BIOL 2020 Chapter 20 Cellular Communities Tissues Stem

BIOL 2020 Chapter 20 Cellular Communities: Tissues, Stem Cells, and Cancer Extracellular Matrix and Connective Tissue Epithelial Sheets and Cell Junctions Tissue Maintenance and Renewal (stem cells) Cancer Cells are squishy and tiny. Each is enclosed in a membrane only 1/100, 000 mm thick. How can solid, sturdy organisms (like us) be built of cells?

Levels of Organization

From Cells to Tissues How are the cells held together? • Focus on 6 types of cell-cell or cell-matrix junctions How do different types of cells come about? • Differentiation (differential gene expression in different cell types) How does tissue arrangement in organisms occur? • Describe the 4 types of tissues How do tissues attach to each other?

Epidermal tissue: outer cells Mesenchymal tissue: inner cells 20 -1 a pine needle showing cell types Organs are made of precisely arranged cells of different tissue types Each cell contains an internal cytoskeleton, also secretes an external extracellular matrix which gives added strength Each tissue type consists of specific cell types attached to specific matrix
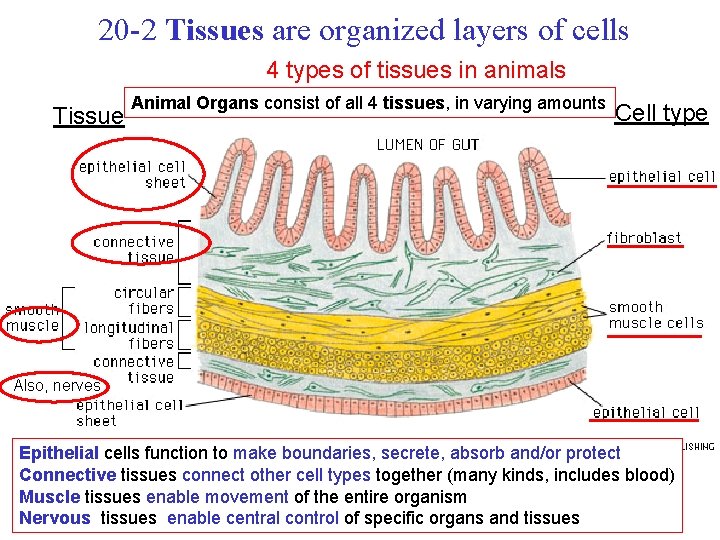
20 -2 Tissues are organized layers of cells 4 types of tissues in animals Tissue Animal Organs consist of all 4 tissues, in varying amounts Cell type Also, nerves Epithelial cells function to make boundaries, secrete, absorb and/or protect Connective tissues connect other cell types together (many kinds, includes blood) Muscle tissues enable movement of the entire organism Nervous tissues enable central control of specific organs and tissues

Multicellularization evolved separately in plants and animals – So their organization differs: Animals have predator/ prey relationships and need to be mobile, so required a strong but flexible scaffolding system • To move, Cells must be able to change shape and transmit forces – Animal strength comes from the cytoskeleton and connections between cells and to the extracellular matrix to which cells are attached – Animal cells are much more diverse than plant cells: tissues vary in cell type and in the type/amount of extracellular matrix they produce Plants are sedentary (sessile) so evolved semi-rigid cell walls, but weak cells – Plant strength comes from their cell walls (not from cytoskeletal junctions) » If wall is removed, plant cells are weak and burst and die • General plant plan is many boxes cemented together with cell walls – Individual cells can control the cell wall structure they produce » Thick and hard makes wood » Thin and flexible makes leaves, etc

20 -3 the cell wall of Pectin (mostly in outer (growing) walls, wall only) plants: primary and Cellulose (in inner, more rigid walls with 2 o wall) secondary 1 o Pectin provides protection from compression Cellulose provides tensile strength (protection from stretching/pulling forces) Root tissue stem tissue Plant cells lack intermediate filaments, so have little tensile strength. Structural strength comes from the walls they lay down.
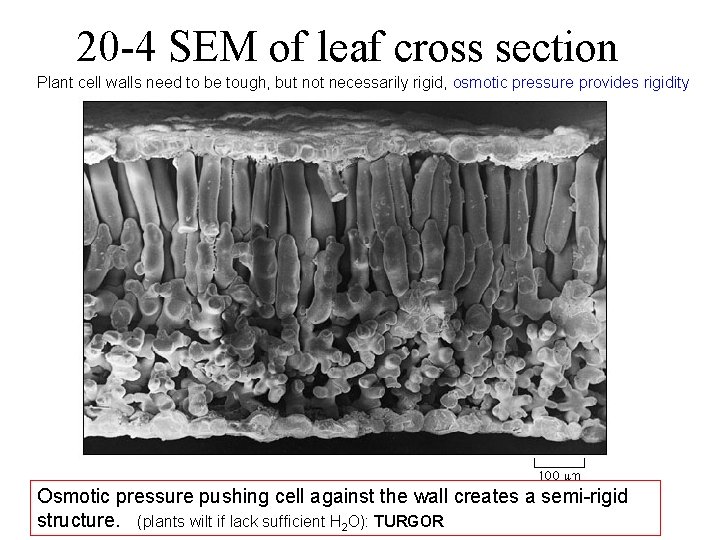
20 -4 SEM of leaf cross section Plant cell walls need to be tough, but not necessarily rigid, osmotic pressure provides rigidity Osmotic pressure pushing cell against the wall creates a semi-rigid structure. (plants wilt if lack sufficient H 2 O): TURGOR
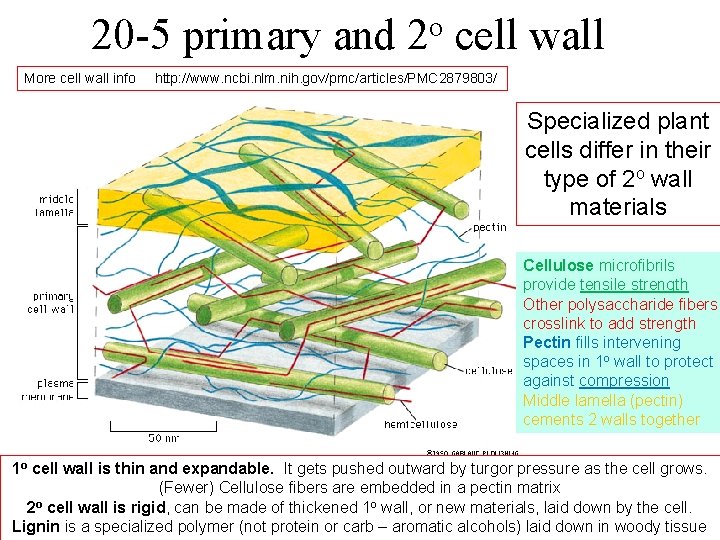
20 -5 primary and More cell wall info o 2 cell wall http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 2879803/ Specialized plant cells differ in their type of 2 o wall materials Cellulose microfibrils provide tensile strength Other polysaccharide fibers crosslink to add strength Pectin fills intervening spaces in 1 o wall to protect against compression Middle lamella (pectin) cements 2 walls together 1 o cell wall is thin and expandable. It gets pushed outward by turgor pressure as the cell grows. (Fewer) Cellulose fibers are embedded in a pectin matrix o 2 cell wall is rigid, can be made of thickened 1 o wall, or new materials, laid down by the cell. Lignin is a specialized polymer (not protein or carb – aromatic alcohols) laid down in woody tissue
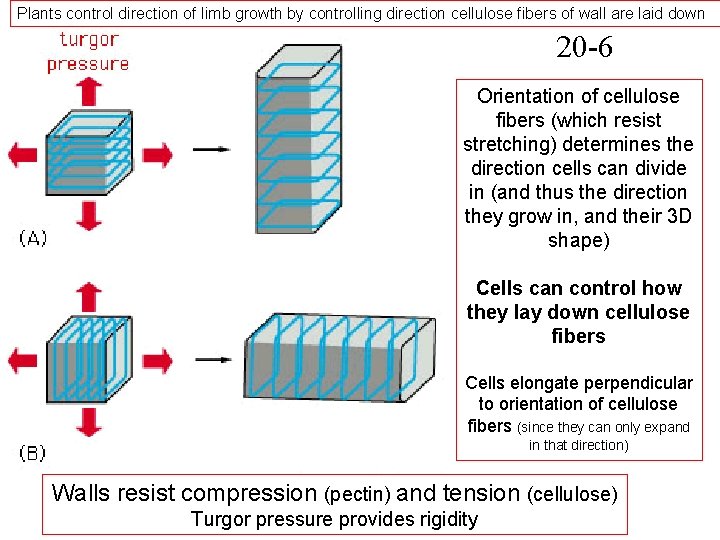
Plants control direction of limb growth by controlling direction cellulose fibers of wall are laid down 20 -6 Orientation of cellulose fibers (which resist stretching) determines the direction cells can divide in (and thus the direction they grow in, and their 3 D shape) Cells can control how they lay down cellulose fibers Cells elongate perpendicular to orientation of cellulose fibers (since they can only expand in that direction) Walls resist compression (pectin) and tension (cellulose) Turgor pressure provides rigidity
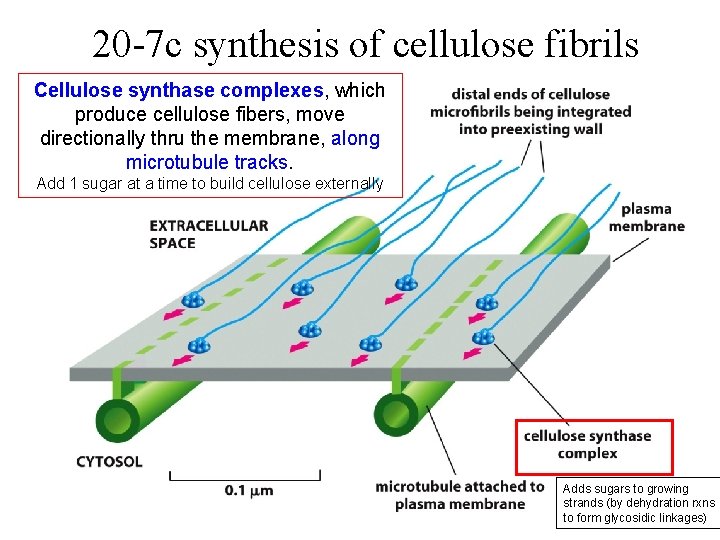
20 -7 c synthesis of cellulose fibrils Cellulose synthase complexes, which produce cellulose fibers, move directionally thru the membrane, along microtubule tracks. Add 1 sugar at a time to build cellulose externally Adds sugars to growing strands (by dehydration rxns to form glycosidic linkages)

20 -7 thus, plant 3 D shape is determined indirectly by the cytoskeleton Cellulose fibers Outside cell Underlyiing microtubules inside cell

Animal tissue types 4 traditional tissue types Epithelial tissue Connective tissue (includes loose and fibrous CT, blood, bone, cartilage, fat ) Muscle tissue Nervous tissue Really just 2 categories: connective tissue (CT) and the rest: CT has few cells and lots of ECM, its ECM provides its mechanical strength Rest are various specialized cells producing very little ECM. Their mechanical strength comes from their cytoskeleton and their cell-cell and cell-matrix junctions

Animal connective tissue The cells of connective tissue are embedded in a great amount of extracellular material. This extracellular matrix is secreted by the CT cells. It consists of protein fibers (mostly collagen and elastin) embedded in an amorphous mixture of proteinpolysaccharide ("proteoglycan") molecules. Tensile compression Each connective tissue type is determined by the: 1 - particular cell type, and 2 - the type of matrix these cells secrete Mostly ECM is made of Collagen and elastin fibers, Proteoglycans and empty space, with comparatively few cells in it

Connective tissue • 6 types: Loose CT, Fibrous CT, Adipose tissue, Blood, Cartilage, and Bone CT – Range in rigidity from liquid blood to solid bone – Differ in type of cell and type of matrix the cell produces The type of CT depends on 1) type of cells present and 2) type of matrix produced by those cells Loose and fibrous CT are fibroblast cells with a collagen and elastin matrix (Loose CT makes up most ECM, Fibrous CT is ligaments and tendons) Fat is adipose cells, with very little matrix Cartilage is chondrocytes, with a rubbery, shock absorbing proteoglycan matrix Bone is osteocytes, with a hard, mineralized matrix containing Ca. PO 4 Blood is RBCs and WBCs with a liquid matrix (plasma)
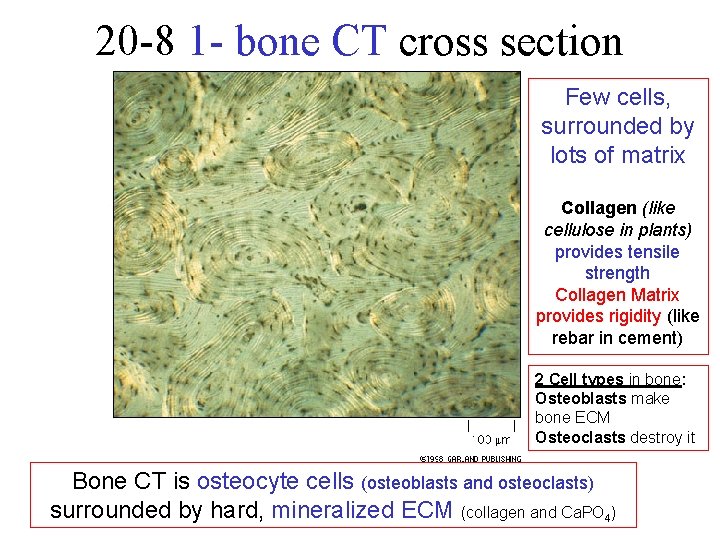
20 -8 1 - bone CT cross section Few cells, surrounded by lots of matrix Collagen (like cellulose in plants) provides tensile strength Collagen Matrix provides rigidity (like rebar in cement) 2 Cell types in bone: Osteoblasts make bone ECM Osteoclasts destroy it Bone CT is osteocyte cells (osteoblasts and osteoclasts) surrounded by hard, mineralized ECM (collagen and Ca. PO 4)
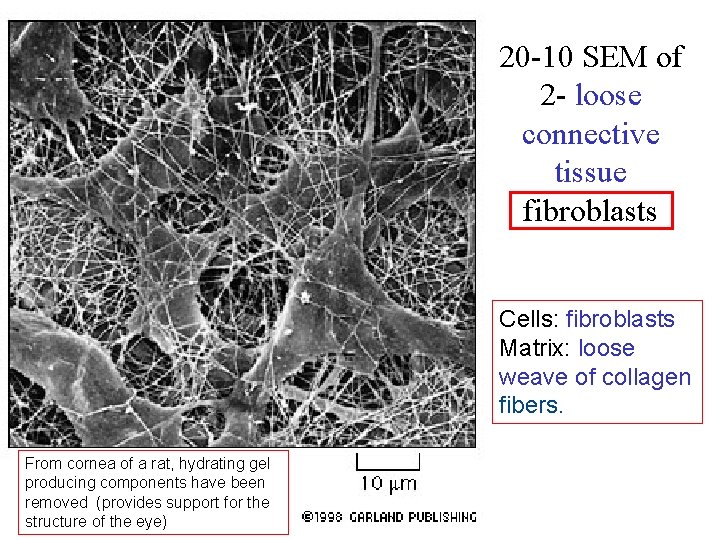
20 -10 SEM of 2 - loose connective tissue fibroblasts Cells: fibroblasts Matrix: loose weave of collagen fibers. From cornea of a rat, hydrating gel producing components have been removed (provides support for the structure of the eye)

6 Connective tissues vary in type of cells they contain, and type of matrix those cells produce Blood has many types of cells (RBC’s, many different white blood cells, etc) in liquid matrix (plasma) Fat is adipose cells with very little extra cellular matrix Tendons and Ligaments are Fibrous CT, made of fibroblast cells and ECM made of parallel collagen filaments Most CT lining organs and connecting different tissues is Loose CT, made of fibroblast cells with ECM of collagen filaments in a meshwork Cartilage is chondrocyte cells with a rubbery matrix that resists compression, made of lots of proteoglycans and collagen Bone is osteocyte cells, and hard, mineralized matrix of collagen and Ca. PO 4 Primary fiber of ECM is collagen
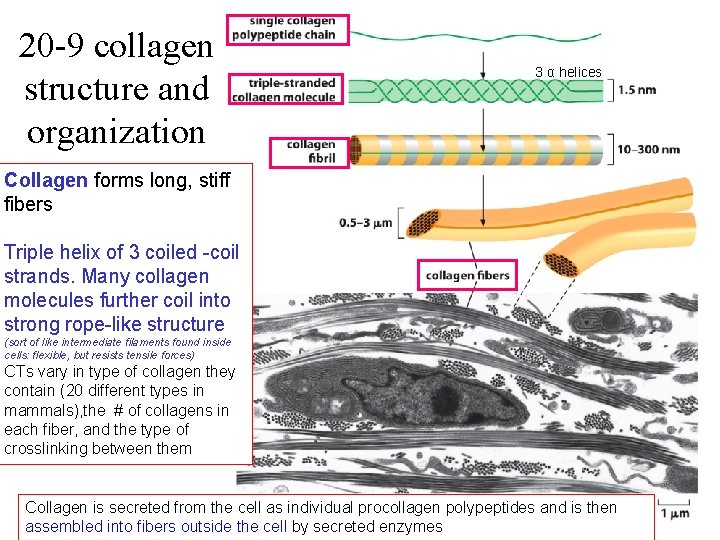
20 -9 collagen structure and organization 3 α helices Collagen forms long, stiff fibers Triple helix of 3 coiled -coil strands. Many collagen molecules further coil into strong rope-like structure (sort of like intermediate filaments found inside cells: flexible, but resists tensile forces) CTs vary in type of collagen they contain (20 different types in mammals), the # of collagens in each fiber, and the type of crosslinking between them Collagen is secreted from the cell as individual procollagen polypeptides and is then assembled into fibers outside the cell by secreted enzymes
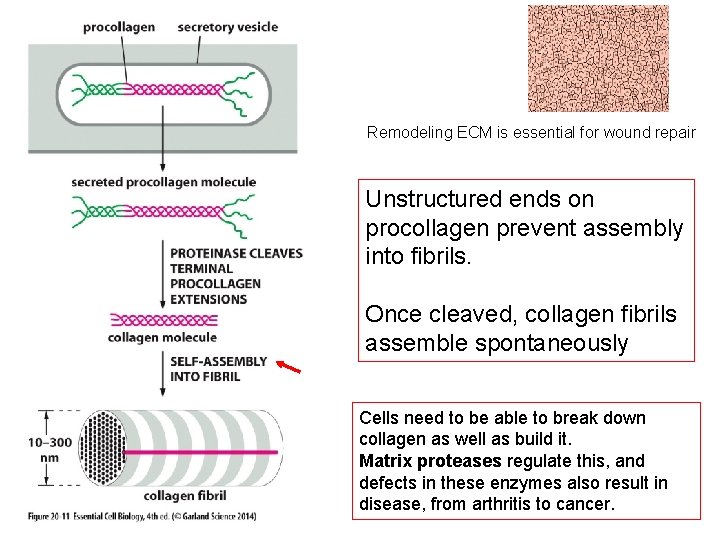
Remodeling ECM is essential for wound repair Unstructured ends on procollagen prevent assembly into fibrils. Once cleaved, collagen fibrils assemble spontaneously Cells need to be able to break down collagen as well as build it. Matrix proteases regulate this, and defects in these enzymes also result in disease, from arthritis to cancer.
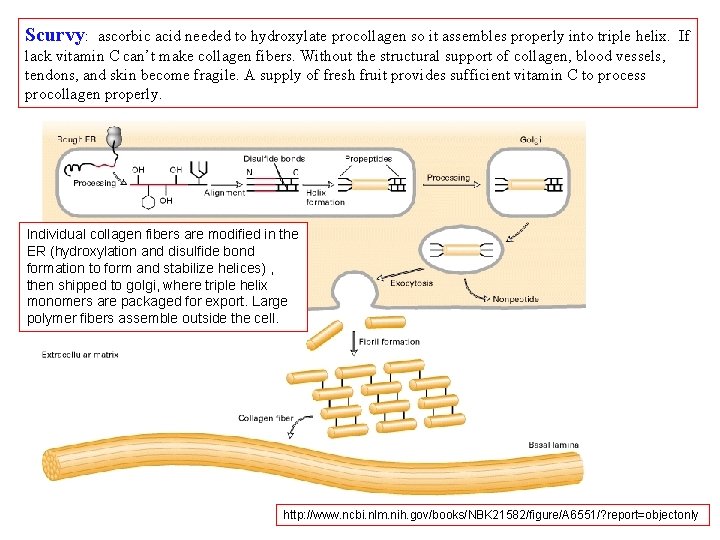
Scurvy: ascorbic acid needed to hydroxylate procollagen so it assembles properly into triple helix. If lack vitamin C can’t make collagen fibers. Without the structural support of collagen, blood vessels, tendons, and skin become fragile. A supply of fresh fruit provides sufficient vitamin C to process procollagen properly. Individual collagen fibers are modified in the ER (hydroxylation and disulfide bond formation to form and stabilize helices) , then shipped to golgi, where triple helix monomers are packaged for export. Large polymer fibers assemble outside the cell. http: //www. ncbi. nlm. nih. gov/books/NBK 21582/figure/A 6551/? report=objectonly

Collagen details you do not need to know collagen subtypes for the test Collagen types I – V different CT types use different collagen types Type I collagen is found throughout the body except in cartilaginous tissues. It is found in skin, tendon, vascular, ligature, organs and is the main component of bone. It is also synthesized in response to injury and in the fibrous nodules in fibrous diseases. Over 90% of the collagen in the body is type I. Type II collagen is the main component of cartilage. It is also found in developing cornea and vitreous humour. These are formed from two or more collagens or copolymers rather than a single type of collagen. Type III collagen is found in the walls of arteries and other hollow organs and usually occurs in the same fibril with type I collagen. Type IV forms the basis of cell basement membrane Type V collagen and type XI collagen are minor components of tissue and occur as fibrils with type I and type II collagen respectively. Type V forms cell surfaces, hair and placenta. Collagen-related diseases most commonly arise from genetic defects or nutritional deficiencies that affect the biosynthesis, assembly, postranslational modification, secretion, or other processes involved in normal collagen production. http: //www. news-medical. net/health/Collagen-Types-and-Linked-Disorders. aspx

Mutations in collagen structure cause numerous diseases. collagen requires a glycine at every 3 rd aa site Trimer assembly begins at the NH 2 terminus 1. Would you expect collagen mutations to be detrimental if only one of the two copies of a collagen gene is defective? three collagen chains have to come together to form the triple helix, so any defective molecule will impair assembly, even if normal collagen chains are present at the same time. Collagen mutations are therefore dominant; that is, they have a deleterious effect even in the presence of a normal copy of the gene. 2. A puzzling observation is that the change of a glycine residue into another amino acid is most detrimental if it occurs toward the amino terminus of the rodforming domain. Suggest an explanation for this. The different severity of the mutations results from a polarity in the assembly process. Collagen monomers assemble into the triple-helical rod starting from their amino-terminal ends. A mutation in an “early” glycine therefore allows only short rods to form, whereas a mutation farther downstream allows for longer, more normal rods.

Collagen need to know Primary function: component of extra cellular matrix. Provides tensile strength to tissues Many Collagen fibers are produced by cells of connective tissues, forming the extra cellular matrix Mammals have 20 different types of collagen. Defects in the structure or assembly of these proteins cause numerous diseases Procollagen assembles into coiled coil trimers intracellulary, then gets exported, ends cleaved off, and assembled into collagen fibers outside the cell Collagen is the main protein component of bone, tendons, skin, etc. About 25% of the total protein mass in animals is collagen. It is the most prevalent protein in our bodies Leather is “pickled collagen”
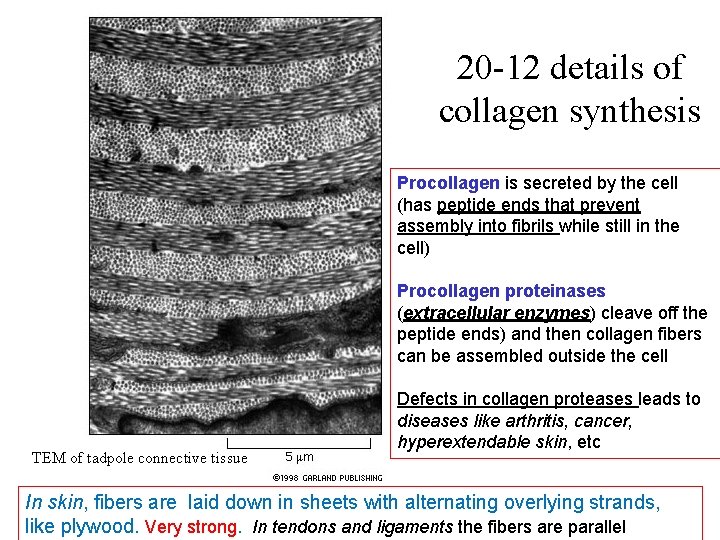
20 -12 details of collagen synthesis Procollagen is secreted by the cell (has peptide ends that prevent assembly into fibrils while still in the cell) Procollagen proteinases (extracellular enzymes) cleave off the peptide ends) and then collagen fibers can be assembled outside the cell TEM of tadpole connective tissue Defects in collagen proteases leads to diseases like arthritis, cancer, hyperextendable skin, etc In skin, fibers are laid down in sheets with alternating overlying strands, like plywood. Very strong. In tendons and ligaments the fibers are parallel
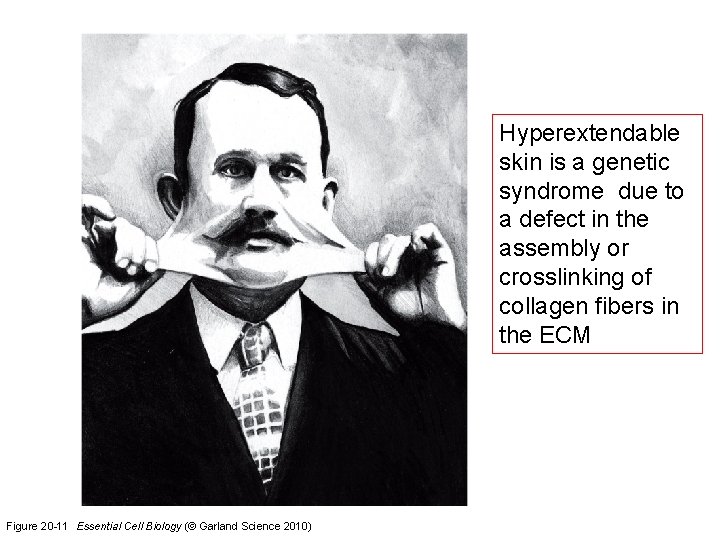
Hyperextendable skin is a genetic syndrome due to a defect in the assembly or crosslinking of collagen fibers in the ECM Figure 20 -11 Essential Cell Biology (© Garland Science 2010)
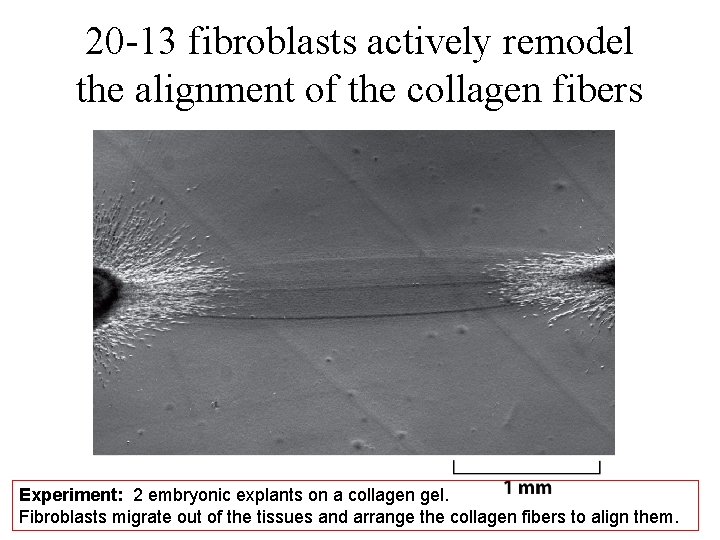
20 -13 fibroblasts actively remodel the alignment of the collagen fibers Experiment: 2 embryonic explants on a collagen gel. Fibroblasts migrate out of the tissues and arrange the collagen fibers to align them.
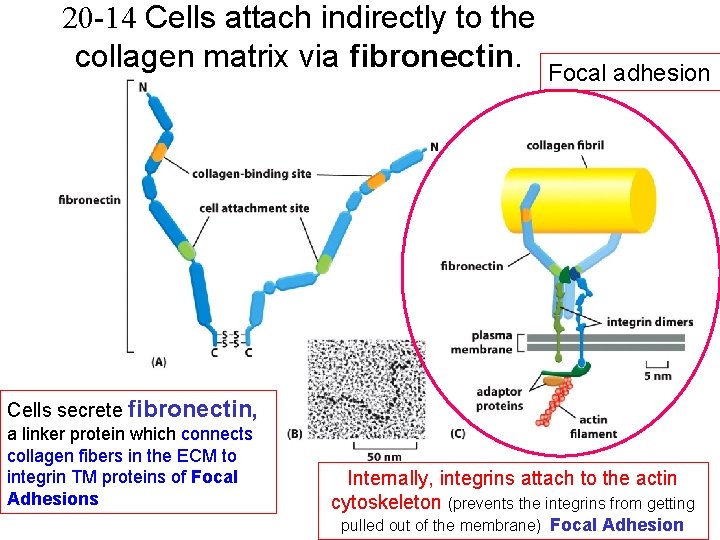
20 -14 Cells attach indirectly to the collagen matrix via fibronectin. Focal adhesion Cells secrete fibronectin, a linker protein which connects collagen fibers in the ECM to integrin TM proteins of Focal Adhesions Internally, integrins attach to the actin cytoskeleton (prevents the integrins from getting pulled out of the membrane) Focal Adhesion
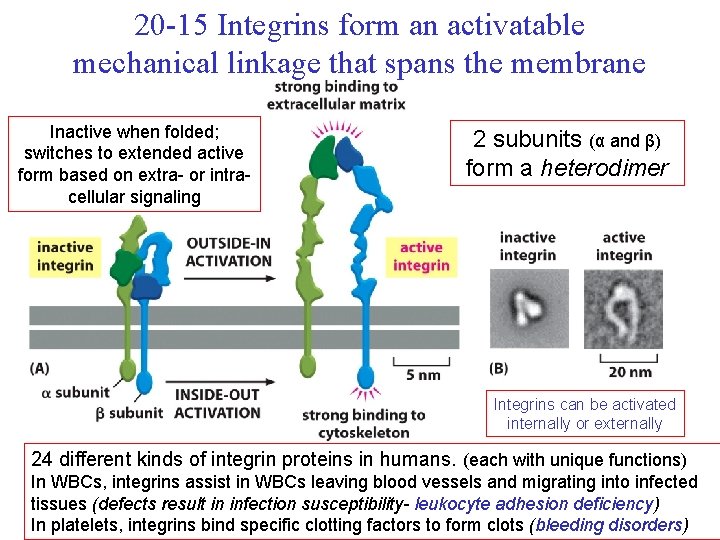
20 -15 Integrins form an activatable mechanical linkage that spans the membrane Inactive when folded; switches to extended active form based on extra- or intracellular signaling 2 subunits (α and β) form a heterodimer Integrins can be activated internally or externally 24 different kinds of integrin proteins in humans. (each with unique functions) In WBCs, integrins assist in WBCs leaving blood vessels and migrating into infected tissues (defects result in infection susceptibility- leukocyte adhesion deficiency) In platelets, integrins bind specific clotting factors to form clots (bleeding disorders)

Location quiz Where are the following proteins located and what is their function? Integrins TM protein of Focal Adhesion junctions, links cell to ECM via fibronectin, also links to cytoskeleton internally. (integrins are also found in a different basal cell junction: hemi-desmosomes) Collagen ECM fibers, laid down by fibroblasts of Loose CT. How are the fibers built? Fibronectin Extracellular Linker protein connecting integrin proteins of focal adhesion to the collagen fibers of the ECM Actin microfilaments Cytosolic cytoskeletal fibers, attach to integrins of focal adhesion to enable cells to contract and crawl. Also adds tensile strength to the cell.
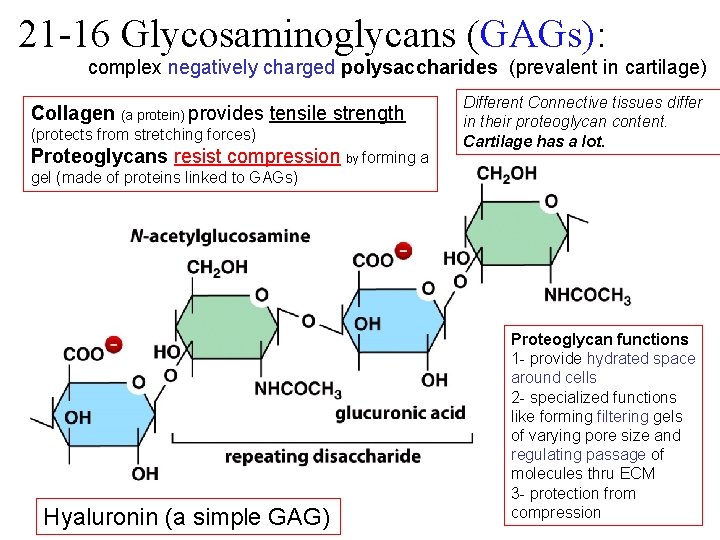
21 -16 Glycosaminoglycans (GAGs): complex negatively charged polysaccharides (prevalent in cartilage) Collagen (a protein) provides tensile strength (protects from stretching forces) Proteoglycans resist compression by forming a Different Connective tissues differ in their proteoglycan content. Cartilage has a lot. gel (made of proteins linked to GAGs) Hyaluronin (a simple GAG) Proteoglycan functions 1 - provide hydrated space around cells 2 - specialized functions like forming filtering gels of varying pore size and regulating passage of molecules thru ECM 3 - protection from compression

20 -17 proteoglycans (cartilage) Create large macromolecules with bottlebrush shape GAGs are very hydrophilic, with extended shape so they occupy large volumes Neg. charge attracts cations (Na+) which attracts water, forming gels at very [low] GAG, GAG Protein, protein Eye jelly is almost all one GAG and water. Dense CT (tendons and ligaments have almost no GAGs) Very strong and resilient against compression since osmotically active and form counter pressure (KNEE cartilage)

Supporting connective tissue Gives strength, support, and protection to the soft parts of the body. Bone, cartilage, blood, adipose Binding connective tissue It binds body parts Loose CT (ECM) together. Fibrous connective tissue It is distributed throughout the body. It serves as a packing and binding material for most of our organs. Fibrous CT (tendons and ligaments)
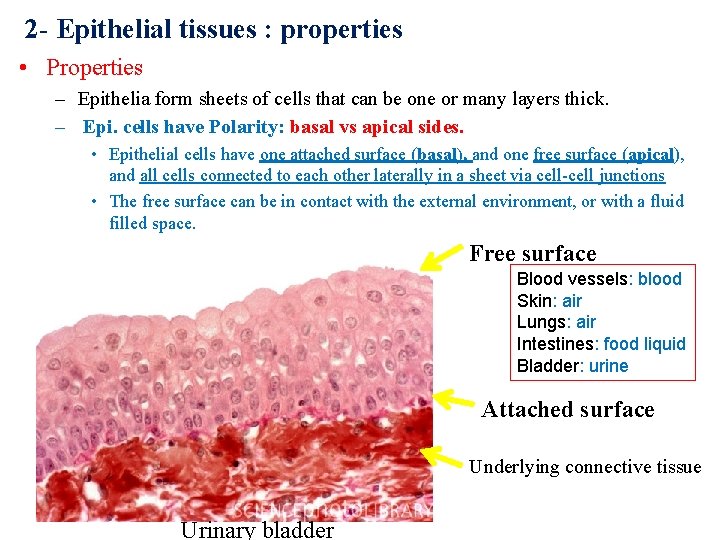
2 - Epithelial tissues : properties • Properties – Epithelia form sheets of cells that can be one or many layers thick. – Epi. cells have Polarity: basal vs apical sides. • Epithelial cells have one attached surface (basal), and one free surface (apical), and all cells connected to each other laterally in a sheet via cell-cell junctions • The free surface can be in contact with the external environment, or with a fluid filled space. Free surface Blood vessels: blood Skin: air Lungs: air Intestines: food liquid Bladder: urine Attached surface Underlying connective tissue Urinary bladder
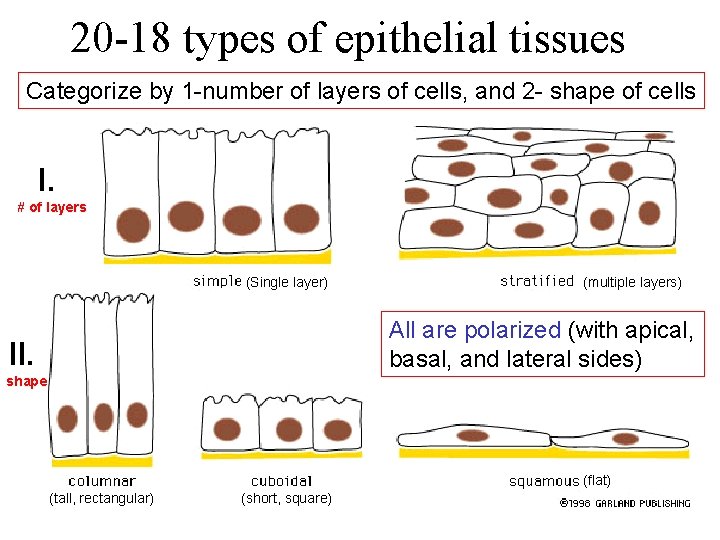
20 -18 types of epithelial tissues Categorize by 1 -number of layers of cells, and 2 - shape of cells I. # of layers (Single layer) (multiple layers) All are polarized (with apical, basal, and lateral sides) II. shape (flat) (tall, rectangular) (short, square)
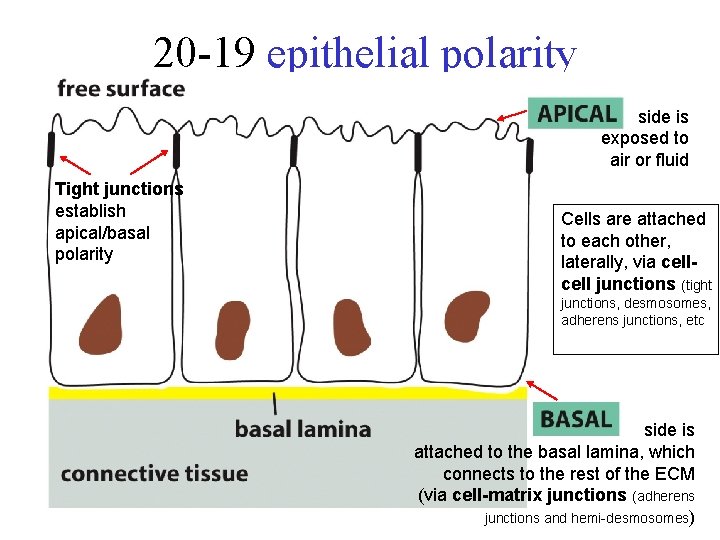
20 -19 epithelial polarity side is exposed to air or fluid Tight junctions establish apical/basal polarity Cells are attached to each other, laterally, via cell junctions (tight junctions, desmosomes, adherens junctions, etc side is attached to the basal lamina, which connects to the rest of the ECM (via cell-matrix junctions (adherens junctions and hemi-desmosomes)
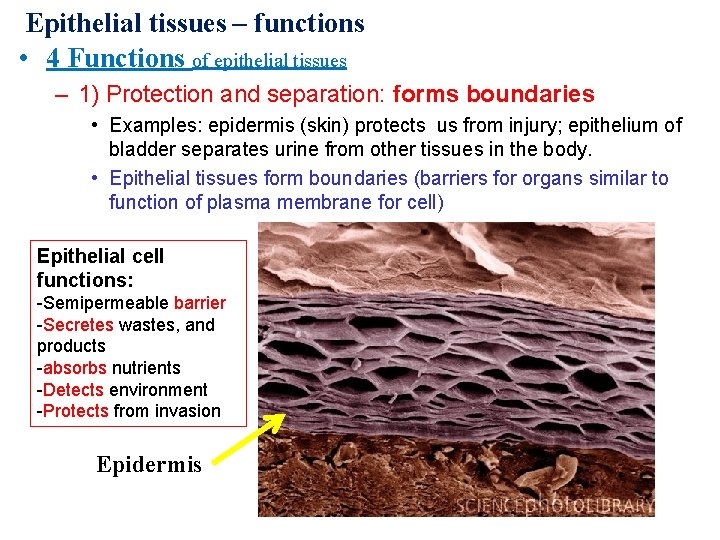
Epithelial tissues – functions • 4 Functions of epithelial tissues – 1) Protection and separation: forms boundaries • Examples: epidermis (skin) protects us from injury; epithelium of bladder separates urine from other tissues in the body. • Epithelial tissues form boundaries (barriers for organs similar to function of plasma membrane for cell) Epithelial cell functions: -Semipermeable barrier -Secretes wastes, and products -absorbs nutrients -Detects environment -Protects from invasion Epidermis
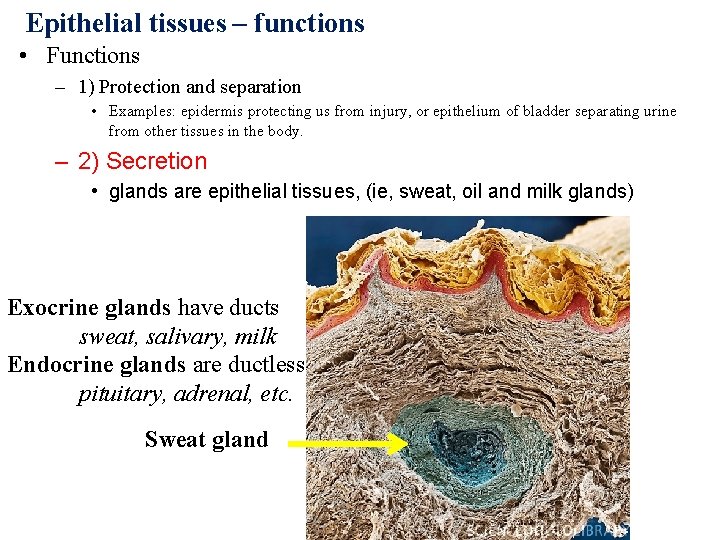
Epithelial tissues – functions • Functions – 1) Protection and separation • Examples: epidermis protecting us from injury, or epithelium of bladder separating urine from other tissues in the body. – 2) Secretion • glands are epithelial tissues, (ie, sweat, oil and milk glands) Exocrine glands have ducts sweat, salivary, milk Endocrine glands are ductless pituitary, adrenal, etc. Sweat gland
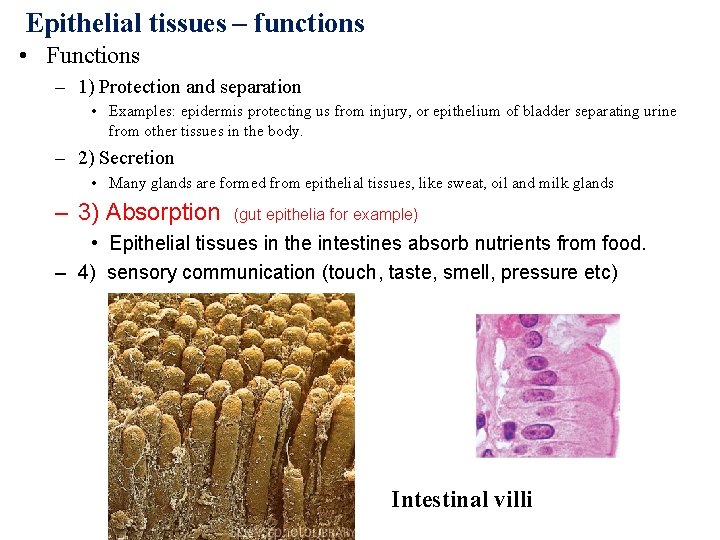
Epithelial tissues – functions • Functions – 1) Protection and separation • Examples: epidermis protecting us from injury, or epithelium of bladder separating urine from other tissues in the body. – 2) Secretion • Many glands are formed from epithelial tissues, like sweat, oil and milk glands – 3) Absorption (gut epithelia for example) • Epithelial tissues in the intestines absorb nutrients from food. – 4) sensory communication (touch, taste, smell, pressure etc) Intestinal villi
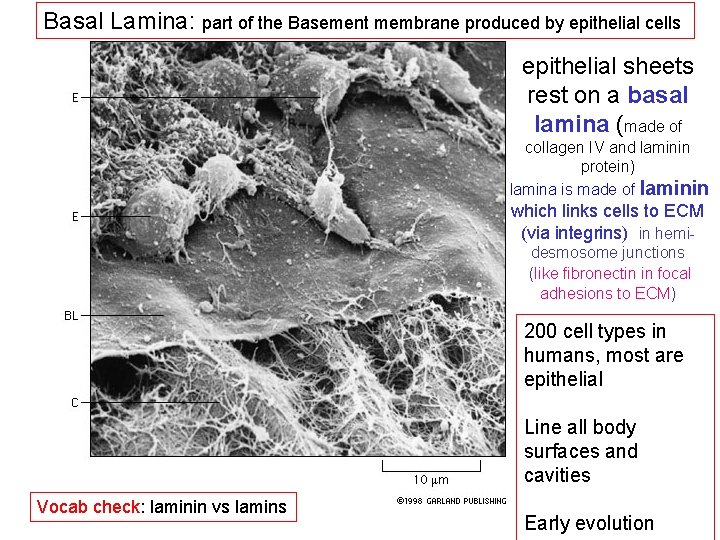
Basal Lamina: part of the Basement membrane produced by epithelial cells epithelial sheets rest on a basal lamina (made of collagen IV and laminin protein) llamina is made of laminin which links cells to ECM (via integrins) in hemidesmosome junctions (like fibronectin in focal adhesions to ECM) 200 cell types in humans, most are epithelial Line all body surfaces and cavities Vocab check: laminin vs lamins Early evolution
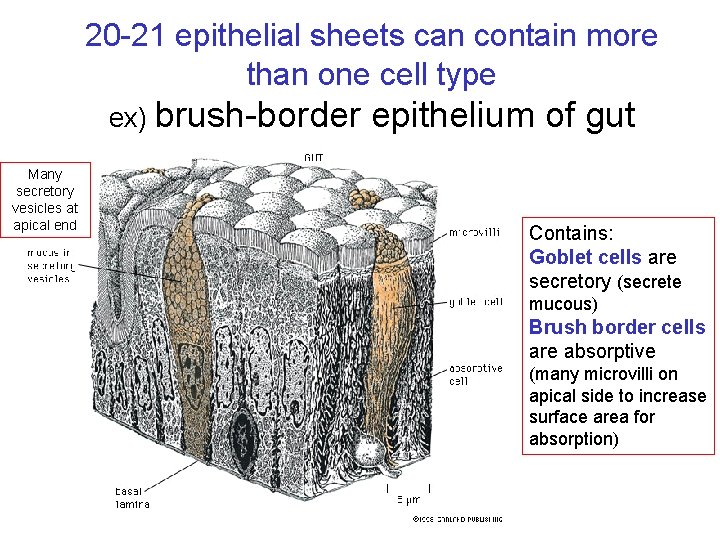
20 -21 epithelial sheets can contain more than one cell type ex) brush-border Many secretory vesicles at apical end epithelium of gut Contains: Goblet cells are secretory (secrete mucous) Brush border cells are absorptive (many microvilli on apical side to increase surface area for absorption)
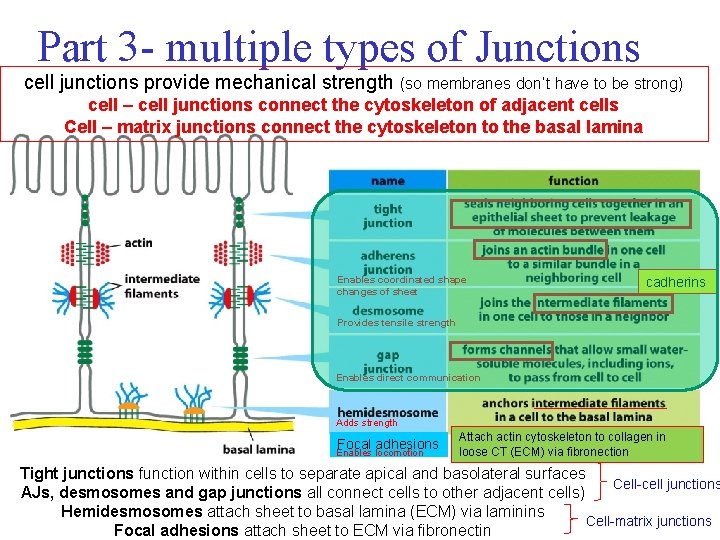
Part 3 - multiple types of Junctions cell junctions provide mechanical strength (so membranes don’t have to be strong) cell – cell junctions connect the cytoskeleton of adjacent cells Cell – matrix junctions connect the cytoskeleton to the basal lamina Enables coordinated shape changes of sheet cadherins Provides tensile strength Enables direct communication Adds strength Focal adhesions Enables locomotion Attach actin cytoskeleton to collagen in loose CT (ECM) via fibronection Tight junctions function within cells to separate apical and basolateral surfaces Cell-cell junctions AJs, desmosomes and gap junctions all connect cells to other adjacent cells) Hemidesmosomes attach sheet to basal lamina (ECM) via laminins Cell-matrix junctions Focal adhesions attach sheet to ECM via fibronectin
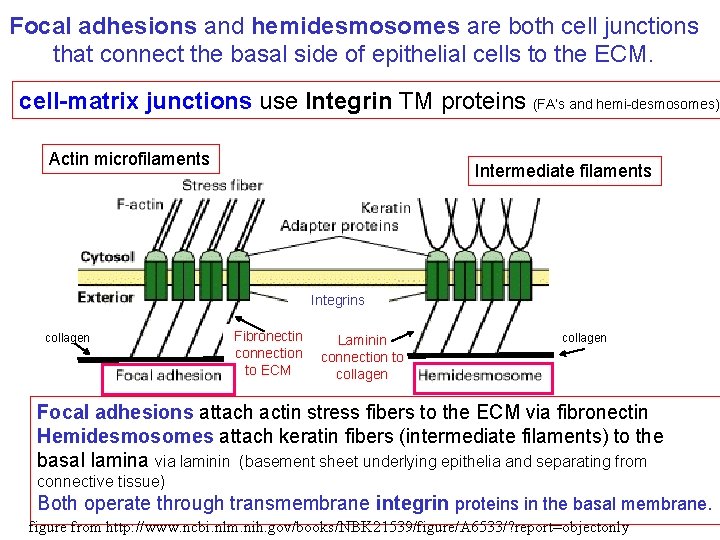
Focal adhesions and hemidesmosomes are both cell junctions that connect the basal side of epithelial cells to the ECM. cell-matrix junctions use Integrin TM proteins (FA’s and hemi-desmosomes) Actin microfilaments Intermediate filaments Integrins collagen Fibronectin connection to ECM Laminin connection to collagen Focal adhesions attach actin stress fibers to the ECM via fibronectin Hemidesmosomes attach keratin fibers (intermediate filaments) to the basal lamina via laminin (basement sheet underlying epithelia and separating from connective tissue) Both operate through transmembrane integrin proteins in the basal membrane. figure from http: //www. ncbi. nlm. nih. gov/books/NBK 21539/figure/A 6533/? report=objectonly

Review: compare focal adhesions and hemidesmosomes Focal adhesion hemidesmosome 1 - Transmembrane protein? integrins 2 - cytoskeletal connection? actin filaments intermediate filaments (stress fibers) 3 - protein connection from integrin to ECM? 4 - intracellular adaptor proteins? 5 - cell-cell or cell-matrix? (keratin) fibronectin laminin yes cell-matrix
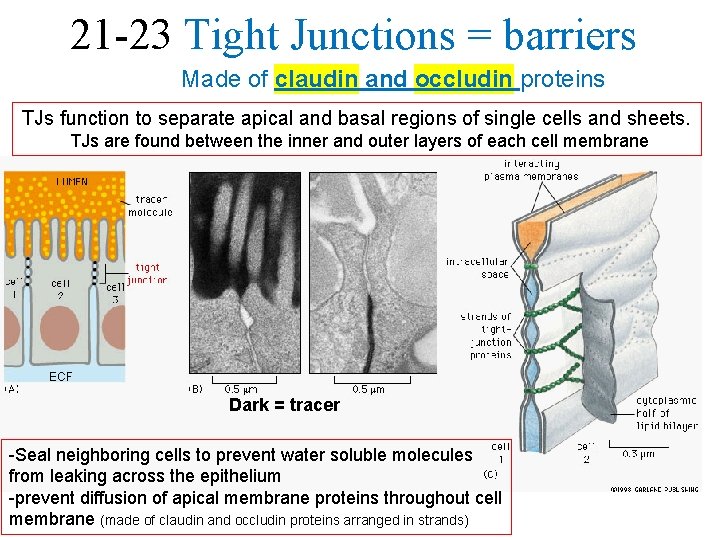
21 -23 Tight Junctions = barriers Made of claudin and occludin proteins TJs function to separate apical and basal regions of single cells and sheets. TJs are found between the inner and outer layers of each cell membrane ECF Dark = tracer -Seal neighboring cells to prevent water soluble molecules from leaking across the epithelium -prevent diffusion of apical membrane proteins throughout cell membrane (made of claudin and occludin proteins arranged in strands)
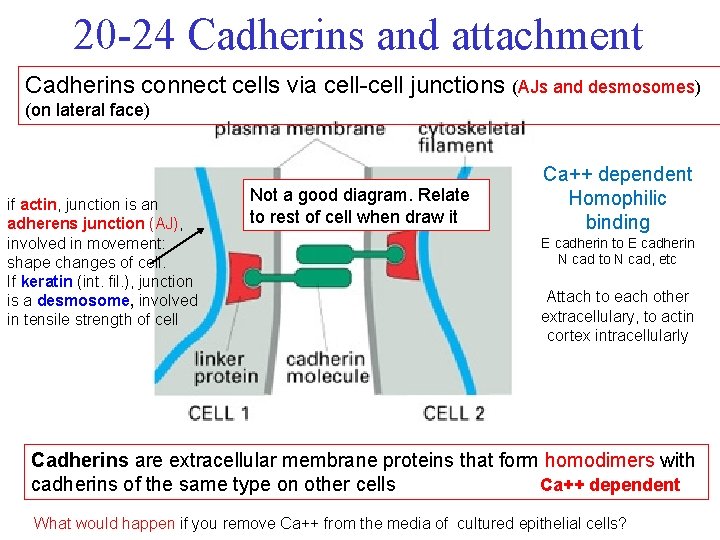
20 -24 Cadherins and attachment Cadherins connect cells via cell-cell junctions (AJs and desmosomes) (on lateral face) if actin, junction is an adherens junction (AJ), involved in movement: shape changes of cell. If keratin (int. fil. ), junction is a desmosome, involved in tensile strength of cell Not a good diagram. Relate to rest of cell when draw it Ca++ dependent Homophilic binding E cadherin to E cadherin N cad to N cad, etc Attach to each other extracellulary, to actin cortex intracellularly Cadherins are extracellular membrane proteins that form homodimers with cadherins of the same type on other cells Ca++ dependent What would happen if you remove Ca++ from the media of cultured epithelial cells?
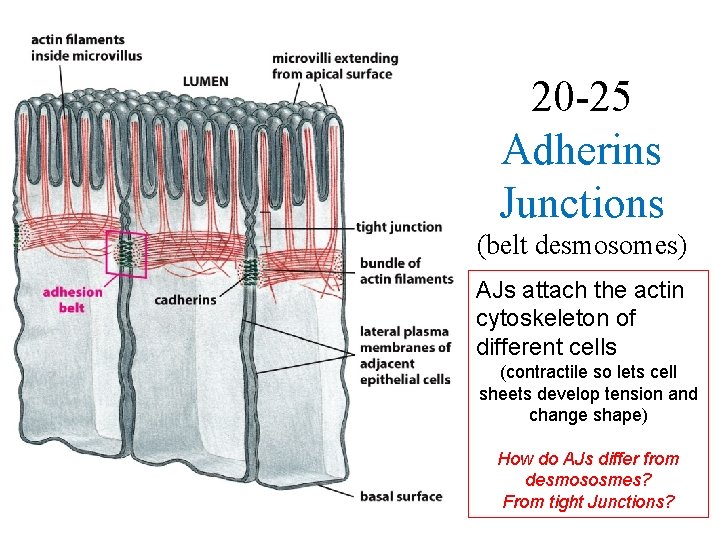
20 -25 Adherins Junctions (belt desmosomes) AJs attach the actin cytoskeleton of different cells (contractile so lets cell sheets develop tension and change shape) How do AJs differ from desmososmes? From tight Junctions?
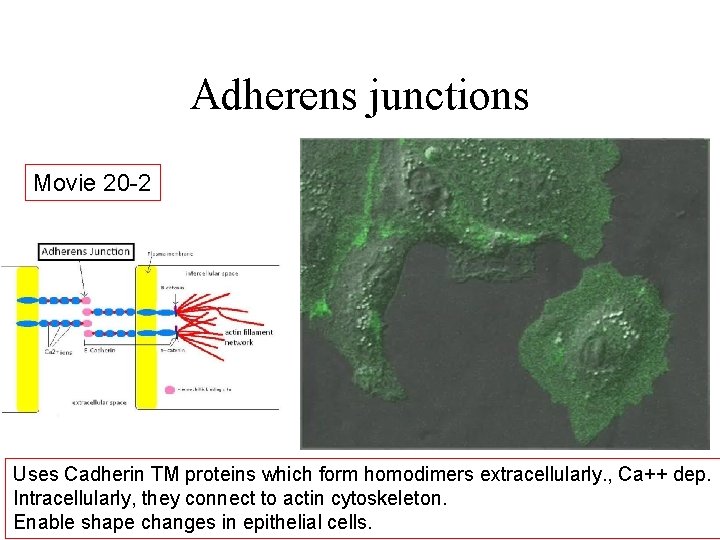
Adherens junctions Movie 20 -2 Uses Cadherin TM proteins which form homodimers extracellularly. , Ca++ dep. Intracellularly, they connect to actin cytoskeleton. Enable shape changes in epithelial cells.
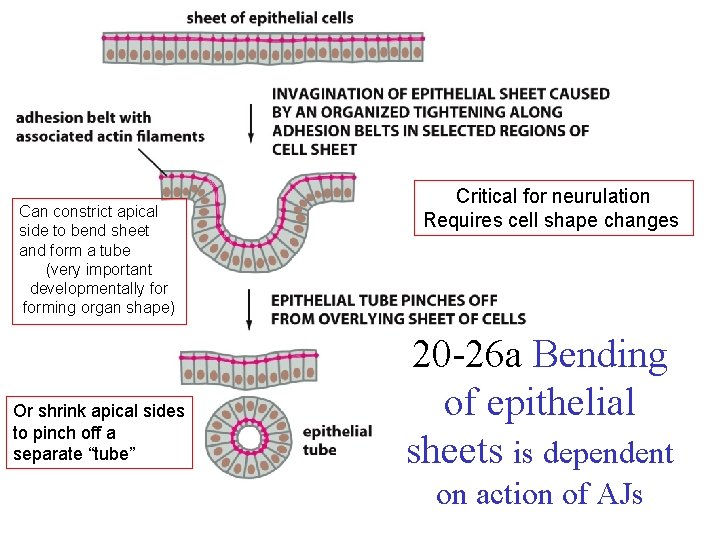
Can constrict apical side to bend sheet and form a tube (very important developmentally forming organ shape) Or shrink apical sides to pinch off a separate “tube” Critical for neurulation Requires cell shape changes 20 -26 a Bending of epithelial sheets is dependent on action of AJs
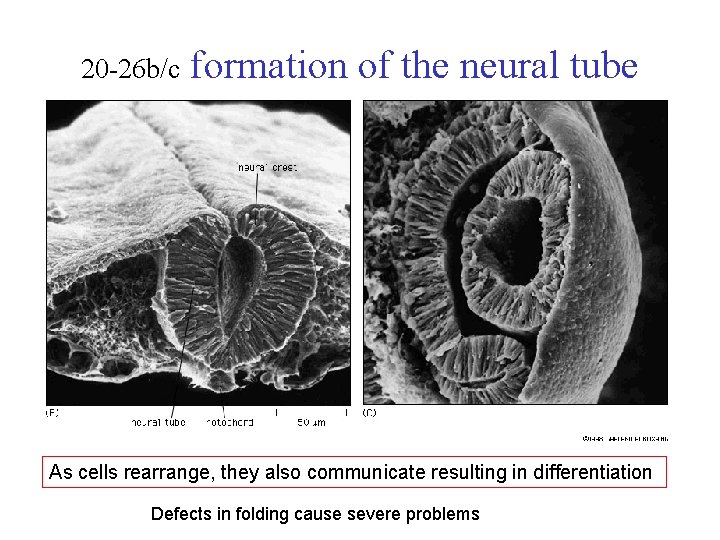
20 -26 b/c formation of the neural tube As cells rearrange, they also communicate resulting in differentiation Defects in folding cause severe problems
- Slides: 50