Bladder Management After Spinal Cord Injury Frazier Rehab

Bladder Management After Spinal Cord Injury Frazier Rehab Institute Spinal Cord Medicine Program

Urinary System • Consists of the kidneys, ureters, bladder, sphincters and urethra • Major functions: – Regulates your body’s electrolytes – Removes waste products and excess water (urine)
How Do You Pee? • Your kidneys filter blood to remove waste products & produce urine • Your urine travels through the ureters to the bladder • Your nerves send messages up the spinal cord to the brain when bladder is ready to empty • Your brain then sends a message down the spinal cord to the bladder telling it to empty • Your sphincter muscles relax, your bladder muscles tighten to push urine from the bladder and the urine leaves the body through the urethra

Urination After Spinal Cord Injury • Messages/signals from the bladder to the brain and vice versa become disrupted or lost completely due to the SCI • Bladder becomes dysfunctional (neurogenic) • The level of your spinal cord injury will affect how urination will occur

Neurogenic Bladder Reflexic. Bladder • AKA Spastic bladder • SCI above Lumbar 1 -2 • Reflexes are triggered to urinate but you may not be aware Areflexic. Bladder • AKA Floppy bladder • SCI below Lumbar 1 • There are no reflexes triggering urination • Bladder will become too full, urine may leak and/or back up to kidneys

Bladder Management Goals • Maintain good function of your bladder and kidneys • Develop a realistic management • Prevent complications

Bladder Management Programs Options may include: • • • Intermittent catheterization (IC or CIC) Indwelling or Suprapubiccatheter External (condom) catheter Manual techniques to trigger voiding Behavioral strategies Medications/Surgeries

Intermittent Catheterization (IC or CIC) • AKA “in & out” catheterization • Preferred method • Catheter is inserted into the bladder, drains the urine then the catheter is removed • Performed every 4 -6 hours – Timing varies depending on fluid intake – Each IC should be less than 500 cc

Catheters • Many different kinds of catheters available • Options dependent on insurance • Briefs can be purchased at local stores or off the Internet – Not covered under insurance

Straight Catheters

Closed System Catheters

Male Coude’ Caths
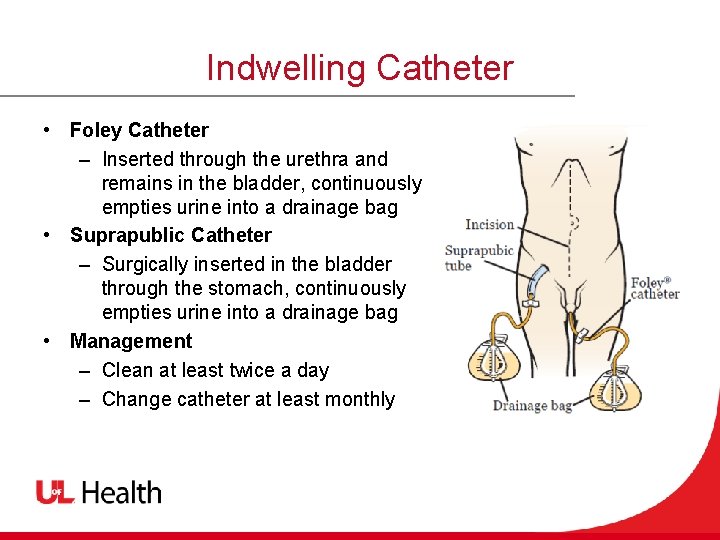
Indwelling Catheter • Foley Catheter – Inserted through the urethra and remains in the bladder, continuously empties urine into a drainage bag • Suprapublic Catheter – Surgically inserted in the bladder through the stomach, continuously empties urine into a drainage bag • Management – Clean at least twice a day – Change catheter at least monthly

External Catheters - Males • AKA Texas or condom catheters • Beneficial for males who experience spontaneous voiding – No external options for females due to anatomy • Fits over the penis and connects to drainage bag to keep you dry • Adhesive on the condom catheter holds it in place – Must be careful when removing to avoid skin breakdown

Other Techniques Manual Technique • Triggers sphincter relaxation = involuntary bladder contraction to cause voiding – Suprapubic tapping – Thigh scratching – Anal/Rectal manipulation • Increase abdominal pressure = causes voiding – Valsalva – Crede’ • Risks – AD – Recurrent UTI – Kidney or bladder stones – Deterioration of bladder or kidney functions Behavioral Strategies • Timed voiding • Pelvic muscle exercises – Kegel

Surgical Procedures • Mitrofanoff – Surgical procedure to construct a new passageway for urine using the appendix – Allows a catheter to be passed through the abdomen and directly into bladder • Bladder Augmentation – Surgical enlargement of bladder – Reduces need for frequent catheterization

Medications for Bladder Management • Help prevent bladder spasms to promote storage – Oxybutinin – Trospium – Myrbetriq – Botuliunumtoxin (Botox) • Helps promote emptying – Flomax – Bethanechol

Urinary Tract Infection (UTI) • Bacteria that multiplies in the urinary tract and can cause an infection

Signs & Symptoms of UTI • • • Cloudy and/or foul smelling urine Increase in mucous or sediment Increase in bladder or general spasms Pain or burning with urination Increase in frequency or incontinence Low back or flank pain Blood in urine Elevated temp/fever or chills Nausea/vomiting Just not feeling well

UTI • Asymptomatic – Not a true infection – Colonization – Presence of odor or cloudiness alone not an indicator • Symptomatic – – – Increased spasms Incontinence Fever Feeling poorly AD

Detection & Treatment of UTI • Call MD if you suspect UTI • May need urine specimen (UA C&S) to determine if true infection • Treatment may include use of antibiotics

Ways to Prevent UTI • Proper fluid intake – 2 L daily • Routine bladder emptying – Be consistent with bladder management – Keep volumes below 500 cc • Good hygiene • Proper positioning and draining of collection device (leg bag/bedside drainage bags) • Daily cleaning of drainage devices and proper cleaning of catheters • Medications • Follow up with Urology

Conclusion • It may take time and effort, but proper bladder management can be achieved in those with a spinal cord injury • Try to keep a healthy urinary system by staying educated, sticking to a regimen and using preventative measures • Follow the recommendations of your healthcare providers

References • Paralyzed Veterans of America. (2019, February). Retrieved from Bladder Management Following Spinal Cord Injury: What You Should Know: https: //www. pva. org • Urologic Management and Renal Disease in Spinal Cord Injury. (2018). In S. Kirshblum, & V. W. Lin, Spinal Cord Medicine (pp. 332 -386). Demos Medical; 3 edition.
- Slides: 24