BIODEFENCE Epidemiology of Plague Shahid Beheshti University of

������ BIODEFENCE Epidemiology of Plague Shahid Beheshti University of medical sciences, 2005 By: Hatami H. MD. MPH 1


1 - Definition • A special zoonosis involving rodents and their fleas • Transmits to various animals and to human 3

Importance – One of three WHO quarantinable • diseases – Estimated 200 million deaths recorded • Three prior pandemics – Justinian 541 AD – Black Death 1346 – China 1855 4

Importance • Naturally occurring human outbreaks parallel and follow epizootics – BT event may also spawn sylvatic plague – Following disasters – Disruption of rat habitats – Transport of disease through rat relocation 5

Bioweapon Potential • One of top 6 agents identified by CDC (category A) • Known attempted uses – In kaffa – Japanese (Unit 731) WWII infected fleas released over China • Weapons programs – U. S. terminated 1970 – Russia unknown 6

Bioweapon Potential • Estimated Effect – Aerosol release 50 kg Y. pestis over city of 5 million people • 150, 000 infected • 36, 000 die 7

Bioweapon Potential Delivery Mechanism • Aerosol – Bioweapons programs developed techniques to aerosolize plague directly – Pneumonic form would be expected – Proven infectivity of primates 8

Factors suggesting BT aerosol • Several cases of primary pneumonic (no or few bubonic) • Peak in number of previously healthy persons with cough, fever, death • Many with GI symptoms • Occurs in non-endemic area 9

Factors suggesting BT aerosol • Epidemic of severe/fatal pneumonia (hemoptysis) • Symptoms 1 -6 days after exposure • Occurs in persons without risk factors 10

2 - Etiologic agent • Taxonomy –Family Enterobacteriaceae – 11 Yersinia species – 3 human pathogens • Y. pestis • Y. pseudotuberculosis • Y. enterocolitica 11

Microbiology • Staining – Gram negative coccobacillus – Giemsa, Wright, Wayson stains – bipolar staining 12

Environmental Survival – Requires host – Does not survive in environment well – Can live weeks in water, moist soil – Lives months/years at just above freezing temperature – Lives only 15 minutes in 55 C – Lives in dry sputum, corpses, flea feces – Inactivated by sunlight in a few hours 13

Pathogenesis • Highly virulent and invasive Four routes human disease: 1) Flea-bite (most common) 2) Handling infected animals- skin contact, scratch, bite 3) Inhalation – from humans or animals 4) Ingesting infected meat 14

Pathogenesis • Intracellular organism – Survives in monocytes/macrophages • Inhalation (pneumonic form) – Deposition into alveoli – Classic lobular pneumonia • Resulting manifestation – liquefaction necrosis, residual scarring 15


ـ ﺩﻭﺭﻩ ﻧﻬﻔﺘگﻲ 1 • Incubation Period • 1 -7 days • Longer in immunized individuals • For primary pneumonia, 1 -4 days Ref. : Control of communicable diseases 17

ـ ﺳﻴﺮ ﻃﺒﻴﻌﻲ 2 Clinical Features • Three types of Disease –Bubonic –Septicemic –Pneumonic 18

Clinical Features • Bubonic – Classic – Predominates (84%) • Usually from bite of infectious flea • Contact ingestion of infected animals 19

Clinical Features –Buboes • Enlarged tender lymph nodes • Usually unilateral Image: Armstrong & Cohen • Usually inguinal/femoral in adults • Cervical/submaxillary more common in age < 10 20

Clinical Features • Bubonic – Mortality • • • 40 -60% untreated, <5% treated Overall case fatality 14% in U. S. Usually from delayed Dx and Rx – Complications • Often develop bacteremia • Some develop: – Septicemia (secondary septicemic plague) – Pneumonic (secondary pneumonic plague) – meningitis 21

Clinical Features • Septicemic – Historically 12% – Secondary if complication of bubonic – Primary if no buboes detected 22

Clinical Features • Septicemic – Similar to other gram-negative sepsis – Mortality • Overall 50% • > 90% untreated • Usually from late diagnosis and Rx 23

Clinical Features • Pnuemonic • Approx. 2% all plague are primary pneumonic • Secondary if preceding bubonic (most cases) or septicemic 24

Clinical Features • Pneumonic – Primary if result of droplet inhalation • From other pneumonic plague patients or infected animals • From expected if aerosolized as a bioweapon – Extremely infectious via droplets and purulent sputum 25

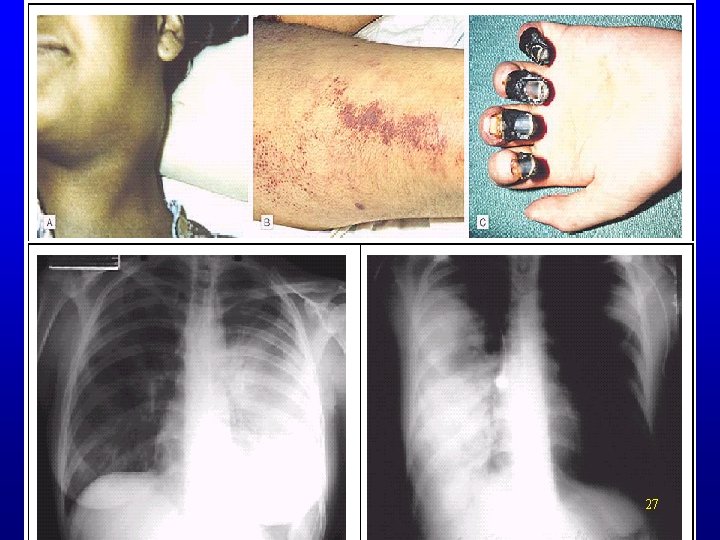
Clinical Features • Pneumonic – Mortality • Nearly 100% untreated or if delayed > 24 hrs after symptom onset • High despite treatment • Overall case fatality 57% in U. S. 26
27

Clinical Features • In BT event pneumonic form most likely • Pneumonic – – incubation 1 -6 days for primary Initial–acute flu-like , myalgia, malaise Often prominent GI , abd pain Severe pneumonia • • • Within 24 hr of onset Cough, hemoptysis Progresses to cyanosis, stridor – Death usually occurs 2 -4 days after exposure 28

Clinical Features • Immunity – Several days after infection • <5% never – Transient, not life-long immunity after surviving – May not protect against a large inoculum – Antibody levels normalize in months-years 29



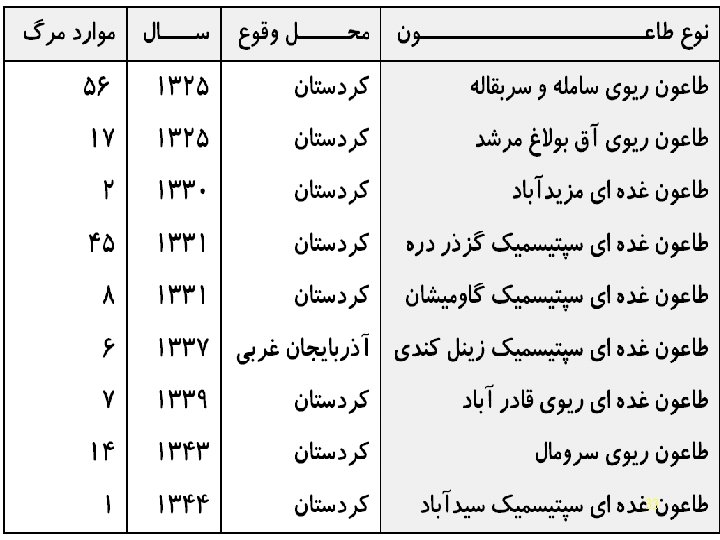
Geographic distribution – Globally • Approximately 1500 cases/year since 1965 • 25 countries reported cases • > 50% Eastern, S. Africa, – U. S. • 390 cases/year reported 1947 -96 • Southwest region of U. S. endemic 32
33
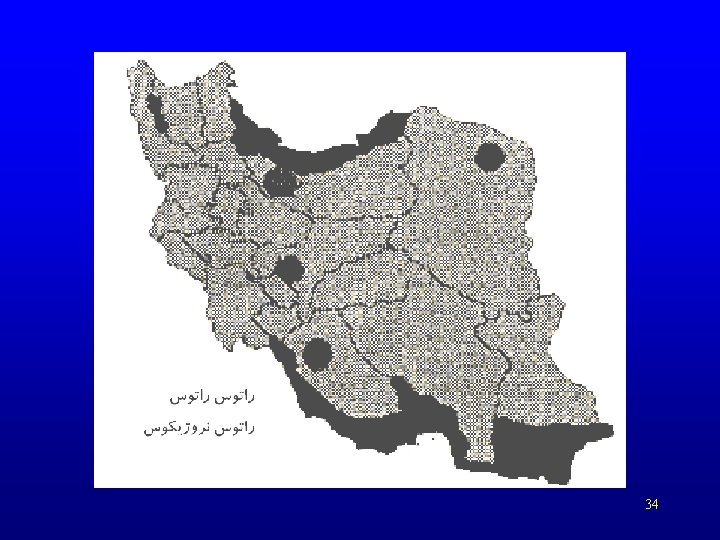
34
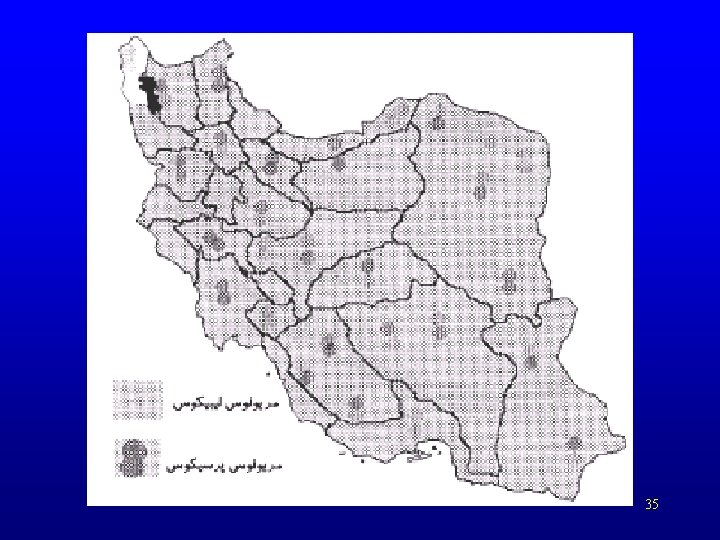
35




Risk factors – Close contact with case – Contact with infected animal – Living or recent travel in endemic area – Residing in crowded conditions – Cool, wet weather – Exposure to a known intentional release 39


ـ ﻣﻴﺰﺍﻥ ﺣﻤﻼﺕ ﺛﺎﻧﻮﻳﻪ 8 • Pneumonic plague may be highly communicable under appropriate climatic conditions 41


Transmission • Mostly endemic sylvatic plague with sporadic cases • Person to person spread • Higher risk in: • Overcrowding, • Indoor contacts, • Cold/wet weather • Fleas may remain infective for months 43
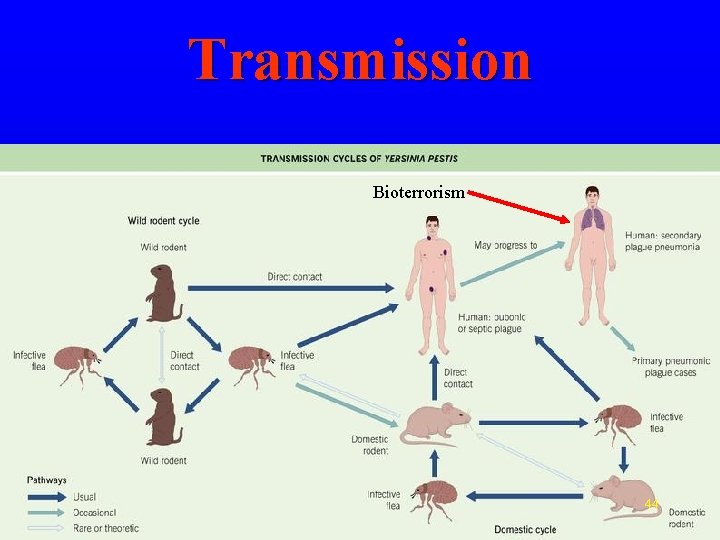
Transmission Bioterrorism 44

Period of communicability • Duration of isolation – 2 days after initiating antibiotics and clinically improved –After sputum cultures negative 45

Reservoir • • Wild rodents Rabies & hares Wild carnivores Domestic cats 46

ﺝ ـ پﻴﺸگﻴﺮﻱ ﻭ ﻛﻨﺘﺮﻝ ﻃﺎﻋﻮﻥ • Primary Prevention: n Prevention of disease in “well” individuals • Secondary Prevention: n n n Identification and intervention in early stages of disease Tertiary Prevention: Prevention of further deterioration, reduction in complications 47


Prevention • Vaccination - Bubonic only – Killed virulent strain • No longer commercially available – Series • 3 primary (0 , 3 mo and 6 mo later) • boosters at 6 mo intervals 49

Prevention • Vaccination – Indications • Lab workers • Military personnel stationed in endemic areas – Efficacy • Based on WWII (0 cases) and Vietnam (3 cases) troops • Protects vs. bubonic only, not pneumonic 50
Infection Control Respiratory Droplet Precautions – Wear mask, gown, gloves, eye protection – Suspected cases - isolate • Immediately respiratory (even for bubonic) • Avoid unnecessary close contact 1 st 48 hrs of abx • Duration – 2 days after initiating antibiotics and clinically improved – After sputum cultures negative 51

Infection Control • Respiratory Droplet Precautions – Mask during transport – Can cohort if not enough room • Contacts – consider isolation – Recommended for those receiving PEP • During 1 st 48 hrs of Rx – Not recommended for those refusing PEP • but still observe 7 days 52

Infection Control • Standard Precautions – Successfully treated cases after 48 hr of abx • Laboratory safety – Alert lab if suspected – BSL-2 for normal procedures – BSL-3 if hi risk aerosolizing or resistant strains 53

Infection Control • Corpses – Standard strict precautions by trained personnel – Transport same as live patient – Avoid aerosolizing procedures or use HEPA filters and negative pressure room 54

Infection Control • Outbreak measures • Establish source • Define geographical boundaries • Establish active surveillance • Laboratory confirmation of cases • Isolation of pneumonic cases • Rapid treatment of cases and contacts • Flea and rodent control 55

Infection Control • National control programs – Surveillance – Early diagnosis, treatment & isolation of cases – Environmental sanitation & exposure avoidance – Public education 56

Decontamination • Environment – Aerosol dispersed within an hour – fragile – No evidence residual bacteria are a threat – No environmental decon. indicated – May need surveillance measures for rodents/fleas in area 57

Decontamination • Patient rooms –Usual cleaning –Use standard precautions –Disinfect contaminated linens –Standard disinfectants 58

Post-exposure Prophylaxis • Also for mass causalities • For all asymptomatic contacts of suspected untreated pneumonic cases – Contact within last 6 days – Untreated pneumonic = <48 hr approp treatment – Those within 2 meters of case – Household, hospital contacts – Those who might have been exposed to initial aerosol – Seek out homeless, mental handicaps, 59 homebound

Post-exposure Prophylaxis • Antibiotics – 1 st choices • Tetracyclines – Doxycycline » 100 po bid adults and kids >45 kg » 2. 2 mg/kg po bid for kids <45 kg – Tetracycline – equivalent dosages • Fluoroquinolones – Ciprofloxacin » 500 mg po bid for adults » 20 mg/kg po bid (max 1 g/day) for kids – Others at equivalent dosages 60

Post-exposure Prophylaxis • Alternatives – Chloramphenical 25 mg/kg po qid • Not in kids <2 yo • For pregnant & breastfeeding women – Same as adults above but no tetracycline – Doxycycline may be used • Duration – 7 days since last exposure PEP – 10 days for mass casualties 61


Diagnosis • No rapid tests available – treat first • Report suspected cases to local health dept if no risk factor for naturally occurring disease • Send out samples if not done in hospital • Obtain specimens as indicated: – Blood – attempt 4 samples q 30 min – Bubo aspirate (inject 1 -2 cc saline and aspirate with 20 Ga needle) – Sputum 63 – CSF

Diagnosis • CXR • Inoculate on/in infusion broth, blood agar, Mc. Conkey agar • Biochemical profiles if automated system has capacity to detect • Stains – Gram and Wayson’s or Giemsa • DFA testing • Acute serum for F 1 antibody • CDC sample for bacteriophage lysis 64

Treatment • Start immediately upon suspicion of diagnosis • Delay >1 day after symptoms usually fatal 65

Treatment • Antibiotics – General • Contained casualties – IV • Mass casualties – po equivalent, same as postexposure prophylaxis • Also need intensive supportive care – Ventilation – Pressors usually not needed • Who to treat – Suspected cases » Index » If suspected release – anyone with fever, cough 66

Treatment • Special populations – Children • Same as adults but try avoid TCN if <8 yo • No chloramphenicol for <2 yo (grey baby syndrome) – Pregnant women • • Try to avoid streptomycin 1 st choice gentamicin, same adult dose 2 nd choice doxy, same adult dose 3 rd choice cipro, same adult dose – Breastfeeding women • Same recommendations as pregnant – Immunosuppressed – no different than competent 67

Treatment • Antibiotics for contained casualties – (For mass casualties, same as PEP) – 1 st choices • Streptomycin - FDA-approved – 30 mg/kg IM divided q 8 -12 kids (max 2 g/day) – 1 g IM bid adult – bacteriocidal • gentamicin –as effective, more avail, qd dosing – 5 mg/kg iv qd, w/levels or load 2 mg/kg then 1. 7 mg/kg q 8 – 2. 5 mg/kg im/iv q 8 h kids (q 12 hr for <1 wk or premature) 68

Treatment – 2 nd choices • tetracyclines - as good in vitro, good human data – doxycycline » single 200 mg iv loading dose (some sources) » 100 mg iv bid or 200 mg iv qd adults& kids >45 kg » 2. 2 mg/kg iv q 12 hr (max 200 mg) kids <45 kg » Better absorption, distribution, half-life than TCN » 1 st choice po therapy for mass casualties – tetracycline » 500 mg po qid adults » 6. 25 -12. 5 mg/kg po qid kids >9 yo 69

Treatment – 2 nd choices • Fluoroquinolones–better in vitro, no human data – ciprofloxacin » » 400 mg iv q 12 hr adults 15 mg/kg iv q 12 hr kids (max 1 g/day) – Levofloxacin – Ofloxacin • Chloramphenicol – 1 st choice for meningitis +/- aminoglycoside – Crosses blood-brain barrier – 25 mg/kg iv q 6 hr adults & kids, keep level 520 μg/ml – Avoid in kids <2 yo (grey baby syndrome) 70

Treatment – 2 nd choices • Alternatives – sulfonamides – If other antibiotics not available – Ineffective for pneumonic – TMP-SMX • Generally ineffective – Β-lactams, rifampin, aztreonam, macrolides 71

Treatment • Antibiotic resistance rare – May be expected in BT scenario (engineered agents) 72

Treatment • Switch to po when improved, tolerates • Usual response – Bubonic – improved in 2 -3 d, afebrile 2 -5 d • Duration – 10 -14 days or 3+ days after afebrile, improving • Supportive care – Volume status maintenance – Hemodynamic monitoring • pressors not usually needed – Support of multiorgan failure 73

Treatment • Bubo care – Usually recedes with antibiotics – Rarely become fluctuant/abscessed – Unnecessary I & D increases contact’s risks 74




- Slides: 78