Bipolar Disorder in Children and Adolescents Some Tips

Bipolar Disorder in Children and Adolescents: Some Tips for Parents and Other Caregivers David J. Miklowitz, Ph. D. Professor of Psychiatry Division of Child and Adolescent Psychiatry UCLA Semel Institute and Department of Psychiatry, Oxford University Child and Adolescent Mood Disorders Clinic www. semel. ucla. edu/champ (310) 825 -2836

Upon Hearing the Diagnosis of Bipolar Disorder… “The endless questioning finally ended. My psychiatrist looked at me, there was no uncertainty in his voice. “Manic-depressive illness. ” I admired his bluntness. I wished him locusts on his lands and a pox upon his house. Silent, unbelievable rage. I smiled pleasantly. He smiled back. The war had just begun. ” --Kay Redfield Jamison “An Unquiet Mind” (1993)

Thirty Years of research on bipolar disorder has taught me that….

managing bipolar disorder is more than just taking medicines.

Pediatric (under age 18) Bipolar Disorder w About 2% prevalence across nations 1 w At risk for the 4 S’s 2: w School problems w Substance abuse w Suicide w Social dysfunction w High rate of familial transmission 3, 4 w Stronger genetic load in youth than in adults 4 w Early onset = poor prognosis 5 Van Meter et al. , J Clin Psychiatry 2011; 2 Goldberg et al. , J Nerv Ment Dis. , 2004; 3 Goodwin and Jamison, Manic-Depressive Illness, 1997; 4 Faraone et al. , Biological Psychiatry, 2003; 5 Leverich GS et al. (2007), J Pediatr 150(5): 485 -490 1

A 10 -year Old Girl’s Description of Bipolar Disorder “When I feel happy, I get real bouncy… I’m hopping all over the place, and my mind seems to be focused on one thing for a short time. Sometimes, I don’t necessarily feel bouncy, just kind of light and airy, like a butterfly. I sort of flit and float from place to place, physically and in my mind. When I feel depressed, I’m like…dead. I just sit there lifelessly, and my body just sort of flops around, like a Beanie Baby. Also, my mind just sort of drifts away and wanders aimlessly into space. ” Birmaher, B. 2004. Course and outcome of bipolar disorder in youth (COBY). NIMH Pediatric Bipolar Disorders conference, Washington DC.

The 8 Family and Self-Care Principles for Managing Bipolar Disorder 1. 2. 3. 4. 5. 6. 7. 8. Monitor moods daily – know about early warning signs Recognize and manage stress triggers Stabilize sleep/wake rhythms Know your position on medications Develop a mania prevention plan Work on family communication and problem-solving Obtain reasonable accommodations at school or work Get regular therapy or join a support group From: Miklowitz DJ (2011). The Bipolar Disorder Survival Guide, 2 nd Ed

Principle #1 Monitor moods and know your child’s early warning signs
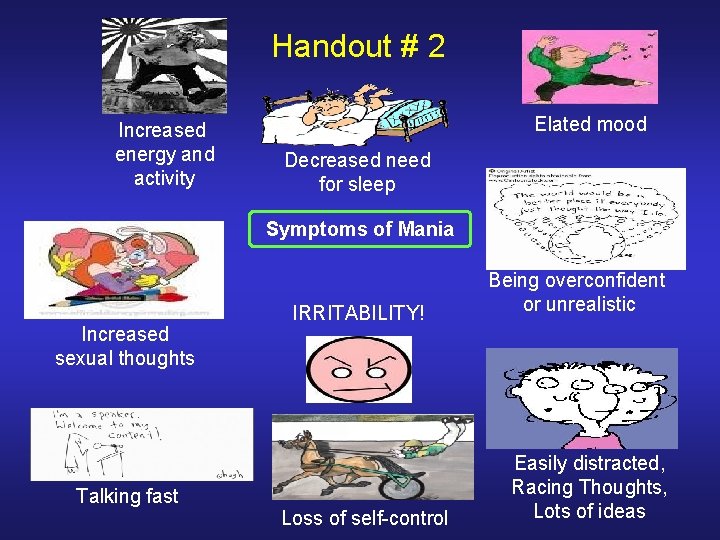
Handout # 2 Increased energy and activity Elated mood Decreased need for sleep Symptoms of Mania Increased sexual thoughts Talking fast IRRITABILITY! Loss of self-control Being overconfident or unrealistic Easily distracted, Racing Thoughts, Lots of ideas

Handout # 2 b Low mood or sadness Tearfulness Low self-esteem Trouble concentrating Increase or Decrease in Appetite Crave Sweets or Carbohydrates Symptoms of Depression Some people also: • feel really tired or low in energy • wish they weren’t alive • feel worthless or guilty • talk or move slowly • lack of thoughts Sleeping too much or too little Loss of interest in activities/boredom

Daily monitoring of mood symptoms w Keep a daily mood chart w “This is one of the things you can do in addition to taking medications to gain more control of your moods” w How are your (your child’s) moods affected by stress, alcohol, medications?



Best Bipolar Apps w i. Mood. Journal w e. Moods w T 2 Mood Tracker w Moody Me w i. Mind & Mood w Mood. Track

Principle #2 w Recognize your stress triggers

Examples of Stress for Kids w Loss of a loved one w Family conflicts (between kid and sibling or parent; between parents) w High familial criticism w Beginning of school year w Events that change sleep cycles w Bullying/peer problems
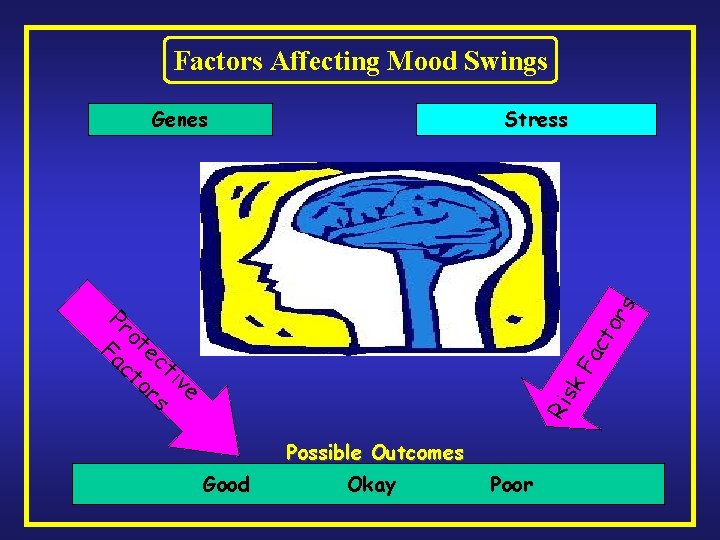
Factors Affecting Mood Swings Genes Stress Ris k. F ac to r s Pr ot Fa ec ct ti or ve s Possible Outcomes Good Okay Poor

Managing Stress: The 3 -Minute Breathing Space w Sit in comfortable chair with your back upright w Close eyes or stare at an object. For 60 seconds, be aware of noises in the room – acknowledge each sensation, thought, or feeling, whether pleasant or unpleasant w For 60 seconds, focus on in-breath and out-breath; if attention shifts, gently escort yourself back to your breathing w For 60 seconds, shift your attention to your entire body – notice posture and sensations in different parts of the body as you breathe in and out w Slowly open your eyes and come back in contact with the room Source: Segal, Williams, & Teasdale, 2001; Mindfulness-based cognitive therapy for depression. NY: Guilford

Principle #3 w Stabilize your sleep/wake rhythms

Good Sleep Hygiene w Establish a regular bedtime and wake time w Vary a maximum of 1 hour/day w Avoid “sleep bingeing” on weekends w Separate kid from cell phone/IPAD, etc. w Avoid caffeine and other stimulants at night w Avoid alcohol, illicit drugs, or activating over-the-counter medications w Exercise early in the day, not right before bed w Avoid working in bedroom before bed w When traveling, normalize sleep/wake rhythms as soon as possible

Principle #4 w Know your position on medications
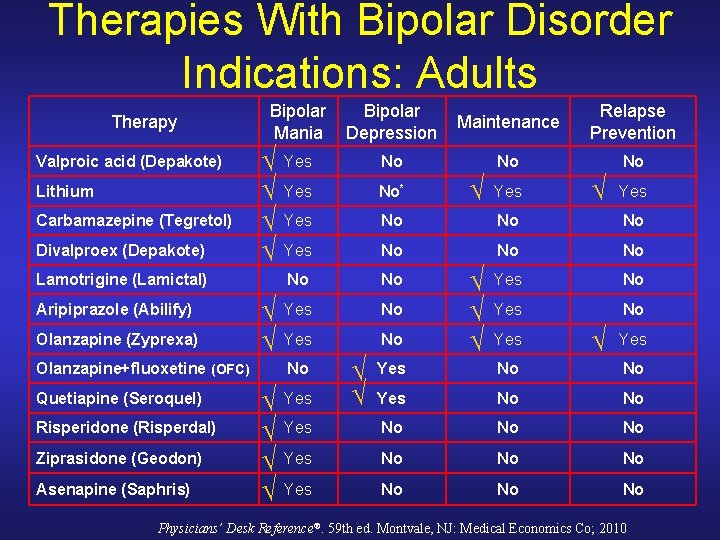
Therapies With Bipolar Disorder Indications: Adults Therapy Bipolar Mania Bipolar Depression Maintenance Relapse Prevention No No No Divalproex (Depakote) √ Yes Lamotrigine (Lamictal) No No √ Yes No Valproic acid (Depakote) Lithium Carbamazepine (Tegretol) Aripiprazole (Abilify) Olanzapine (Zyprexa) Olanzapine+fluoxetine (OFC) Quetiapine (Seroquel) Risperidone (Risperdal) Ziprasidone (Geodon) Asenapine (Saphris) No √ Yes No* Yes √ Yes No No No Yes No No √ √ √ Yes No No Yes No No No Physicians’ Desk Reference®. 59 th ed. Montvale, NJ: Medical Economics Co; 2010
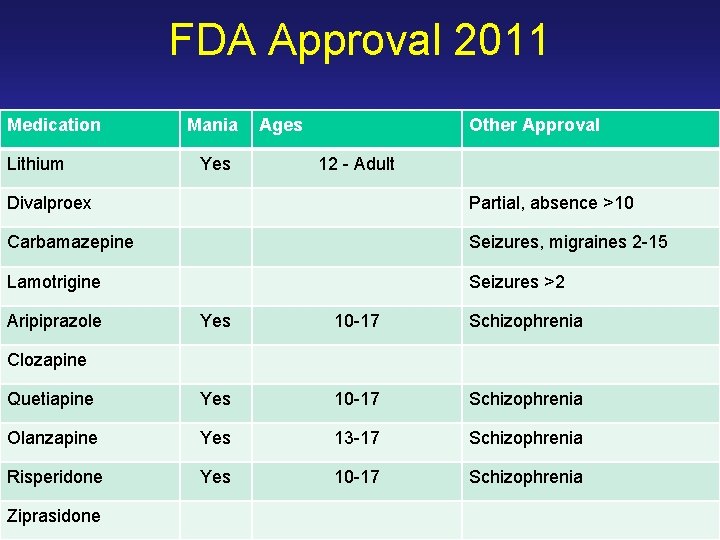
FDA Approval 2011 Medication Lithium Mania Yes Ages Other Approval 12 - Adult Divalproex Partial, absence >10 Carbamazepine Seizures, migraines 2 -15 Lamotrigine Seizures >2 Aripiprazole Yes 10 -17 Schizophrenia Quetiapine Yes 10 -17 Schizophrenia Olanzapine Yes 13 -17 Schizophrenia Risperidone Yes 10 -17 Schizophrenia Clozapine Ziprasidone

Troubleshooting Medication Adherence w Discuss side effects with doctor w Develop strategies for pill storage and use w Role of medications in family: w Does kid feel she’s taking meds for herrself or others? w Pressures from family members to discontinue medications? w What is the symbolic significance of taking medications (loss of creativity? Giving up emotions)? w “Grieving over the lost healthy self” 1 Miklowitz 2 Frank DJ & Goldstein MJ. Bipolar Disorder: A Family-Focused Treatment Approach. NY: Guilford Press, 1997. E, et al. Biol Psychiatry 48(6): 593 -604, 2000.

Who Should be in Charge of My Child’s/Teen’s Medications? w If kid is to take responsibility, he or she must buy into the diagnosis and treatment plan w The kid must be cognitively able to handle the dosing requirements w Issue of boundaries - is kid more or less likely to take meds. if parents take a directive role? w Older kids are more likely to be able to take responsibility than younger kids w Make sure that medications do not become the battleground in which autonomy battles are fought

Principle #5 w Develop a mania prevention plan

The Mania Prevention Contract w List prodromal signs w List circumstances in which, historically, these have been most likely to occur w What can you do? w What can your spouse/parents/siblings do? w The psychiatrist? Therapist? w Have all emergency contact info in one place 27

Handout #11 Prevention Action Plan Stressors or Triggers 1 2 3 4 5 6 7 8 9 10 Early Warning Signs Coping Skills Overcoming Obstacles

Things to do to Reduce Chances of Mania w Contact physician for medication change w Avoid driving w leave credit cards at home w Take someone who you trust along with you when going out at night w For life decisions: use the 2 -person rule and the 48 hr rule

Relapse Prevention Plan for Phil, age 17 Early Warning Signs • Sleeps less, gets up more during night • Gets irritable, cranky, reacts to everything • Obsessed with video games and pornography websites • Talks loudly about elaborate money-making schemes Recent Stressful Events • Family conflict (ongoing) • Fired from job (1 month ago) • Dog died (2 months ago) Coping Strategies • Contact Dr. Benson for medication check • Try to have the same bedtime as rest of the family • Talk about family problems with Pete (brother) • Stay away from friends who make me want to smoke weed

Principle #6 w Work on communication and problemsolving
A mother’s perspective…. “That’s me on that string…my son is like a big baby puppeteer, keeping us all on a string with his vicious mood swings. Worst of all he seems delighted that he can do it. ”

Five Stages of Parental Acceptance of Bipolar Disorder in an Offspring 1. “It’s just growing pains” 2. “I’m going to put my foot down” 3. “Tough love” 4. “It’s just a brain disorder” 5. Achieving balance between accepting the disorder and not letting it rule one’s life

How Can The Family Help? • Help child get treatment and support services (e. g. , IEP) • Support use of medication • Maintain tolerant and calm home atmosphere (What behavior is controllable and what isn’t)? • Have fair expectations for performance after an episode • Make sure the needs of healthy siblings are recognized • Keep regular family routines • Maintain“substance-free homes” • Know your own limits

The Four Basic Communication Skills • Expressing Positive Feelings • Active Listening • Making Positive Requests for Change • Expressing Negative Feelings about Specific Behaviors

Active Listening • Look at the Speaker • Attend to What is Said • Nod Head, Say “Uh-Huh” • Ask Clarifying Questions • Check Out What You Heard

Making a Positive Request • Look at the Person • Say Exactly What You Would Like Him or Her to Do • Tell Him or Her How You Would Feel When S/He Did That • In Making Positive Requests, Use Phrases Like: • “I would like you to _____. ” • “I would really appreciate it if you would _____. ” • “It’s very important to me that you help me with _____. ”

Principle #7 w Obtain “reasonable accommodations” at school

Reasonable Accommodations in the School Setting w Develop an IEP plus monitor follow-up w Help teachers distinguish bipolar disorder from ADHD w Develop plan to manage behavioral problems w Allow later starts to the school day w Allow more frequent breaks, time outs w Have “escape hatches” for child during periods of escalation (e. g. , in-school counseling) w Reducing overstimulation in classroom w Excused absences for medical appointments w Alternative school environments Note: make sure kid is on board with changes!

Disclosure and Stigma: How Much Should We Tell Others About What’s Going On? w What’s the purpose of the disclosure? What do you expect to achieve? w Who should be told – teacher, friends’ parents? What do you want them to do with the information? w Is purpose of disclosure primarily to alleviate your own distress? If so, consider support group as alternative setting

Principle #8 w Get regular therapy or join a support group w Should have a “psychoeducational” focus w Weekly or biweekly is optimal

Family-Focused Therapy (FFT)

Family-Focused Treatment (FFT) of Bipolar Disorder w w 12 outpatient sessions over 4 months Assessment of patient and family Engagement phase Psychoeducation about bipolar disorder (symptoms, early recognition, etiology, treatment, selfmanagement) w Communication enhancement training (behavioral rehearsal of effective speaking and listening strategies) w Problem-solving skills training Miklowitz DJ. The Bipolar Disorder Survival Guide: What You and Your Family Need to Know. Second Edition. New York, NY: The Guilford Press; 2010.
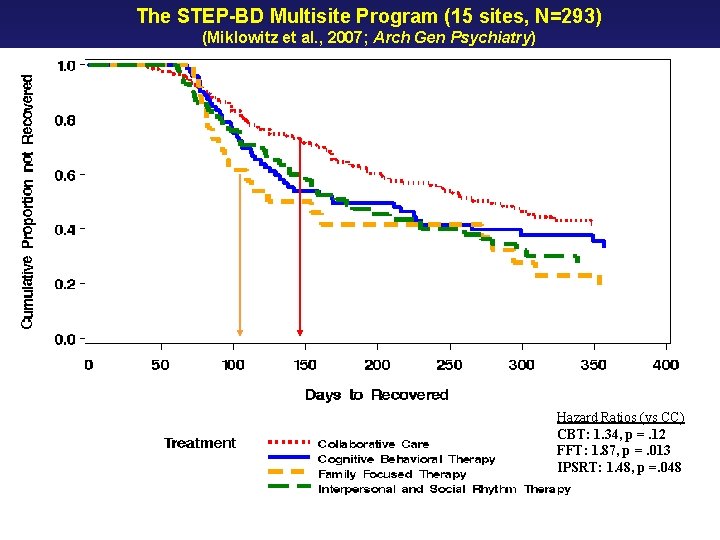
The STEP-BD Multisite Program (15 sites, N=293) (Miklowitz et al. , 2007; Arch Gen Psychiatry) 2(3) = 8. 02, p = 0. 046 Hazard Ratios (vs CC) CBT: 1. 34, p =. 12 FFT: 1. 87, p =. 013 IPSRT: 1. 48, p =. 048
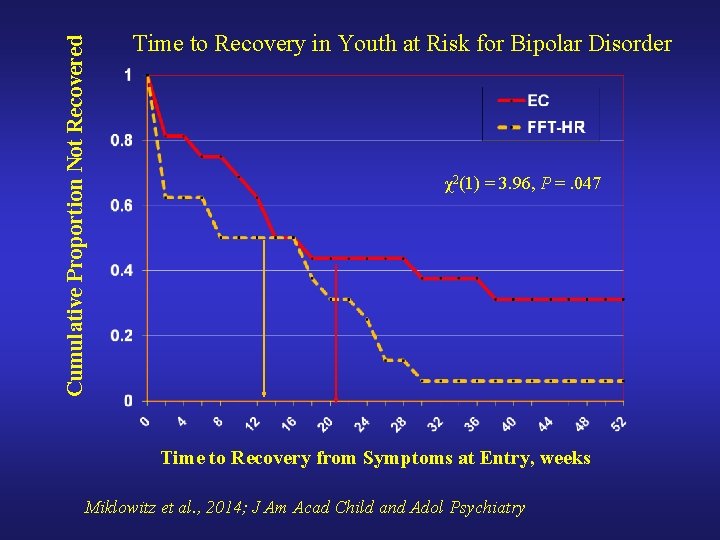
Cumulative Proportion Not Recovered Time to Recovery in Youth at Risk for Bipolar Disorder χ2(1) = 3. 96, P =. 047 Time to Recovery from Symptoms at Entry, weeks Miklowitz et al. , 2014; J Am Acad Child and Adol Psychiatry

I cannot imagine leading a normal life without both taking lithium and having had the benefits of psychotherapy…ineffably, psychotherapy heals. It makes some sense of the confusion, reigns in the terrifying thoughts and feelings, returns some control and hope and possibility of learning from it all…It is where I have believed – or have learned to believe – that I might someday be able to contend with all of this. ” -Kay Jamison, Ph. D. , An Unquiet Mind, 1995

Summary: The 8 Self-Care Principles 1. 2. 3. 4. 5. 6. 7. 8. Monitor moods daily – know about early warning signs Recognize and manage stress triggers Stabilize sleep/wake rhythms Know your position on medications Develop a mania prevention plan Work on family communication and problem-solving Obtain reasonable accommodations at school or work Get regular therapy or join a support group From: Miklowitz DJ (2011). The Bipolar Disorder Survival Guide, 2 nd Ed



UCLA Child and Adolescent Mood Disorders Program (CHAMP) www. semel. ucla. edu/champ (310) 825 -2836
- Slides: 50