Biochemistry Microbiology and Immunology January 7 2022 Week

Biochemistry, Microbiology and Immunology January 7, 2022 Week 9: 8 The immune system
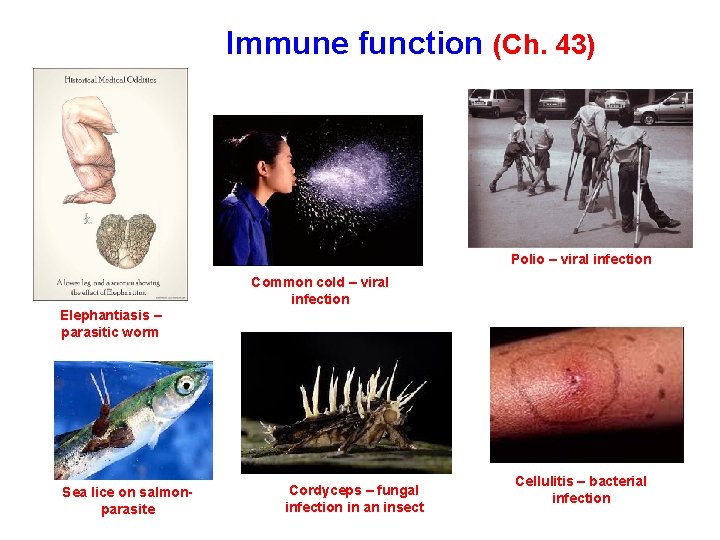
Immune function (Ch. 43) Polio – viral infection Common cold – viral infection Elephantiasis – parasitic worm Sea lice on salmonparasite Cordyceps – fungal infection in an insect Cellulitis – bacterial infection

Overview of animal immune systems (Fig. 43. 2) Innate immunity - animals/plants - rapid - small # receptors Adaptive immunity - vertebrates only - slower - vast # receptors

Innate immunity – occurs in all animals (and plants) • Non-specific mechanisms providing rapid initial response to a pathogen • Immune response is the same regardless of whether pathogen has been encountered previously (not “adaptive”) Barrier defences – first stop pathogens from entering body Toxic chemical secretions on toad’s skin – kills microbes Skin Mucous membranes lining exchange surfaces

Barrier Defenses • Barrier defenses include the skin and mucous membranes of the respiratory, urinary, and reproductive tracts • Mucus traps and allows for the removal of microbes • Many body fluids including saliva, mucus, and tears are hostile to microbes • The low p. H of skin and the digestive system prevents growth of microbes

Innate immunity – second, deal with pathogen if it breaches barrier defences and enters the body • Animals must be able to tell pathogens (“non-self”) from their own tissues, cell, proteins (“self”) • Molecular recognition: specific receptors detect a small number of highly conserved molecules present in many different pathogens - lipopolysaccharide (LPS) - peptidoglycans • uses Toll or Toll-like receptors (proteins discovered in Drosophila, 10 -11 in mice/humans) Recognition leads to range of responses to deal with pathogen: Encapsulation and phagocytosis Expression of antimicobial proteins Local inflammation Fever (systemic inflammation)
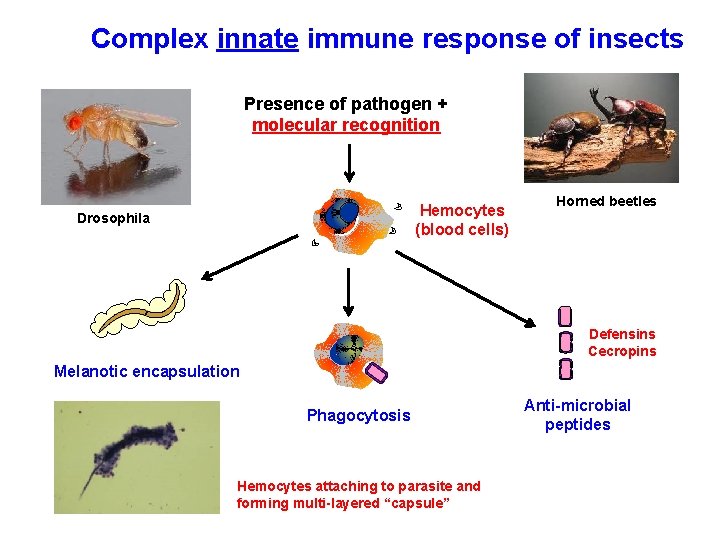
Complex innate immune response of insects Presence of pathogen + molecular recognition Hemocytes (blood cells) Drosophila Horned beetles Defensins Cecropins Melanotic encapsulation Phagocytosis Hemocytes attaching to parasite and forming multi-layered “capsule” Anti-microbial peptides
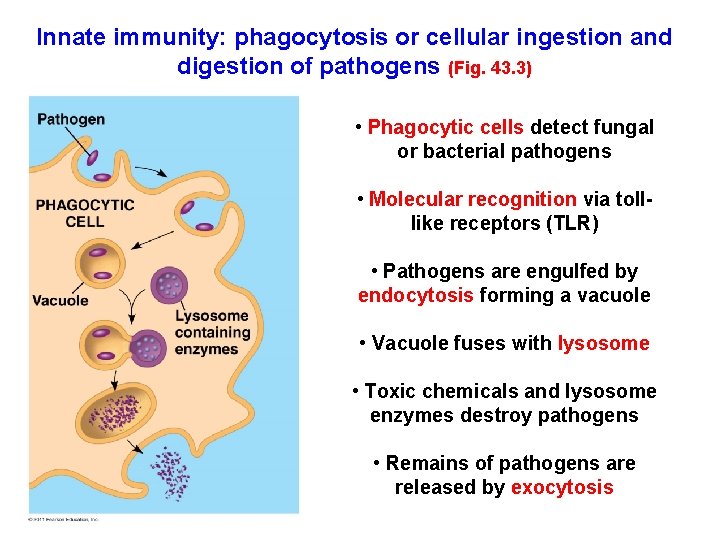
Innate immunity: phagocytosis or cellular ingestion and digestion of pathogens (Fig. 43. 3) • Phagocytic cells detect fungal or bacterial pathogens • Molecular recognition via tolllike receptors (TLR) • Pathogens are engulfed by endocytosis forming a vacuole • Vacuole fuses with lysosome • Toxic chemicals and lysosome enzymes destroy pathogens • Remains of pathogens are released by exocytosis

• A white blood cell engulfs a microbe, then fuses with a lysosome to destroy the microbe • There are different types of phagocytic cells: – Neutrophils engulf and destroy microbes – Macrophages are part of the lymphatic system and are found throughout the body – Eosinophils discharge destructive enzymes – Dendritic cells stimulate development of acquired immunity

Antimicrobial Peptides and Proteins • Peptides and proteins function in innate defense by attacking microbes directly or impeding their reproduction • Interferon proteins provide innate defense against viruses and help activate macrophages • About 30 proteins make up the complement system, which causes lysis of invading cells and helps trigger inflammation
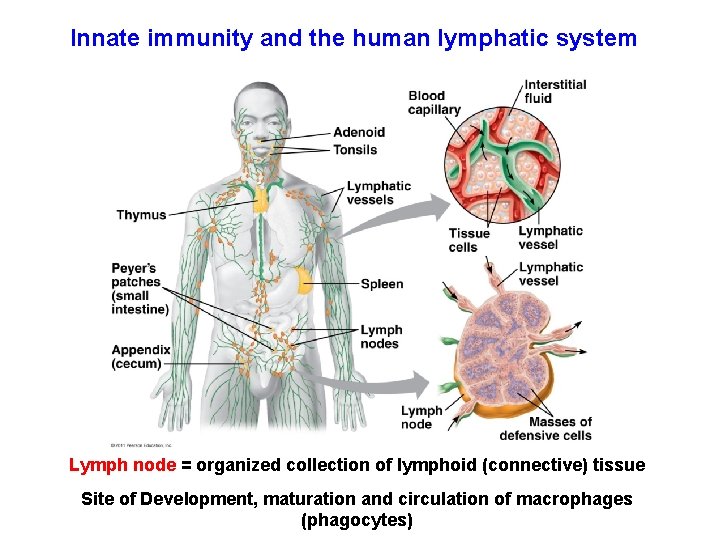
Innate immunity and the human lymphatic system Lymph node = organized collection of lymphoid (connective) tissue Site of Development, maturation and circulation of macrophages (phagocytes)
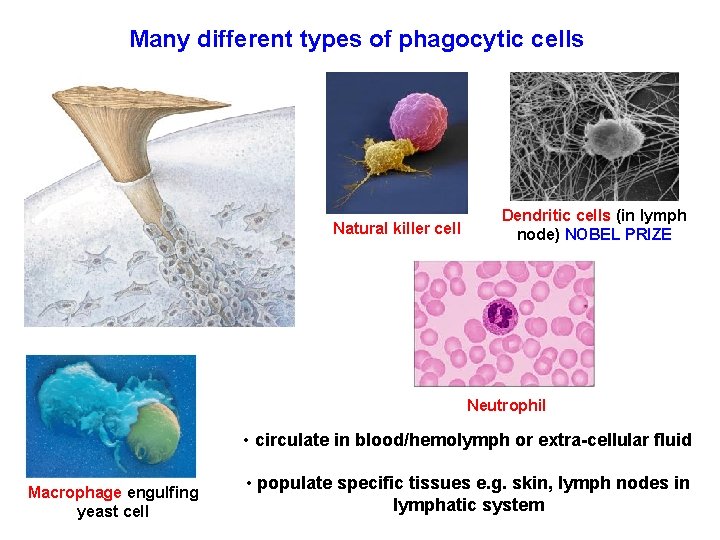
Many different types of phagocytic cells Natural killer cell Dendritic cells (in lymph node) NOBEL PRIZE Neutrophil • circulate in blood/hemolymph or extra-cellular fluid Macrophage engulfing yeast cell • populate specific tissues e. g. skin, lymph nodes in lymphatic system

Inflammatory Responses • Following an injury, mast cells release histamine, which promotes changes in blood vessels; this is part of the inflammatory response • These changes increase local blood supply and allow more phagocytes and antimicrobial proteins to enter tissues • Pus, a fluid rich in white blood cells, dead microbes, and cell debris, accumulates at the site of inflammation

• Inflammation can be either local or systemic (throughout the body) • Fever is a systemic inflammatory response triggered by pyrogens released by macrophages, and toxins from pathogens • Septic shock is a life-threatening condition caused by an overwhelming inflammatory response
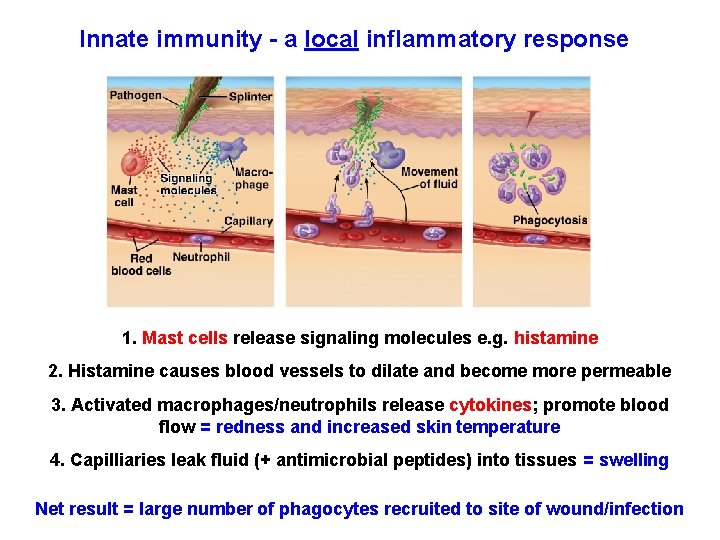
Innate immunity - a local inflammatory response 1. Mast cells release signaling molecules e. g. histamine 2. Histamine causes blood vessels to dilate and become more permeable 3. Activated macrophages/neutrophils release cytokines; promote blood flow = redness and increased skin temperature 4. Capilliaries leak fluid (+ antimicrobial peptides) into tissues = swelling Net result = large number of phagocytes recruited to site of wound/infection

Innate immunity: fever is a systemic (not localised) inflammatory response Substances released by activated macrophages in response to pathogens cause the bodies’ thermostat to reset to a higher temperature Humans 37°C - 41°C Lobster 16°C - 21°C Large-mouth bass 29°C - 32°C Leech 21°C - 30°C Fever might be positive if it enhances phagocytosis or speeds up reactions to accelerate tissue repair – body’s natural response to infection!

Innate immunity: Ectotherms can respond to pathogens with a fever using behavioural thermoregulation Increased body temperature Infection 39°C to 43°C Bacterial pathogen Desert iguana (Diposaurus) Is fever adaptive? Higher temperatures decrease growth rates of some pathogens

Natural Killer Cells • All cells in the body (except red blood cells) have a class 1 MHC: (Major histocompatibility complex (MHC) is a cell surface molecule encoded by a large gene family in all vertebrates. ) • Cancerous or infected cells no longer express this protein (MHC); natural killer (NK) cells attack these damaged cells

Innate Immune System Evasion by Pathogens • Some pathogens avoid destruction by modifying their surface to prevent recognition or by resisting breakdown following phagocytosis • Tuberculosis (TB) is one such disease and kills more than a million people a year

Overview of animal immunity Innate immunity - animals/plants - rapid - small # receptors Adaptive immunity - vertebrates only - slower - vast # receptors

Adaptive immunity: only in vertebrates Animals produce vast number and diversity of receptors: each recognising a small part of pathogen molecule (antigen) = very specific “Adaptive” because immune response is enhanced by previous exposure to pathogen = “immunological memory” Relies on B- and T-cells (lymphocytes, a type of white blood cell) Antigen receptors B cells develop and mature in bone marrow (from stem cells) T cells develop in bone marrow but move to, and mature in, thymus gland (see Fig. 43. 7) Up to 100, 000 antigen receptors on each single B or T cell (all recognise same antigen) B cell BUT millions of different types of antigen receptors on different cells
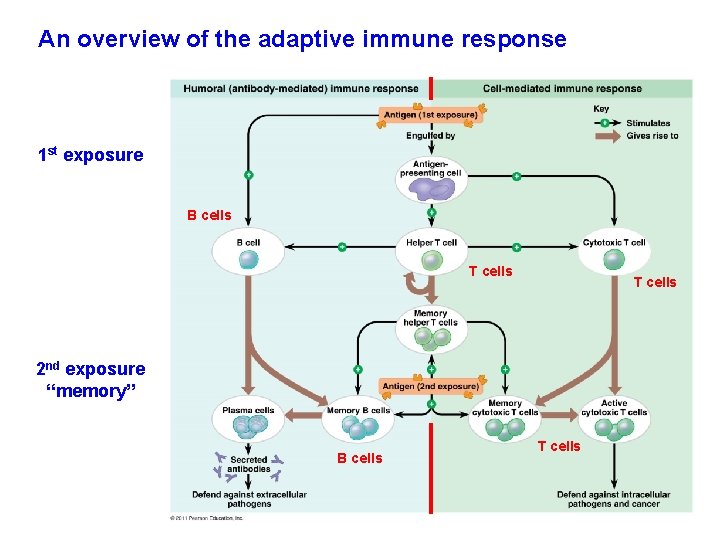
An overview of the adaptive immune response 1 st exposure B cells T cells 2 nd exposure “memory” B cells T cells

In acquired immunity, lymphocyte receptors provide pathogen-specific recognition • White blood cells called lymphocytes recognize and respond to antigens, foreign molecules • Lymphocytes that mature in the thymus above the heart are called T cells, and those that mature in bone marrow are called B cells
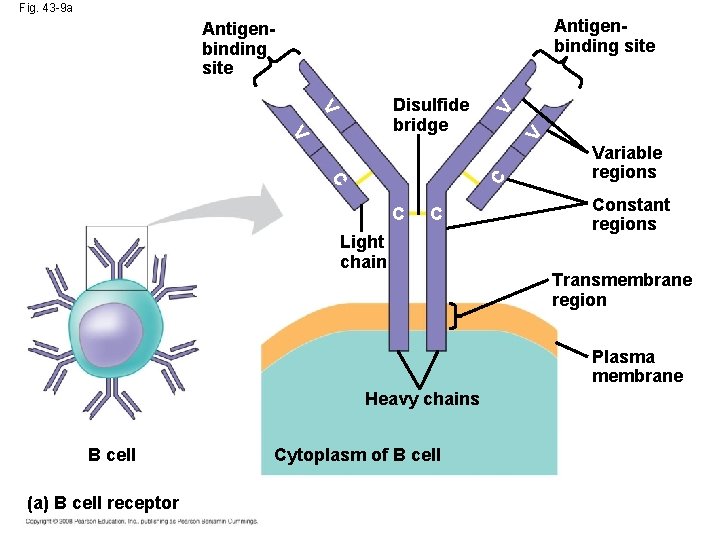
Fig. 43 -9 a Antigenbinding site C C V V V Disulfide bridge V Antigenbinding site C C Light chain Variable regions Constant regions Transmembrane region Plasma membrane Heavy chains B cell (a) B cell receptor Cytoplasm of B cell
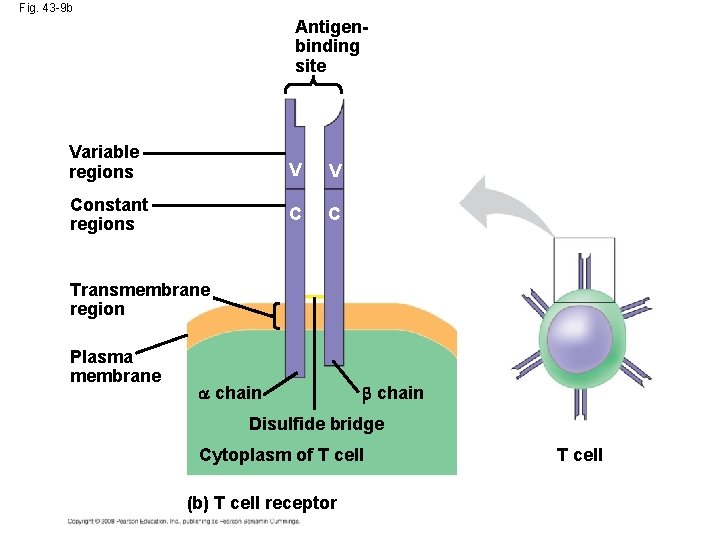
Fig. 43 -9 b Antigenbinding site Variable regions V V Constant regions C C Transmembrane region Plasma membrane chain Disulfide bridge Cytoplasm of T cell (b) T cell receptor T cell
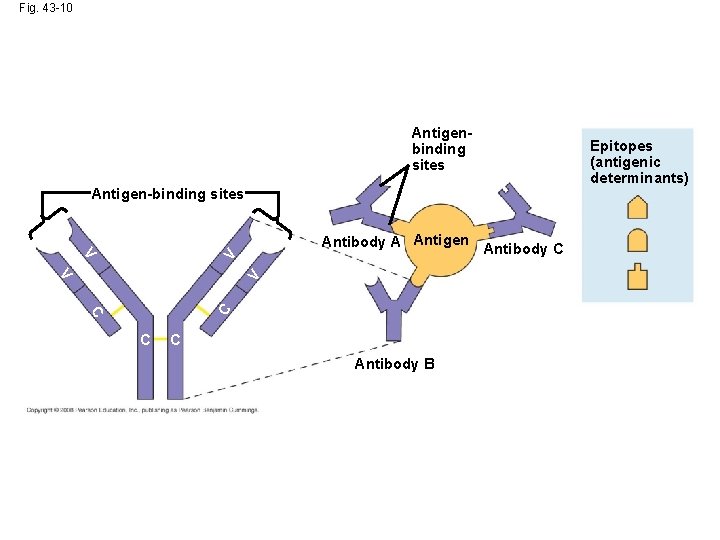
Fig. 43 -10 Antigenbinding sites Antigen-binding sites V V Antibody A Antigen Antibody C C C V V C C Antibody B Epitopes (antigenic determinants)

Acquired immunity defends against infection of body cells and fluids • Acquired immunity has two branches: the humoral immune response and the cell-mediated immune response • Humoral immune response involves activation and clonal selection of B cells, resulting in production of secreted antibodies • Cell-mediated immune response involves activation and clonal selection of cytotoxic T cells • Helper T cells aid both responses

• Lymphocytes contribute to immunological memory, an enhanced response to a foreign molecule encountered previously • Cytokines are secreted by macrophages and dendritic cells to recruit and activate lymphocytes
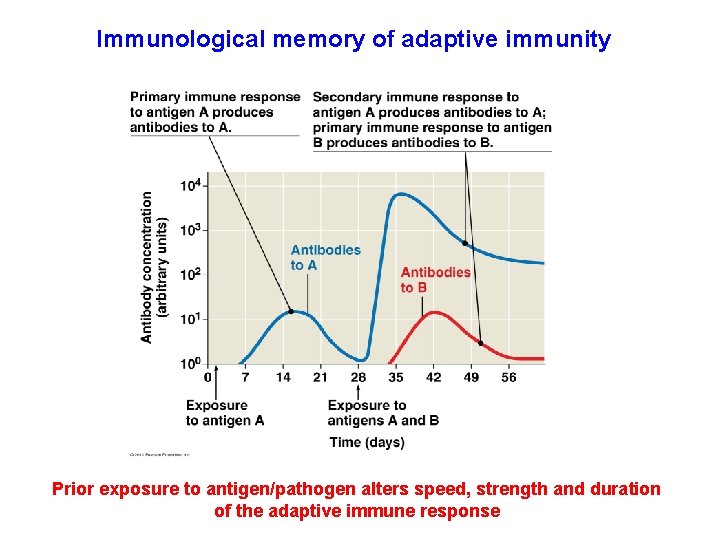
Immunological memory of adaptive immunity Prior exposure to antigen/pathogen alters speed, strength and duration of the adaptive immune response
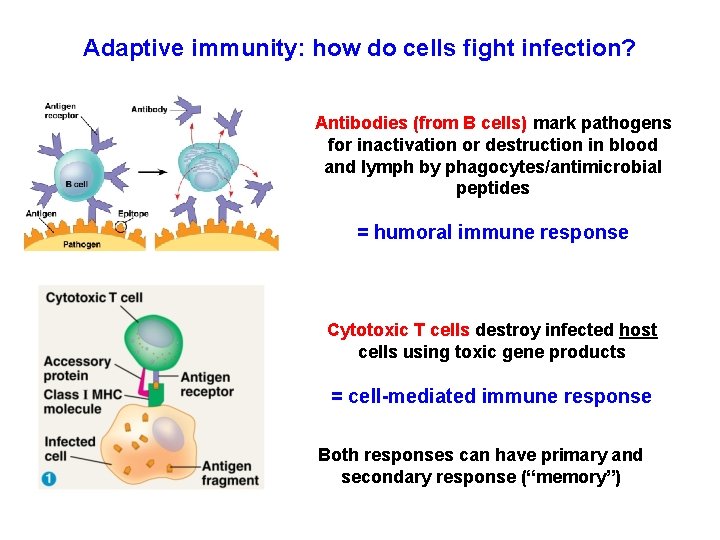
Adaptive immunity: how do cells fight infection? Antibodies (from B cells) mark pathogens for inactivation or destruction in blood and lymph by phagocytes/antimicrobial peptides = humoral immune response Cytotoxic T cells destroy infected host cells using toxic gene products = cell-mediated immune response Both responses can have primary and secondary response (“memory”)
Immunisation – manipulating the adaptive immune system Immunisation introduces antigens into the body - induces primary immune response and immunological memory - subsequent encounter with pathogen triggers rapid and stronger secondary response Less than one in a million children has allergic reaction to immunisation Measles virus Measles kills 200, 000 people each year DO THE MATH!
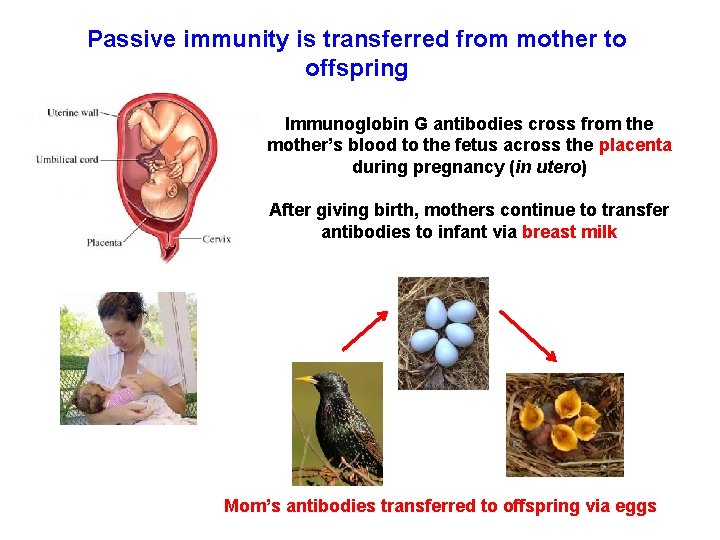
Passive immunity is transferred from mother to offspring Immunoglobin G antibodies cross from the mother’s blood to the fetus across the placenta during pregnancy (in utero) After giving birth, mothers continue to transfer antibodies to infant via breast milk Mom’s antibodies transferred to offspring via eggs

Antibody Classes • The five major classes of antibodies, or immunoglobulins, differ in distribution and function • Polyclonal antibodies are the products of many different clones of B cells following exposure to a microbial antigen • Monoclonal antibodies are prepared from a single clone of B cells grown in culture
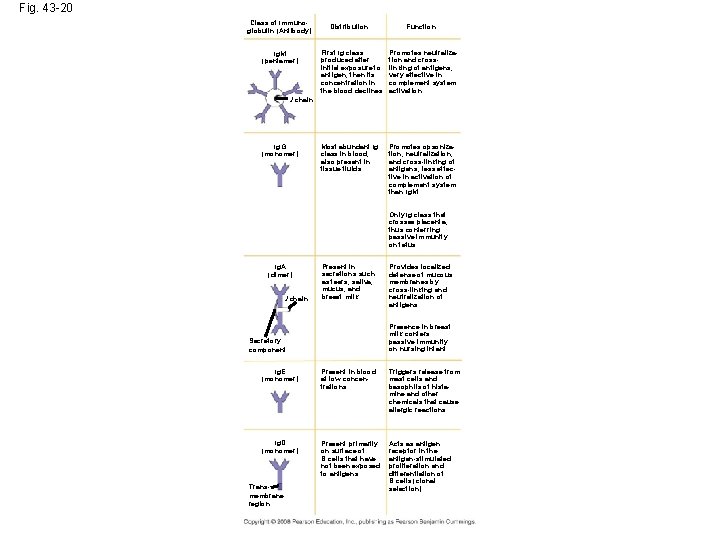
Fig. 43 -20 Class of Immunoglobulin (Antibody) Ig. M (pentamer) Distribution Function First Ig class produced after initial exposure to antigen; then its concentration in the blood declines Promotes neutralization and crosslinking of antigens; very effective in complement system activation Most abundant Ig class in blood; also present in tissue fluids Promotes opsonization, neutralization, and cross-linking of antigens; less effective in activation of complement system than Ig. M J chain Ig. G (monomer) Only Ig class that crosses placenta, thus conferring passive immunity on fetus Ig. A (dimer) J chain Present in secretions such as tears, saliva, mucus, and breast milk Provides localized defense of mucous membranes by cross-linking and neutralization of antigens Presence in breast milk confers passive immunity on nursing infant Secretory component Ig. E (monomer) Present in blood at low concentrations Triggers release from mast cells and basophils of histamine and other chemicals that cause allergic reactions Ig. D (monomer) Present primarily on surface of B cells that have not been exposed to antigens Acts as antigen receptor in the antigen-stimulated proliferation and differentiation of B cells (clonal selection) Transmembrane region
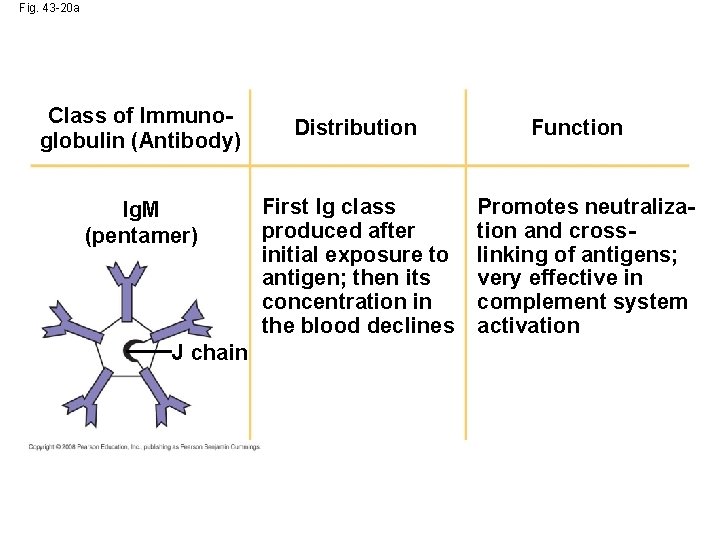
Fig. 43 -20 a Class of Immunoglobulin (Antibody) Ig. M (pentamer) J chain Distribution First Ig class produced after initial exposure to antigen; then its concentration in the blood declines Function Promotes neutralization and crosslinking of antigens; very effective in complement system activation
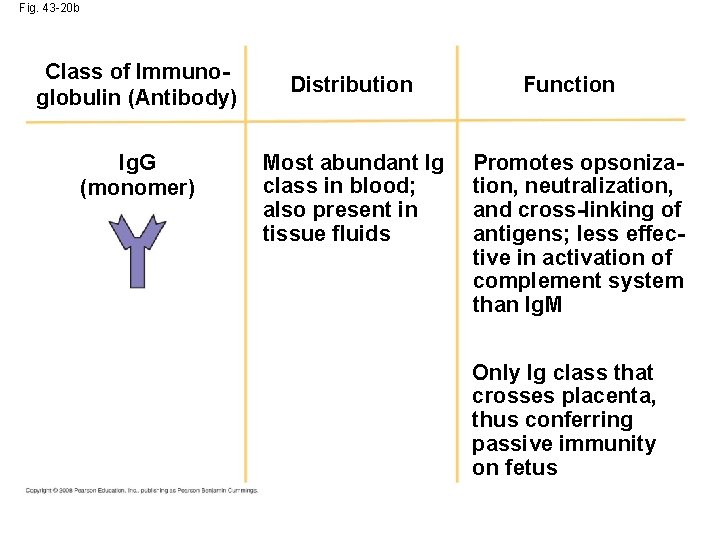
Fig. 43 -20 b Class of Immunoglobulin (Antibody) Ig. G (monomer) Distribution Most abundant Ig class in blood; also present in tissue fluids Function Promotes opsonization, neutralization, and cross-linking of antigens; less effective in activation of complement system than Ig. M Only Ig class that crosses placenta, thus conferring passive immunity on fetus
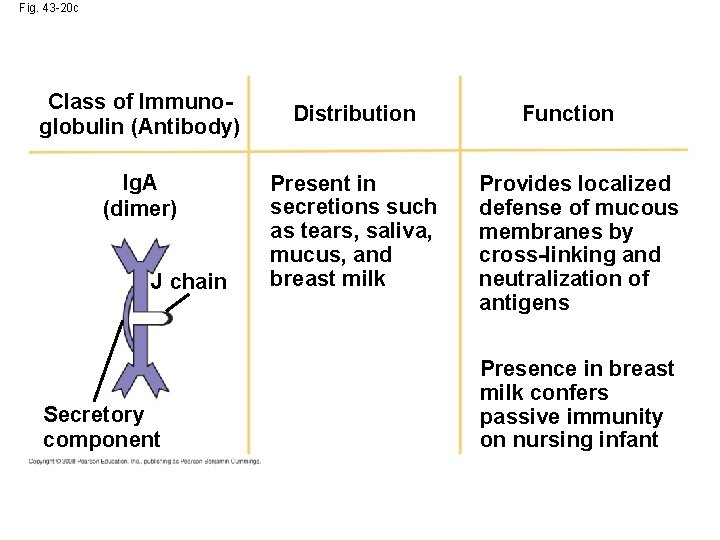
Fig. 43 -20 c Class of Immunoglobulin (Antibody) Ig. A (dimer) J chain Secretory component Distribution Present in secretions such as tears, saliva, mucus, and breast milk Function Provides localized defense of mucous membranes by cross-linking and neutralization of antigens Presence in breast milk confers passive immunity on nursing infant
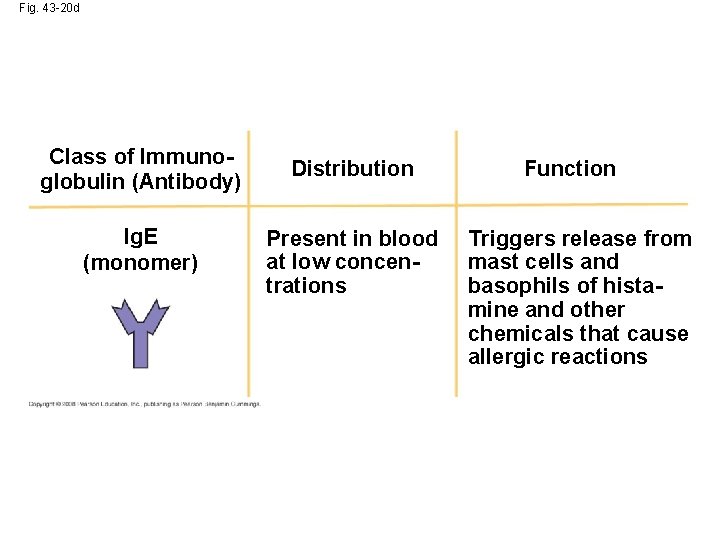
Fig. 43 -20 d Class of Immunoglobulin (Antibody) Ig. E (monomer) Distribution Present in blood at low concentrations Function Triggers release from mast cells and basophils of histamine and other chemicals that cause allergic reactions
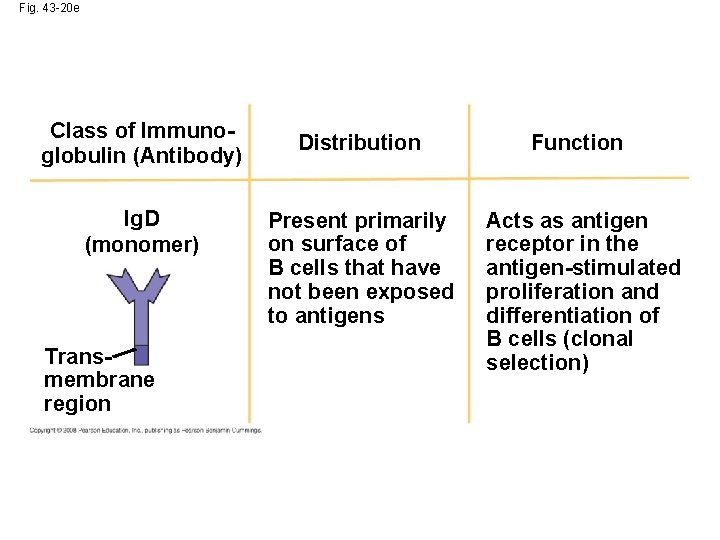
Fig. 43 -20 e Class of Immunoglobulin (Antibody) Ig. D (monomer) Transmembrane region Distribution Present primarily on surface of B cells that have not been exposed to antigens Function Acts as antigen receptor in the antigen-stimulated proliferation and differentiation of B cells (clonal selection)

The Role of Antibodies in Immunity • Neutralization occurs when a pathogen can no longer infect a host because it is bound to an antibody • Opsonization occurs when antibodies bound to antigens increase phagocytosis • Antibodies together with proteins of the complement system generate a membrane attack complex and cell lysis
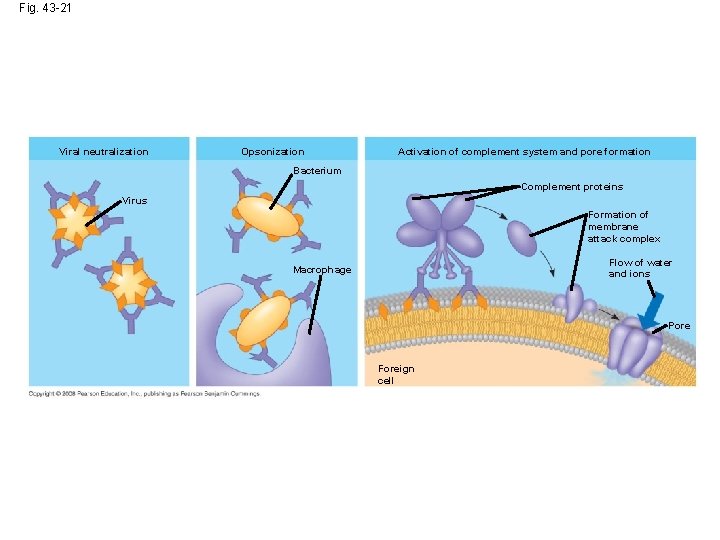
Fig. 43 -21 Viral neutralization Opsonization Activation of complement system and pore formation Bacterium Complement proteins Virus Formation of membrane attack complex Flow of water and ions Macrophage Pore Foreign cell

Immune Rejection • Cells transferred from one person to another can be attacked by immune defenses • This complicates blood transfusions or the transplant of tissues or organs

Blood Groups • Antigens on red blood cells determine whether a person has blood type A (A antigen), B (B antigen), AB (both A and B antigens), or O (neither antigen) • Antibodies to nonself blood types exist in the body • Transfusion with incompatible blood leads to destruction of the transfused cells • Recipient-donor combinations can be fatal or safe

Tissue and Organ Transplants • MHC molecules are different among genetically nonidentical individuals • Differences in MHC molecules stimulate rejection of tissue grafts and organ transplants • Chances of successful transplantation increase if donor and recipient MHC tissue types are well matched • Immunosuppressive drugs facilitate transplantation • Lymphocytes in bone marrow transplants may cause the donor tissue to reject the recipient

Allergies • Allergies are exaggerated (hypersensitive) responses to antigens called allergens • In localized allergies such as hay fever, Ig. E antibodies produced after first exposure to an allergen attach to receptors on mast cells
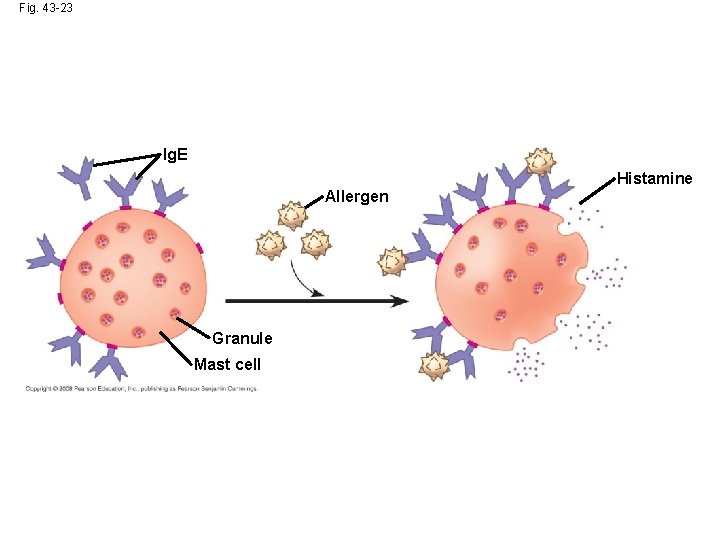
Fig. 43 -23 Ig. E Allergen Granule Mast cell Histamine

• The next time the allergen enters the body, it binds to mast cell–associated Ig. E molecules • Mast cells release histamine and other mediators that cause vascular changes leading to typical allergy symptoms • An acute allergic response can lead to anaphylactic shock, a life-threatening reaction that can occur within seconds of allergen exposure

Autoimmune Diseases • In individuals with autoimmune diseases, the immune system loses tolerance for self and turns against certain molecules of the body • Autoimmune diseases include systemic lupus erythematosus, rheumatoid arthritis, insulindependent diabetes mellitus, and multiple sclerosis
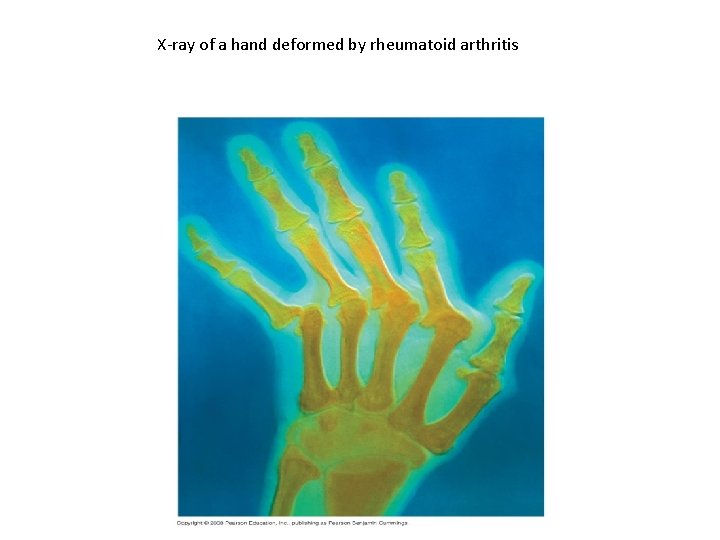
X-ray of a hand deformed by rheumatoid arthritis

Immunodeficiency Diseases • Inborn immunodeficiency results from hereditary or developmental defects that prevent proper functioning of innate, humoral, and/or cellmediated defenses • Acquired immunodeficiency results from exposure to chemical and biological agents • Acquired immunodeficiency syndrome (AIDS) is caused by a virus

Antigenic Variation • Through antigenic variation, some pathogens are able to change epitope expression and prevent recognition • The human influenza virus mutates rapidly, and new flu vaccines must be made each year • Human viruses occasionally exchange genes with the viruses of domesticated animals • This poses a danger as human immune systems are unable to recognize the new viral strain

Latency • Some viruses may remain in a host in an inactive state called latency • Herpes simplex viruses can be present in a human host without causing symptoms

Attack on the Immune System: HIV • Human immunodeficiency virus (HIV) infects helper T cells • The loss of helper T cells impairs both the humoral and cell-mediated immune responses and leads to AIDS • HIV eludes the immune system because of antigenic variation and an ability to remain latent while integrated into host DNA

• People with AIDS are highly susceptible to opportunistic infections and cancers that take advantage of an immune system in collapse • The spread of HIV is a worldwide problem • The best approach for slowing this spread is education about practices that transmit the virus

Cancer and Immunity • The frequency of certain cancers increases when the immune response is impaired • Two suggested explanations are – Immune system normally suppresses cancerous cells – Increased inflammation increases the risk of cancer
- Slides: 55