Blood Flow and Blood Pressure Cardiovascular System Functions

Blood Flow and Blood Pressure

Cardiovascular System Functions Heart, blood vessels, and blood work to transport § Oxygen and nutrients to cells § Wastes from cells to liver and kidneys § Hormones, immune cells, and clotting proteins to specific target cells § Maintain pressure in vessels so blood will flow to organs and tissues
Blood Vessels heart arteries arterioles capillaries venules veins § Arteries—relatively large, main vessels that conduct blood away from the heart § Arterioles—small branching vessels in peripheral tissues that decrease in diameter (increase in resistance) § Capillaries—where diffusion takes place between blood and interstitial fluid (ECF; 3 rd space) § Venules—collect blood from capillaries § Veins—return blood to heart
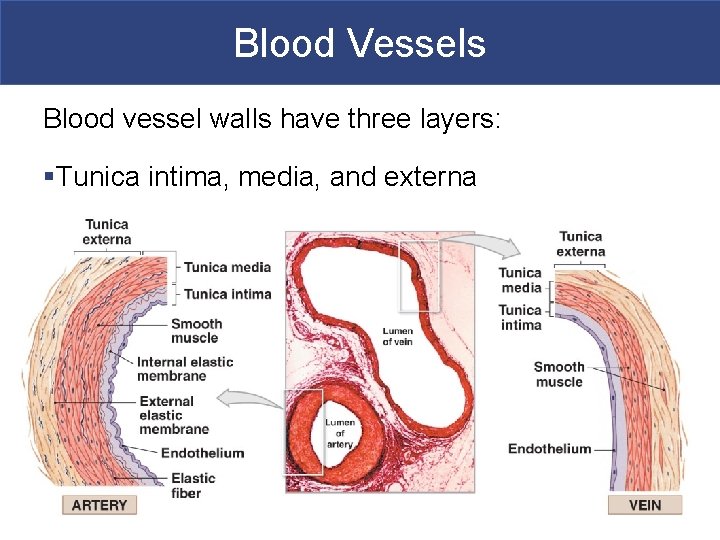
Blood Vessels Blood vessel walls have three layers: §Tunica intima, media, and externa

Capillary Fluid Exchange § Fluid circulates between capillary blood and interstitium to move nutrients into the interstitial fluid (ISF) for cell use and wastes out of the ISF for removal by blood § Fluid movement occurs via osmosis (not transport) through openings between adjacent endothelial cells § Fluid movement in to interstitium is driven by hydrostatic pressure § Fluid movement into blood is driven by osmotic pressure (oncotic pressure)

Capillary Filtration (movement of fluid in to interstitium) § Driven by hydrostatic pressure (pressure in the vessel/ MAP) § Water and small solutes forced through gaps between endothelial cells § Leaves larger solutes (glucose + albumins) in bloodstream
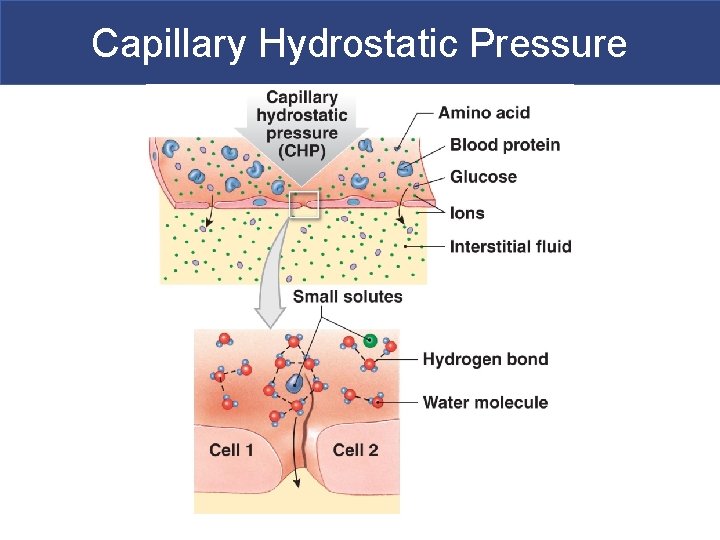
Capillary Hydrostatic Pressure

Capillary Reabsorption (movement of fluid back into capillary) § Driven by blood colloid osmotic pressure § Slightly higher colloid osmotic pressure in blood (68%) vs. interstitium due to suspended blood proteins (albumin) that are too large to cross capillary walls
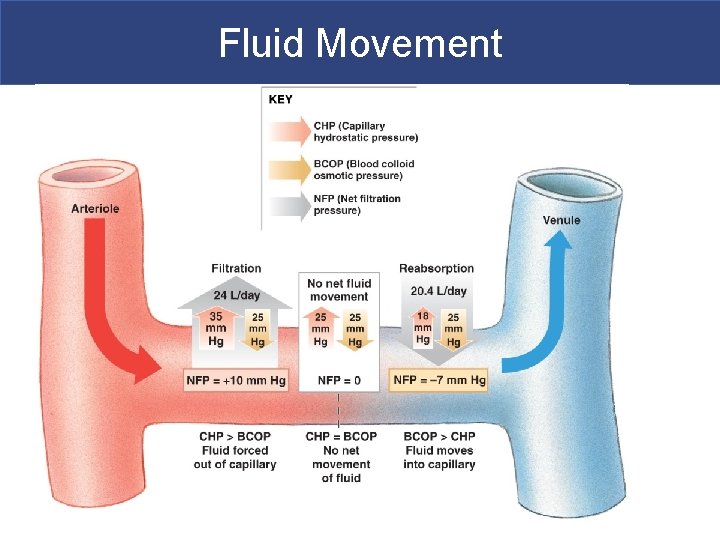
Fluid Movement

Capillary Exchange of Fluid § Capillary Exchange § At arterial end of capillary § Fluid moves into interstitial fluid because hydrostatic pressure is higher than blood colloid osmotic pressure § At venous end of capillary § Fluid moves out of interstitial fluid because hydrostatic pressure is less than blood colloid osmotic pressure § capillary fluid movement animation

Fluid Recycling § Capillaries filter more out (24 L/day) than they reabsorb (20 L/day) § Excess fluid enters lymphatic vessels § Ensure constant plasma and interstitial fluid communication § Accelerate distribution of nutrients, hormones, and dissolved gases through tissues § Transport insoluble lipids and tissue proteins that cannot cross capillary walls § Flush bacterial toxins and chemicals to immune system tissues

Capillary Dynamics § When does CHP and reabsorption? and how does that affect filtration § When does BCOP and reabsorption? and how does that affect filtration

Capillary Dynamics § Dehydration—lose H 2 O/decrease in blood volume, so how does that affect CHP and BCOP? § Increases BCOP and decreases CHP § Accelerates reabsorption (why? ? ) § Excess blood volume—how does that affect CHP and BCOP? § Increased CHP § Decreased BCOP § Accelerates filtration (why? ? ) resulting in edema § Hemorrhaging § Reduces CHP and NFP and this leads to increased reabsorption of interstitial fluid (recall of fluids)

Capillary Dynamics Dehydration can be caused by: § Loose water to environment so blood volume decreases § Decrease in hydrostatic pressure § Increase in plasma protein concentration

Capillary Dynamics Edema can be caused by several factors: § Increase in capillary permeability-leaky capillaries via trauma, or histamine release due to inflammation or allergic reaction § Decrease in plasma protein concentration-burns, malnutrition or cirrhosis of the liver § Increase in hydrostatic pressure-cardiac/ renal failure, obstruction of blood flow, lymphatic obstruction (breast cancer surgery), or increase in blood volume
Blood Flow Rate § The cardiovascular system is regulated to ensure blood flow through capillaries in periphery § Why? § The heart must generate enough pressure to overcome vessel resistance to keep blood flowing § How does it do this? (think CO=SV X HR)
Blood Flow Rate § Flow rate=volume of blood that flows through the systemic circuit per minute § Flow rate is dependent on pressure differences and resistance within the cardiovascular system § F= ∆ P/R § Flow rate is directly proportional to pressure difference § Flow rate is indirectly proportional resistance

Blood Flow Rate § Which body position yields more resistance to blood flow laying down or standing and why? § Flow= P/R § Lying down=resistance of blood vessels § Standing=resistance of blood vessels + gravity

Pressure Gradient (∆P) § Blood flows from high low pressure § The pressure gradient (∆P) = P at one end of a blood vessel - P at the other end of a blood vessel § The greater the difference=the faster blood flows
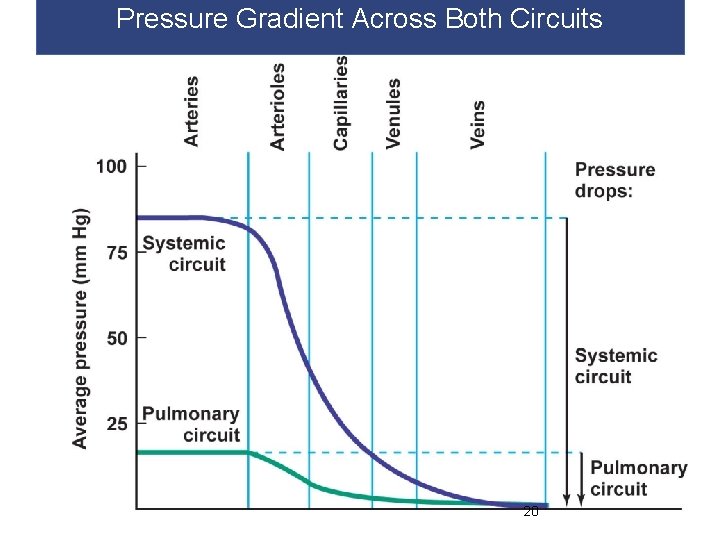
Pressure Gradient Across Both Circuits 20
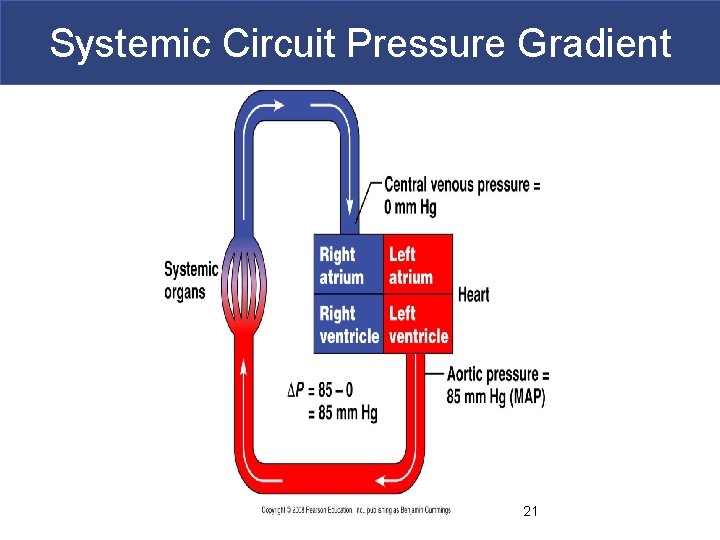
Systemic Circuit Pressure Gradient 21
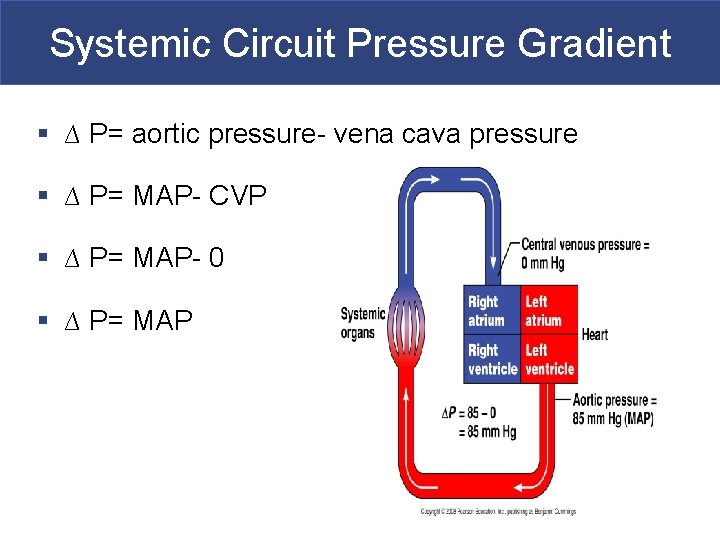
Systemic Circuit Pressure Gradient § ∆ P= aortic pressure- vena cava pressure § ∆ P= MAP- CVP § ∆ P= MAP- 0 § ∆ P= MAP

Resistance Flow through network is effected by resistance (TPR) Poiseulle’s Law R= 8 Lη/ π r 4 Flow = P/R Resistance (R) is due to: §Length of vessel (L) §Viscosity of fluid = § dependent on amount of RBC’s and plasma proteins §Internal radius of vessel (r 4) § arterioles (and small arteries) can regulate their radii
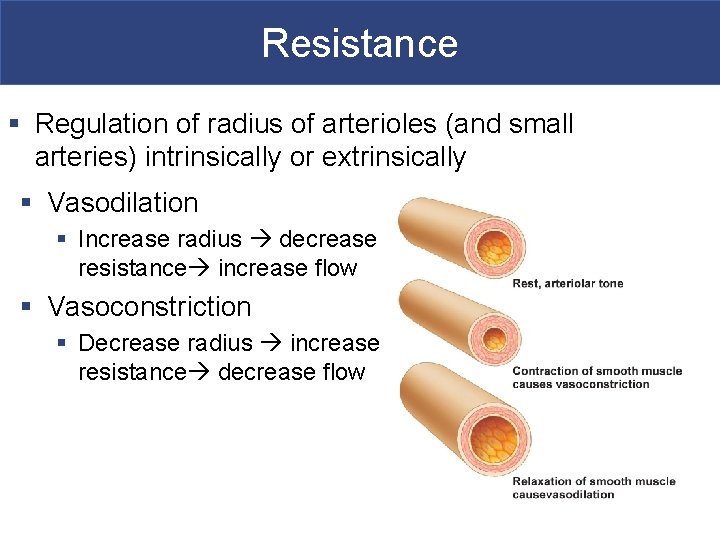
Resistance § Regulation of radius of arterioles (and small arteries) intrinsically or extrinsically § Vasodilation § Increase radius decrease resistance increase flow § Vasoconstriction § Decrease radius increase resistance decrease flow
Blood Flow Rate § Flow rate= ∆ P/R § Capillaries regulate flow rate at the tissue level intrinsically § Cardiovascular control centers regulate blood flow rate and blood pressure on a large scale (via nervous input to heart and blood vessels) extrinsically

Intrinsic Control of Arterioles § Change in metabolic activity § Usually linked to CO 2 and O 2 levels (↑ CO 2 vasodilation ↑ blood flow) § Locally secreted chemicals can promote vasoconstriction or most commonly vasodilation - inflammatory chemicals (histamine, nitric oxide) § Changes in blood flow - decreased blood flow increased metabolic wastes vasodilation increase blood flow § Stretch of arterial wall (myogenic response) - Stretch of arterial wall due to increased pressure reflex constriction
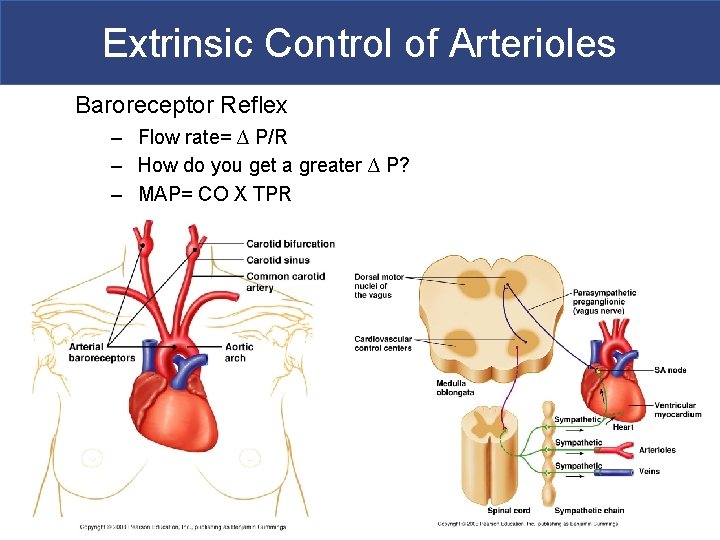
Extrinsic Control of Arterioles Baroreceptor Reflex – Flow rate= ∆ P/R – How do you get a greater ∆ P? – MAP= CO X TPR
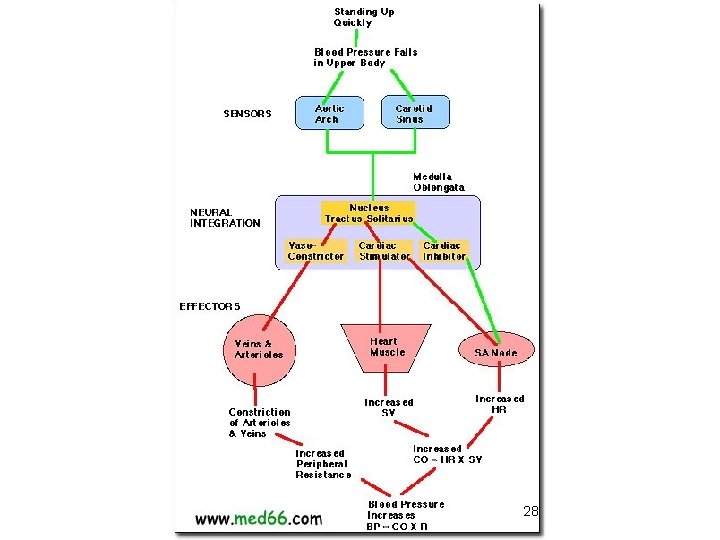
28
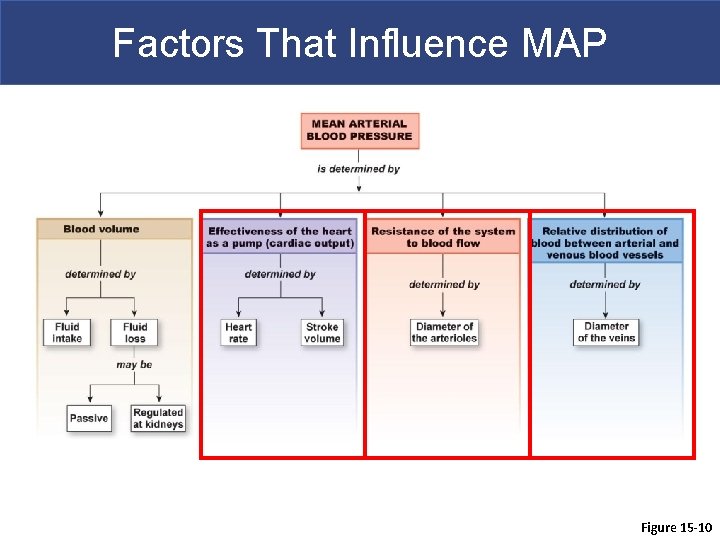
Factors That Influence MAP Figure 15 -10
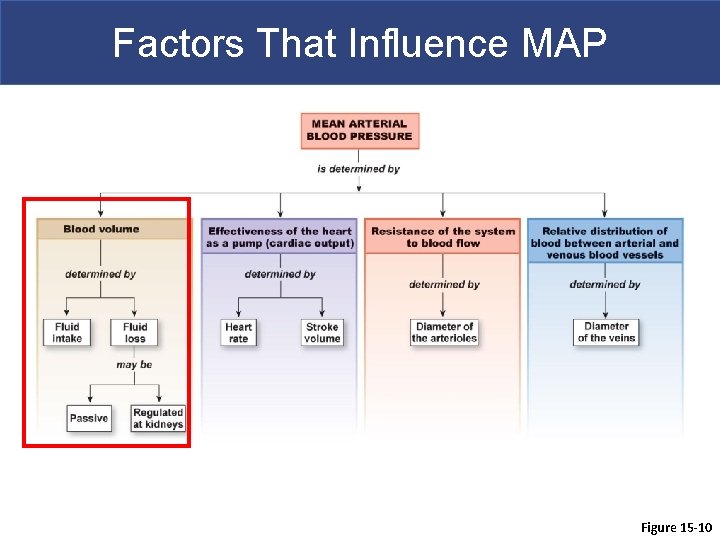
Factors That Influence MAP Figure 15 -10

Blood Pressure Regulation § Blood volume is regulated by aldosterone (when low BP) and atrial natriuretic peptide/brain natriuretic peptide (when high BP) § Blood osmolarity is regulated by kidneys via antidiuretic hormone
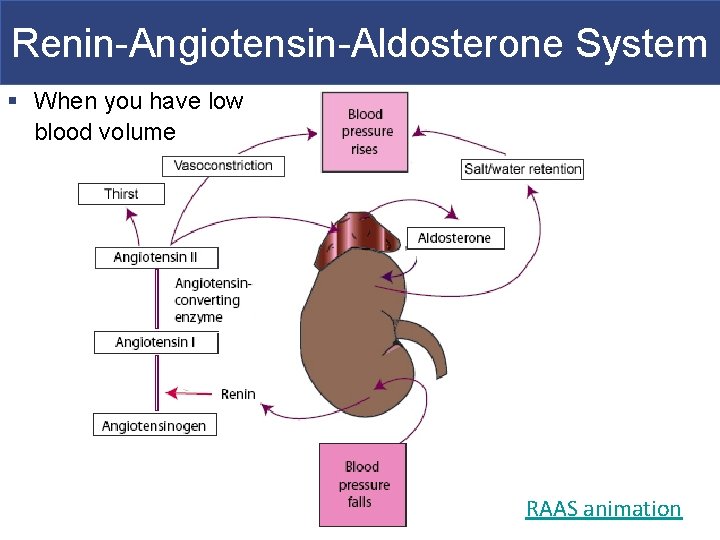
Renin-Angiotensin-Aldosterone System § When you have low blood volume RAAS animation
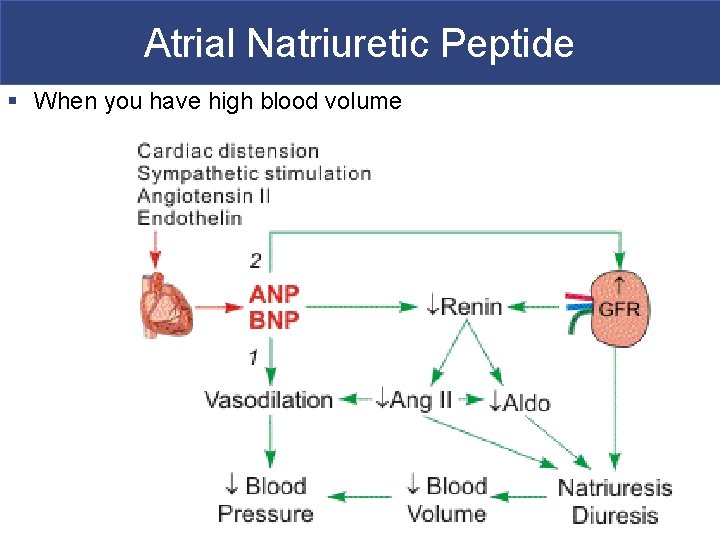
Atrial Natriuretic Peptide § When you have high blood volume
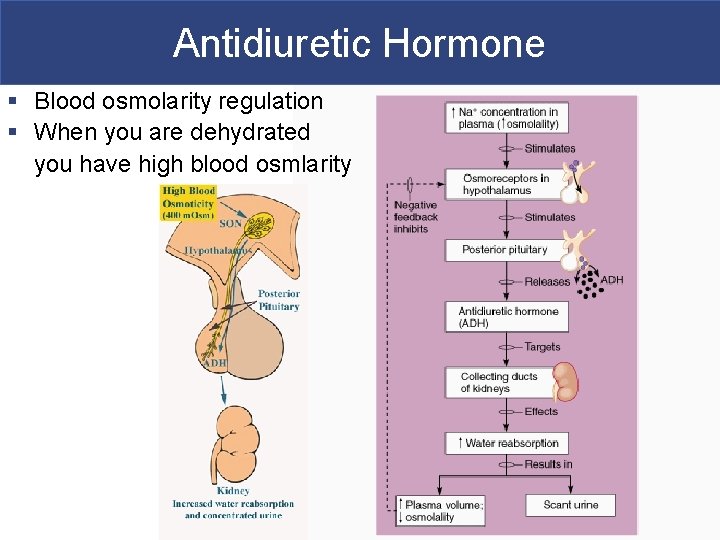
Antidiuretic Hormone § Blood osmolarity regulation § When you are dehydrated you have high blood osmlarity
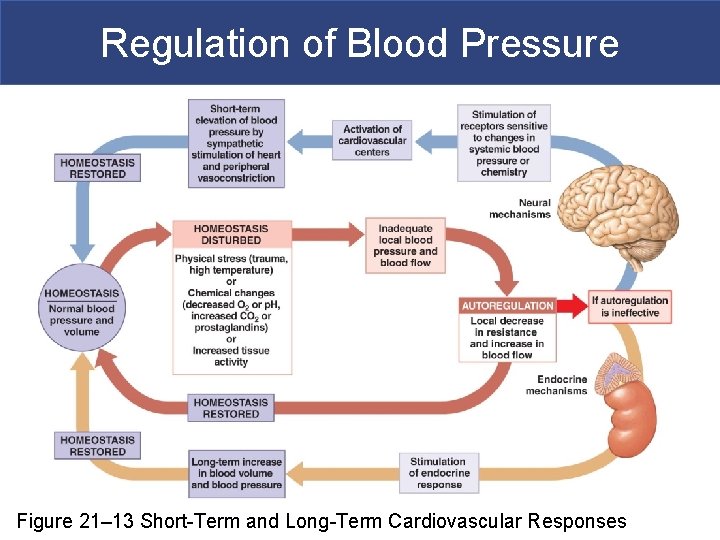
Regulation of Blood Pressure Figure 21– 13 Short-Term and Long-Term Cardiovascular Responses
- Slides: 35