BIOLOGICAL PRINCIPLES IN FPD The principles of tooth

BIOLOGICAL PRINCIPLES IN FPD

The principles of tooth preparation may be divided into: 1. Biological considerations 2. Mechanical considerations 3. Esthetic considerations
BIOLOGIC Conservation of tooth structure Avoidance of over contouring Supragingival margins Harmonious occlusion Protection against tooth fracture ESTHETIC MECHANICAL Retention form Resistance form Deformation Minimum display of metal Maximum thickness of porcelain Porcelain occlusal surfaces Subgingival margins

BIOLOGICAL CONSIDERATIONS 1. Adjacent teeth 2. Soft tissues 3. The tooth being prepared 4. Periodontium
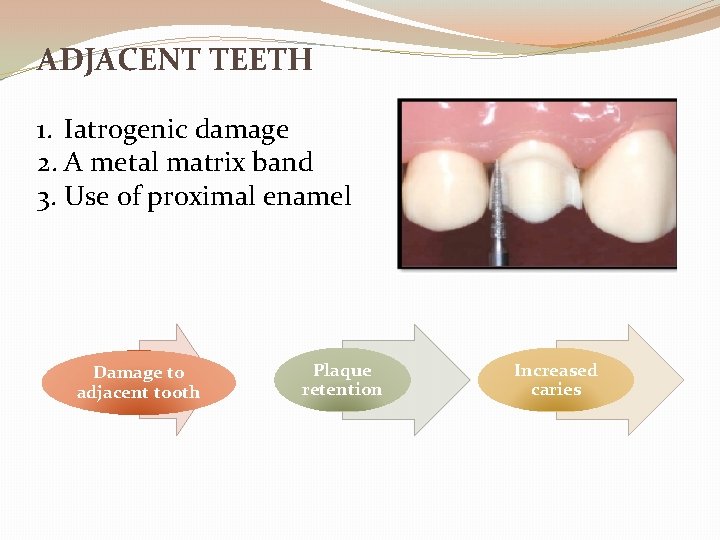
ADJACENT TEETH 1. Iatrogenic damage 2. A metal matrix band 3. Use of proximal enamel Damage to adjacent tooth Plaque retention Increased caries

PULP • Extreme temperature • Chemical irritation • Microorganisms • Reversible pulpitis • Irreversible pulpitis • Pulpal damage
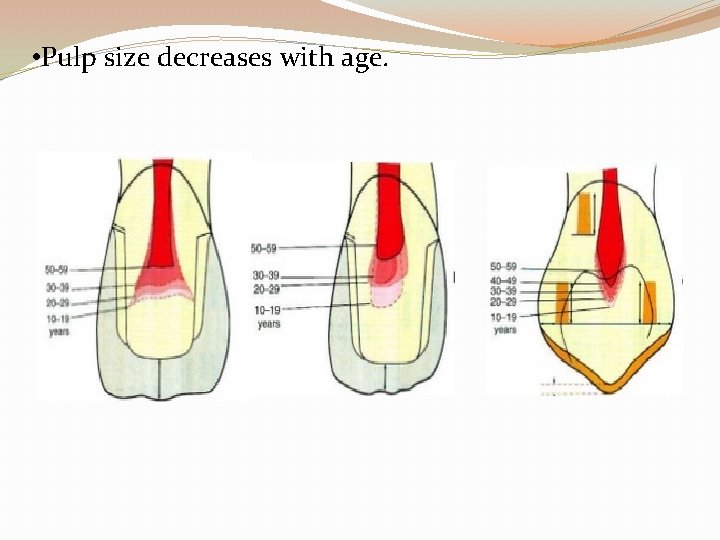
• Pulp size decreases with age.

TEMPERATURE • Excessive pressure • Higher rotational speeds • The type, shape, and condition of the cutting instrument

CHEMICAL ACTION • Chemical action of certain dental materials can cause pulpal damage when they are applied to freshly cut dentin. • Chemical agents are used for cleaning and degreasing tooth preparations.

BACTERIAL ACTION • Bacteria that were left behind or gained access to the dentin because of microleakage. • Many dental materials like zinc phosphate cement have an antibacterial effect.

�The design of a preparation for a cast restoration & the execution of the design are governed by five principles: 1) Preservation of tooth structure 2) Retention & Resistance 3) Structural durability 4) Marginal integrity 5) Preservation of the periodontium
CONSERVATION OF TOOTH STRUCTURE Thickness of remaining dentin inversely proportional to the pulpal response DEPTH OF REDUCTION

GUIDELINES TO CONSERVE TOOTH STRUCTURE 1. Use of partial coverage rather than complete coverage restorations 2. Preparation of teeth with the minimum practical convergence angle (taper) between axial walls 3. Preparation of the occlusal surface so that reduction follows the anatomic planes to give uniform thickness in the restoration 4. Preparation of the axial surfaces so that a maximal thickness of residual tooth structure surrounding pulpal tissues is retained.
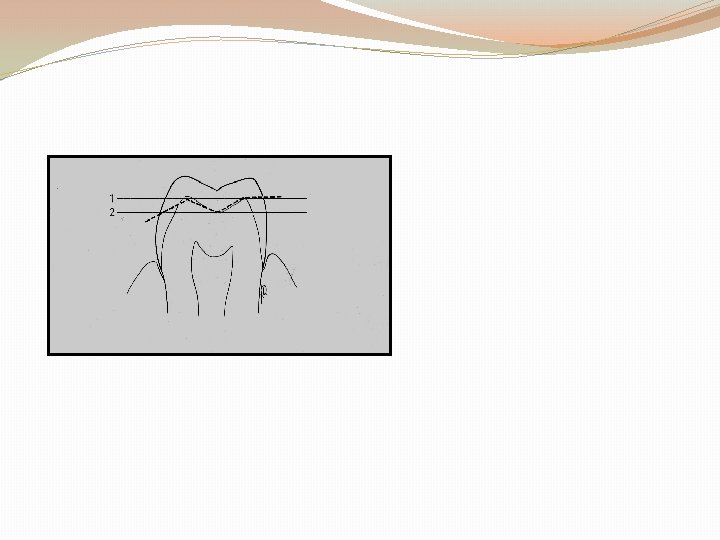

5. Selection of a margin geometry that is conservation and yet compatible with the other principles of tooth preparation. 6. Avoidance of unnecessary apical extension of the preparation.
Axial reduction Occlusal consideration s Contour CONSIDERATIONS AFFECTING FUTURE DENTAL HEALTH Preventing Margin tooth placement fracture Margin adaptation
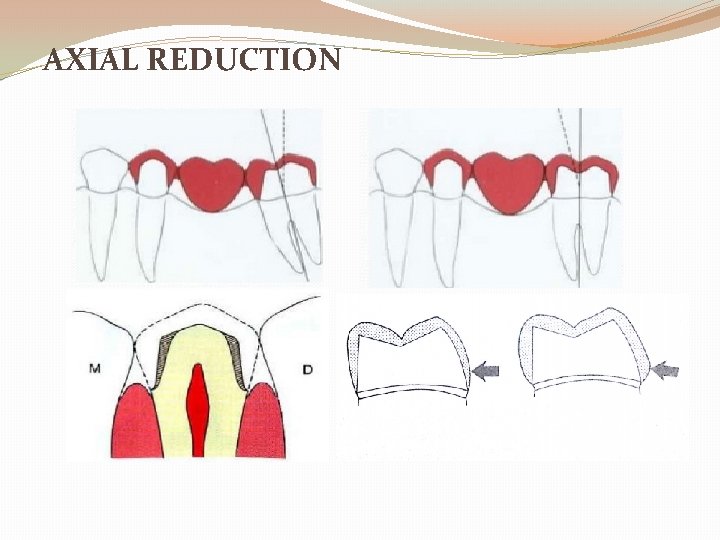
AXIAL REDUCTION


MECHANICAL CONSIDERATIONS: 3 factors: - • Retention form • Resistance form • Preventing deformation of restoration

Retention & Resistance For a restoration to accomplish its purpose, it must stay in place on the tooth. RETENTION: - prevents the removal of the restoration along the path of insertion or long axis of the tooth preparation. RESISTANCE: - prevents dislodgment of the restoration by forces directed in an apical or oblique direction & prevents any movement of the restoration under occlusal forces.

1. Retention Form: The quality of the restoration that prevents the restoration from being dislodged by force parallel to the path of withdrawal called as retention form. Various factors: 1. Magnitude of dislodging force 2. Geometry of tooth preparation 3. Roughness of fitting surface of restoration 4. Materials being cemented 5. Film thickness of luting agents

a) Magnitude of dislodging forces: Forces can be exerted with a floss under the connectors but mainly force is exerted by adhesiveness of foods. The magnitude of dislodging force depends on: 1. Stickiness of food 2. Surface area of restorations 3. Texture of restoration being pulled b) Geometry of tooth preparation: Most fixed prosthesis depend on the geometric form of tooth preparation rather than on adhesion tooth retention as most of the dental cements are non-adhesive and act by increasing the frictional resistance between tooth and restoration. Cement is effective only if the restoration has a single path of withdrawal. .

The more nearly parallel the opposing walls of a preparation, the greater should be the retention. Most retentive preparation should be one with parallel walls, but the parallel walls are impossible to create in the mouth without producing preparation undercuts. An UNDERCUT is defined as a divergence between opposing axial walls, or wall segments, in a cervicalocclusal direction.

Taper: Parallel walls give maximum retention but sometimes undercuts may be created. Retention decreased as taper increased. E. g. Retention of GALILTH with 100 taper was half that of 50 taper. Recommended taper is 5 -80 with a rotary instrument held at constant angle.

Surface Area: • Crowns with long axial walls are more retentive than crowns with short axial walls. • Molar crowns are more retentive than premolar crowns of similar taper. Stress Concentration: Cohesive failure occurs within the cement as the stress within cement is less than that of induced stresses. Stresses are seen to concentrate around the junction of axial and occlusal surfaces. Types of Preparation: It is seen that retention of complete crowns is almost twice as that of partial coverage. Grooves or boxes in a preparation which limit the path of withdrawal enhances the retention
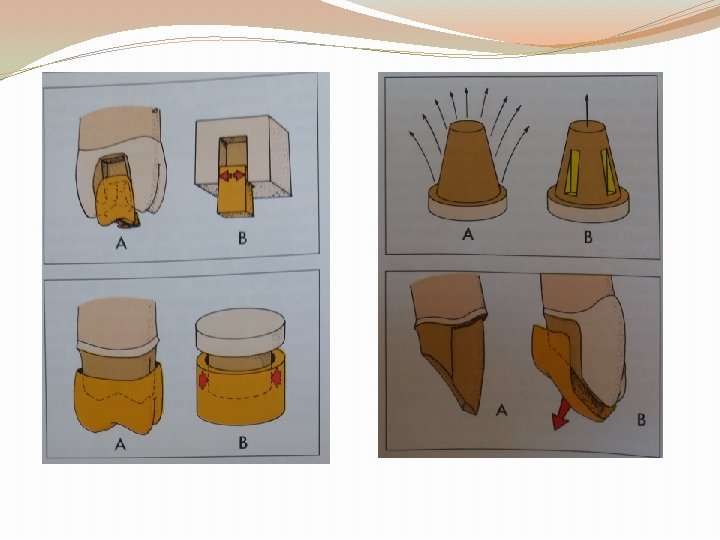
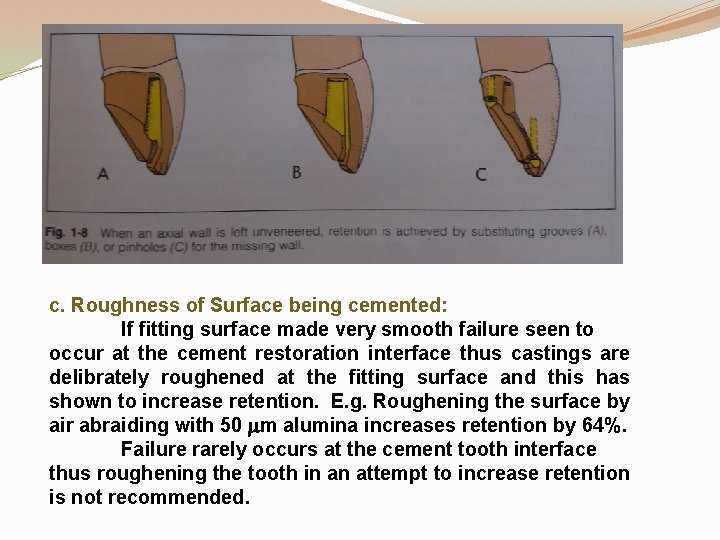
c. Roughness of Surface being cemented: If fitting surface made very smooth failure seen to occur at the cement restoration interface thus castings are delibrately roughened at the fitting surface and this has shown to increase retention. E. g. Roughening the surface by air abraiding with 50 m alumina increases retention by 64%. Failure rarely occurs at the cement tooth interface thus roughening the tooth in an attempt to increase retention is not recommended.

d. Materials being cemented: Retention is affected by both casting metal and core build up material. It is seen that the more reactive the alloy is the more will be retention with certain luting agents. So, base metal alloys are more reactive than the less reactive high gold content metals. A study examining adhesion between cement and core materials found that cement adhered better to amalgam than composite or cast gold. e. Type of luting agents: Adhesive resin cements are supposed to be most durable

FREEDOM OF DISPLACEMENT: �Retention is improved by geometrically limiting the numbers of paths along which a restoration can be removed from the tooth preparation. �Maximum retention is achieved when there is only one path.

LENGTH: �Occlusogingival length is an important factor in both retention & resistance. �Longer preparations will have more surface area & therefore will be more retentive. �The length must be great enough to interfere with the arc of casting pivoting about a point on the margin on the opposite side of the restoration.

1. Retention is influenced by occlusogingival length of the axial walls 2. Proximal walls should be nearly equal in vertical length (the retention of the retainer is only as effective as the shortest wall) 3. Proximal walls ideally possess a 5 to 8⁰ taper 4. Facial and lingual walls are more convergent from the occlusal one – third to provide a narrowed occlusal table. 5. Short axial walls require accessory methods of retention
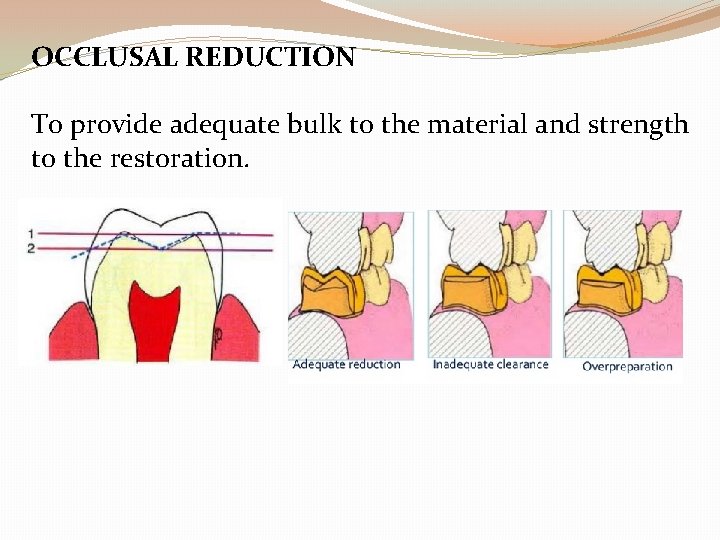
OCCLUSAL REDUCTION To provide adequate bulk to the material and strength to the restoration.

OCCLUSAL REDUCTION: - Gold alloys – 1. 5 mm (FC) & 1 mm(NFC) Metal-ceramic crowns- 1. 5 -2 mm(FC)&1 -1. 5 mm(NFC) All-ceramic crowns – 2 mm of clearance on preparation
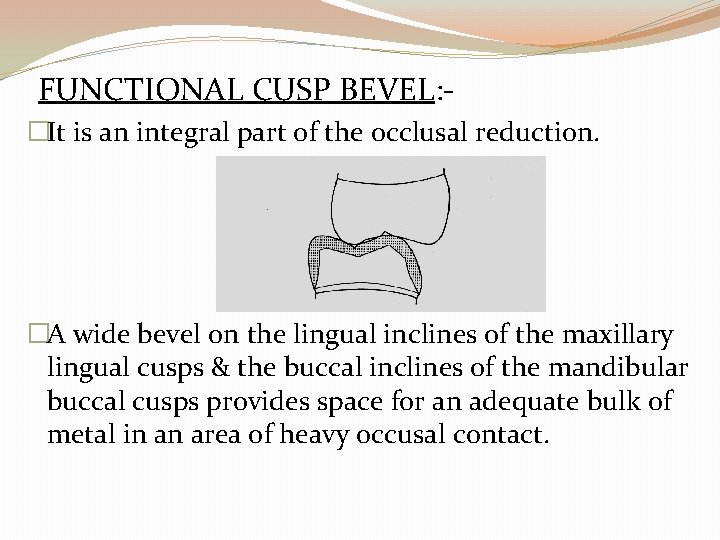
FUNCTIONAL CUSP BEVEL: �It is an integral part of the occlusal reduction. �A wide bevel on the lingual inclines of the maxillary lingual cusps & the buccal inclines of the mandibular buccal cusps provides space for an adequate bulk of metal in an area of heavy occusal contact.
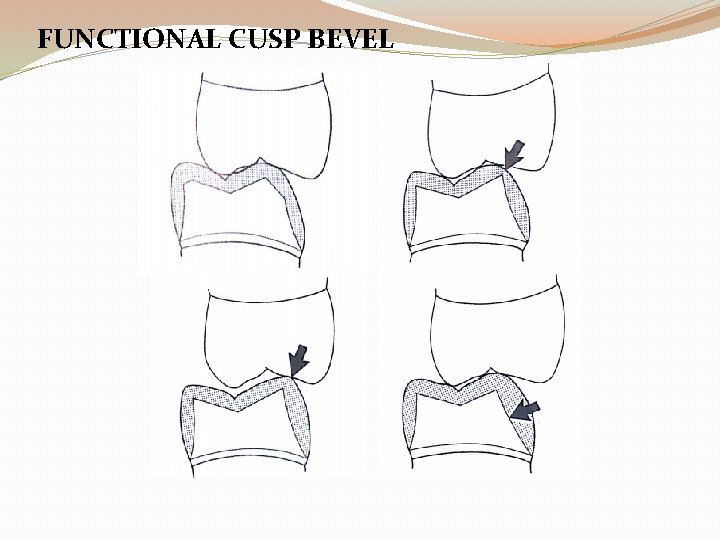
FUNCTIONAL CUSP BEVEL

Resistance Form: Restorations are also subjected to horizontal or oblique forces e. g. mastication/ parafunctional habits. Lateral forces tend to displace the restoration by causing rotation around the gingival margins. This rotation is prevented by areas of the preparation that are placed under compression called as Resistance areas. Many such areas make up the resistance form. Adequate resistance depends on: - • Magnitude and direction of dislodging forces • Geometry of tooth preparation • Physical properties of luting agents.
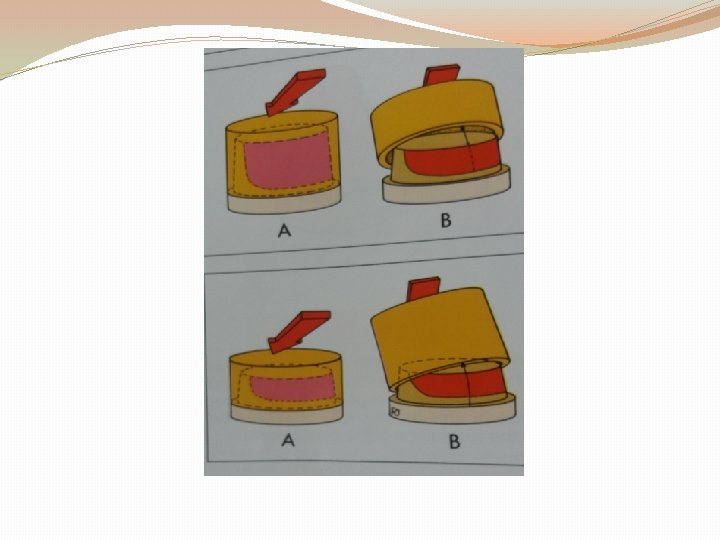

1. Magnitude and direction of dislodging forces: In normal occlusion biting force distributed over all the teeth. Similarly in FPD, occlusal load should be well distributed and favourably directed. In patients with pipe smoking, bruxism habits, oblique forces are exerted over FPDs. Thus, an ideal restoration should be able to withstand these forces as well as the normal axial forces. 2. Geometry of tooth preparation: Particular areas of axial walls help prevent rotation of the crown.
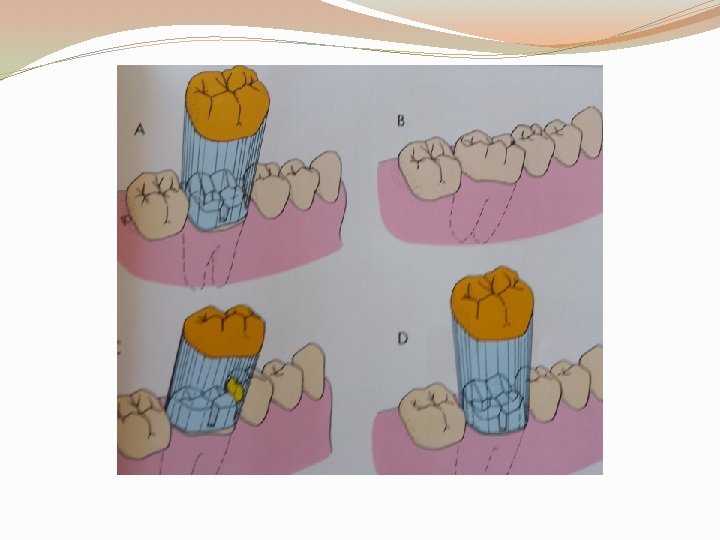
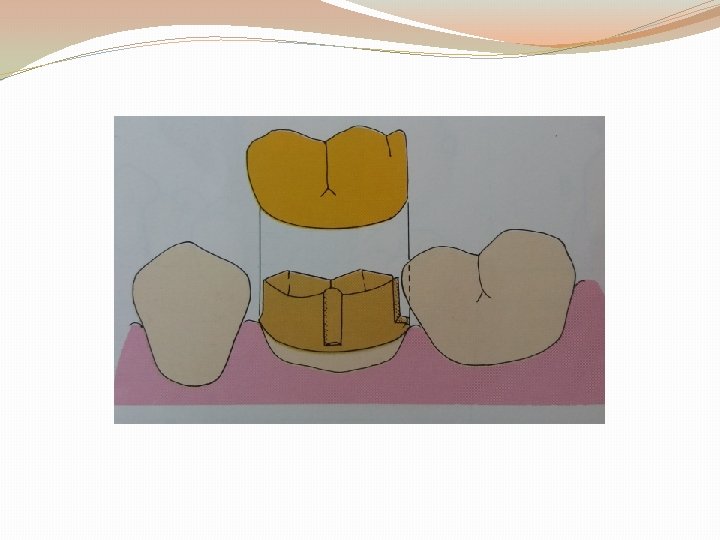

PATH OF INSERTION: �It is an imaginary line along which the restoration will be placed onto or removed from the preparation. �the paths of all the abutment preparations must parallel each other. �Surveying visually, since it is the primary means of insuring that the preparation is neither undercut nor over-tapered.
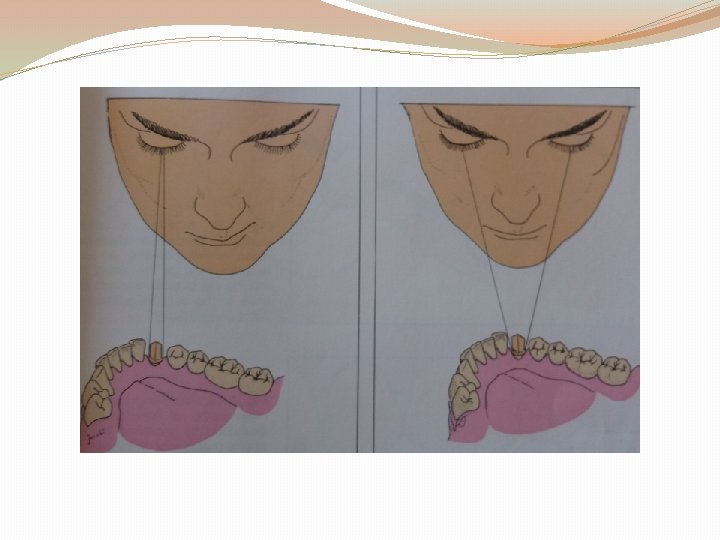
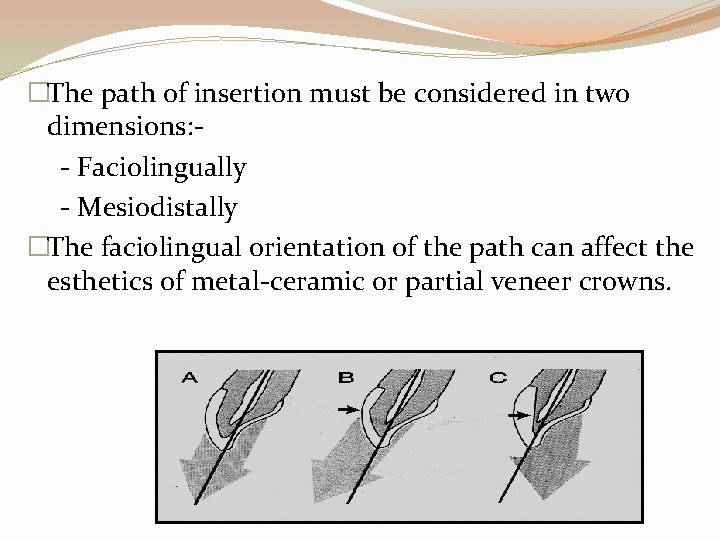
�The path of insertion must be considered in two dimensions: - Faciolingually - Mesiodistally �The faciolingual orientation of the path can affect the esthetics of metal-ceramic or partial veneer crowns.
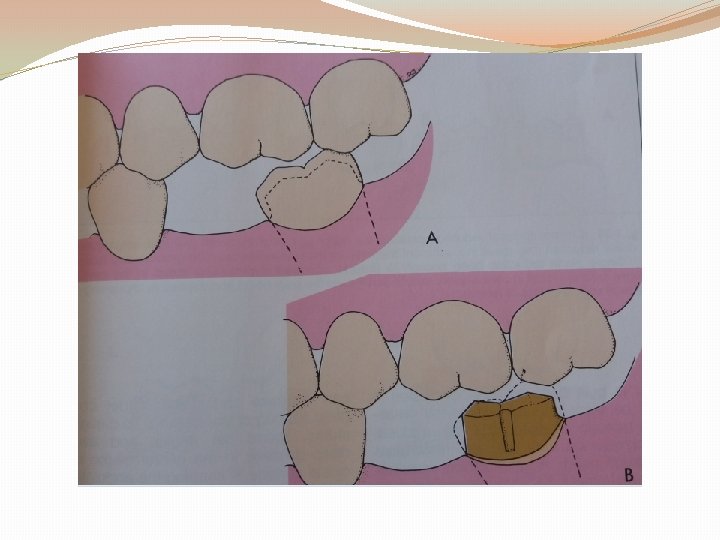

1. increase preparation taper and rounding of axial walls decreased resistance. 2. Shorter tooth preparation with large diameter little resistance form. 3. Partial coverage crown has less resistance than a complete coverage (as no buccal resistance areas). 4. Resistance can also be improved by placing grooves and boxes especially with walls being perpendicular to the direction of applied forces. U-shaped grooves better than V-shaped. These grooves and pinholes interfere with rotational movement and subject other areas of luting agent to compression.

5 ways to resist displacing forces: - • 4 -100 axial taper • Suitable gingival finish lines • Contouring and placing suitable contact areas • Incorporating occlusal locks, dove tails, boxes • Tapered and parallel pins.

Physical Properties of Luting Agent: According to ADA No. 8, the compressive strength of Zinc phosphate at 24 hrs must be more than 70 mpa. Silicophosphate has higher strength whereas GIC, Zinc polycarboxylate, and Zinc oxide eugenol have lesser. Increase in temperature alters the compressive strength e. g. reinforced zinc oxide eugenol when temperature increased from 230 C to body temperature compressive strength is halved. Zinc oxide eugenol has a higher modulus of elasticity than polycarboxylate cement. So, retention for polycarboxylate cement depends more on the taper of preparation than for Zinc oxide eugenol.

Deformation Can occur as a result of; • Inappropriate alloy selection • Inadequate tooth preparation • Poor metal ceramic framework Alloy Selection: • Type I and Type II gold for intracoronal cast restorations not for FPD’s. Type III and Type IV for FPD as they are harder and stronger, hardness can be further increased by heat treatment. • High noble metal content metal ceramic restorations have hardness equivalent to type IV alloys. • Ni-Cr alloys are harder indicated for long span bridges or where larger forces are expected.
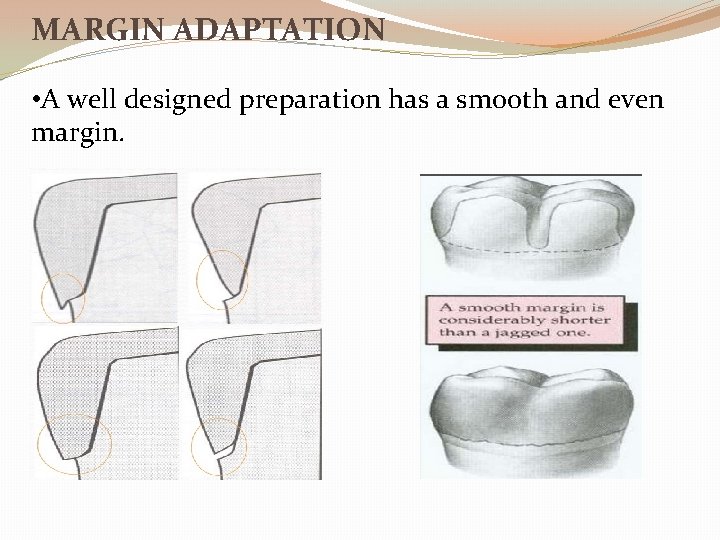
MARGIN ADAPTATION • A well designed preparation has a smooth and even margin.
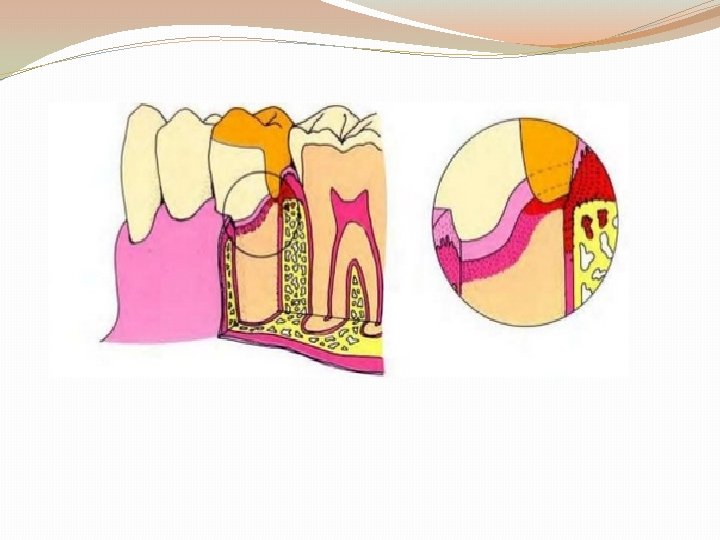

MARGIN GEOMETRY Guidelines for margin design: 1. Ease of preparation without overextension or unsupported enamel 2. Ease of identification in the impression and on the die 3. A distinct boundary to which the wax pattern can be finished 4. Sufficient bulk of material 5. Conservation of tooth structure

MARGIN PLACEMENT: �Whenever possible the margin of the preparation should be supragingival. ØAdvantages of supragingival margins are: - • They can be easily finished. • They are more easily kept clean • Easy to make impressions with less damage to soft tissue. • Restorations –easily evaluated –at recall.

Subgingival margin indications : 1. Dental caries, cervical erosion, or restorations extend subgingivally. 2. The proximal contact area extends to the gingival crest 3. Additional retention and/or resistance is needed. 4. The margin of a metal- ceramic crown is to be hidden behind the labiogingival crest 5. Root sensitivity cannot be controlled by more conservative procedures, such as the application of dentin bonding agents 6. Modification of the axial contour is indicated, as to provide an undercut to provide retention for the clasp of a partial removable dental prosthesis
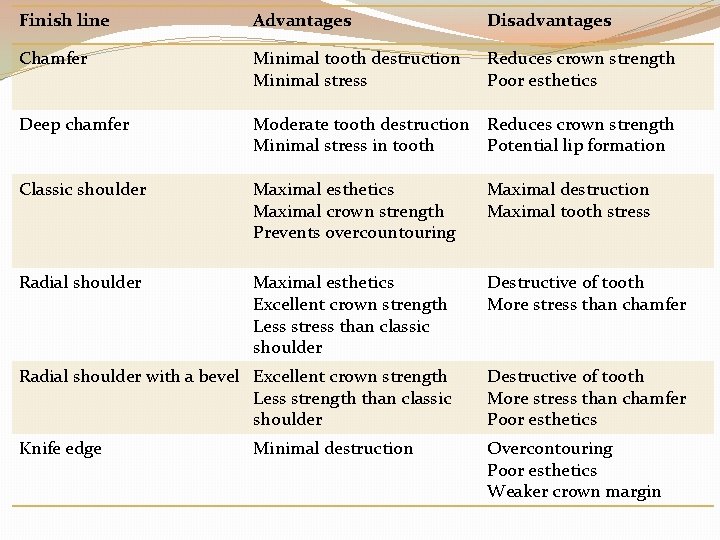
Finish line Advantages Disadvantages Chamfer Minimal tooth destruction Minimal stress Reduces crown strength Poor esthetics Deep chamfer Moderate tooth destruction Reduces crown strength Minimal stress in tooth Potential lip formation Classic shoulder Maximal esthetics Maximal crown strength Prevents overcountouring Maximal destruction Maximal tooth stress Radial shoulder Maximal esthetics Excellent crown strength Less stress than classic shoulder Destructive of tooth More stress than chamfer Radial shoulder with a bevel Excellent crown strength Less strength than classic shoulder Destructive of tooth More stress than chamfer Poor esthetics Knife edge Overcontouring Poor esthetics Weaker crown margin Minimal destruction

5. Preservation of periodontium The placement of finish lines has a direct bearing on the ease of fabricating a restoration & on the ultimate success of the restoration. Margins that are smooth & fully exposed to cleansing action give best results. Finish lines should be placed in enamel when it is possible to do so. Subgingival restorations are described as a major etiologic factor in periodontitis. The deeper the restoration margin resides in the gingival sulcus the greater the inflammatory response.

ESTHETIC CONSIDERATIONS • • • Make a full assessment of the appearance of each patient. Observe which teeth show while talking, smiling etc. The esthetic requirements are then made with relation to the oral hygiene needs and potential for diseases.

- Slides: 57