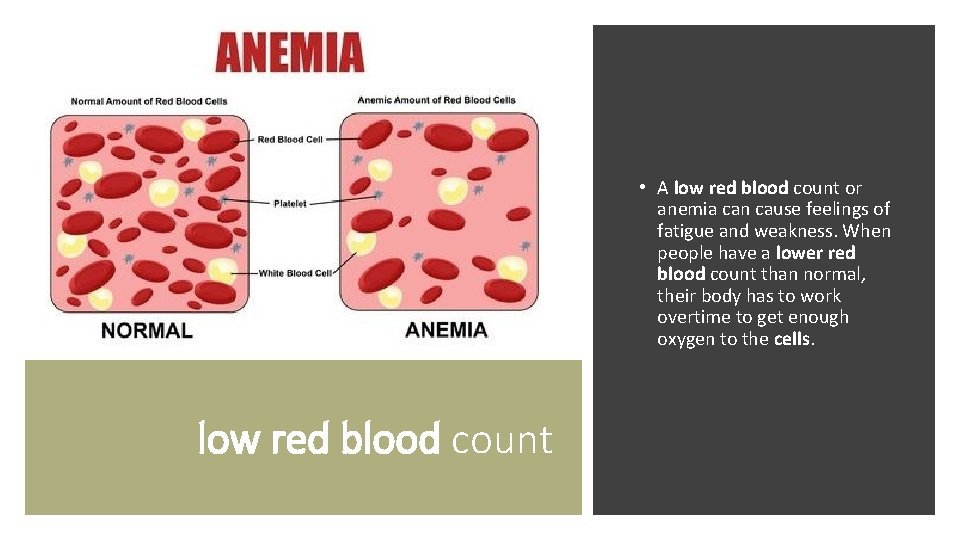
• A low red blood count or anemia can cause feelings of fatigue and weakness. When people have a lower red blood count than normal, their body has to work overtime to get enough oxygen to the cells. low red blood count

high red blood count • Polycythemia vera (a blood disorder in which the bone marrow produces too many red blood cells) • The main problem caused by polycythaemia vera is that the high number of red cells increases the blood's 'thickness' (viscosity). • Blood flow to organs is reduced and, rarely, blood clots can form.
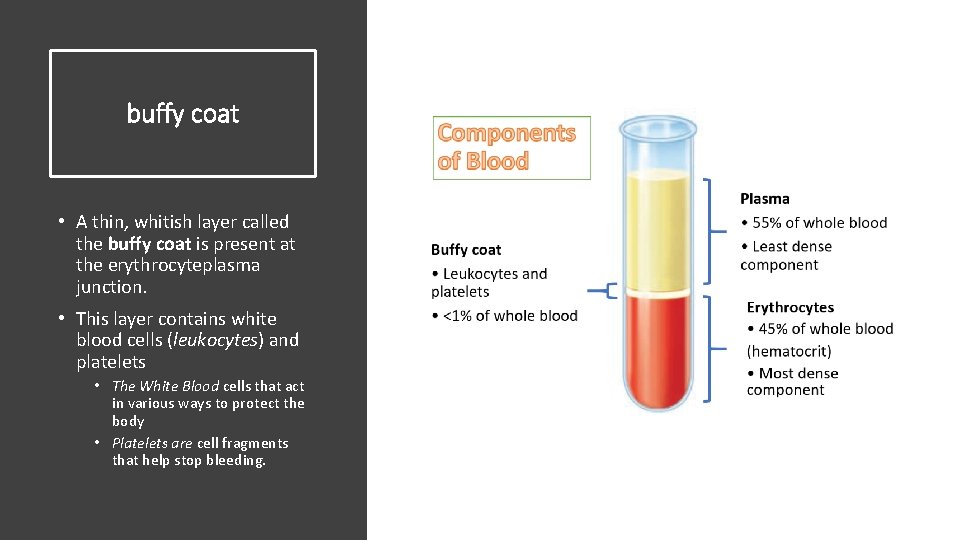
buffy coat • A thin, whitish layer called the buffy coat is present at the erythrocyteplasma junction. • This layer contains white blood cells (leukocytes) and platelets • The White Blood cells that act in various ways to protect the body • Platelets are cell fragments that help stop bleeding.

Physical Characteristics and Volume Blood is slightly alkaline, with a p. H between 7. 35 and 7. 45.
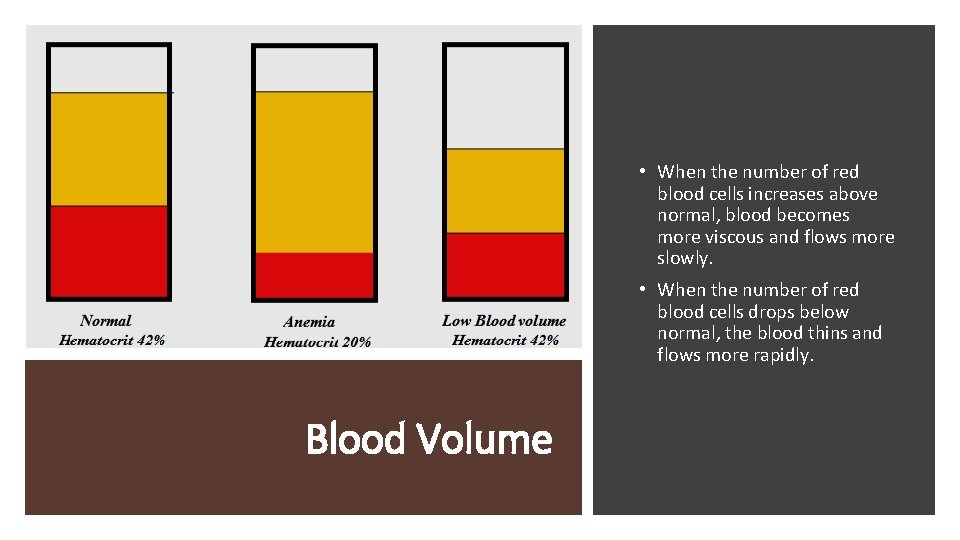
• When the number of red blood cells increases above normal, blood becomes more viscous and flows more slowly. • When the number of red blood cells drops below normal, the blood thins and flows more rapidly. Blood Volume
• Blood accounts for approximately 8% of body weight. • Blood volume in healthy adult males = 5– 6 L. • Blood volume in healthy adult females = 4– 5 L. Blood Volume

• Water = 90% of plasma volume • Functions in dissolving and suspending medium for solutes of blood • Functions to absorb heat Composition of Plasma – Water

Solutes Composition of Plasma – Solutes • Electrolytes • Most abundant solutes by number; • cations include sodium, potassium, calcium, magnesium • anions include chloride, phosphate, sulfate, and bicarbonate • Functions to maintain osmotic pressure • Functions to maintain normal blood p. H

Composition of Plasma – Solutes • Plasma proteins 8% (by weight) of plasma; • contribute to osmotic pressure • maintain water balance in blood • Other specialized function
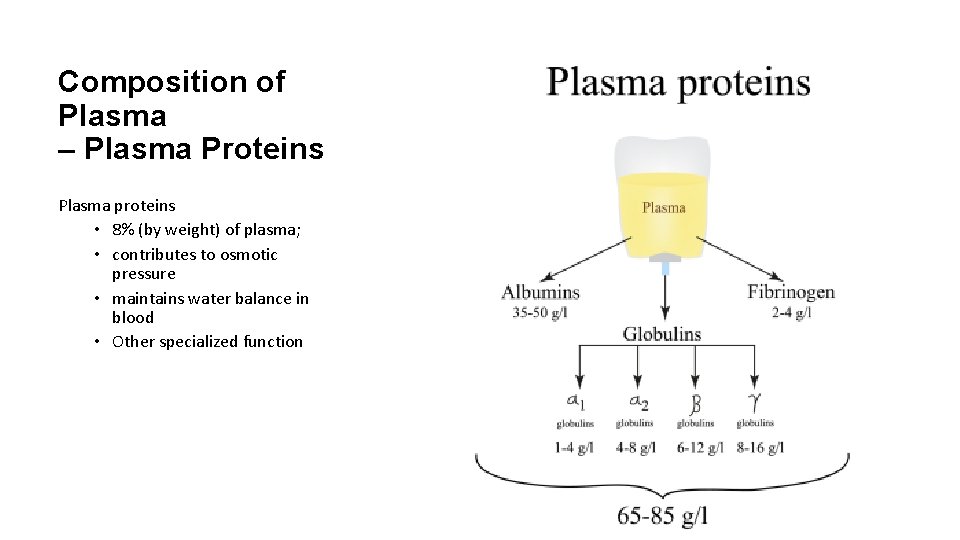
Composition of Plasma – Plasma Proteins Plasma proteins • 8% (by weight) of plasma; • contributes to osmotic pressure • maintains water balance in blood • Other specialized function

Albumin • 60% of plasma proteins • Produced by liver • It acts as a carrier to shuttle certain molecules through the circulation • It is an important blood buffer Composition of Plasma – Plasma Proteins • It is the major blood protein contributing to the plasma osmotic pressure (the pressure that helps to keep water in the bloodstream).

Composition of Plasma – Plasma Proteins Globulins = 36% of plasma proteins • Globulin is categorized into three main groups: • alpha globulins • beta globulins • gamma globulins
Composition of Plasma – Plasma Proteins GLOBULINS • alpha globulins and beta globulins are primarily transport proteins • Produced by liver; most are transport proteins that bind to lipids, metal ions, and fatsoluble vitamins

Composition of Plasma – Plasma Proteins GLOBULINS • gamma globulins are mainly comprised of immunoglobulins (Igs), also known as antibodies • Antibodies released by plasma cells during immune response
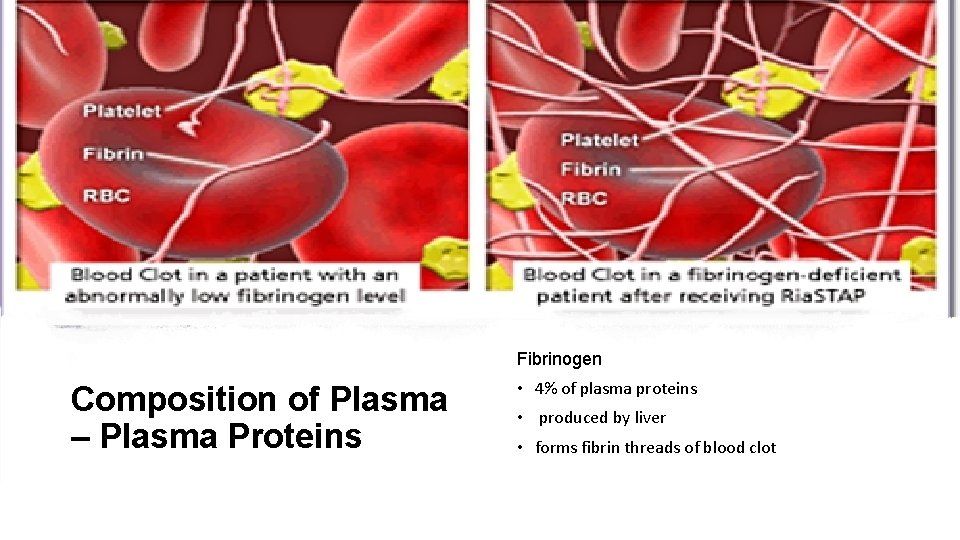
Fibrinogen Composition of Plasma – Plasma Proteins • 4% of plasma proteins • produced by liver • forms fibrin threads of blood clot

Composition of Plasma – Nonprotein nitrogenous substances By-products of cellular metabolism • Urea • Uric Acid • Creatinine • Ammonium Salts

Nutrients Composition of Plasma – Nutrients • Materials absorbed from digestive tract and transported for use throughout body • Glucose and other simple carbohydrates • Amino acids (protein building blocks) • Fatty acids - glycerol and triglycerides (fat digestion products) • Cholesterol • Vitamins
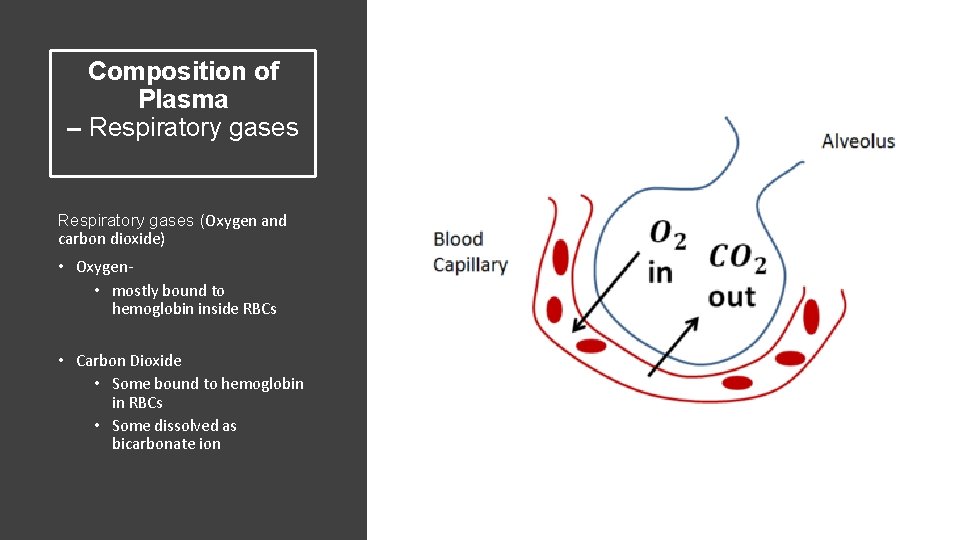
Composition of Plasma – Respiratory gases (Oxygen and carbon dioxide) • Oxygen • mostly bound to hemoglobin inside RBCs • Carbon Dioxide • Some bound to hemoglobin in RBCs • Some dissolved as bicarbonate ion
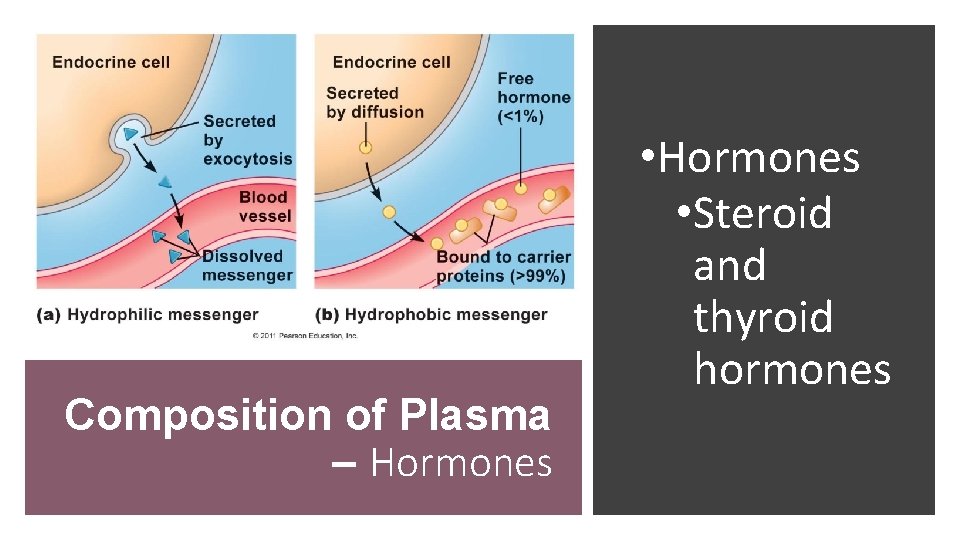
Composition of Plasma – Hormones • Steroid and thyroid hormones

• When the blood starts to become too acidic (acidosis), both the lungs and the kidneys are called into action to restore plasma’s normal, slightly alkaline p. H (7. 4). • Body organs make dozens of adjustments, day in and day out, to maintain the many plasma solutes at lifesustaining levels. p. H of Blood
The formed elements of blood • The formed elements of blood— • Erythrocytes • Leukocytes • Platelets

Cells or not? • Erythrocytes have no nuclei or organelles. • Platelets are cell fragments. • Only leukocytes are complete cells. The formed elements of blood Short life-span • Most types of formed elements survive in the bloodstream for only a few days. Reproduction • Most blood cells do not divide. • Instead, stem cells divide continuously in red bone marrow to replace them.
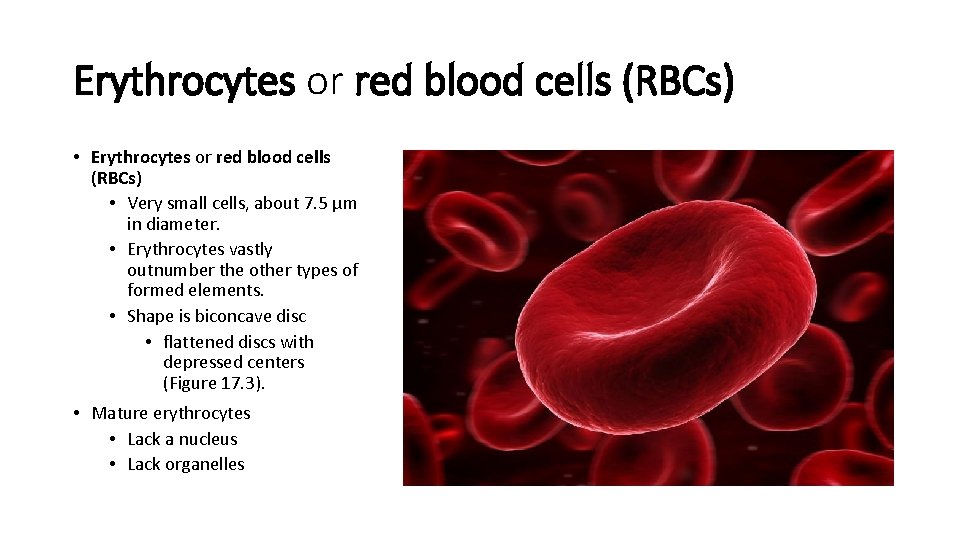
Erythrocytes or red blood cells (RBCs) • Very small cells, about 7. 5 μm in diameter. • Erythrocytes vastly outnumber the other types of formed elements. • Shape is biconcave disc • flattened discs with depressed centers (Figure 17. 3). • Mature erythrocytes • Lack a nucleus • Lack organelles
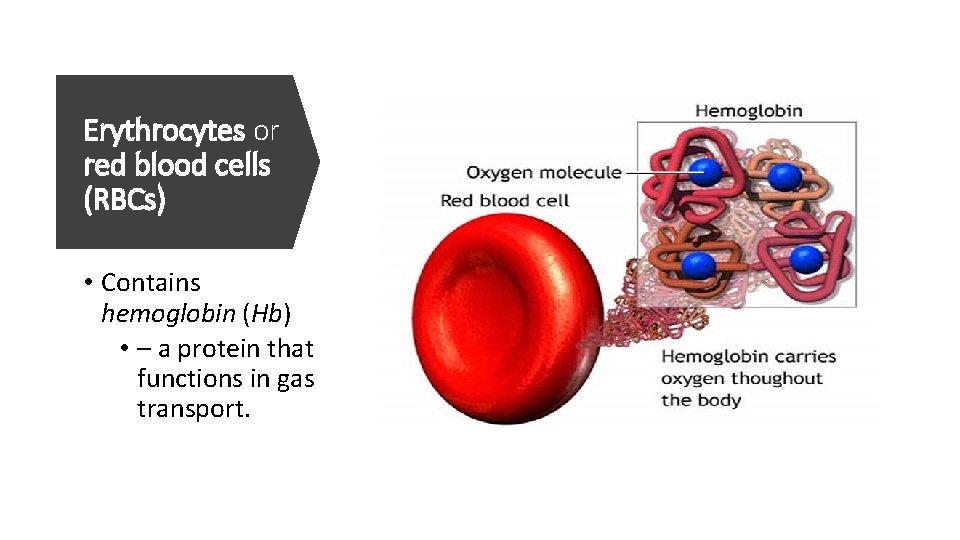
Erythrocytes or red blood cells (RBCs) • Contains hemoglobin (Hb) • – a protein that functions in gas transport.

Erythrocytes or red blood cells (RBCs) • spectrin • attaches to the cytoplasmic face of RBC plasma membranes to maintain the biconcave shape of an erythrocyte. • the spectrin net is deformable, allowing erythrocytes to change shape as necessary
Erythrocytes or red blood cells (RBCs) • picks up oxygen in the capillaries of the lungs and releases it to tissue cells across other capillaries throughout the body. • transports ~ 20% of the carbon dioxide released by tissue cells back to the lungs.

Characteristics that contribute to erythrocyte gas transport functions: Erythrocytes or red blood cells (RBCs) • Shape – Biconcave Disc • High surface area-to-volume ratio – • Its small size and shape provide a huge surface area relative to volume (about 30% more surface area than comparable spherical cells). • Large Surface Area – • The disc shape maximizes the surface area to allow for maximal diffusion of gas. • Hemoglobin – Ability to bind O 2 and CO 2 • This molecule binds to and transports respiratory gases (oxygen and carbon dioxide). • Energy Efficient - Don’t need to use any of the oxygen they carry • Lack mitochondria • Generate ATP anaerobically • Don’t reproduce
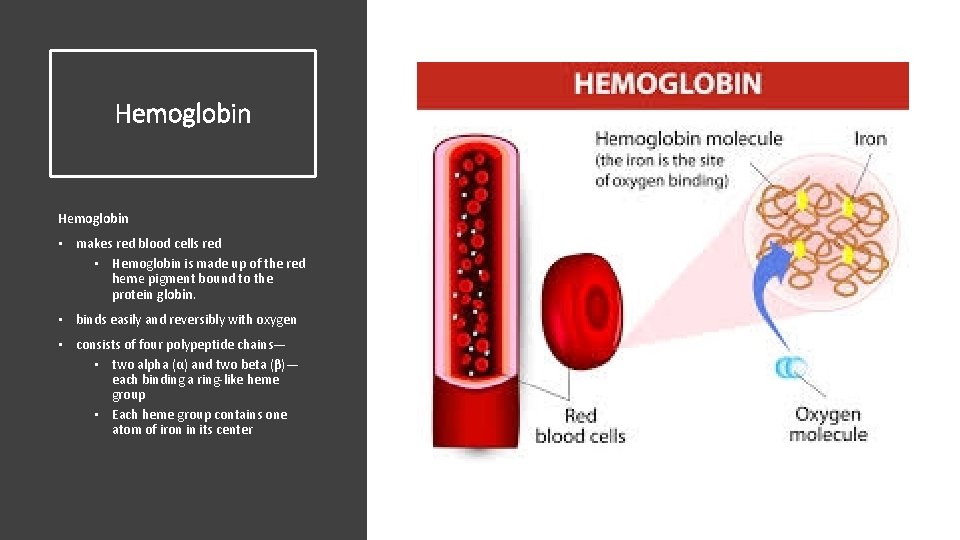
Hemoglobin • makes red blood cells red • Hemoglobin is made up of the red heme pigment bound to the protein globin. • binds easily and reversibly with oxygen • consists of four polypeptide chains— • two alpha (α) and two beta (β)— each binding a ring-like heme group • Each heme group contains one atom of iron in its center
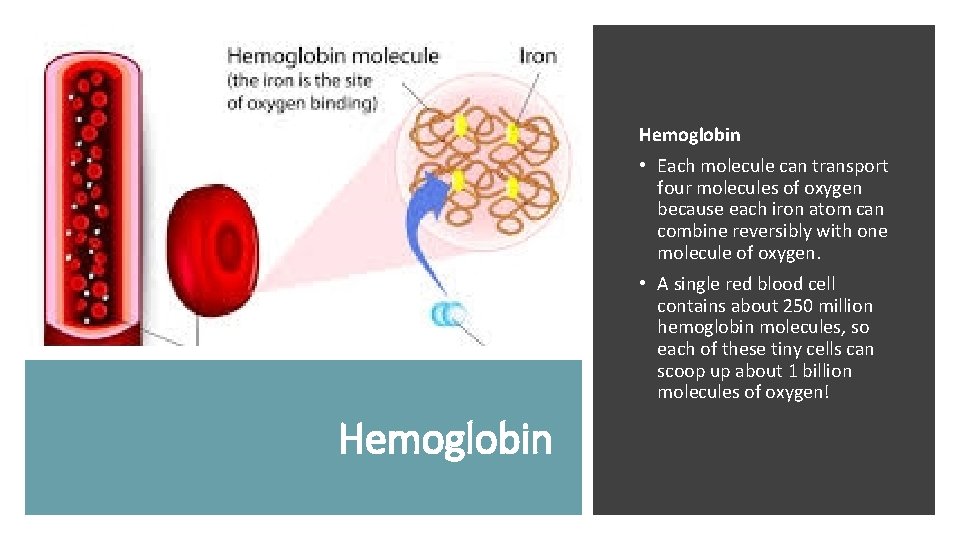
Hemoglobin • Each molecule can transport four molecules of oxygen because each iron atom can combine reversibly with one molecule of oxygen. • A single red blood cell contains about 250 million hemoglobin molecules, so each of these tiny cells can scoop up about 1 billion molecules of oxygen! Hemoglobin

Oxygen-deficient blood moves to the lungs Oxygen loading from the lungs and oxygen transport to tissue cells Oxygen diffuses from the alveoli (air sacs) of the lungs into the blood stream Oxygen diffuses into the erythrocytes and binds to the iron atom in the center of hemoglobin. When oxygen binds to iron, the hemoglobin, now called oxyhemoglobin, assumes a new three dimensional shape and becomes ruby red.
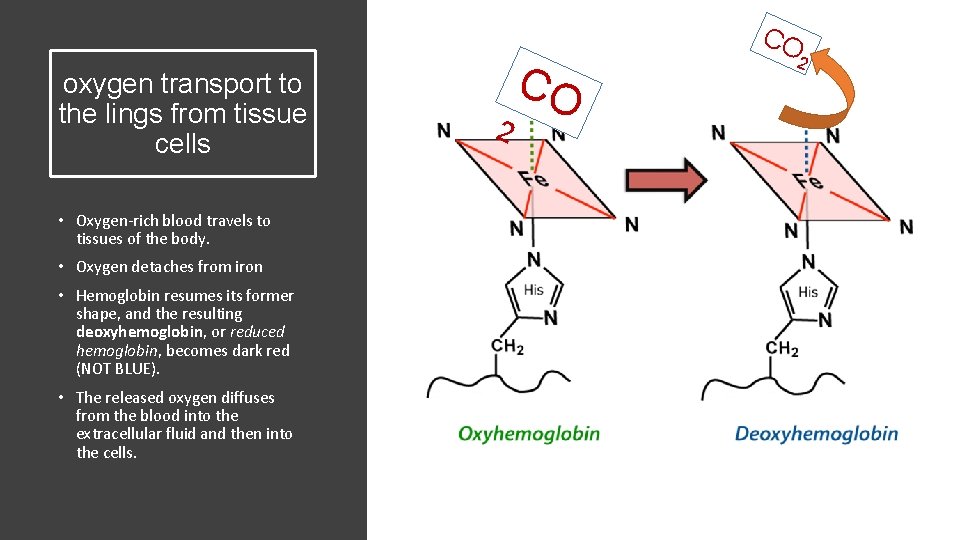
oxygen transport to the lings from tissue cells • Oxygen-rich blood travels to tissues of the body. • Oxygen detaches from iron • Hemoglobin resumes its former shape, and the resulting deoxyhemoglobin, or reduced hemoglobin, becomes dark red (NOT BLUE). • The released oxygen diffuses from the blood into the extracellular fluid and then into the cells. 2 CO CO 2
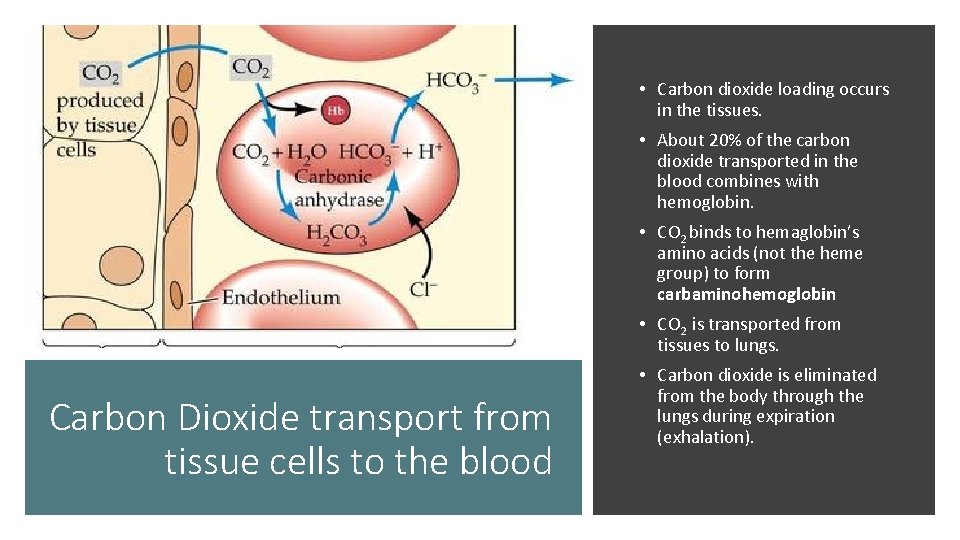
• Carbon dioxide loading occurs in the tissues. • About 20% of the carbon dioxide transported in the blood combines with hemoglobin. • CO 2 binds to hemaglobin’s amino acids (not the heme group) to form carbaminohemoglobin • CO 2 is transported from tissues to lungs. Carbon Dioxide transport from tissue cells to the blood • Carbon dioxide is eliminated from the body through the lungs during expiration (exhalation).
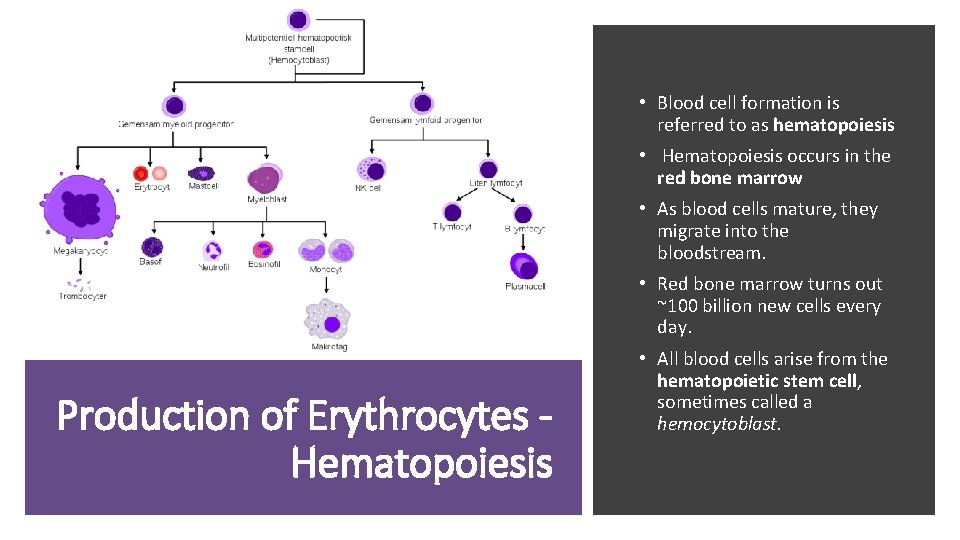
• Blood cell formation is referred to as hematopoiesis • Hematopoiesis occurs in the red bone marrow • As blood cells mature, they migrate into the bloodstream. • Red bone marrow turns out ~100 billion new cells every day. Production of Erythrocytes Hematopoiesis • All blood cells arise from the hematopoietic stem cell, sometimes called a hemocytoblast.
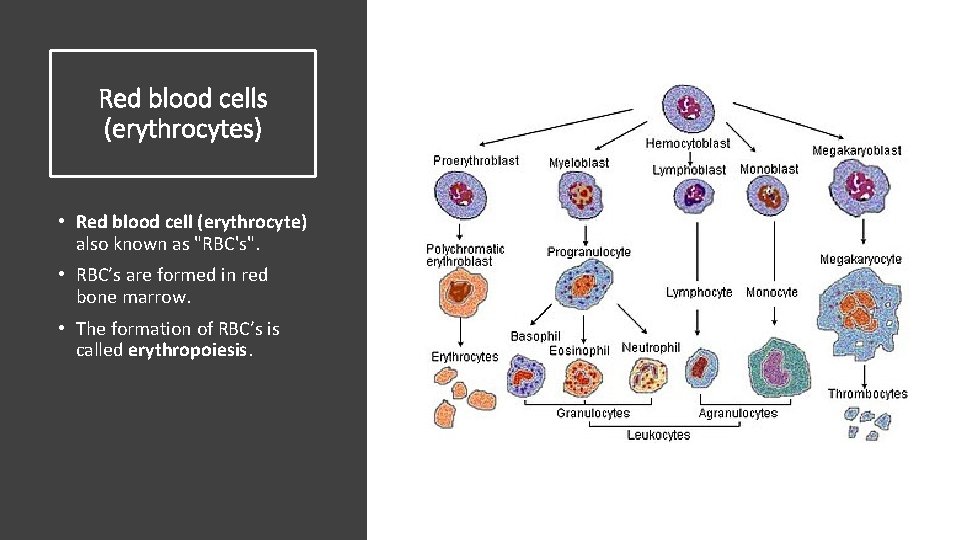
Red blood cells (erythrocytes) • Red blood cell (erythrocyte) also known as "RBC's". • RBC’s are formed in red bone marrow. • The formation of RBC’s is called erythropoiesis.

Red blood cells (erythrocytes) - Characteristics Anucleate - Red blood cells lose nuclei upon maturation Lack Essentially All Organelles Do not reproduce themsleves Shape - take on a biconcave, dimpled, disc shape. Small - They are about 7 -8 micrometers in diameter.

Red blood cells (erythrocytes) Characteristics Simple - RBC's lack a nucleus (no DNA) and no organelles Numerous - There about 1000 x more red blood cells than white blood cells. Short-lived - RBC's live about 120 days and do not self repair. Easily replaced - Myeloid tissue will produce about 200 billion RBCs a day! Carry hemoglobin - RBC's contain hemoglobin which transports oxygen from the lungs to the rest of the body, such as to the muscles, where it releases the oxygen load. • Red in Color - The hemoglobin gets it’s red color from their respiratory pigments. • • •
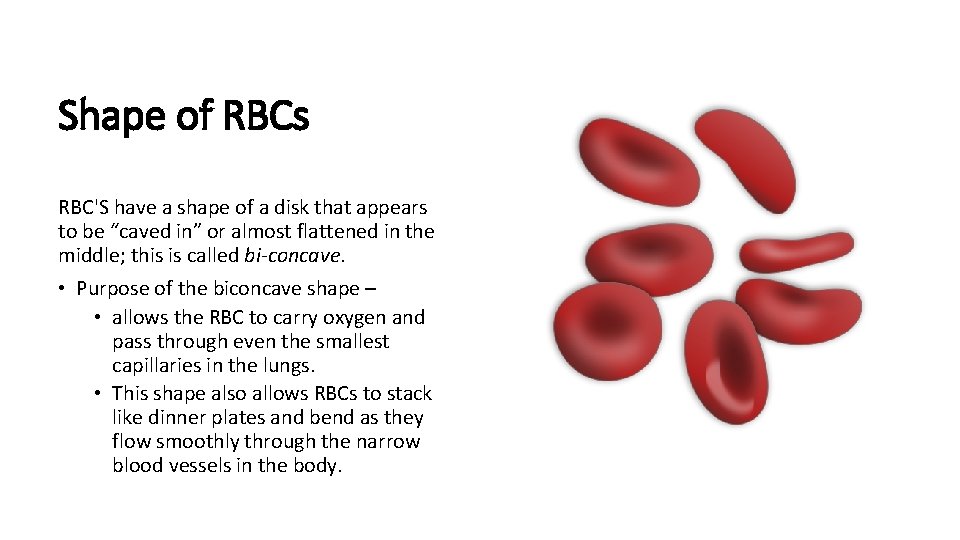
Shape of RBCs RBC'S have a shape of a disk that appears to be “caved in” or almost flattened in the middle; this is called bi-concave. • Purpose of the biconcave shape – • allows the RBC to carry oxygen and pass through even the smallest capillaries in the lungs. • This shape also allows RBCs to stack like dinner plates and bend as they flow smoothly through the narrow blood vessels in the body.
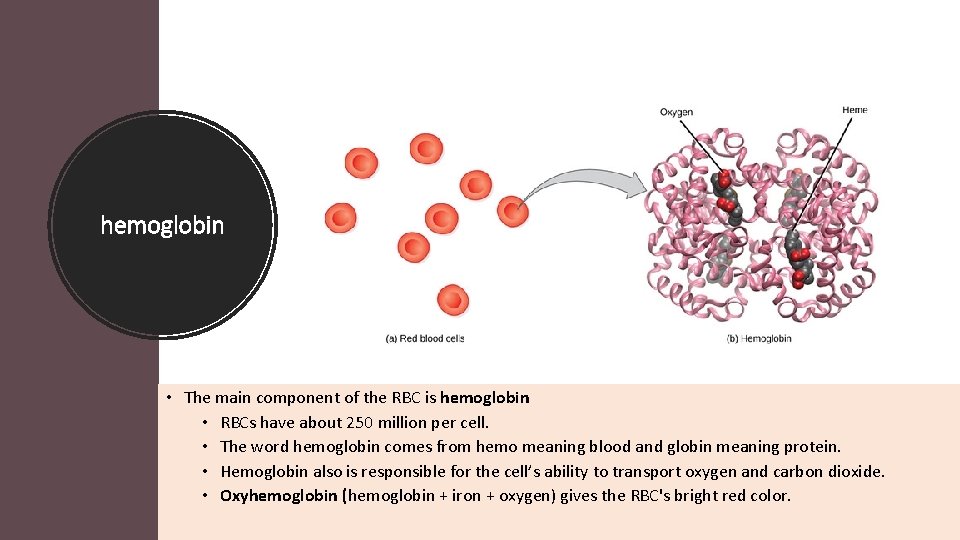
hemoglobin • The main component of the RBC is hemoglobin • RBCs have about 250 million per cell. • The word hemoglobin comes from hemo meaning blood and globin meaning protein. • Hemoglobin also is responsible for the cell’s ability to transport oxygen and carbon dioxide. • Oxyhemoglobin (hemoglobin + iron + oxygen) gives the RBC's bright red color.
The thickness of blood is called viscosity The greater the viscosity of blood, the more friction there is and more pressure is needed to force blood through.

Functions of RBCs – gas transport • The main function is the transportation of oxygen throughout the body (oxyhemoglobin) and the ability of the blood to carry out carbon dioxide which is called (carbaminohemoglobi n).
Normal p. H of blood ranges between 7. 35 -7. 45; blood is slightly Alkaline. A drop in p. H below 7. 35 is a condition is also called Acidosis. A jump in p. H higher then 7. 45 is a condition called "Alkalosis". Functions of RBCs To maintain the homeostasis (or balance, ) the blood has tiny molecules within the RBC that help prevent drops or increases from happening.

Red blood cells are broken down and hemoglobin is released. The globin part of the hemoglobin is broken down into amino acid components, which in turn are recycled by the body. Destruction of RBCs The iron is recovered and returned to the bone marrow to be reused. The heme portion of the molecule experiences a chemical change and then gets excreted as bile pigment (bilirubin) by the liver. Heme portion after being broken down contributes to the color of feces and your skin color changing after being bruised.
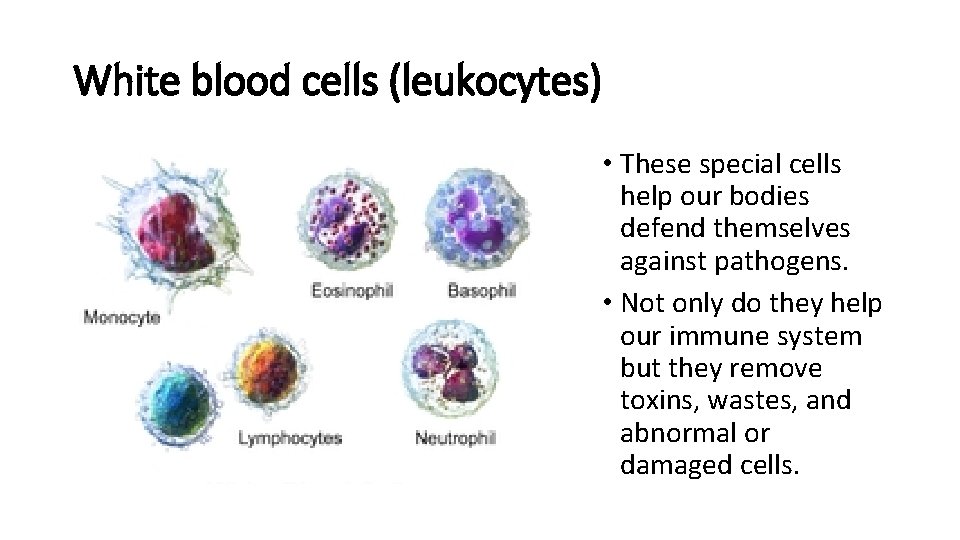
White blood cells (leukocytes) • These special cells help our bodies defend themselves against pathogens. • Not only do they help our immune system but they remove toxins, wastes, and abnormal or damaged cells.
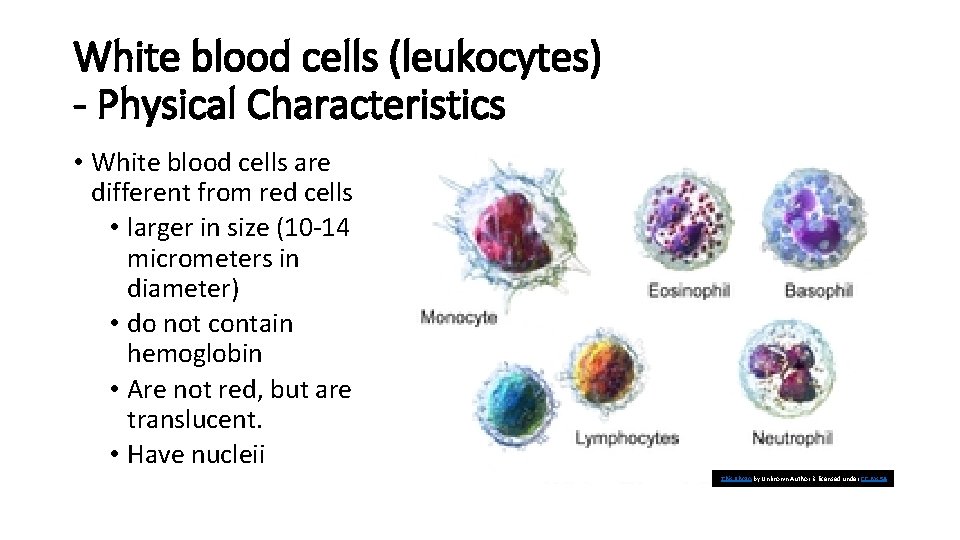
White blood cells (leukocytes) - Physical Characteristics • White blood cells are different from red cells • larger in size (10 -14 micrometers in diameter) • do not contain hemoglobin • Are not red, but are translucent. • Have nucleii This Photo by Unknown Author is licensed under CC BY-SA

White Blood Cells - Granular vs Agranular • The Granular phenotype are able to stain blue. • The Agranular phenotype are able to stain red. • Granular Cells - • Neutrophils make up 50 -70% of Granular cells • Eosinophils make up 2 -4%, • Basophils 0 -1%. • Agranular Cells - • Monocytes make up 2 -8% of Agranular cells. • B and T Lymphocytes make up 2030%.
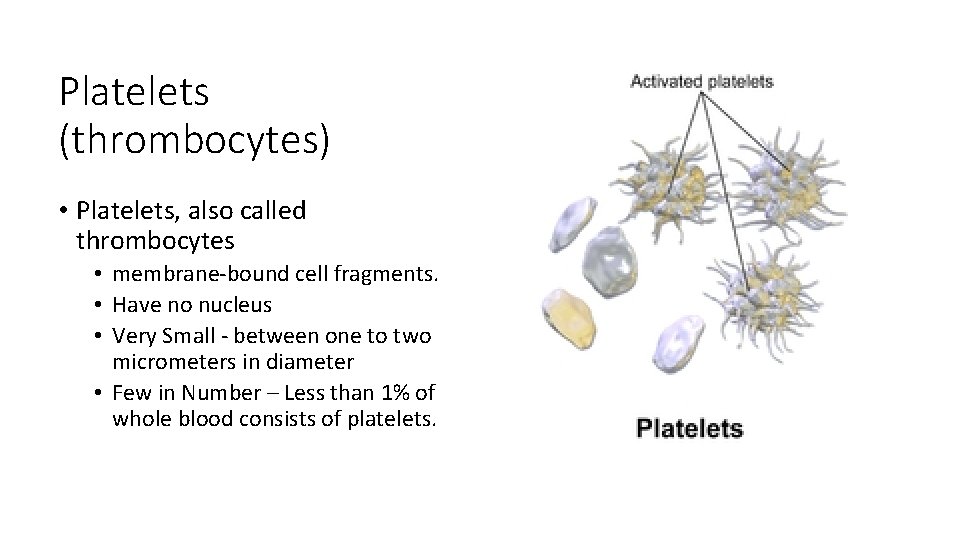
Platelets (thrombocytes) • Platelets, also called thrombocytes • membrane-bound cell fragments. • Have no nucleus • Very Small - between one to two micrometers in diameter • Few in Number – Less than 1% of whole blood consists of platelets.
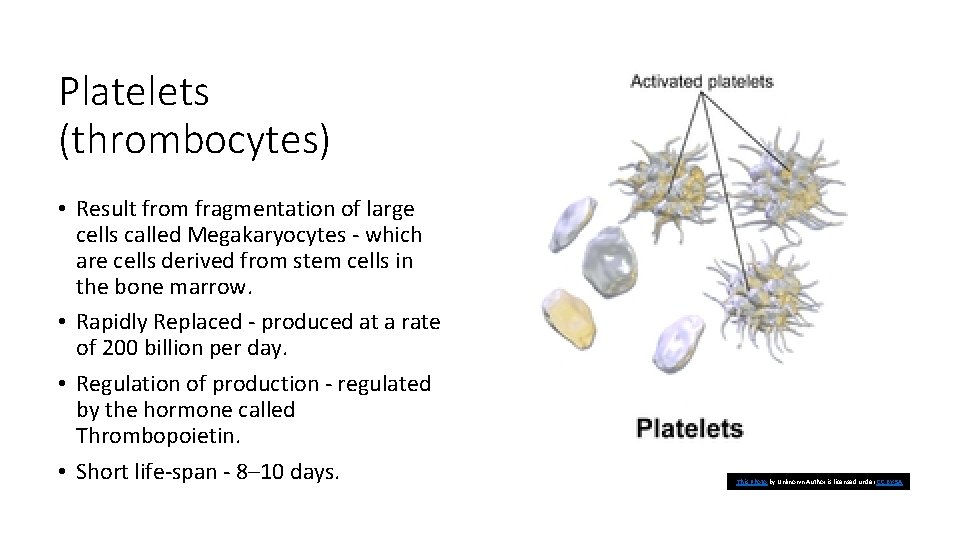
Platelets (thrombocytes) • Result from fragmentation of large cells called Megakaryocytes - which are cells derived from stem cells in the bone marrow. • Rapidly Replaced - produced at a rate of 200 billion per day. • Regulation of production - regulated by the hormone called Thrombopoietin. • Short life-span - 8– 10 days. This Photo by Unknown Author is licensed under CC BY-SA

FUNCTION TO CLOT BLOOD Platelets (thrombocytes) • The sticky surface of the platelets allow them to accumulate at the site of broken blood vessels to form a clot. • This aids in the process of hemostasis ("blood stopping"). Platelets secrete factors that… • Increase local platelet aggregation - thromboxane A • Enhance vasoconstriction - serotonin • Promote blood coagulation - thromboplastin

(1) vascular spasm, vasoconstriction, or intense contraction of blood vessels Hemostasis (Coagulation or Clotting) – 3 stages (2) formation of a platelet plug (3) blood clotting or coagulation.
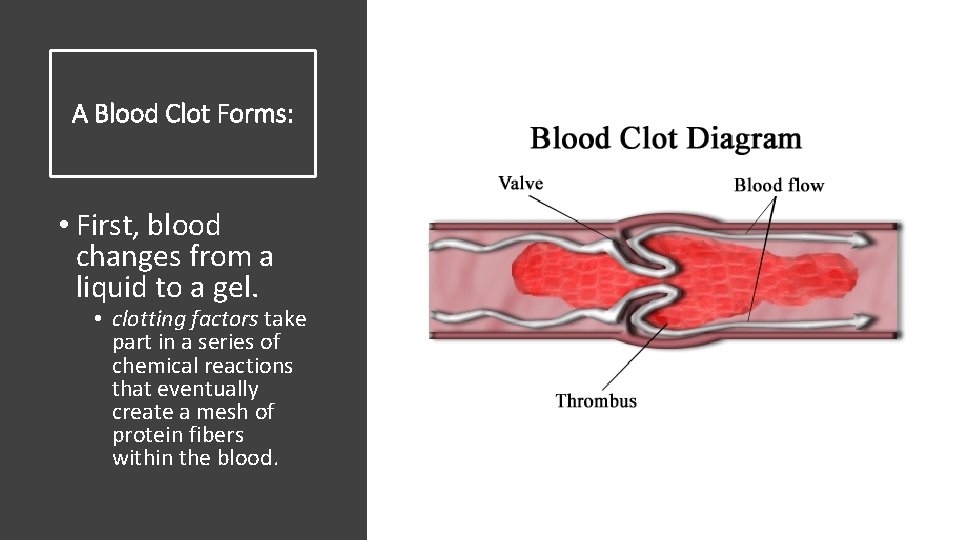
A Blood Clot Forms: • First, blood changes from a liquid to a gel. • clotting factors take part in a series of chemical reactions that eventually create a mesh of protein fibers within the blood.
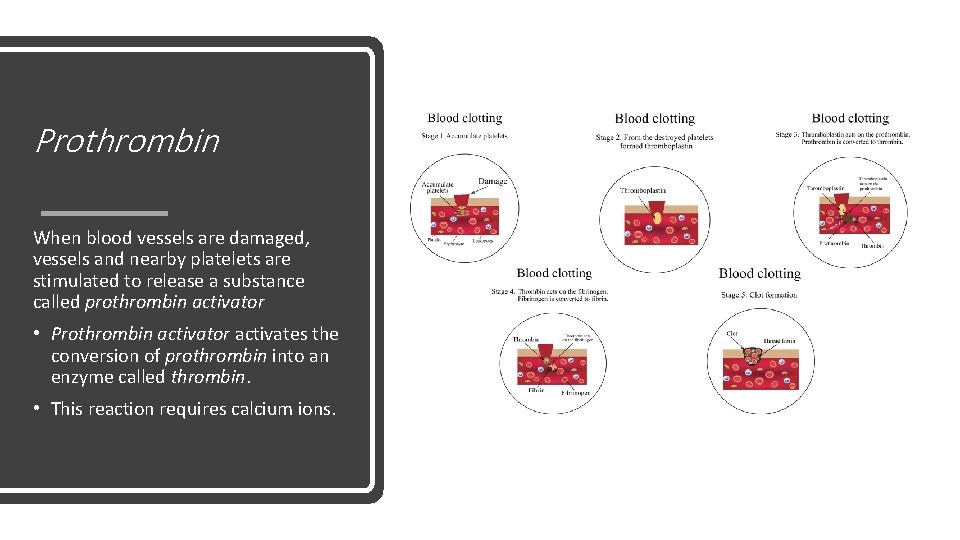
Prothrombin When blood vessels are damaged, vessels and nearby platelets are stimulated to release a substance called prothrombin activator • Prothrombin activator activates the conversion of prothrombin into an enzyme called thrombin. • This reaction requires calcium ions.
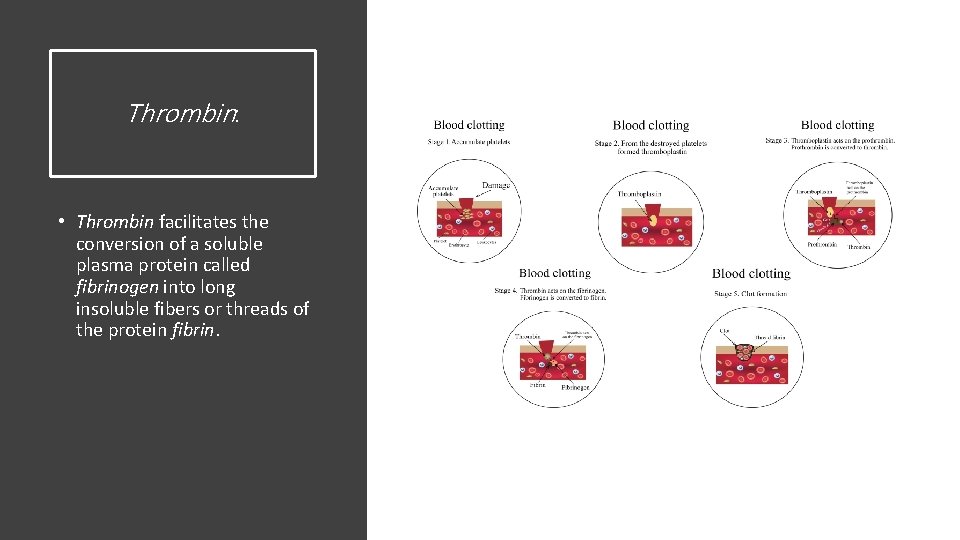
Thrombin: • Thrombin facilitates the conversion of a soluble plasma protein called fibrinogen into long insoluble fibers or threads of the protein fibrin.
Fibrin: • Fibrinogen is cleaved by thrombin to form its active form, "fibrin. " • Fibrin threads wind around the platelet plug at the damaged area of the blood vessel, forming an interlocking network of fibers and a framework for the clot. • This net of fibers traps and helps hold platelets, blood cells and other molecules tight to the site of injury, functioning as the initial clot. • This temporary fibrin clot can form in less than a minute, and usually does a good job of reducing the blood flow. • Next, platelets in the clot begin to shrink, tightening the clot and drawing together the vessel walls.
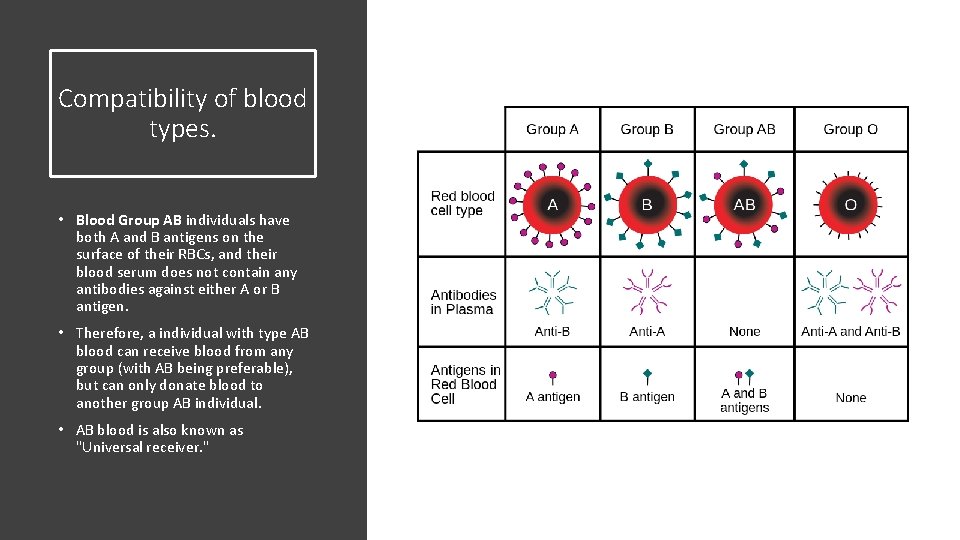
Compatibility of blood types. • Blood Group AB individuals have both A and B antigens on the surface of their RBCs, and their blood serum does not contain any antibodies against either A or B antigen. • Therefore, a individual with type AB blood can receive blood from any group (with AB being preferable), but can only donate blood to another group AB individual. • AB blood is also known as "Universal receiver. "
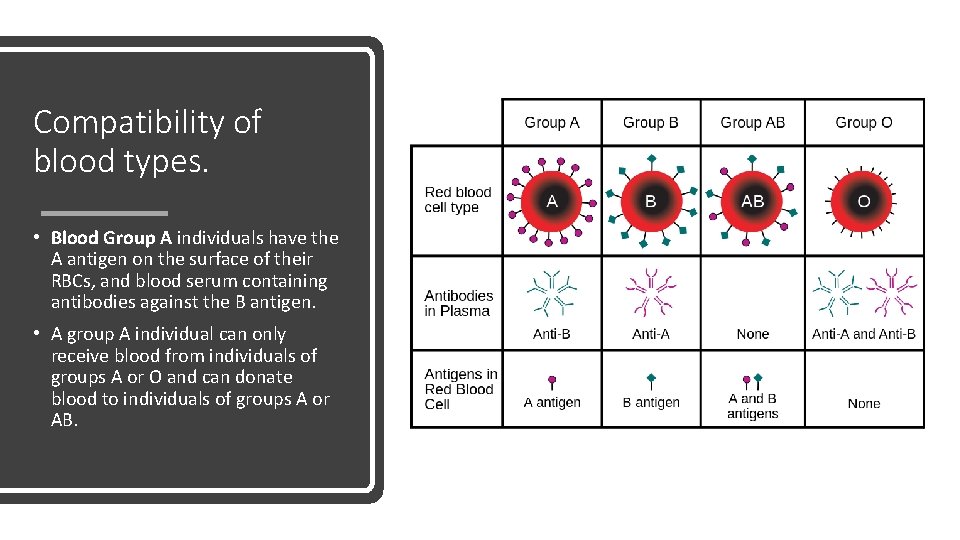
Compatibility of blood types. • Blood Group A individuals have the A antigen on the surface of their RBCs, and blood serum containing antibodies against the B antigen. • A group A individual can only receive blood from individuals of groups A or O and can donate blood to individuals of groups A or AB.
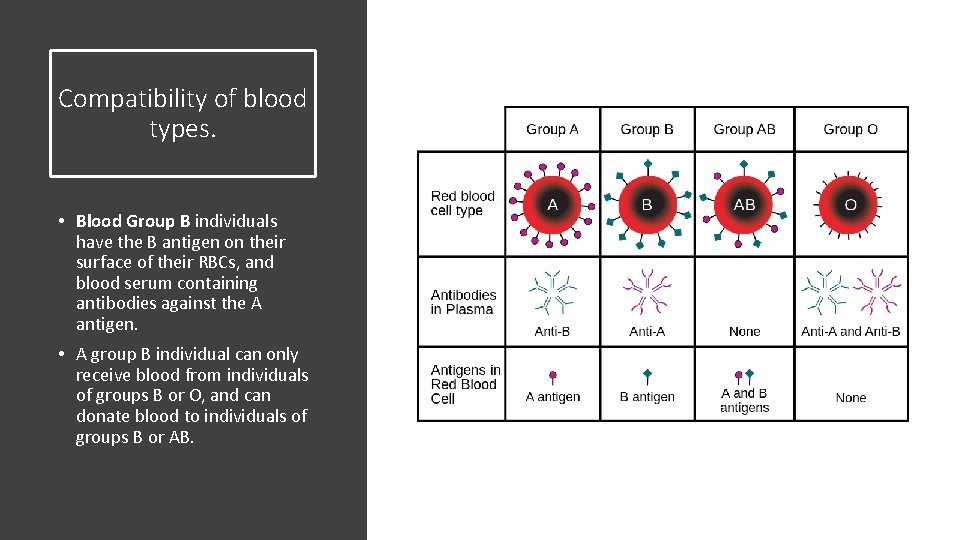
Compatibility of blood types. • Blood Group B individuals have the B antigen on their surface of their RBCs, and blood serum containing antibodies against the A antigen. • A group B individual can only receive blood from individuals of groups B or O, and can donate blood to individuals of groups B or AB.
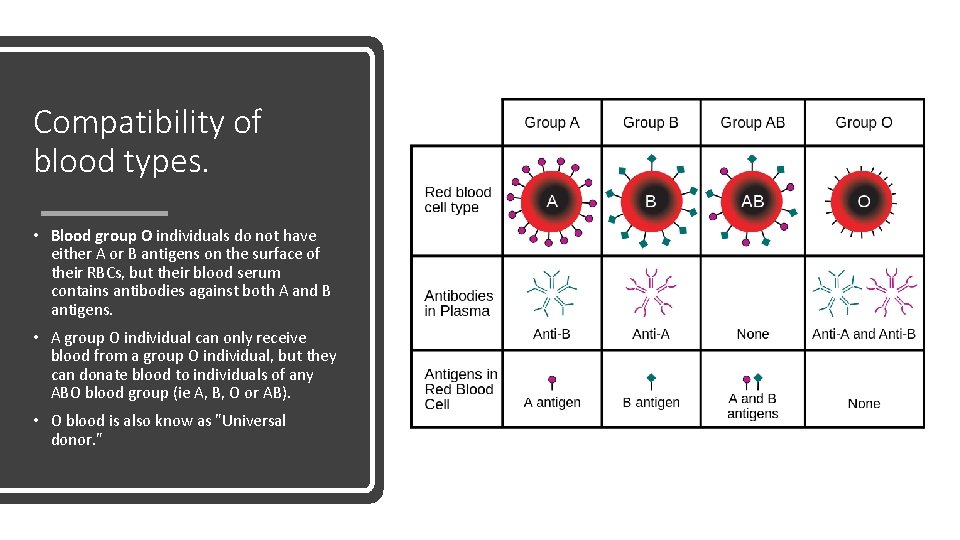
Compatibility of blood types. • Blood group O individuals do not have either A or B antigens on the surface of their RBCs, but their blood serum contains antibodies against both A and B antigens. • A group O individual can only receive blood from a group O individual, but they can donate blood to individuals of any ABO blood group (ie A, B, O or AB). • O blood is also know as "Universal donor. "
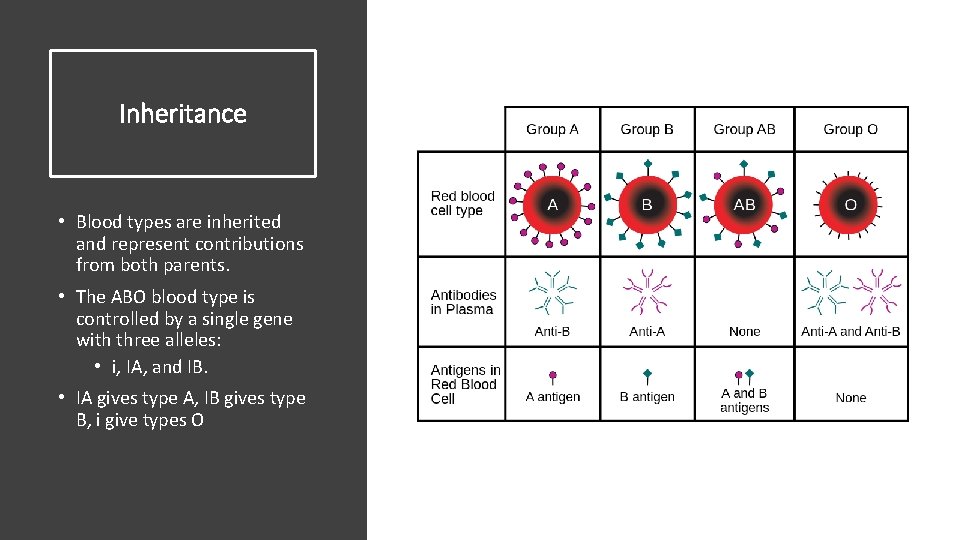
Inheritance • Blood types are inherited and represent contributions from both parents. • The ABO blood type is controlled by a single gene with three alleles: • i, IA, and IB. • IA gives type A, IB gives type B, i give types O

Compatibility in Blood/Plasma Transfusions An O donor you can't give type O plasma to a type A, B or AB, because a person with type O blood has A and B antibodies and the recipient would have an immune response. An AB donor could give plasma to anyone, since they have no antibodies.
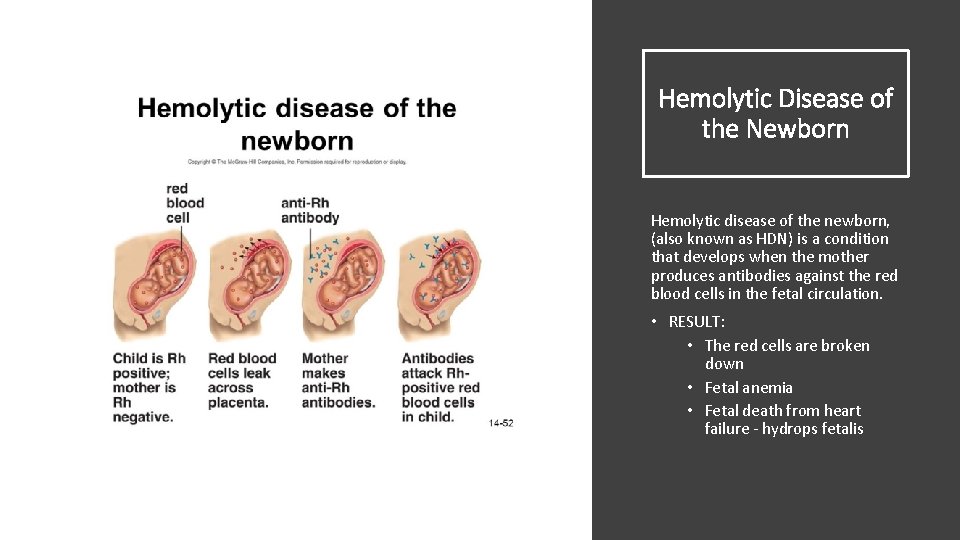
Hemolytic Disease of the Newborn Hemolytic disease of the newborn, (also known as HDN) is a condition that develops when the mother produces antibodies against the red blood cells in the fetal circulation. • RESULT: • The red cells are broken down • Fetal anemia • Fetal death from heart failure - hydrops fetalis
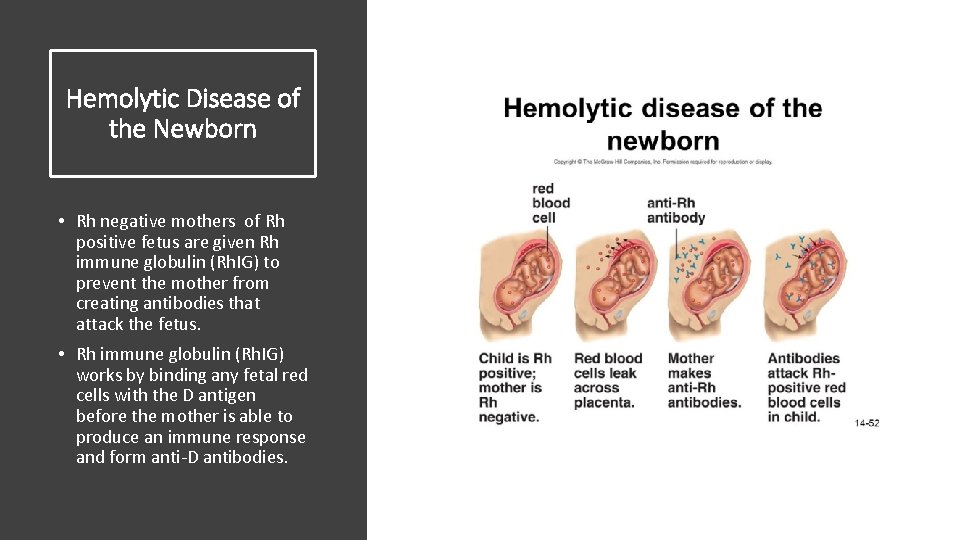
Hemolytic Disease of the Newborn • Rh negative mothers of Rh positive fetus are given Rh immune globulin (Rh. IG) to prevent the mother from creating antibodies that attack the fetus. • Rh immune globulin (Rh. IG) works by binding any fetal red cells with the D antigen before the mother is able to produce an immune response and form anti-D antibodies.
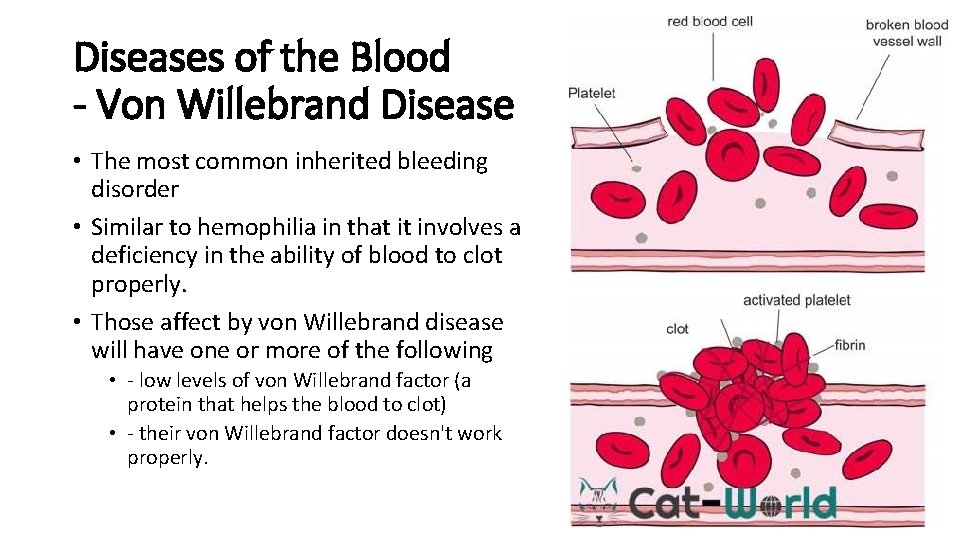
Diseases of the Blood - Von Willebrand Disease • The most common inherited bleeding disorder • Similar to hemophilia in that it involves a deficiency in the ability of blood to clot properly. • Those affect by von Willebrand disease will have one or more of the following • - low levels of von Willebrand factor (a protein that helps the blood to clot) • - their von Willebrand factor doesn't work properly.
• Disseminated intravascular coagulation (DIC), also called consumptive coagulopathy, is a pathological process in the body where the blood starts to coagulate throughout the whole body. • This depletes the body of its platelets and coagulation factors, and there is a paradoxically increased risk of hemorrhage. Diseases of the Blood - Disseminated Intravascular Coagulation • It occurs in critically ill patients, especially those with Gramnegative sepsis (particularly meningococcal sepsis) and acute promyelocytic leukemia.
• low or no blood protein • inability to produce blood clots Diseases of the Blood - Hemophilia • There are two types of Hemophilia: • Type A, which is a deficiency in factor VIII • Type B, (Christmas disease) a deficiency on factor IX. Because people with hemophilia do not have the ability to make blood clots, even a little cut may kill them, or the smallest bump or jar to the body could cause severe bruising that doesn't get better for months.
Diseases of the Blood - Factor V Leiden • The opposite of Hemophilia • a variant of human factor V causes a hypercoagulability • the most common hereditary hypercoagulability disorder • Causes a slightly higher risk of developing blood clots • Those that test positive for factor V should avoid (oral contraceptives, obesity, smoking, and high blood pressure. )
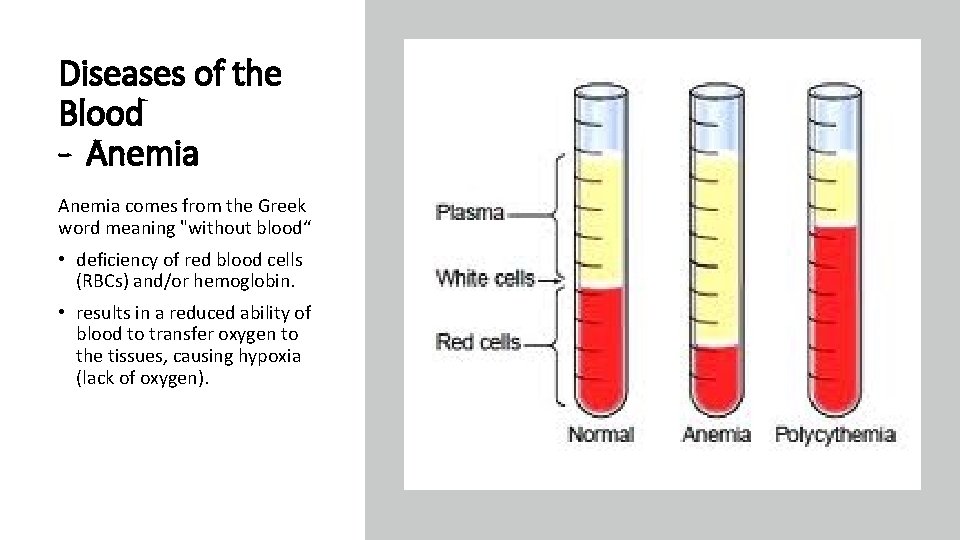
Diseases of the Blood - Anemia comes from the Greek word meaning "without blood“ • deficiency of red blood cells (RBCs) and/or hemoglobin. • results in a reduced ability of blood to transfer oxygen to the tissues, causing hypoxia (lack of oxygen).
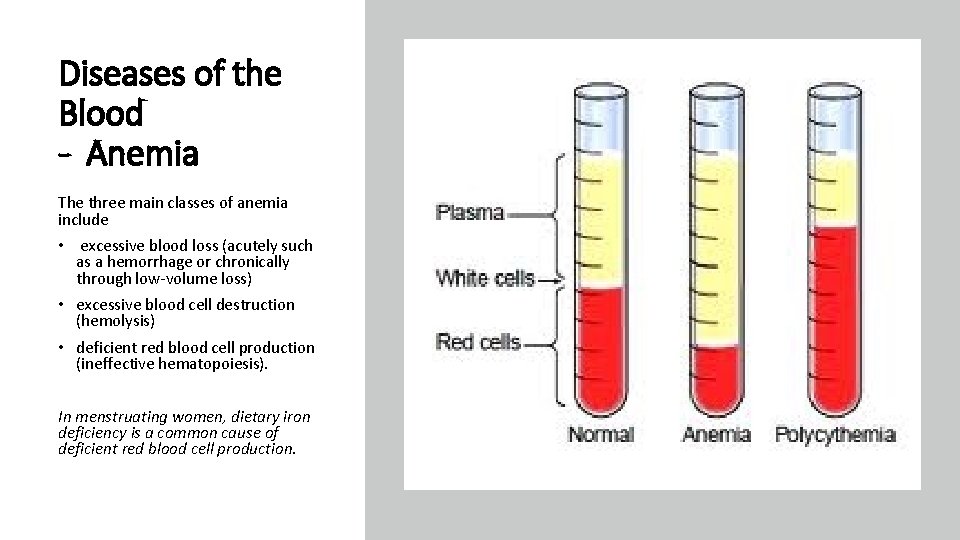
Diseases of the Blood - Anemia The three main classes of anemia include • excessive blood loss (acutely such as a hemorrhage or chronically through low-volume loss) • excessive blood cell destruction (hemolysis) • deficient red blood cell production (ineffective hematopoiesis). In menstruating women, dietary iron deficiency is a common cause of deficient red blood cell production.
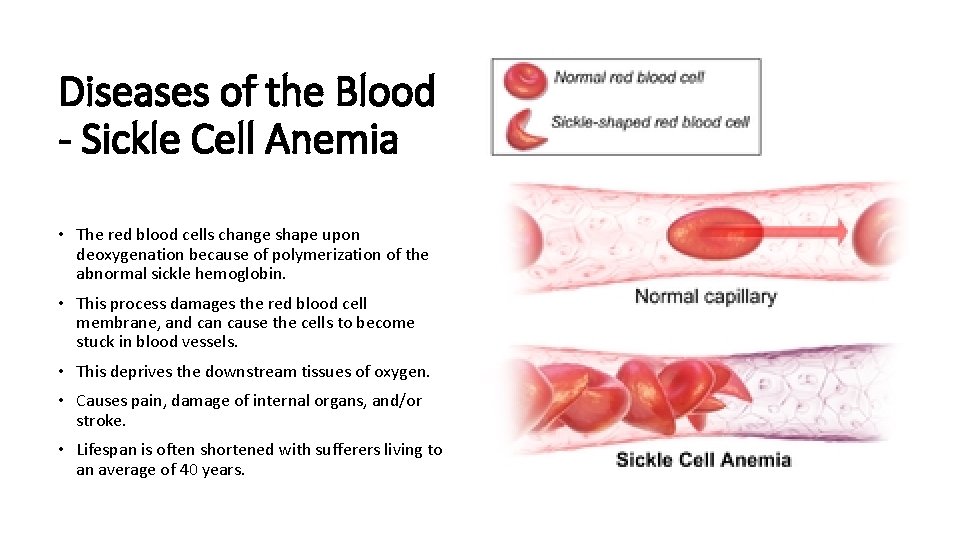
Diseases of the Blood - Sickle Cell Anemia • The red blood cells change shape upon deoxygenation because of polymerization of the abnormal sickle hemoglobin. • This process damages the red blood cell membrane, and can cause the cells to become stuck in blood vessels. • This deprives the downstream tissues of oxygen. • Causes pain, damage of internal organs, and/or stroke. • Lifespan is often shortened with sufferers living to an average of 40 years.
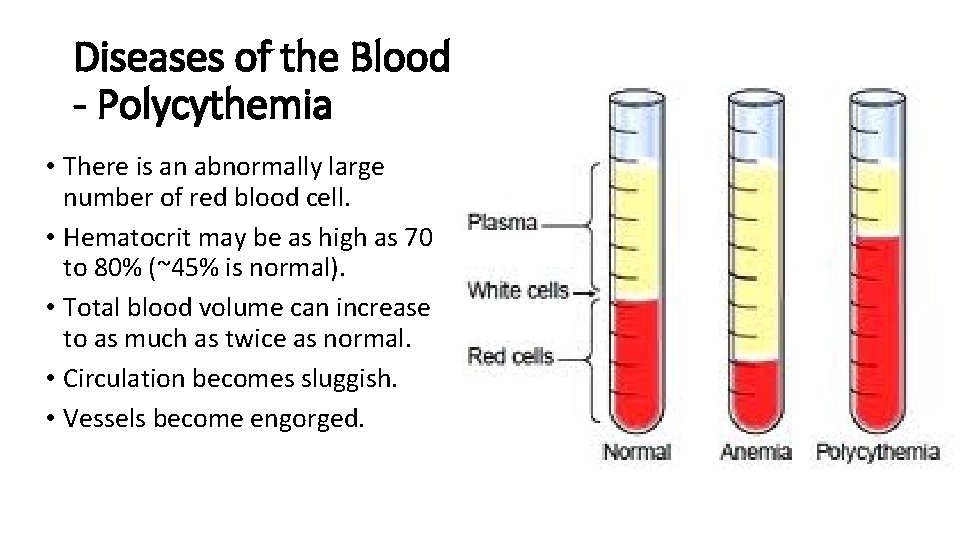
Diseases of the Blood - Polycythemia • There is an abnormally large number of red blood cell. • Hematocrit may be as high as 70 to 80% (~45% is normal). • Total blood volume can increase to as much as twice as normal. • Circulation becomes sluggish. • Vessels become engorged.
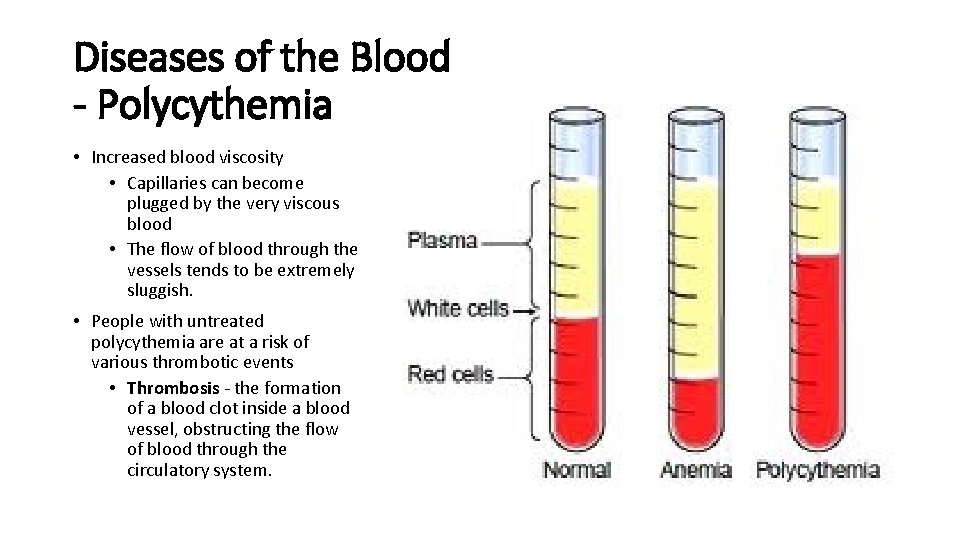
Diseases of the Blood - Polycythemia • Increased blood viscosity • Capillaries can become plugged by the very viscous blood • The flow of blood through the vessels tends to be extremely sluggish. • People with untreated polycythemia are at a risk of various thrombotic events • Thrombosis - the formation of a blood clot inside a blood vessel, obstructing the flow of blood through the circulatory system.
- Slides: 79