Blood Component Therapy Salwa I Hindawi MSc FRCPath

Blood Component Therapy Salwa I Hindawi MSc FRCPath CTM Mohamad H Qari, MD, RCPA Director of Blood Transfusion Services Associate Professor and Chairman/Hematology Dept. 4 th year medical students

RBC Agglutination 4 th year medical students
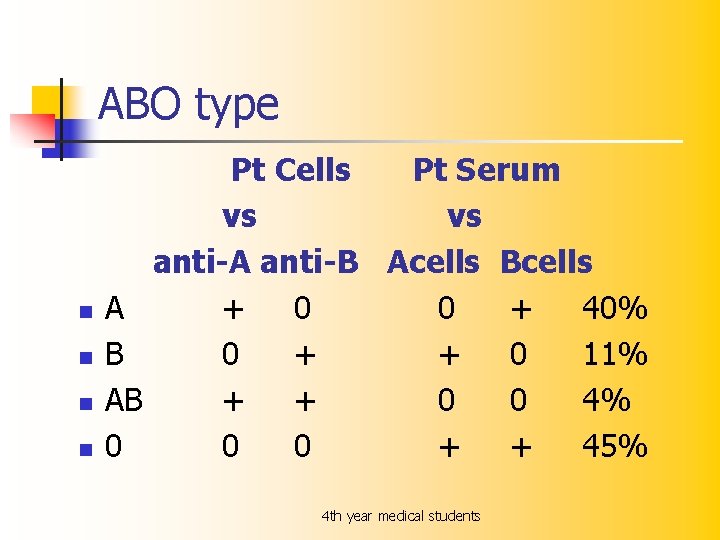
ABO type n n A B AB 0 Pt Cells Pt Serum vs vs anti-A anti-B Acells Bcells + 0 0 + 40% 0 + + 0 11% + + 0 0 4% 0 0 + + 45% 4 th year medical students

BLOOD COMPONENT THERAPY It is the transfusion of specific blood components required by the patient. Principles n n n Use blood products only when it is essential. Replace only the deficient component, if possible. Identify the cause and nature of the deficiency and if possible, treat it. 4 th year medical students
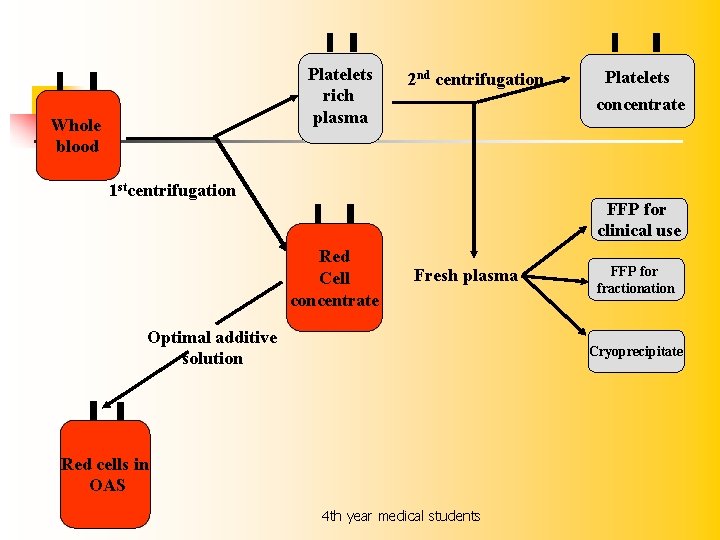
Platelets rich plasma Whole blood 2 nd centrifugation Platelets concentrate 1 stcentrifugation FFP for clinical use Red Cell concentrate Fresh plasma Optimal additive solution FFP for fractionation Cryoprecipitate Red cells in OAS 4 th year medical students

Blood COMPONENTS AVAILABLE FROM THE BLOOD BANK n n n Whole blood Packed RBCs Platelets Single donor platelets (Apheresis) Fresh Frozen Plasma (FFP) Cryoprecipitate 4 th year medical students

Indication for Red Blood Cells Transfusion n Red blood cells are component of choice to maintain an adequate supply of oxygen to meet tissue demands. One unit increase the haemoglobin level by 1 g/d. L in a 70 kg recipient. 4 th year medical students

Indication for Transfusion of Whole Blood n n Fresh whole blood<5 days old is often used for exchange transfusion in newborns. Stored whole blood can be used in actively bleeding patients who have lost > 30 -40% of their blood volume. 4 th year medical students

Indication for red blood cells Transfusion n n Symptomatic anaemia Acute blood loss>30 -40% of blood volume. Pre-operative Hb< 8 g/dl and operative procedure associated with major blood loss. Evidence of inadequate oxygen delivery. 4 th year medical students

Administration and Dose n n n Red blood cells transfusion has to be ABO & Rh specific. This component must be administered through a suitable transfusion set Dose of 4 ml/kg raises venous Hb by about 1 g/dl. 4 th year medical students

Specifications n n n Whole blood volume 450 mls+63 mls of CPD-A 1 anticoagulant. Packed RBCs volume 250 mls± 50 mls. Hct=0. 55 -0. 75. Anticoagulant CPD-A 1 store at 4 c°± 2 c° for 35 days. SAG-M for 42 days. 4 th year medical students

Indication for Platelet Transfusion n Decrease platelet production (Bone marrow failure) n n Therapeutic: for patient who are bleeding associated with BMF caused by either disease, therapy or irradiation. Prophylactic: >10 x 109/L to decrease morbidity in patients with thrombocytopenia due to B. M. F. 4 th year medical students

Cont, Platelet Transfusion n n In acute D. I. C (Disseminated intravasculr coagulation). In neonatal alloimmune thrombocytopenia (NAIT) from donor known to be negative for the appropriate HPA or mother platelet. Platelet function disorders or thrombocytopenia <50 x 10 9/L going for invasive procedure, for operation in critical sites such as the brain or eyes the platelet count should be raised to 100 x 109/L. In massive blood transfusion, the platelet count to be maintained above 50 x 109 /L. 4 th year medical students

Administration of Platelet Concentrate: n n ABO compatible platelet are preferred but not necessary. Platelet concentrate should be transfused as soon as possible after reaching the ward with standard blood transfusion sets with 170 mm filters. The transfusion should normally be completed within 30 minutes. Observation during platelet transfusion should include pulse& temperature before& after transfusion. 4 th year medical students

Indications For The Use Of FFP n n n n Definite indication: Replacement of single factor deficiencies Immediate reversal of warfarin effect Vitamin K deficiency Acute disseminated intravascular coagulation Thrombotic thrombocytopenic purpura Inherited deficiencies of inhibitors of coagulation: at, protein S, protein C. CI esterase inhibitor deficiency 4 th year medical students

Conditional uses of FFP n n n FFP is only indicated in the presence of bleeding and disturbed coagulation. Massive transfusion Liver disease Cardiopulmonary bypass surgery Special Paediatric indications: sever sepsis, DIC. 4 th year medical students

Administration of FFP n n n 1 unit of FFP= APPROXIMATELY 200 ML Dose = 12 -15 ml/kg Should be administered within 2 hours of thawing. PT & PTT used for monitoring in addition to the clinical assessment. ABO compatible FFP should be used. Compatibility testing is not required. Group O should only be given to group O recipient. Group A or B FFP can be given to group O recipient. Group AB FFP should be reserved for group AB recipients and for emergencies. 4 th year medical students

Indications for The Use Of Cryoprecipitate 1 -congenital or Acquired Fibrinogen Deficiency. 2 -Haemophilia A, von. Willebrand’s Disease. 3 -factor X 111 Deficiency 4 -disseminated intravascular coagulopathy(DIC). 4 th year medical students

Administration of Cryoprecipitate n n n n n 1 unit of cryo= approximately 10 -20 ml Adult dose equivalent to 10 units of cryo For factor replacement the dose can be calculated according to the volume of the factor in the concentrate. Fibrinogen 150 -300 mg/pack Von Willebrand factor 80 -120 u/pack Factor V 111 c 80 -120 u/pack Factor X 111 20 -30% of factor X 111 present in the FFP. Should be ABO compatible to avoid risk of haemolysis caused by donor anti. A or anti. B. Should be administered within 4 hours of thawing. 4 th year medical students

Platelet, Apheresis An adult dose of Platelets prepared from anticoagulated blood which is separated into components by apheresis machine with retention of the platelets and a portion of the plasma. The remaining elements may be returned to the donor 4 th year medical students

Specification Volume 200 – 800 mls Platelet count > 240 x 109 / unit Leucocyte count < 5 x 108 / unit PH at end of shelf life 6. 4 -7. 4 Availability: On request. Shelf life storage: 5 days at 22 ± 2°c gently agitated 4 th year medical students

4 th year medical students
- Slides: 22