Biochemistry of Coagulation Ahmad Shihada Silmi Msc FIBMS

Biochemistry of Coagulation Ahmad Shihada Silmi Msc, FIBMS Staff Specialist in Hematology Medical Technology Department Islamic University of Gaza 2012










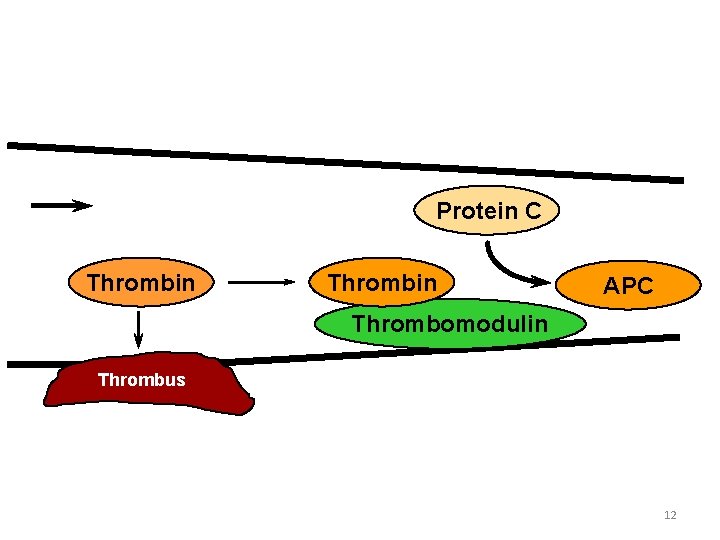
The Protein C Anticoagulant Pathway Blood Flow Thrombin Protein C Thrombin APC Thrombomodulin Thrombus at site of injury Anticoagulation downstream 12
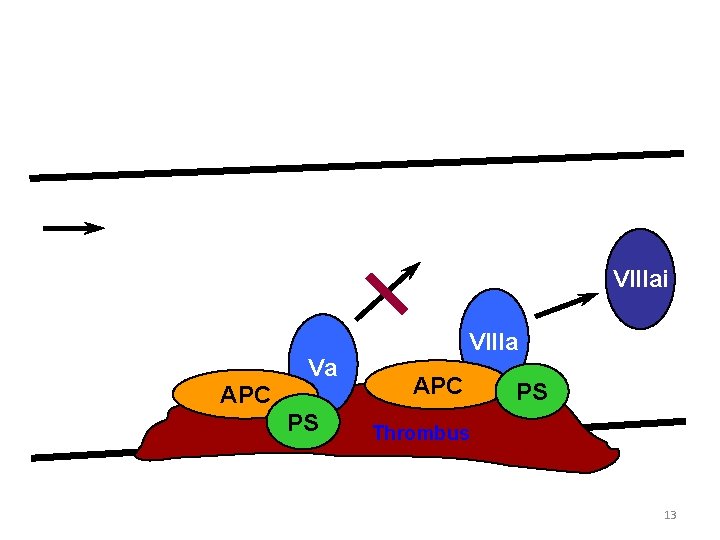
The Protein C Anticoagulant Pathway Blood Flow Vai Factor V Leiden Va APC PS VIIIai VIIIa APC PS Thrombus 13

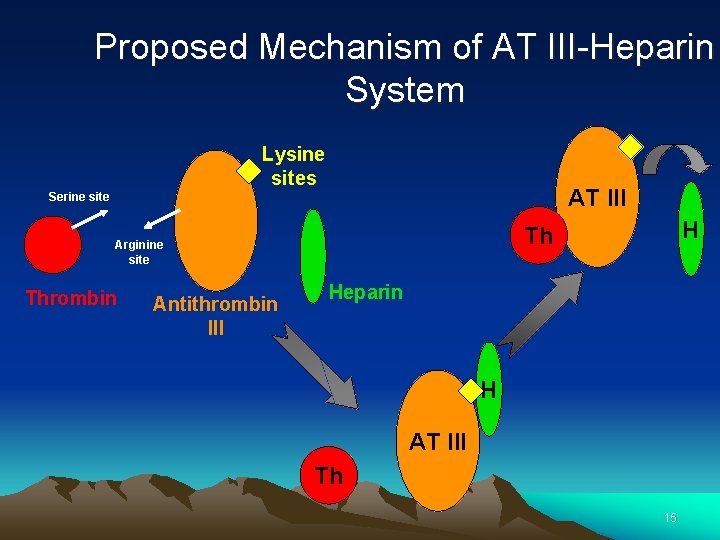
Proposed Mechanism of AT III-Heparin System Lysine sites AT III Serine site Thrombin Antithrombin III H Th Arginine site Heparin H AT III Th 15


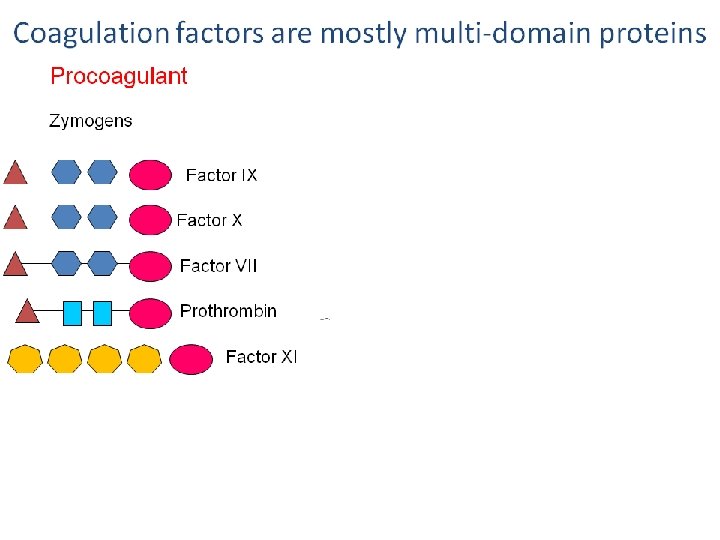










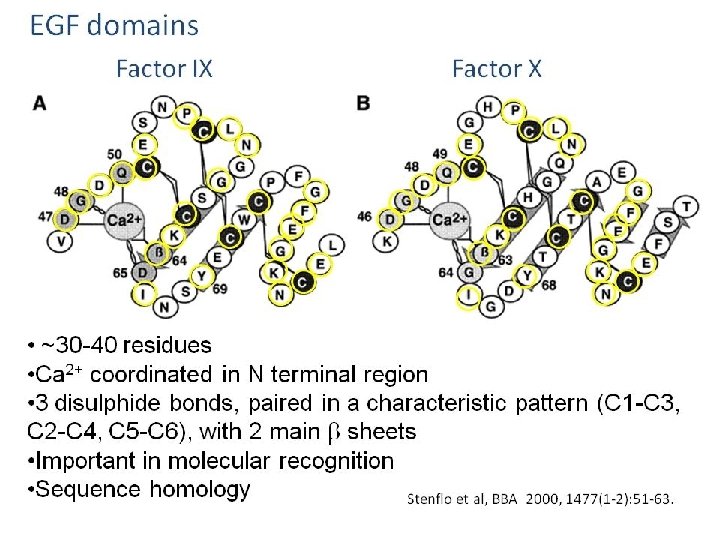







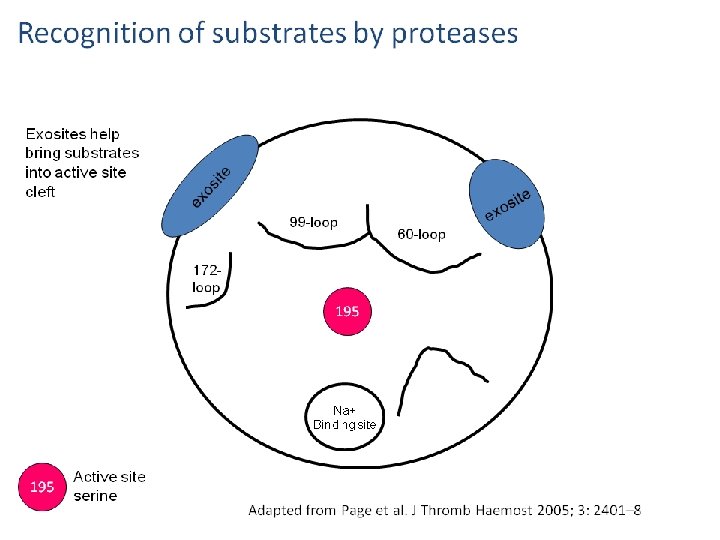
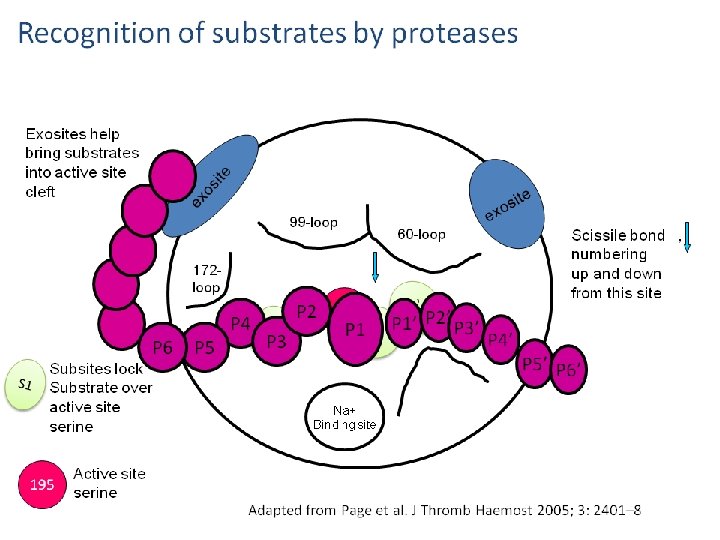
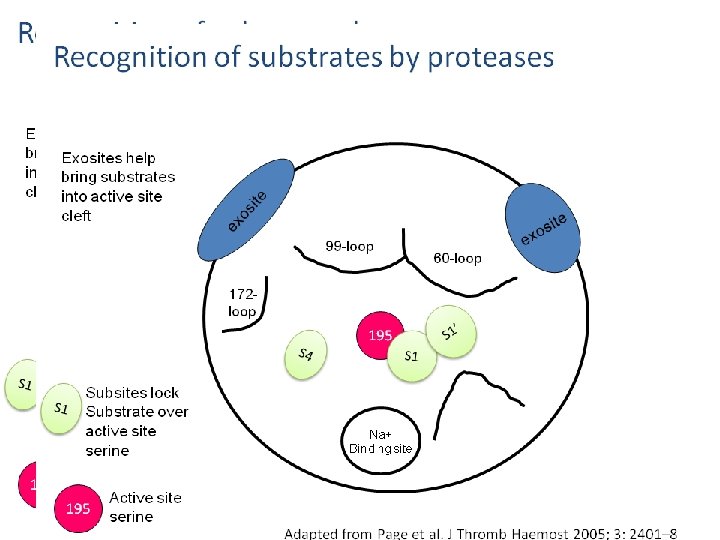








Fibrinolytic Pathway Fibrinolysis is initiated when fibrin is formed and eventually dissolves the clot. 47

Fibrinolytic Pathway PAI-1 Plasminogen Tissue Plasminogen Activator ( Urokinase (u. PA) Exogenous: streptokinase XL-Fibrin, fibrinogen Plasmin Inhibitor Plasmin XL- fibrin degradation products (FDP) 48
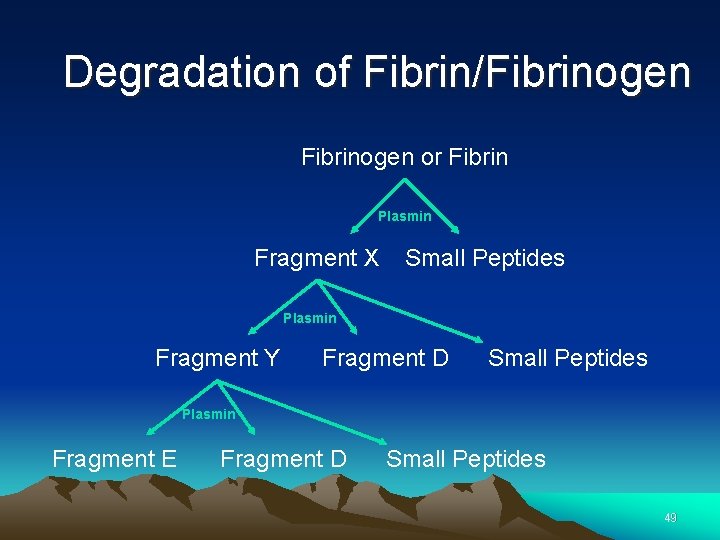
Degradation of Fibrin/Fibrinogen or Fibrin Plasmin Fragment X Small Peptides Plasmin Fragment Y Fragment D Small Peptides Plasmin Fragment E Fragment D Small Peptides 49

Approach to evaluate Fibrinolysis D-Dimer, a measure of fibrin degradation products, is the final product formed during the fibrinolysis process by plasmin 50

Approach to evaluate Fibrinolysis cont, – Elevated levels of D-Dimer are indicative of on -going fibrinolysis • Found high in : • (DVT) • (PE) • (DIC) • D-Dimer levels also rise during the normal pregnancy and very high levels are associated with complications. 51

Bleeding Disorders 52

Clinical Features of Bleeding Disorders Platelet disorders Coagulation factor disorders Site of bleeding Skin Deep in soft tissues Mucous membranes (joints, muscles) (epistaxis, gum, vaginal, GI tract) Petechiae Yes No Ecchymoses (“bruises”) Small, superficial Large, deep Hemarthrosis / muscle bleeding Extremely rare Common Bleeding after cuts & scratches Yes No Bleeding after surgery or trauma Immediate, usually mild Delayed (1 -2 days), often severe 53

Hematologic disorders causing bleeding – Coagulation factor disorders – Platelet disorders 54

Coagulation factor disorders Inherited bleeding disorders – Hemophilia A and B – Von Willebrands disease – Other factor deficiencies Acquired bleeding disorders – Liver disease – Vitamin K deficiency/warfarin overdose – DIC 55

Hemophilia A and B Coagulation factor deficiency Inheritance Incidence Severity Complications Hemophilia A Hemophilia B Factor VIII Factor IX X-linked recessive 1/10, 000 males 1/50, 000 males Related to factor level <1% - Severe - spontaneous bleeding 1 -5% - Moderate - bleeding with mild injury 5 -25% - Mild - bleeding with surgery or trauma Soft tissue bleeding 56

Hemophilia Clinical manifestations (hemophilia A & B are indistinguishable) Hemarthrosis (most common) Fixed joints Soft tissue hematomas (e. g. , muscle) Muscle atrophy Shortened tendons Other sites of bleeding Urinary tract CNS, neck (may be life-threatening) Prolonged bleeding after surgery or dental extractions 57

Hemarthrosis (acute) 58

von Willebrand Disease: Clinical Features von – – – Willebrand factor Synthesis in endothelium and megakaryocytes Forms large multimer Carrier of factor VIII Anchors platelets to subendothelium Bridge between platelets Inheritance Incidence Clinical - autosomal dominant - 1/10, 000 features - mucocutaneous bleeding 59

Laboratory evaluation of von Willebrand disease Classification – Type 1 Partial quantitative deficiency – Type 2 Qualitative deficiency – Type 3 Total quantitative deficiency Diagnostic tests: Assay 1 von. Willebrand type 2 3 __________________________ v. WF antigen v. WF activity Multimer analysis ß ß Normal ßß ßß Absent 60

Vitamin K deficiency Source of vitamin K Green vegetables Synthesized by intestinal flora Required for synthesis Factors II, VII, IX , X, Protein C and S Causes of deficiency Malnutrition Biliary obstruction Malabsorption Antibiotic therapy Treatment Vitamin K Fresh frozen plasma 61

Common clinical conditions associated with Disseminated Intravascular Coagulation • Activation of both coagulation and fibrinolysis Triggered by • Sepsis • Trauma – Head injury – Fat embolism • Malignancy • Obstetrical complications – Amniotic fluid embolism – Abruptio placentae • Vascular disorders • Reaction to toxin (e. g. snake venom, drugs) • Immunologic disorders – Severe allergic reaction – Transplant rejection 62

Disseminated Intravascular Coagulation (DIC) Mechanism Systemic activation of coagulation Intravascular deposition of fibrin Thrombosis of small and midsize vessels with organ failure Depletion of platelets and coagulation factors Bleeding 63
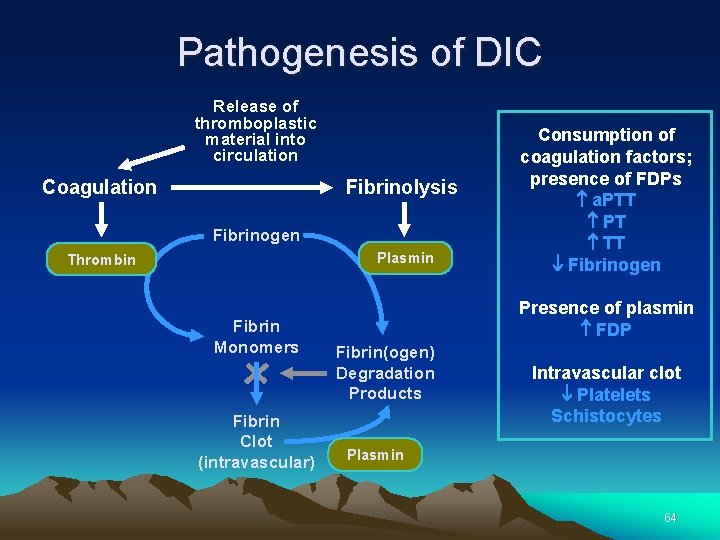
Pathogenesis of DIC Release of thromboplastic material into circulation Coagulation Fibrinolysis Fibrinogen Plasmin Thrombin Fibrin Monomers Fibrin Clot (intravascular) Consumption of coagulation factors; presence of FDPs a. PTT PT TT Fibrinogen Presence of plasmin FDP Fibrin(ogen) Degradation Products Intravascular clot Platelets Schistocytes Plasmin 64

Classification of platelet disorders • Quantitative disorders – Abnormal distribution – Dilution effect – Decreased production – Increased destruction • Qualitative disorders – Inherited disorders (rare) – Acquired disorders • Medications • Chronic renal failure • Cardiopulmonary bypass 65

Laboratory Evaluation of Bleeding Overview CBC and smear Platelet count RBC and platelet morphology Thrombocytopenia TTP, DIC, etc. Coagulation Prothrombin time Partial thromboplastin time Coagulation factor assays 50: 50 mix Fibrinogen assay Thrombin time fibrinogen defects FDPs or D-dimer Extrinsic/common pathways Intrinsic/common pathways Specific factor deficiencies Inhibitors (e. g. , antibodies) Decreased fibrinogen Qualitative/quantitative von Willebrand factor Bleeding time Platelet function analyzer (PFA) Platelet function tests v. WD In vivo test (non-specific) Qualitative platelet disorders and v. WD Qualitative platelet disorders Platelet function Fibrinolysis (DIC) 66
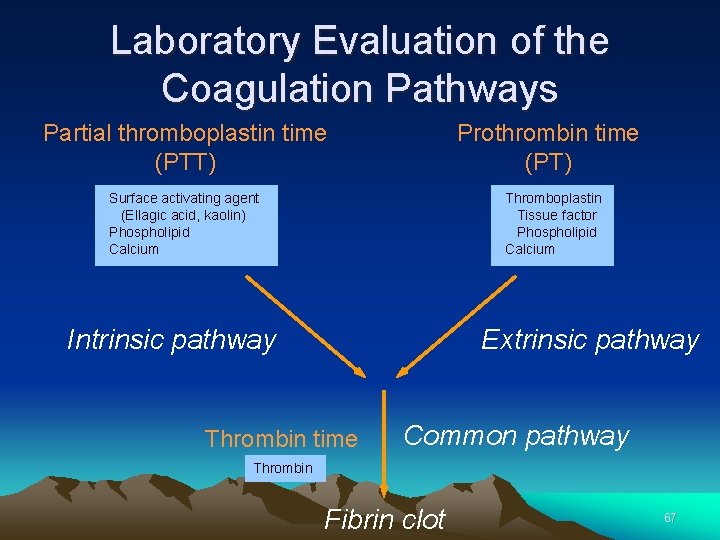
Laboratory Evaluation of the Coagulation Pathways Partial thromboplastin time (PTT) Prothrombin time (PT) Surface activating agent (Ellagic acid, kaolin) Phospholipid Calcium Thromboplastin Tissue factor Phospholipid Calcium Intrinsic pathway Extrinsic pathway Thrombin time Common pathway Thrombin Fibrin clot 67

Pre-analytic errors Problems with blue-top tube – Hct ≥ 55 or ≤ 15 – Lipemia, hyperbilirubinemia, hemolysis – Partial fill tubes – Vacuum leak and citrate evaporation Problems with phlebotomy – – – Heparin contamination Wrong label Slow fill Underfill Vigorous shaking Biological effects Laboratory errors – Delay in testing – Prolonged incubation at 37°C – Freeze/thaw deterioration 68
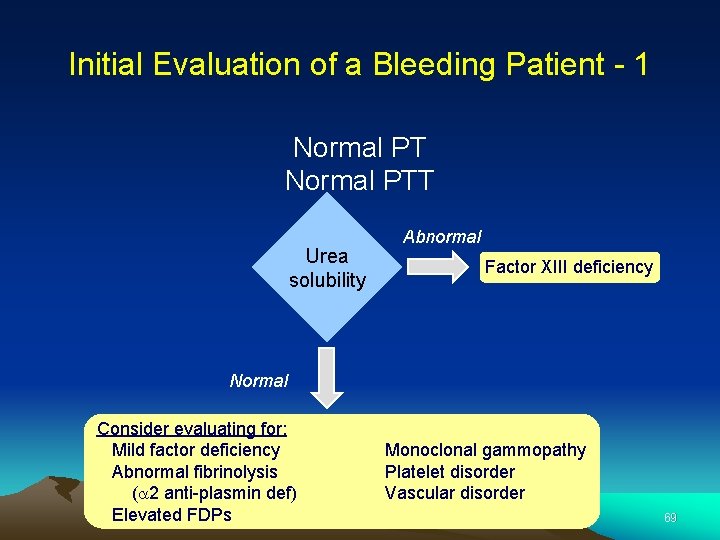
Initial Evaluation of a Bleeding Patient - 1 Normal PTT Urea solubility Abnormal Factor XIII deficiency Normal Consider evaluating for: Mild factor deficiency Abnormal fibrinolysis (a 2 anti-plasmin def) Elevated FDPs Monoclonal gammopathy Platelet disorder Vascular disorder 69

Initial Evaluation of a Bleeding Patient - 2 Normal PT Abnormal PTT Repeat with 50: 50 mix is abnormal Test for inhibitor activity: Specific factors: VIII, IX, XI Non-specific (anti-phospholipid Ab) 50: 50 mix is normal Test for factor deficiency: Isolated deficiency in intrinsic pathway (factors VIII, IX, XI) Multiple factor deficiencies (rare) 70
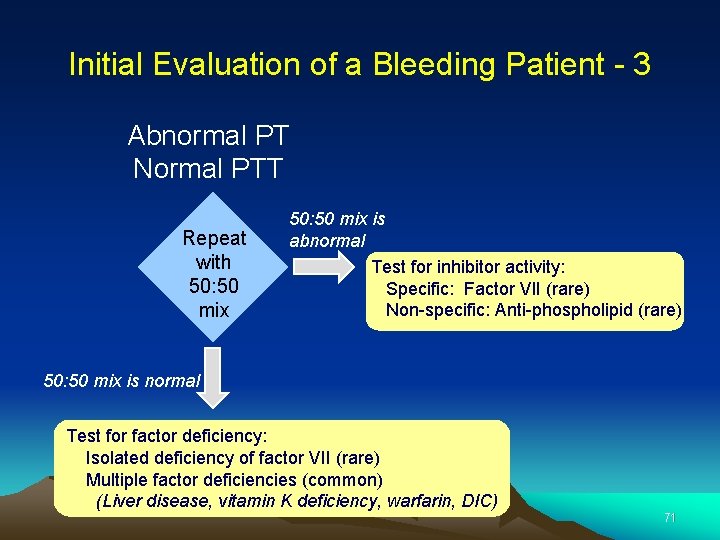
Initial Evaluation of a Bleeding Patient - 3 Abnormal PT Normal PTT Repeat with 50: 50 mix is abnormal Test for inhibitor activity: Specific: Factor VII (rare) Non-specific: Anti-phospholipid (rare) 50: 50 mix is normal Test for factor deficiency: Isolated deficiency of factor VII (rare) Multiple factor deficiencies (common) (Liver disease, vitamin K deficiency, warfarin, DIC) 71

Initial Evaluation of a Bleeding Patient - 4 Abnormal PTT Repeat with 50: 50 mix is abnormal Test for inhibitor activity: Specific : Factors V, X, Prothrombin, fibrinogen (rare) Non-specific: anti-phospholipid (common) 50: 50 mix is normal Test for factor deficiency: Isolated deficiency in common pathway: Factors V, X, Prothrombin, Fibrinogen Multiple factor deficiencies (common) (Liver disease, vitamin K deficiency, warfarin, DIC) 72

Coagulation factor deficiencies Summary Sex-linked recessive Factors VIII and IX deficiencies cause bleeding Prolonged PTT; PT normal Autosomal recessive (rare) Factors II, V, VII, X, XI, fibrinogen deficiencies cause bleeding Prolonged PT and/or PTT Factor XIII deficiency is associated with bleeding and impaired wound healing PT/ PTT normal; clot solubility abnormal Factor XII, prekallikrein, HMWK deficiencies do not cause bleeding 73

Thrombin Time Bypasses factors II-XII Measures rate of fibrinogen conversion to fibrin Procedure: – Add thrombin with patient plasma – Measure time to clot Variables: – Source and quantity of thrombin 74

Causes of prolonged Thrombin Time Heparin Hypofibrinogenemia Dysfibrinogenemia Elevated FDPs or paraprotein Thrombin inhibitors (Hirudin) Thrombin antibodies 75

Approach to the thrombocytopenic patient History – Is the patient bleeding? – Are there symptoms of a secondary illness? (neoplasm, infection, autoimmune disease) – Is there a history of medications, alcohol use, or recent transfusion? – Are there risk factors for HIV infection? – Is there a family history of thrombocytopenia? – Do the sites of bleeding suggest a platelet defect? Assess the number and function of platelets – CBC with peripheral smear – Bleeding time or platelet aggregation study 76
77

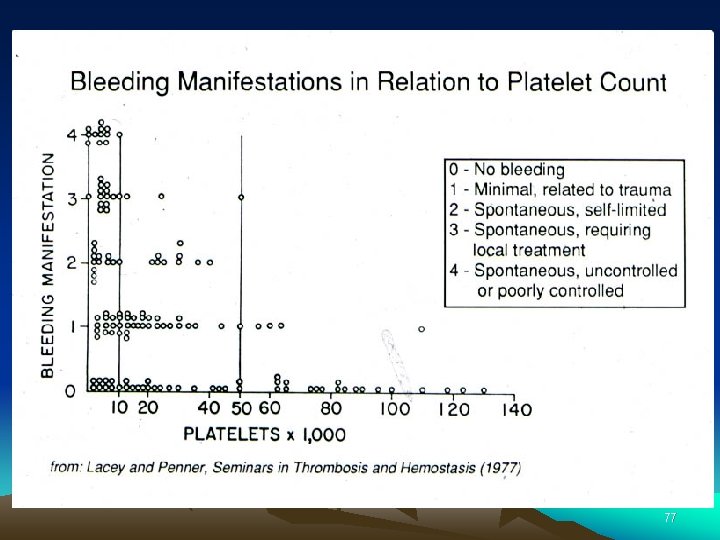
Bleeding time and bleeding 5 -10% time of patients have a prolonged bleeding Most of the prolonged bleeding times are due to aspirin or drug ingestion Prolonged bleeding time does not predict excess surgical blood loss Not recommended for routine testing in preoperative patients 78

Conclusion Special Coagulation is a specialized, complex and dynamic field! 79
- Slides: 79