Bioterrorism Agents Epidemiology Program Overview Bioterrorism Background Deliberate

Bioterrorism Agents Epidemiology Program Overview

Bioterrorism Background • • Deliberate release of viruses, bacteria or other germs May be difficult to detect May not cause immediate illness Separated into three categories by CDC • Category A • Category B • Category C

High Priority Agents • Category A • Easily spread; high death rates • Anthrax, botulism, plague, smallpox, tularemia, and selected hemorrhagic fever viruses • Category B • Moderately easy to disseminate • Brucellosis, food safety threats, Q fever, and other agents • Category C • Could be engineered for mass dissemination • Emerging infectious diseases
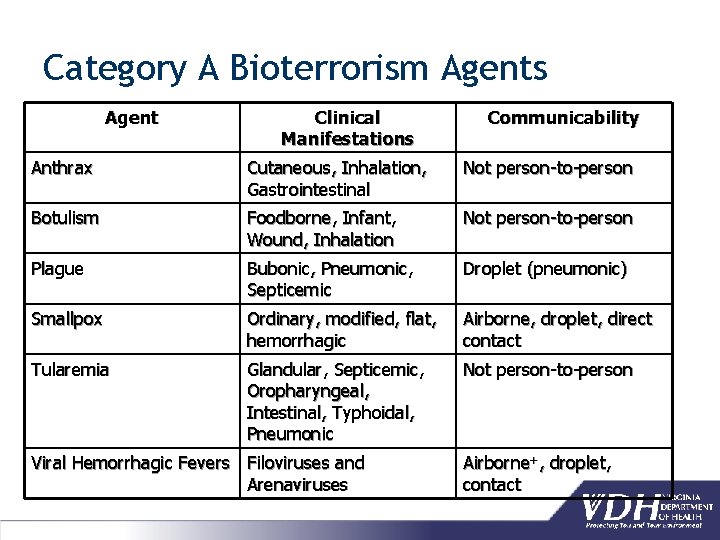
Category A Bioterrorism Agents Agent Clinical Manifestations Communicability Anthrax Cutaneous, Inhalation, Gastrointestinal Not person-to-person Botulism Foodborne, Infant, Wound, Inhalation Not person-to-person Plague Bubonic, Pneumonic, Septicemic Droplet (pneumonic) Smallpox Ordinary, modified, flat, hemorrhagic Airborne, droplet, direct contact Tularemia Glandular, Septicemic, Oropharyngeal, Intestinal, Typhoidal, Pneumonic Not person-to-person Viral Hemorrhagic Fevers Filoviruses and Arenaviruses Airborne+, droplet, contact

Anthrax • Infection through contact with infected animals/animal products or intentional exposure • Possible indicators of bioterrorism • Severe acute febrile disease with fulminant course and death • Gram-positive bacilli in skin biopsy, blood smears, CSF • Chest radiographs showing widened mediastinum

Botulism • Occurrence • Single cases occur sporadically • Foodborne botulism – 1 VA case reported in 2007 • Public health staff coordinate receipt of antitoxin • Possible indicators of bioterrorism: • Outbreak of multiple cases of descending, flaccid paralysis; • Outbreak with unusual toxin type (e. g. , C, D, F, G or type E not acquired from aquatic food) • Outbreak with common geographic features but without common dietary exposure • Multiple simultaneous outbreaks with no common source

Plague • Caused by the bacterium Yersinia pestis • Infection through bite of infected fleas, close contact with infected animals; inhalation of infective aerosols • Possible indicators of bioterrorism: • Cases in locations without enzootic infection • Cases in persons without known risk factors (e. g. , travel history, exposure to rodents/fleas) • Sudden outbreak of illness in patients presenting with severe pneumonia and sepsis

Smallpox • High risk of smallpox: • Febrile prodrome, and • Classic smallpox lesions, and • Lesions in the same stage of development • Moderate risk of smallpox: • Febrile prodrome plus: • One other high-risk criteria or • Four or more of the following: • • • Centrifugal distribution of lesions; First lesions in pharynx or oral mucosa; Patient appears toxic; Slow evolution of rash; Lesions on the palms and soles

Smallpox If moderate or high-risk for smallpox: • Rapidly report to DSI and communicate with other programs (EP&R, OCOM) • Collect information on CDC worksheet: Evaluating Patients for Smallpox • http: //emergency. cdc. gov/agent/smallpox/diagn osis/pdf/spox-patient-eval-wksheet. pdf • Coordinate specimen collection/submission to DCLS • Make infection control recommendations • Consider activation of Smallpox Response Plan

Tularemia • Occurrence • About 200 cases/year in the U. S. • 1 case reported in Virginia in 2010; Several in 2011 • Possible indicators of bioterrorism: • Increase in cases of acute, febrile illness • Cases progressing to pharyngitis, bronchiolitis, pneumonitis, pleuritis, hilar lymphadenitis • Laboratory findings: • Small, gram-negative coccobacilli

Viral Hemorrhagic Fevers (VHF) • Caused by several families of viruses • Filoviruses (Ebola, Marburg) • Arenaviruses (Lassa, Machupo) • Infection through contact with rodents (Lassa, Machupo); animal hosts for Ebola and Marburg unknown; person-to-person • Clinical presentation • Fever; fatigue; dizziness; rash; myalgias; bleeding; shock; multi-organ failure

VHF and Bioterrorism • Patients without relevant travel history and exposure • Suspected index case: • Temperature >101 F for less than three weeks; • Severe illness; • At least two of the following: hemorrhagic or purpuric rash, epistaxis, hematemesis, hemoptysis, blood in stool, or other hemorrhagic signs/symptoms; and • No predisposing factors for hemorrhagic manifestations

Category A Agents Public Health Response Rapidly reportable Require immediate public health follow-up • Consult with DSI and coordinate/communicate with EP&R and OCOM • Collect information on relevant Case Report Forms • Coordinate collection/submission of specimens to DCLS • Make infection control recommendations • Respiratory form of the diseases = consider BT May see naturally occurring cases • Botulism: infant/foodborne • Bubonic/pneumonic plague in those with travel and exposure history in western states • Tularemia: Exposure to rabbits, ticks

Category B Agents Public Health Response Laboratory Reports from Private Labs • Q Fever • Brucella species n Follow-up: Collect information on patient’s symptoms, why the test was ordered, evaluate possible exposures, consider confirmatory testing at DCLS. Record information on relevant Case Report Forms. n Ensure that isolates are forwarded to DCLS n
- Slides: 14