Bleeding Disorders Dr Somaya Taha Saleem Review of

Bleeding Disorders Dr. Somaya Taha Saleem
Review of Hemostasis Function of : Coagulatory system Platelets Endothelium Fibrinolytic system Thrombosis Bleeding Both (DIC)

HEMOSTASIS DEPENDENT UPON: - Vessel Wall Integrity - Adequate Numbers of Platelets - Proper Functioning Platelets - Adequate Levels of Clotting Factors - Proper Function of Fibrinolytic Pathway
NORMAL CLOTTING Response to vessel injury 1. Vasoconstriction to reduce blood flow 2. Platelet plug formation (von will brand factor binds damaged vessel and platelets) , 3. Activation of clotting cascade with generation of fibrin clot formation 4. Inhibitors: ATIII, protein C & protein S. 5. Fibrinlysis (clot breakdown)

Hemostasis: Vasoconstriction & Plug Formation Figure 16 -12: Platelet plug formation
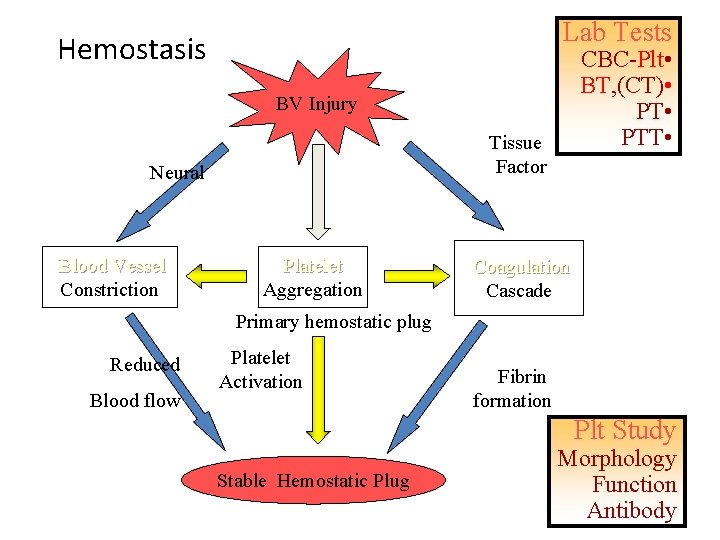
Lab Tests Hemostasis CBC-Plt • BT, (CT) • PTT • BV Injury Tissue Factor Neural Blood Vessel Constriction Platelet Aggregation Coagulation Cascade Primary hemostatic plug Reduced Blood flow Platelet Activation Fibrin formation Plt Study Stable Hemostatic Plug Morphology Function Antibody

Abnormal bleeding , causes : 1 -Vascular disorders 2 - Thrombocytopenia 3 - Defective platelet function or 4 - Defective coagulation The pattern of bleeding is depending on the etiology

Clinical forms of bleeding Mucosal bleeding: epistaxis, bleeding gum, menorrhagia, . . Skin: petechiae, purpura, ecchymosis Deep hematoma: muscle, joints. . Wound bleeding Hematurea, . . .
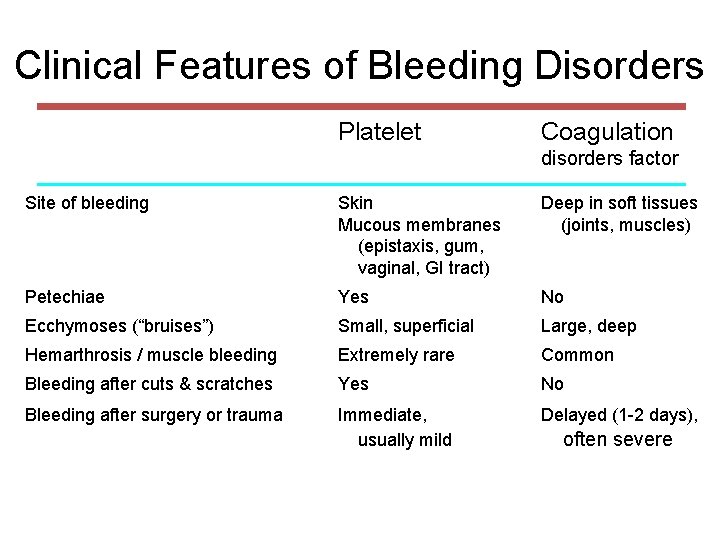
Clinical Features of Bleeding Disorders Platelet Coagulation disorders factor Site of bleeding Skin Mucous membranes (epistaxis, gum, vaginal, GI tract) Deep in soft tissues (joints, muscles) Petechiae Yes No Ecchymoses (“bruises”) Small, superficial Large, deep Hemarthrosis / muscle bleeding Extremely rare Common Bleeding after cuts & scratches Yes No Bleeding after surgery or trauma Immediate, usually mild Delayed (1 -2 days), often severe
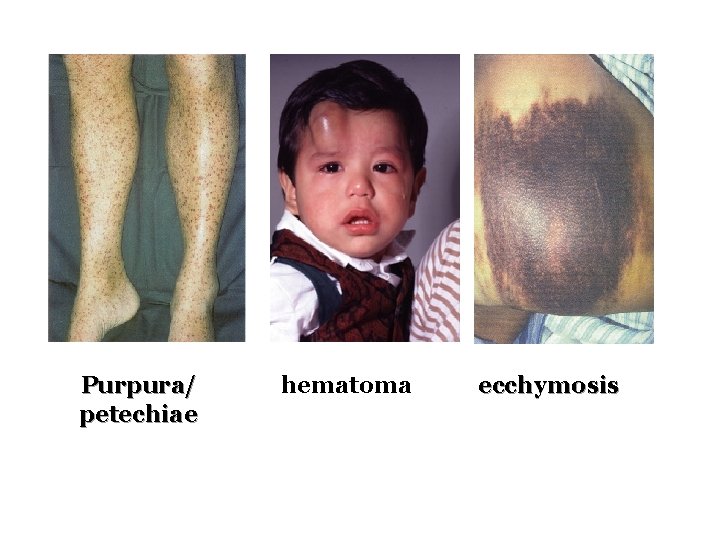
Purpura/ petechiae hematoma ecchymosis

LABORATORY EVALUATION Routine: PLATELET COUNT - BLEEDING TIME (BT), ASSESSMENT OF PLATELET COUNT AND FUNCTION - PROTHROMBIN TIME (PT), Extrinsic Pathway - PARTIAL THROMBOPLASTIN TIME (PTT) , Intrinsic Pathway - THROMBIN TIME (TT), Time for Thrombin To Convert Fibrinogen Fibrin A Measure of Fibrinolytic Pathway Specific Factors assay, plt function tests, . . . •

PLATELET COUNT NORMAL 150, 000 - 450, 000 CELLS/MM 3 • < 100, 000 Thrombocytopenia 50, 000 - 100, 000 Mild Thrombocytopenia < 50, 000 Sever Thrombocytopenia

Bleeding Disorders Causes : Platelets : abnormal number or function Clotting Factor Vessels Quantity Quality
Vascular causes of bleeding Congenital malformations Infections ( viral , bacterial, . . ) Immune vasculitis (Henoch- Schonlen purpura) Vit C deficiency Mucosal/ Bleeding skin Senile purpura. time. .

Clotting Disorders Thrombocytosis and Thrombocytopenia Thrombocytosis An abnormal increase in the number of platelets Thrombocytopenia An abnormal decrease in the number of platelets Sequestration Destruction (ITP) Decreased production.

Coagulatory disorders Congenital Hemophilia A ( factor VIII: C) Hemophilia B (factor IX) Von Willibrand diseases( factor VIII: vw) Acquired Vit K def. Liver diseases Inhibitors DIC

Haemophilia A F VIII deficiency. X linked recessive. Females carriers, males get the disease. Severity: - Mild: >5 - <40% - Moderate: 1 – 5% - Severe: <1%.

Hemophilia A Clinically : Prolonged bleeding after surgery or dental extractions. bleeding after trauma , Haemarthrosis (most common) Soft tissue hematomas (e. g. , muscle) Nerve entrapment Muscle atrophy Shortened tendons

Hemophilia A Lab finding : Normal plt, bleeding time, PT, TT Prolonged APTT Mixing studies and factor assay Gene studies Diagnosis: Isolated prolongation of P. T. T

Management: A-Replacement: 1 -FVIII 2 -Cryoprecipitate. FVIII, fibrinogen, XIII. 3 - FFP (fresh frozen plasma). B- Physiotherapy. C- Patient education: disease, treatment, marriage, psychosocial

Haemophilia B ( F IX deficiency) As Haemophilia A Treatment: F IX concenterate or FFP.
Complications of therapy Formation of inhibitors (antibodies) Viral infections Hepatitis B- Human parvovirus Hepatitis C- Hepatitis A HIV- Others

Von Willibrand disease Autosomal dominant. Both sexes. factor VIII: wv def Both plt and coagulatory disorder Clinically: both mucosal and deep tissue bleeding Lab finding: Normal plt count, abn plt function test Prolonged Bleeding time Normal PT. prolonged APTT
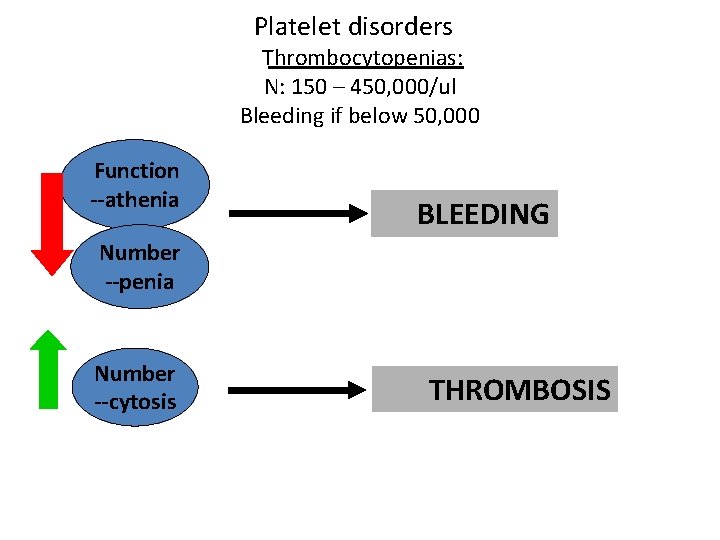
Platelet disorders Thrombocytopenias: N: 150 – 450, 000/ul Bleeding if below 50, 000 Function --athenia BLEEDING Number --penia Number --cytosis THROMBOSIS

Causes: A-Marrow disorder: Aplastic anemia Acute leukaemias Bone marrow infiltrations. B – Peripheral destruction: I. T. P & other immune disorders. Hypersplenism DIC Symptoms: Skin: Purpura, ecchymoses, bruises. mucous membranes: Epistaxis, mouth etc.

thrombocytopenic purpura ITP Immune. Platelet antibodies. Acute: Clinical Haematology: Low Platelets. Bone marrow: Increased megakaryocytes. Treatment: Steroids Observe. Chronic ITP Adults , Less responsive to steroids

Platelet Dysfunction Hereditary or acquired. Platelet type bleeding. Prolonged bleeding time. Abnormal platelet aggregation tests.

Hereditary : A large group. Platelet type bleeding. Normal platelet count. Prolonged BT Acquired: Drugs. Ureamia Myeloproliferative disorders.

Blood transfusions

Blood Products and Blood Typing Blood Types • Antigens – A, B, AB, O • Rh factor – Rh+ = ~85% • Rh- = ~15% •
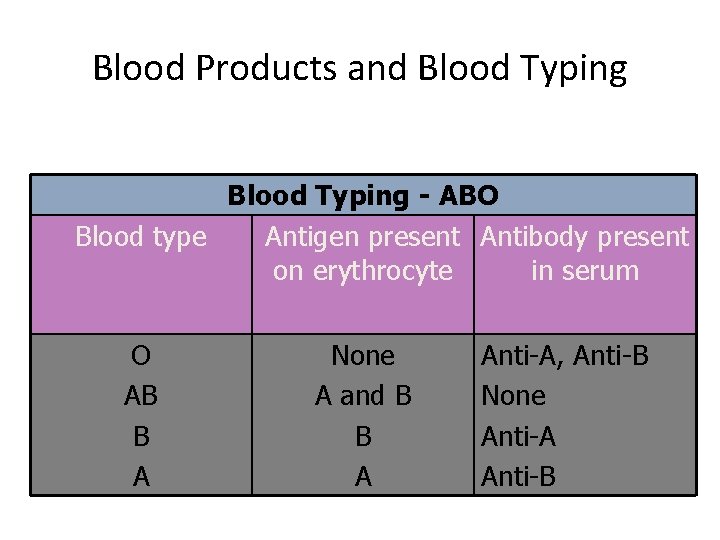
Blood Products and Blood Typing - ABO Blood type Antigen present Antibody present on erythrocyte in serum O AB B A None A and B B A Anti-A, Anti-B None Anti-A Anti-B

Blood Products and Blood Typing Compatibility Among ABO Blood Groups Reaction with serum of Recipient Donor Cells AB B A O - + + + - = no reaction+ = reaction

Donor Selection reject any pt with: Age > 50 yr, Weight < 45 kg. HB < 12. 5 g/dl for female, 13. 5 for male Chronic disease, hypertension, DM …. etc Abortion up to three month P/H of hepatitis B, C, HIV, . previous transfusion for six month pregnancy and three month after delivery

Tests done before BT Blood grouping : (ABO+ Rh) Crosshatching: Microbiology tests: HIV, HBV, HCV, Other viruses: HTLV, CMV VDRL (syphilis)

Blood Products (Components) Whole blood. Packed cells. Platelets. Granulocytes. Fresh frozen plasma. Cryoprecipitate. Factors, plasma proteins.

Patient and donor RBC selection by ABO and Rh type Patient Donor AA, O BB, O AB A, B, AB, O O O Rh(+), Rh(-)

Transfusion Reactions I. Immunologic 1. Alloimmunization 2. Hemolytic transfusion reactions - immediate - delayed 3. Febric transfusions reactions 4. Allergic 5. Immunosuppressive effects 6. Transfusion-related acute lung injury 7. Post-transfusion purpura 8. Graft-versus-host disease

Transfusion Reactions II. Nonimmunologic 1. Volume overload 2. Massive transfusion: metabolic, hypothermia, dilutional, pulmonary microembolism 3. Transfudion hemosiderosis 4. Infections - Hepatitis(A, B, C, , G, other - HIV - CMV - EBV - Bacterial contamination - Malaria - other organisms

Thank you
- Slides: 39