BIPOLAR DISORDER Alison C Lynch MD MS April

BIPOLAR DISORDER Alison C. Lynch MD MS April 19, 2017

• No disclosures
Objectives—Bipolar disorder • Overview of bipolar disorder • Diagnosis • Identification • Treatment • Cases to illustrate common issues • Is it bipolar disorder? • Pregnancy • Chronic conditions • Starting meds • Urgencies/emergencies

Bipolar disorder is common • ~2. 6% of US population (5. 7 million Americans) • Sixth leading cause of disability worldwide • Average of onset is 25 years old • About 2/3 of people with bipolar disorder have at least one close relative with bipolar disorder or major depression • Gender distribution ~1: 1

Bipolar disorder causes serious problems • People with bipolar disorder experience severe mood swings that impair their daily life and negatively affect their relationships
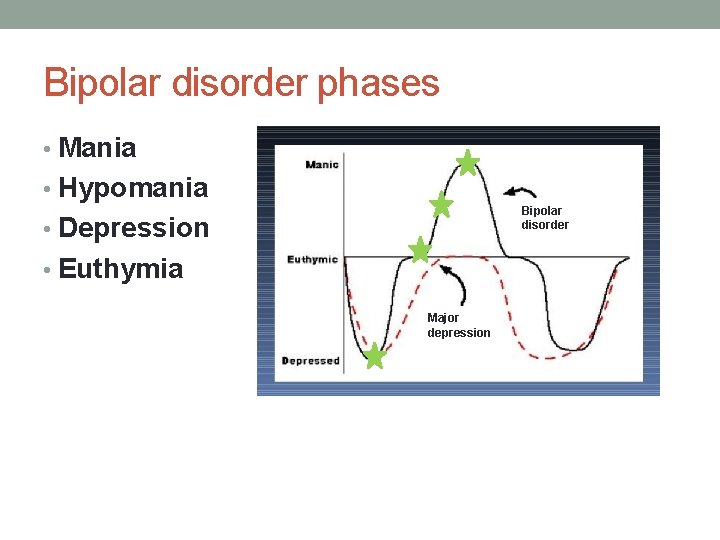
Bipolar disorder phases • Mania • Hypomania Bipolar disorder • Depression • Euthymia Major depression

Types of bipolar disorder • Type I: at least 1 episode of mania (+/- depression) • Type II: hypomania + depression • Rapid cycling: at least 4 episodes of depression, mania, or both in 1 year • Mixed features: features of mania and depression simultaneously

Bipolar disorder is often missed • Especially bipolar II • Can look like depression, as people are more likely to seek care for this problem than for mania/hypomania • 20 -40% of people diagnosed with MDD have a bipolar illness • Treatment resistant depression? • We are still trying to understand how frequently TRD is actually bipolar • About half of people with bipolar disorder are getting treatment for it an any given time

Recognizing bipolar disorder • Consider bipolar in people with depression (in particular those who have not responded to antidepressant treatment) • Ask about history of mania or hypomania symptoms • Ask about family history of bipolar disorder • Screen with the Mood Disorders Questionnaire (MDQ)
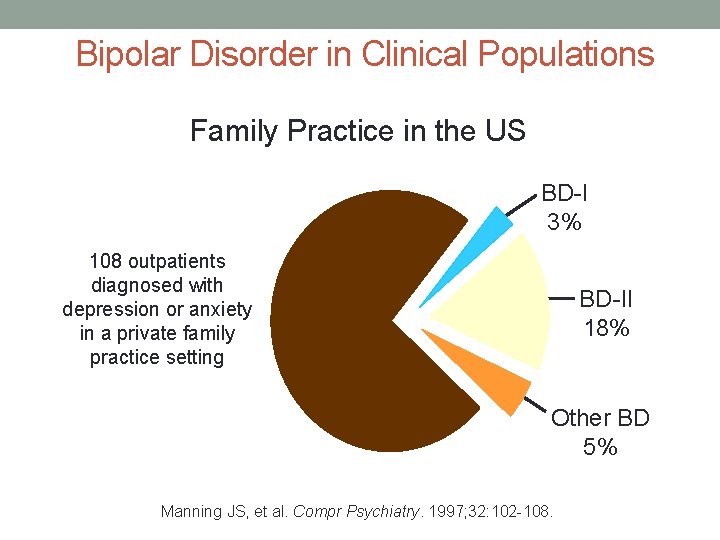
Bipolar Disorder in Clinical Populations Family Practice in the US BD-I 3% 108 outpatients diagnosed with depression or anxiety in a private family practice setting BD-II 18% Other BD 5% Manning JS, et al. Compr Psychiatry. 1997; 32: 102 -108.

http: //www. integration. samhsa. gov/images/res/MDQ. pdf
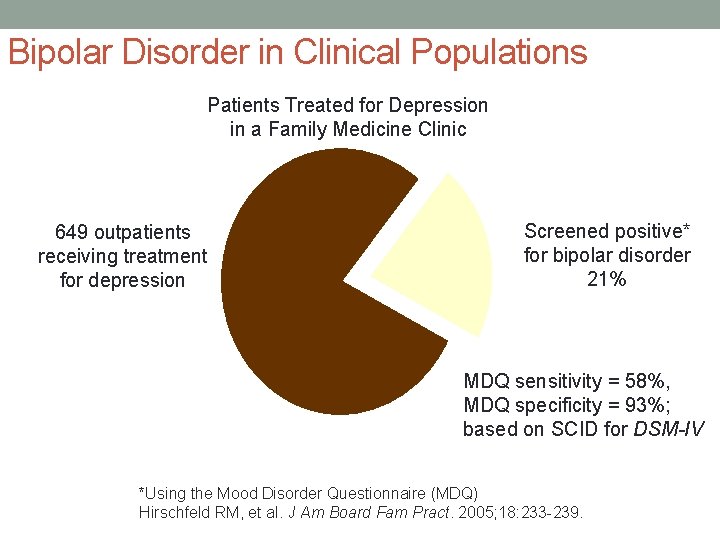
Bipolar Disorder in Clinical Populations Patients Treated for Depression in a Family Medicine Clinic 649 outpatients receiving treatment for depression Screened positive* for bipolar disorder 21% MDQ sensitivity = 58%, MDQ specificity = 93%; based on SCID for DSM-IV *Using the Mood Disorder Questionnaire (MDQ) Hirschfeld RM, et al. J Am Board Fam Pract. 2005; 18: 233 -239.


Is it bipolar or is it borderline? • BPAD • Borderline PD • Episodes of mania or • Longstanding pattern of swings: • moods, • relationships, • self-image, and • behavior • Mood cycles can fluctuate • • depression lasting days to weeks More physical and mental energy and activity than normal Racing thoughts and ideas Talking more and faster Making big plans Risk taking Impulsiveness (substance abuse, sex, spending, etc. ) Less sleep, but no feeling of being tired • • throughout the day Overly strong emotional responses to upsetting life events Often try to hurt themselves Often have chaotic relationships with people History of trauma as a child is more common

Treatment is beneficial • Lithium • Reduces relapse (prophylaxis) • Reduces suicides • Improves the course of the illness • May lower risk of dementia in people with bipolar • Treatment in general • Reduces suicide rate • Reduces mortality risk from chronic disease

FDA-Indicated Treatments • Acute Mania: Monotherapy • Lithium • Chlorpromazine • Risperidone • Divalproex • Quetiapine • Ziprasidone • Olanzapine • Aripiprazole • Carbamazepine ER • Acute Mania: Combination with lithium or valproate • Olanzapine • Quetiapine • Aripiprazole • Lithium • Lamotrigine • Olanzapine • Aripiprazole • Quetiapine (in combination) • Maintenance • Bipolar Depression • Olanzapine / fluoxetine combination • Quetiapine

Sometimes it is best to start a drug now • Lithium: 300 mg qhs x 3 d, then 600 mg qhs • Check 12 hour level after 1 wk • TSH, creatinine • Depakote: ER 500 mg qhs, increase dose by 250 mg up to 1000 -1500 mg qhs • Check 12 hour level after 3 d at steady dose • CBC, LFTs, weight • Lamotrigine: 25 mg qd x 2 wks, then 50 mg qd x 2 wks, then 100 mg qd • Watch for rash, advise how to manage • Better for depression than mania

Primary care providers need to know about mood stabilizers • Lithium • Drug level affected by many antihypertensives (including ACE-Is, diuretics) • Long-term use can cause chronic kidney injury • Hypothyroidism • Pregnancy category D • Valproic acid/Depakote • Weight gain • Liver enzyme elevation, thrombocytopenia • Pregnancy category D • Lamotrigine • Stevens Johnson Syndrome • Pregnancy category D

Numerous treatment options exist • Psychotherapy is beneficial for bipolar • Cognitive behavior therapy • Family-focused therapy • Interpersonal and social rhythm therapy • Psychoeducation • Combine psychotherapy with medications

Symptom-targeted strategies can also be helpful • Restore or maintain a good sleep pattern • Sleep hygiene, trazodone • Symptom monitoring • Build/maintain a good support system • Stress management • Take medications consistently (pill box, reminder system, medication set up services) • Avoid triggers including drugs and alcohol

Bipolar disorder affects lifespan • Bipolar shortens life expectancy by 9 years • Higher mortality rate, esp due to chronic medical conditions • Suicide (19%, 8 -10 x rate of general population) • Accidents/unintentional injuries (~10 x rate) • Increased risk of chronic diseases • Cardiovascular disease (31%) • Cancer (14%) • COPD (>2 x), diabetes (~3 x) • Influenza/pneumonia (~4 x rate of gen pop)

Gender can affect bipolar course • Women more likely to have BPAD-II than man • Women more likely to have seasonal pattern of symptoms • Women more likely to have depression, mixed mania, rapid cycling • Women more likely to have co-morbid thyroid disease, migraine, obesity, and anxiety disorder • Women more likely to experience delayed diagnosis and delayed treatment • Mood stabilizers work the same in men and women

Co-occurring substance abuse is common with bipolar disorder • Among people with bipolar type I, ~60% have a substance abuse diagnosis • ~46% have an alcohol misuse disorder • ~40% misuse drugs other than alcohol • Co-occurring conditions make diagnosis and treatment more complicated • Sometimes someone may appear manic but they might actually be intoxicated on meth, K 2, or another substance

Case 1 • Patient with depression who does not get better with antidepressant treatment • Medication nonadherence is the most common cause of depression treatment failure • Maybe they are not on the right medicine • Treatment-resistant depression: 2 medication trials at therapeutic dose for at least 2 months each without improvement • Consider bipolar depression, as it often does not respond to usual antidepressant medications

Case 2 • Patient is new to you, has previously been diagnosed with bipolar disorder, is currently stable on lithium, quetiapine, and diazepam; would like you to write prescriptions to continue this treatment. • Other health conditions include obesity, HTN, arthritis, asthma. • Pearls: bipolar disorder is underdiagnosed and misdiagnosed; common conditions that may present like bipolar disorder are depression and borderline personality disorder; ask about discrete manic or hypomanic episodes
Case 3 • You see a 29 yo female with depression and start your preferred SSRI. Patient gets manic.

Case 4 • Patient shows up in primary care clinic and is clearly manic. What should you do? • Psychiatry consult • Hospitalize? • Emergency room • Start a mood stabilizer

Case 5 • Patient with history of bipolar disorder, not taking medications now, depressed. • Start a medication to treat depression—which one? • Lithium, depakote, lamotrigine • Atypical antipsychotic
Case 6 • Patient with bipolar disorder, 29 yo female, taking lithium 1200 mg qhs. Gets pregnant, now her psychiatrist won’t see her because he doesn’t take care of pregnant patients. She comes to you for help.

Bipolar disorder complicates pregnancy and lactation • Pregnancy neither protects from nor exacerbates bipolar disorder • Many women require ongoing treatment during pregnancy and lactation • Mood stabilizers pose risk to developing fetus and nursing infant • Postpartum period is a time of high risk for onset and recurrence of bipolar disorder (including postpartum psychosis), consider prophylaxis

Case 7 • Patient with bipolar disorder, stable on medications. What advice should you give to maintain stability? • Sleep • Travel • Stress management • Medication adherence • Diet/exercise/weight • Screening and prevention • Chronic conditions
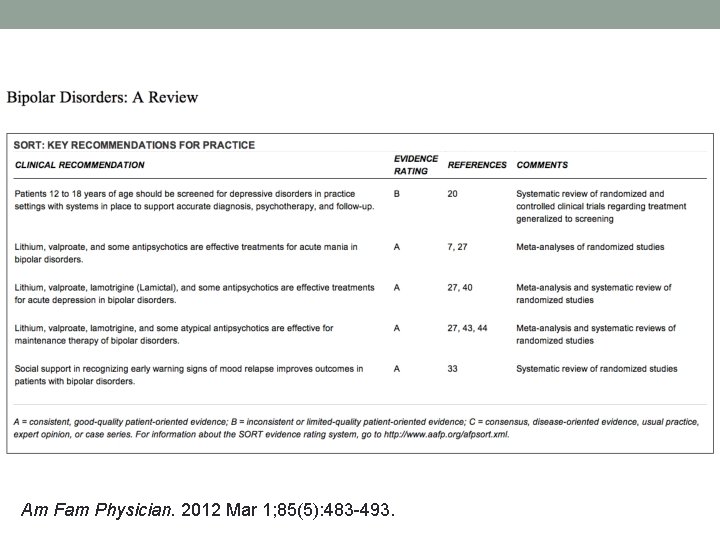

Am Fam Physician. 2012 Mar 1; 85(5): 483 -493.


DSM 5 updated the diagnosis of bipolar disorder • Tries to address prior underdiagnosis of bipolar disorder (esp type II) and overuse of NOS specifier • Recognition that sometimes a person does not fully meet the diagnostic criteria for severity or duration of hypomania but likely still has a bipolar illness (specifiers) • MDE specifiers • REMOVE SLIDE WHEN NEEDED INFO HAS BEEN MOVED
- Slides: 35