Biological markers research in Bipolar Disorder Pedro Zuzarte

Biological markers research in Bipolar Disorder Pedro Zuzarte Advanced Medical Research Institute of Canada University of Toronto, Canada University of Lisbon, Portugal

“The art of simplicity is a puzzle of complexity” (Douglas Horton)
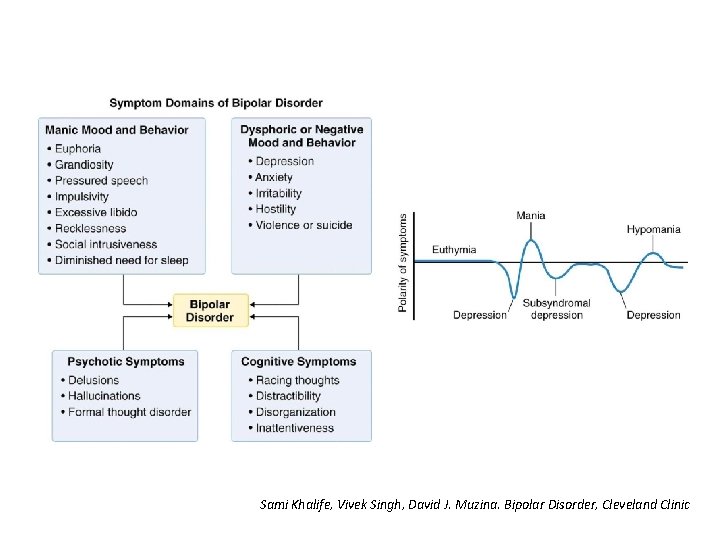
Sami Khalife, Vivek Singh, David J. Muzina. Bipolar Disorder, Cleveland Clinic
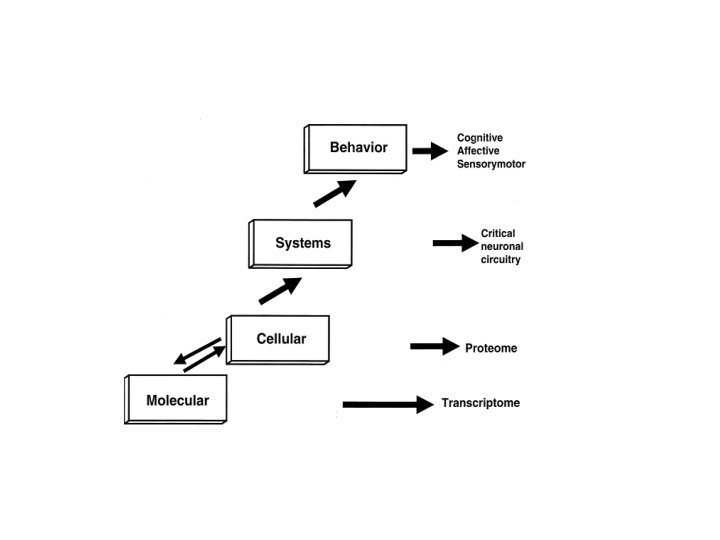
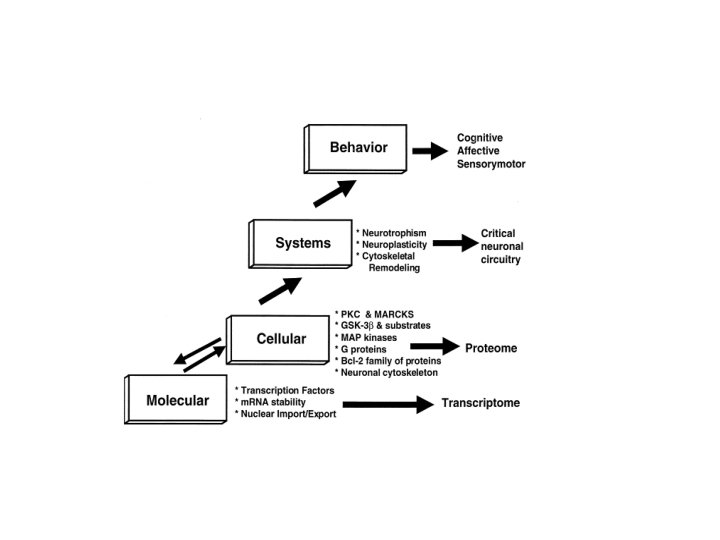
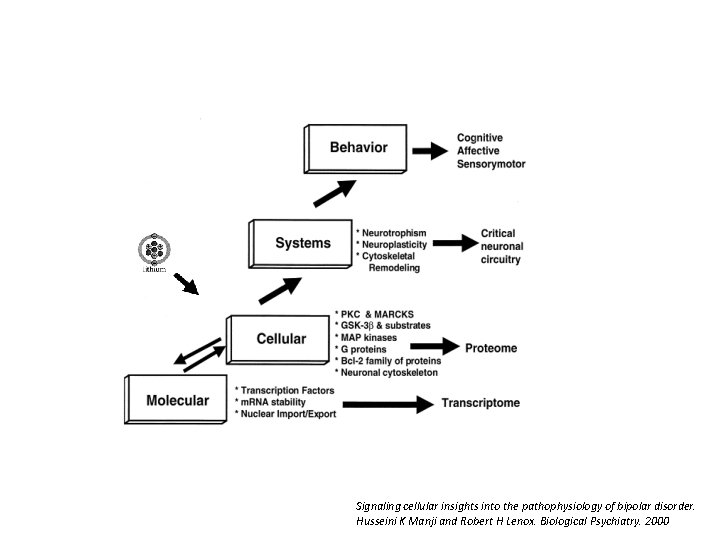
Signaling cellular insights into the pathophysiology of bipolar disorder. Husseini K Manji and Robert H Lenox. Biological Psychiatry. 2000
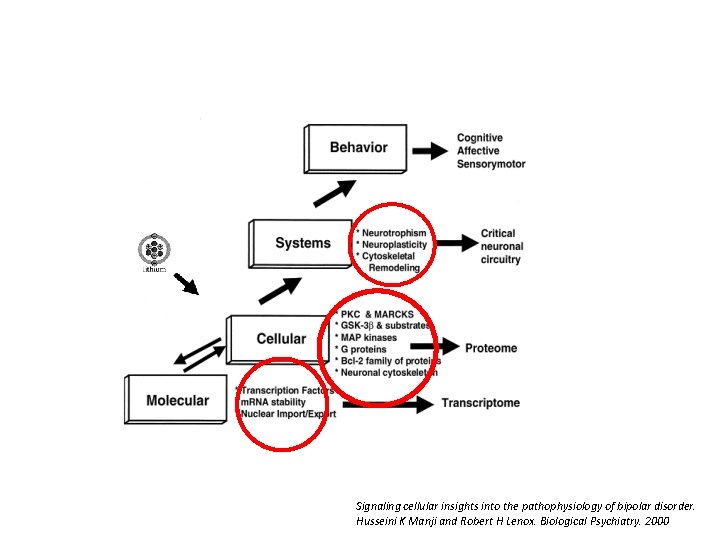
Signaling cellular insights into the pathophysiology of bipolar disorder. Husseini K Manji and Robert H Lenox. Biological Psychiatry. 2000

All the scientific findings in recent years are beginning to offer a provisional "unified field theory" of Bipolar Disorder seems to be a neurodevelopmental condition with interconnected functional abnormalities that often appear early in life and worsen over time
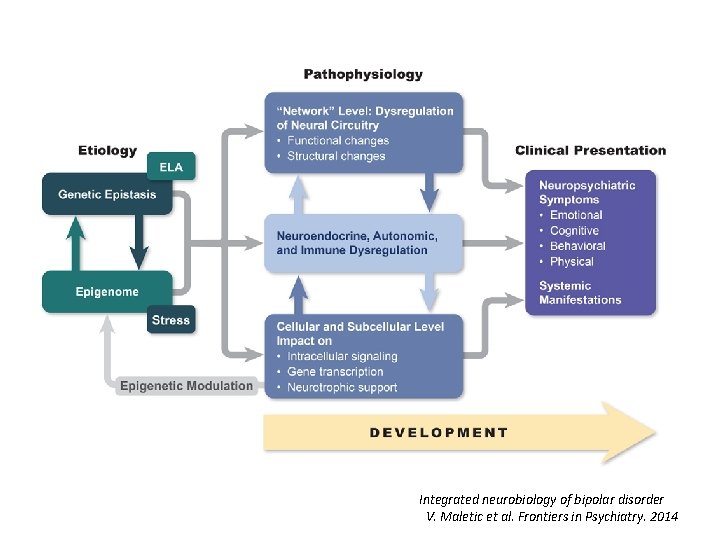
Integrated neurobiology of bipolar disorder V. Maletic et al. Frontiers in Psychiatry. 2014
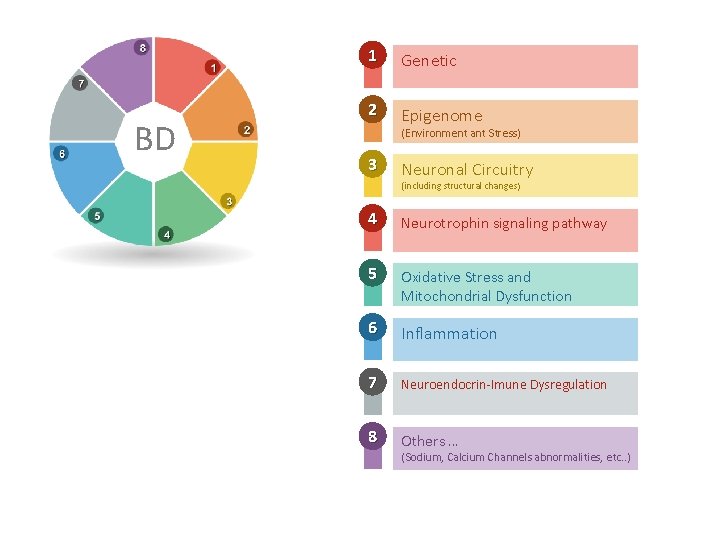
BD 1 Genetic 2 Epigenome (Environment ant Stress) 3 Neuronal Circuitry (including structural changes ) 4 Neurotrophin signaling pathway 5 Oxidative Stress and Mitochondrial Dysfunction 6 Inflammation 7 Neuroendocrin-Imune Dysregulation 8 Others … (Sodium, Calcium Channels abnormalities, etc. . )

Pathophysiological research promise the identification of “characteristics that are objectively measured and evaluated as indicators of normal biologic processes, pathogenic processes, or pharmacologic responses” to a therapeutic intervention Biomarkers: Medicines and emerging science EMEA (2014)
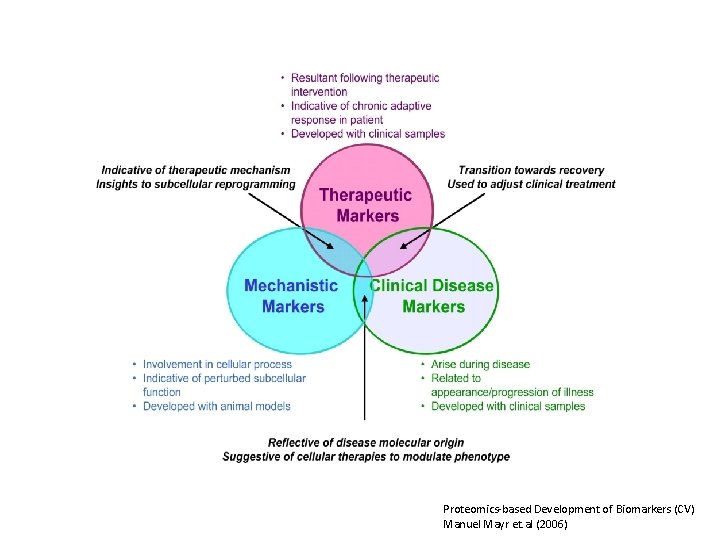
Proteomics-based Development of Biomarkers (CV) Manuel Mayr et. al (2006)
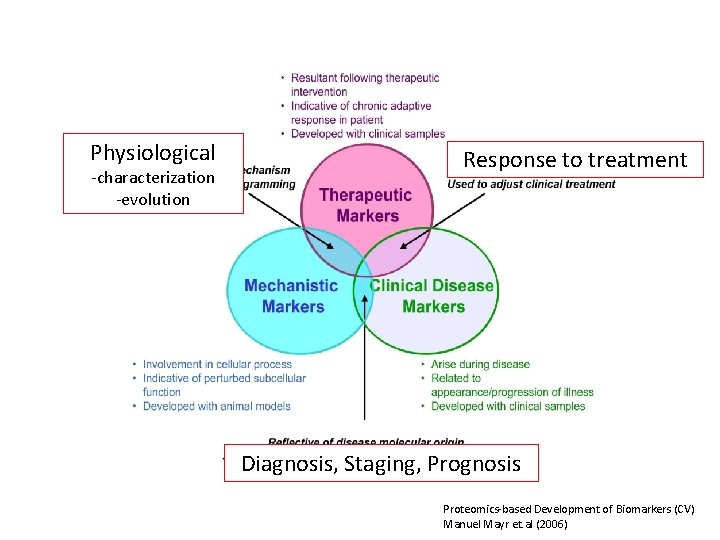
Physiological -characterization -evolution Response to treatment Diagnosis, Staging, Prognosis Proteomics-based Development of Biomarkers (CV) Manuel Mayr et. al (2006)
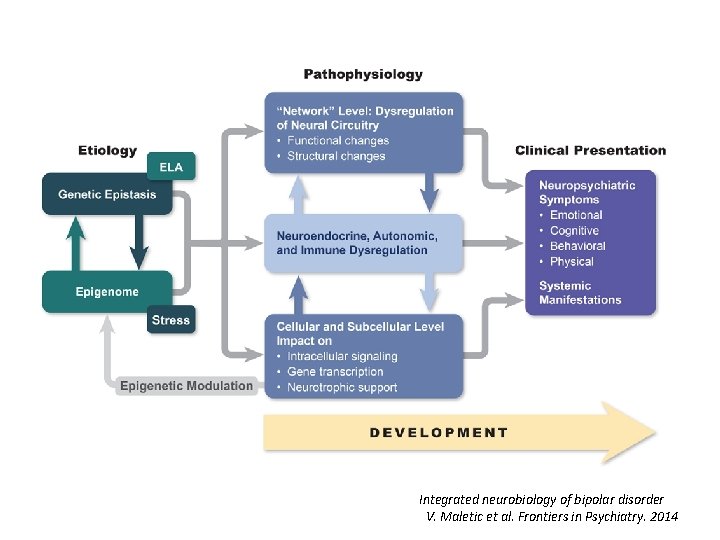
Integrated neurobiology of bipolar disorder V. Maletic et al. Frontiers in Psychiatry. 2014
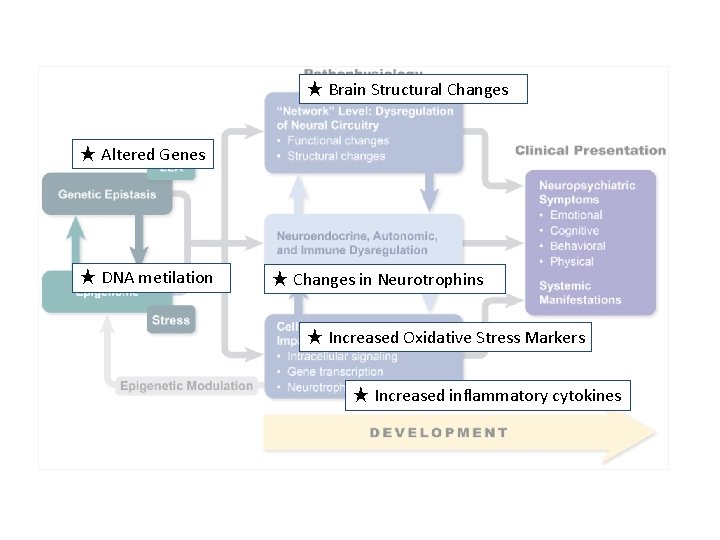
★ Brain Structural Changes ★ Altered Genes ★ DNA metilation ★ Changes in Neurotrophins ★ Increased Oxidative Stress Markers ★ Increased inflammatory cytokines

1. For this work we hypothesized that older patients with BD would have increased levels of oxidative stress, when compared to healthy individuals Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319
Background Oxidative stress is the process through which the production of reactive oxygen species (i. e. , free radicals) overwhelms the antioxidant system leading to potential damage to proteins, lipids and DNA 1 ROS (Reactive Oxigen Species) O 2 • -, OH • , NO • . . . Superóxido dismutase (SOD) Glutationa peroxidase (GPx) Catalase (CAT) Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319

Background Oxidative stress damage has been consistently reported in younger patients with bipolar disorder 2 -3 In both from postmortem brain 4 -9 and blood samples 10 -17: • • Increased oxidative damage to proteins in postmortem prefrontal cortex from patients with BD 4, 5 Increased nitration-induced damage to protein tyrosine has been seen in both BD and SCH 4, 5 Lipids are also consistent targets of oxidation (i. e. , lipid peroxidation) in patients with BD Lipid peroxidation in the anterior cingulate cortex 19 and prefrontal cortex 5… Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319

Background A meta-analysis revealed that increased serum level of lipid peroxidation is the most consistent finding of oxidative stress associated with BD* *Oxidative stress markers in bipolar disorder: a meta-analysis. J Affect Disord 2008; 111: 135 e 144 Andreazza AC, Frey BN, et al Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319

Background Oxidative stress is also associated with brain aging 20 This is demonstrated by accumulation of oxidative damage 21 to proteins and lipids and the negative association between aging and the glutathione enzymes, the major antioxidant system. 22 Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319
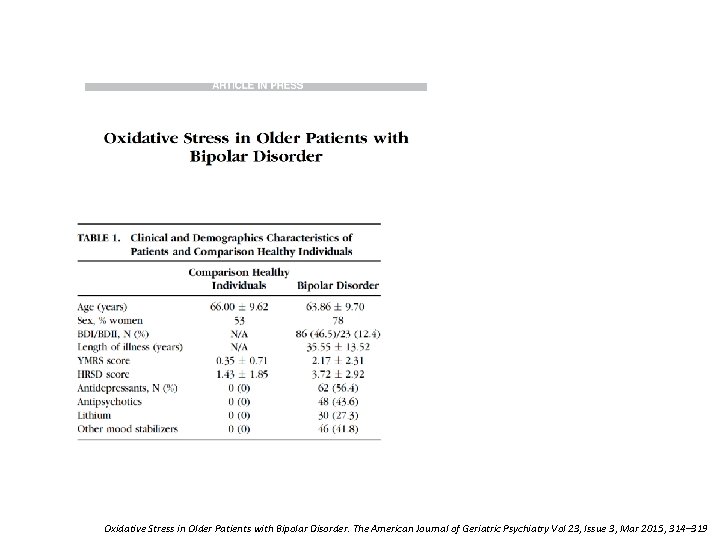
Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319
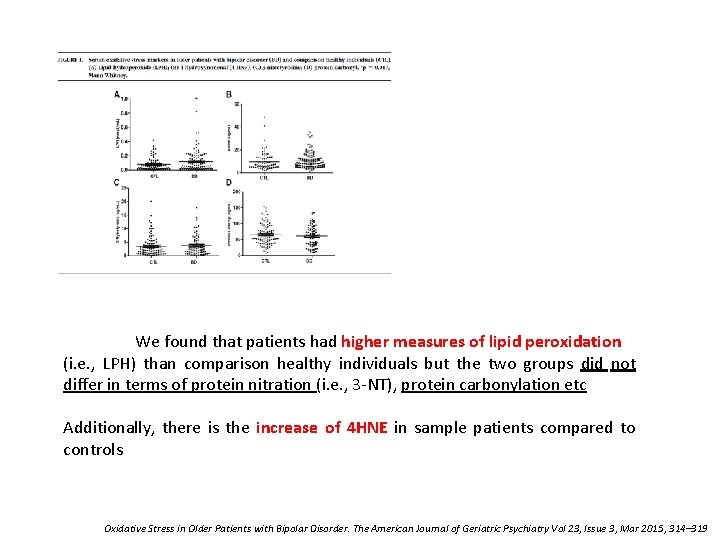
We found that patients had higher measures of lipid peroxidation (i. e. , LPH) than comparison healthy individuals but the two groups did not differ in terms of protein nitration (i. e. , 3 -NT), protein carbonylation etc Additionally, there is the increase of 4 HNE in sample patients compared to controls Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319
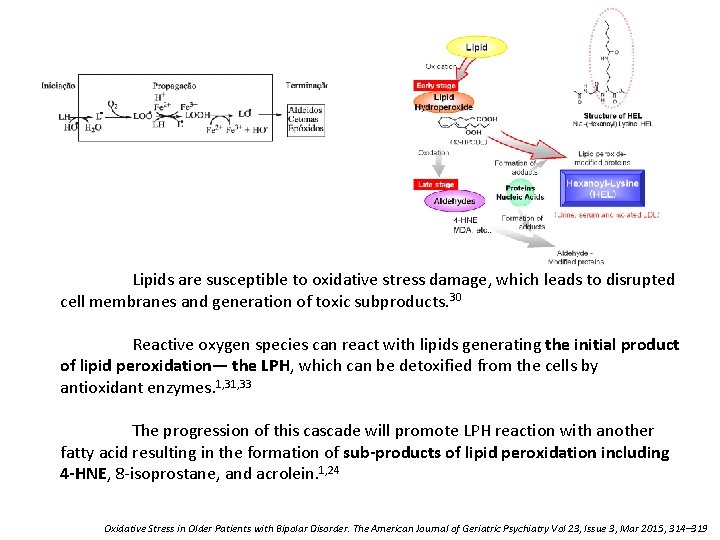
Lipids are susceptible to oxidative stress damage, which leads to disrupted cell membranes and generation of toxic subproducts. 30 Reactive oxygen species can react with lipids generating the initial product of lipid peroxidation— the LPH, which can be detoxified from the cells by antioxidant enzymes. 1, 33 The progression of this cascade will promote LPH reaction with another fatty acid resulting in the formation of sub-products of lipid peroxidation including 4 -HNE, 8 -isoprostane, and acrolein. 1, 24 Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319
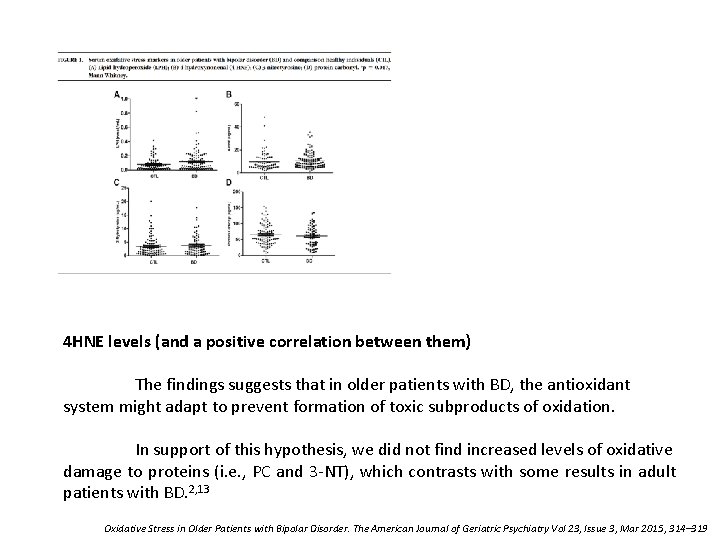
4 HNE levels (and a positive correlation between them) The findings suggests that in older patients with BD, the antioxidant system might adapt to prevent formation of toxic subproducts of oxidation. In support of this hypothesis, we did not find increased levels of oxidative damage to proteins (i. e. , PC and 3 -NT), which contrasts with some results in adult patients with BD. 2, 13 Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319
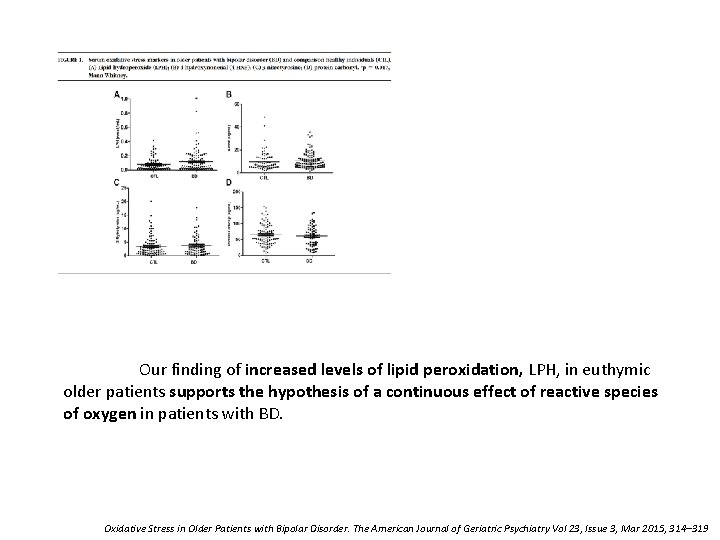
Our finding of increased levels of lipid peroxidation, LPH, in euthymic older patients supports the hypothesis of a continuous effect of reactive species of oxygen in patients with BD. Oxidative Stress in Older Patients with Bipolar Disorder. The American Journal of Geriatric Psychiatry Vol 23, Issue 3, Mar 2015, 314– 319


Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder type II: longitudinal and cross-sectional analyses Torbjørn Elvsåshagen; Pedro Zuzartex; Lars T. Westlyex…Ulrik F. Malt; Trevor Young; Ana Andreazza x These authors contributed equally to the present work. Submitted to Biological Psychiatry Journal (IF 9. 47) 1. For this work we examined dentate gyrus–cornu ammonis (CA-4) volume longitudinally in patients with BD-II and healthy controls. 2. In addition, we investigated whether BD-II is associated with elevated peripheral levels of oxidative stress 3. Finally we analyzed whether these oxidative stress markers are related to dentate gyrus–CA 4 volume
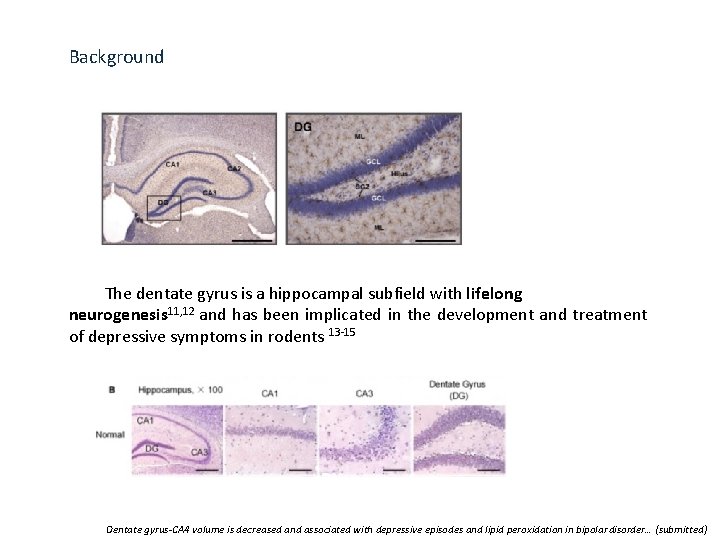
Background The dentate gyrus is a hippocampal subfield with lifelong neurogenesis 11, 12 and has been implicated in the development and treatment of depressive symptoms in rodents 13 -15 Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
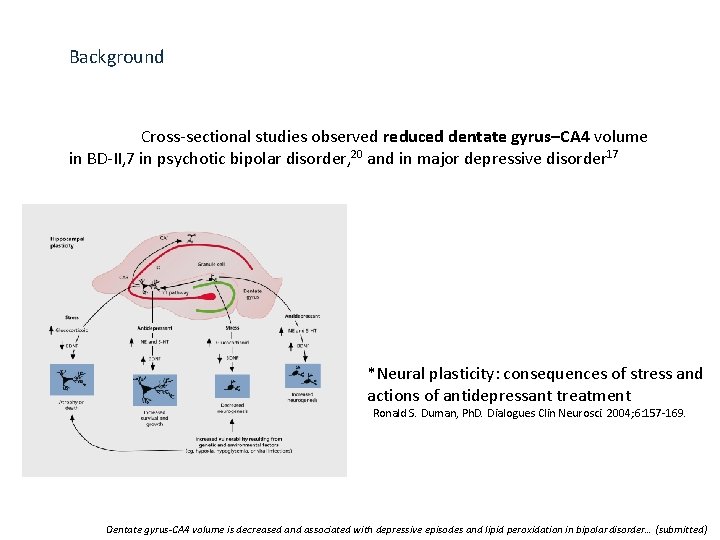
Background Cross-sectional studies observed reduced dentate gyrus–CA 4 volume in BD-II, 7 in psychotic bipolar disorder, 20 and in major depressive disorder 17 *Neural plasticity: consequences of stress and actions of antidepressant treatment Ronald S. Duman, Ph. D. Dialogues Clin Neurosci. 2004; 6: 157 -169. Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)

Background Cross-sectional findings 7, 18, 20 indicate a link between smaller dentate gyrus and depressive episodes. However there has been no longitudinal study of hippocampal subfield volumes in subjects with mood disorders Furthermore the mechanisms underlying dentate gyrus–CA 4 decreases in these illnesses remain unknown Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)

Background Increased oxidative stress can damage several cellular components, including membrane-bound polyunsaturated fatty acids and might thereby compromise neuronal viability in bipolar disorder. 10, 26 We hypothesized that oxidative stress-related neuronal damage is an important contributor to dentate gyrus–CA 4 volume reductions in BD-II 7 and in psychotic bipolar disorder Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
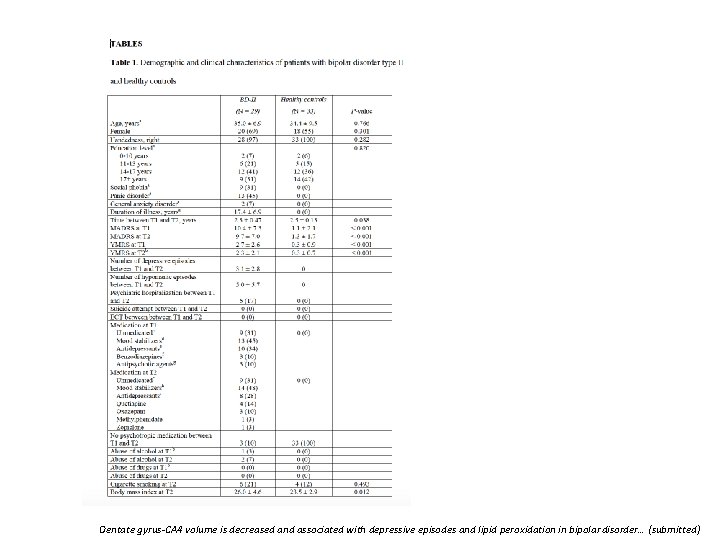
Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
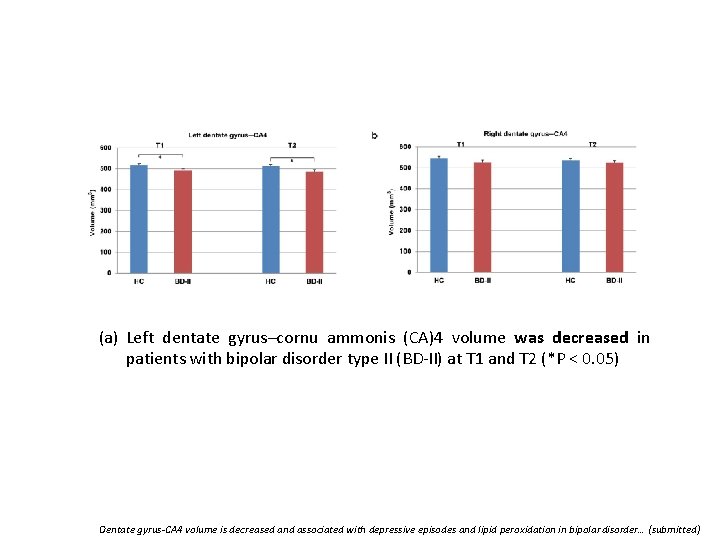
(a) Left dentate gyrus–cornu ammonis (CA)4 volume was decreased in patients with bipolar disorder type II (BD-II) at T 1 and T 2 (*P < 0. 05) Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
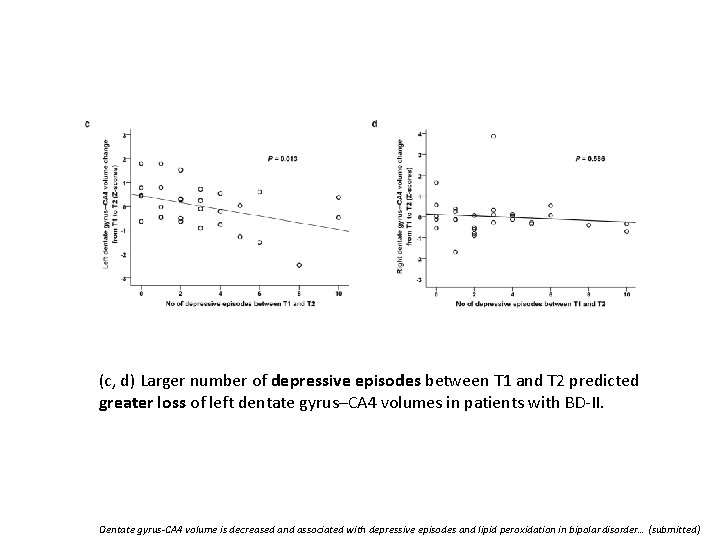
(c, d) Larger number of depressive episodes between T 1 and T 2 predicted greater loss of left dentate gyrus–CA 4 volumes in patients with BD-II. Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
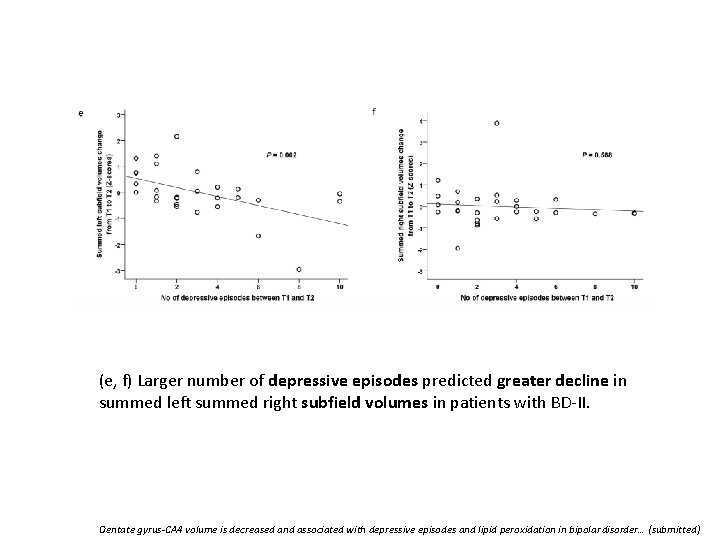
(e, f) Larger number of depressive episodes predicted greater decline in summed left summed right subfield volumes in patients with BD-II. Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
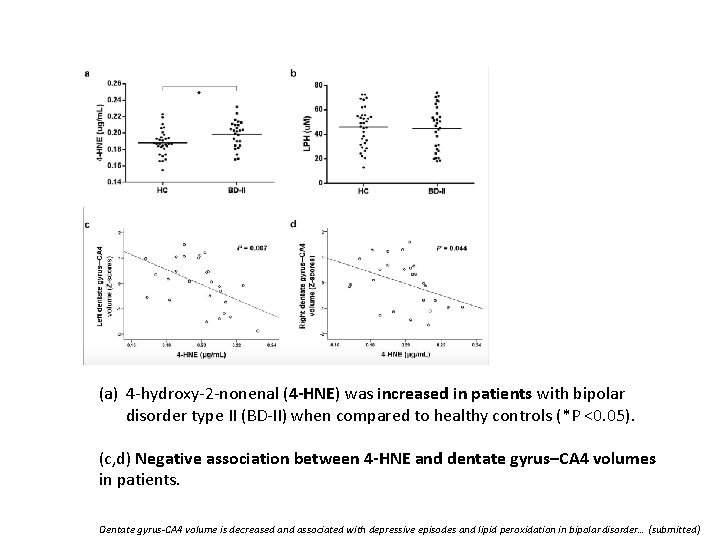
(a) 4 -hydroxy-2 -nonenal (4 -HNE) was increased in patients with bipolar disorder type II (BD-II) when compared to healthy controls (*P <0. 05). (c, d) Negative association between 4 -HNE and dentate gyrus–CA 4 volumes in patients. Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)

In summary: 1. At T 1, left dentate gyrus–CA 4 was 5. 4% smaller in subjects with BD-II than controls 2. At T 2, left dentate gyrus–CA 4 was 4. 9% smaller in patients than controls 1. Dentate gyrus–CA 4 was on average 1. 1% smaller at T 2 than at T 1 2. No significant time x group (patients vs. controls) interaction was found (P = 0. 713) 3. However we found that larger number of depressive episodes between T 1 and T 2 predicted greater loss of left dentate gyrus–CA 4 volumes in patients (P = 0. 013) • The estimated dentate gyrus–CA 4 volume loss for each depressive episode was 4 mm 3 (0. 8% of mean volume at T 1) • No significant effect of number of hypomanic episodes, psychiatric hospitalization, other comorbidities, medication etc. . (all P > 0. 05). Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)

6. 4 -HNE was significantly higher in patients than controls (6% mean increase. P = 0. 016) 7. Negative association between 4 -HNE and left dentate gyrus–CA 4 volume in patients (P = 0. 007) 8. No significant associations were found between LPH or other oxidative stress markers. Dentate gyrus-CA 4 volume is decreased and associated with depressive episodes and lipid peroxidation in bipolar disorder… (submitted)
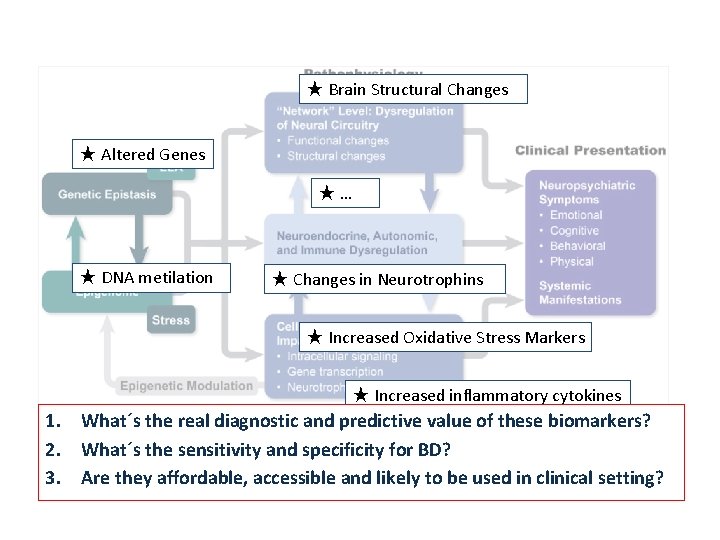
★ Brain Structural Changes ★ Altered Genes ★… ★ DNA metilation ★ Changes in Neurotrophins ★ Increased Oxidative Stress Markers ★ Increased inflammatory cytokines 1. What´s the real diagnostic and predictive value of these biomarkers? 2. What´s the sensitivity and specificity for BD? 3. Are they affordable, accessible and likely to be used in clinical setting?

REFERENCES I Halliwell B: Biochemistry of oxidative stress. Biochem Soc Trans 2007; 35: 1147 e 1150 2. Kapczinski F, Dal-Pizzol F, Teixeira AL, et al: Peripheral biomarkers and illness activity in bipolar disorder. J Psychiatr Res 2011; 45: 156 e 161 3. Andreazza AC, Young LT: The neurobiology of bipolar disorder: identifying targets for specific agents and synergies for combination treatment. Int J Neuropsychopharmacol 2013; 17: 1 e 14 4. Andreazza AC, Shao L, Wang JF, et al: Mitochondrial complex I activity and oxidative damage to mitochondrial proteins in the prefrontal cortex of patients with bipolar disorder. Arch Gen Psychiatry 2010; 67: 360 e 368 5. Andreazza AC, Wang JF, Salmasi F, et al: Specific subcellular changes in oxidative stress in prefrontal cortex from patients with bipolar disorder. J Neurochem 2013; 127: 552 e 561 6. Gawryluk JW, Wang JF, Andreazza AC, et al: Decreased levels of glutathione, the major brain antioxidant, in post-mortem prefrontal cortex from patients with psychiatric disorders. Int J Neuropsychopharmacol 2011; 14: 123 e 130 7. Gawryluk JW, Wang JF, Andreazza AC, et al: Prefrontal cortex glutathione S-transferase levels in patients with bipolar disorder, major depression and schizophrenia. Int J Neuropsychopharmacol 2011; 14: 1069 e 1074 8. Konradi C, Eaton M, Mac. Donald ML, et al: Molecular evidence for mitochondrial dysfunction in bipolar disorder. Arch Gen Psychiatry 2004; 61: 300 e 308 9. Konradi C, Sillivan SE, Clay HB: Mitochondria, oligodendrocytes and inflammation in bipolar disorder: evidence from transcriptome studies points to intriguing parallels with multiple sclerosis. Neurobiol Dis 2012; 45: 37 e 47 10. Ozcan ME, Gulec M, Ozerol E, et al: Antioxidant enzyme activities and oxidative stress in affective disorders. Int Clin Psychopharmacol 2004; 19: 89 e 95 11. Andreazza AC, Frey BN, Erdtmann B, et al: DNA damage in bipolar disorder. Psychiatry Res 2007; 153: 27 e 32 12. Andreazza AC, Cassini C, Rosa AR, et al: Serum S 100 B and antioxidant enzymes in bipolar patients. J Psychiatry Res 2007; 41: 523 e 529 13. Andreazza AC, Kauer-Sant’anna M, Frey BN, et al: Oxidative stress markers in bipolar disorder: a meta-analysis. J Affect Disord 2008; 111: 135 e 144 14. Andreazza AC, Kapczinski F, Kauer-Sant’Anna M, et al: 3 -Nitrotyrosine and glutathione antioxidant system in patients in the early and late stages of bipolar disorder. J Psychiatry Neurosci 2009; 34: 263 e 271 15. Frey BN, Martins MR, Petronilho FC, et al: Increased oxidative stress after repeated amphetamine exposure: possible relevance as a model of mania. Bipolar Disord 2006; 8: 275 e 280 16. Frey BN, Andreazza AC, Houenou J, et al: Biomarkers in bipolar disorder: a positional paper from the International Society for Bipolar Disorders Biomarkers Task Force. Aust NZ J Psychiatry REFERENCES II 1. Angst J. The emerging epidemiology of hypomania and bipolar II disorder. J Affect Disord 1998; 50: 143 -151. 2. Phillips ML, Kupfer DJ. Bipolar disorder diagnosis: challenges and future directions. Lancet 2013; 381: 1663 -1671. 3. Angst J, Cui L, Swendsen J, Rothen S, Cravchik A, Kessler RC et al. Major depressive disorder with subthreshold bipolarity in the National Comorbidity Survey Replication. Am J Psychiatry 2010; 167: 1194 -1201. 4. Angst J, Gamma A, Benazzi F, Ajdacic V, Eich D, Rossler W. Toward a re-definition of subthreshold bipolarity: epidemiology and proposed criteria for bipolar-II, minor bipolar disorders and hypomania. J Affect Disord 2003; 73: 133 -146. 5. Rihmer Z, Pestality P. Bipolar II disorder and suicidal behavior. Psychiatr Clin North Am 1999; 22: 667 -673. 6. Novick DM, Swartz HA, Frank E. Suicide attempts in bipolar I and bipolar II disorder: a review and meta-analysis of the evidence. Bipolar Disord 2010; 12: 1 -9. 7. Elvsashagen T, Westlye LT, Boen E, Hol PK, Andersson S, Andreassen OA et al. Evidence for reduced dentate gyrus and fimbria volume in bipolar II disorder. Bipolar Disord 2013; 15: 167 -176. 8. Andreazza AC, Kauer-Sant'anna M, Frey BN, Bond DJ, Kapczinski F, Young LT et al. Oxidative stress markers in bipolar disorder: a meta-analysis. J Affect Disord 2008; 111: 135144. 9. Kapczinski F, Vieta E, Andreazza AC, Frey BN, Gomes FA, Tramontina J et al. Allostatic load in bipolar disorder: implications for pathophysiology and treatment. Neurosci Biobehav Rev 2008; 32: 675 -692. 10. Berk M, Kapczinski F, Andreazza AC, Dean OM, Giorlando F, Maes M et al. Pathways underlying neuroprogression in bipolar disorder: focus on inflammation, oxidative stress and neurotrophic factors. Neurosci Biobehav Rev 2011; 35: 804 -817. 11. Spalding KL, Bergmann O, Alkass K, Bernard S, Salehpour M, Huttner HB et al. Dynamicsof hippocampal neurogenesis in adult humans. Cell 2013; 153: 1219 -1227. 12. Eriksson PS, Perfilieva E, Bjork-Eriksson T, Alborn AM, Nordborg C, Peterson DA et al. Neurogenesis in the adult human hippocampus. Nat Med 1998; 4: 1313 -1317. 13. Santarelli L, Saxe M, Gross C, Surget A, Battaglia F, Dulawa S et al. Requirement of hippocampal neurogenesis for the behavioral effects of antidepressants. Science 2003; 301: 805 -809. 14. Sahay A, Hen R. Adult hippocampal neurogenesis in depression. Nat Neurosci 2007; 10: 1110 -1115. Snyder JS, Soumier A, Brewer M, Pickel J, Cameron HA. Adult hippocampal neurogenesis buffers stress responses and depressive behaviour. Nature 2011; 476: 458 -461. 16. Van Leemput K, Bakkour A, Benner T, Wiggins G, Wald LL, Augustinack J et al. Automated segmentation of hippocampal subfields from ultra-high resolution in vivo MRI. Hippocampus 2009; 19: 549 -557. 17. Huang Y, Coupland NJ, Lebel RM, Carter R, Seres P, Wilman AH et al. Structural changes in hippocampal subfields in major depressive disorder: a high-field magnetic resonance imaging study. Biol Psychiatry 2013; 74: 62 -68. 18. Gold SM, Kern KC, O'Connor MF, Montag MJ, Kim A, Yoo YS et al. Smaller cornu ammonis 2 -3/dentate gyrus volumes and elevated cortisol in multiple sclerosis patients with depressive symptoms. Biol Psychiatry 2010; 68: 553 -559. 19. Ho NF, Hooker JM, Sahay A, Holt DJ, Roffman JL. In vivo imaging of adult human hippocampal neurogenesis: progress, pitfalls and promise. Mol Psychiatry 2013; 18: 404 -416. 20. Mathew I, Gardin TM, Tandon N, Eack S, Francis AN, Seidman LJ et al. Medial Temporal Lobe Structures and Hippocampal Subfields in Psychotic Disorders: Findings From the Bipolar-Schizophrenia Network on Intermediate Phenotypes (B-SNIP) Study. JAMA
- Slides: 41