BioMechanical Characteristics of Pressure Offloading Surfaces Occams Razor

Bio-Mechanical Characteristics of Pressure Offloading Surfaces

“Occam’s Razor” “The solution to a problem with multiple subsets of possible solutions is the simplest (most linear) answer” “Cutting Through the Bull”

The Challenge Defined in a Nut Shell (Bio-Mechanical/Hemodynamic) Maintaining a bio-mechanical environment which does not interfere with the level of peripheral blood flow required to support normal tissue metabolism as well as maintaining proper soft tissue symmetry Bio-Mechanical Culprit: Gravity + Mass = Pressure

Mechanical Forces ØPressure: is a static, scalar mechanical force in its purest form. Without a defined direction it cannot cause a Subcutaneous Infarction ØShear: is a quantifiable force created by definable vectored combinations of pressure. As an example horizontal and vertical shear

The Root Bio-Mechanical Cause of a Subcutaneous Infarction is “Vertical Shear” NOT Pressure ØWhat is Vertical Shear? ØA surface supporting an object is a mirror reflecting energy (pressure) back to the object in suspension Horizontal Vertical “For every action we have an equal an opposite reaction” …Hopefully
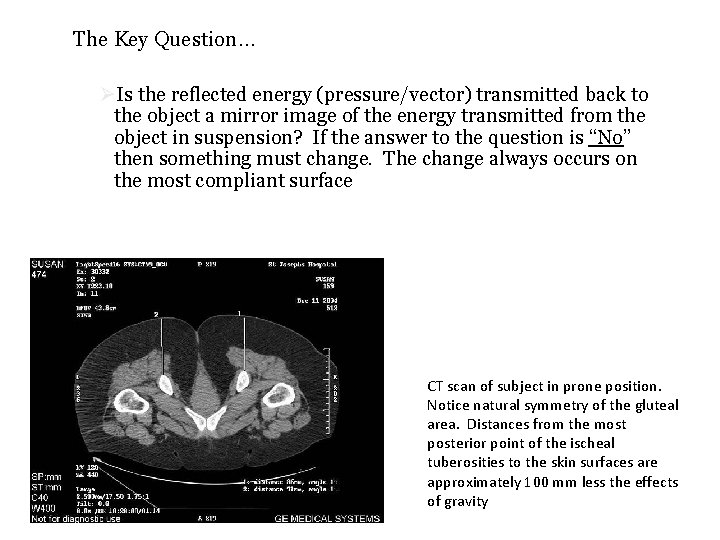
The Key Question… ØIs the reflected energy (pressure/vector) transmitted back to the object a mirror image of the energy transmitted from the object in suspension? If the answer to the question is “No” then something must change. The change always occurs on the most compliant surface CT scan of subject in prone position. Notice natural symmetry of the gluteal area. Distances from the most posterior point of the ischeal tuberosities to the skin surfaces are approximately 100 mm less the effects of gravity
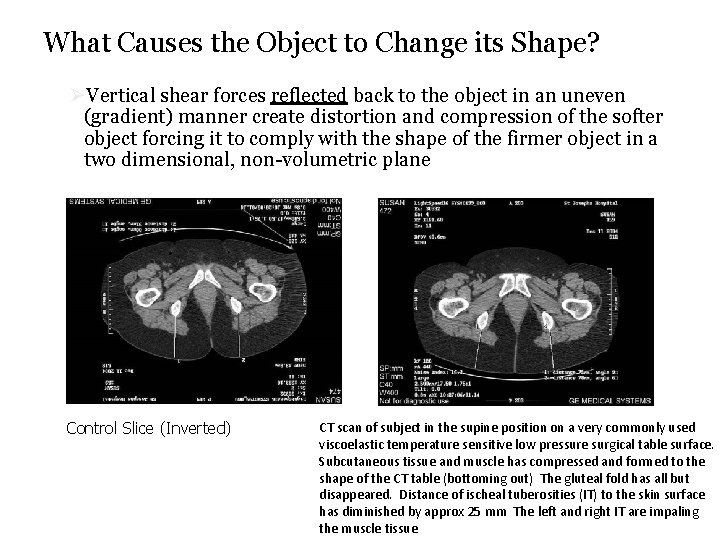
What Causes the Object to Change its Shape? ØVertical shear forces reflected back to the object in an uneven (gradient) manner create distortion and compression of the softer object forcing it to comply with the shape of the firmer object in a two dimensional, non-volumetric plane Control Slice (Inverted) CT scan of subject in the supine position on a very commonly used viscoelastic temperature sensitive low pressure surgical table surface. Subcutaneous tissue and muscle has compressed and formed to the shape of the CT table (bottoming out) The gluteal fold has all but disappeared. Distance of ischeal tuberosities (IT) to the skin surface has diminished by approx 25 mm The left and right IT are impaling the muscle tissue

Visualizing the Reality of the Situation… ØRemember the human body occupies a three dimensional plane… We are not flat we are slightly cylindrical. In this world the sum of the angles of a triangle does not equal 180 degrees

Bio-Mechanics Will Set You Free… “The support surface industry thinks in a two dimensional, Euclidian (Flat) world… It makes buying clothes a lot simpler… In most cases they do not have a clear grasp/understanding of the technology they are promoting let alone convey this information correctly to the end user” Until we change our way of visualizing and evaluating the efficacy of what is commonly referred to as a therapeutic support surface we are all in big trouble… ”The Doughnut Theory”, “Zero Pressure Theory” ?

“The Most Ideal But Most Clinically Impractical Support Medium” What is it?

Lets Try to Incorporate the Ideal Model Into a Practical Clinical Solution, But Before We Do That We Need To Understand What It Is We Are Trying To Accomplish From a Physiological Prospective Definitions: A Subcutaneous Infarction (SI) – Mechanical stress induced ischemic necrosis of three dimensional soft tissue predominantly of nutritionally and mobility impaired individuals due to placement on a non-compliant support surface Would a Myocardial Infarction or a cerebral infarction be a reasonable physiological analog? After all they are all a consequence of the failure of localized circulation? Well nourished 48 year old male underwent a 5 hour cardiac surgery procedure (CABG) Torsion alopecia and reddening on the scalp present immediately post-op. Pressure sore appeared on the buttocks and scalp approximately 10 days post-op. Patient was fully ambulatory

Notice the total lack of the use of the terms “Pressure Ulcer”, “Decubitus Ulcer” or “Bed Sore” in our definition! Key Terms In Our Definition: Ø Ø Mechanical Stress Induced Three Dimensional Soft Tissue

A Different Perspective We want to deemphasize the term pressure as it only applies in a two dimensional space such as skin interface pressure/pressure mapping. A clinically meaningless and dangerous method of evaluating a support medium. As well as the terms bed and Decubitus as they only define a physical location or position of the subject. Why not “wheelchair sore”? Concentrating on pressure alone deemphasized the need to engage the subject in a three dimensional volumetric environment
What exactly is soft tissue stress? Tissue Stress is the mechanical response to vertical shear created by gradient pressures reflected from a poorly anatomically profiled support medium Soft Tissue Stress causes tissue to strain (tensile stress) Tissue may tear along with microcirculation causing an eventual ischemic/hypoxic event. At a very minimum microcirculation may become compressed or elongated interrupting blood flow Aside from insults related to tissue stress we also have to contend with the primary mechanical cause of the ischemic event: Ø As layers of subcutaneous and muscle tissue distort to comply with vertical shear pressures, we have the additional mechanical stress caused by the bony prominences impaling into the fascia and muscle tissue at shear pressures many times greater than that which is observed at the skin/support surface interface (wedge amplification effect). The argument that a skin interface pressure measured below 32 mmhg is acceptable needs to be tossed out the window. In the three dimensional world of SI’s it’s not reality

Classification of Support Devices Currently Available Pressure Redistribution 1. Static/non powered 2. Dynamic/powered Non-pressure redistribution Alternating pressure surfaces Passive Intervention Active Intervention
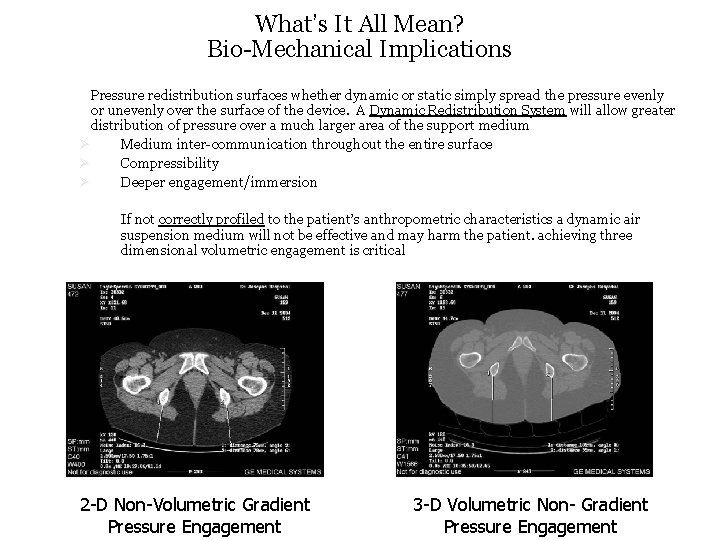
What’s It All Mean? Bio-Mechanical Implications Pressure redistribution surfaces whether dynamic or static simply spread the pressure evenly or unevenly over the surface of the device. A Dynamic Redistribution System will allow greater distribution of pressure over a much larger area of the support medium Ø Medium inter-communication throughout the entire surface Ø Compressibility Ø Deeper engagement/immersion If not correctly profiled to the patient’s anthropometric characteristics a dynamic air suspension medium will not be effective and may harm the patient. achieving three dimensional volumetric engagement is critical 2 -D Non-Volumetric Gradient Pressure Engagement 3 -D Volumetric Non- Gradient Pressure Engagement

Air Fluidized Therapy Proper profiling is not an issue with an air fluidized bed a true three dimensional support surface. (Some limitations on surface area), (bad for taller and contracted people) Ideal for skin flaps and grafts from a bio-mechanical prospective. This does not apply to hybrid systems employing both air suspension and fluidized surfaces

Static Surfaces Static surfaces redistribute pressure over a much smaller localized area surrounding a bony prominence. The ability of a static surface to redistribute pressure is directly related to its surface area and depth

The Myths and Realities of… “Alternating Pressure Surfaces” “ZERO PRESSURE” What could be better… Lower average interface pressures than a “Low Air Loss Surface” since half the surface is always at Zero Pressure… More effective Pressure relief… …Lower cost

Bio-Mechanical Considerations of Alternating Pressure Considerations: Very high vertical shear generation with gross deformation of soft tissue Severe mechanical trauma for aging skin… Why? Less moisture. . . Decreased collagen formation… Loss of elasticity… Pressure relief or HYPOXIA? Pressure redistribution/relief or Reactive Hyperemia? Which is it? Can it be both? Reperfusion Injury…

Do We Agree With These Concepts Ø Q: What Causes Pressure Sores? A: The primary and most common cause of pressure sores is constant or excessive pressure to a bony prominence. Patients who are immobile, even for a short period of time, such as during an operation, can begin the development of a pressure wound. Other causes include heat, moisture (such as perspiration), shear, friction and nutrition. Ø Q: What is Alternating Pressure? A: Alternating Pressure is the industry term for the sequential inflation and deflation of air cells in the mattress to address constant pressure, the leading cause of pressure sores. An electronic controller, which is usually placed on the footboard of the bed, delivers a continuous flow of air into the mattress. The mattress is made up of a series of air cells. The inflated air cells support the patient’s body while on the mattress. The deflated air cells allow nothing to touch the rest of the body therefore providing pressure relief. The electronic controller is programmed to alternate the air cells every few minutes, so that the deflated cells will become inflated while the inflated air cells become deflated. Ø Q: Do air cells run horizontally or vertically along the bed? A: For maximum therapy and patient comfort, air cells should run horizontally across the bed. This ensures that the patient’s body receives both support and pressure relief from head to foot. Ø Q: Do all Alternating Pressure systems provide the same therapy? A: No. Since it is the deflated air cells that provide therapy, it is important that the system have the capability to deflate or remove, the air cell away from the body as much as possible. Some systems claim to be alternating pressure but studies show there is little, if any, differentiation between the inflated and the deflated air cells. Some systems deflate every third air cell instead of every other. This means that the patient is only receiving therapy over 1/3 of the body at one time instead of the ideal 1/2 of the body. It is crucial to achieve a proper balance between the deflated and inflated air cells. While the deflated air cells provide pressure relief, it is also important to provide just enough inflated pressure to appropriately support the patient’s weight, so the patient doesn’t hit the bottom of the mattress (termed “bottoming-out”). Ø Q: What is Low Air Loss? A: Low Air Loss is the industry term for a therapeutic mattress system where low volumes of air escape out of the mattress. While the purpose of alternating pressure is to address constant pressure, low air loss assists in the management of heat and moisture, two other causes of pressure sores. Ø Q: Do all Low Air Loss systems provide the same therapy? A: No. In order for a low air loss system to benefit the patient, air must somehow reach the patient’s skin. It is common for inexpensive systems to have air escape through pinholes in the air cells. Once the cover or sheet is placed on top of the air cells, air is never allowed to reach the patient’s skin and little, if any, therapy is being provided. The most effective low air loss systems allow a gentle and diffused flow of air to directly reach the patient’s skin.

Low Air Loss, What Is It? What is… “True Low Air Loss”? “False Low Air Loss? What is “Air Loss” anyway? Is my automobile true low air loss or false low air loss? Is my vacuum cleaner true low air loss? What do these questions have in common? Would a dynamic air suspension system operate if it did not vent air? How much air vented against the patient’s skin is therapeutic in nature. Objective or subjective data? Perhaps it may vary with metabolic activity… One setting not good for everyone… Should Insensible Water Loss be a consideration?
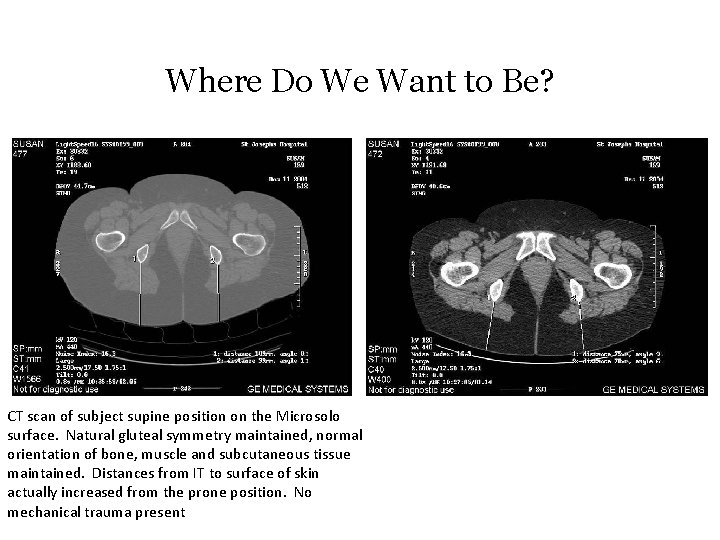
Where Do We Want to Be? CT scan of subject supine position on the Microsolo surface. Natural gluteal symmetry maintained, normal orientation of bone, muscle and subcutaneous tissue maintained. Distances from IT to surface of skin actually increased from the prone position. No mechanical trauma present
- Slides: 23