Birth injuries Birth traumas Definition Birth injury refers

Birth injuries ((Birth traumas))

Definition: Birth injury refers to both avoidable and unavoidable mechanical and hypoxic-ischemic injuries to the fetus during birth process. Predisposing factors: 1. Inappropriate or deficit medical skills or attentions. 2. Macrosomia (large size baby). 3. Prematurity. 4. Cephalopelvic disproportion. 5. Dystocia. 6. Prolonged labor. 7. Breech presentation.
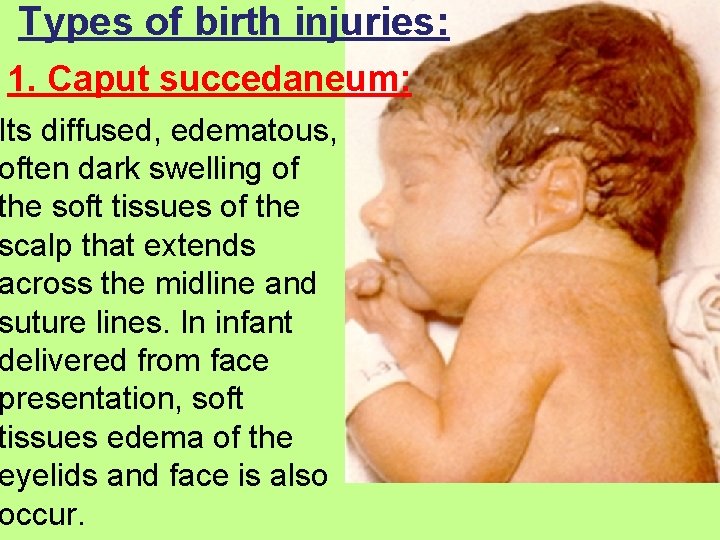
Types of birth injuries: 1. Caput succedaneum: Its diffused, edematous, often dark swelling of the soft tissues of the scalp that extends across the midline and suture lines. In infant delivered from face presentation, soft tissues edema of the eyelids and face is also occur.

C. succedaneum may be seen after prolonged labor in both full-term and premature infants. Molding of the head often associated with C. succedaneum and is the result of pressure induced from overriding the parietal and frontal bones against their respective sutures. The C. succedaneums usually disappear within 1 st few days of life.
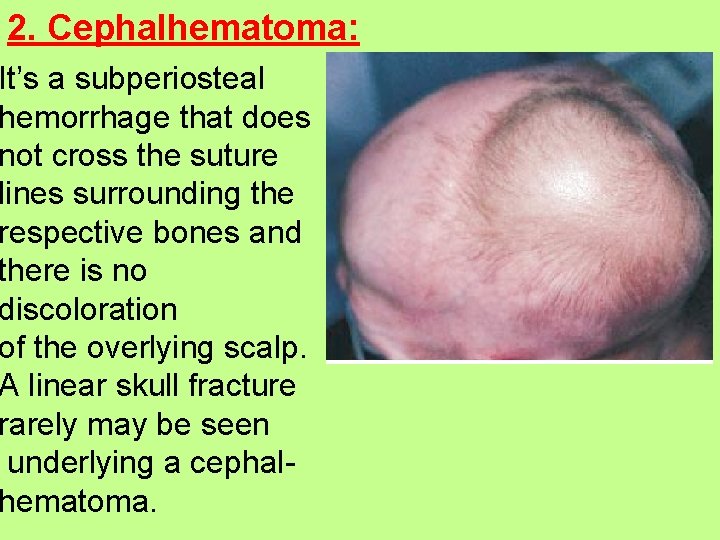
2. Cephalhematoma: It’s a subperiosteal hemorrhage that does not cross the suture lines surrounding the respective bones and there is no discoloration of the overlying scalp. A linear skull fracture rarely may be seen underlying a cephalhematoma.

Most cephalhematomas are resolved within 2 wk-3 mo depending on their sizes, and with time, its may organize, calcify and form a central depression. Treatment of C. succedaneum and cephalhematoma: both are required no specific treatments and they are resolved spontaneously, but rarely they might be sever enough to cause shock and hyperbilirubinemia required treatment with phototherapy especially in premature infants.
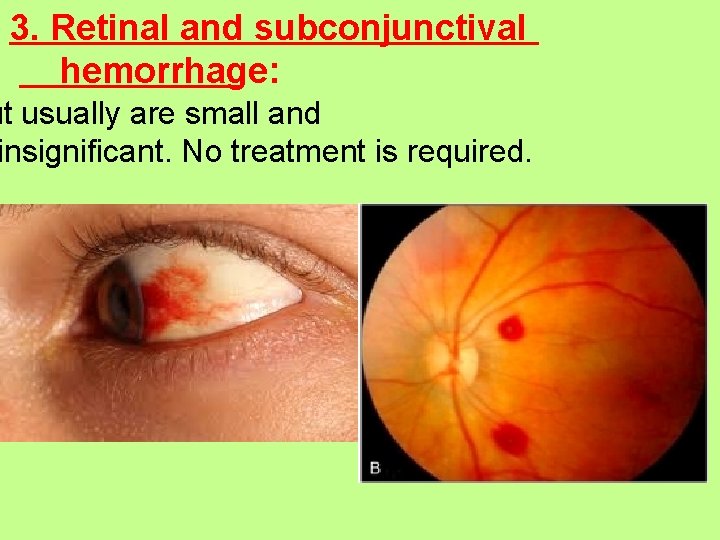
3. Retinal and subconjunctival hemorrhage: ut usually are small and insignificant. No treatment is required.

4. Spinal cord or spine injuries: occurs in infants following excessive rotational (at C 3 -4) or longitudinal (at C 7 -T 1) force transmitted to the neck during vertex or breech presentations. Fractures of vertebrae are rare and may cause direct damage to the spinal cord that results in transaction and permanent sequelae or hemorrhage, edema, and neurological signs (complete flaccid paralysis, absent deep tendon reflexes, absence of response to painful stimuli), in addition to apnea and asphyxia.
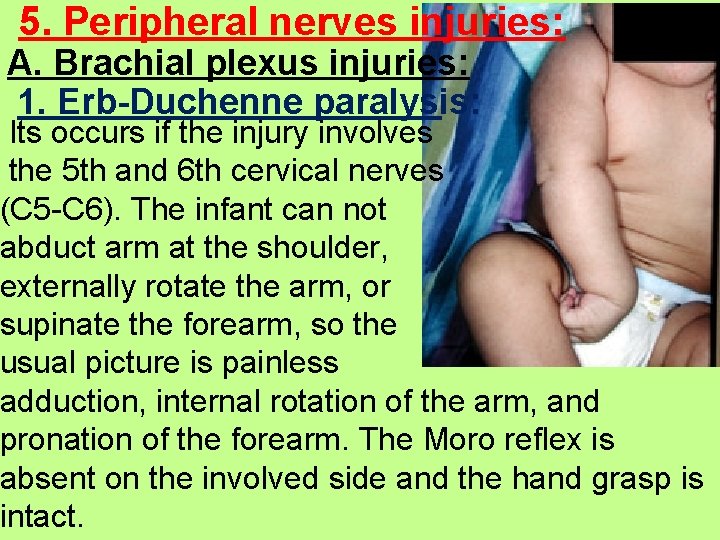
5. Peripheral nerves injuries: A. Brachial plexus injuries: 1. Erb-Duchenne paralysis: Its occurs if the injury involves the 5 th and 6 th cervical nerves (C 5 -C 6). The infant can not abduct arm at the shoulder, externally rotate the arm, or supinate the forearm, so the usual picture is painless adduction, internal rotation of the arm, and pronation of the forearm. The Moro reflex is absent on the involved side and the hand grasp is intact.
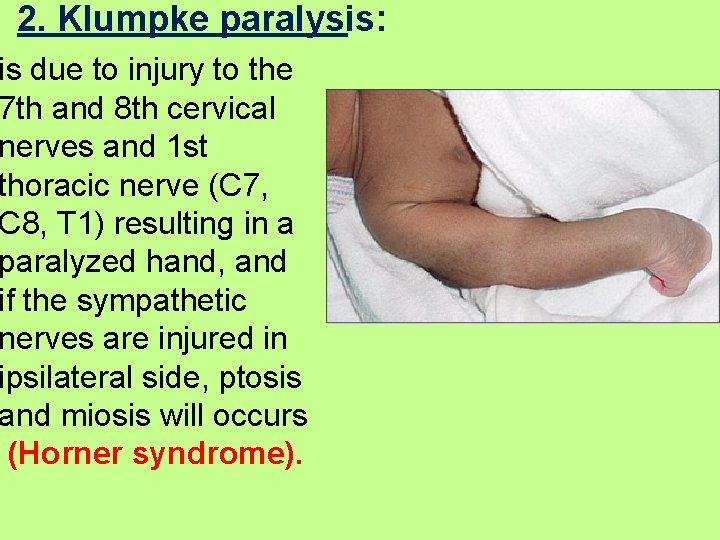
2. Klumpke paralysis: is due to injury to the 7 th and 8 th cervical nerves and 1 st thoracic nerve (C 7, C 8, T 1) resulting in a paralyzed hand, and if the sympathetic nerves are injured in ipsilateral side, ptosis and miosis will occurs (Horner syndrome).

Treatment of Erb-Duchenne and Klumpke paralysis: 1. Positioning to avoid contractures. 2. Active and passive range of motion exercises. 3. If the deficit persists, nerve grafting may be of benefit. 3. Phrenic nerve palsy: It's due to injury to the 3 rd, 4 th, and 5 th cervical nerves (C 3, C 4, and C 5) resulting in diaphragmatic paralysis and respiratory distress.

B. Facial nerve injury: Is due to compression of the 7 th cranial nerve between the facial bone and the mother's pelvic bones or the physician's forceps. This peripheral nerve injury characterized by asymmetric crying face in which the normal side moves normally including the forehead, while the affected side is flaccid, the eye does not close, absent nasolabial fold, and the side of moth droops at rest. When there is a central injury to the facial nerve, only the lower two thirds of the face (not the forehead) is involved.

6. Fractures injuries: A. Cranial bones fractures: Are rare, usually linear, and require no treatment other than observation for very rare delayed (1 -3 mo) complications (e. g. liptomeningeal cyst). Depressed skull fractures are unusual but may be seen with complicated forceps delivery.

B. Fractures of the clavicle: usually are unilateral and are noted in macrosomic infants following shoulder dystocia. Infant presents with asymmetric Moro reflex (no response in affected side) and decrease movements of the affected side. The prognosis is excellent; many infants require no treatment or a simple figure-of-eight bandage to immobilize the bone.

C. Extremity fractures: are less common than clvicular fractures and nvolve the humerus more often than femur. Treatment by immobilization and a triangular splint bandage for the humerus fractures and traction suspension of the leg for femoral fractures. The prognosis is excellent.

D. facial bones fractures: are rare, but dislocation of the cartilaginous part of the nasal septum is common which might causing feeding difficulty, respiratory distress, asymmetric nares, and flattened laterally displaced nose. Treatment by reduction of the dislocation by elevating the cartilage back into the vomeral groove.

7. Visceral traumas: Traumas to liver, spleen, or adrenal glands are noted in macrosomic infants and in very premature infants, with or without breech or vaginal delivery. Rupture of liver with subcapsular hematoma formation may result in anemia, hypovolemia, shock, hemoperitoneum, and DIC. Adrenal hemorrhage may be asymptomatic, as noted by a high incidence of normal infants with calcified adrenal glands, but sever adrenal hemorrhage may present with a flank mass, jaundice, and hematuria, with or without shock.

Intracranial hemorrhage: 1. Subdural hemorrhage & hematoma: Its occurs in association with birth trauma, cephalo-pelvic disproportion, forceps delivery, large for GA infants, post natal head trauma, and inherited coagulation defects e. g. hemophilia. Clinical features: anemia, vomiting, seizures, and hydrocephalus which may occur in infant at age of 1 -2 mo. Treatment: of all subdural hematomas is surgical evacuation.

2. Subarachnoid hemorrhage: Its may spontaneous or associated with hypoxia or due to bleeding from cerebral arteriovenous malformation. Clinical features: Seizures are common presenting manifestation, with rare post hemorrhagic hydrocephalus. Treatment: directed at seizures and hydrocephalus.

3. Periventricular and intraventricular hemorrhage (IVH): They are common among VLBW and the risk decreases with increasing gestational age. Up to 50% of infants under 1500 gm weight have evidence of intracranial Hge. Pathogenesis: is unknown (they usually are not due to coagulation disorders), but the initial site of bleeding may be the weak blood vessels in the periventricular germinal matrix.

Clinical features: most of periventricular and IVH occurs in the first 3 days of life, its unusual for IVH to occur after the 5 th day of life. The clinical manifestations include seizures, apnea, bradycardia, lethargy, coma, hypotension, metabolic acidosis, anemia not corrected by blood transfusion, bulging fontanel and cutaneous mottling.

Diagnosis of IVH: The diagnosis is confirmed and the severity graded by ultrasonographic examination through Grade I: Bleeding is confined to the germinal matrix. Grade II: Blood noted in the ventricles without ventricular enlargement. Grade III: Ventricular dilatation (enlargement). Grade IV: Blood in the dilated ventricles and in the cerebral cortex.

Grade I & II are asymptomatic, while grade III & IV are symptomatic, and grade IV have poor prognosis and rapidly progress to shock and coma. Treatment: Is supportive, including: 1. Ventilation for apnea. 2. Blood transfusion for shock. 3. Correction of metabolic acidosis. Treatment of post hemorrhagic hydrocephalus aily lumbar punctures or by ventricular-peritoneal shunt.
- Slides: 23