Bleeding in Patients Undergoing Percutaneous Coronary Interventions A

Bleeding in Patients Undergoing Percutaneous Coronary Interventions: A Risk Model From 302, 152 Patients in the NCDR. Sameer K. Mehta MD, Andrew D. Frutkin MD, Sunil V. Rao MD, Fang–Shu Ou MS, Eric D. Peterson MD, MPH, John A. Spertus MD, MPH, Steven P. Marso MD, on behalf of the NCDR The Mid America Heart Institute and Duke Clinical Research Institute. American Heart Association Scientific Sessions – November 5, 2007

Presenter Disclosure Information Sameer K. Mehta MD et al. Bleeding in Patients Undergoing Percutaneous Coronary Interventions: A Predictive Model From 302, 152 Patients in the NCDR. No authors report any disclosures or conflicts of interest.

Bleeding and PCI n The incidence of major bleeding in patients undergoing PCI is as high as 5%. n Bleeding events have been associated with an increased incidence of adverse outcomes, including death, MI, and stroke. n A tool that helps physicians assess the risk of bleeding in PCI patients may allow physicians to individualize antithrombotic and antiplatelet therapy while mitigating the risk of bleeding. Goodman et al. Circulation 2003. Eikelboom et al. Circulation 2007. Rao et al. American Journal of Cardiology 2005.

Aims n n n To determine the risk factors of bleeding in a large, contemporary, real-world cohort of patients undergoing PCI. To develop a risk model for bleeding. To test the validity of this risk model in clinically important subgroups.

Methods n n n Version 3. 04 of NCDR Cath-PCI Registry Contains data from PCI procedures performed from Jan. 1, 2004 to March 31, 2006 at over 600 U. S. hospitals. Exclusions: Non-index PCI Patients who died same day as PCI Patients with missing bleeding data Centers that did not report any bleeding events

Methods (2) n Final study population: – – – n 302, 152 patients 302, 152 PCI procedures 440 U. S. hospitals Determined predictors of bleeding with generalized estimating equation models. – Models adjusted for age, sex, weight, GFR, PCI status, presence of ACS, cardiogenic shock, intra-aortic balloon pump treatment, history of MI, diabetes, cerebrovascular disease, peripheral vascular disease, hypertension, COPD, prior PCI, NYHA class, prior valve surgery, Caucasian, prior CHF, smoker, family history of CAD, EF, dyslipidemia, prior CABG, and CHF.

Methods (3) n Risk model training set. n n Risk model validation set n n n 241, 512 patients (80% of total) 60, 640 patients (20% of total) Variable selection via backward selection and clinical judgment Goodness of fit determined by calibration plot Discrimination assessed by c-statistic Risk model tested in various clinically meaningful subgroups

NCDR Bleeding Definitions Primary Endpoint: Bleeding from any source n Percutaneous entry site: n n n during hospitalization; transfusion and/or cause a drop in hemoglobin >3. 0 g/dl; hematoma n >10 cm for femoral access, n >2 cm for radial access, n or >5 cm for brachial access. n Retroperitoneal: n transfusion and/or cause a drop in hemoglobin >3. 0 g/dl.

NCDR Bleeding Definitions (2) n GI: n n GU: n n transfusion and/or cause a drop in hemoglobin >3. 0 g/dl. Other/Unknown: n n During hospitalization transfusion and/or cause a drop in hemoglobin >3. 0 g/dl.
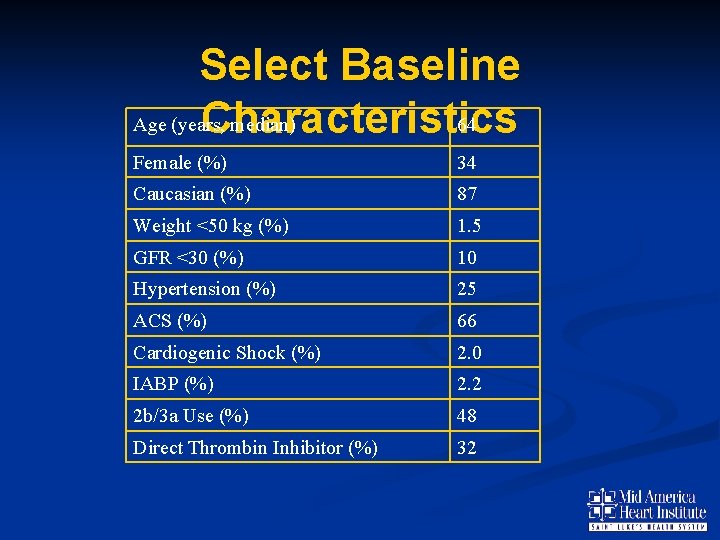
Select Baseline Age (years, median) 64 Characteristics Female (%) 34 Caucasian (%) 87 Weight <50 kg (%) 1. 5 GFR <30 (%) 10 Hypertension (%) 25 ACS (%) 66 Cardiogenic Shock (%) 2. 0 IABP (%) 2. 2 2 b/3 a Use (%) 48 Direct Thrombin Inhibitor (%) 32
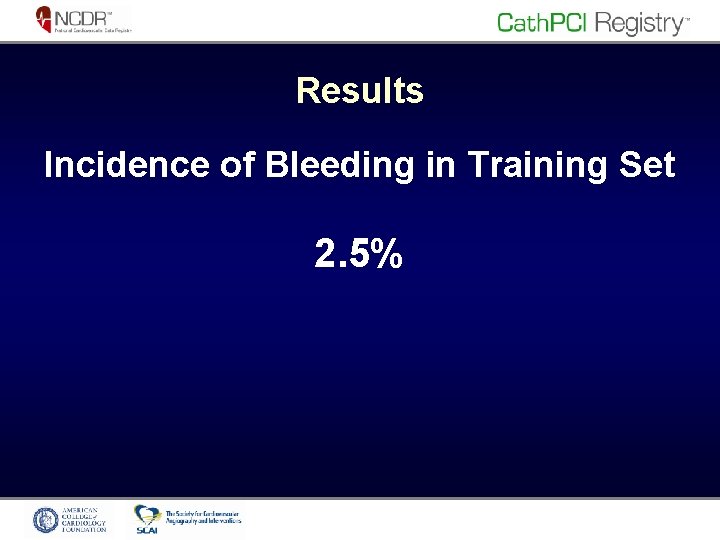
Results Incidence of Bleeding in Training Set 2. 5%
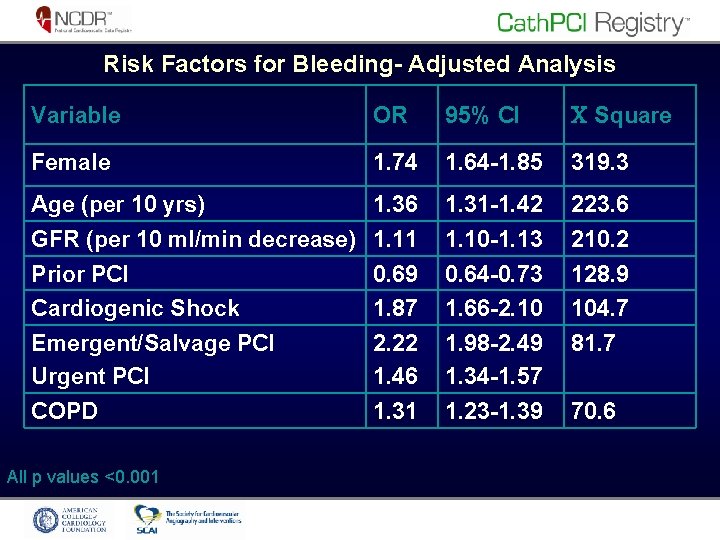
Risk Factors for Bleeding- Adjusted Analysis Variable OR 95% CI Square Female 1. 74 1. 64 -1. 85 319. 3 Age (per 10 yrs) 1. 36 1. 31 -1. 42 223. 6 GFR (per 10 ml/min decrease) 1. 11 1. 10 -1. 13 210. 2 Prior PCI 0. 69 0. 64 -0. 73 128. 9 Cardiogenic Shock 1. 87 1. 66 -2. 10 104. 7 Emergent/Salvage PCI Urgent PCI 2. 22 1. 46 1. 98 -2. 49 1. 34 -1. 57 81. 7 COPD 1. 31 1. 23 -1. 39 70. 6 All p values <0. 001
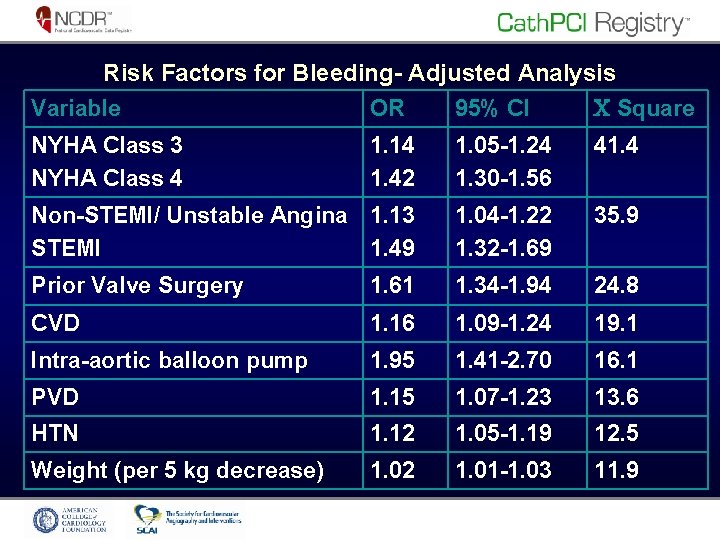
Risk Factors for Bleeding- Adjusted Analysis Variable OR 95% CI Square NYHA Class 3 NYHA Class 4 1. 14 1. 42 1. 05 -1. 24 1. 30 -1. 56 41. 4 Non-STEMI/ Unstable Angina 1. 13 STEMI 1. 49 1. 04 -1. 22 1. 32 -1. 69 35. 9 Prior Valve Surgery 1. 61 1. 34 -1. 94 24. 8 CVD 1. 16 1. 09 -1. 24 19. 1 Intra-aortic balloon pump 1. 95 1. 41 -2. 70 16. 1 PVD 1. 15 1. 07 -1. 23 13. 6 HTN 1. 12 1. 05 -1. 19 12. 5 Weight (per 5 kg decrease) 1. 02 1. 01 -1. 03 11. 9
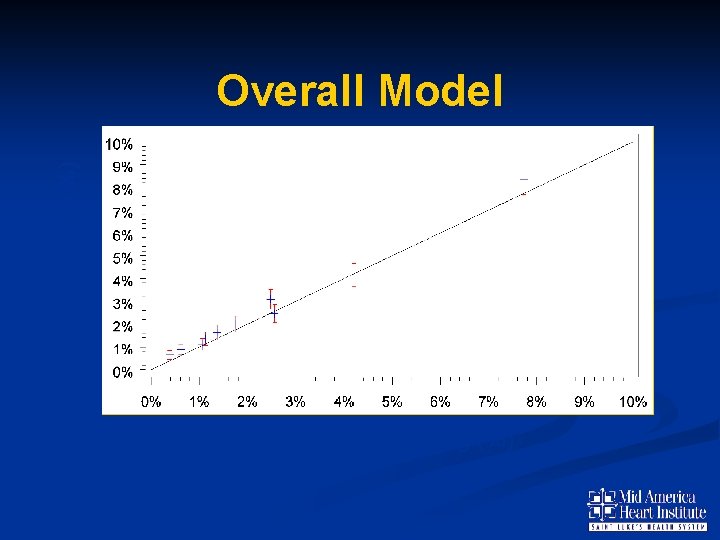
Predicted Bleeding (%) Overall Model N= 60, 640 C Statistic =0. 73 Observed Bleeding (%)
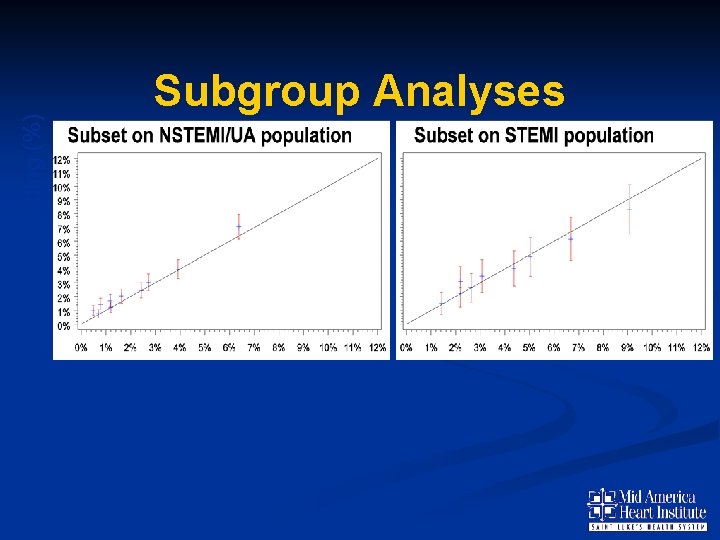
Predicted Bleeding (%) Subgroup Analyses N= 30, 872 N= 9, 130 C Statistic =0. 72 C Statistic =0. 70 Observed Bleeding (%)
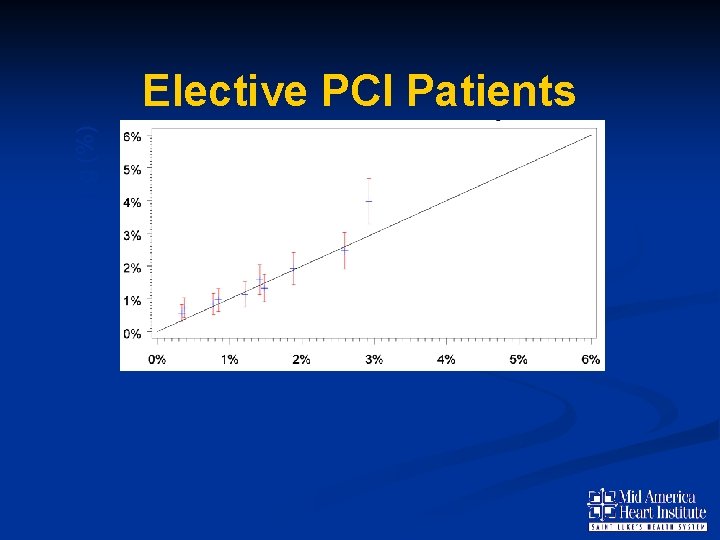
Predicted Bleeding (%) Elective PCI Patients N= 29, 733 C Statistic =0. 67 Observed Bleeding (%)
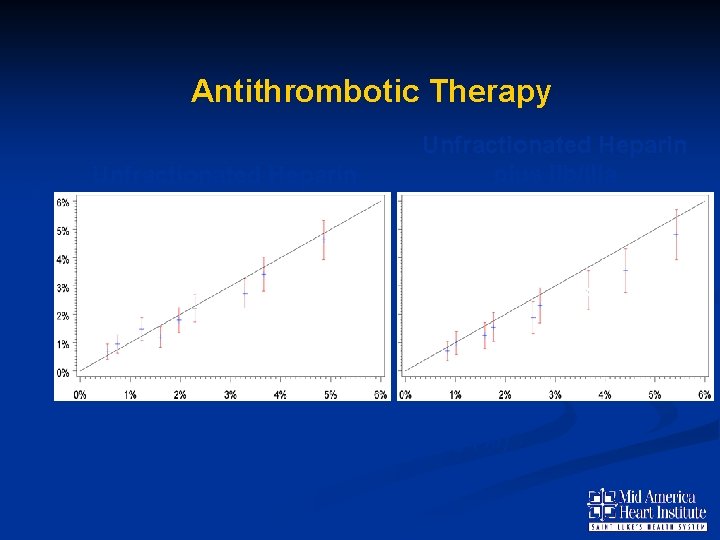
Predicted Bleeding (%) Antithrombotic Therapy Unfractionated Heparin plus IIb/IIIa N= 22, 666 N=24, 969 C Statistic =0. 73 Observed Bleeding (%) C Statistic =0. 72
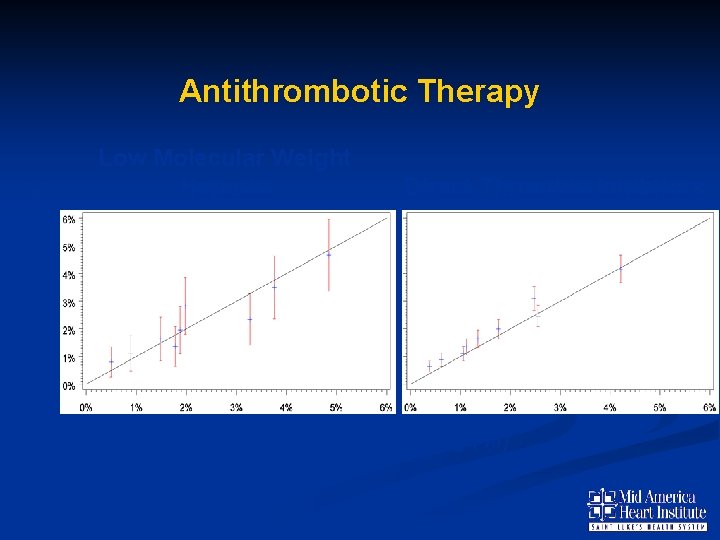
Predicted Bleeding (%) Antithrombotic Therapy Low Molecular Weight Heparin Direct Thrombin Inhibitors N= 10, 108 N= 19, 316 C Statistic =0. 68 C Statistic =0. 73 Observed Bleeding (%)

Conclusions n Identified risk factors for bleeding in PCI patients n Developed a risk model that predicted the risk of bleeding in patients undergoing PCI n Model performed well in various clinically important subgroups

Limitations n Bleeding definitions differ between NCDR and TIMI/ GUSTO n Low reported incidence of bleeding events

Future Directions n n Risk Score for Bleeding. Implementation of predictive model/ risk score into randomized studies of patients undergoing PCI.
- Slides: 21