Biopotential Electrodes and its Applications Ms J Rajeswari

Bio-potential Electrodes and its Applications Ms. J. Rajeswari Assistant Professor, Department of Electrical and Electronics Engineering, Velammal College of Engineering and Technology

� Biomedical engineering is the application of knowledge and technologies to solve the problem of the living system. � It involves diagnosis, treatment and prevention of disease in human. Biomedical engineering 2
� It involves measurement of biological signals like ECG, EMG, or any electrical signals generated in the human body. � Biomedical Instrumentation helps physicians to diagnose the problem and provide treatment. Biomedical Instrumentation 3
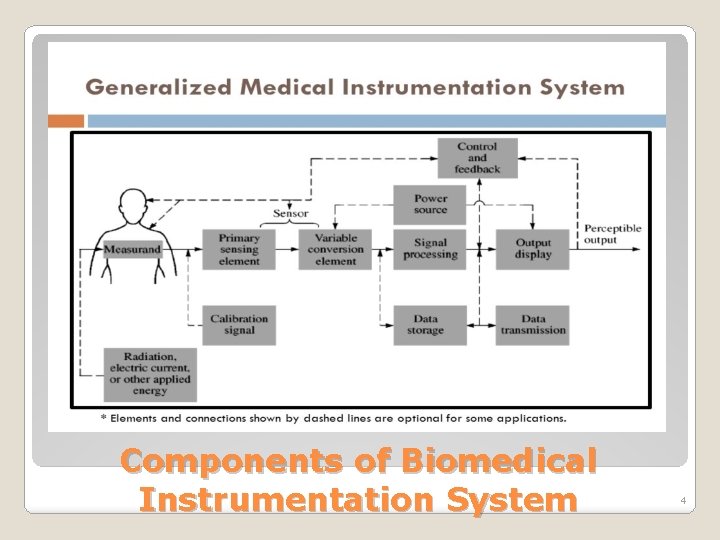
Components of Biomedical Instrumentation System 4

�Measurand: The measurand is the physical quantity. �Human body acts as the source for measurand, and it generates biosignals. �Example: body surface or blood pressure in the heart Components of Biomedical Instrumentation System 5
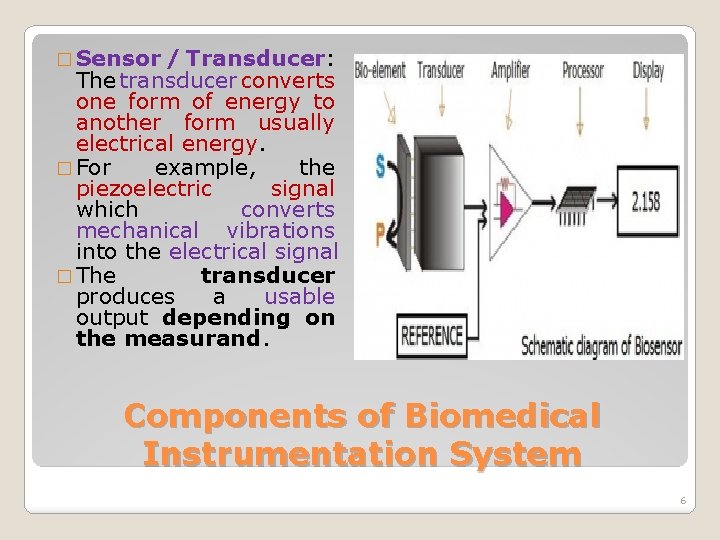
� Sensor / Transducer: The transducer converts one form of energy to another form usually electrical energy. � For example, the piezoelectric signal which converts mechanical vibrations into the electrical signal � The transducer produces a usable output depending on the measurand. Components of Biomedical Instrumentation System 6
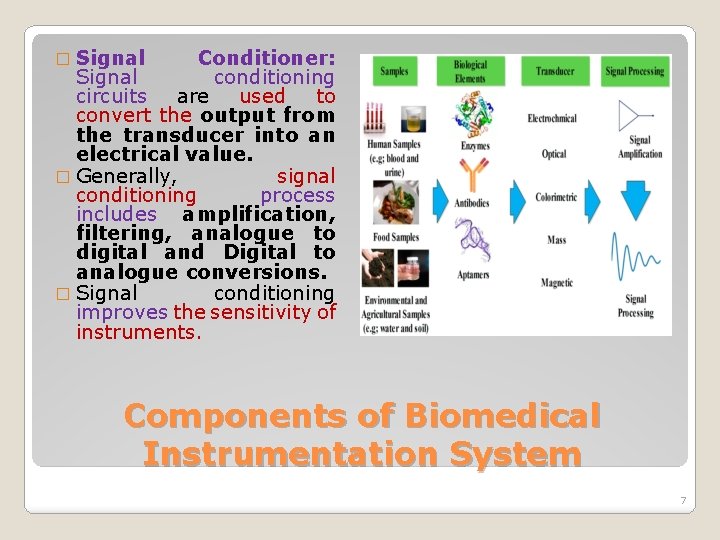
� Signal Conditioner: Signal conditioning circuits are used to convert the output from the transducer into an electrical value. � Generally, signal conditioning process includes amplification, filtering, analogue to digital and Digital to analogue conversions. � Signal conditioning improves the sensitivity of instruments. Components of Biomedical Instrumentation System 7
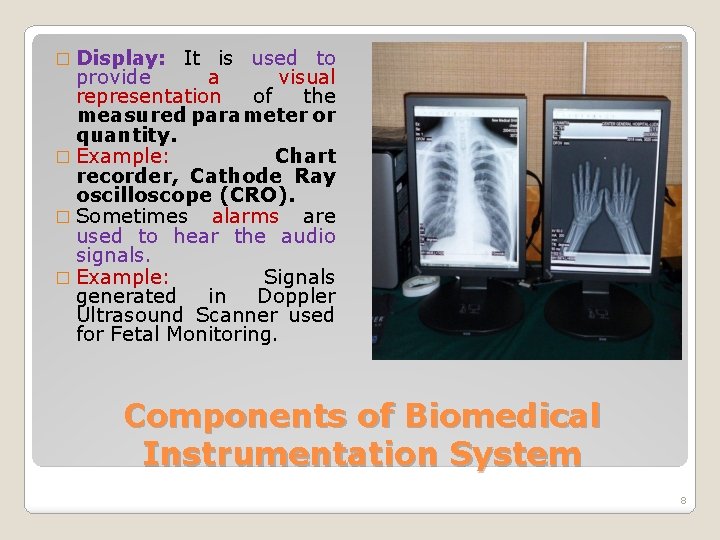
� Display: It is used to provide a visual representation of the measured parameter or quantity. � Example: Chart recorder, Cathode Ray oscilloscope (CRO). � Sometimes alarms are used to hear the audio signals. � Example: Signals generated in Doppler Ultrasound Scanner used for Fetal Monitoring. Components of Biomedical Instrumentation System 8

�Data Storage and Data Transmission: Data storage is used to store the data and can be used for future reference. �Recently Electronic Health records are utilized in hospitals. �Data transmission is used in Telemetric systems, where data can be transmitted from one location to another remotely. Components of Biomedical Instrumentation System 9
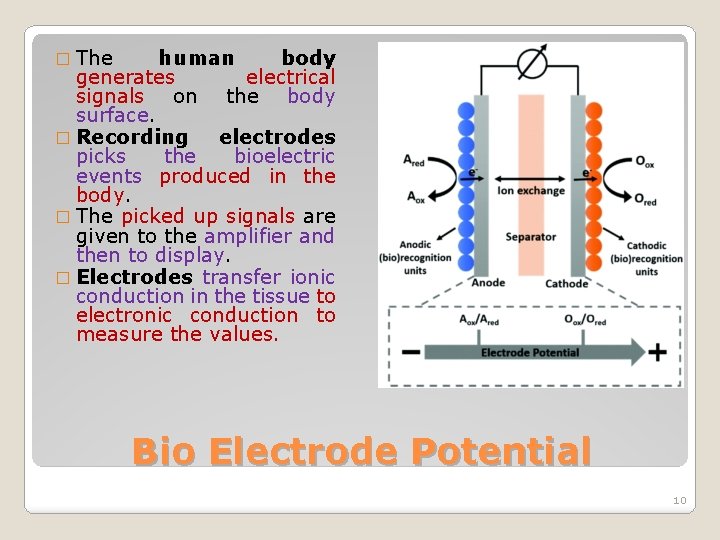
� The human body generates electrical signals on the body surface. � Recording electrodes picks the bioelectric events produced in the body. � The picked up signals are given to the amplifier and then to display. � Electrodes transfer ionic conduction in the tissue to electronic conduction to measure the values. Bio Electrode Potential 10
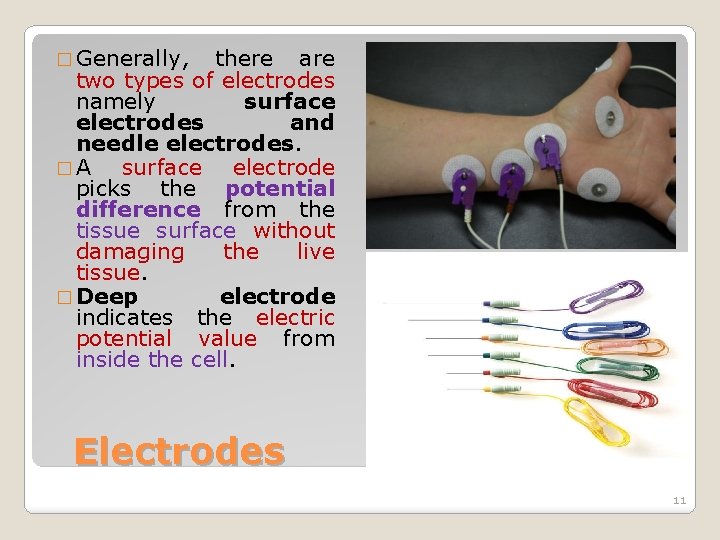
� Generally, there are two types of electrodes namely surface electrodes and needle electrodes. �A surface electrode picks the potential difference from the tissue surface without damaging the live tissue. � Deep electrode indicates the electric potential value from inside the cell. Electrodes 11
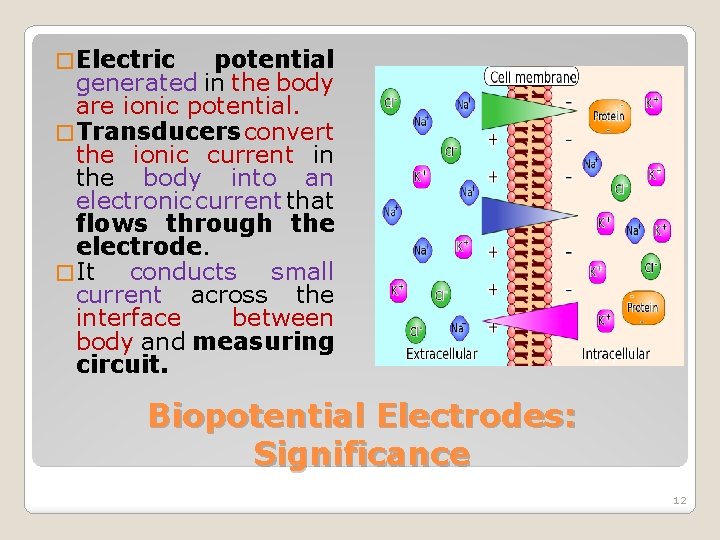
� Electric potential generated in the body are ionic potential. � Transducers convert the ionic current in the body into an electronic current that flows through the electrode. � It conducts small current across the interface between body and measuring circuit. Biopotential Electrodes: Significance 12

�A net volume of current passes across the interface from the electrode to electrolyte. �At the electrodeelectrolyte interface, current flows from left to right Biopotential Electrodes: Significance 13
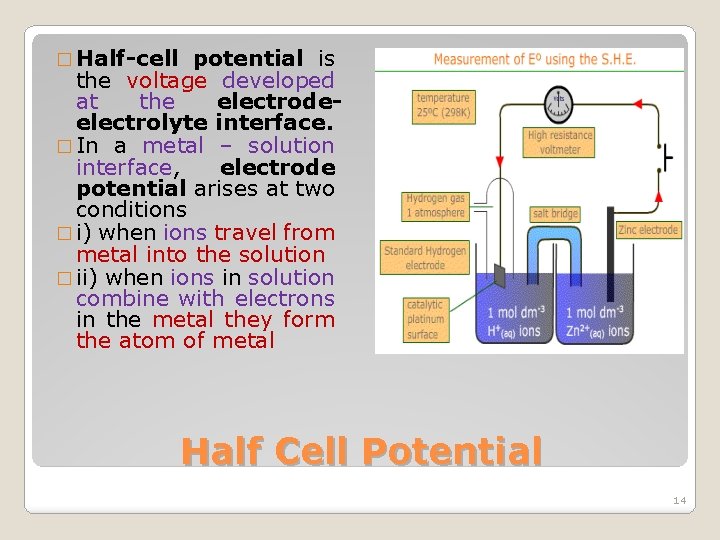
� Half-cell potential is the voltage developed at the electrodeelectrolyte interface. � In a metal – solution interface, electrode potential arises at two conditions � i) when ions travel from metal into the solution � ii) when ions in solution combine with electrons in the metal they form the atom of metal Half Cell Potential 14

� Electrode is a solid electric conductor through which an electric current enters or leaves an electrolytic cell. � It converts ionic potentials to electronic potentials. � Different types of electrodes used for biological measurements depend on the anatomical locations, from where the bioelectric signals are measured. � Bioelectric electrodes acquire the signals like ECG, EEG, EMG, etc. Electrodes 15

Types of Electrodes 16

� Surface electrode measures the potential available from the surface of the skin. � It senses the signal from heart, brain and nerves. � Larger surface electrodes sense the ECG signals. � Smaller surface electrodes sense the EMG and EEG signals Surface Electrodes 17

� ECG measurement technique uses either rectangular or circular shaped plate electrodes made of nickel, silver or German silver materials. � It has a smaller contact area and do not seal completely on the patient. Surface Electrodes : Metal Plate Electrodes 18

� Electrodes are pasted on the skin using electrolyte paste. � The electrode slippage and plate displacement are the two major disadvantages of this electrode type. � They are very sensitive, leading to measurement errors. � Since it is suitable for application on four limbs of the body, they called limb electrodes. Surface Electrodes : Metal Plate Electrodes 19

�During surgical procedure since patient’s legs are immobile, limb electrodes are preferred. �Chest electrodes interfere with the surgery, so not used for ECG measurement. �At the same time for a long-term patient monitoring limb-electrodes are not used. Surface Electrodes : Metal Plate Electrodes 20

� To measure ECG from various positions on the chest, Suction cup electrodes are used. � It suits well to attach electrodes on flat surface of the body and on soft tissue regions. � They have a good contact surface. Surface Electrodes : Suction Cup Electrodes or Welsh Cup Electrodes 21

� Physically they are large but the skin contacts only the electrode rim. � It has high contact impedance. � They have a plastic syringe barrel, suction tube and cables. � Recently, due to infection and cleaning procedures, these electrodes are not used. Surface Electrodes : Suction Cup Electrodes or Welsh Cup Electrodes 22
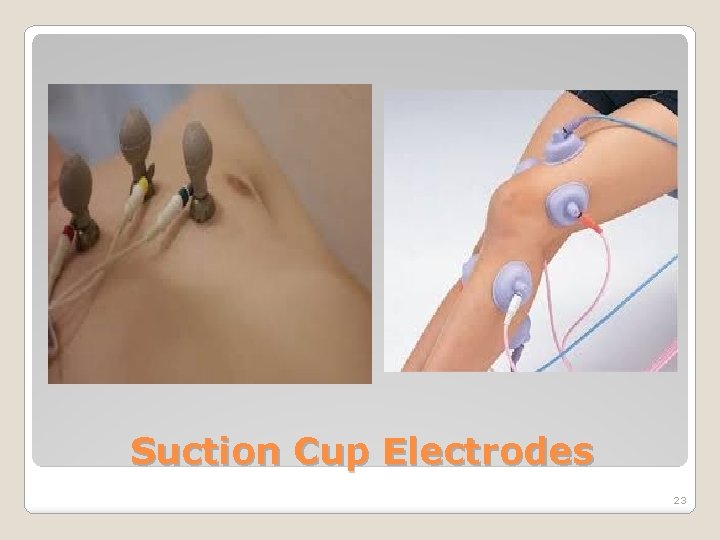
Suction Cup Electrodes 23

� � � In the surface electrode, the pressure of surface electrode against the skin squeezes out the electrode paste. To avoid this problem, adhesive electrodes are used. It has a lightweight metallic screen. They have a pad at behind for placing electrode paste. This adhesive backing hold the electrode on place and tight. It also helps to avoid evaporation of electrolyte present in the electrode paste. Surface Electrodes : Adhesive Type Electrodes 24

Surface Electrodes : Adhesive Type Electrodes 25

� In metal plate or limb electrodes, the major disadvantage is the movement errors. � Motion artefact occurs due to the motion at the interface between electrode and electrolyte. � The interface gets stabilized using Floating electrodes. Floating Electrodes 26

� The floating electrodes do not contact the human subject directly. � They contact the subject via electrolytic paste or jelly. � The advantage of this type is the mechanical stability. Floating Electrodes 27
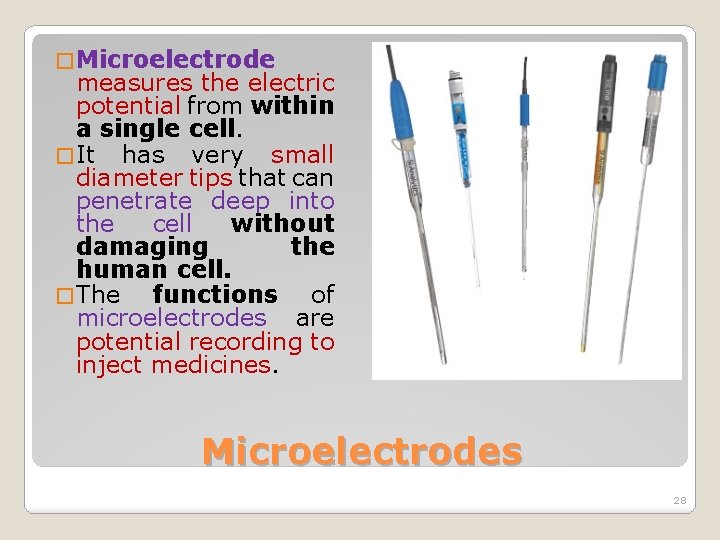
� Microelectrode measures the electric potential from within a single cell. � It has very small diameter tips that can penetrate deep into the cell without damaging the human cell. � The functions of microelectrodes are potential recording to inject medicines. Microelectrodes 28

�Generally, when microelectrode is inside cell, reference electrode is outside the cell. �It has high impedances in range of mega ohm due to their small size. �Two types of microelectrode are �Metal Microelectrode �Non- Metallic (Micropipette) Microelectrode 29
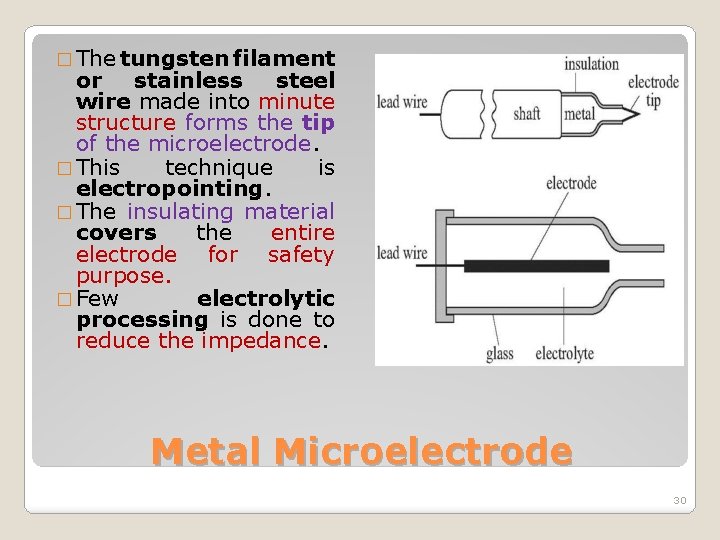
� The tungsten filament or stainless steel wire made into minute structure forms the tip of the microelectrode. � This technique is electropointing. � The insulating material covers the entire electrode for safety purpose. � Few electrolytic processing is done to reduce the impedance. Metal Microelectrode 30

�Measurement of bioelectric potentials requires two electrodes. �Resulting voltage potential is the difference between potential of microelectrode and reference electrode. Metal Microelectrode 31

�The total sum of three potentials is as follows E=EA+EB+EC �Where, EA – metal electrode – electrolyte potential at microelectrode tip. �EB – Reference electrode – electrolyte potential. �EC – Variable cell membrane potential. Metal Microelectrode 32
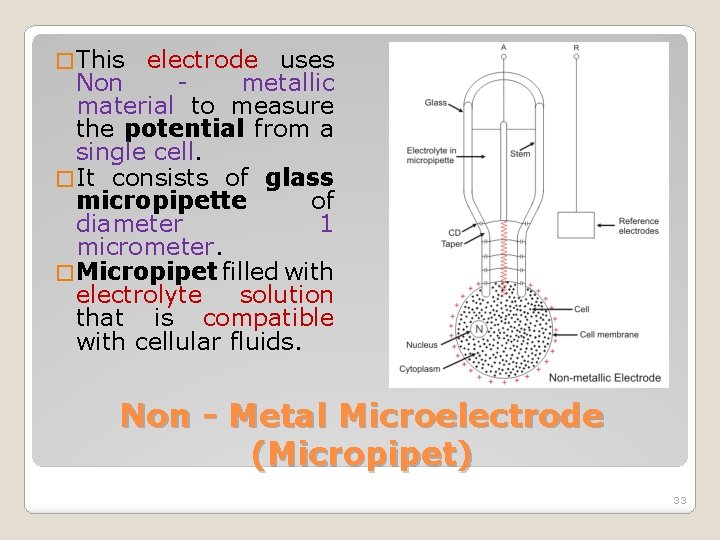
� This electrode uses Non metallic material to measure the potential from a single cell. � It consists of glass micropipette of diameter 1 micrometer. � Micropipet filled with electrolyte solution that is compatible with cellular fluids. Non - Metal Microelectrode (Micropipet) 33

� Stem of Micropipet has a thin flexible wire made out of chloride silver, stainless steel or tungsten. � One end of the Micropipet attaches to the rigid support and other free end rests on the cell. Non - Metal Microelectrode (Micropipet) 34

�The potential voltage generated is as follows. �E=EA+EB+EC+ED �EA – potential voltage between the metal wire and an electrolyte filled inside Micropipet. �EB – potential between the reference electrode and extracellular fluid. �EC – variable cell membrane potential. �ED – potential at the tip due to electrolytes present inside pipet and the cell Non - Metal Microelectrode (Micropipet) 35

� When electrode gets closer to the bioelectric generator, it penetrates into the skin. � Therefore, the electrode should be sharp for penetration to obtain and record the bioelectric events. Depth and Needle Electrodes 36
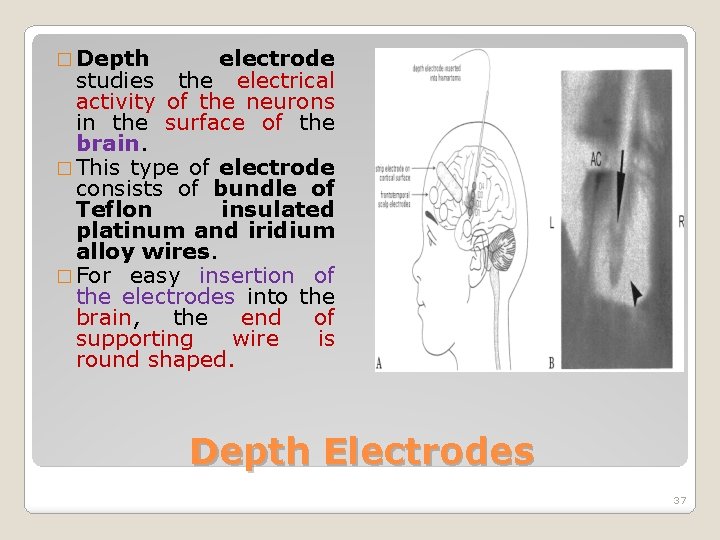
� Depth electrode studies the electrical activity of the neurons in the surface of the brain. � This type of electrode consists of bundle of Teflon insulated platinum and iridium alloy wires. � For easy insertion of the electrodes into the brain, the end of supporting wire is round shaped. Depth Electrodes 37

�Number of individualelectrodes forms the electrode array or bundle. �In the bundle of electrodes, end of each individual wires has the individual electrode Depth Electrodes 38
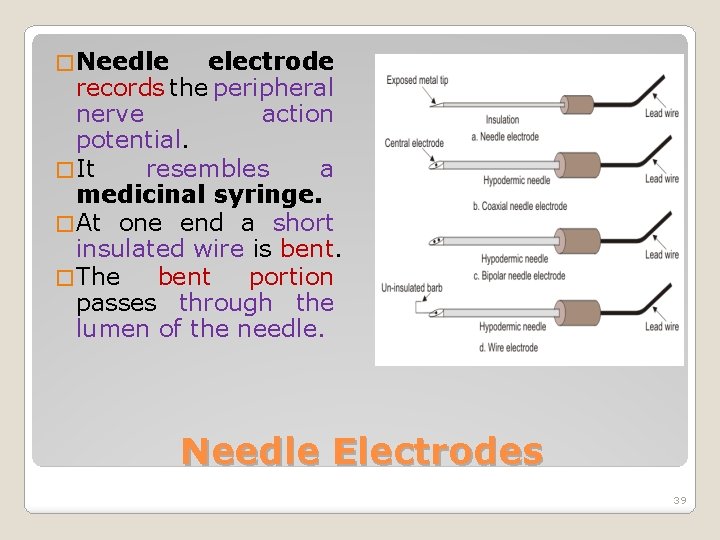
� Needle electrode records the peripheral nerve action potential. � It resembles a medicinal syringe. � At one end a short insulated wire is bent. � The bent portion passes through the lumen of the needle. Needle Electrodes 39

� This setup goes into the muscle. � Now the needle is withdrawn. � The bent wire remains inside the muscle. � Two type of needle electrodes namely � Mono-polar Electrode: This type uses single reference electrode placed on the skin. Bi - polar Electrode: This type has one reference electrode and one active electrode. Needle Electrodes 40

� Generally, biological/bioelectric signals have low amplitude and low frequency. � Therefore, to increase the amplitude level of biosignals, amplifiers are designed. � The outputs from these amplifiers are used for further analysis and they appear as ECG, EMG, or any bioelectric waveforms. � Such amplifiers are defined as Bio Amplifiers or Biomedical Amplifier 41

� � � The biological amplifier should have a high input impedance value. The range of value lies between 2 MΩ and 10 MΩ depending on the applications. Higher impedance value reduces distortion of the signal. When electrodes pick up biopotentials from the human body, the input circuit should be protected. Every bio-amplifier should consist of isolation and protection circuits, to prevent the patients from electrical shocks. Basic Requirements for Biological Amplifiers 42

� Since the output of a bioelectric signal is in millivolts or microvolt range, the voltage gain value of the amplifier should be higher than 100 d. B. � Throughout the entire bandwidth range, a constant gain should be maintained. � A bio-amplifier should have a small output impedance. Basic Requirements for Biological Amplifiers 43

�A good bio-amplifier should be free from drift and noise. � Common Mode Rejection Ratio (CMRR) value of amplifier should be greater than 80 d. B to reduce the interference from common mode signal. � The gain of the bioamplifier should be calibrated for each measurement. Basic Requirements for Biological Amplifiers 44

�Differential Amplifier �Instrumentation Amplifier �Chopper Amplifier �Isolation Amplifier Types of Bio Amplifiers 45

Must be a low-noise device ◦ Its output is amplified many times, so any noise injected here also gets amplified many times! � Should be dc coupled to the electrodes ◦ Include no series capacitors in the input leads (input bias currents build charge on series input capacitors). ◦ To preserve low frequency content of the input signals. � Preamplifier 46

Use relatively low gain for the preamplifier ◦ Input bias currents can build charge on polarizable electrodes, creating a dc offset in the input signals. ◦ Use a high-input impedance Op. Amp to reduce these charging effects. ◦ High gain will saturate the output of the preamplifier. � Employ capacitive coupling for later stages of the amplifier circuit to avoid saturation effects. � Preamplifier 47
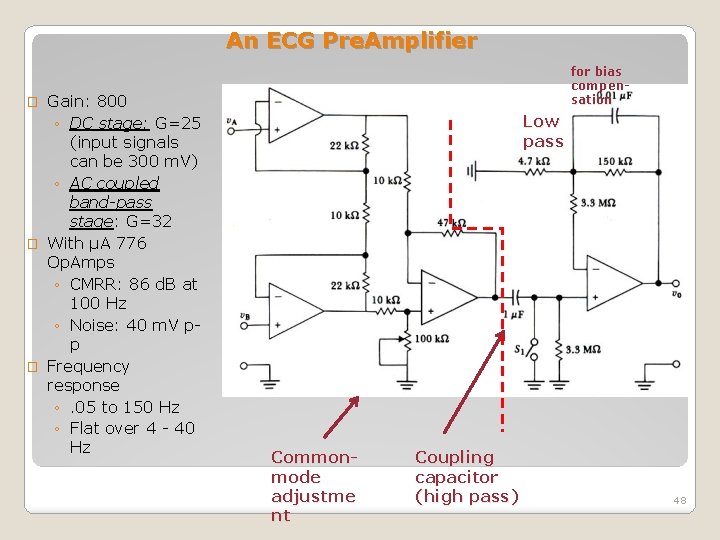
An ECG Pre. Amplifier Gain: 800 ◦ DC stage: G=25 (input signals can be 300 m. V) ◦ AC coupled band-pass stage: G=32 � With µA 776 Op. Amps ◦ CMRR: 86 d. B at 100 Hz ◦ Noise: 40 m. V pp � Frequency response ◦. 05 to 150 Hz ◦ Flat over 4 - 40 Hz for bias compensation � Low pass Commonmode adjustme nt Coupling capacitor (high pass) 48
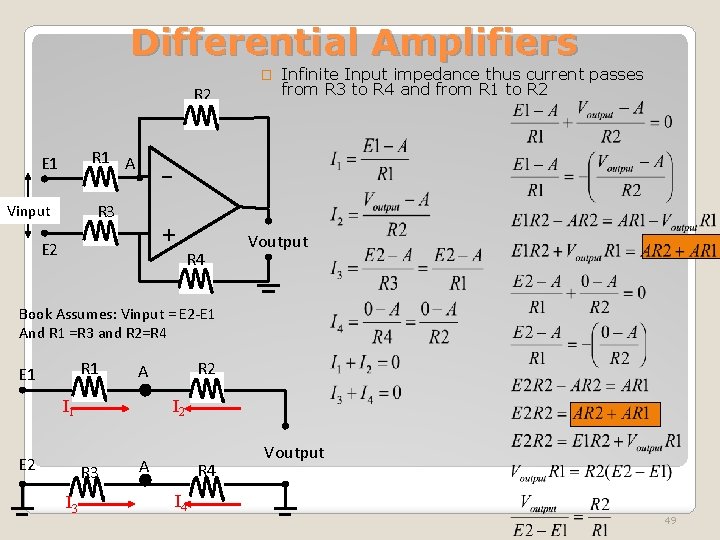
Differential Amplifiers � R 2 R 1 A E 1 - R 3 Vinput Infinite Input impedance thus current passes from R 3 to R 4 and from R 1 to R 2 + E 2 R 4 Voutput Book Assumes: Vinput = E 2 -E 1 And R 1 =R 3 and R 2=R 4 R 1 E 1 I 1 E 2 I 2 R 3 I 3 R 2 A A R 4 I 4 Voutput 49

�In differential mode noise common to both input signals is cancelled R 2 1 V E 1 R 1 A R 3 3 V E 2 + 2 V R 4 Voutput Advantages of Differential Amplifier 50

Differential Amplifier 51

�In biomedical applications, high gain and the high input impedance are attained with an instrumentation amplifier. �Usually, a 3 -amplifier setup forms the instrumentation amplifier circuit. �The output from the transducer is given as input to the instrumentation amplifier. Instrumentation Amplifier 52
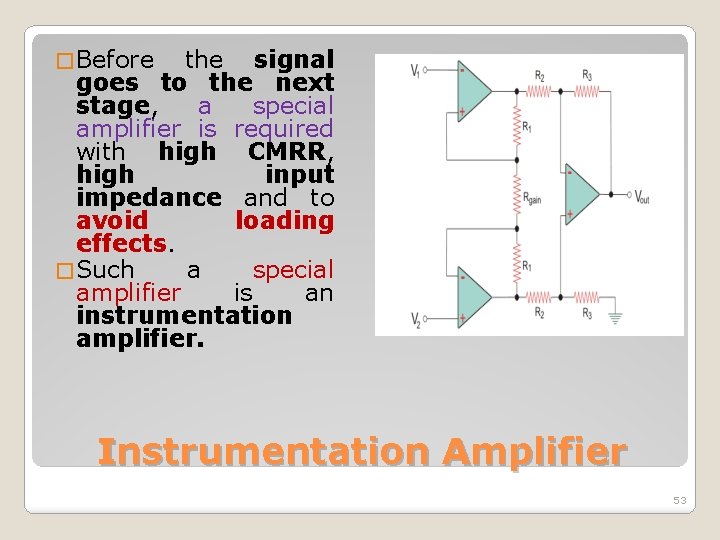
� Before the signal goes to the next stage, a special amplifier is required with high CMRR, high input impedance and to avoid loading effects. � Such a special amplifier is an instrumentation amplifier. Instrumentation Amplifier 53
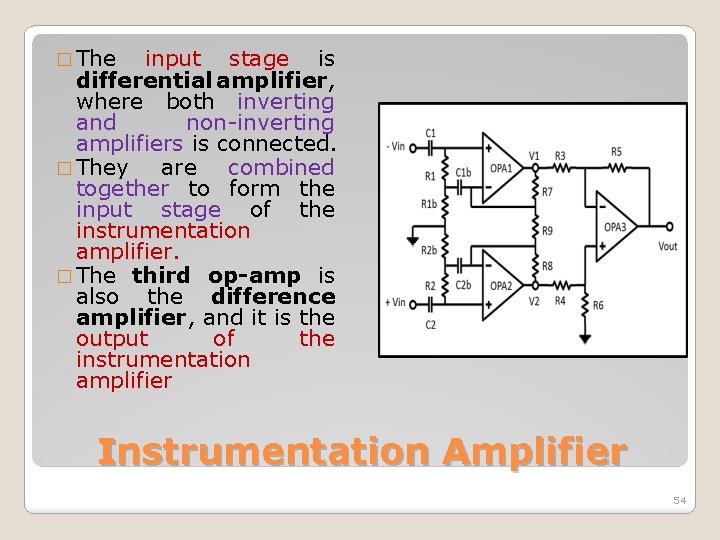
� The input stage is differential amplifier, where both inverting and non-inverting amplifiers is connected. � They are combined together to form the input stage of the instrumentation amplifier. � The third op-amp is also the difference amplifier, and it is the output of the instrumentation amplifier Instrumentation Amplifier 54

�The output Vout is the difference between two input signals given at the input points. �VO 1 is the output from op-amp 1 and VO 2 is the output from op-amp 2. Instrumentation Amplifier 55
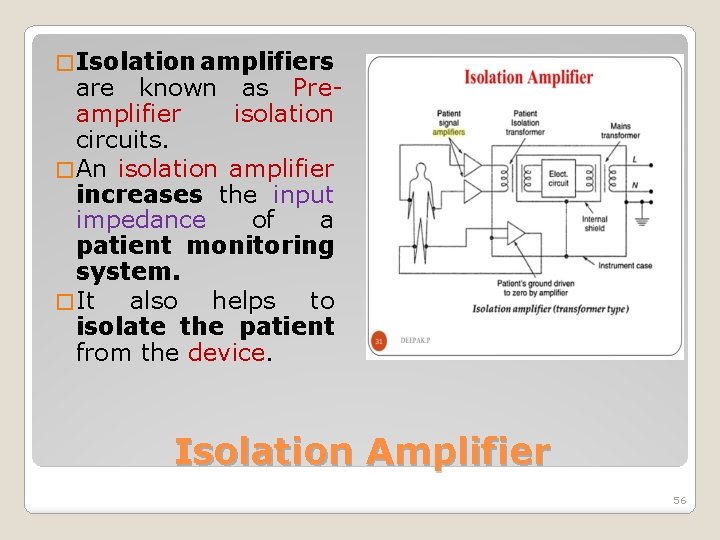
� Isolation amplifiers are known as Preamplifier isolation circuits. � An isolation amplifier increases the input impedance of a patient monitoring system. � It also helps to isolate the patient from the device. Isolation Amplifier 56
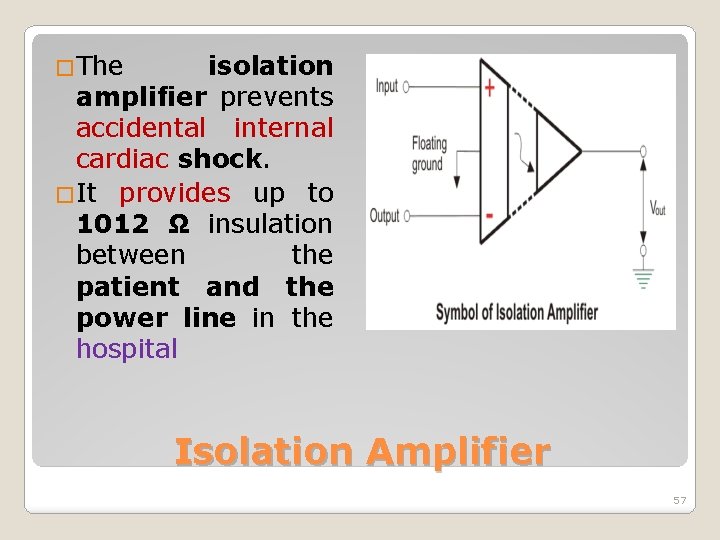
�The isolation amplifier prevents accidental internal cardiac shock. �It provides up to 1012 Ω insulation between the patient and the power line in the hospital Isolation Amplifier 57
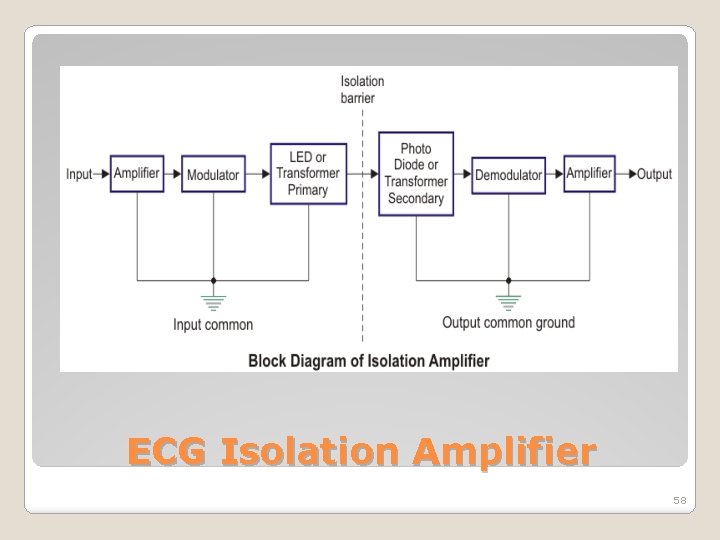
ECG Isolation Amplifier 58

�During ECG measurement, signals generated from all leads are sent to the low pass filter. �This filter is named as Electro surgery filters because it decreases the interference between electrosurgery and radio frequency. �Next block is the high voltage and overvoltage protection that can withstand large voltage during defibrillation ECG Isolation Amplifier 59
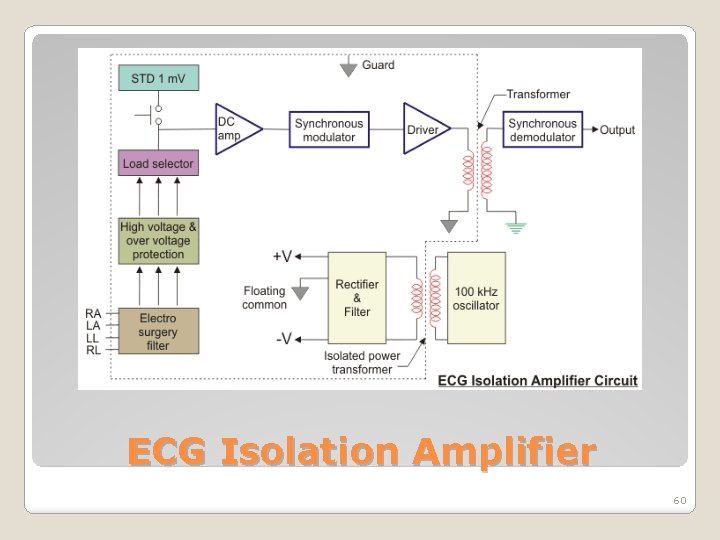
ECG Isolation Amplifier 60
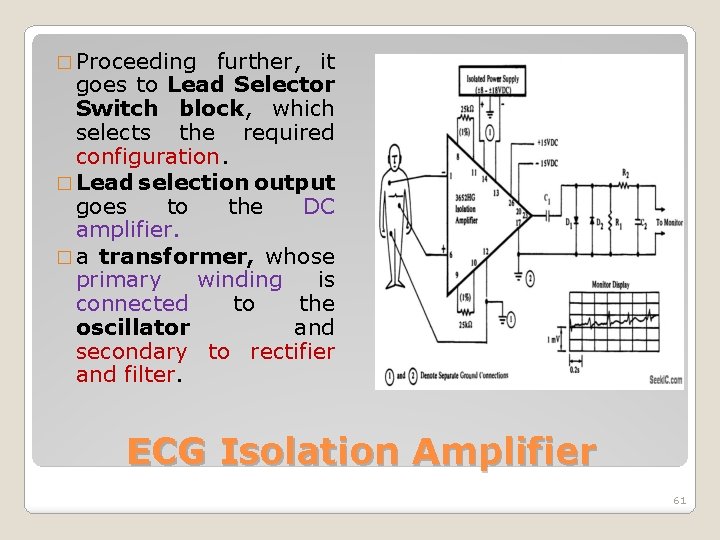
� Proceeding further, it goes to Lead Selector Switch block, which selects the required configuration. � Lead selection output goes to the DC amplifier. � a transformer, whose primary winding is connected to the oscillator and secondary to rectifier and filter. ECG Isolation Amplifier 61

�ECG signal is modulated with the Synchronous modulator. �The second transformer delivers the output to the synchronous demodulator. �The output from the demodulator is fed as input to the power amplifier ECG Isolation Amplifier 62

� When recording biopotentials noise and drift are the two problems encountered. � Noise is due to the recording device and by the patient when they move. � Drift is a shift in baseline created due to various thermal effects. Chopper Amplifier 63
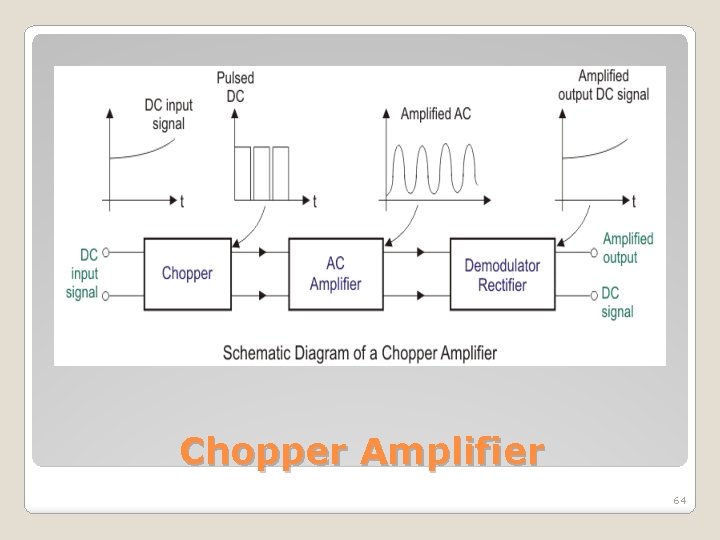
Chopper Amplifier 64

�A DC amplifier has a shift or sudden peak in the output when the input is zero. �Therefore, a chopper amplifier solves the problems of drift in DC amplifiers. �The name Chop means to sample the data. �The amplifier circuit samples the analog signal and is known as chopper amplifier Chopper Amplifier 65

�The general diagram of a chopper amplifier is as shown. �The first block chopper accepts the DC input signal and converts them to an AC signal. �The AC amplifier block amplifies the chopped AC signal. �Next, in the demodulator rectifier block, an amplified chopped AC signal is converted to amplified DC signal. Chopper Amplifier 66
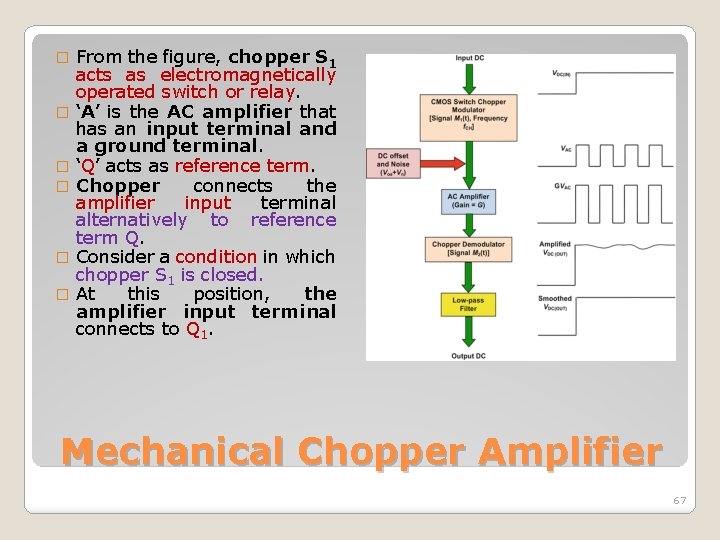
� � � From the figure, chopper S 1 acts as electromagnetically operated switch or relay. ‘A’ is the AC amplifier that has an input terminal and a ground terminal. ‘Q’ acts as reference term. Chopper connects the amplifier input terminal alternatively to reference term Q. Consider a condition in which chopper S 1 is closed. At this position, the amplifier input terminal connects to Q 1. Mechanical Chopper Amplifier 67
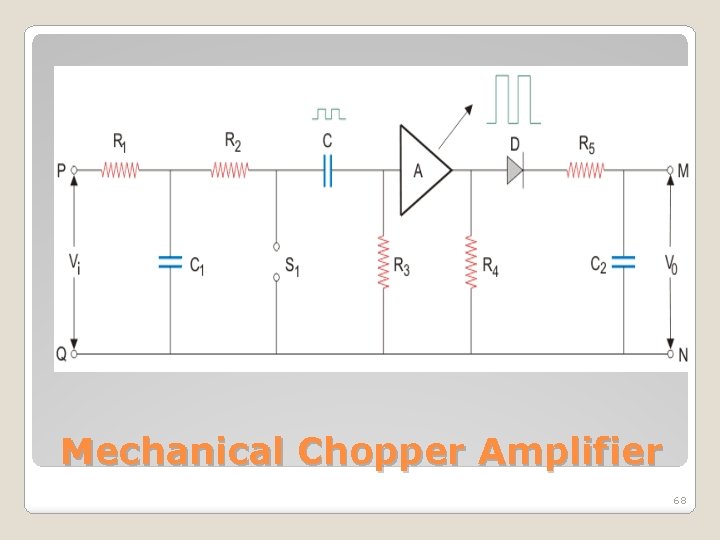
Mechanical Chopper Amplifier 68

� The entire circuit is short-circuited, so input voltage is zero. � Now, let us consider the reverse operation when chopper S 1 is open. � The AC amplifier starts receiving the signal from P terminal. � Finally, the amplifier input has an alternating voltage that varies between zero and input voltage. Mechanical Chopper Amplifier 69

�At this stage, conversion of DC signal to square wave pulse occurs with amplification. �Diode ‘D’ rectifies the chopped signal. �At the output terminal M and N, the amplified DC output signal occurs. �Chopping or sampling rate determines the chopper response time. Mechanical Chopper Amplifier 70
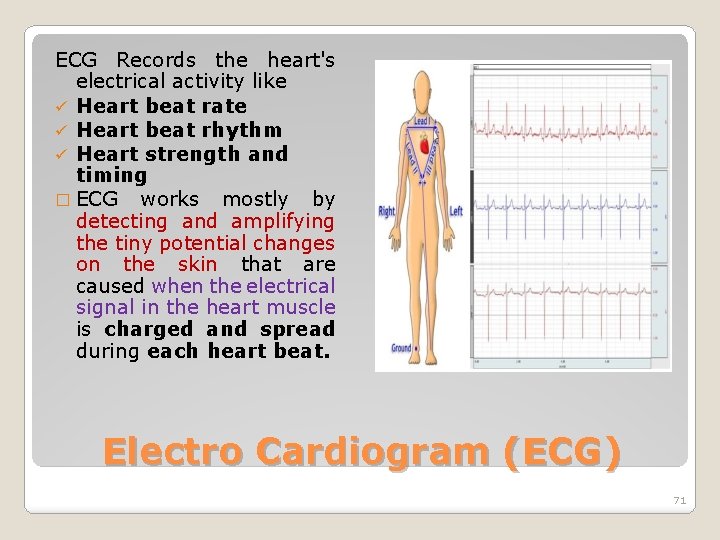
ECG Records the heart's electrical activity like ü Heart beat rate ü Heart beat rhythm ü Heart strength and timing � ECG works mostly by detecting and amplifying the tiny potential changes on the skin that are caused when the electrical signal in the heart muscle is charged and spread during each heart beat. Electro Cardiogram (ECG) 71
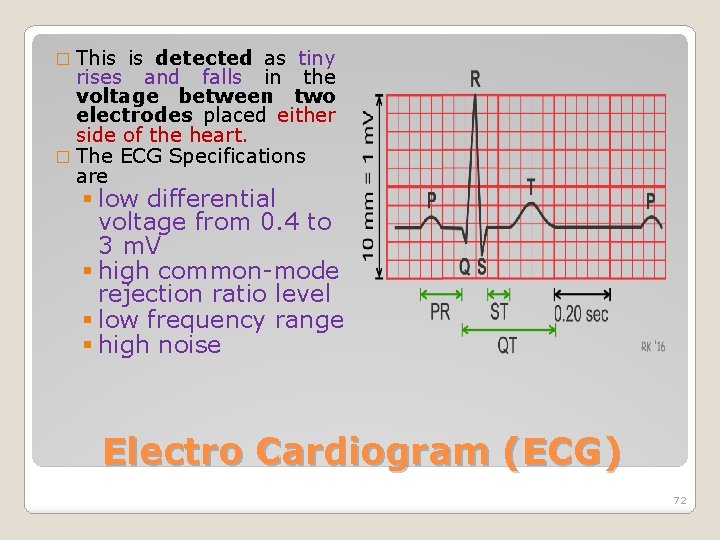
� This is detected as tiny rises and falls in the voltage between two electrodes placed either side of the heart. � The ECG Specifications are § low differential voltage from 0. 4 to 3 m. V § high common-mode rejection ratio level § low frequency range § high noise Electro Cardiogram (ECG) 72
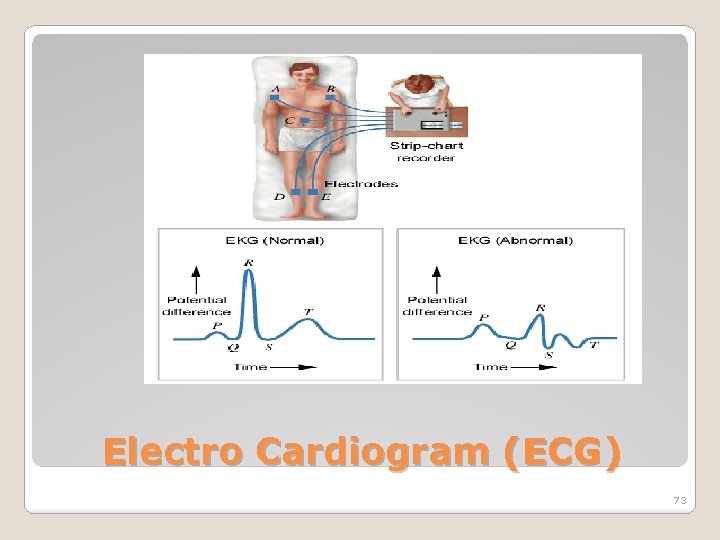
Electro Cardiogram (ECG) 73
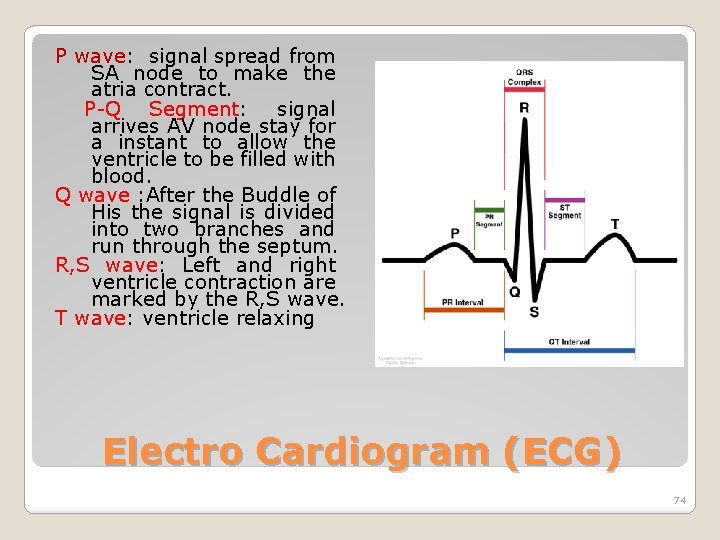
P wave: signal spread from SA node to make the atria contract. P-Q Segment: signal arrives AV node stay for a instant to allow the ventricle to be filled with blood. Q wave : After the Buddle of His the signal is divided into two branches and run through the septum. R, S wave: Left and right ventricle contraction are marked by the R, S wave. T wave: ventricle relaxing Electro Cardiogram (ECG) 74
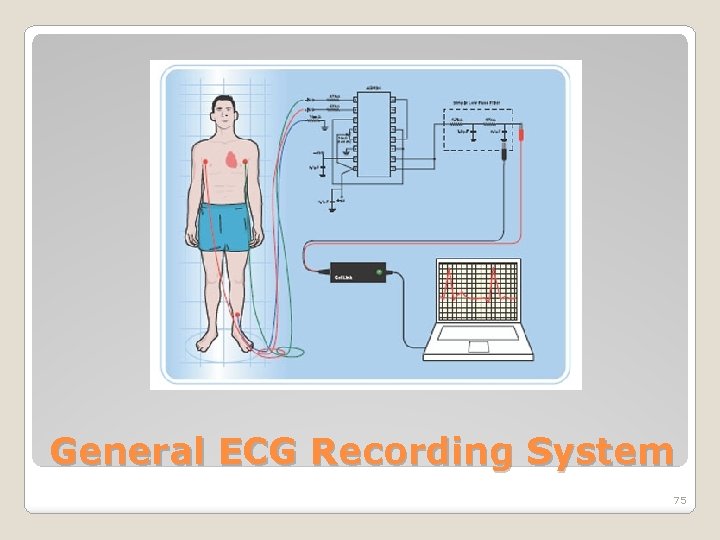
General ECG Recording System 75
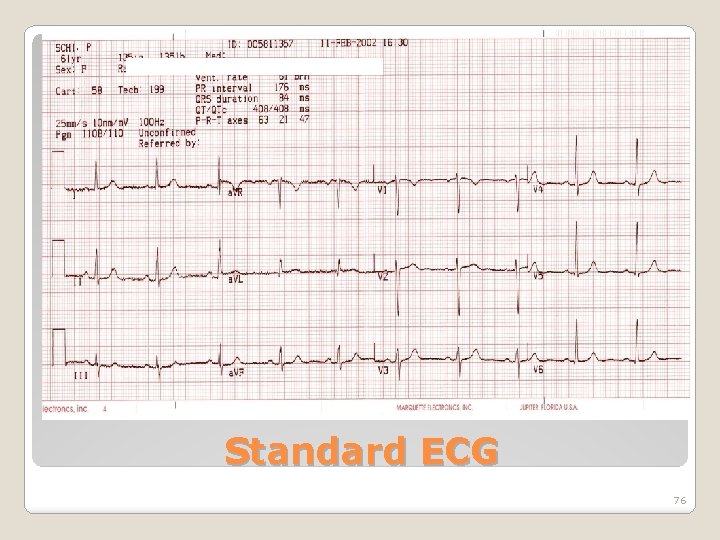
Standard ECG 76

�Typical Leads RA = right arm LA = Left arm LL = left leg RL = right leg C = Chest �Different leads result in different waveform shapes and amplitudes Electro Cardiogram (ECG) 77

are those designated by Lead I, III which form Einthoven Triangle: ◦ Lead I = LA connection to non inverting amp. Input and RA connecting to inverting amp. Input ◦ Lead II = LL connection to amp Non inverting input RA connect to inverting input and LA shorted to RL ◦ Lead III = LL connected to non inverting input LA connected to inverting input Bipolar Limb Leads 78
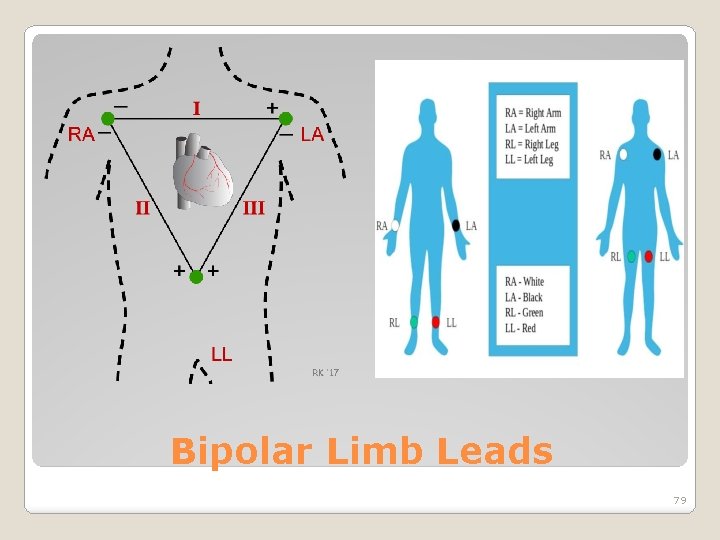
Bipolar Limb Leads 79

leads that look at composite potential from 3 limbs simultaneously where signal from 2 limbs are summed in a resistor network and then applied to an inverting amplifier input and the remaining limb electrode is applied to the non-inverting input Lead a. VR = RA connected to non-inverting input while LA and LL are summed at inverting input augmented (amplified) Voltage for Right arm (a. VR) Lead a. VL = LA connected to non-inverting input while RA and LL are summed at inverting input augmented (amplified) Voltage for Left arm (a. VL) Lead a. VF = LL connected to non-inverting input while RA and LA are summed at inverting input augmented (amplified) Voltage for Foot (a. Vf) Unipolar Limb Leads 80

Unipolar Limb Leads 81
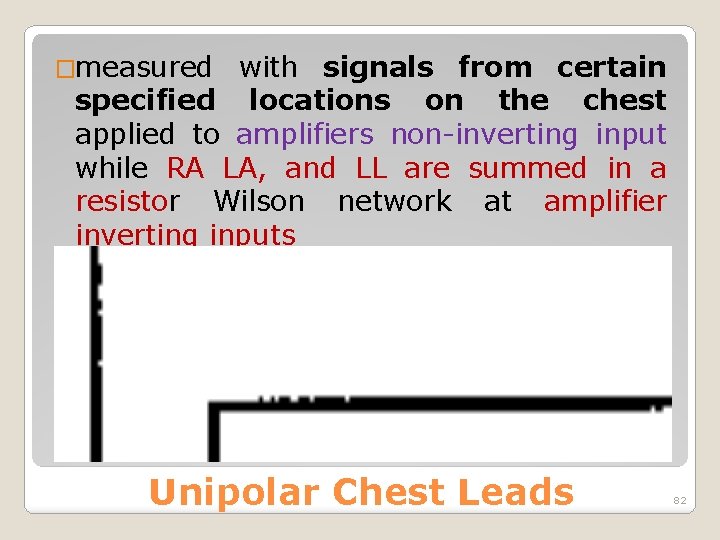
�measured with signals from certain specified locations on the chest applied to amplifiers non-inverting input while RA LA, and LL are summed in a resistor Wilson network at amplifier inverting inputs Unipolar Chest Leads 82
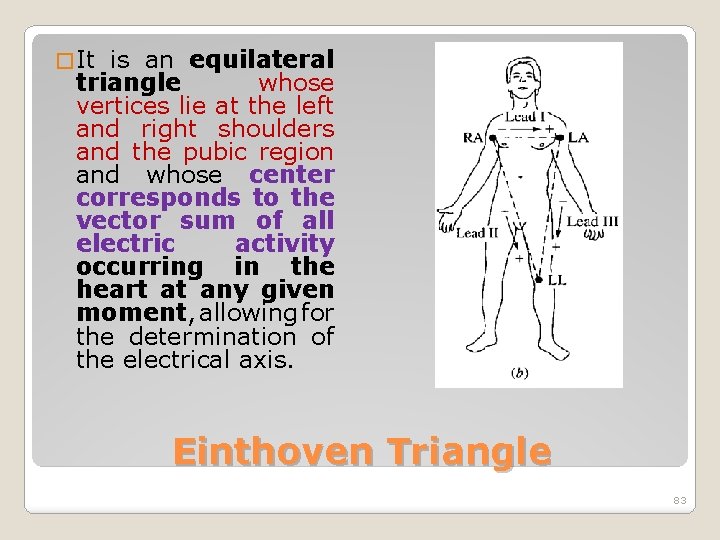
� It is an equilateral triangle whose vertices lie at the left and right shoulders and the pubic region and whose center corresponds to the vector sum of all electric activity occurring in the heart at any given moment, allowing for the determination of the electrical axis. Einthoven Triangle 83
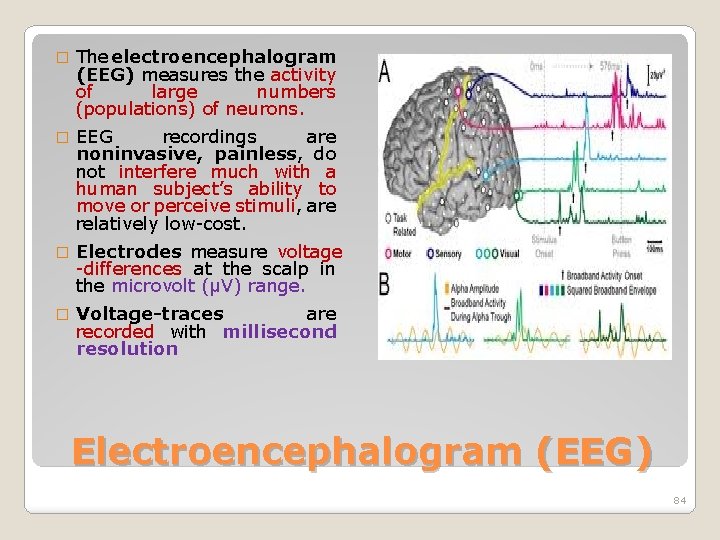
� The electroencephalogram (EEG) measures the activity of large numbers (populations) of neurons. � EEG recordings are noninvasive, painless, do not interfere much with a human subject’s ability to move or perceive stimuli, are relatively low-cost. � Electrodes measure voltage -differences at the scalp in the microvolt (μV) range. � Voltage-traces are recorded with millisecond resolution Electroencephalogram (EEG) 84
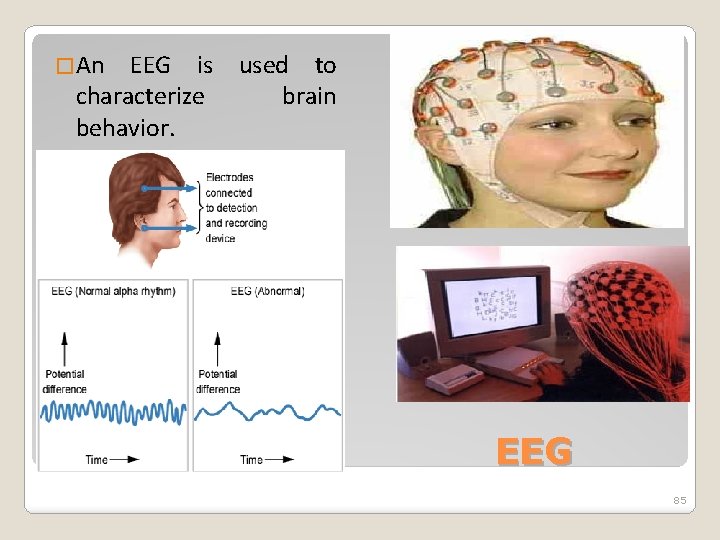
�An EEG is used to characterize brain behavior. EEG 85
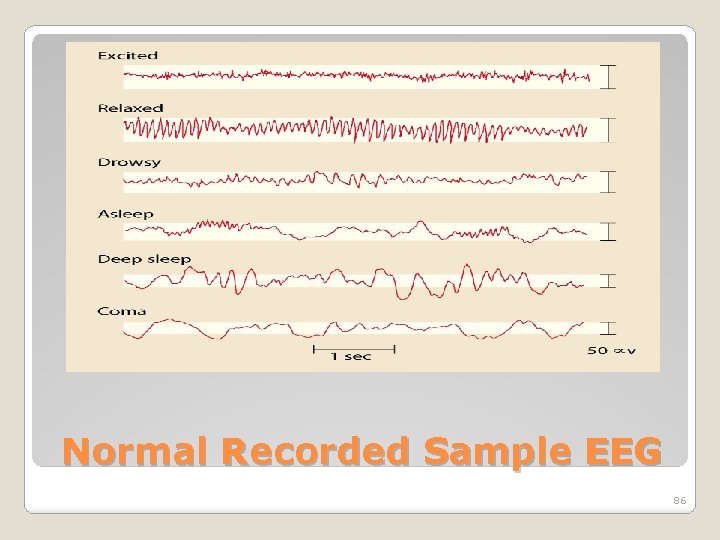
Normal Recorded Sample EEG 86
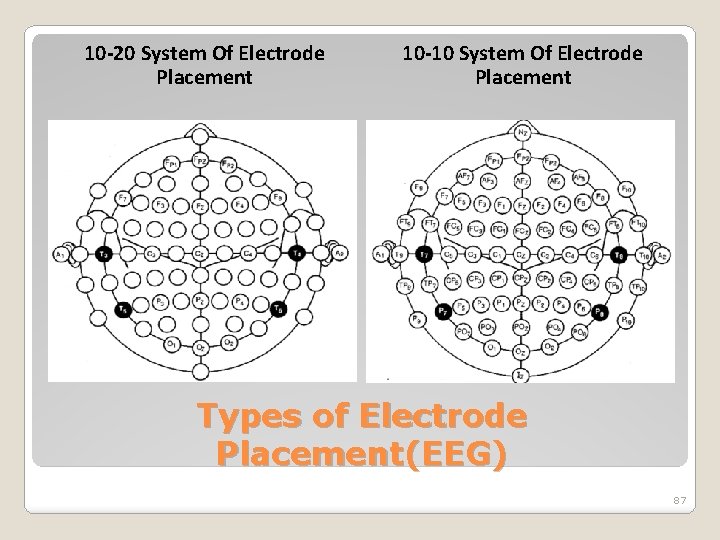
10 -20 System Of Electrode Placement 10 -10 System Of Electrode Placement Types of Electrode Placement(EEG) 87
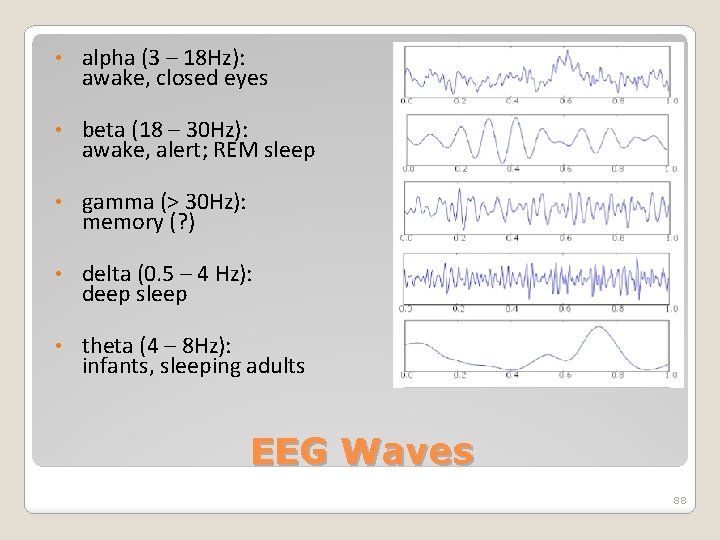
• alpha (3 – 18 Hz): awake, closed eyes • beta (18 – 30 Hz): awake, alert; REM sleep • gamma (> 30 Hz): memory (? ) • delta (0. 5 – 4 Hz): deep sleep • theta (4 – 8 Hz): infants, sleeping adults EEG Waves 88
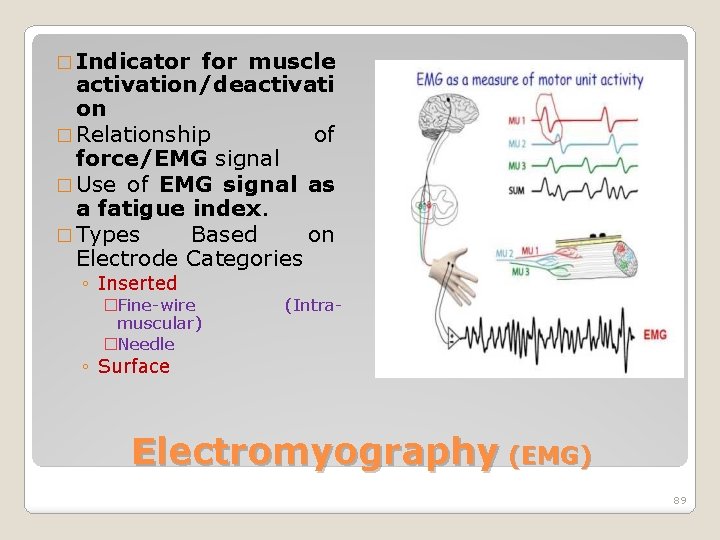
� Indicator for muscle activation/deactivati on � Relationship of force/EMG signal � Use of EMG signal as a fatigue index. � Types Based on Electrode Categories ◦ Inserted �Fine-wire muscular) �Needle (Intra- ◦ Surface Electromyography (EMG) 89
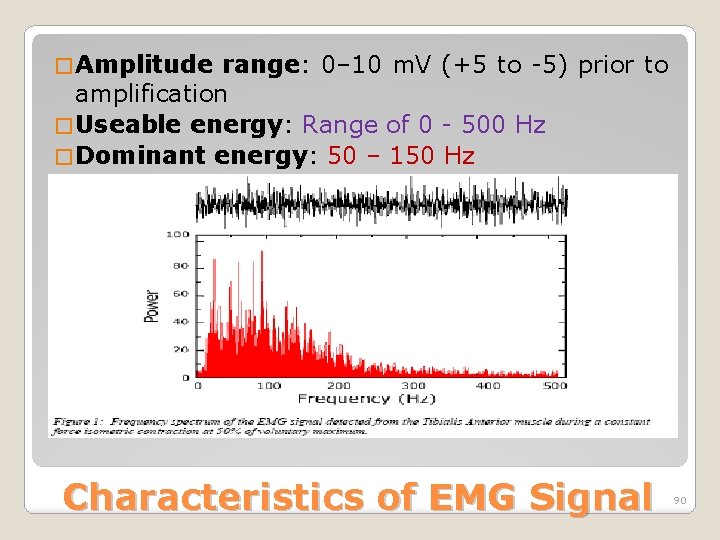
� Amplitude range: 0– 10 m. V (+5 to -5) prior to amplification � Useable energy: Range of 0 - 500 Hz � Dominant energy: 50 – 150 Hz Characteristics of EMG Signal 90
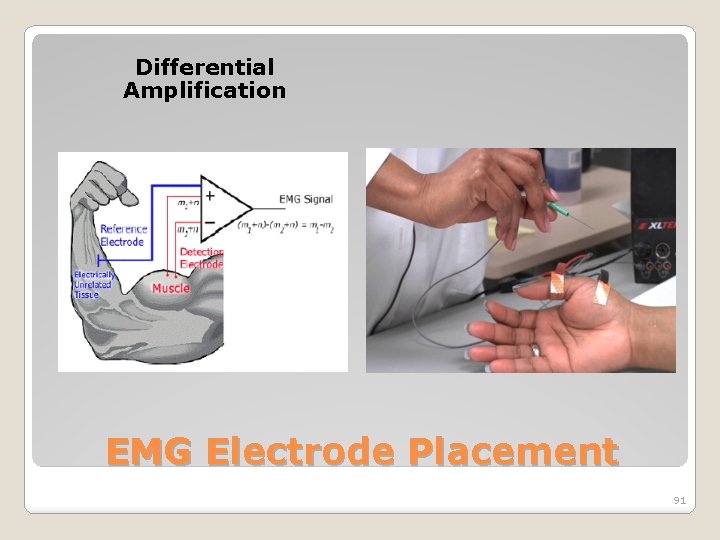
Differential Amplification EMG Electrode Placement 91
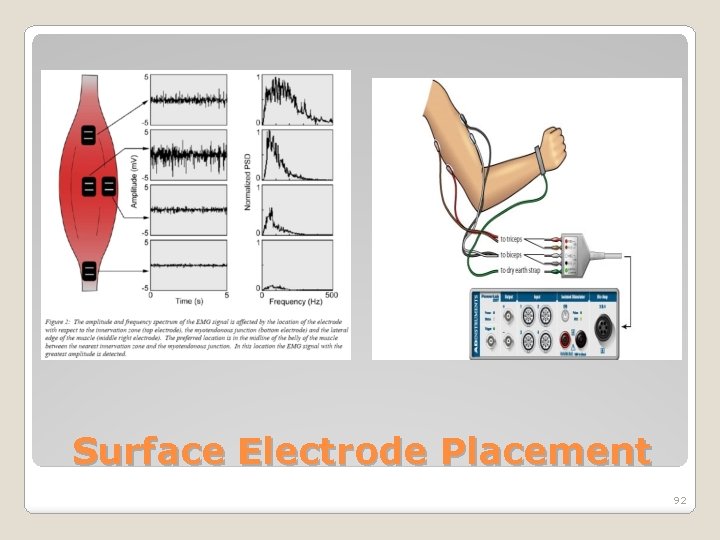
Surface Electrode Placement 92
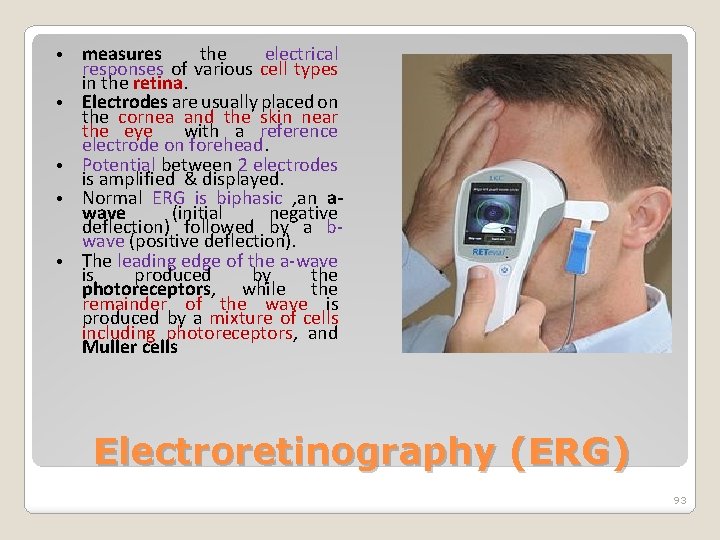
• • • measures the electrical responses of various cell types in the retina. Electrodes are usually placed on the cornea and the skin near the eye with a reference electrode on forehead. Potential between 2 electrodes is amplified & displayed. Normal ERG is biphasic , an awave (initial negative deflection) followed by a bwave (positive deflection). The leading edge of the a-wave is produced by the photoreceptors, while the remainder of the wave is produced by a mixture of cells including photoreceptors, and Muller cells Electroretinography (ERG) 93
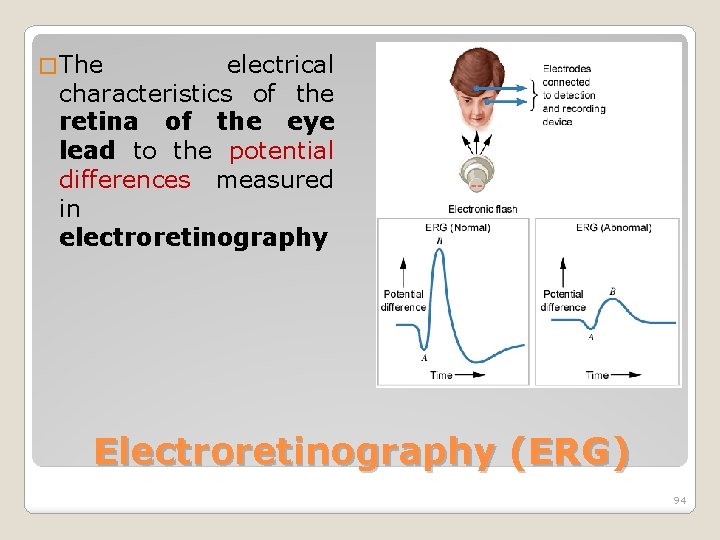
� The electrical characteristics of the retina of the eye lead to the potential differences measured in electroretinography Electroretinography (ERG) 94
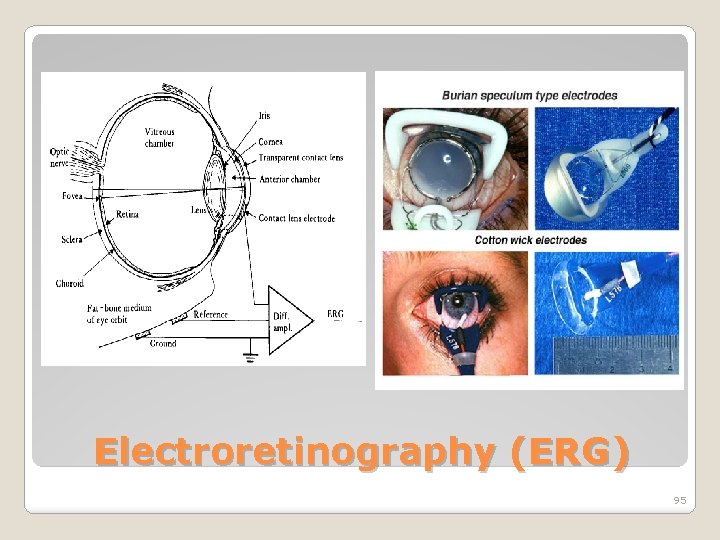
Electroretinography (ERG) 95
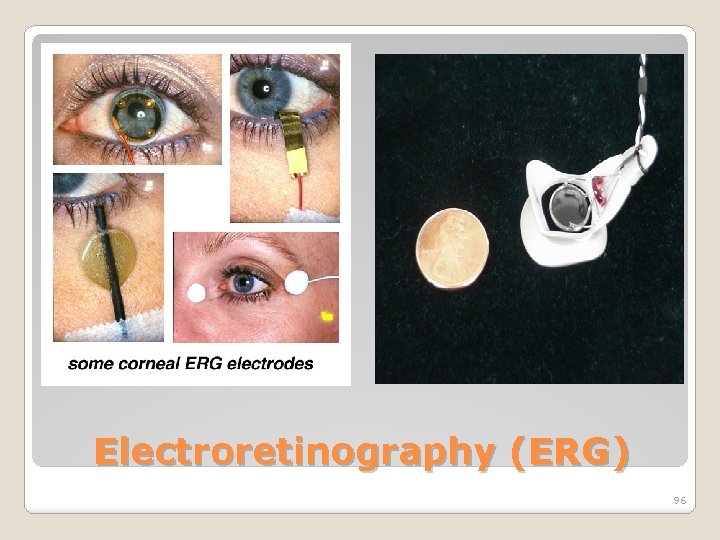
Electroretinography (ERG) 96
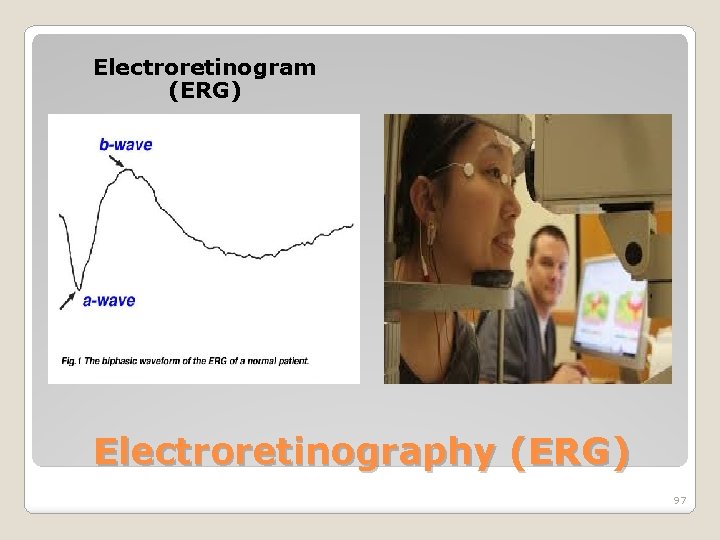
Electroretinogram (ERG) Electroretinography (ERG) 97

�Electrical safety is very important in hospitals as patients may be undergoing a diagnostic or treatment procedure where the protective effect of dry skin is reduced. �Also patients may be unattended, unconscious and may not respond normally to an electric current. �Further, electrically conductive solutions, such as blood and saline, are often present in patient treatment areas and may drip or spill on electrical equipment. Electrical Safety 98
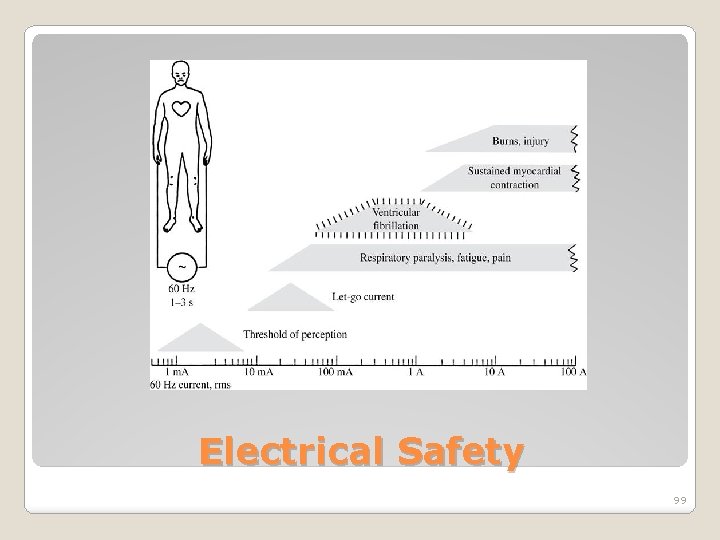
Electrical Safety 99

Electrical Safety 100

Electrical Safety 101

�https: //www. electrical 4 u. com/surface- electrodes/ �https: //www. electrical 4 u. com/biologicalamplifiers/ �https: //slideplayer. com/slide/3333523/ �J. Webster: Medical Instrumentation, References 102

103

104

105

106
- Slides: 106