Bleeding Disorders Meera Shreedhara 82508 What is it

Bleeding Disorders Meera Shreedhara 8/25/08

What is it? n A bleeding disorder is an acquired or inherited tendency to bleed excessively
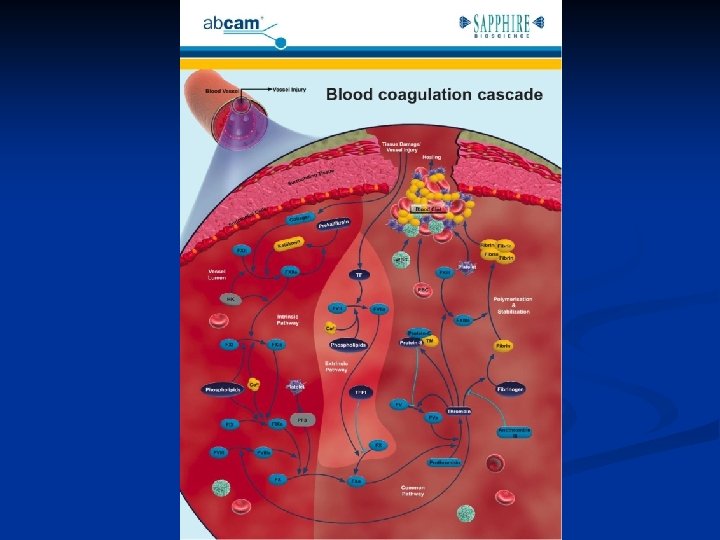
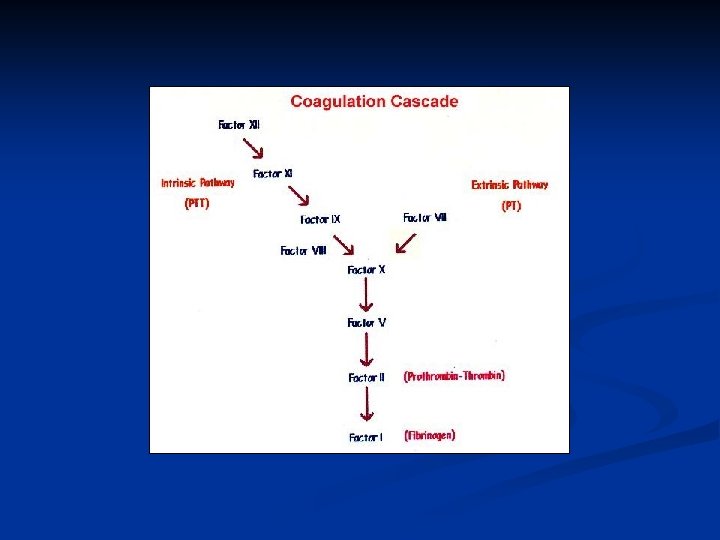

Mechanisms of bleeding Vascular Integrity n Platelets n Clotting factors n Fibrinolysis n n Derangement of any of these factors can cause abnormal bleeding

Key to diagnosis History n

Bleeding history n n n n n Epistaxis Gingival hemorrhage Mucosal Bleeding Heavy Menses Child birth Easy bruisability Bleeding following tooth extractions Hematomas Bleeding following surgery Hemarthrosis

Medication History Aspirin n Warfarin n NSAIDS n B- Lactam antibiotics n Clopidogrel and other antiplatelet agents n Herbal medications. n

Nutritional history Vit K deficiency n Vit C deficiency n Broad spectrum antibiotics n

Clinical Characterisitc Platelet defect Clotting factor deficiency Site of bleeding Skin, mucous membranes (gingivae, nares, GI and genitourinary tracts) Deep in soft tissues (joints, muscles) Bleeding after minor cuts Yes Not usually Petechiae Present Absent Ecchymoses Small, superficial Large, palpable Hemarthroses, muscle hematomas Rare Common Bleeding after surgery Immediate, mild Delayed, severe
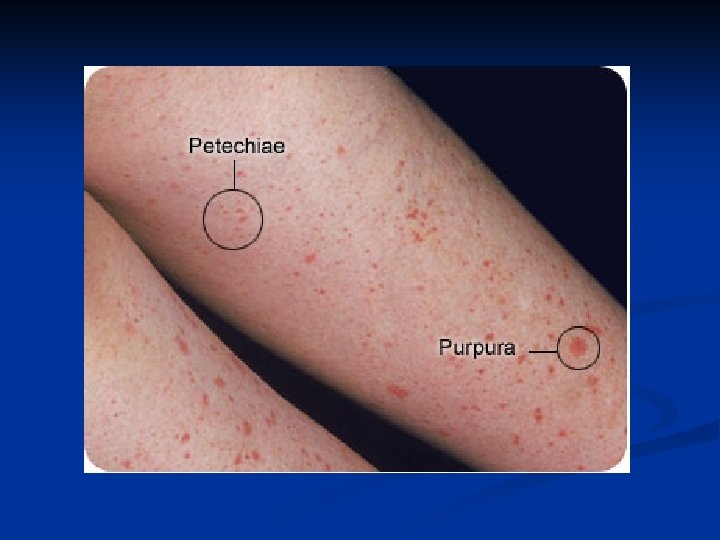
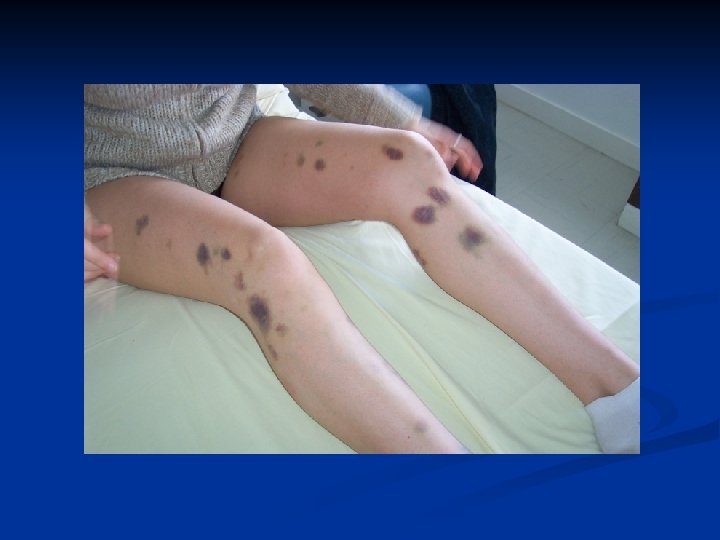
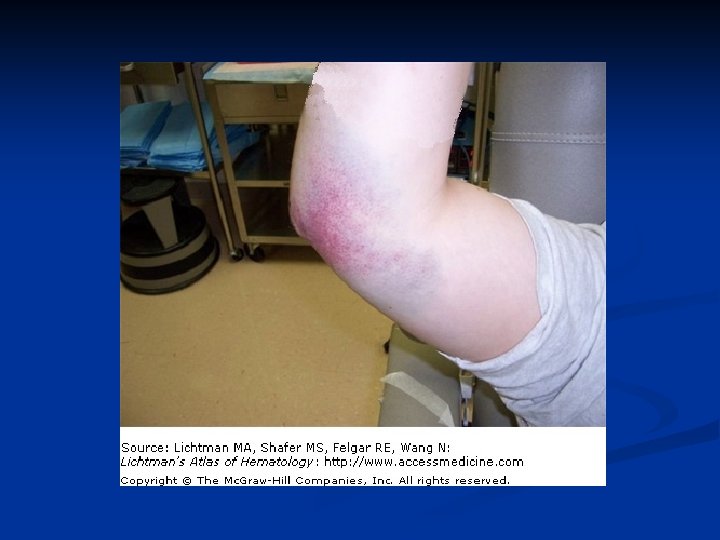
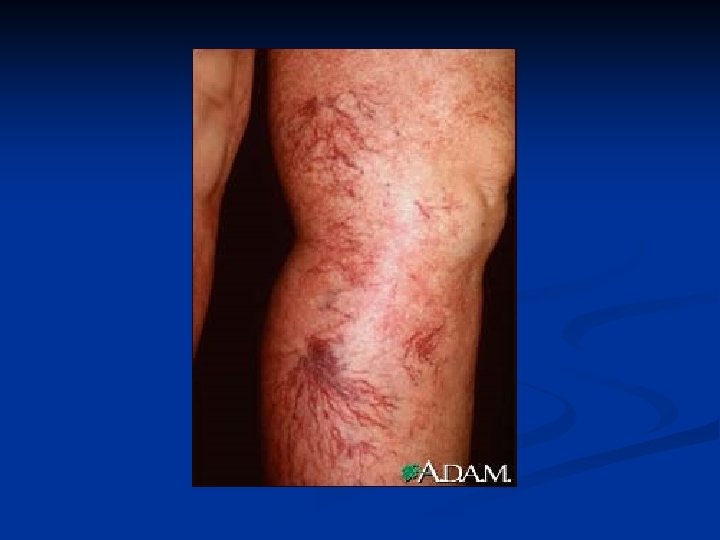

History Should the pt undergo a limited or extensive workup? n Is this acquired or hereditary? n Is this likely a disorder of clotting factors, platelets, fibrinolysis or v. WF? n Do medications or intercurrent illnesses play a role? n What is the immediate cause for which a workup is being done? n

Hereditary n Deficiency of coagulation factors n n Platelet disorders n n Glanzmann thrombasthenia Bernard-Soulier syndrome Platelet granule disorders Fibrinolytic disorders n n n Hemophilia Fibrinogen deficiency Von Willebrand disease Alpha 2 antiplasmin deficiency PAI 1 deficiency Structural disorders n n Hemorrhagic Telangiectasias Ehler Danlos syndrome

Acquired Thrombocytopenis n Liver disease n Renal failure n Vit K deficiency n Acquired antibodies to coagulation factors n DIC n Drugs n Vascular n

Lab testing Platelet count n Bleeding time-Measure of the interaction of platelets with the blood vessel wall. n Thrombocytopenia (platelet count usually below 50, 000/micro. L), n Qualitative platelet abnormalities (eg, uremia), n von Willebrand disease (VWD), n Vascular purpura, n Severe fibrinogen deficiency n

Platelet function assay n n n Expose platelets within citrated whole blood to high shear (5, 000 to 6, 000/sec) within a capillary tube and monitor the drop in flow rate as the platelets form a hemostatic plug within the center of a membrane coated with collagen and either ADP or epinephrine Abnormal closure times are an indication of platelet dysfunction, they are not specific for any disorder The test is coagulation factor independent PFA-100™ is more sensitive (>70 percent) than the bleeding time (20 to 30 percent) in detecting all subtypes of von Willebrand's disease (v. WD) Exception is type 2 N v. WD, in which the hemostatic defect resides in the Factor VIII binding site on v. WF

Platelet function assay Collagen/epinephrine closure time (CEPI-CT)Abnormal in Aspirin intake n Collagen/adenosine diphosphate (CADT-CT)Normal in aspirin intake n

Prothrombin time Measure of the extrinsic pathway and common pathway n Bypasses the intrinsic pathway and uses thromboplastins to substitute for platelets n Within the combined pathway, factors VII, X, and prothrombin are vitamin-K dependent and are altered by warfarin n
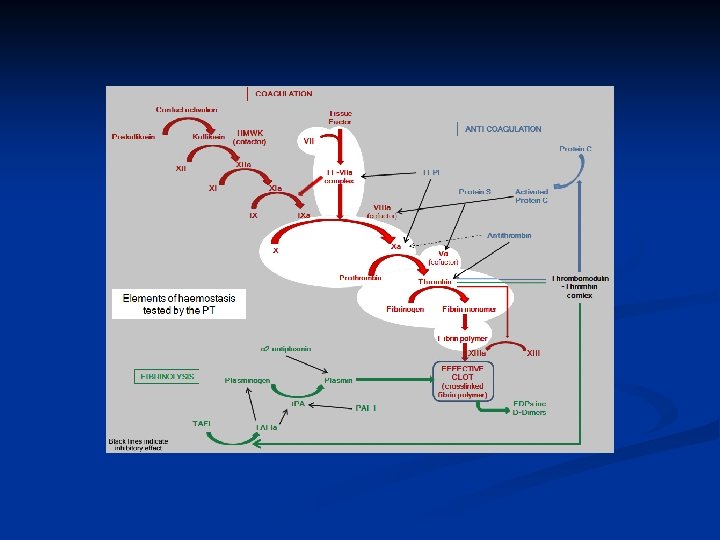

Prolonged PT n n n Vitamin K deficiency Liver disease, which decreases the synthesis of both vitamin K-dependent and -independent clotting factors. Deficiency or inhibition of factors VII, X, II (prothrombin), V, or fibrinogen The infrequent antiphospholipid antibodies (lupus anticoagulant phenomenon) with antiprothrombin activity Heparin does NOT prolong the PT

a. PTT Measures the intrinsic and common pathways of coagulation n Uses partial thromboplastins; they are incapable of activating the extrinsic pathway n Prolonged in deficiency of, or an inhibitor to, any of the clotting factors except for factor VII n Prolonged in the presence of Lupus Anticoagulant. n Used to monitor heparin activity n
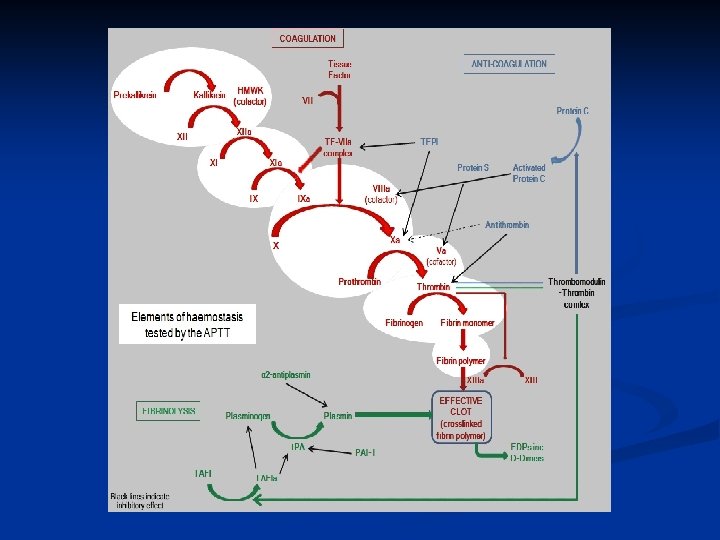
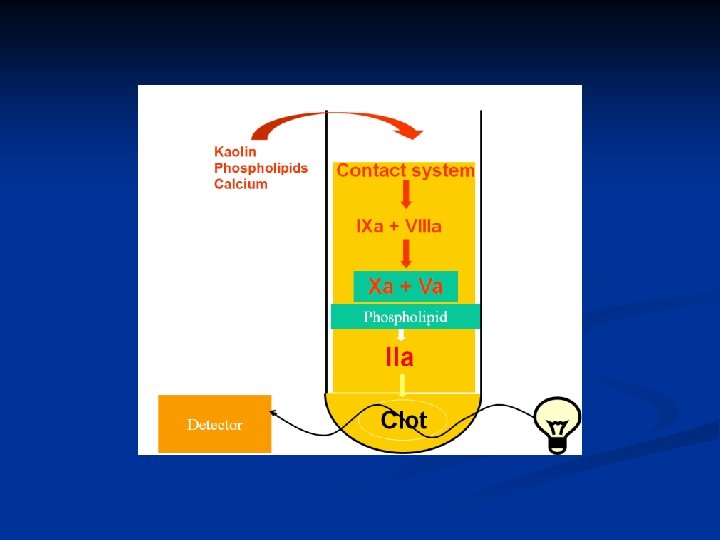

Thrombin time Measure conversion of fibrinogen to fibrin monomers and the formation of initial clot by thrombin n Hypofibrinogenemia, n Dysfibrinogens n Increased fibrin split products n Heparin increases TT but not RT n
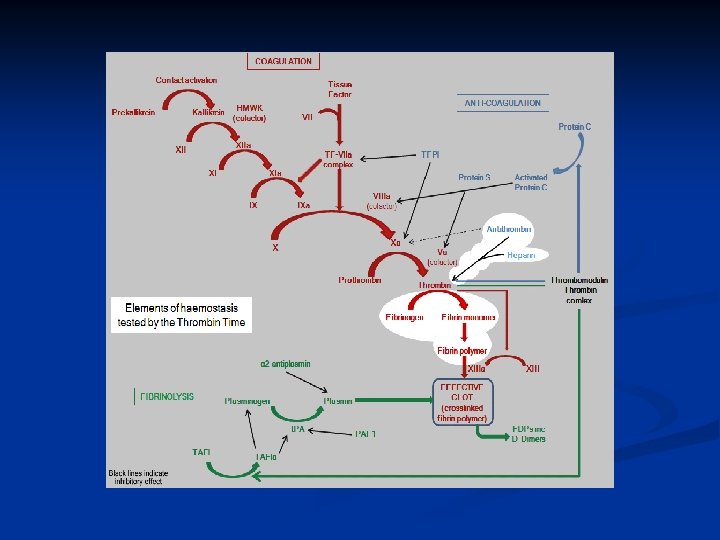

Factor deficiencies/ inhibitors n n n A prolonged a. PTT can be due to a deficiency (or absence) of a coagulation factor or the presence of a coagulation factor inhibitor Mixing studies help differentiate this Lupus anticoagulants can result in a prolonged a. PTT that is not correctable by the addition of normal plasma Overcome by adding excess platelet phospholipid (particularly a hexagonal phase phospholipid) or by assessing the diluted Russell's viper venom time
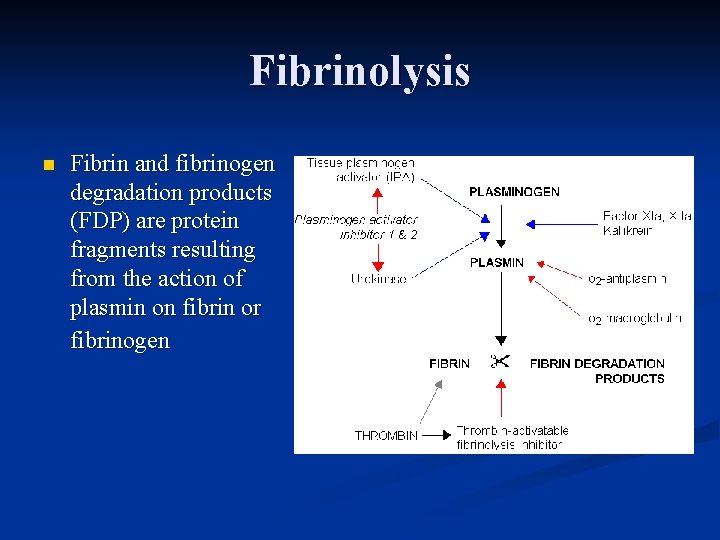
Fibrinolysis n Fibrin and fibrinogen degradation products (FDP) are protein fragments resulting from the action of plasmin on fibrin or fibrinogen

Fibrinolysis FDP assays do not differentiate between fibrin degradation products and fibrinogen degradation products n Fibrin D-dimers are degradation products of cross-linked fibrin n D-dimers specifically reflect fibrinolysis of cross-linked fibrin (ie, the fibrin clot) – so are more reliable indicators of thrombosis n

Fibrinolysis Assays for plasminogen, n Tissue plasminogen activator (t-PA), n Alpha-2 antiplasmin, n Plasminogen activator inhibitor-1 (PAI-1), n Thrombin-activatable fibrinolysis inhibitor (TAFI). n

Normal PT and PTT Thrombocytopenia n v. WD n Factor 13 deficiency n Platelet dysfunction n Vascular purpuras n Psychogenic purpura n

Normal PT and Prolonged a. PTT Hemophilia A n Hemophilia B n Factor XI deficiency n Factor VIII inhibitor n Malignancy, n Clonal lymphoproliferative disorders, n Pregnancy, n Rheumatologic disorders n

Prolonged PT and normal a. PTT Factor VII deficiency n Warfarin therapy n Early liver disease n Early DIC n

Prolonged PT and PTT Vit K deficiency n Liver disease n Warfarin treatment n Acquired inhibitor to factor V n Factor X deficiency- seen in Amyloidosis n DIC n

Acute Promyelocytic Leukemia n n n DIC is often seen at presentation or during treatment Medical Emergency as Cerebral hemorrhage can occur in upto 4% of untreated pts Promyelocytes seen on smear Reciprocal translocation between the long arms of chromosomes 15 and 17, with the creation of a fusion gene, PML/RAR-alpha Immediate initiation of ATRA induces de deifferentiation

Hemophilia A and B are X-linked recessive diseases n Severe disease <1 % factor activity, n Moderate disease- 1 to 5 % n Mild disease >5 % n The most common sites are into joints and muscles and from the gastrointestinal tract n

Treatment The two components to therapy are treatment of active bleeding and inhibitor ablation via immune tolerance induction n Cryoprecipitate has high levels of factor VIII n Porcine Factor VIII n Recombinant human Factor VIII n The choice of factor VIII product usually is based upon safety, purity, and cost. n

Dosing One international unit (IU) of clotting factor is that amount present in 1 m. L of pooled normal plasma n Dose of F VIII (IU) = Weight (kg) x (Desired % increase) x 0. 5 n n Depends on the clinical indication and the presence of inhibitors

von Willebrand’s disease Most common of the inherited bleeding disorders n In 1926, Erik von Willebrand described the first patient with the disease n Von Willebrand factor (VWF) binds to both platelets and endothelial components, forming an adhesive bridge between platelets and vascular subendothelial structures and between adjacent platelets at sites of endothelial injury n

Acquired von Willebrand’s disease n Malignant diseases n n n n n Monoclonal gammopathy of unknown significance Multiple Myeloma Non-Hodgkin's lymphoma Chronic lymphocytic leukemia Waldenstrom's macroglobulinemia Essential thrombocythemia. Polycythemi a vera Chronic myelogenous leukemia Wilms tumor Other carcinomas n Immunologic disorders n n n Other disorders n n n n Systemic lupus erythematosus Other autoimmune diseases Hypothyroidism Ventricular septal defect Aortic stenosis Mitral valve prolapse Gastrointestinal angiodyplasia Uremia Hemoglobinopathies Drugs and other agents n n Valproic acid Antibiotics

Treatment DDAVP n Replacement of v. WF n EACA n Tranexamic acid n Recombinant factor 7 n

Its better to bleed than clot!

Therapies other than factor replacement DDAVP n EACA n Tranexamic Acid n Factor 7 inhibitor- Novoseven n

Liver disease Vs DIC Low factor V levels can be used as evidence for either reduced hepatic synthetic function or increased consumption, as in DIC n Factor VIII is not manufactured by hepatocytes; factor VIII levels are usually normal or increased in liver disease n
- Slides: 46