Biochemical Tests 1111 1112 Na 133 137 K


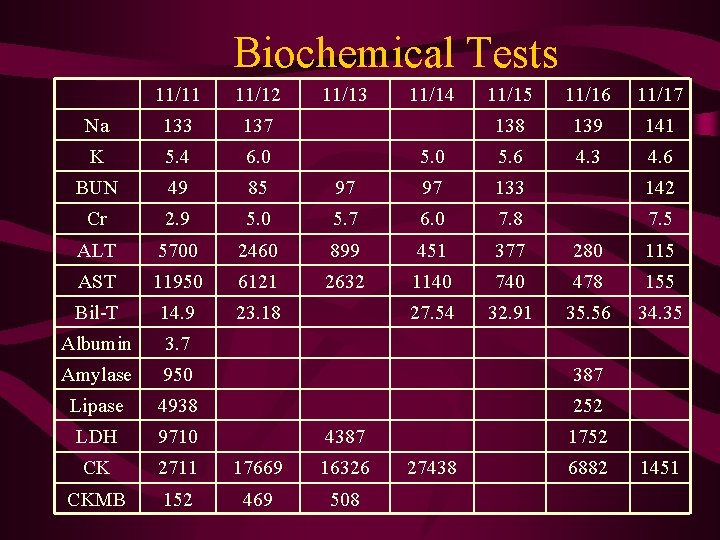
Biochemical Tests 11/11 11/12 Na 133 137 K 5. 4 6. 0 BUN 49 85 Cr 2. 9 ALT 11/13 11/14 11/15 11/16 11/17 138 139 141 5. 0 5. 6 4. 3 4. 6 97 97 133 142 5. 0 5. 7 6. 0 7. 8 7. 5 5700 2460 899 451 377 280 115 AST 11950 6121 2632 1140 740 478 155 Bil-T 14. 9 23. 18 27. 54 32. 91 35. 56 34. 35 Albumin 3. 7 Amylase 950 387 Lipase 4938 252 LDH 9710 CK 2711 17669 16326 CKMB 152 469 508 4387 1752 27438 6882 1451
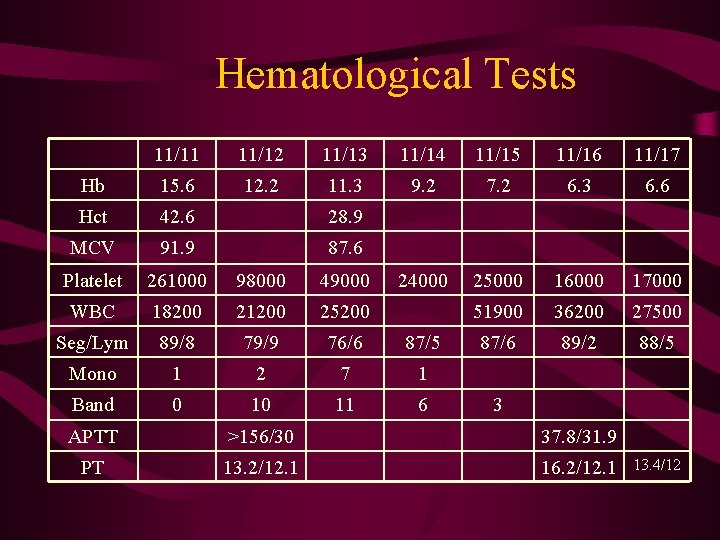
Hematological Tests 11/11 11/12 11/13 11/14 11/15 11/16 11/17 Hb 15. 6 12. 2 11. 3 9. 2 7. 2 6. 3 6. 6 Hct 42. 6 28. 9 MCV 91. 9 87. 6 Platelet 261000 98000 49000 24000 25000 16000 17000 WBC 18200 21200 25200 51900 36200 27500 Seg/Lym 89/8 79/9 76/6 87/5 87/6 89/2 88/5 Mono 1 2 7 1 Band 0 10 11 6 3 APTT >156/30 37. 8/31. 9 PT 13. 2/12. 1 16. 2/12. 1 13. 4/12

Active Problem • Acute renal failure • Acute hepatic failure • Acute pancreatitis • Acute hemolysis • Rhabdomyolysis • DIC
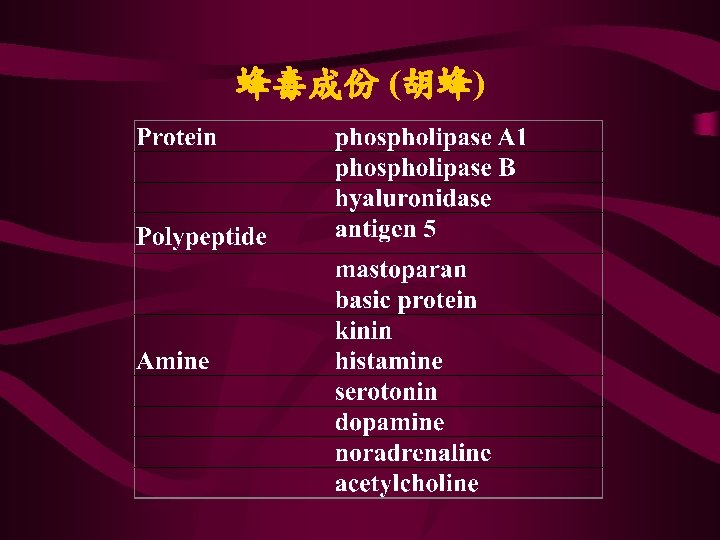


Toxicological Mechanism • Phospholipase A 2 - hemolysin • Mast cell degranulating peptides- exist in honeybee venom (MCD peptide) and in vespid venom (mastoparan) • Hyaluronidase - disruption of the hyaluronic acid connective tissue matrix, allowing for spread of venom into tissue.

Toxicological Mechanism Melittin (honeybee) • local pain, alters membrane integrity • cell surface-active agent direct hemolysin, platelets aggregation Apamin (honeybee) • profound effect on spinal cord function, causing hyperactivity, muscle spasms and seizures


Mechanism of Hypersensitivity • Antigenic substance: phospholipase、 hyaluronidase、acid phosphatase (honeybee) 或 phospholipase A & B、hyaluronidase、 antigen 5 (wasp). • Ig. E-medicated, sensitization (several days) • Late-onset allergic reaction: Ig. G and Ig Emedicated, onset several hours to 10 days

Natural Immunity • When natural immunity to Hymenoptera venom develops, it is usually due to the development of large amounts of Ig. G antibodies which block the combination of venom antigen with Ig. E and prevents or lessens immunologic response


Clinical Manifestations

CLINICAL EFFECTS • Nonallergic Local Reaction • Toxic Reaction • Hypersensitivity (Local, Systemic) • Late-onset allergic reactions

Nonallergic Local Reaction • wheal, pain, irritation, itching, and redness • Symptoms generally resolve within a few hours. • Stings in the mouth or throat may be especially dangerous because local edema may cause respiratory obstruction. • Not Ig. E-mediated, a response to toxic and inflammatory venom components such as vasoactive amines and peptides.

Toxic Reaction • Multiple stings (eg, more than 50 wasp stings) • S/S: edema, fatigue, vomiting, diarrhea, headache, hypotension, seizures, unconsciousness, and renal failure. • Delayed toxic reactions are rare, but do occur: hemolysis, coagulopathy, thrombocytopenia, rhabdomyolysis, liver dysfunction, and disseminated intravascular coagulation.

Hypersensitivity • Not dose-dependent • Risk factor: 1. short interval (less than 2 months) between the innocuous sting and the successive sting. 2. stings on the head and neck • Atopy does not increase the incidence of anaphylactic reaction although asthmatic patients have more severe reactions to stings than nonatopic patients

Hypersensitivity Local allergic reaction • Extensive local swelling, often exceeding 10 cm, may persist for several days. • Large local reactions do not predict progression to systemic reactions. • The risk of eventual anaphylaxis in such individuals is only 5% to 10%, despite the presence of venom-specific Ig. E.

Hypersensitivity • Systemic allergic reactions: may occur within 30 minutes of a sting • S/S: cutaneous (generalized urticaria, erythema, pruritus, and angioedema), respiratory (edema of the tongue, epiglottis, and larynx; bronchial constriction causing dyspnea, stridor, dysphagia, or wheezing), and/or vascular symptoms (cardiovascular collapse, hypotension, and loss of consciousness). • The cause of death is usually respiratory obstruction, cardiovascular collapse, or both.

Hypersensitivity Systemic allergic reactions • Individuals who have had an anaphylactic reaction to an Hymenoptera sting have a 35% to 60% chance of developing anaphylaxis from subsequent stings by an identical insect.

Late-onset Allergic Reactions • Occur several hours to as long as 10 days after a sting • Range from typical anaphylactic and serum sickness-like reactions: local swelling, urticaria, throat edema, generalized rash, fever, lymphadenopathy, swelling, and arthralgia. • These effects may be mediated by venomspecific Ig. G and venom-specific Ig. E

CLINICAL EFFECTS Drug interaction • NSAID may increase sensitivity to bee stings • Beta-blockers may increase the severity and duration of the anaphylactic response and interfere with the treatment and recovery from anaphylaxis because of their effect on beta-adrenergic receptors in the respiratory and cardiovascular systems • Calcium channel blockers - recurrent severe anaphylactic responses (triphasic)

CLINICAL EFFECTS Idiosyncratic reaction • stress-induced myocardial infarctions in the elderly; • delayed neurologic reactions • reactions associated with unusual sting sites, such as the uvula and cornea.















- Slides: 40