Bioabsorbable Stent Unsolved Issues Cahallenges in Japan Takashi

Bioabsorbable Stent: Unsolved Issues & Cahallenges in Japan Takashi Akasaka, MD, Ph. D, FESC Department of Cardiovascular Medicine Wakayama Medical University, Japan

Disclosure Statement of Financial Interest Takashi Akasaka, MD, Ph. D Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation with the organization(s) listed below. • Grant/Research Support : Abbott Vascular Japan Boston Scientific Japan Goodman Inc. St. Jude Medical Japan Terumo Inc. • Consulting Fees/Honoraria : Daiichi-Sankyo Pharmaceutical Inc. Goodman Inc. St. Jude Medical Japan Terumo Inc.


Backgrounds Ø Theoretically, bioresorbable vascular scaffolds (BVS) may overcome the shortcomings of permanent metallic prosthesis. Ø However, whether BVS are as safe and effective as metallic DES prior to complete bioresorption is currently unknown. Aim Therefore, a randomized, controlled trial comparing the clinical and angiographic outcomes of BVS with those of Xience cobalt-chromium everolimus-eluting stents (Co. Cr-EES) was designed to support regulatory approval of the Absorb BVS in Japan.

ABSORB Japan Prospective, randomized, active control, single-blind, non-inferiority, multi-center Japanese study Inclusion: Patients with up to 2 de novo target lesions in separate native coronary arteries Lesion length ≤ 24 mm, Dmax ≥ 2. 5 mm to ≤ 3. 75 mm, %DS ≥ 50% to <100% Exclusion: AMI, EF <30%, e. GFR <30 m. L/min/1. 73 m 2, LMCA, Ostial lesion, Excessive vessel tortuosity, Heavy calcification, Myocardial bridge, Bifurcation with side branch ≥ 2 mm Randomized 2: 1 BVS Co. Cr-EES Tx. with single study device Diameter: 2. 5, 3. 0. 3. 5 mm Length: 8, 12, 18, 28 mm Primary Clinical Endpoint: Target Lesion Failure (TLF): Cardiac death, TV-MI, Ischemia Driven-TLR at 12 months Major Secondary Angiographic Endpoint: In-segment Late Lumen Loss at 13 months

Sample Size Calculation & 12 -Month TLF (ABSORB Japan) • • Randomization ratio: 2 to 1 Non-inferiority study design Significance level: 5% (one tail) Assumed event rate of 12 -month TLF in the Co. Cr-EES arm: 9% Non-inferiority Margin: 8. 6% Power: 90% Required Sample Size: 390 patients (BVS: 260, Co. Cr-EES: 130) Total Sample Size: 400 patients assuming dropouts If the non-inferiority P-value from the one-sided Farrington-Manning test is <0. 05, BVS is regarded as non-inferior to Co. Cr-EES for the primary endpoint. True rate was based on results from SPIRIT III RCT and SPIRIT III Japan, and 95% UCI was applied. Non-inferiority margin was ½ of treatment effect of Co. Cr-EES over BMS, i. e. (1 st Gen DES – BMS) + (Co. Cr-EES – 1 st Gen DES)

Investigational Sites (38) • • • • • Shin-Tokyo Hospital, Chiba Saitama Sekishinkai Hospital, Saitama Saiseikai Yokohamashi Tobu Hospital, Kanagawa Shonan Kamakura General Hospital, Kanagawa The Cardiovascular Institute, Tokyo Women's Medical University Hospital, Tokyo Kurashiki Central Hospital, Okayama Kansai Rosai Hospital, Hyogo Shinkoga Hospital, Fukuoka Iwate Medical University Hospital, Iwate Sakakibara Heart Institute, Tokyo Kyoto University Hospital, Kyoto Saiseikai Kumamoto Hospital, Kumamoto Osaka University Hospital, Osaka Tokushima Red Cross Hospital, Tokushima Miyazaki Medical Association Hospital, Miyazaki Teikyo University Hospital, Tokyo Fujita Health University Hospital, Aichi Kanto Rosai Hospital, Kanagawa • • • • • National Cerebral and Cardiovascular Center, Osaka Kurume University Hospital, Fukuoka Kokura Memorial Hospital, Fukuoka Hokkaido Social Insurance Hospital, Hokkaido Showa University Hospital, Tokyo Sakurabashi Watanabe Hospital, Osaka Yamaguchi University Hospital, Yamaguchi Mitsui Memorial Hospital, Tokyo The University of Tokyo Hospital, Tokyo Tokai University Hospital, Kanagawa Japanese Red Cross Nagoya Daini Hospital, Aichi Tenri Hospital, Nara Toho University Ohashi Medical Center, Tokyo Kobe University Hospital, Hyogo Saitama Medical Center Jichi Medical University, Saitama Dokkyo Medical University Hospital, Tochigi Juntendo University Hospital, Tokyo Wakayama Medical University Hospital, Wakayama Tsukuba Medical Center Hospital, Ibaraki

ABSORB Japan Study Organization Study Protocol Committee: Takeshi Kimura (Principal Investigator), Ken Kozuma, and Kengo Tanabe Data management: Abbott Vascular Safety Oversight Committee: Harvard Clinical Research Institute (HCRI) Clinical Events Committee: Harvard Clinical Research Institute (HCRI) Angiographic Core laboratory: Beth Israel Deaconess Medical Center, Inc. , Angiographic Core Lab, IVUS Core laboratory: Cardiovascular Core Analysis Laboratory (CCAL), Stanford University OCT Core laboratory: Cardialysis BV, Rotterdam, the Netherlands MSCT Core laboratory: Cardiocore Japan
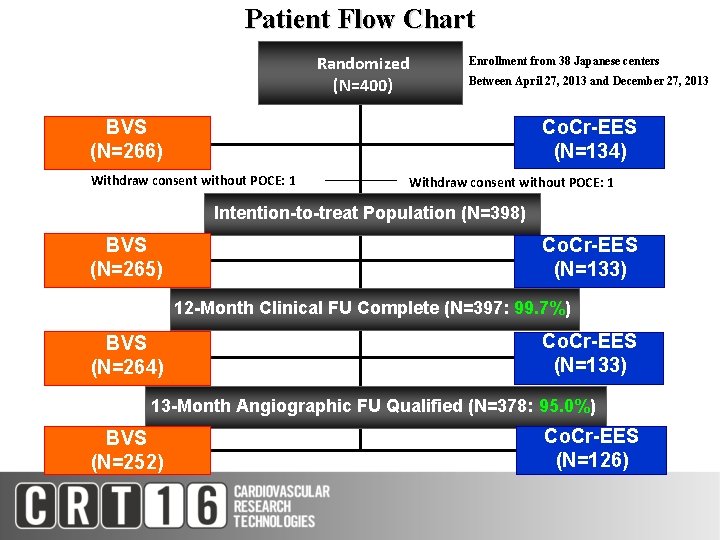
Patient Flow Chart Randomized (N=400) Enrollment from 38 Japanese centers Between April 27, 2013 and December 27, 2013 Co. Cr-EES (N=134) BVS (N=266) Withdraw consent without POCE: 1 BES (N=1617) BVS (N=265) BVS BES (N=263) Withdraw consent without POCE: 1 Intention-to-treat Population (N=398) EES (N=1618) Co. Cr-EES (N=133) (N=266) 12 -Month Clinical FU Complete (N=397: ) 99. 7%) BES Co. Cr-EES BVS (N=133) (N=1601) (N=264) 13 -Month Angiographic FU Qualified (N=378: 95. 0%) BVS (N=252) Co. Cr-EES (N=126)
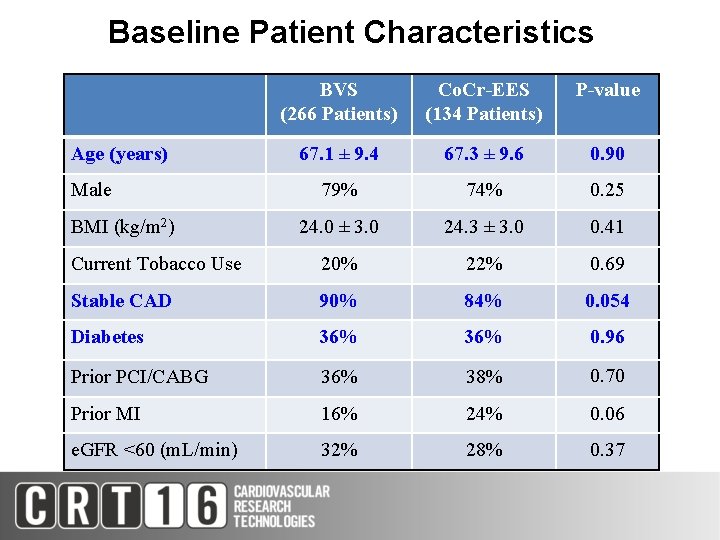
Baseline Patient Characteristics BVS (266 Patients) Co. Cr-EES (134 Patients) P-value 67. 1 ± 9. 4 67. 3 ± 9. 6 0. 90 79% 74% 0. 25 24. 0 ± 3. 0 24. 3 ± 3. 0 0. 41 Current Tobacco Use 20% 22% 0. 69 Stable CAD 90% 84% 0. 054 Diabetes 36% 0. 96 Prior PCI/CABG 36% 38% 0. 70 Prior MI 16% 24% 0. 06 e. GFR <60 (m. L/min) 32% 28% 0. 37 Age (years) Male BMI (kg/m 2)
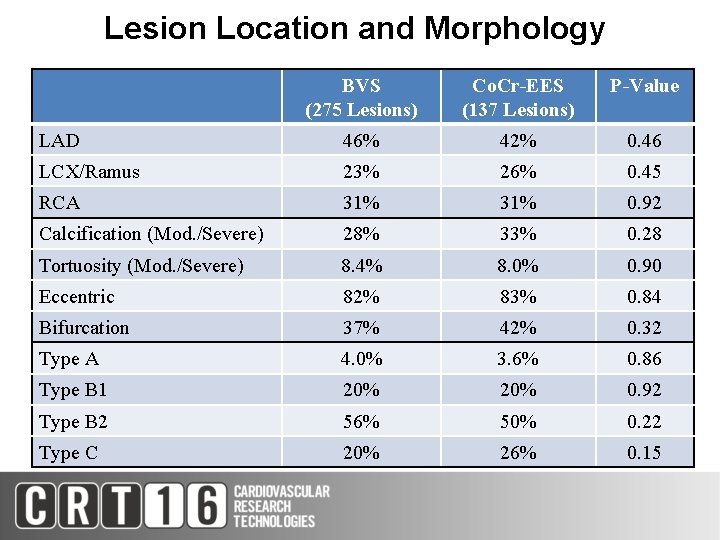
Lesion Location and Morphology BVS (275 Lesions) Co. Cr-EES (137 Lesions) P-Value LAD 46% 42% 0. 46 LCX/Ramus 23% 26% 0. 45 RCA 31% 0. 92 Calcification (Mod. /Severe) 28% 33% 0. 28 Tortuosity (Mod. /Severe) 8. 4% 8. 0% 0. 90 Eccentric 82% 83% 0. 84 Bifurcation 37% 42% 0. 32 Type A 4. 0% 3. 6% 0. 86 Type B 1 20% 0. 92 Type B 2 56% 50% 0. 22 Type C 20% 26% 0. 15
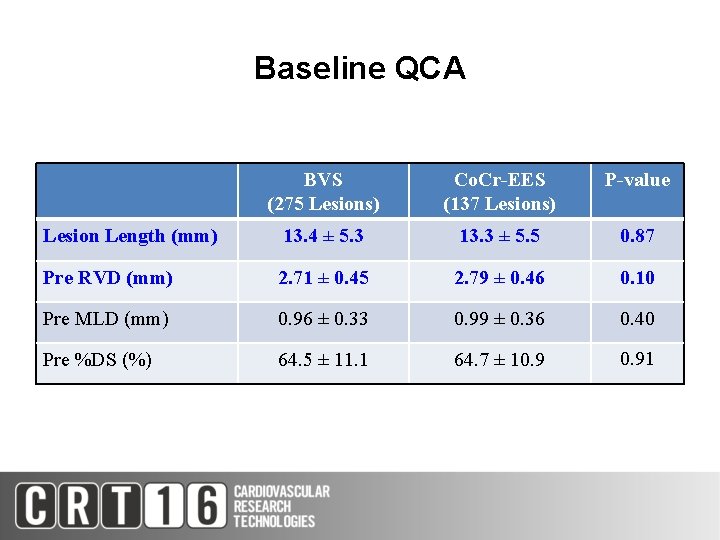
Baseline QCA BVS (275 Lesions) Co. Cr-EES (137 Lesions) P-value Lesion Length (mm) 13. 4 ± 5. 3 13. 3 ± 5. 5 0. 87 Pre RVD (mm) 2. 71 ± 0. 45 2. 79 ± 0. 46 0. 10 Pre MLD (mm) 0. 96 ± 0. 33 0. 99 ± 0. 36 0. 40 Pre %DS (%) 64. 5 ± 11. 1 64. 7 ± 10. 91
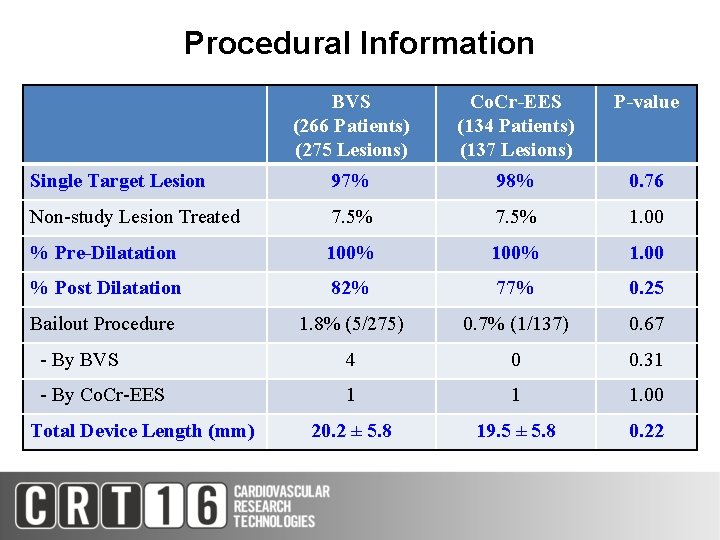
Procedural Information BVS (266 Patients) (275 Lesions) Co. Cr-EES (134 Patients) (137 Lesions) P-value Single Target Lesion 97% 98% 0. 76 Non-study Lesion Treated 7. 5% 1. 00 % Pre-Dilatation 100% 1. 00 % Post Dilatation 82% 77% 0. 25 Bailout Procedure 1. 8% (5/275) 0. 7% (1/137) 0. 67 - By BVS 4 0 0. 31 - By Co. Cr-EES 1 1 1. 00 20. 2 ± 5. 8 19. 5 ± 5. 8 0. 22 Total Device Length (mm)
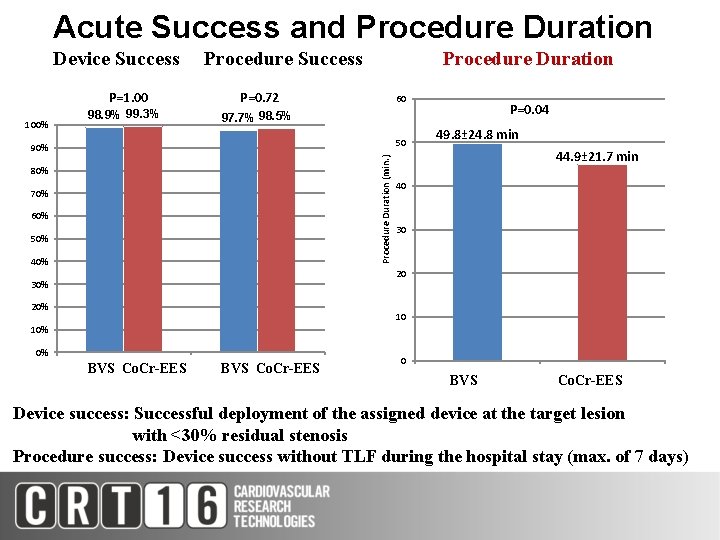
Acute Success and Procedure Duration Device Success Procedure Duration Acute Success P=1. 00 100% 98. 9% 99. 3% P=0. 72 60 Procedure Duration P=0. 04 97. 7% 98. 5% 50 Procedure Duration (min. ) 90% 80% 70% 60% 49. 8± 24. 8 min 44. 9± 21. 7 min 40 BVS 30 Co. Cr-EES 50% 40% 20 30% 20% 10 10% 0% Device Success BVS Co. Cr-EES Procedural Success BVS Co. Cr-EES 0 BVS Co. Cr-EES Device success: Successful deployment of the assigned device at the target lesion with <30% residual stenosis Procedure success: Device success without TLF during the hospital stay (max. of 7 days)
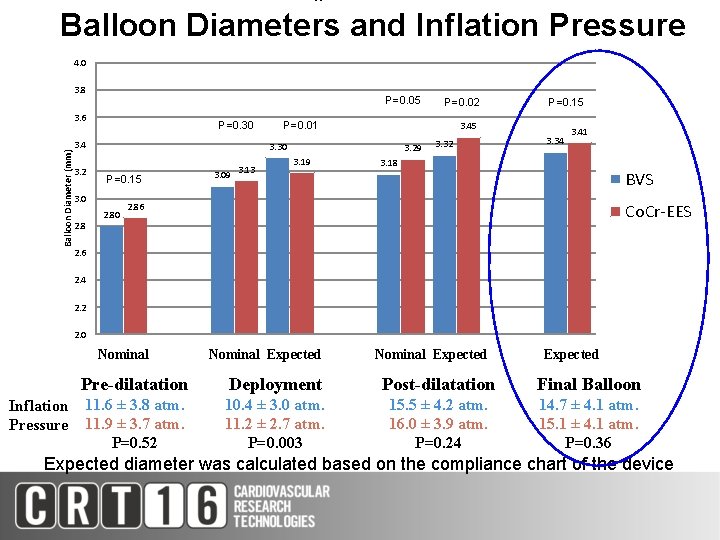
Balloon Diameters and Inflation Pressure 4. 0 3. 8 P=0. 05 Balloon Diameter (mm) 3. 6 P=0. 30 3. 4 3. 2 P=0. 15 3. 0 2. 8 P=0. 01 2. 80 3. 13 3. 29 3. 19 P=0. 15 3. 45 3. 30 3. 09 P=0. 02 3. 34 3. 41 3. 18 BVS 2. 86 Co. Cr-EES 2. 6 2. 4 2. 2 2. 0 Nominal Pre-dilatation Inflation Pressure Pre-dilatation 11. 6 ± 3. 8 atm. 11. 9 ± 3. 7 atm. P=0. 52 Nominal Expected Deployment 10. 4 ± 3. 0 atm. 11. 2 ± 2. 7 atm. P=0. 003 Nominal Expected Post-dilatation Final Balloon 16. 0 ± 3. 9 atm. P=0. 24 15. 1 ± 4. 1 atm. P=0. 36 Post-dilatation 15. 5 ± 4. 2 atm. Final 14. 7 ± 4. 1 atm. Expected diameter was calculated based on the compliance chart of the device
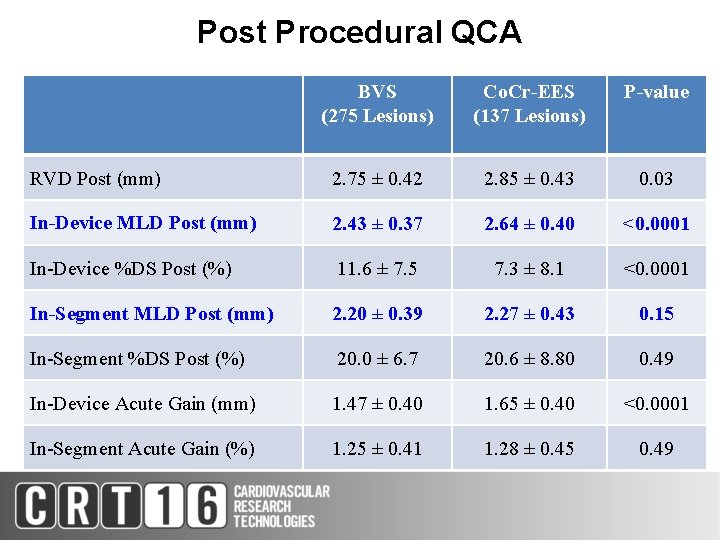
Post Procedural QCA BVS (275 Lesions) Co. Cr-EES (137 Lesions) P-value RVD Post (mm) 2. 75 ± 0. 42 2. 85 ± 0. 43 0. 03 In-Device MLD Post (mm) 2. 43 ± 0. 37 2. 64 ± 0. 40 <0. 0001 In-Device %DS Post (%) 11. 6 ± 7. 5 7. 3 ± 8. 1 <0. 0001 In-Segment MLD Post (mm) 2. 20 ± 0. 39 2. 27 ± 0. 43 0. 15 In-Segment %DS Post (%) 20. 0 ± 6. 7 20. 6 ± 8. 80 0. 49 In-Device Acute Gain (mm) 1. 47 ± 0. 40 1. 65 ± 0. 40 <0. 0001 In-Segment Acute Gain (%) 1. 25 ± 0. 41 1. 28 ± 0. 45 0. 49
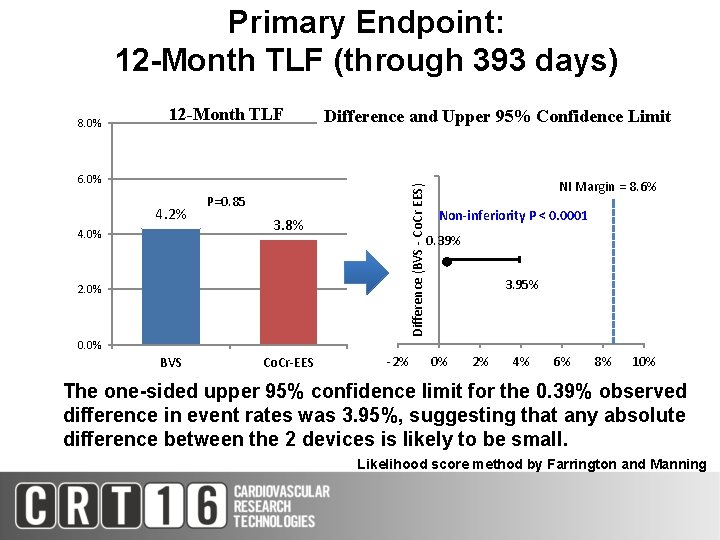
Primary Endpoint: 12 -Month TLF (through 393 days) 8. 0% 12 -Month TLF Difference and Upper 95% Confidence Limit 4. 2% 4. 0% Difference (BVS - Co. Cr EES) 6. 0% P=0. 85 3. 8% 2. 0% NI Margin = 8. 6% Non-inferiority P < 0. 0001 0. 39% ● 3. 95% 0. 0% BVS Co. Cr-EES -2% 0% 2% 4% 6% 8% 10% The one-sided upper 95% confidence limit for the 0. 39% observed difference in event rates was 3. 95%, suggesting that any absolute difference between the 2 devices is likely to be small. Likelihood score method by Farrington and Manning
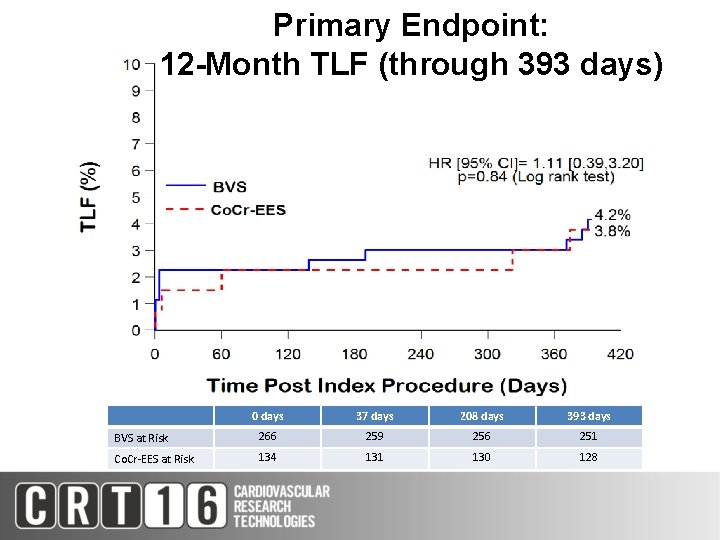
Primary Endpoint: 12 -Month TLF (through 393 days) 0 days 37 days 208 days 393 days BVS at Risk 266 259 256 251 Co. Cr-EES at Risk 134 131 130 128
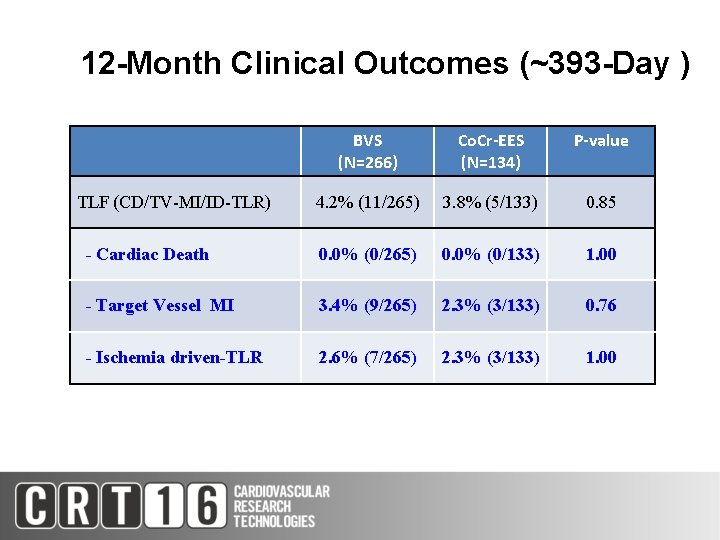
12 -Month Clinical Outcomes (~393 -Day ) BVS (N=266) Co. Cr-EES (N=134) P-value 4. 2% (11/265) 3. 8% (5/133) 0. 85 - Cardiac Death 0. 0% (0/265) 0. 0% (0/133) 1. 00 - Target Vessel MI 3. 4% (9/265) 2. 3% (3/133) 0. 76 - Ischemia driven-TLR 2. 6% (7/265) 2. 3% (3/133) 1. 00 TLF (CD/TV-MI/ID-TLR)

12 -Month Definite/Probable ST 0 days 37 days 208 days 393 days BVS at Risk 266 262 260 257 Co. Cr-EES at Risk 134 132 131

Characteristics of ST Cases • The 6 ST cases appear to be at high risk for ST (BVS: 1. 5% / 4 cases, Co. Cr-EES: 1. 5% / 2 cases) – Small residual in-segment MLD post-procedure (4 BVS, 2 Co. Cr-EES) – DAPT discontinuation (1 BVS, 1 Co. Cr-EES) – Diabetes (2 BVS, 1 Co. Cr-EES) – No post-dilatation or underexpansion (2 BVS, 0 Co. Cr-EES)
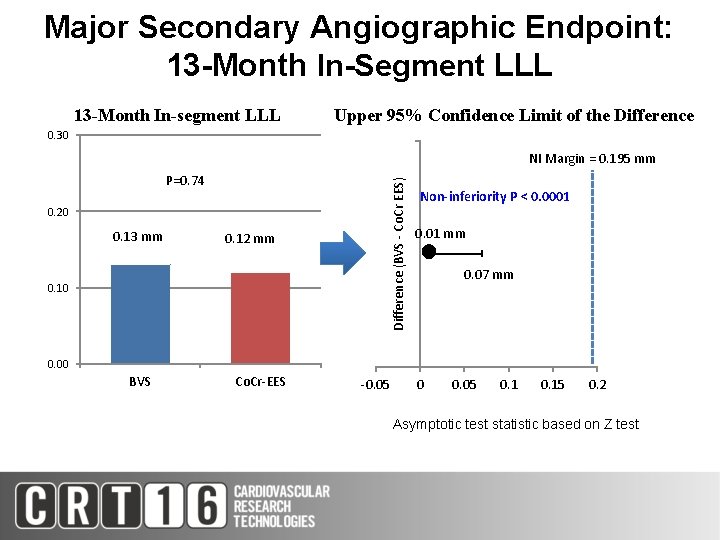
Major Secondary Angiographic Endpoint: 13 -Month In-Segment LLL 13 -Month In-segment LLL Upper 95% Confidence Limit Differnce and 95% UCLof the Difference 0. 30 P=0. 74 0. 20 0. 13 mm 0. 12 mm 0. 10 Difference (BVS - Co. Cr EES) NI Margin = 0. 195 mm Non-inferiority P < 0. 0001 0. 01 mm ● 0. 07 mm 0. 00 BVS Co. Cr-EES -0. 05 0. 15 0. 2 Asymptotic test statistic based on Z test
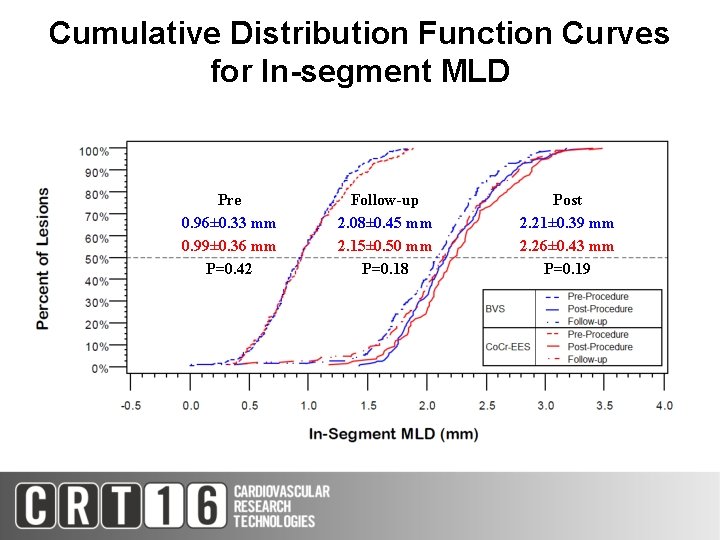
Cumulative Distribution Function Curves for In-segment MLD Pre 0. 96± 0. 33 mm 0. 99± 0. 36 mm P=0. 42 Follow-up 2. 08± 0. 45 mm 2. 15± 0. 50 mm P=0. 18 Post 2. 21± 0. 39 mm 2. 26± 0. 43 mm P=0. 19
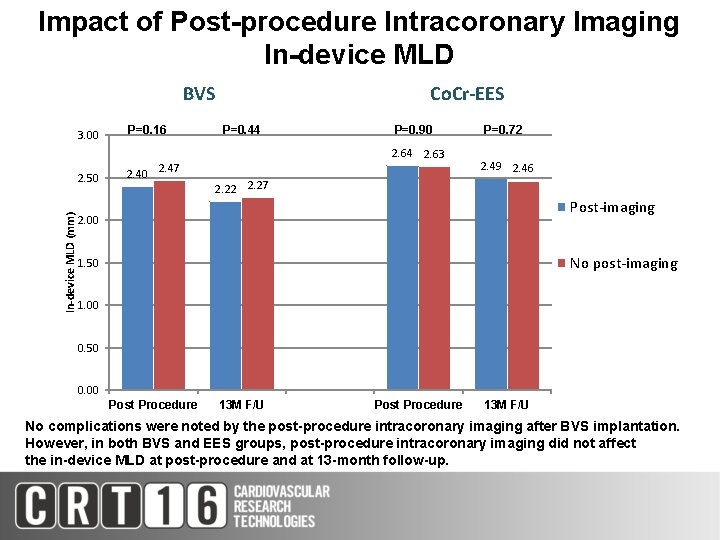
Impact of Post-procedure Intracoronary Imaging In-device MLD (mm) BVS 3. 00 P=0. 16 2. 50 2. 47 Co. Cr-EES P=0. 44 P=0. 90 2. 64 2. 63 P=0. 72 2. 49 2. 46 2. 22 2. 27 Post-imaging 2. 00 No post-imaging 1. 50 1. 00 0. 50 0. 00 Post Procedure 13 M F/U No complications were noted by the post-procedure intracoronary imaging after BVS implantation. However, in both BVS and EES groups, post-procedure intracoronary imaging did not affect the in-device MLD at post-procedure and at 13 -month follow-up.

Study Limitations 1. Large non-inferiority margin for the primary clinical endpoint, particularly with event rate lower than anticipated • • ABSORB Japan was designed to support regulatory approval of the Absorb BVS in Japan. The Japanese Regulatory Agency requested a clinical primary endpoint and agreed to a relatively large non-inferiority margin to keep the study sample size reasonable. Although TLF rates of both BVS and Co. Cr-EES were lower than the anticipated rate of 9%, the 0. 39% observed difference (P=0. 85) suggest that the 2 devices are similar. 2. Underpowered to evaluate the low frequency events such as ST 3. Inclusion of a highly selected patient population • • The study provides data for a patient population typical of pivotal studies for approval. Data in broader patient populations will be studied in subsequent trials.

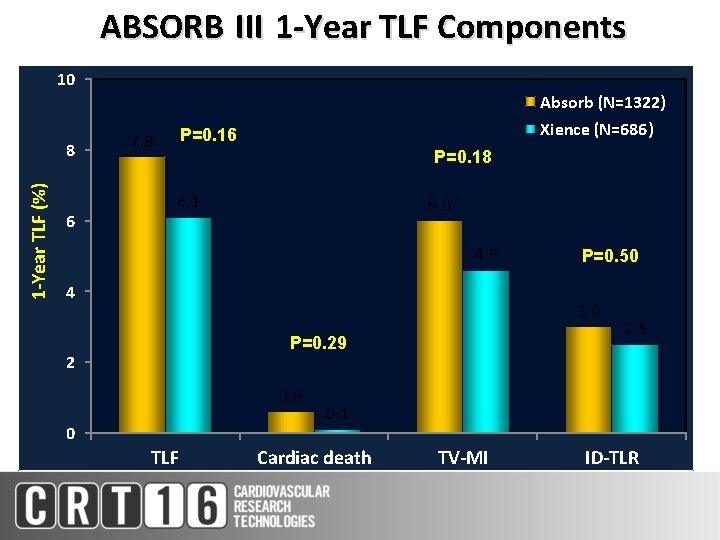
ABSORB III 1 -Year TLF Components 10 Absorb (N=1322) 1 -Year TLF (%) 8 6 Xience (N=686) P=0. 16 7. 8 P=0. 18 6. 1 6. 0 4. 6 4 P=0. 50 3. 0 P=0. 29 2 0. 6 0 TLF 2. 5 0. 1 Cardiac death TV-MI ID-TLR

Device Thrombosis to 1 Year Absorb (N=1322) Xience (N=686) p-value 1. 54% 0. 74% 0. 13 - Early (0 to 30 days) 1. 06% 0. 73% 0. 46 - Late (> 30 to 1 year) 0. 46% 0. 00% 0. 10 - Definite* (1 year) 1. 38% 0. 74% 0. 21 - Probable (1 year ) 0. 15% 0. 00% 0. 55 Device Thrombosis (def*/prob) *One “definite ST” in the Absorb arm by ITT was in a pt that was treated with Xience
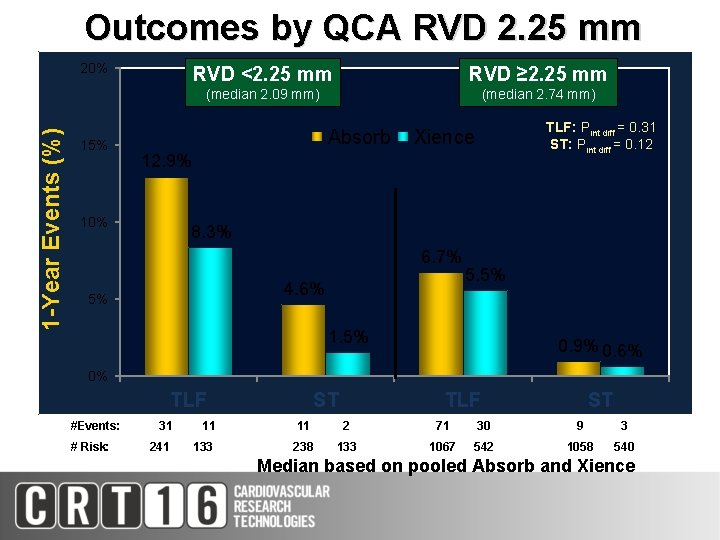
Outcomes by QCA RVD 2. 25 mm 1 -Year Events (%) 20% 15% RVD <2. 25 mm RVD ≥ 2. 25 mm (median 2. 09 mm) (median 2. 74 mm) Absorb TLF: Pint diff = 0. 31 ST: Pint diff = 0. 12 Xience 12. 9% 10% 8. 3% 6. 7% 4. 6% 5% 5. 5% 1. 5% 0. 9% 0. 6% 0% TLF #Events: 31 11 # Risk: 241 133 ST TLF ST 11 2 71 30 9 3 238 133 1067 542 1058 540 Median based on pooled Absorb and Xience
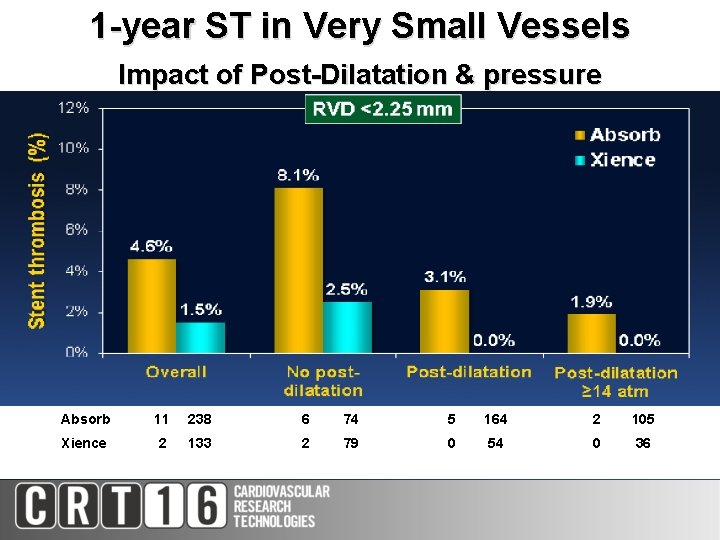
1 -year ST in Very Small Vessels Impact of Post-Dilatation & pressure Absorb 11 238 Xience 2 133 6 74 5 164 2 105 2 79 0 54 0 36
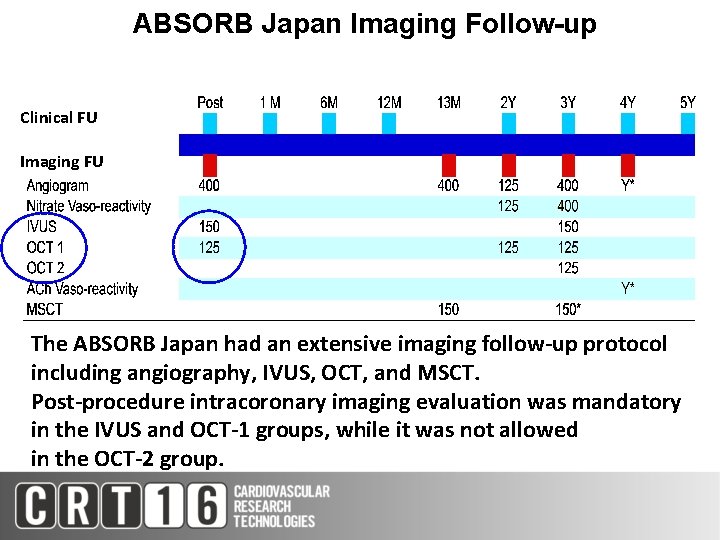
ABSORB Japan Imaging Follow-up Clinical FU Imaging FU The ABSORB Japan had an extensive imaging follow-up protocol including angiography, IVUS, OCT, and MSCT. Post-procedure intracoronary imaging evaluation was mandatory in the IVUS and OCT-1 groups, while it was not allowed in the OCT-2 group.
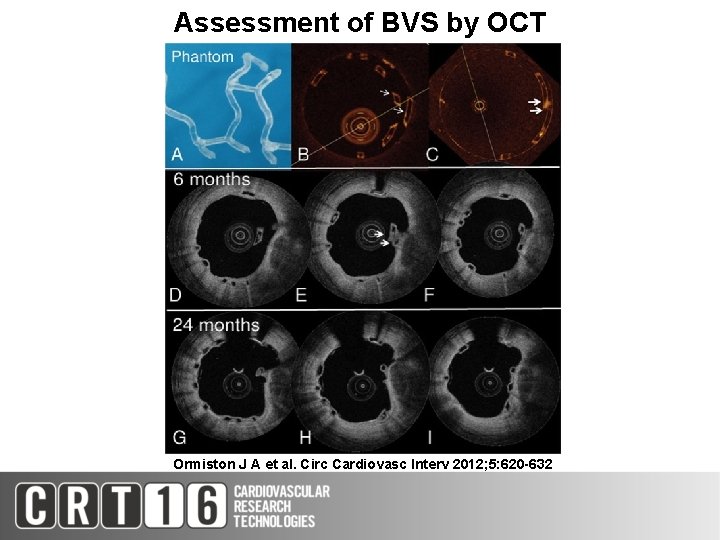
Assessment of BVS by OCT Ormiston J A et al. Circ Cardiovasc Interv 2012; 5: 620 -632
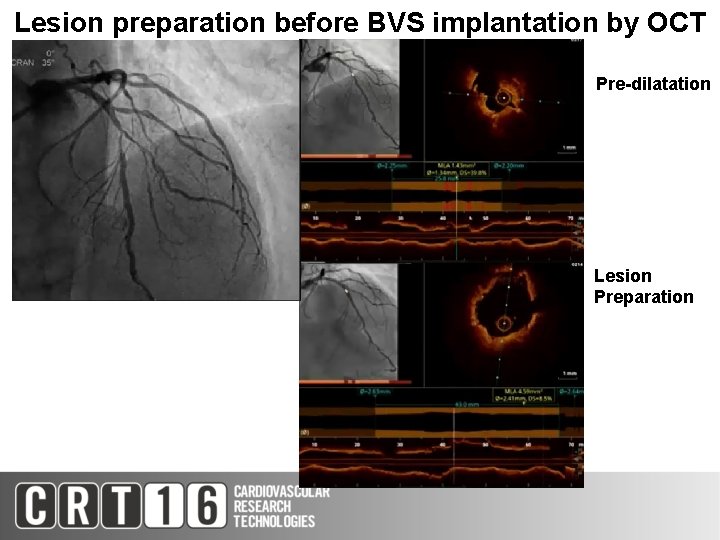
Lesion preparation before BVS implantation by OCT Pre-dilatation Lesion Preparation

Conclusions Ø In the ABSORB Japan trial, BVS demonstrated a similar mid-term (12 -month) clinical safety and efficacy profile as Co. Cr-EES, with comparable 13 -month angiographic outcomes. Ø A risk of scaffold thrombosis has been reported in BVS, especially in cases with small RVD, lesion preparation before BVS implantation and post dilation with high pressure may allow us to reduce scaffold thrombosis. Ø Further coronary imaging studies using OCT, etc. , may demonstrate the mechanism of scaffold thrombosis in BVS in detail in the near future.

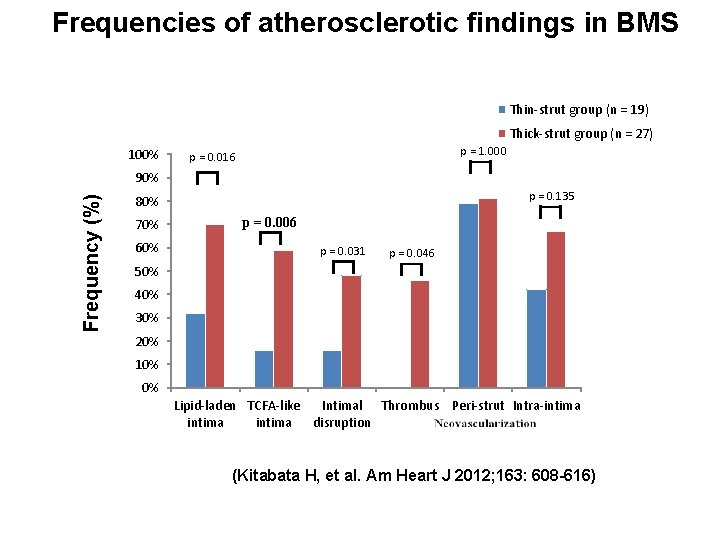
Frequencies of atherosclerotic findings in BMS Thin-strut group (n = 19) Thick-strut group (n = 27) 100% p = 1. 000 p = 0. 016 Frequency (%) 90% p = 0. 135 80% 70% 60% p = 0. 006 p = 0. 031 p = 0. 046 50% 40% 30% 20% 10% 0% Lipid-laden TCFA-like Intimal Thrombus Peri-strut Intra-intima disruption (Kitabata H, et al. Am Heart J 2012; 163: 608 -616)
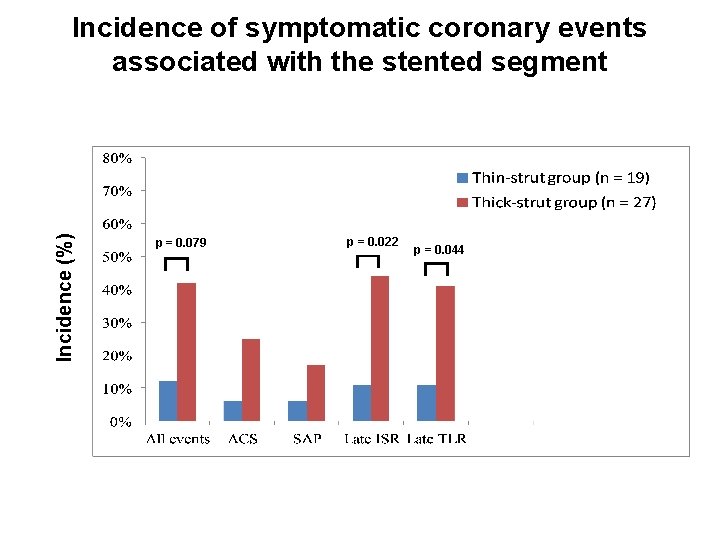
Incidence (%) Incidence of symptomatic coronary events associated with the stented segment p = 0. 079 p = 0. 022 (Kitabata H, et al. Am Heart J 2012; 163: 608 -616) p = 0. 044
- Slides: 37