blocker and Organophosphate Toxicity Mark Wahba Preceptor Dr

-blocker and Organophosphate Toxicity Mark Wahba Preceptor Dr. I. Vicas Core rounds March 25 th, 2004

-blockers

Teaching points • Recognize an overdose – “Toxidrome” • Management – What is most effective treatment?

Facts • One of the most widely prescribed classes of drugs • Indications: – Supraventricular dysrhythmias, hypertension, angina, thyrotoxicosis, migraine, glaucoma, essential tremor

Pharmacology Review

Pharmacology Review • autonomic nerve fibres can be classified in two groups • based on the chemical nature of the neurotransmitters

Pharmacology review Adrenergic Receptors • Found in CNS and Sympathetic NS • Stimulated by Norepinephrine and Epinephrine • two classes of receptors in SNS – – • Stimulation of receptor results in activation of adenyl cyclase, conveting AMP to c-AMP which opens ion channels
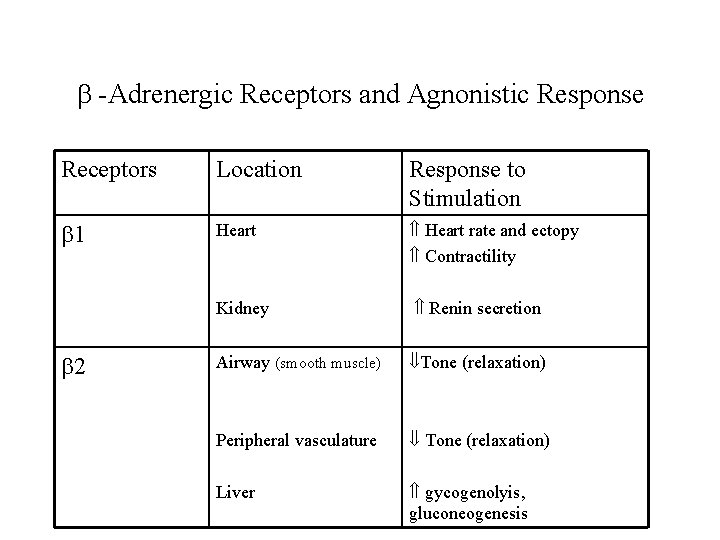
-Adrenergic Receptors and Agnonistic Response Receptors Location Response to Stimulation 1 Heart rate and ectopy Contractility Kidney Renin secretion Airway (smooth muscle) Tone (relaxation) Peripheral vasculature Tone (relaxation) Liver gycogenolyis, gluconeogenesis 2

Selectivity • Nonselctive • 1 and 2 – – – Propranolol Nadolol Timolol Pindolol Labetalol Sotalol • Selective • 1 – – Metoprolol Atenolol Esmolol Acebutolol

Pharmacology • rapidly absorbed after oral ingestion • peak effect in 1 -4 hours for regular release • Sustained release products may take up to 6 h to show effects and may last up to 72 h

Pharmacology • large volume of distribution therefore Hemodialysis is often not effective • blood levels are not useful • Varying degrees of lipophilicity • high lipid solubility leads to a larger volume of distribution – drug penetrates into the CNS eg. propranolol

Blocker overdose • • • Box 146 -8. Manifestations and Complications of Blocker Overdose in Order of Decreasing Frequency * * 1. Bradycardia (65/90 cases) 2. Hypotension (64/90) 3. Unconsciousness (50/90) 4. Respiratory arrest or insufficiency (34/90) 5. Hypoglycemia (uncommon in adults) 6. Seizures (common only with propranolol, 16/90) 7. Symptomatic bronchospasm (uncommon) 8. VT or VF (6/90) 9. Mild hyperkalemia (uncommon) 10. Hepatotoxicity, mesenteric ischemia, renal failure (rare or single case reports) ------------------------------------ • • * Data in parentheses from Langemeijer JJM et al: Neth J Med 40: 308, 1992. * VT, Ventricular tachycardia; VF, ventricular fibrillation. •

Clinical Features • CV- most pronounced effect on CV system – Bradycardia and AV block, hypotension are hallmarks – QRS widening, vent dysrhythmias: VT, VF, torsade de pointes may occur – Direct agonistic effect on 1 receptors • CNS- unconsciousness, seizures – Hypoperfusion, hypoglycemia

Clinical Features • Respiratory - Hypoxia – CHF or bronchospasm if hx of asthma • Metababolic - hypoglycemia – More common in children or people with diabetes – Is rarely severe

Management • Airway • Breathing – Bronchospasm-antagonism of 2 receptors • Only an issue if asthmatic or COPD – Congestive Heart Failure- antagonism of 1 receptors • Rare, usualy bradycardia and hypotension • Circulation
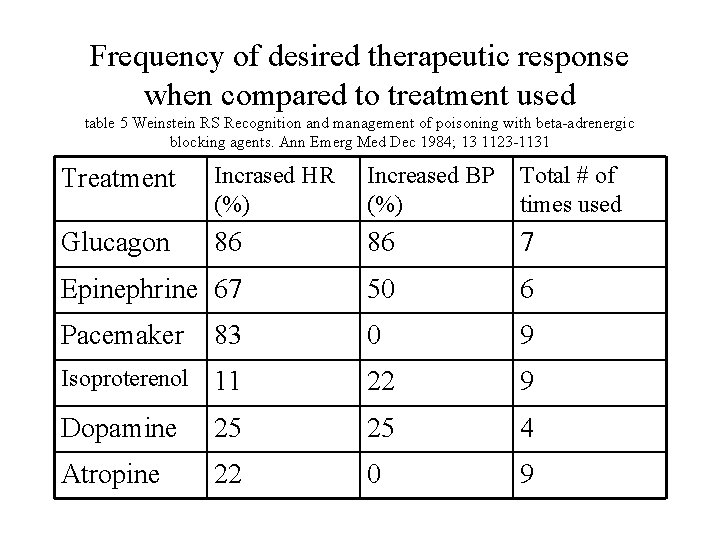
Frequency of desired therapeutic response when compared to treatment used table 5 Weinstein RS Recognition and management of poisoning with beta-adrenergic blocking agents. Ann Emerg Med Dec 1984; 13 1123 -1131 Treatment Incrased HR (%) Increased BP (%) Total # of times used Glucagon 86 86 7 Epinephrine 67 50 6 Pacemaker 83 0 9 Isoproterenol 11 22 9 Dopamine 25 25 4 Atropine 22 0 9
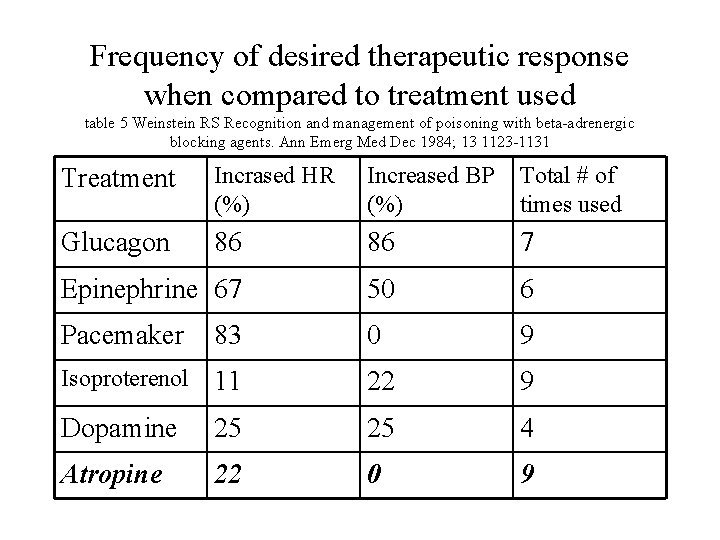
Frequency of desired therapeutic response when compared to treatment used table 5 Weinstein RS Recognition and management of poisoning with beta-adrenergic blocking agents. Ann Emerg Med Dec 1984; 13 1123 -1131 Treatment Incrased HR (%) Increased BP (%) Total # of times used Glucagon 86 86 7 Epinephrine 67 50 6 Pacemaker 83 0 9 Isoproterenol 11 22 9 Dopamine 25 25 4 Atropine 22 0 9

Management • Circulation • Fluids: 20 -40 ml/kg bolus crystalloid, may repeat • Atropine: 0. 5 mg for adults up to 3 mg, 0. 02 mg/kg for children (minimum 0. 1 mg) – H/r has a poor effect on raising heart rate and BP

Management • Glucagon: does not depend on -receptors for its action – increases intacellular c. AMP through non-adrenergic pathways • has both inotropic and chronotropic effects • helps to counteract hypoglycemia • 2 -10 mg IV bolus. (Children 50 mcg/kg) – Has 20 min 1/2 life – May run an infusion of 2 -5 mg/h – Side effect is nausea and vomiting

Management • Hyperinsulinemia-Euglycemia – based on an animal model – exact mechanism unclear • thought to be secondary to increased myocardial glucose utilization resulting from the high-dose insulin drips • Load with 1 u/kg of insulin • Then infusion of insulin at 0. 1 -1. 0 U/kg/hr • need glucose infusions +/or boluses to maintain euglycemia – Start with bolus of 2 ampules of D 50 – monitor blood glucose levels closely: q 1 h

Management • Vasopressors: epinephrine, dopamine, norepinephrine, isoproterenol – May need higher than average doses • Vent dysrhythmias: avoid 1 A and 1 C as they may potentiate AV block or prodysrhythmic effect. • Overdrive pace with pacemaker and Mg. SO 4 for torsades de pointes
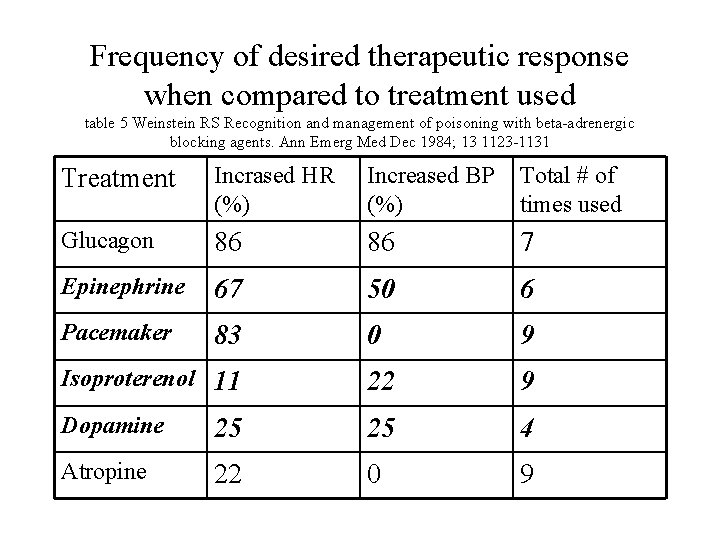
Frequency of desired therapeutic response when compared to treatment used table 5 Weinstein RS Recognition and management of poisoning with beta-adrenergic blocking agents. Ann Emerg Med Dec 1984; 13 1123 -1131 Treatment Incrased HR (%) Increased BP (%) Total # of times used Glucagon 86 86 7 Epinephrine 67 50 6 Pacemaker 83 0 9 Isoproterenol 11 22 9 Dopamine 25 25 4 Atropine 22 0 9

Management • Decontamination – Activated charcoal, can multidose b/c some -blockers undergo enterohepatic circulation – Whole bowel irrigation if delayed release preparation • Elimination – Hemodiaylsis unlikely to be beneficial • Find an antidote – Win Nobel prize here

Treatment of -blocker Poisoning Modified from Rosens box 146 -9 • Phase 1 - Resuscitation -boluses of fluids, glucagon, HIE, atropine • Phase 2 - Stabilization – Infusions of • Glucagon • Hyperinsulinemia-Euglycemia • Vasopressors • Early cardiac pacing

Disposition • If asymptomatic after 8 hours, ? send to psych • If unstable may need ICU

Medical/Legal Pitfalls from http: //www. emedicine. com/emerg/topic 59. htm • Failure to recognize beta-blocker toxicity as a cause of bradycardia and hypotension without a history of intentional overdose • Failure to administer activated charcoal because of missed diagnosis of beta-blocker intoxication • Administering ipecac syrup before the onset of sedation and seizures • Failure to adequately monitor a patient on multiple cardiac vasopressors (eg, use of Swan-Ganz catheter and/or arterial blood pressure monitoring) • Medically clearing a patient with beta-blocker toxicity before an 8 - to 10 -hour observation period • Failure to administer large enough doses of antidotes, including catecholamines, glucagon, calcium, and potentially insulin

Organophosphates

Teaching Points • Understand why the toxidrome occurs • Recognize the toxidrome • Recognize why early treatment with Pralidoxime is important

History • Organophosphorous compounds and carbamates – Known as cholinesterase inhibitors • Pesticides and insecticides – Parathion, House hold insect sprays-Malathion

Pharmacology Review • The autonomic nerve fibres can be classified in two groups • Based on the chemical nature of the neurotransmitters
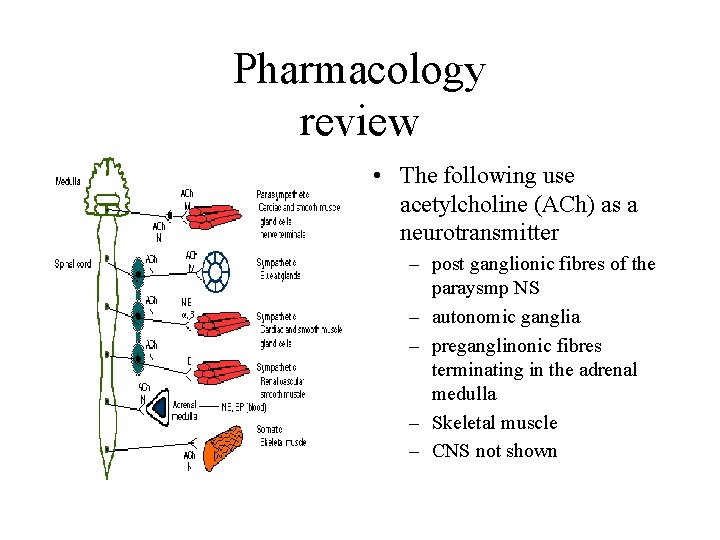
Pharmacology review • The following use acetylcholine (ACh) as a neurotransmitter – post ganglionic fibres of the paraysmp NS – autonomic ganglia – preganglinonic fibres terminating in the adrenal medulla – Skeletal muscle – CNS not shown

Cholinergic Receptors • Muscarinic • Nicotinic • heart rate (vagal • heart rate and blood stimulation) pressure ( NE from • blood pressure by postgang symp vasodilation neurons) • salivation • skeletal muscle • gut motlity activity • bronchial secretions • detrusor muscle tone
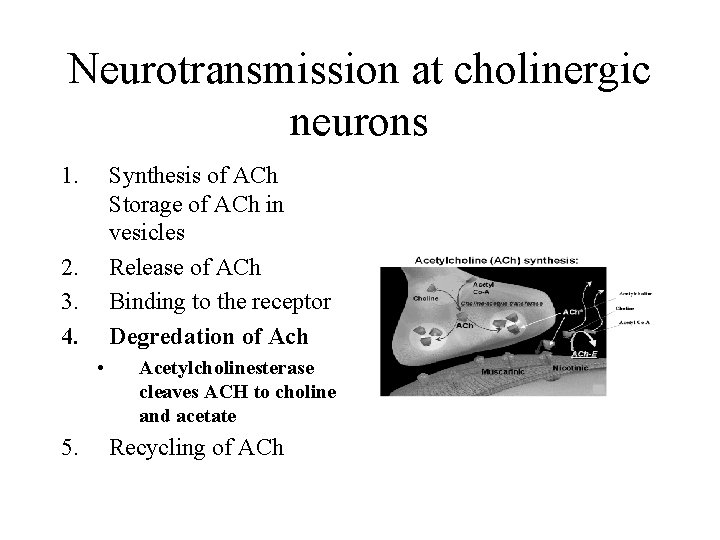
Neurotransmission at cholinergic neurons 1. Synthesis of ACh Storage of ACh in vesicles Release of ACh Binding to the receptor Degredation of Ach 2. 3. 4. • 5. Acetylcholinesterase cleaves ACH to choline and acetate Recycling of ACh

Organophosphates (OP) mechanism of toxicity • Inhibit the enzyme acetylcholinesterase (ACh. E) • Causes accumulation of excessive Ach • Overstimulation of the cholinergic receptors • How? – OPs covalently bind to ACh. E inactivating the enzyme

“Aging” • Permanent binding of the OP to the ACh. E enzyme occurs in variable amounts of time 1. Covalent binding of OP with ACh. E 2. Inactivates the enzyme 3. ACh. E enzyme releases an alkyl group – • known as “aging” Loss of the alkyl group makes it impossible for chemical reactivators (pralidoxime) to break the bond between the OP and ACh. E – Military agents ‘age’ in minutes or seconds

Carbamates • Also inhibit ACh. E – Medical carbamates: Physostigmine, edrophonium • Produce similar clinical effects • However, reactivation occurs much more quickly than with OPs b/c binding is reversible • Toxicity is brief and self-limited • Treatment with Pralidoxime is not required

Exposure • Absorbed by inhalation, ingestion, cutaneously • Highly lipophilic • OPs are easily absorbed and stored in fat tissue • May lead to persistent toxicity lasting for days after exposure

Clinical Presentation • May occur 1 -2 h after exposure – Inhalational exposure • may be delayed – skin exposure – with agents that must undergo metabolism to their active form

History and Physical • What agent were they • Muscarinic, Nicotinic exposed to? and CNS effects • How were they exposed? • Work: Protective equipment? Is it cleaned after each use? Frequency of exposure?

Muscarinic Effects • Muscarninc effect causes parasympathetic hyperstimulation of end organs • “DUMBELS” – – – – D - Defecation U - Urination M - Miosis B - Bronchospasm, Bronchorrhea, Bradycardia E - Emesis and Abdominal pain L - Lacrimation S - Salivation

Nicotinic Effects • Nicotinic effect causes adrenal gland secretion of epi and NE • Days of the week – – – M - Muscle cramps T - Tachycardia W - Weakness t. H - Hypertension F - Fasiculations S - Sugar (hyperglycemia)

CNS Effects • Agitation • Seizures • Coma • Other: pt may have a strong “garlicky” odor

Classification of Organophosphate Poisoning • From: Tafuri & Roberts Organophosphate Poisoning Annals of emergency Medicine Feb 1987, 16, 2 193 -202 • Latent poisoning • Clinical mainfestations: none • Serum cholinesterase: >50% of normal value

Classification of Organophosphate Poisoning • Mild poisoning • Clinical mainfestations: fatigue, H/A, dizziness, paresthesias, N, V, diaphoresis, salivation, wheezing, abd pain, diarrhea, able to ambulate • Serum cholinesterase: 20 -50% of normal value

Classification of Organophosphate Poisoning • Moderate poisoning • Clinical mainfestations: previous sympt, generalized weakness, dysarthria, fasiculations, miosis, can’t ambulate • Serum cholinesterase: 10 -20% of normal value

Classification of Organophosphate Poisoning • Severe poisoning • Clinical mainfestations: marked miosis, loss of pupilary light reflex, fasiculaitons, flacid paralysis, respiratory distress, cyanosis, unconsciousness • Serum cholinesterase: <10% of normal value

Laboratory evidence of poisoning • measure decreases in plasma pseudocholinesterase (PCh. E) and RBC ACh. E level • RBC ACh. E more reliable – 25% depression from baseline indicates exposure – Recovers within months of exposure • PCh. E sensitive but not specific (may be genetically low) – Recovers within weeks of exposure • However, wide interindividual variability • Most helpful in continuous monitoring – Workplace health surveillance program

Treatment • Decontamination • Staff: must wear chemical protective clothing in grossly contaminated pts – Decontaminate in high flow ventilation room or outdoors – Wear nitrile or buyl rubber gloves, eyeshields, protective clothing

Treatment • Patient: find out what they and caregivers have already done • Skin: remove all contaminated clothing and irrigate with copious amounts of fluid – Must permanently discard contaminated leather articles • Ingestion: activated charcoal

Treatment • Airway • excessive salivation • vomiting • may require aggressive suctioning

Treatment • Breathing • Bronchospasm and bronchorrhea hypoxia – “drown in their own secrections” • respiratory muscle dysfunction ventilatory support – Preceded by neck muscle weakness • Succinylcholine’s effects can be prolonged in presence of OP toxicity

Atropine • Belladonna alkaloid • Antimuscarinic – No effect on nicotinic receptor • Competitive inhibitor of ACh – Competitively binds to muscarinic receptor preventing ACh from binding • Prevents bradycardia, bronchospasm, bronchorrhea

Atropine • End-point of atropinization is drying of respiratory secretions – Primary cause of death is pt ‘drowning in their own secretions’ • 0. 5 -2 mg IV repeat as needed • Large doses may be needed: 100 -500 mg IV/hour • If Atropine is used, must use pralidoxime

Pralidoxime • Synthetic pyridinium compound • “Reactivates” inhibited ACh. E at both muscarinic and nicotinic receptors – Makes the enzyme active again • has a “charged group that approaches an anionic site on the ACh. E enzyme which displaces the OP and regenerates the enzyme” – Lippincott’s Illustrated Reviews Pharmacology 2 nd ed. Harvey RA editor. Lippinocott-Raven New York

Pralidoxmine • Reverses muscular weakness and fasiculations – 1 -2 g bolus (20 -40 mg/kg in children) over 30 -60 min – or infusion of 200 -500 mg/h (5 -10 mg/kg/h in children) titrating to desired clinical response • Must give early before aging has occurred and enzyme is irreversibly bound

Pralidoxime • The OP Fenthion will leach out of fat stores for days to weeks • Infusion may needed for several days – OP toxicity will continue until new ACh is synthesized by the body

Treatment • • • Circulation If bradycardic atropine If hypotensive think dehydration fluid

Treatment • Elimination • Dialysis not indicated b/c of large Vd • Body eventualy metabolizes the OP and it is excreted in the urine

Treatment • Find an Antidote – Two parts 1. Atropine 2. Pralidoxime

Treatment • General Management – BZD for agitation, seizures – ICU for ventilatory support – ECG, Foley, O 2 sat monitor etc • Disposition: – Most pts that require medical intervention will be hospitalized and need observation for at least 24 hours

Medical & Legal Pitfalls http: //www. emedicine. com/emerg/topic 346. htm • Failure to recognize cholinergic symptoms and delaying intervention may result in increased morbidity and mortality • Failure to adequately decontaminate the exposed patient may result in secondary contamination of others • Failure to consider the possibility of an intermediate syndrome or organophosphateinduced delayed neurotoxicity

Real Life • Tokyo, Japan 1995 five containers of nerve agent Sarin place on Subway • 5000 -6000 people exposed • 3227 evaluated in emergency departments • 493 admitted to hospitals • 12 died • 135 ambulance personnel developed symptoms • 33 hospitalized • Many hospital staff also required treatment • Neither ambulance personnel nor hospital staff had any protection

Key Points • Protect staff from Contamination • Treat with Pralidoxime early to prevent aging

Thanks Dr. Vicas

References • • • Poisoning & Drug Overdose 4 th ed, Olson KR ed. Lange/Mcgraw Hill Toronto 2004 Rosen’s Lippincott’s Illustrated Reviews Pharmacology 2 nd ed. Harvey RA editor. Lippinocott. Raven New York http: //www. ovc. uoguelph. ca/Bio. Med/Courses/Public/Pharmacology/pharmsite/98309/ANS_Intro/ANS_intro. html Emergency Medicine Reports / April 21/ 2003 / Chemical Warfare Agents Part II: Nerve Agents, Blood Agents, and Protective Gear Author: Charles E. Stewart Emergency Medicine Reports / May 24/ 1999 /Neuromuscular Transmission Failure in the ED: Recognition, Assessment, and Targeted Management of a Life-Threatening Disorder, Masood Haque, MD Weinstein RS Recognition and management of poisoning with beta-adrenergic blocking agents. Ann Emerg Med Dec 1984; 13 1123 -1131 http: //www. emedicine. com/emerg/topic 59. htm http: //www. emedicine. com/emerg/topic 346. htm From: Tafuri & Roberts Organophosphate Poisoning Annals of emergency Medicine Feb 1987, 16, 2 193 -202
- Slides: 65