Blood Dr Anderson GCIT Components of Blood Functions
Blood Dr. Anderson GCIT

Components of Blood • Functions • Distribution of materials to the tissues in the body • • o 2/co 2 transport hormones nutrients metabolic wastes • Regulation • • solute concentration body temperature p. H Balance Fluid volume (water concentration) • Protection • clotting • immune response
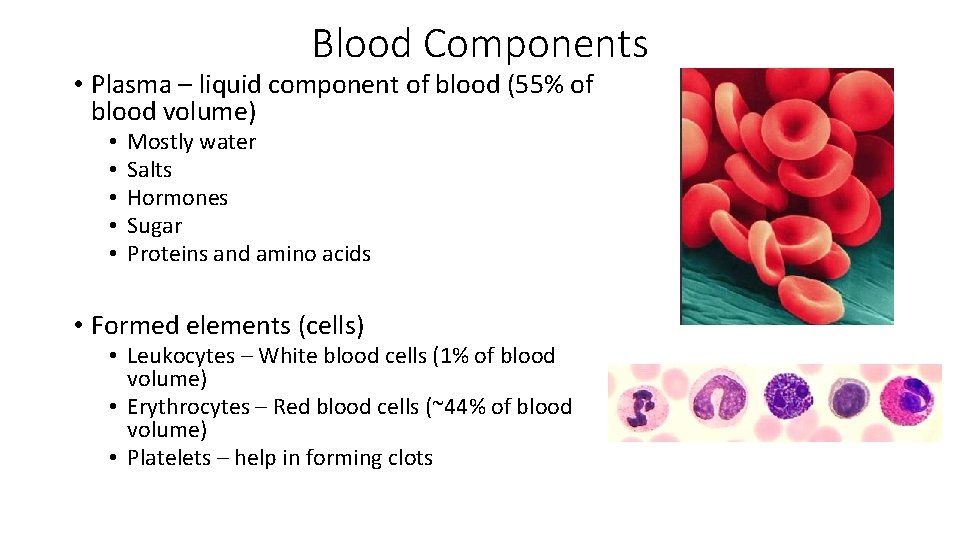
Blood Components • Plasma – liquid component of blood (55% of blood volume) • • • Mostly water Salts Hormones Sugar Proteins and amino acids • Formed elements (cells) • Leukocytes – White blood cells (1% of blood volume) • Erythrocytes – Red blood cells (~44% of blood volume) • Platelets – help in forming clots

Plasma • 90% water • Solutes • • Proteins – transport proteins (chaperones) Enzymes Antibodies Fibrinogen (forms fibrin to clot blood after injury) • The proper chemical balance of plasma is essential for tissue function! • Examples?
Metabolites in Plasma • Cellular Metabolites (Nitrogen containing compounds) • Urea, uric acid, creatine, ammonia (NH 3) • Electrolytes • Cations – Na+, K+, Mg+, Ca+ • Anions – Cl-, PO 4 -, SO 4 -, CO 3 - • Respiratory Gases • CO 2, O 2

Formed Elements • Erythrocytes – Red Blood Cells (RBC’s) • • Biconcave cells NO Nucleus! Mostly composed of hemoglobin molecules They do NOT use O 2 for respiration (use anaerobic respiration instead) • Why are all of these things adaptive? ?
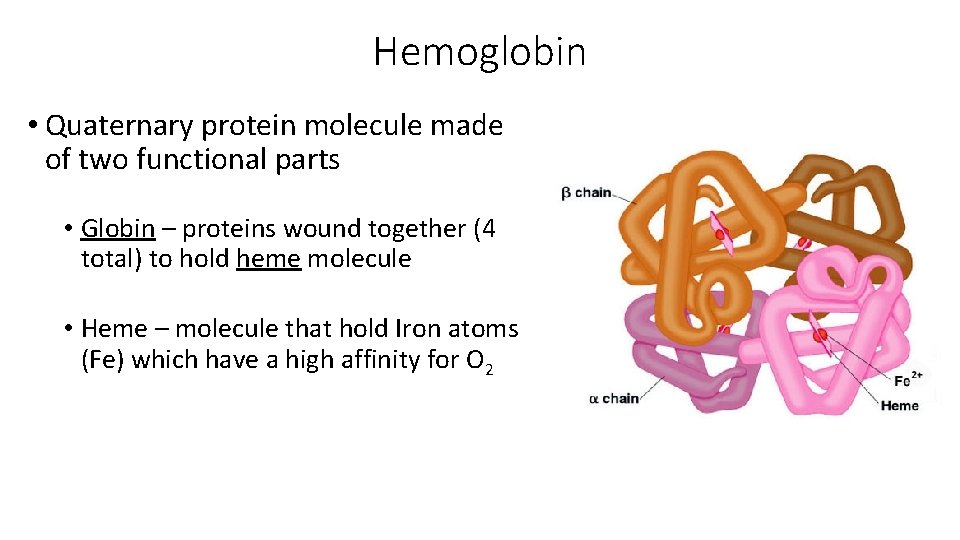
Hemoglobin • Quaternary protein molecule made of two functional parts • Globin – proteins wound together (4 total) to hold heme molecule • Heme – molecule that hold Iron atoms (Fe) which have a high affinity for O 2

Sickle Cell Anemia • In sickle-cell anemia, globin proteins are not formed correctly, making O 2 transport difficult • Low O 2 content changes the cell to be sickle-shaped (no longer biconcave) • This causes “traffic jams” in the bloodstream, leading to clots
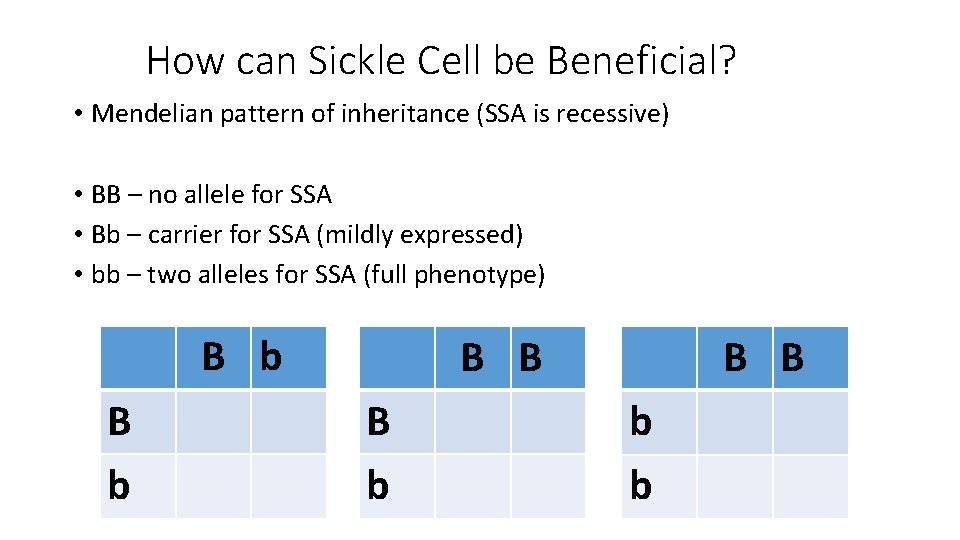
How can Sickle Cell be Beneficial? • Mendelian pattern of inheritance (SSA is recessive) • BB – no allele for SSA • Bb – carrier for SSA (mildly expressed) • bb – two alleles for SSA (full phenotype) B b B B B b b
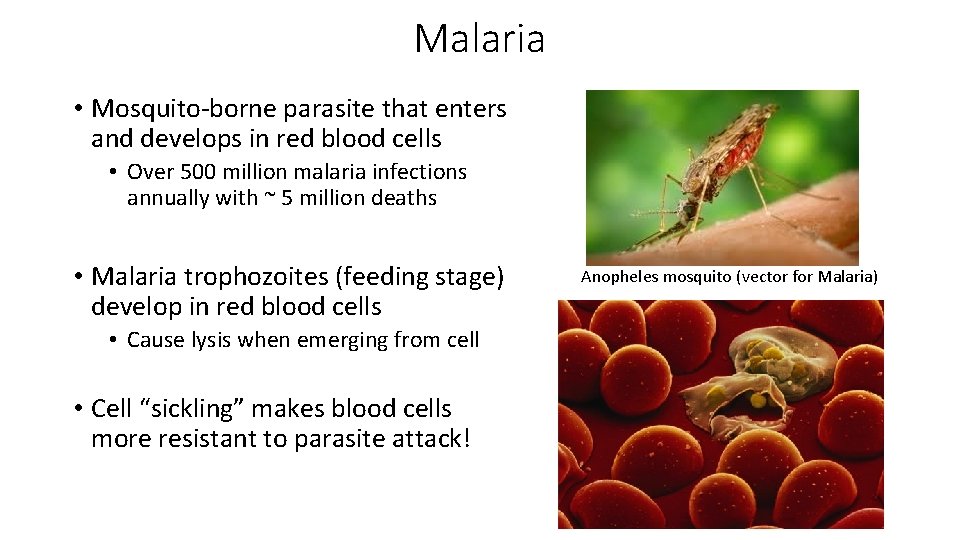
Malaria • Mosquito-borne parasite that enters and develops in red blood cells • Over 500 million malaria infections annually with ~ 5 million deaths • Malaria trophozoites (feeding stage) develop in red blood cells • Cause lysis when emerging from cell • Cell “sickling” makes blood cells more resistant to parasite attack! Anopheles mosquito (vector for Malaria)
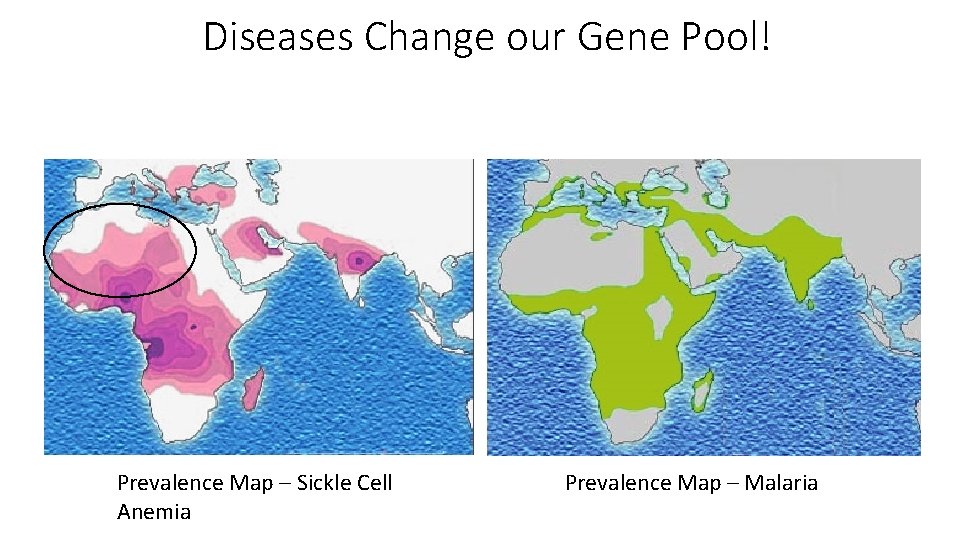
Diseases Change our Gene Pool! Prevalence Map – Sickle Cell Anemia Prevalence Map – Malaria

Will we lose our appendix through evolutionand why?

Anemia • A decrease in the capacity of the blood to carry oxygen to the tissues • Leads to general fatigue and malaise • Increased cardiac output • What factors can cause anemia? 1. Lack of Iron (nutrition) 2. Hemoglobin production (nutrition) 3. Hemorrhage/ disease

Leukocytes • Specifically engage different invaders of the body (pathogen types) • Divided into granulocytes and agranulocytes due to their appearance under the microscope • Granulocytes – many stained organelles giving them a “grainy” appearance • Agranulocytes – few or no organelles

Specific Jobs of Leukocytes Granulocytes • Basophils – produce histamine leading to inflammatory response • Rarest population • Neutrophils – phagocytose bacteria and viruses • 3 -6 nuclear lobes • Eosinophils – lead attack against parasitic worms • Bilobed nucleus • Also phagocytose bacteria

Specific Jobs of Leukocytes - Lymphocytes • Lymphocytes – produce antibodies against specific invaders • B lymphocytes – produce antibodies to pathogens • T lymphocytes • produce cytokines that direct immune response • Destroy infected cells • These cells are the heart of adaptive immunity, as they and their clones will “remember” the antibodies they produced

Specific Jobs of Leukocytes - Monocytes • Monocytes – function to phagocytose bacteria and other invading pathogens • Will mature into macrophages which can leave the blood vessels and enter tissues (diapedesis) where pathogens frequently enter
Differential Hemocyte Count • Depending on the pathogen, infection will cause changes in the proportion of WBC’s in the blood
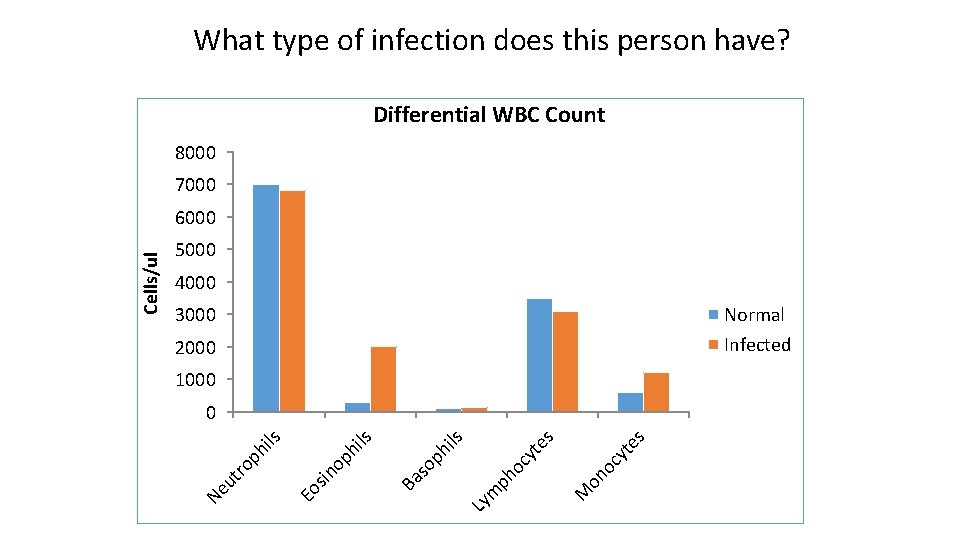
What type of infection does this person have? Differential WBC Count 8000 7000 5000 4000 3000 Normal Infected 2000 1000 es oc on M Ly m ph o cy yt te s hi ls so p Ba op sin Eo ut ro ph ils hi ls 0 Ne Cells/ul 6000
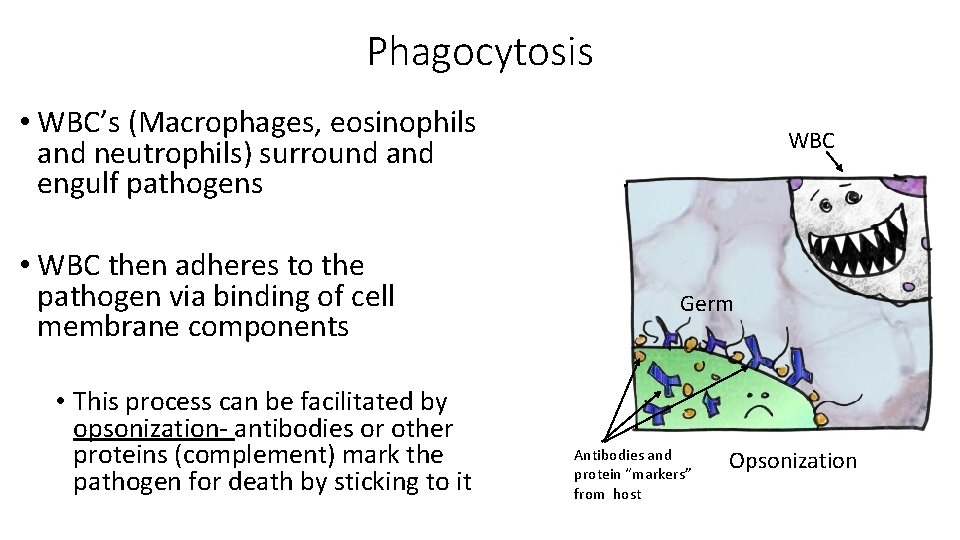
Phagocytosis • WBC’s (Macrophages, eosinophils and neutrophils) surround and engulf pathogens • WBC then adheres to the pathogen via binding of cell membrane components • This process can be facilitated by opsonization- antibodies or other proteins (complement) mark the pathogen for death by sticking to it WBC Germ Antibodies and protein “markers” from host Opsonization

Phagocytosis • Once adherence is complete, pathogens are engulfed via endocytosis, which forms a phagosome • The contents of the phagosome are then digested by merging with a lysosome (vesicle in the cell containing digestive enzymes)
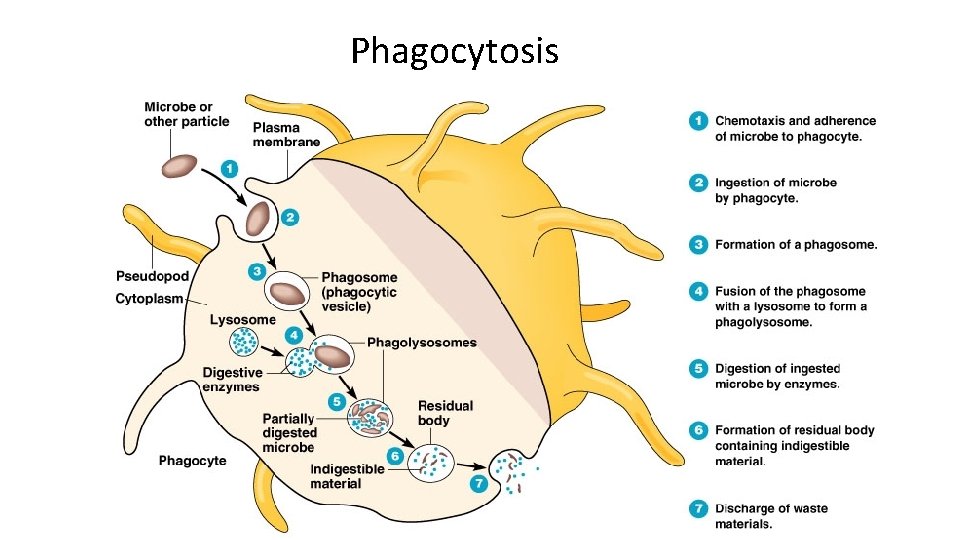
Phagocytosis
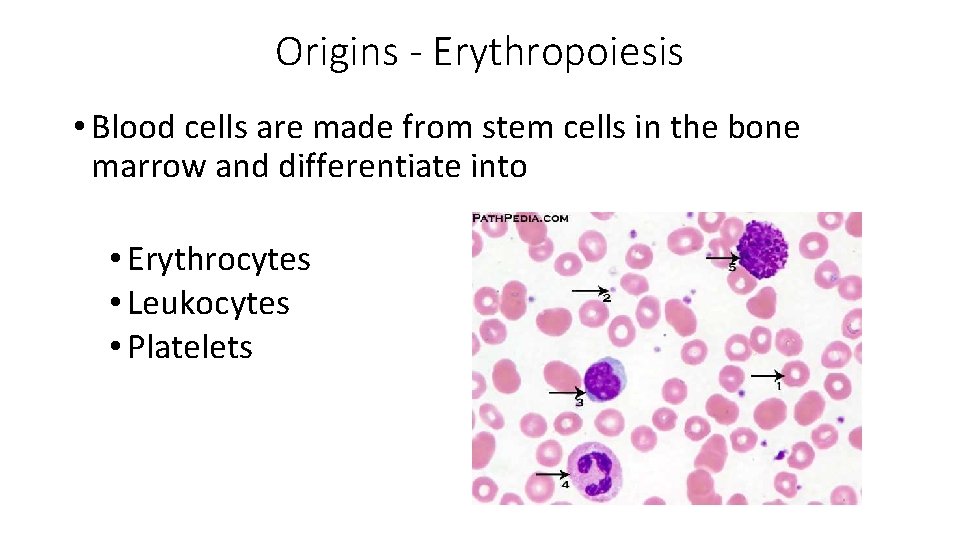
Origins - Erythropoiesis • Blood cells are made from stem cells in the bone marrow and differentiate into • Erythrocytes • Leukocytes • Platelets
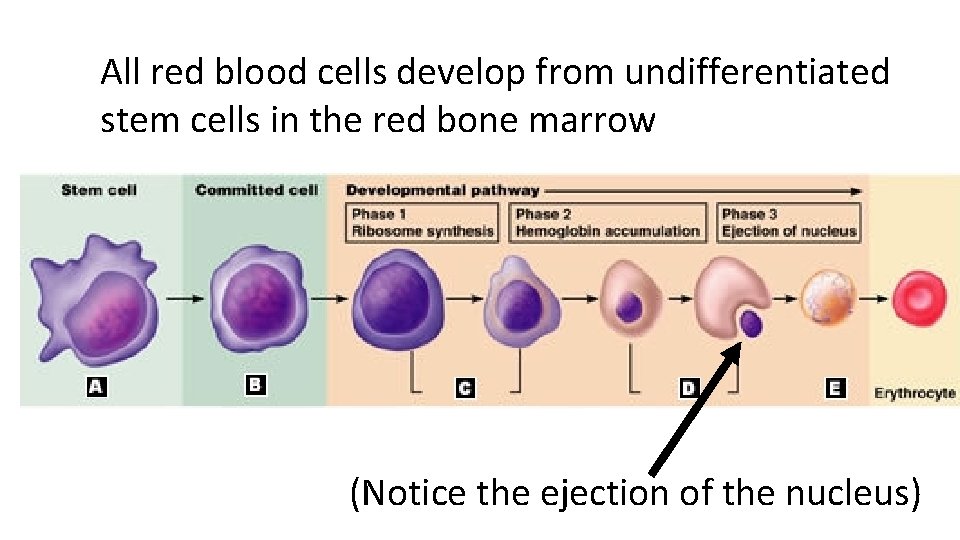
All red blood cells develop from undifferentiated stem cells in the red bone marrow (Notice the ejection of the nucleus)
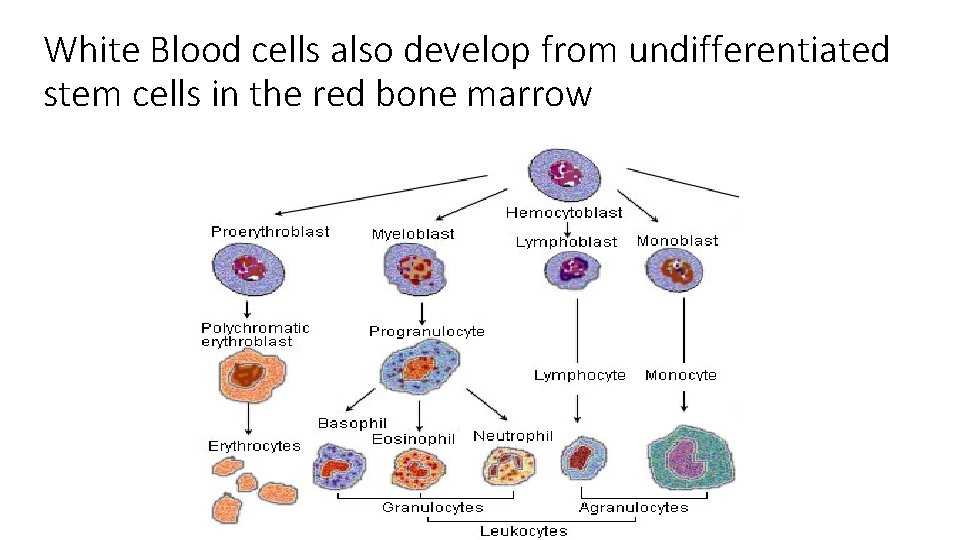
White Blood cells also develop from undifferentiated stem cells in the red bone marrow

Platelets • Essential for blood clotting • Form from a megakaryocyte that breaks off bits of its cytoplasm and membrane • Cytoplasmic “chunks” enter blood stream and form platelets

Blood Typing Dr. A
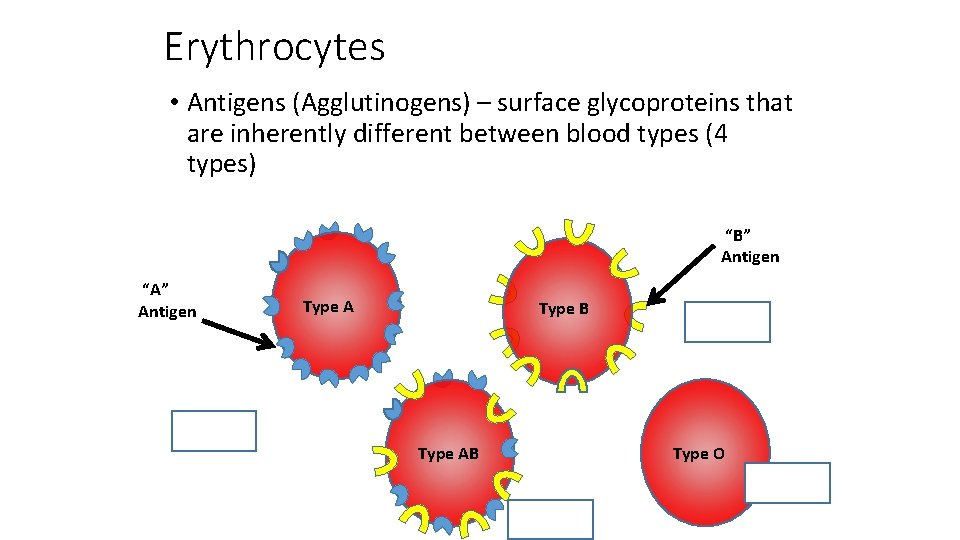
Erythrocytes • Antigens (Agglutinogens) – surface glycoproteins that are inherently different between blood types (4 types) “B” Antigen “A” Antigen Type A Type B Type AB Type O

Antibodies • Proteins that are created by the immune system to recognize “non-self” organisms/chemicals • Antigens on bacteria, fungi, protozoans, other pathogens • People with different blood types have antibodies that will attack “non-self” antigens erythrocytes
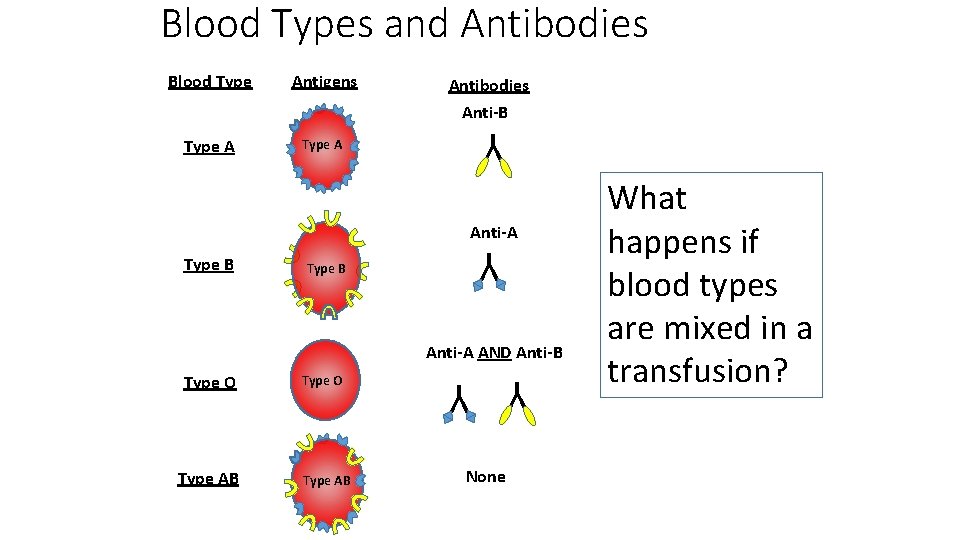
Blood Types and Antibodies Blood Type Antigens Antibodies Anti-B Type A Y Type A Anti-A Type B Y Type B Anti-A AND Anti-B Type AB Type O Type AB Y Y Type O None What happens if blood types are mixed in a transfusion?
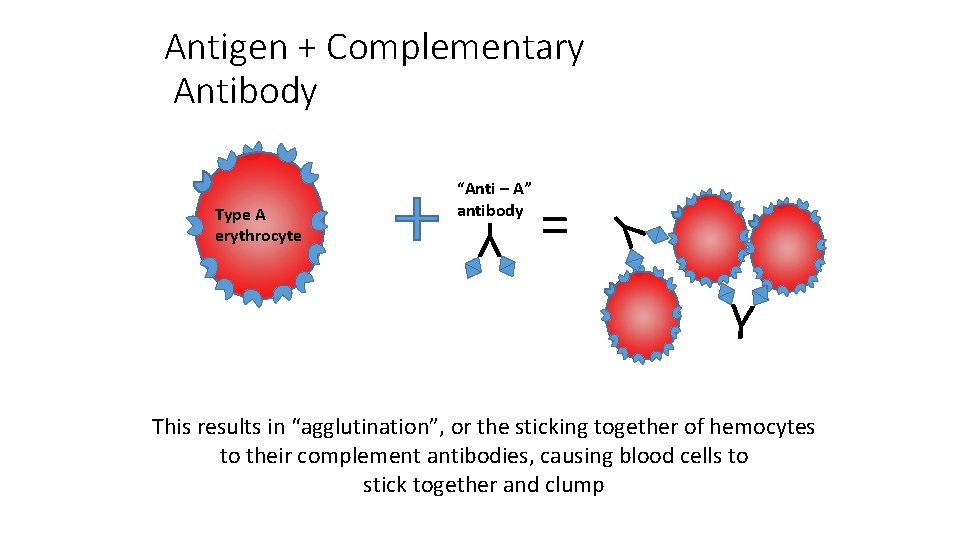
Antigen + Complementary Antibody = Y Y Type A erythrocyte “Anti – A” antibody Y This results in “agglutination”, or the sticking together of hemocytes to their complement antibodies, causing blood cells to stick together and clump

Rh Factor • In addition to the glycoproteins that equate to blood type (A, B) the “Rh” glycoprotein can be either present or absent • People that are “Rh negative” have the antibodies to the Rh antigen • This is what is represented by the + or – in blood types; (e. g. O+ = O blood type with RH factor (antigen), and therefore no antibodies to Rh)

Rh Factor and Adaptive Immunity • The immune system has a memory, after exposure to an antigen, your body will “remember” what antibodies to make to attack that antigen • This becomes a problem in women that are Rhnegative, and are pregnant with an Rh positive baby • Why?

Rh Factor and Adaptive Immunity • After a first pregnancy, blood from the baby can “mix” with blood from the mother • If the baby is Rh+ and the mother Rh-, the mother’s body will produce antibodies to Rh • Future pregnancies could be at risk, therefore, immune modulators must be administered (Rho. Gam)
Clotting (Hemostasis) • A coordinated series of events to stop the flow (loss) of blood 1. Vascular spasm 2. Platelet plug formation 3. Coagulation
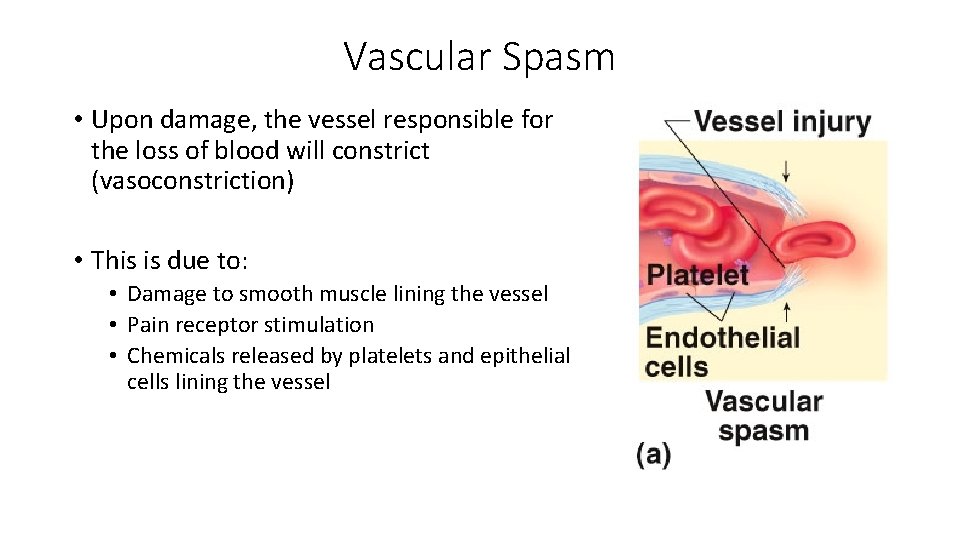
Vascular Spasm • Upon damage, the vessel responsible for the loss of blood will constrict (vasoconstriction) • This is due to: • Damage to smooth muscle lining the vessel • Pain receptor stimulation • Chemicals released by platelets and epithelial cells lining the vessel
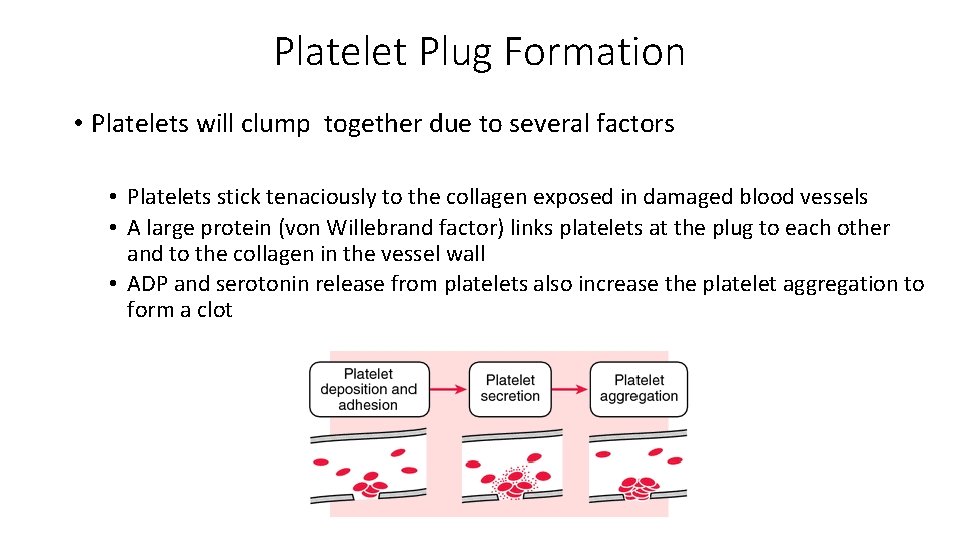
Platelet Plug Formation • Platelets will clump together due to several factors • Platelets stick tenaciously to the collagen exposed in damaged blood vessels • A large protein (von Willebrand factor) links platelets at the plug to each other and to the collagen in the vessel wall • ADP and serotonin release from platelets also increase the platelet aggregation to form a clot
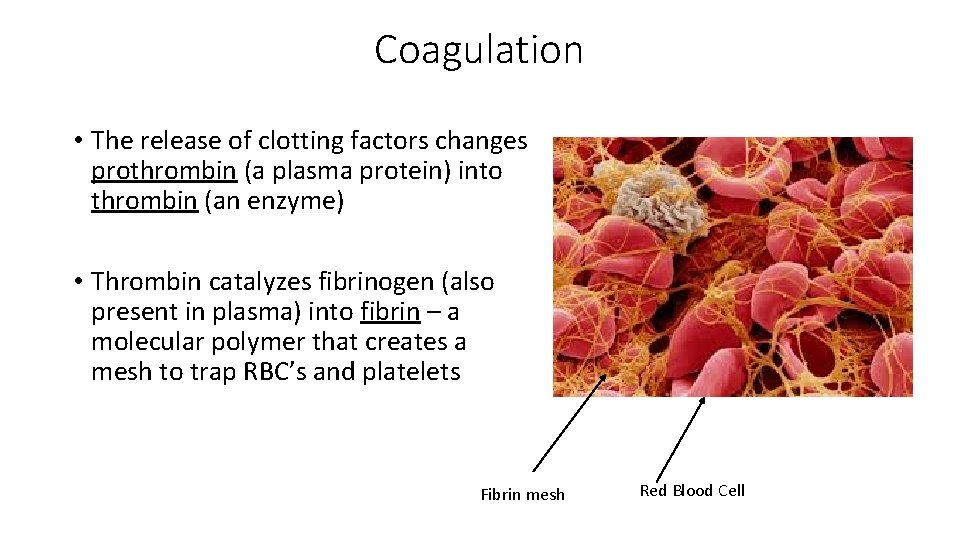
Coagulation • The release of clotting factors changes prothrombin (a plasma protein) into thrombin (an enzyme) • Thrombin catalyzes fibrinogen (also present in plasma) into fibrin – a molecular polymer that creates a mesh to trap RBC’s and platelets Fibrin mesh Red Blood Cell
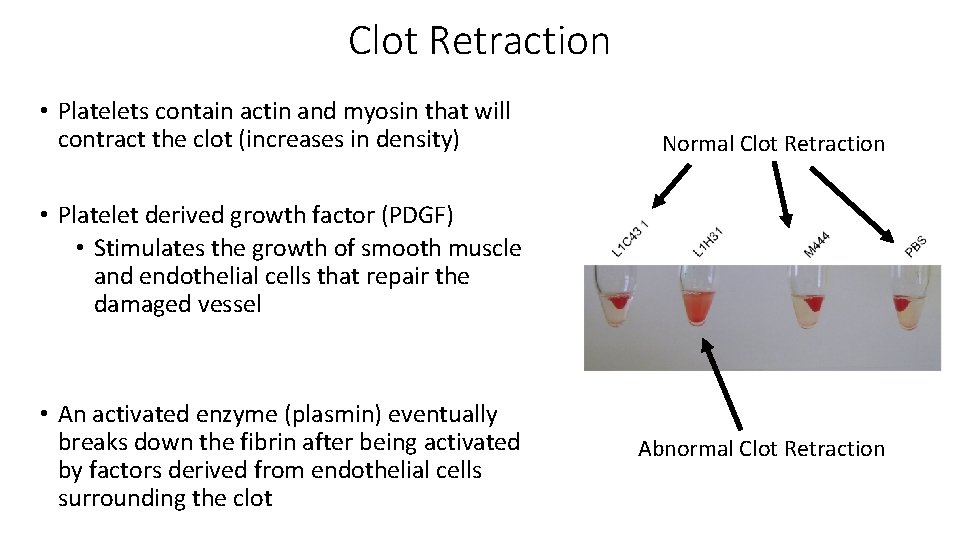
Clot Retraction • Platelets contain actin and myosin that will contract the clot (increases in density) Normal Clot Retraction • Platelet derived growth factor (PDGF) • Stimulates the growth of smooth muscle and endothelial cells that repair the damaged vessel • An activated enzyme (plasmin) eventually breaks down the fibrin after being activated by factors derived from endothelial cells surrounding the clot Abnormal Clot Retraction

Clotting Issues • Embolism – clot breaks from vessel wall and moves through the blood vessels • How can this be a problem? • Clots can be broken up via anticoagulants (aspirin, warfarin, heparin) which inhibits clotting factors
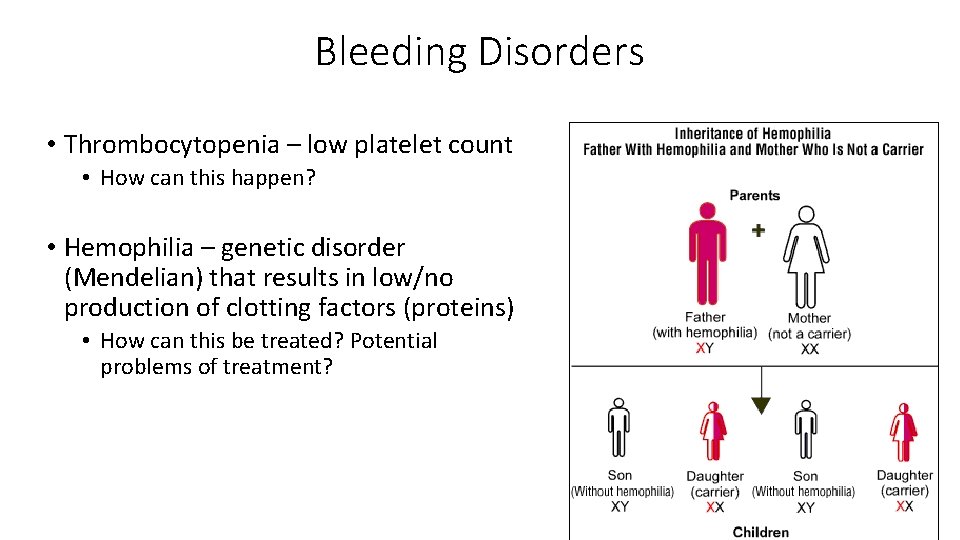
Bleeding Disorders • Thrombocytopenia – low platelet count • How can this happen? • Hemophilia – genetic disorder (Mendelian) that results in low/no production of clotting factors (proteins) • How can this be treated? Potential problems of treatment?
- Slides: 41